Abstract
Objective
The study explores the attitudes of people with chronic health conditions towards the use of group-based telerehabilitation.
Design
A qualitative research study.
Setting
The setting involved semi-structured focus groups via videoconferencing software.
Participants
A purposive sample of 18 people with chronic health conditions including cardiorespiratory, neurological and musculoskeletal conditions was recruited via national patient advocacy and support groups in Ireland and clinical contacts. The sample included both those who had, and had not, previously engaged in telerehabilitation programmes.
Procedures
An online questionnaire collected demographic information and data regarding previous telerehabilitation participation and telerehabilitation preferences. Focus groups were conducted using videoconferencing software, in accordance with the Consolidated Criteria for Reporting Qualitative Research (COREQ) Checklist, and analysed using thematic analysis following Braun and Clarke's methodology. Findings were triangulated with quantitative questionnaire data.
Results
Four focus groups were conducted including participants with chronic cardiorespiratory (
Conclusions
Telerehabilitation is convenient for people with chronic conditions; however, concerns exist regarding the use of technology and the limitations of this healthcare delivery method. The role of telerehabilitation is valued, and future programmes should acknowledge patient preferences including a hybrid model of care, exercise and educational content, social interaction and synchronous components.
Introduction
Chronic conditions, including cardiorespiratory (CR), neurological and musculoskeletal (MSK) conditions, are a leading cause of morbidity and disability worldwide. 1 The increasing prevalence and burden of chronic disease present a significant socioeconomic burden and challenges health care services. 2 Group rehabilitation programmes emphasising patient education and exercise are an integral aspect of chronic condition management.3–5 Nevertheless, healthcare services often lack the capacity to deliver these programmes, while patient engagement can be effected by barriers such as time and travel limitations.6,7
Telerehabilitation (rehabilitation via telecommunication technologies such as videoconferencing or telephone calls) can increase service accessibility and patient engagement by overcoming barriers to traditional in-person rehabilitation. Furthermore, telerehabilitation is as effective as traditional in-person rehabilitation for many people with chronic conditions.8–10 The recent COVID-19 pandemic accelerated the adoption of telerehabilitation for patients with many health conditions. Notwithstanding the potential benefits of telerehabilitation, resistance has been demonstrated by both patients and healthcare providers, leading to reduced uptake of these services. 11
Despite clinical heterogeneity between diverse chronic conditions, their recommended self-management programmes are similar, often consisting of progressive exercise training and education to optimise general health. 12 While there is plentiful research investigating single-condition rehabilitation programmes (e.g. cardiac rehabilitation),13–15 recent evidence points to the potential efficacy of generic rehabilitation programmes which include patients with a diverse range of chronic conditions.12,16,17
Patient attitudes towards telerehabilitation have been explored in condition-specific cohorts.18–21 However, less is known about how patients perceive generic group telerehabilitation programmes designed for a range of chronic health conditions. Therefore, the aim of this research is to explore the attitudes of people with a range of chronic health conditions towards group-based telerehabilitation and the acceptability of generic telerehabilitation programmes.
Methods
This study employed a qualitative approach involving online, semi-structured focus groups and was conducted and reported in accordance with the Consolidated Criteria for Reporting Qualitative Research (COREQ) Checklist. 22 Ethical approval for this study was granted by the Faculty of Education and Health Sciences Research Ethics Committee in the University of Limerick (EHSREC 10_RA01).
We recruited a diverse sample of adults with chronic health conditions, including both those who had and had not previously engaged in condition-specific telerehabilitation programmes, using a purposive sampling technique. A diverse sample was sought to ensure a range of chronic health conditions were included, specifically participants with CR, neurological and MSK conditions. All participants had undertaken some form of condition-specific rehabilitation previously, in various settings, including in-person, telerehabilitation, group and individual settings. Participants were recruited via national patient advocacy and support groups in Ireland that serve these patient cohorts, as well as the clinical contacts of the authors.
Patient advocacy and support group leaders were contacted by email outlining the research project and were provided with invitation leaflets outlining the study aims and the eligibility criteria. These were then shared with potential participants via relevant social media and telecommunication platforms to seek expressions of interest. Interested participants who contacted the authors were then provided with a patient information leaflet containing further detail regarding the study processes and eligibility details. Participants were eligible for inclusion if they were aged 18 years or older, had fluent spoken or written English, and had a diagnosis of any chronic CR, neurological or MSK condition. Therefore, people with acute orthopaedic, mental health or cancer diagnoses (for example) were not eligible.
