Abstract
Objective
To compare the effectiveness of a McKenzie Method intervention in patients with sciatica with guideline-based patient education.
Design
Multi-centre, assessor-blinded, parallel-group, randomised trial
Setting
Two tertiary hospitals providing operative spinal care.
Subjects
Sciatica patients with magnetic resonance imaging-confirmed lumbar disc herniation compressing a nerve root.
Interventions
The McKenzie group received specific back exercises for seven visits combined with an educational book, and the Control group received a single session of self-management guidance according to usual practices.
Main measures
The primary outcome was the number of surgical operations. Secondary outcomes were pain measured using the Visual Analogue Scale, disability using the Oswestry Disability Index and health-related quality of life using a RAND-36 questionnaire at baseline and 24-month follow-up.
Results
Altogether 66 patients, mean age of 43 years, of which 50% were females with long-lasting sciatica, mean 16 weeks, were randomised to two groups. Nineteen patients (29%) had surgery. There was no significant difference in surgery rates between the groups. Back and leg pain decreased, and disability improved in both groups. Health-related quality of life improved in six dimensions out of eight in both groups. There were no significant between-group changes in the patient-reported outcomes at the follow-up.
Conclusions
Multiple sessions of McKenzie-based back exercises with a McKenzie-specific patient's educational book produced effects equal to guideline-based advice at long-term follow-up. However, the power of these results is diminished due to the small patient population and confounding factors.
Introduction
Sciatica is a clinical diagnosis based on symptoms of lumbosacral radicular pain to the lower leg(s). 1 Lumbar disc herniation is the common cause of sciatica. 2 Spontaneous regression of lumbar disc herniation occurs commonly as the herniation loses its volume; thus, the natural course is often favourable.3,4 Four to 6 weeks is the recommended conservative management for sciatica in primary care.1,5,6 If symptoms persist, magnetic resonance imaging is considered.7–9 Surgery is indicated by severe radicular pain or with serious or progressive neurologic deficits when imaging demonstrates stenosis caused by lumbar disc herniation.5,6,8 Koes et al. 5 estimated that only 5%– 20% of patients with symptomatic lumbar disc herniation require surgery. Systematic reviews comparing surgery and usual conservative care favour surgery because it results in faster pain relief, but no statistically significant differences in pain and disability after 1 year were found.9,10
The McKenzie Method is a mechanical diagnosis, and therapy has shown to be a reliable and validated method for assessing, classifying and treating the lumbar spine. The method has been given the highest rating of any musculoskeletal therapy classification system for low back-related leg pain.11–13 The McKenzie Method classifies the patients’ signs and symptoms by pain behaviour into validated syndromes to define appropriate management strategies using standardised mechanical loading testing.11,13 In the ‘derangement syndrome’, the radicular pain is decreased or abolished distally and remains above the knee or in the lumbar area with specific exercises. This centralisation phenomenon has been shown to predict good non-surgical treatment outcomes.14–16 Sciatica patients, who cannot be classified into the McKenzie syndromes are determined to be in the group ‘other’, in which radiating pain below the knee is classified as ‘mechanically unresponsive radicular syndrome’ in which patients have been shown to be more likely to undergo disc surgery. 15
Based on the previous results of the McKenzie Method,14–16 the aim of this present study was to evaluate if physiotherapist-directed McKenzie Method in conjunction with a specific education book is more effective than a guideline-based education alone. The primary outcome was surgery rates. Secondary outcomes were the self-reported back and leg pain intensities, disability and health-related quality of life.
Methods
This study was a prospective multi-centre, assessor-blinded, parallel-group randomised controlled trial performed between January 2018 and December 2021. The study was approved by the Ethics Committee of the Pirkanmaa Hospital Districts, Tampere, Finland (ETL-code R12198) and registered in the Clinical Trial.gov site ID: NCT03572452. The procedure of the study was performed according to the relevant guidelines and regulations of the Declaration of Helsinki.5,6,8,17 The study is reported according to the Consolidated Standards of Reporting Trials (CONSORT) extension for non-pharmacologic trials. 18 The trial was funded by the Jenny and Antti Wihuri Foundation, Helsinki, Finland (number 07.10.2015). The funders had no role in the study design, data collection and analysis, publication or preparation of the manuscript. Experimental treatments were provided to patients at no cost.
Inclusion criteria were Finnish-speaking sciatica patients aged from 18 to 60 years with magnetic resonance imaging–confirmed lumbar disc herniation with nerve root compression and radicular pain of duration longer than 6 weeks. Exclusion criteria were previous low back surgery, treatment of the current back pain episode using the McKenzie Method, pregnancy and unwillingness to undergo surgery. Further, symptoms indicating cauda equina syndrome or lower limb palsy that hinders normal functioning, previous injury from high-impact trauma such as a car accident or high fall and osteoporotic fractures were also excluded. Additional exclusion criteria included signs of serious diseases or ‘red-flag’ symptoms such as any findings suggestive of malignancy; general symptoms such as inflammation, fever, chills or losing weight for an unknown reason; back problems complicated by other diseases such as fibromyalgia, polyneuropathy, neurological diseases, cerebrovascular diseases, central spinal stenosis, myelopathy, syringomyelia and long-term neuropathic pain not related to sciatica.
