Abstract
Contraceptive use has been linked with women’s empowerment and positive health and well-being outcomes. This research examines contraceptive use in Nigeria using an analytical sample of 17,511 women in the 2018 Demographic Health Survey data, first modeling contraception use in general or Some Form of Contraceptive Use with logistic regressions, and second, considering Modern and Traditional Contraceptive Methods as separate, discrete outcomes for the first time using multinomial logistic regressions. We find that women are least likely to use some form of contraception when their partners alone make these healthcare decisions, and that women who make joint earnings decisions with their husband are more likely than women who make earnings decisions alone, to use contraception. Higher educational attainment, more wealth, increased age, being Christian or Catholic compared with Muslim, and living in an urban area are associated with using Some Form of Contraception, all else being equal. When considering Modern and Traditional Contraceptive Methods as distinct outcomes, we find that these same factors shape women’s use of Modern Methods and in similar directions and magnitudes, while most of these relationships hold in similar directions for Traditional Methods, this research fills the gap in modeling Traditional Methods and reveals novel regional differences in Traditional Contraceptive Use. Specifically, the South East and South West Regions are more likely than the North Central region to use Traditional Contraceptive Methods compared with using no method. Finally, we show that a Nigerian woman’s decision-making power, alone or jointly with her husband, translates into a positive influence on using any form of contraception.
Introduction
Contraceptive use among women of childbearing age is a key aspect of reproductive health, with far-reaching potential to improve maternal and child well-being, alleviate poverty, and advance gender equality. Despite these benefits, the uptake of contraceptive methods remains low across many African countries, including Nigeria, where it is below 15% for modern contraceptive methods (Abubakar and Abubakar, 2024). Evidence from demographic and health surveys over the past 20 years reveals that progress in contraceptive uptake has been modest in Nigeria (Abubakar and Abubakar, 2024), which has a high fertility rate, a high maternal mortality rate, and the largest population compared with other African countries.
At the same time, there is broad agreement that the arrival of contraceptive use heralded a new dawn for both women’s quality of life and economic development (Trombley, 2022). After the 1994 Conference on Population Development, a consensus emerged that any effort aimed at empowering women must include access to contraceptives and reproductive health facilities (Do and Kurimoto, 2012), as there is a mutual, two-way relationship between these two areas. While contraceptive use positively affects women’s empowerment, women’s empowerment also increases contraceptive use. Several studies provide evidence of health and socioeconomic advantages associated with using contraceptives. These advantages include better health outcomes and survival rates for mothers, newborns, and infants (Akinyemi et al., 2015; Izugbara et al., 2016), a reduction in poverty rates, and better educational outcomes for women (Bahamondes et al., 2015; Stevenson et al., 2021; Yeatman et al., 2022). Taken together, these studies point to the ability of women to control their reproductive capacity as central to increasing women’s and their family’s health and socioeconomic well-being.
In contrast, a relationship has also been established between the low rates of contraceptive use and high maternal and child mortality rates (Monjok, 2010). Around the world, contraceptives are credited with the aversion of 2.7 million women’s deaths, which amounts to 60 million years of healthy lives saved (Darroch et al., 2008). At the level of individuals or households, women and children from families with high fertility rates are more likely to experience maternal deaths and childhood illnesses and deaths, respectively (Cleland et al., 2012). Indeed, having lower economic development is associated with having a high total fertility rate (i.e. more than 5 children per woman) (Casterline, 2010; Hall and Bass, 2012). The social demographer, Oppenheim Mason (1997), theorized that economic development reduces fertility partly through economics (i.e. higher costs of children), partly through social change (i.e. gender equality, female education), and partly through improved access to reproductive health and family planning. In this way, contraceptive usage goes together with economic development and increasing women’s educational attainment and labor market participation (Gordon, 2002). Research that seeks to explain contraceptive uptake must consider all these factors, as well as their interrelationships.
Beyond controlling fertility, women’s contraceptive use is also a social protection tool, safeguarding both their individual rights and their health rights. A relationship has been established between increased women’s empowerment and contraceptive use for women in 32 countries in sub-Saharan Africa (Yaya et al., 2018), yet there is still work to be done to disentangle what specific measures of women’s empowerment are relevant to move the needle on contraceptive uptake within specific countries and cultures. Likewise, women’s equality and empowerment are the essence of Goal 5 of the 17 United Nations Sustainable Development Goals (UN SDGs), because women’s empowerment is integral to sustainable economic and human development at the individual and community levels (Bass, 2004). Specific to contraceptive use, the UN SDG agenda has set a target of universal access to sexual and reproductive health and reproductive rights by 2030 to bring about increased empowerment for women (United Nations, 2019). Women who face constrained autonomy and reproductive rights are less likely to secure formal education and decent work, and, in turn, this limits their health and life chances as well as the well-being of their children.