Participants were contacted by email to ensure they had read and understood the information leaflet and to address any outstanding concerns. Interested individuals then provided online consent and were provided with an invitation to the online focus group.
In advance of the focus groups, participants completed brief online questionnaires to collect demographic data and their thoughts on telerehabilitation programmes. The online questionnaire collected demographic information including participants’ age, sex, chronic health condition(s), previous telerehabilitation experience and future telerehabilitation preferences including acceptability of generic telerehabilitation programmes for individuals with various chronic conditions. The questionnaire included multiple choice questions and statements using a five-point Likert scale to indicate participant levels of agreement to collect data regarding preferences for future telerehabilitation programmes and acceptability of a generic telerehabilitation programme (see Supplemental Material S1 for the full questionnaire).
Qualitative data were collected through semi-structured focus groups using a videoconferencing platform (Microsoft Teams). Each focus group lasted between 30 minutes and 60 minutes with participants located in their own homes. Focus groups were conducted by the first author (CBW), a female physiotherapist with three years of postgraduate physiotherapy and research experience who was completing PhD research at the University of Limerick exploring the use of telerehabilitation for people with chronic health conditions. Participants did not have a relationship with the interviewer prior to study commencement. Options to use telephone calls were available if participants did not have access to video conferencing software. This was to ensure participation by individuals with a range of technological access and abilities; however, all participants opted to engage using the videoconferencing platform. Four focus groups were conducted according to the following patient groupings: (a) one focus group included CR patients only (
Baseline demographic data and information pertaining to attitudes towards telerehabilitation collected in the questionnaire were analysed descriptively. Qualitative data were automatically transcribed using Microsoft Teams software. Thereafter, the first author (CBW) checked the transcripts and edited minor errors relating to sound quality and accent variation, by comparing the transcripts to the video recordings. Transcripts were returned to focus group participants for comment or correction to ensure accuracy. A bottom–up thematic analysis, using the principles of grounded theory, was conducted on data collected through the focus groups. 27 The transcripts were initially reviewed by CBW to familiarise with the data. Transcripts were then coded to identify patterns in the data. The transcripts were also reviewed by a second author (RC; a physiotherapist with qualitative research experience) and coded to identify patterns in the data. Both authors independently organised the codes into categories and developed a list of themes and subthemes. A codebook of themes and subthemes were discussed and agreed upon collaboratively by all research team members. A sample of 40% of the collected data were then re-coded individually by two independent authors (CBW and RC) using the established codebook to ensure agreement. As a high level of agreement between coders was demonstrated, the remainder of the data was coded by one independent author using the established themes and subthemes. Qualitative findings were triangulated with relevant quantitative questionnaire data to ensure trustworthiness. Data management and analysis were supported using Microsoft Word and Excel software for organisation, storage and analyses by CBW and RC.
Results
A total of 18 participants with chronic health conditions, including 10 males (55.6%), with a mean (SD) age of 58.7 (12.8) years, were recruited. Due to the method of recruitment, the number of people who were contacted to participate is unknown. Therefore, it was not possible to calculate a participation rate.