Patients (n = 162) diagnosed with sciatica in primary healthcare facilities, who had failed to improve with conservative treatments, were referred for further investigations to the spine clinic of the tertiary healthcare district hospitals of Central Finland and South Ostrobothnia, Finland, which are the only hospitals providing operative spinal care in these areas comprising a total population of 770,000. If the medical examination at the spine clinics suggested that a patient may have radiculopathy and possibly would need surgery for treatment, the patient was referred to a lumbar magnetic resonance imaging scan. The criteria for surgery were disc herniation compressing a nerve root, paresis, significant disability and pain, which did not improve using conservative care.
While waiting for their imaging, patients underwent the baseline McKenzie-based assessment by physiotherapists, formally trained and certified in the McKenzie Method with between 15 and 25 years of clinical experience in applying the method. 11 Patients were classified according to the McKenzie Method, randomised and assigned to the McKenzie (n = 34) and the Control (n = 32) groups. The clinical assessment and physiotherapy counselling lasted ∼90 min. Every patient received oral and written information about the study, and they were approved to participate in the study after they signed an informed consent before randomisation. Patients were free to withdraw from the study at any time for any reason.
All patients were advised to avoid bed rest and to continue their normal routines as actively as possible including physical activities with limits permitted by their signs and symptoms. 19 They received a booklet related to the above-mentioned items translated into Finnish. 20 Patients were told to contact the emergency department at the hospital straightaway, if they had weakening of a leg muscle or cauda equina symptoms.19,20 The patients were not informed about the number of therapy sessions before entering of the study, and only maximum number of therapy sessions in the McKenzie group was defined beforehand.
Patients in the experimental group could choose the nearest clinic, where a certified McKenzie therapist was available for their therapy. The treatment period started 1–2 weeks after the baseline assessments and imaging. Fifteen certified McKenzie therapists with an average of 15 (range 2–28) years of experience in the method participated in the implementation of the therapies. The treatment protocol was presented to all therapists in a face-to-face manner, and they also received printed instructions on how to manage the treatment procedures. In the beginning and at the end of the therapy period, a clinical evaluation was done by using the McKenzie Institute's formal lumbar assessment chart as a part of the history taking and physical examination. 11 The physiotherapist-directed McKenzie back exercises were used, combined with hands-on techniques in conjunction with a McKenzie-specific patient's education book. The book has been specifically written for low back pain patients to empower them to take control of their own symptoms. 21 The treatment included an educational component and home-exercise programme with exercises done several times a day according to symptom response. Patients’ individual therapy sessions were once per week for 60 min, up to a maximum of seven visits. The treatments were stopped if a proximal change in sciatica pain location was not observed, and symptoms increased or remained worse after two or three treatment sessions. All patients in the McKenzie group were given an exercise diary to record the numbers of exercises done daily and to rate their low back and leg pain intensities weekly during the intervention period.
Control group patients received a single educational session from a physiotherapist as part of normal practices according to guidelines and recommendations after assessment and classifications at baseline.5,6 This lasted for at least 90 min and included information on the good prognosis of sciatica, the spontaneous regression of intervertebral disc herniation (natural healing)3,4 and pain tolerance and medication. In addition, patients received ergonomic counselling and advice to stay normally active and continue physical activities as recommended by the guidelines.5,6
Background sociodemographic and clinical characteristics were collected with questionnaires. For primary outcomes, the surgery rates were collected from the hospital database at the 24-month follow-up. Back and leg pain intensities during the previous week were measured by the Visual Analogue Scale (VAS) (0 = no pain to 100 mm = worst possible pain). 22 Current disability was reported with the Oswestry Disability Index Finnish Version 2.0 (total scores: 0 = minimal disability to 100 = bed-bound or exaggeration of symptoms). 23 Health-related quality of life was assessed with the RAND-36 Finnish version, 24 which assessed quality of life based on eight health dimensions: general health perceptions, pain, physical functioning, role limitations caused by physical health problems, emotional well-being, social functioning, role limitation caused by emotional problems and energy/fatigue. These eight scores range from 0 to 100 with higher scores indicating better health status and lower scores indicating disability. Data on the use of other treatments not included in the study protocol were collected from self-reported questionnaires. The target sample size of 172 (86 per research group) was estimated to achieve 85% power (α = 0.05) of detecting 25% difference in surgery rates in 24 months (Controls 85% and McKenzie Method 65%) by using the log-rank test (Freedman method). 25
Patients were allocated to the McKenzie or to the Control group using a computer-generated four-block randomisation list from a sealed envelope programme for clinical trials, 26 compiled by a physiotherapist not involved in the clinical examination or treatments. The drawn group was hidden in a sealed envelope so that the person randomising the patient did not know the allocated treatment. All outcome assessors were blinded to the treatment group assignment.