More evidence is needed about the role of women’s decision-making power vis-à-vis their partners and contraceptive use in Nigeria, while also considering relevant socioeconomic and cultural factors. Moreover, studies to date have modeled Some Form of Contraceptive Use (Yaya et al., 2018) and Modern Methods of Contraceptive Use (Abubakar and Abubakar, 2024; OlaOlorun and Hindin, 2014; Viswan et al., 2017), but we found no study has considered both Modern and Traditional Contraceptive Use as distinctive forms of contraception within the same model. There is a need to provide this type of comprehensive consideration using the Nigeria Demographic Health Survey (DHS) data. There is also a need for policymakers to consider broader social and cultural factors – such as rurality, religion, and geographic region – while including individual factors, such as women’s lower socioeconomic or wealth status, that also may affect their contraceptive usage (Casterline, 2010).
This research will address these gaps in the literature by testing for the effect of women’s decision-making power vis-à-vis her husband in two areas of decision-making – her healthcare decisions and how her earnings are spent – on the likelihood that she uses contraception. We will first model her propensity to use Some Form of Contraception, and second model her propensity to Use Modern Contraception and Traditional Contraception, each compared with the reference category of using no contraceptive method. Because social processes cluster together, we control for age, religion, rural/urban residence, region of residence, as well as socioeconomic status, which we operationalize as educational level and wealth status, in our models to account for potentially confounding interrelationships.
Understanding low contraceptive uptake in the Nigerian and African contexts
It is critical to understand the factors related to low contraceptive intake in Nigeria, because it is the most populous country in Africa and the sixth most populous nation globally, with 223.8 million people and a population growth rate of 3.2% (World Health Organization (WHO), 2020). Nigeria has a high total fertility rate, 5.3 children per woman, which is markedly higher than the overall fertility rate of 4.1 children per woman for Africa as a whole (WHO, 2020). Nigeria has one of the highest rates of maternal mortality in both West and sub-Saharan Africa. In 2015, 58,000 maternal deaths occurred in Nigeria (WHO, 2020). This means that Nigeria had the second highest absolute number of mothers dying during childbirth in the world in 2015, being second only to India. Moreover, maternal mortality is not felt evenly in Nigeria, as the rural northeast and northwest regions experienced an increase in maternal mortality over the period 2005–2018 (World Health Organization, 2005, 2020).
Nigeria reported a contraceptive-use rate of 6% in 2003 (Population Reference Bureau, 2003), 9.7% in 2008, and 9.7% in 2013 (Austin, 2015), and 12% in 2018 (Fadeyibi et al., 2022). When it comes to issues pertaining to reproductive health, women who come from countries that are developing, such as Nigeria, may have little or no say in whether they can use a contraceptive, especially if they reside in a particular region or rural area dominated by cultural norms limiting women’s status or where patriarchy is the cultural norm. Adding nuance, Feyisetan (2000) points to patriarchal cultural norms within the Yoruba ethnic group to explain why decision-making is left to men on the timing or number of children to have. Corroborating this claim, other studies show that in countries where pervasive patriarchal cultural norms prevail, even when women seem to be increasingly educated and gaining economic independence, men seem to remain in control of decisions relating to women’s reproductive health and fertility (Trombley, 2022). In these contexts of contraceptive uptake, Ogburn’s (1922) cultural lag theory aptly describes this time delay in societies between changes in material culture, such as increased access to education, employment, and birth control methods for women, and changes in non-material culture, such as the norms encouraging high fertility and a specific division of labor in the family.
The high value placed on childbearing and parenthood in many African cultures runs counter to contraceptive use. Because patriarchy is ingrained in some societies, even when women gain some socioeconomic autonomy, they still have high fertility preferences, which has been associated with a cultural norm of wanting to please their husbands (Mason, 1987). Similarly, other research (Wyrod, 2016: 6) explains how the intersection of traditional values, poverty, and development efforts to combat HIV transmission reinforced local gender norms prioritizing men over women, because these efforts did not ‘curtail the traditional male sexual privileges’’. Similarly, Majola (2014) explains how traditional gender roles intersect with low incomes to create a ‘sexual economy’ wherein South African women have limited power to negotiate condom use, resulting in transactional sexual relations, and in turn, low condom and contraceptive use. In addition to women’s fertility wishes, these studies highlight how it is also men’s expectations that can shape the decision to use contraception. Moreover, other research (Trinitapoli and Yeatman, 2018) makes the case that fertility desires are dynamic and context-dependent, rather than being fixed or stable; fertility preferences change over time in relation to health (e.g. HIV transmission risk), caregiving responsibilities, labor market opportunities, and partnership changes. Therefore, research endeavoring to explain contraceptive use should account for decision-making processes within households. Because of this, this research will consider two areas of decision-making between women and their partners, economic and health, as focal variables in this analysis.
Feminist theory, women’s empowerment, and contraceptive use in Africa
Feminist theories have described women’s contraceptive use as women’s declaration of autonomy over their reproduction and reproductive health. Trombley (2022: 1) contends that contraceptive use is a pathway to increased women’s autonomy, because it holds the seeds for the repositioning of women in society as women ‘reclaim their agency and transform the societies they live in’. No matter the angle from which it is observed, feminist theories point to controlling reproduction as being crucial to the liberation of women. It represents a means for women to be free to plan and organize their lives, and it gives women the power to share and redistribute their time however they want. Muller (1974) contends that it is therefore the backdrop for the separation of personal and reproductive identities. The arrival of the pill, a modern contraceptive method, removed the costs for women to enter and stay in long-term careers (Goldin and Katz, 2000). After the pill’s arrival, women were able to exercise more control over their reproduction and could delay their age at first marriage and reduce the penalties for pursuing an education instead of childbirth. As Malhotra (2012) and earlier feminist scholars (Goldin and Katz, 2000; Gordon, 2002; Lerner, 1993) note, gaining authority over contraception has allowed women to push back against patriarchal constraints, most notably those shaping the gendered division of labor.