Participant characteristics are described in Table 1. The primary chronic health conditions reported were CR (
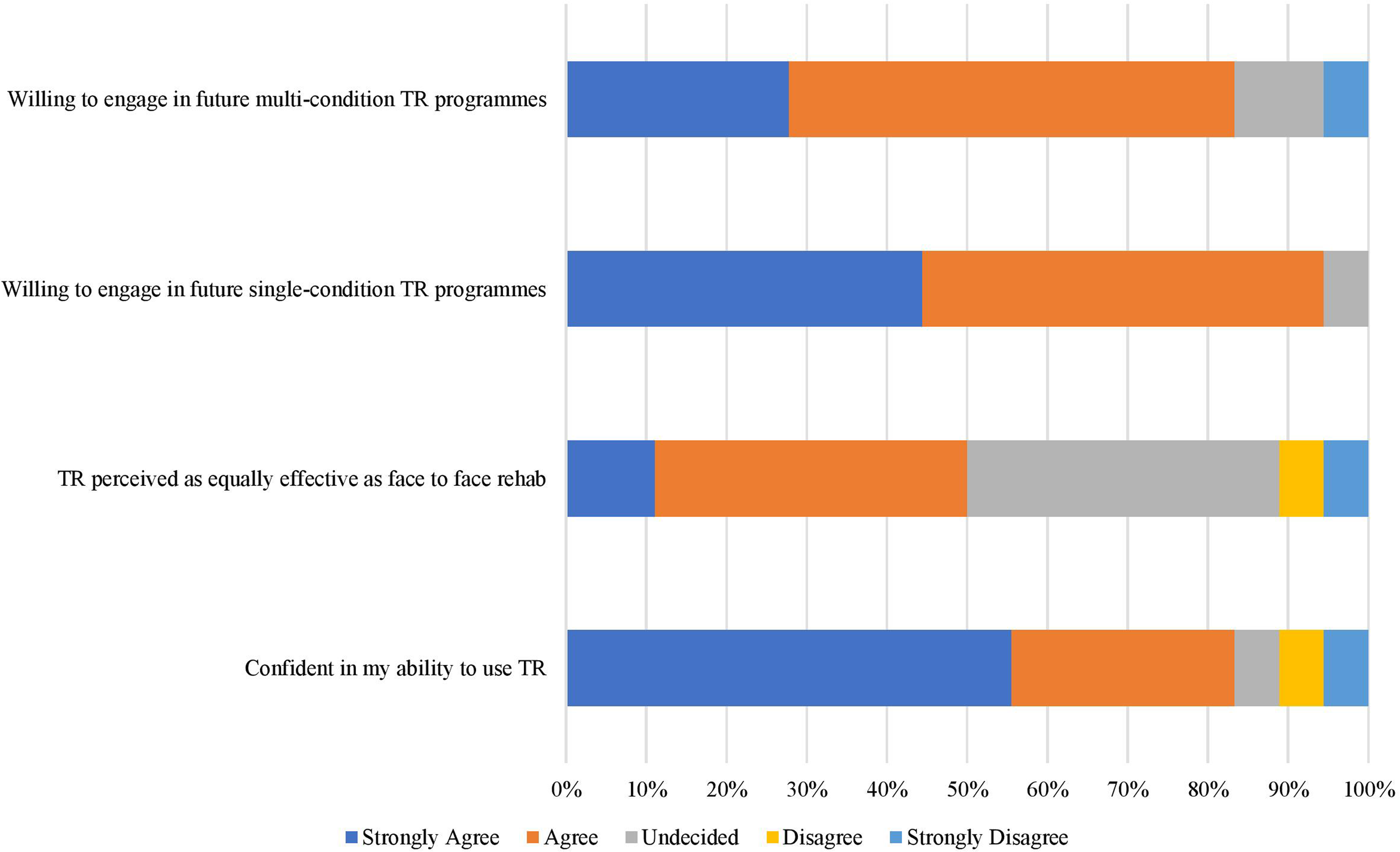
Participant attitudes towards engaging in telerehabilitation (TR) programmes.