The results are presented as means with standard deviations (SDs), medians with interquartile ranges (IQRs), or as counts with percentages. Statistical comparison between the groups was performed by t-test, Mann–Whitney test or chi-square test, when appropriate. The Kaplan–Meier method was applied to estimate the cumulative surgery rates during 24 months. The log-rank test was applied to test the differences in surgery rates between groups with an exact P-value. Repeated measures of the changes in primary and secondary outcomes were compared between the McKenzie and Control groups with mixed-effect models and an unstructured covariance structure (i.e., the Kenward–Roger Method for calculating the degrees of freedom). Fixed effects included group, time and group x time interactions. The repeated measurements were taken at different time points, including at baseline and at 3, 12 and 24 months. Mixed models allowed analysis of unbalanced datasets without imputation; therefore, we analysed all available data with the full analysis set. In the case of violation of the assumptions (non-normality), a bootstrap-type or permutation test was used. Normal distributions were evaluated graphically and with the Shapiro–Wilk test. All analyses were performed in Stata 17.0 (Stata Corp LP; College Station, Texas, USA). 25
Results
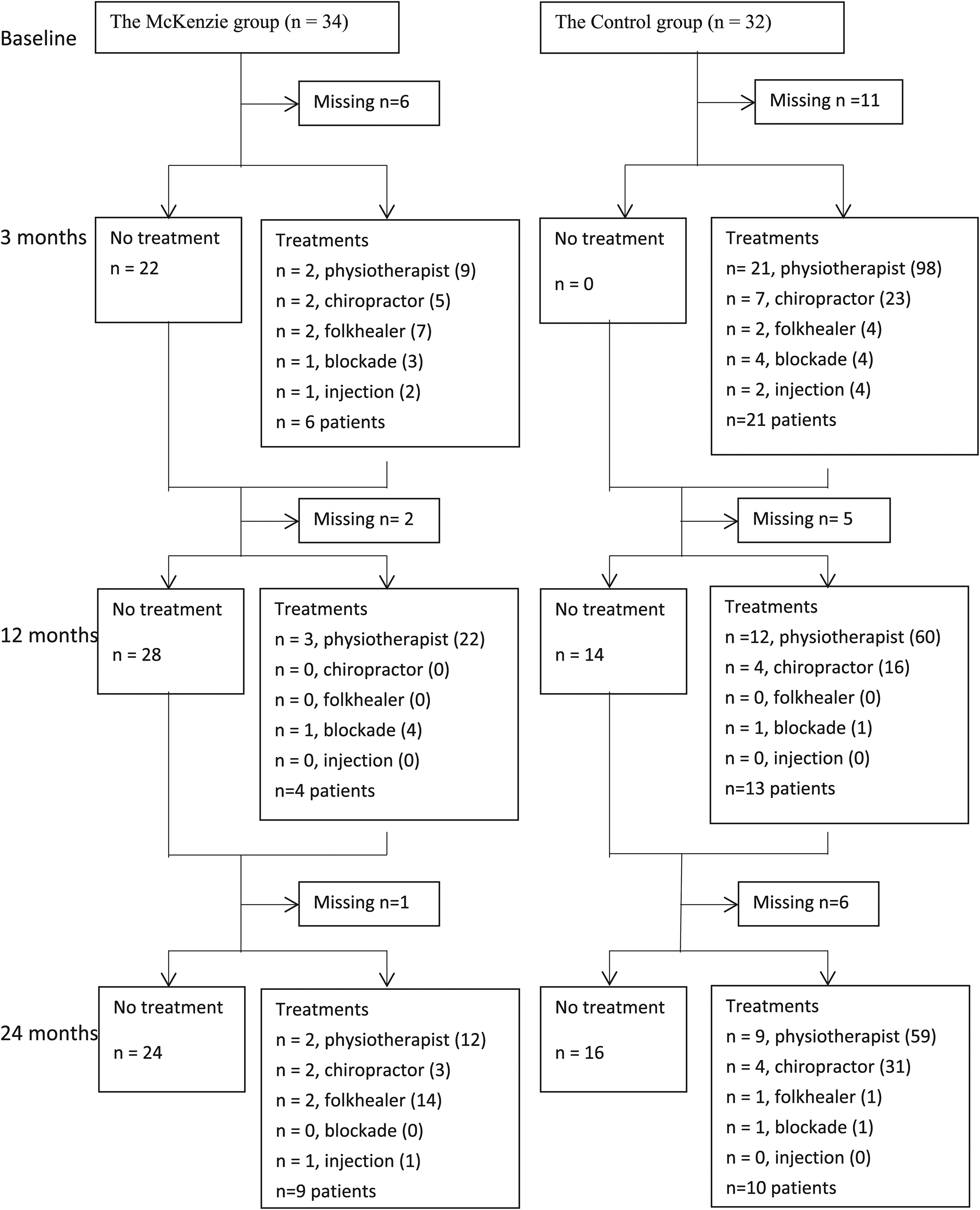
Altogether 66 patients (50% female) with a mean age of 43 years were randomised to two groups, which were similar with respect to sociodemographic data (Table 1). Out of the patients, 83% had a positive straight leg–raising test, in conjunction with other dermatomal patterns related to radiculopathy due to nerve root compression. The median duration of present radicular symptoms was 16 weeks in both groups. The clinical characteristics and outcome measures did not differ between these groups at baseline except that the patients in the McKenzie group had suffered low back pain for a significantly longer time and had more sensory disturbances than the Controls. The trial flow and reasons for exclusion from the study are shown in Figure 1.