Feminist theorists hold that when women are freed from both the bearing and raising of children, this fuels fertility and maternal mortality decline. These declines directly or latently enable a transformation in gender relations in society. This happens because women are allowed to participate actively within society, politics, and other realms as they exercise more control over their time. Similarly, Rosaldo et al. (1974) note that gender equality for women in a society is achieved when time is freed up in the lives of women, allowing women to play an active role in changing culture and giving them access so they can contribute in the labor market and the public sphere. Women therefore begin to transform the societies in which they live. Generally, feminists agree and argue that one of the reasons for the gendered division of labor both in the labor market and in households is because of the burden of childbearing that women bear alone (Goldin and Katz, 2000; Gordon, 2002; Lerner, 1993). Taken together, these studies point to the ability of women to control their reproductive capacity as central to women’s empowerment.
Prior research examining the drivers of contraceptive use in the African context has operationalized women’s empowerment using women’s decision-making as measures. For example, Yaya et al. (2018) found that women with high household decision-making power are 1.23 times more likely to use Some Form of Contraceptives compared with those with lower household decision-making power using data from 32 sub-Saharan African countries. Modeling the Use of Modern Contraception Methods, OlaOlorun and Hindin (2014) found that Nigerian women who are more involved in making household decisions, as measured by a higher decision-making score, also exercise more say in making decisions related to their fertility. Similarly, Viswan et al. (2017) used indices for household decision-making and women’s sexual autonomy to find that higher scores in Nigerian women’s relative power vis-à-vis her partner are associated with higher modern contraceptive use; moreover, they found that women in the highest household decision-making power tertile had more than 1.5 times the odds of using modern contraception compared with women in the lowest tertile.
Other research suggests women’s relationships with their husbands are relevant to understanding women’s empowerment, and in turn, their contraceptive use. Richards and Bass (2018) report that in addition to household decision-making power, women’s higher interpersonal power, which is measured as an index taking into consideration many areas of women’s autonomy vis-à-vis her partner, is associated with greater use of modern forms of contraception in neighboring Ghana. Another study using DHS data from Ghana found that husbands’ support of contraception use in general terms resulted in a five times higher usage of contraceptives for women (Lumor et al., 2023). Likewise, a study of six African countries (i.e. Ghana, Cote d’Ivoire, Burkina Faso, Kenya, Malawi, and Tanzania) found that wives who discuss family planning with their partners are more likely to be using contraception than women who report never having discussed this with their partner (Stephenson et al., 2007). Most recently, Abubakar and Abubakar, (2024) found that joint decision-making by women and their partners on contraceptive use is associated with an increased uptake of modern contraceptive methods. Altogether, these studies point to the importance of considering women’s decision-making and autonomy as happening within her relationship with her spouse, and the need to test for different types of specific decision-making in varied household realms as possibly affecting whether women use contraceptives.
Overall, research points to the central role of women’s household decision-making power as a driver of contraceptive use, and that an increase in contraceptive use could be realized by increasing women’s empowerment. At the same time, there remains a need to disentangle what specific forms of decision-making empowerment will move the needle on contraceptive uptake within specific countries and cultures. Equally important, all these studies show that women’s empowerment is interconnected with their educational level and economic status, and that all three of these factors are mutually reinforcing. As women’s educational attainment increases, she is likely to enjoy a higher economic status as well as greater autonomy at the personal and societal levels. Across these studies, there are positive relationships between women’s ability to exercise autonomy and women’s contraceptive use, as well as positive associations across women’s increased education, economic status, women’s autonomy, and modern contraceptive use. This research seeks to fill a gap by considering two specific forms of decision-making – who makes decisions on women’s healthcare and how their earnings are spent – as affecting their contraceptive use, while also considering other factors that may be interrelated.
What factors are associated with contraceptive use in Nigeria?
Women’s contraceptive use in Nigeria has been shown to be associated with other individual and background factors. First, older women and women living in urban areas evidence higher rates of contraceptive use, compared with their younger and rural counterparts (Abubakar and Abubakar, 2024).
Next, women’s higher educational attainment and a higher economic status are both associated with contraceptive uptake in Nigeria and elsewhere. In other words, as education increases, the likelihood of using contraceptives also increases. This link between education and contraceptive use is pivotal, and additionally, other studies have reported the positive relationship between the economic independence of women and contraceptive use (Saleem and Bobak, 2005). Mason (1987) makes the case that increasing women’s educational level is the fundamental way to improve women’s autonomy and social and economic status, pointing to the reinforcing nature across these underlying factors associated with contraceptive uptake. Indeed, Saleem and Bobak (2005) maintain that autonomy is the middle link or intermediary of the relationship that exists between female education and contraceptive use. In agreement, Campbell et al. (2013) maintain that education enlightens women and aids them to consume information critically and to distinguish between facts and opinion. Adding to this, a review (see Blackstone et al., 2017) of 58 studies in African countries finds that both education and employment are positively associated with contraceptive use. This research points to the importance of considering women’s educational attainment and economic status while examining the relationship across women’s empowerment and contraceptive use.