Participant demographics (
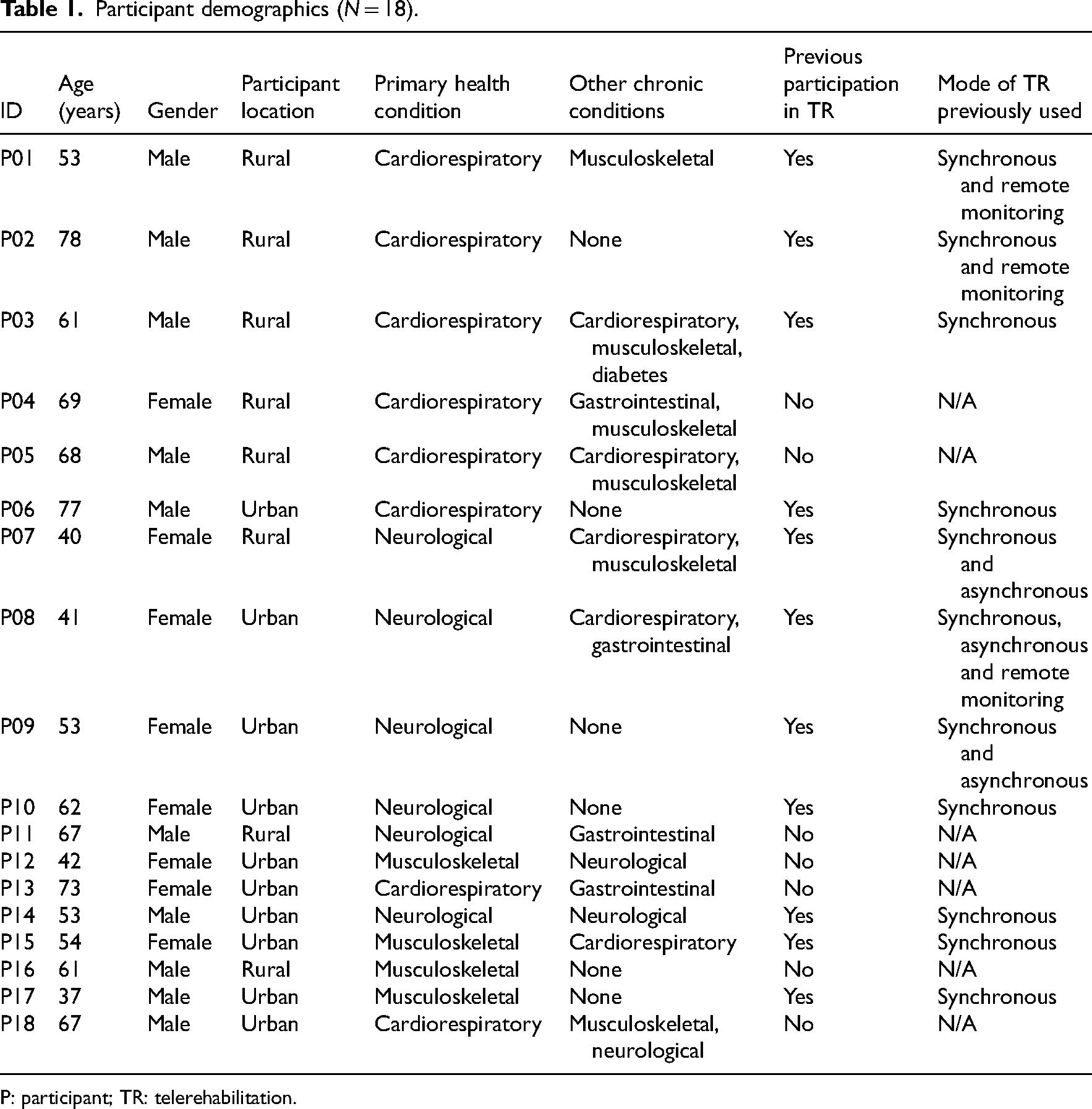
P: participant; TR: telerehabilitation.
The qualitative results are outlined through key themes and subthemes as outlined in Figure 2. The three key themes include (a) benefits and facilitators, (b) challenges and barriers and (c) preferences.

Key themes and subthemes.
Benefits and Facilitators
Convenience
Convenience was stated as a major benefit of telerehabilitation in each focus group. Participants noted the increased accessibility of rehabilitation services and the benefit of avoiding the need to travel to specific locations to attend in-person rehabilitation sessions. Benefits included the absence of fatigue associated with travel to rehabilitation locations and the cost savings to patients by eliminating fuel costs for patients and rental costs associated with the delivery of traditional rehabilitation for healthcare providers and patient advocacy and support groups. Convenience…then like, just not having to go somewhere for me was big thing…And also then I suppose it was mainly about not having to travel. (Participant (P)16, male (M), MSK)
The convenience of participating from the safety and comfort of one's own home, particularly when unwell, was also cited. It's great if you’re not feeling well, you don’t have to get up and get out, you can actually attend the classes at home, and in the comfort of your own home, you don’t have to be going out in the rain to go to a hall. (P03, M, CR)
Technology
Participants believed that technology has the ability to increase accessibility of rehabilitation and is ‘ Plus, the fact that a lot of you know we say the physio and all that is all gone up online now so you can go back and check it again. You know if you don't make the class today you can do it online again. (P09, F, N)
The positive impact of external technical support from family members and friends to facilitate patient engagement with telerehabilitation was highlighted. The impact of the provision of training and education on the use of technology to facilitate engagement among patients with chronic health conditions with telerehabilitation was discussed. Leaders in patient groups stated: We need somebody to go in more than once a week for the first month maybe, and teach them (patients) how to use the device and I think it will work then once the right people get them…That's what we need. (P04, F, CR)
Patient Safety
As evident during the recent COVID-19 pandemic, telerehabilitation offered an opportunity for patients to access classes without the risk of spreading infection or additional threats to their health. There's no fear of catching the virus through meeting up with a group, so the zoom is really safe. (P03, M, CR)
Participants also commented on the strategies that optimised patient safety during telerehabilitation, including strategies to limit the risk of falls and injuries. With the online they ask for a contact number…So they’ve got the backup number, the emergency number to contact if I did fall or hurt myself. (P13, F, CR)
The benefit of increased personal attention received from instructors in telerehabilitation classes and how this can be maximised in smaller group classes was also raised.