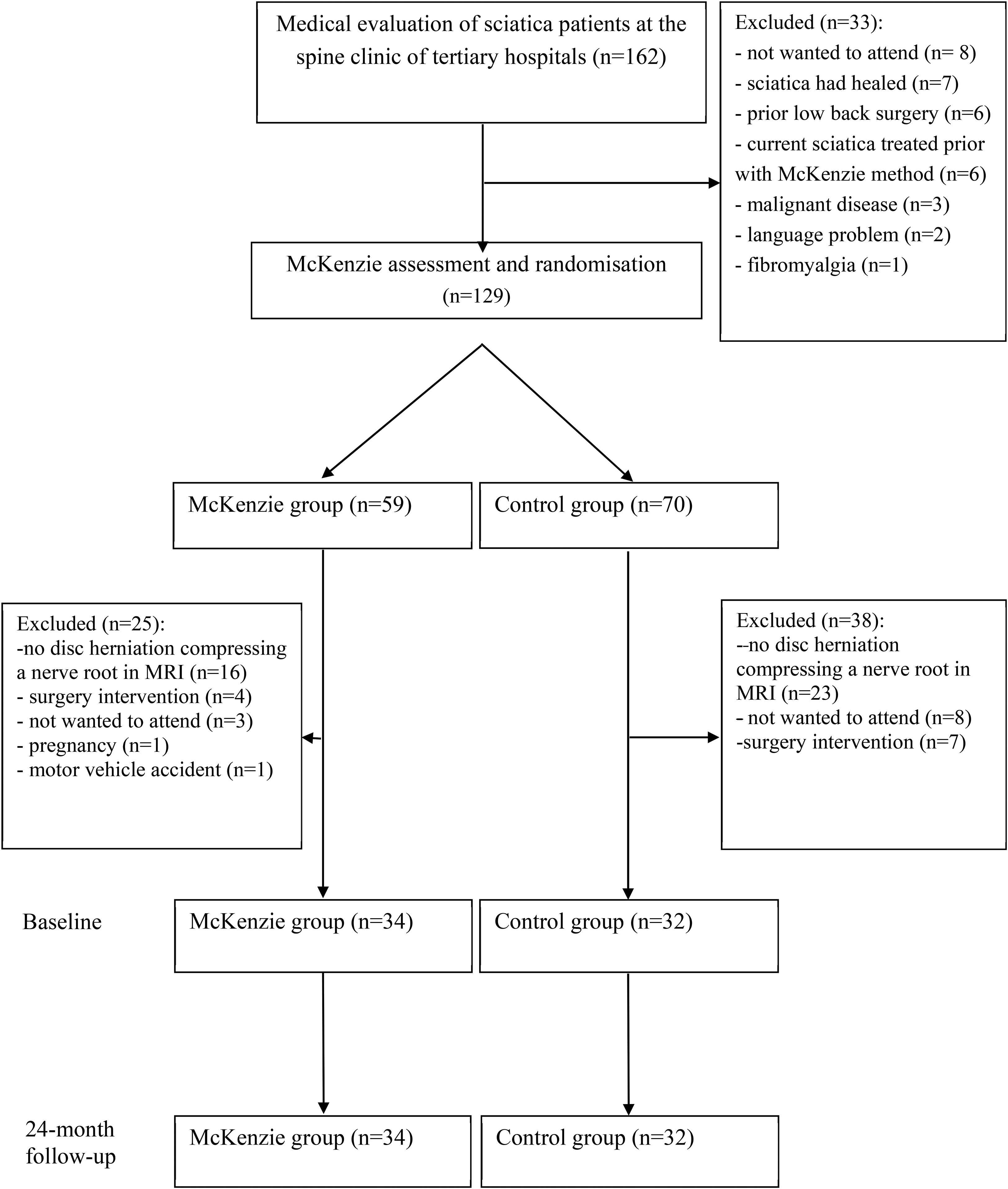
The trial flow chart (n = 66).
Baseline comparison of sociodemographic and clinical characteristics of the sciatica patients assigned in the McKenzie and the Control groups (n = 66).
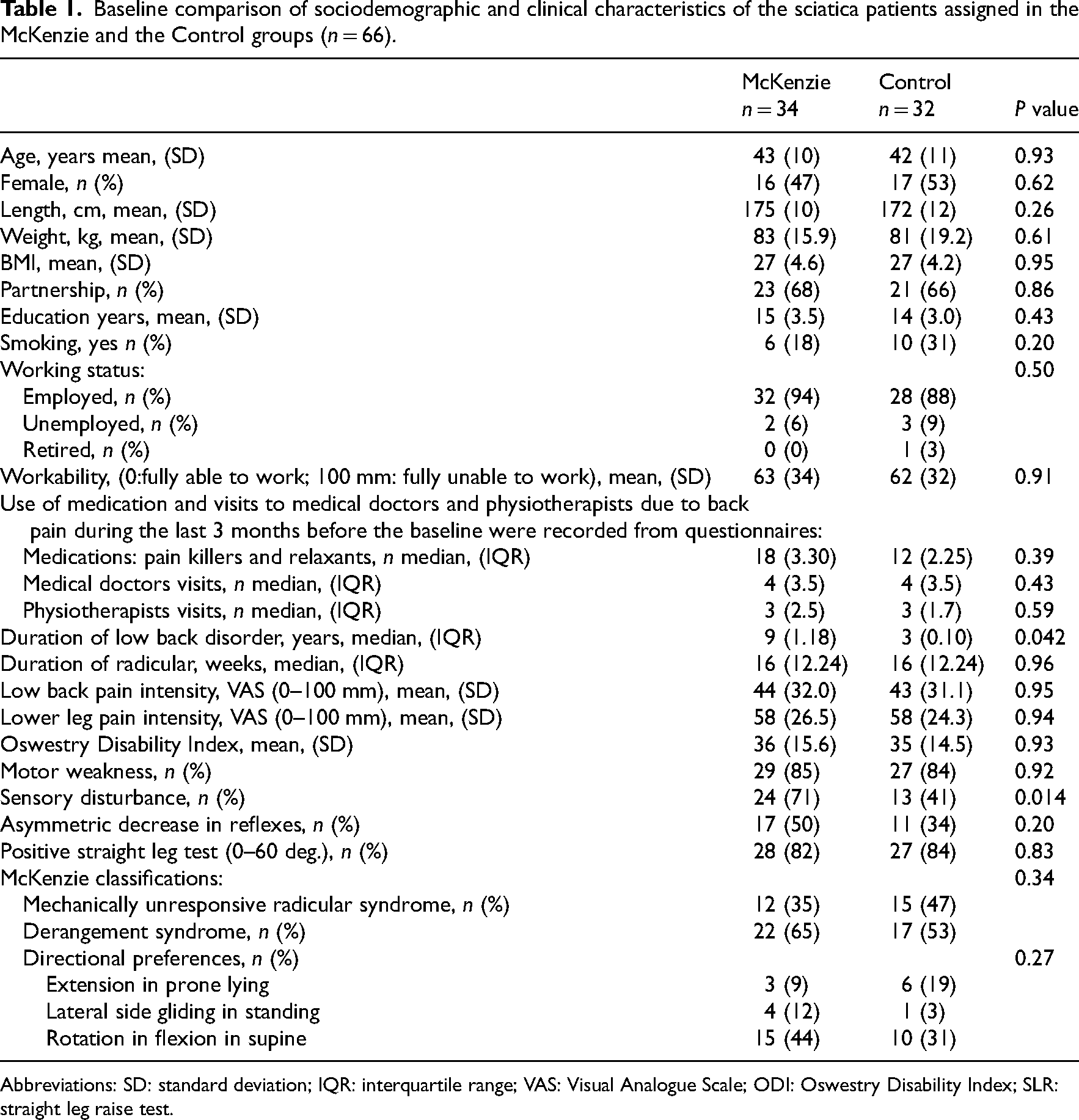
Abbreviations: SD: standard deviation; IQR: interquartile range; VAS: Visual Analogue Scale; ODI: Oswestry Disability Index; SLR: straight leg raise test.