Prior research on Nigeria suggests that religion and region of origin also pattern contraceptive uptake. Muslim women evidence the lowest contraceptive use, compared with Catholic women and women from Other Christian religious make-up. The northeast and northwest regions evidence the lowest contraceptive uptake (with 8.1% and 6.2%, respectively) (Abubakar and Abubakar, 2024). These two regions where contraceptive uptake is the lowest are also predominantly Muslim in religious composition. It is therefore important to consider both religion and region of origin in this examination of what is associated with contraceptive use in Nigeria. Other research using Nigeria DHS data point to both region and urban residence as factors that pattern contraceptive use, finding that Nigerian women living southern regions and urban areas are more likely to use modern contraceptives, compared with those in northern regions and rural areas (Abubakar and Abubakar, 2024; Johnson, 2017; Wang and Cao, 2019). Using data gathered in the low-contraceptive uptake North East region, Kana et al. (2017) found that age, religion, education, and income are key to understanding contraceptive use. Obasohan (2015) found that in addition to the independent effects of education and income, Nigerian women with a Christian religious background were more likely to use contraceptives than their Muslim counterparts, and that women in urban areas, with higher income, and with more autonomy were all more likely to use contraceptives than their counterparts in Nigerian society. These studies point to the need to include education, economic status, urban residence, and regional residence in our analysis.
Finally, the Nigerian contraceptive literature is informed by two distinct modeling strategies, one analyzing the use any form of contraceptive (Yaya et al., 2018) and the second analyzing the use of modern contraceptive methods (Abubakar and Abubakar, 2024; OlaOlorun and Hindin, 2014; Viswan et al., 2017). Our analysis will extend these studies by considering Some Form of Contraceptive Use, and then whether women report Modern, Traditional, or No Contraceptive Method Use within the same model. We posit it is useful to consider whether women are currently using Some Form of Contraceptive, and then to consider Modern and Traditional Contraceptive Use as discrete outcomes within the same model, because whether women use modern or traditional methods, their intent is to limit their fertility. We aim to offer a more comprehensive understanding of what factors affect women’s reproductive health decisions, by differentiating what is associated with contraceptive use generally, and traditional versus modern contraceptive use. To date, we find no other study that has modeled traditional methods for Nigerian women separately, and we would like to add this piece to understanding the Nigerian reproductive puzzle.
Taken together, the prior scholarship suggests two questions which we will address in the following sections. First, what is the effect of women’s decision-making power vis-à-vis her husband on whether she will use contraceptives in general in Nigeria? Specifically, does a woman’s power to make decisions in two areas – her healthcare and how her earnings are spent – affect whether she will use any form of contraception (i.e. contraception in general) and whether she will use modern, traditional, or no contraception, all else being equal?
Data
We use the Nigeria Demographic Health and Survey (DHS) dataset, which is a nationally representative survey which utilized the Population and Housing Census Design sampling frame and was fielded from August to December in 2018 (National Population Commission (NPC) [Nigeria] and ICF, 2019). The Nigeria DHS is used to provide estimates and track development trends using basic health and demographic indicators. The 2018 Nigeria DHS included women aged 15–49 years in the sample households, which is the UN definition for women of reproductive age. This analysis is restricted to married women of reproductive age who completed interviews and provided valid responses to the questions of focus, which resulted in an effective sample size of 17,511 responses. Roughly one-quarter of all women, 25.5%, are unmarried in the 2018 Nigeria DHS, so they are excluded from our analytic sample.
Key variables
Outcome variable
To understand contraceptive usage, the Nigeria DHS asks respondents what current method of contraceptive they use. The responses fall into three categories: (1) No Contraceptive Method; (2) Traditional Contraceptive Method; and (3) Modern Contraceptive Method. Those who said they were currently using no contraceptives were included in the No Contraceptives category. Those who reported using periodic abstinence, withdrawal methods, lactational amenorrhea, periodic abstinence, standard days method, and other traditional methods were included in the second category, Traditional Method. Those who reported using birth control pills, IUDs, injections, male condoms, female sterilization, implants or Norplant, female condoms, emergency, and other types of modern methods were included in the third category, Modern Method.
We treat this variable in two ways. First, we dichotomize the responses to show a difference between those who use No Method coded as 0 and those who Use Some Method whether traditional or modern coded as 1. Second, we also use the variable in its original three-category form, with No Contraceptive Method coded as 0, Traditional Contraceptive Method coded as 1, and Modern Contraceptive Method coded as 2. Figure 1 shows that 86.5% of respondents report that they use no contraceptives, 3.3% report that they use traditional contraceptives, and 10.2% of respondents report that they use modern contraceptives.