Social Benefits
The majority of participants commented on the social benefits and connection that telerehabilitation provided, in particular the potential to establish and maintain new connections and relationships. The benefit of this connection particularly for vulnerable, isolated participants was discussed. I have friends in most other parts of the country, that I didn’t know existed. That's what this is about. It brings the whole country together. I think it's the connection for people…especially during winter when older people can’t get out, or many of us (can’t). (P04, F, CR)
Challenges and Barriers
Technology
The challenges associated with the use of technology, and how this created a barrier which could potentially reduce engagement, were emphasised across each focus group. Discomfort with technology and the associated fear and anxiety, particularly among elderly patients, adversely affected uptake and engagement in these programmes. Zoom is very good, but we lost about two-thirds of our participants from the face-to-face meeting through the Zoom because they either didn’t have Wi-Fi or didn’t feel comfortable with Zoom. (P02, M, CR)
Issues with access to technology, devices, Wi-Fi, poor broadband quality and financial limitations were also cited as challenges and barriers. You might get some freezing and things like that so that's probably a bit of a con as well and then you have to think again in your older population you know Internet access and how tech savvy the older population might be. (P17, M, MSK)
Quality of Telerehabilitation
Participants noted the potential limitations associated with the quality of telerehabilitation. The inability of clinicians to provide “hands-on” assessments and treatments was particularly highlighted by those with chronic MSK conditions. Some participants also raised issues regarding the quality of the interaction between the clinician and patients and the potential for a lack of personal attention from clinicians when delivering rehabilitation remotely. How much you’re getting out of the session in terms of value for money because you know you’re not getting a hands on assessment or you’re not getting a hands on treatment. (P17, M, MSK)
The perceived limitations associated with the quality of telerehabilitation treatment converges with the quantitative data (Figure 1) which shows that only half of participants agreed that telerehabilitation is as equally effective as traditional in-person rehabilitation, while the other half of participants were undecided or did not agree with the statement.
Safety and Social Limitations
Challenges and concerns relating to patient safety when engaging in telerehabilitation were identified, specifically the pressure that patients felt to push themselves beyond their own limits and ability levels. I find it hard to and then I push and I hurt myself afterwards I am like oh my gosh. Maybe that would be easier in a real class to sit back. (P08)
Some participants also suggested potential danger regarding patient privacy issues and concerns associated with the improvisation of the patients’ environment and equipment including technology devices. Yeah, the other one might be I dunno is there a danger around privacy…obviously, you know, there could be perhaps some some risks there. (P16: MSK)
The social challenges and limitations associated with telerehabilitation were highlighted in all of the focus groups. It was perceived that patients missed out on the social aspect of engaging in rehabilitation when participating via telehealth. They also highlighted the limited social element when telerehabilitation is compared to traditional in-person rehabilitation classes. You miss out on the chat and a cup of tea and also the chance for people living alone to actually get out of their house and meet up with their friends. There is a huge difference because when you’re doing classes people are talking to one another and having a laugh, that doesn’t happen on the zoom. (P03, M, CR)
Preferences
The vast majority expressed preference for the option to engage in telerehabilitation in the future and noted the value of telerehabilitation delivery beyond the COVID-19 pandemic. This converges with quantitative data (Figure 1) which shows that all but one participant agreed that they would be willing to engage in future telerehabilitation programmes with other people with similar chronic health conditions. The neurological cohort particularly expressed interest in engaging in future telerehabilitation programmes following previous positive experiences with well-established programmes. The majority of participants stated that they would prefer to engage in a hybrid model of care including a combination of telerehabilitation and in-person rehabilitation. This converges with quantitative data showing a preference for a hybrid approach to future telerehabilitation programmes ( I’d go for a mix of the two. Yeah, I’d go for a blend cause I think they have different values for each of them and you know combination of the two to me it would appear most suitable for the kind of needs I have anyway. (P16, M, MSK)