At the 24-month follow-up, nine (27%) patients from the McKenzie group and 10 (31%) patients from the Control group had surgery, mainly during the first 3 months after randomisation (Figure 2). Only one patient assigned to the McKenzie group had surgery after 12 months from the baseline. There was no significant difference in surgery rates between the groups (P = 0.67). Out of the patients, 39 were diagnosed with ‘derangement syndrome’ (centralisers) and 27 with ‘mechanically unreducible radicular syndrome’ (non-centralisers). Five (8%) centralisers and 14 (21%) non-centralisers had surgery.
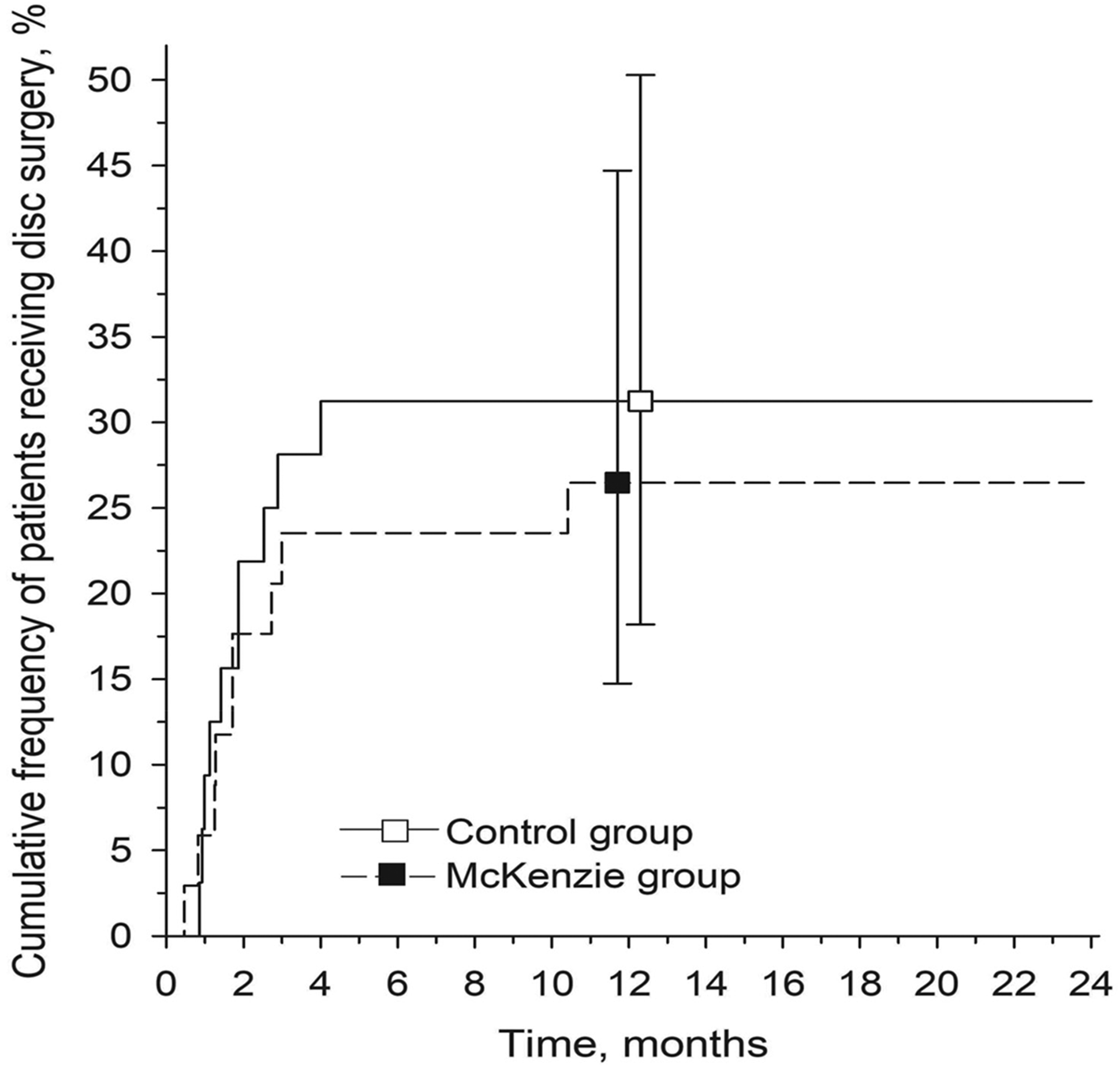
Cumulative surgery rates during the 24-month follow-up (Kaplan–Meier estimate) of patients receiving disc surgery in the McKenzie and control groups. Whiskers represent the 95% CI.