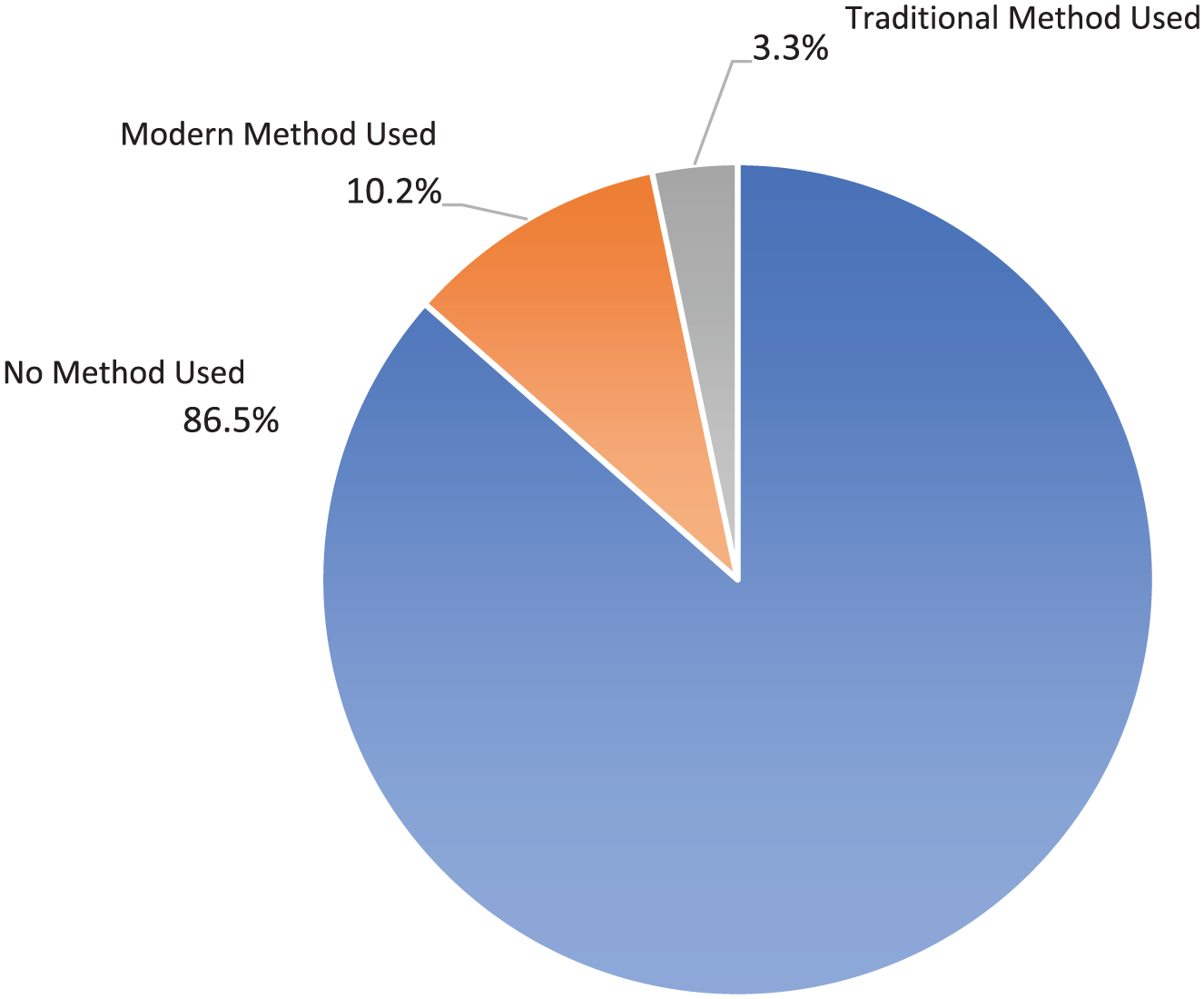
Percentage of women using contraceptives in Nigeria.
Explanatory variables
The two primary explanatory variables in this study are who is the Decision-Maker on Respondent’s Healthcare and the Decision-Maker on Respondent’s Earnings. The Nigeria DHS asks respondents two questions to gather this information: (1) ‘Who makes decisions on your healthcare?’ and (2) ‘Who makes decisions on your earnings?’ For both questions, the responses fall into four categories, with respondent alone coded as 1, joint decision coded as 2, partner or husband coded as 3, and other coded as 4. We treat the ‘other’ category as missing in both variables, because the cell size was extremely small, less than 1% of respondents for the healthcare variable and less than 2% of respondents for the earnings variable. In both cases, collapsing the ‘other’ category with any of the other categories does not make theoretical sense. The resulting Healthcare Decision-Maker and Earnings Decision-Maker variables have three categories. Figure 2 shows that 10.2% of respondents report that they make their own healthcare decisions, 33.8% report that they make joint healthcare decisions with their husbands or partners, and 56.0% of respondents report that their husbands or partners make their healthcare decisions. Adding to this, Figure 2 shows that 69.6% of respondents report that they make their own decisions on earning decisions, 20.9% of respondents report that they make joint decisions regarding their earnings with their partners, and 9.5% of respondents report that their husbands and partners make their earning decisions.