Differences regarding the preferred mode of telerehabilitation delivery were noted across each group. Most participants commented on the value of synchronous modes of telehealth that facilitate real-time interaction between the telerehabilitation instructor and patients. They noted the value of increased guidance, monitoring and motivation from the healthcare professional when using synchronous modes of telehealth such as real-time telephone and video calls. This converges with quantitative data showing that all participants stated a preference for some synchronous component to be included in future telerehabilitation programmes. The advantage of being able to ask questions to the healthcare provider during synchronous telerehabilitation classes was also reported. Well pre-recorded is not a very good idea because I think it should be live. Uh, so we can keep an eye on the people how they are doing. Uh, and ask personal questions as well. So if you pre-recorded you have no idea what you’re doing. (P02, M, CR)
Benefits of asynchronous telerehabilitation included the potential to review the content at patients’ own convenience via recorded content, which can facilitate increased exercise performance among patients who may not be able to attend regular classes. Quantitative data shows a preference by the majority of participants ( If you miss it or you can’t get there at that time having that to fall back on, you know, and a bit of common sense, to take it careful when you’re doing it. Again, it won’t suit some people. I find it convenient. If I couldn’t, if I missed the class to be able to look back. (P01, M, CR)
Most participants valued group telerehabilitation classes but noted a preference for smaller group sizes to ensure sufficient personal attention for each patient from the healthcare professional leading the class. The MSK cohort noted that they had limited experience in group telerehabilitation settings, with most of their experience consisting of one-to-one telerehabilitation sessions with a healthcare professional.
The composition of future potential telerehabilitation offerings was discussed across the groups. The value of exercise and education, which are typically included in rehabilitation programmes, was noted; however, the inclusion of a social component in programmes was also recommended. Yep, we’ve done our exercises twice a week and every two months or that we’d have somebody, a dietitian or maybe somebody talking even on things like what you are entitled to social welfare and all like that…and every now and again as well we go away for a day and we have a Christmas meal and it's important to make it a social thing as well. (P03, M, CR)
The majority valued the delivery of telerehabilitation by a healthcare professional, highlighting the value of synchronous telerehabilitation allowing direct communication with the professional. They also suggested that telerehabilitation programmes should include a variety of exercises to promote patient engagement and expressed preference for the inclusion of some form of objective monitoring during telerehabilitation classes and programmes. The CR cohort in particular noted the importance of objectively monitoring clinical parameters during telerehabilitation programmes. The approach (to telerehabilitation delivery) does change a bit and so going forward if it was something that you’re looking at to sort of improve or to be able to standardize…maybe the way they monitor the people taking the class at the moment. They just have a look, which is fine to make sure that everyone looks OK, but when you’re doing the official pulmonary rehab with the people from the hospital then you have a little oxygen thing on your finger and they’ll ask you every so often what your oxygen was like. (P01, M, CR)
Participants agreed that from previous experience that the standard duration of 45 minutes to 1 hour class length was appropriate for telerehabilitation. There were varied opinions regarding the overall length of programmes. Some expressed a preference for twice weekly classes for a period of 6–8 weeks, while others felt that rolling classes with an ongoing follow-up beyond a 6–8-week period would promote long-term adherence and benefit.