The study was conducted on the condition that it did not interfere with the normal operation of the orthopaedic clinic. Thus, 11 sciatica patients underwent surgery before entering the study. Two patients assigned to the McKenzie group had only two therapy visits, because their surgery dates had been scheduled before they started the therapy.
At the 24-month follow-up, the mean VAS scores for back pain intensity decreased in the McKenzie group by −23 (95% CI −34 to −11) and in the Control group by −20 (−31 to −8), and leg pain decreased in the McKenzie group by −42 (−53 to −30) and in the Control group by −36 (−48 to −24). Disability decreased in the McKenzie group by −24 (−30 to −18) and in the Control group by −21 (−27 to −15) (Figure 3). Six dimensions of the health-related quality of life questionnaire scores improved in both groups significantly during the follow-up, except mental health in the McKenzie group, and vitality and general health in the Control group. At the 24-month follow-up, there were no significant differences in changes between the groups in the health-related quality of life questionnaire scores (Table 2).
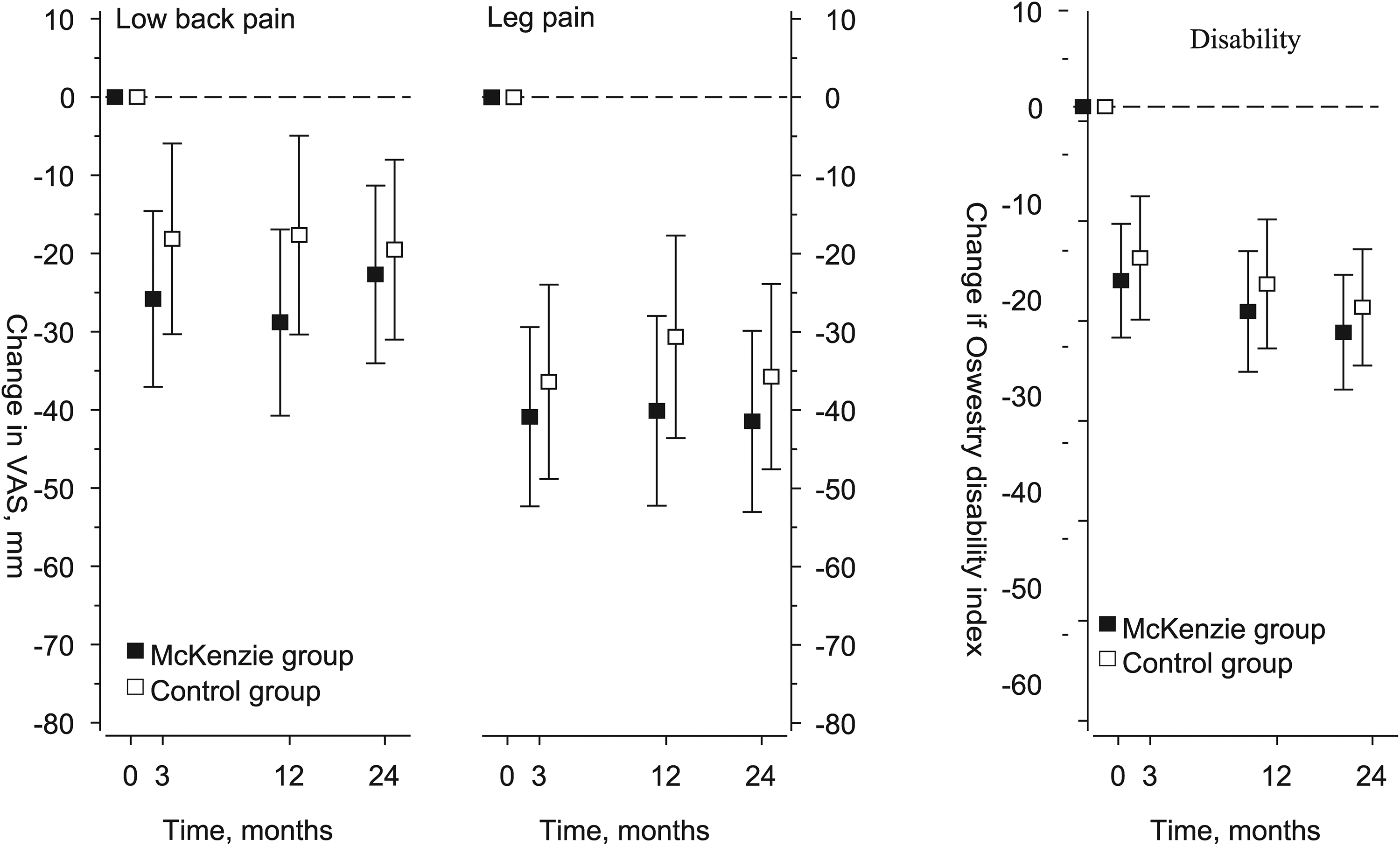
Changes in low back and leg pain intensities measured by using the Visual Analogue Scale (VAS 0–100 mm) and in the Oswestry Disability Index, during the 24-month follow-up in patients with sciatica. Whiskers represent the 95% CI.