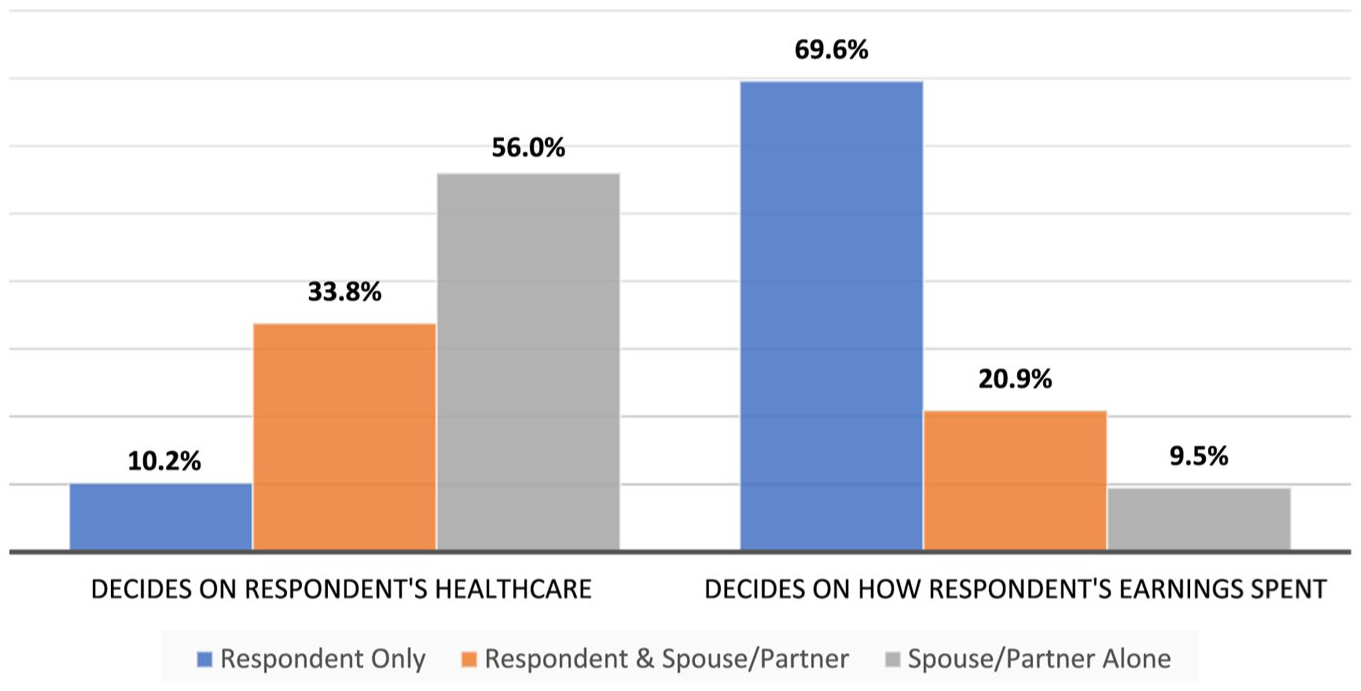
Decision-maker on respondent’s healthcare and earnings.
The control variables in this analysis include age, religious affiliation, rural/urban residence, educational attainment, wealth status, and region of residence. Age is a continuous variable which ranges from 15 to 49 years. The mean age is 29 years with a standard deviation of 9.7 years. Religious affiliation is measured in three discrete categories: Muslim, Christian (non-Catholic Christian denominations), and Catholic. Rural/Urban residence is measured with two categories, urban and rural, with the reference category in this study being rural dwellers.
The Nigeria DHS collects information on the respondent’s educational attainment and wealth status. Educational attainment is measured with four categories. We create three binary indicator variables for those whose educational levels are primary, secondary, and higher than secondary school, and the no formal education category is the reference category. Wealth status is measured as five levels: poorest, poorer, middle, richer, and richest. Poorest is the reference category for this analysis.
Region of residence is a categorical variable which has seven categories: North Central, North West, North East, South–South, South East, and South West. In this analysis, North Central is the reference category, because it represents a more culturally diverse population and includes the country’s capital city of Abuja.
Analytic strategy
In Table 1, we first use binary logistic regressions to test for relationships between who makes decisions on respondent’s healthcare and earnings, and the dichotomous outcome of whether the respondent uses Some Form of Contraceptive (i.e. modern or traditional). The results are presented as odds ratios (OR), or the ratio of odds of using Some Form of Contraception, versus the odds of the reference group, using No Method of Contraception. In Table 2, multinomial logistic regressions are used to model the three-level outcome of No Contraceptive Method, Traditional Contraceptive Method, and Modern Contraceptive Method. The results are presented as relative risk ratios (RRR), also called odds ratios, which indicate the ratio of risk of an event, either using Traditional Contraceptive Method or Modern Contraceptive Method, compared with the risk of the reference (or untreated) group, not using contraception. The relative risk ratio of each event is modeled simultaneously within the same multinomial logistic regression. We compare whether the effects endure across both modeling strategies, testing for differences between women’s decision-making and their use of contraceptive method.
Log odds of some form of contraceptive use for women in Nigeria.