Perspectives regarding generic group telerehabilitation programmes for a range of chronic conditions varied. Similarities in rehabilitation for different chronic health populations such as educational components were noted, in particular by the MSK cohort. I think like that general advice kind of, you know, around lifestyle factors…is not just for musculoskeletal conditions or things like that…certainly lifestyle and stress and diet and exercise and things like that…doesn’t necessarily need to be tied to one specific condition. (P17, M, MSK)
However, concerns were raised regarding how different groups might need different types and intensities of exercise, especially by the CR cohort. Some of the exercise we do, uh, they’re pretty strenuous enough like you know, and is it putting pressure on other people that mightn’t be able to do it. Like you know, I know they say sit down if you get tired and all that like. (P06, M, CR)
Nevertheless, most were open to future generic group rehabilitation if it could be tailored to meet their needs and guided by a healthcare professional. This converges with quantitative data (Figure 1) showing that the majority of participants ( I wouldn’t mind if people had different conditions as long as the person given the class was doing it properly for everyone there. (P01, M, CR)
Discussion
This study provides an insight into the attitudes and preferences of people with chronic health conditions towards the use of group-based telerehabilitation and the acceptability of a generic group telerehabilitation programme for people with different chronic conditions. The perceived benefits of telerehabilitation including convenience, increased accessibility and safety concur with previous international research including elderly patients, 24 chronic CR,19,28 neurological 20 and MSK 23 populations. Likewise, barriers and limitations of telerehabilitation including difficulty with the use of technology, social and safety limitations, limited interaction with rehabilitation providers and the lack of a ‘hands-on’ approach have also been cited previously.19,20,23,29 Strategies identified to overcome the barriers, including provision of training, education and external support with the use of technology, are consistent with previous suggestions of strategies to enhance telerehabilitation engagement. 19
Sociodemographic characteristics, lifestyle and general health-related factors have been found to be important predictors of telerehabilitation adherence.30–33 Access to, and the appropriateness of, telerehabilitation may be greatest among specific patient cohorts, including those with higher sociodemographic status, digital literacy, intrinsic motivation and self-efficacy levels and general health status. If this is not accounted for, telerehabilitation may reinforce existing healthcare inequities.34,35 Creative technological, attitudinal, and financial solutions, such as the provision and optimisation of technology and resources, are required to overcome these disparities and optimise delivery for a more diverse sample.
The recent COVID-19 pandemic forced a rapid adoption of telerehabilitation services for people with chronic health conditions. Despite the recent return to traditional in-person rehabilitation programmes, our study sample recognised the value of future telerehabilitation delivery beyond the pandemic as an adjunct to traditional in-person rehabilitation. A preference for a hybrid model of rehabilitation combining both traditional in-person and telerehabilitation approaches, rather than complete substitution of traditional approaches with telerehabilitation, mirrors previous findings.19,23,24,28 Other preferences for future telerehabilitation programmes included the use of synchronous modes of delivery, with some recorded material also made available, the value of group rehabilitation classes, inclusion of exercise, education and social components to programmes, along with periodic objective monitoring of clinical parameters, echoing previous research findings.36,37
Rehabilitation providing self-management support is a primary intervention for various chronic health conditions. Evidence exploring the effects of generic self-management programmes, such as the Stanford Chronic Disease Self-Management Programme (CDSMP) model that can be used for a heterogeneous sample of patients with chronic conditions, is promising.12,38,39 Generic programmes have been developed under the hypothesis that people with different chronic conditions have comparable challenges and that similar self-management techniques and strategies can be used across a variety of these conditions. 12 However, our findings highlight the mixed attitudes of people with chronic health conditions towards engagement in generic group telerehabilitation programmes for a range of chronic conditions. While some are willing to consider engaging in generic telerehabilitation programmes, others show a reluctance to this due to perceived distinctions across condition-specific rehabilitation programmes.