Baseline and change values of the RAND-36 dimensions.
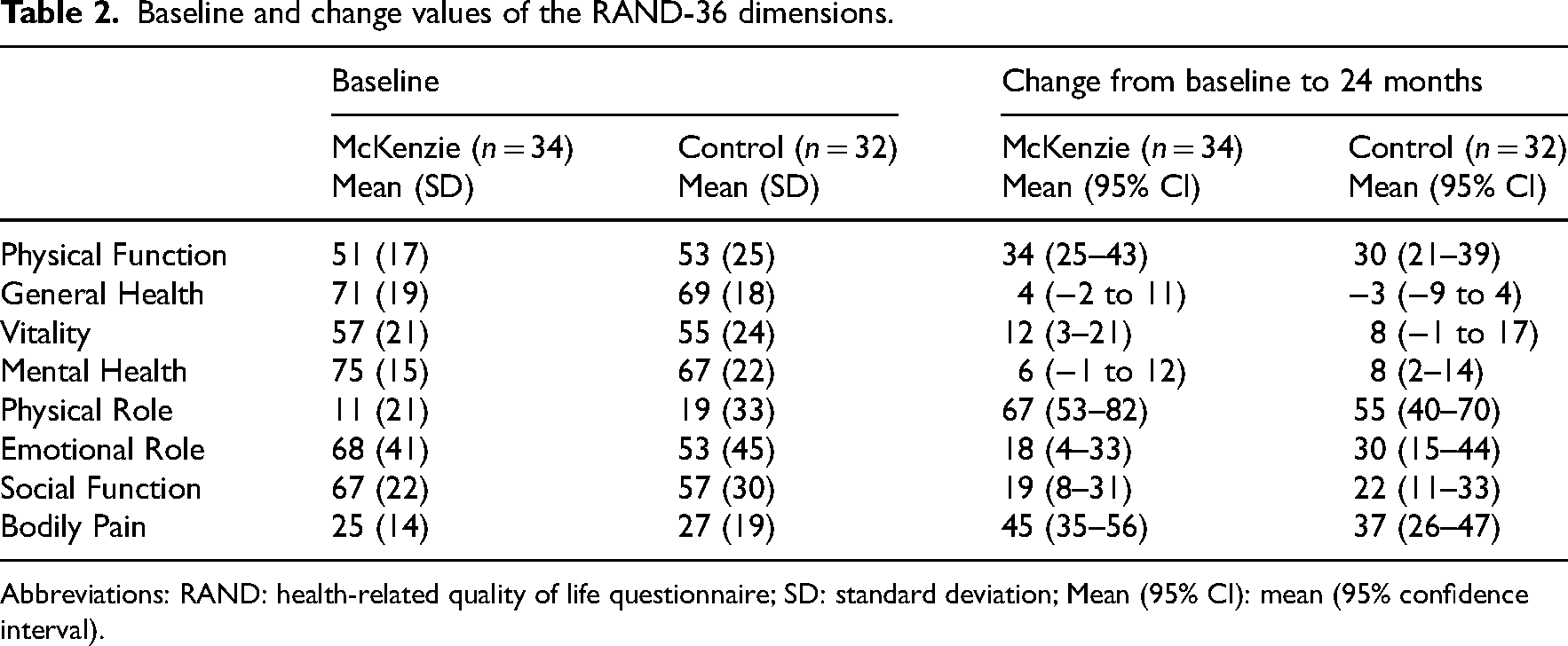
Abbreviations: RAND: health-related quality of life questionnaire; SD: standard deviation; Mean (95% CI): mean (95% confidence interval).
The number of McKenzie treatment visits was on average six (from two to seven visits). Twenty-seven patients (79%) had done home exercises daily from 2 to 20 weeks (mean 13 weeks). The rest (n = 7) had not completed their exercise diaries. Thus, their exercise amounts remain unknown.
From the Control group, a mean of 15 patients (69%) reported that they had received additional therapies during the 24-month follow-up, while from the McKenzie group, a mean of six (26%) had received therapies outside of the study protocol (Figure 4). As adverse events, four patients’ pain worsened during or after the McKenzie treatments: thus, their therapy was stopped after an average of three treatment visits. No other adverse events were noted. There was no re-operation during the follow-up.
The number of additional treatments not included in the study protocol up to 24-month follow-up.
Discussion
Altogether, 19 sciatica patients had surgery due to lumbar disc herniation during the 24-month follow-up, and the surgery rates did not differ between groups. The prevalence rates of herniated disc surgeries may vary markedly between different countries and between different healthcare districts in the same country5,9,27 The total surgery rate of 29% in the present study is in the range from 5% to 54% of previous studies.5,28 The reason for the apparently high surgery rate in the present study may be that the study population comprised patients commonly treated conservatively in primary healthcare for up to 6 weeks according to guidelines before referral to specialist healthcare, or even longer depending on the severity of symptoms and the patient's preference for conservative treatment. Thus, those patients that had already recovered in primary healthcare were not among the study population.