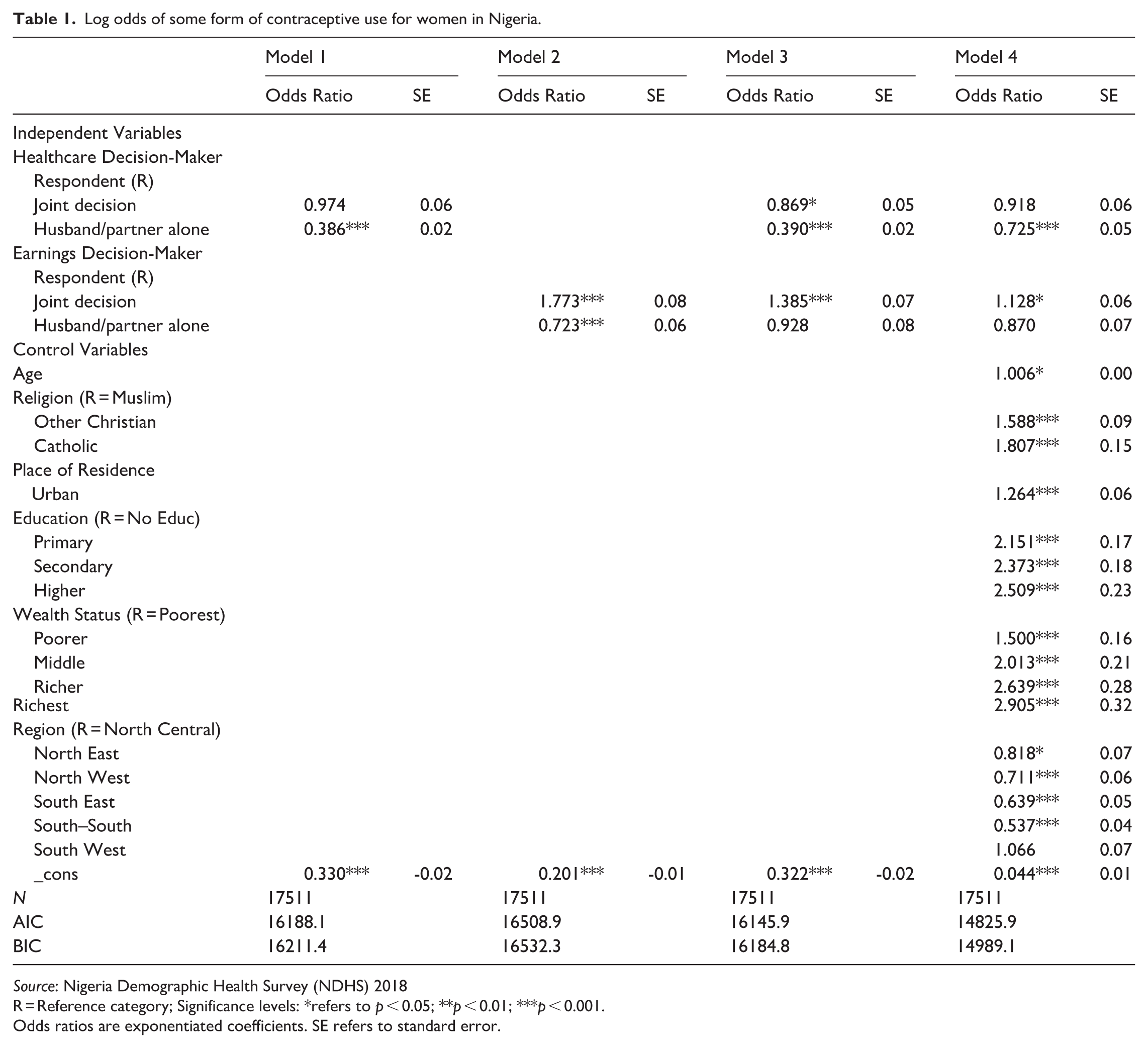
Source: Nigeria Demographic Health Survey (NDHS) 2018
R = Reference category; Significance levels: *refers to p < 0.05; **p < 0.01; ***p < 0.001.
Odds ratios are exponentiated coefficients. SE refers to standard error.
Relative risk of using traditional and modern contraceptives for women in Nigeria.