The strengths of this study include the purposive sampling technique which ensured a diverse sample participated in the study, providing a wide range of perspectives and experiences. Focus groups included participants with a diverse range of chronic conditions and included both those who had and had not previously participated in telerehabilitation programmes. This enhances the generalizability of our findings. This study was conducted and reported in accordance with COREQ reporting guidelines to ensure transparency. 22 Two authors independently coded a sample of each transcript, using an established codebook of themes and subthemes agreed by the authors from initial review of the data, to enhance rigour of the analysis process. Several limitations are also worth noting. Focus groups were conducted via videoconferencing software, which may have deterred the participation of individuals with limited technological access or abilities. Those who agreed to participate could potentially have higher levels of technical literacy and therefore may be more positive about, and accepting of, telerehabilitation. Although options to participate in focus groups via telephone call were provided to support the participation of those who did not have access to videoconferencing software, it is a potential limitation of the study. We acknowledge the small sample size of the study, however, as previously discussed, data collection ceased when saturation was reached within the data arising from the entire mixed sample, aligning with the aims of the study. It also aligns with the recommendations of Guest et al. 26 who suggest that at least three focus groups are enough to identify the most prevalent themes within a data set. The small sample size may limit the generalizability of the findings to a broader population. We acknowledge that thematic analysis of the data collected within each patient subgroup was not performed, nor did we reach data saturation within each of the different patient subgroups; however, the aim of this research was not to compare the themes that arose across the different subgroups. Participants were recruited via national patient advocacy and support groups, as well as the clinical contacts of the authors. Therefore, the participants are more likely to be among a cohort that participates proactively in their own healthcare management which may limit the generalizability of the study findings. Additionally, our study recruited participants from Ireland, a developed country with a very highly developed economy according to the United Nations Human Development Index (HDI). 40 Therefore, the findings may not be representative of the attitudes of patients from other countries, particularly developing and underdeveloped countries. Many of the comments surrounding previous experiences of telerehabilitation were made by participants who had previously participated in telerehabilitation. However, we included participants with no previous experience of participating in telerehabilitation to gain insight into their preferences and expectations for future telerehabilitation programmes to reflect the large number of people with chronic health conditions who are yet to be exposed to telerehabilitation. While the MSK cohort was most concerned with the lack of ‘hands-on’ therapy with telerehabilitation, they also reported the least experience with group-based telerehabilitation. Therefore, we cannot rule out the possibility that a MSK cohort with greater prior experience of telerehabilitation might be less concerned.
The attitudes of people with chronic health conditions towards the use of telerehabilitation and the acceptance of a generic group telerehabilitation for people with a range of chronic health conditions have been explored in this study. Consideration of these perceptions and preferences could help to inform the development and facilitate success of future telerehabilitation programmes.
Offering training and support could help patients overcome challenges associated with telerehabilitation participation. Future programmes should use hybrid delivery models, synchronous and recorded content and include exercise, educational and social components. It is still uncertain if a generic group telerehabilitation programme for different chronic conditions would be acceptable among patients.Clinical message
Supplemental Material
sj-pdf-1-cre-10.1177_02692155231197385 - Supplemental material for Exploring attitudes of people with chronic health conditions towards the use of group-based telerehabilitation: A qualitative study
Supplemental material, sj-pdf-1-cre-10.1177_02692155231197385 for Exploring attitudes of people with chronic health conditions towards the use of group-based telerehabilitation: A qualitative study by Caoimhe Barry Walsh, Roisin Cahalan, Rana S Hinman and Kieran O’Sullivan in Clinical Rehabilitation
Supplemental Material
sj-pdf-2-cre-10.1177_02692155231197385 - Supplemental material for Exploring attitudes of people with chronic health conditions towards the use of group-based telerehabilitation: A qualitative study
Supplemental material, sj-pdf-2-cre-10.1177_02692155231197385 for Exploring attitudes of people with chronic health conditions towards the use of group-based telerehabilitation: A qualitative study by Caoimhe Barry Walsh, Roisin Cahalan, Rana S Hinman and Kieran O’Sullivan in Clinical Rehabilitation
Supplemental Material
sj-pdf-3-cre-10.1177_02692155231197385 - Supplemental material for Exploring attitudes of people with chronic health conditions towards the use of group-based telerehabilitation: A qualitative study
Supplemental material, sj-pdf-3-cre-10.1177_02692155231197385 for Exploring attitudes of people with chronic health conditions towards the use of group-based telerehabilitation: A qualitative study by Caoimhe Barry Walsh, Roisin Cahalan, Rana S Hinman and Kieran O’Sullivan in Clinical Rehabilitation
Footnotes
Acknowledgements
The authors would like to thank those who participated in this study for their contributions and national patient advocacy and support group leaders and clinical contacts of the authors for their support with participant recruitment.
Author contributions
All authors contributed to the study design and interpretation of data and commented on the final manuscript. CBW conducted data collection. CBW, RC and KOS led data analysis. CBW, RC and KOS drafted the manuscript. All authors agreed to the final version of the paper.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: CBW is funded by an Irish Research Council Government of Ireland Postgraduate Scholarship (GOIPG/2022/1854) and a Plassey Campus Life Services Scholarship. RSH is supported by a National Health & Medical Research Council Senior Research Fellowship (#1154217).
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