Rasmussen et al. 29 found that in a register-based study, the annual disc surgery rate of sciatica patients decreased approximately from 60 to 80 per 100,000 before 1997 to 40 per 100,000 in 2001 when sciatica patients were treated in spine clinics using the McKenzie Method, while at the same time, the surgery rates increased in other parts of Denmark where the McKenzie Method was not applied. The reason for the reduction in surgery rates could be the use of the McKenzie Method, but it may be also due to another factor like increased attention to conservative treatment. Skytte et al. 15 analysed the surgery rates of the sciatica patients classified as centralisers (n = 25) and non-centralisers (n = 35) from the study by Rasmussen et al. 29 They showed that after evaluation and classification using the McKenzie Method, the sciatica patients with the non-centralisation phenomenon were six times more likely to have surgeries than centralisers. In the present study, centralisers’ surgery rate was 8% and non-centralisers 21%, results which are in line with earlier published studies.14–16
Albert et al. 14 found in their randomised clinical trial that performing the McKenzie Method to treat leg pain in severe sciatica patients improved their condition markedly, but the difference was not significant compared to the Control exercise group, like in the present study. However, the research design differed from the present study as disc herniations compressing a nerve root were not reported, while in the present study, 59% of patients who had sciatica were excluded from the study as they did not have nerve root compression. Fritz et al. 30 compared treatment with the McKenzie Method to the Control group that received usual care, comprised of education, advice and medications, among patients with sciatica. They found that low back and leg pain intensity decreased, and disability improved significantly more in the McKenzie group compared to usual care at the 12-month follow-up. An important difference compared to the present study is that it is not known how many patients suffered pain due to lumbar disc herniation compressing a nerve root, because the study did not include verification with a magnetic resonance imaging scan.
In the present study, pain and disability decreased clinically significantly in both groups, considering that a minimally clinically important difference in a VAS should be at least 20 mm and at least 10 points in the Oswestry Disability Index score. 31 However, there were no significant between-group change differences. Most dimensions of the health-related quality of life questionnaire reached significant improvements during the follow-up, but there were no group-difference changes. The minimally clinically important difference for the health-related quality of life questionnaire is typically in the range of 3 to 5 points, 32 but there were no significant between-group change differences.
Three-quarters of patients in the Control group received additional therapies due to sciatica, not included in the study protocol, while only a minority in the McKenzie group used additional therapies during follow-up. A reason for the difference may be that patients in the McKenzie group received an introduction to more active self-care empowering them to take control of their own symptoms.21,33,34 A pain neuroscience education approach has shown a moderate level of evidence to improve pain and disability in chronic back pain.35,36 The pain neuroscience approach was not implemented as such in the present study, but many elements of the approach were included in both intervention groups. 20
The present study has several strengths. The trial was performed according to the general scientific recommendations of good clinical trials and implemented in line with the guidelines for approaching lumbar radiculopathy.5,6,8 Disc herniation compressing a nerve root was verified to be the cause of sciatica by magnetic resonance imaging. The core principles of the McKenzie Method were used without adding other treatment modalities as used in previous studies.14,19,30,37
There are some limitations in our study as well. The sample size remained smaller than initially planned. The present study attempted to avoid confounding factors due to other conditions and therefore used relatively strict inclusion and exclusion criteria. The main reason for the large number of excluded patients was that magnetic resonance imaging did not confirm lumbar disc herniation with nerve root compression. Some patients did not want to attend the study due to their preference for surgery as soon as possible, and some others accepted only conservative therapy (Figure 1). Recruiting patients was also affected by the small population of the healthcare districts. Five patients in the Control group received advice and therapy according to McKenzie therapy, which caused partial between-group contamination. Most patients in the Control group and a few in the McKenzie group had multiple types of additional treatments outside the study protocol, which may have predisposed the study to treatment bias. Additional therapies may have affected pain and disability outcomes in those patients who received them. However, because the study was not designed to evaluate these situations and because the study population is too small to do sub-analyses, their effect cannot be estimated. Duration of symptoms and sensory disturbances differed between the groups at baseline, and additional treatments during follow-up may be confounding factors. It would be ethically questionable to prohibit patients from seeking additional help if they needed it. It is also impossible to control for the use of additional treatments in a clinical study, and prohibiting these may cause patients to avoid reporting other therapies, which could make the study unreliable in terms of confounding factors.
The present study suggests that multiple sessions of McKenzie-based therapy produced effects that are equal to those of guideline-based advice. The power of these results is diminished due to the small patient population and confounding factors. The mean differences in the outcomes between the treatment groups were statistically insignificant. As it was not possible to find any relevant differences between the treatment groups within a sample size of about 30 patients in each therapy group, these results may not be sufficiently encouraging for contacting a larger study to achieve sufficient statistical power.
Clinical messages
Most patients with prolonged sciatica sent to tertiary hospital for further investigations avoided surgery.
The McKenzie therapy and the guideline-based advice groups showed similar surgery rates and clinically significant improvements in pain and disability at follow-up.
The guideline-based advice group explored more additional therapies than the McKenzie group.
Footnotes
Acknowledgements
The authors wish to acknowledge the grant support received for the research from the Jenny and Antti Wihuri Foundation, Helsinki, Finland. The authors wish also to acknowledge the physiotherapists who assessed the patients in the hospitals and the physiotherapists who implemented the McKenzie Method therapies.
Author contributions
SK, JY, AH, MK, E-PT and JM were involved in protocol development and gaining ethical approval. SK obtained funding for the study. She had overall responsibility for the conducting of the study and for monitoring progress in collaboration with JY, AH, JM and JR. KK, AV and E-PT designed the study protocol and statistical analysis, which was undertaken by HK. SK wrote the first draft of the manuscript, and all the authors contributed to critically revising it. All authors approved the final version of the manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship and/or publication of this article: this work was supported by the Jenny ja Antti Wihurin Rahasto (grant number 07.10.2015).