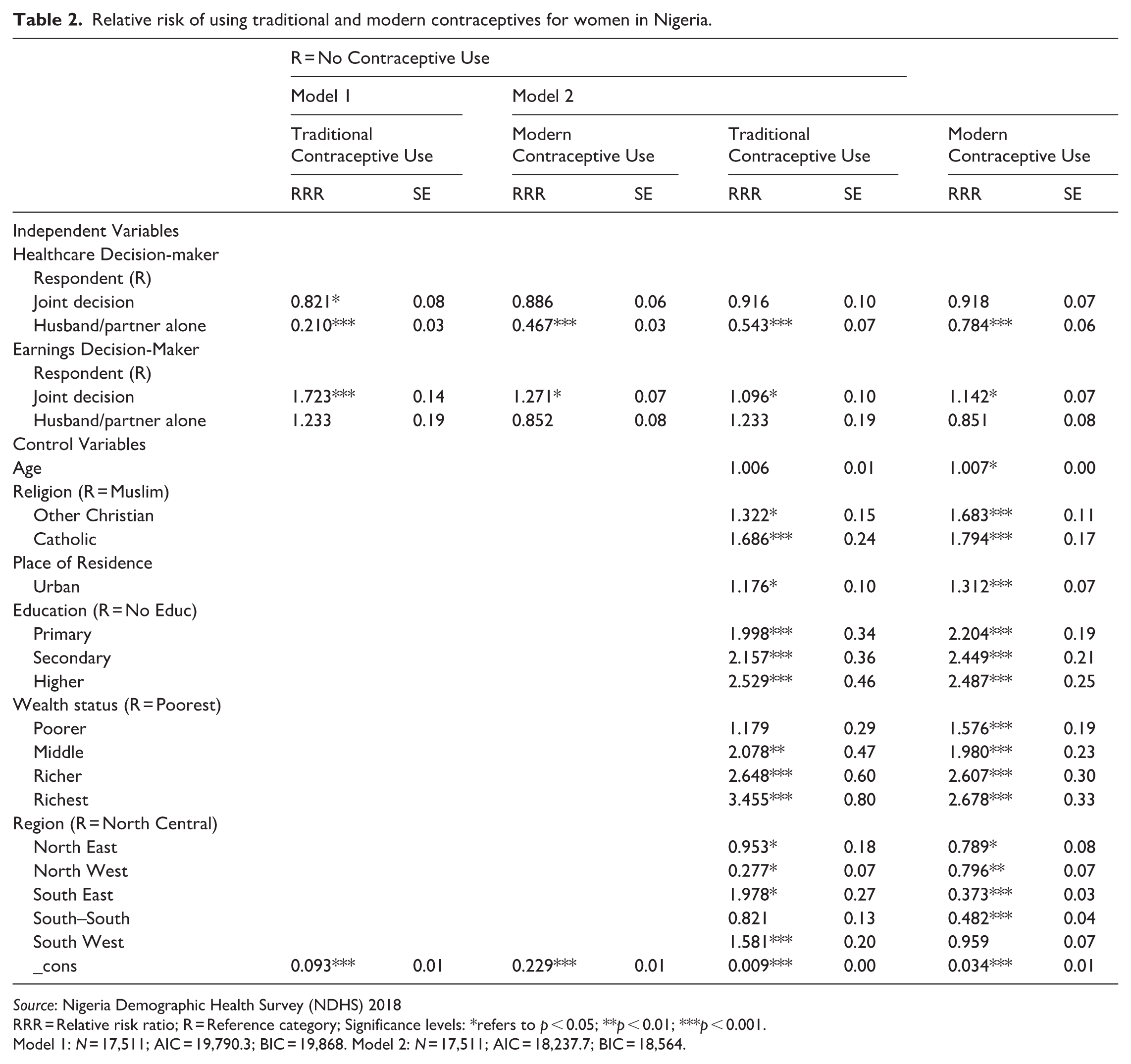
Source: Nigeria Demographic Health Survey (NDHS) 2018
RRR = Relative risk ratio; R = Reference category; Significance levels: *refers to p < 0.05; **p < 0.01; ***p < 0.001.
Model 1: N = 17,511; AIC = 19,790.3; BIC = 19,868. Model 2: N = 17,511; AIC = 18,237.7; BIC = 18,564.
In Table 1, Model 1 tests for bivariate relationships between who is the decision-maker on respondent’s healthcare and whether a woman uses Some Form of Contraception. Model 2 tests for bivariate relationships between who is the decision-maker on respondent’s earnings and contraceptive usage. Model 3 includes both primary explanatory decision-maker variables simultaneously, and Model 4 tests for relationships with the primary explanatory decision-maker variables (i.e. healthcare and earnings) while controlling for demographic and socioeconomic variables that may be related to the explanatory or predictor variables in this analysis. In Table 2, Model 1 tests for relationships across both explanatory decision-maker variables simultaneously, and the respondent’s relative risk of using traditional contraception or modern contraception, and Model 2 tests for these same relationships while controlling for demographic and socioeconomic variables that may be related to the explanatory or predictor variables in this analysis.
Results – predicting some form of contraceptive use
Models 1 and 2 of Table 1 indicate that there are bivariate relationships between who makes decisions and whether women in Nigeria use Some Form of Contraception. Model 1 shows that women whose husbands or partners alone make their healthcare decisions are less likely than women who make their own healthcare decisions to use Some Form of Contraception. Model 2 indicates that women who make their own earnings decisions are more likely to use Some Form of Contraceptive than women whose husbands or partners make their earnings decisions, and that women who make joint earnings decisions are more likely to use Some Form of Contraceptive than women who make their own decisions. Model 3 presents relationships while both explanatory decision-making variables are included.
In Model 4 of Table 1, which controls for background factors, women whose husbands/partners make their healthcare decisions remain less likely (27.5% less so) to use Some Form of Contraception, compared with women who make their own healthcare decisions. Also, women who make joint decisions with their partners about their earnings are more likely than women who make their own earnings decisions to use Some Form of Contraception, either Traditional or Modern, net of other relationships.
Figure 3 presents the predicted probabilities of using Some Form of Contraceptive based upon Model 4, showing on the left side that 20.5% of women who make their own healthcare decisions and 19.3% of women who make joint healthcare decisions use Some Form of Contraceptives, whereas a markedly lower proportion, 16.1%, of women whose husbands/partners make their healthcare decisions use Some Form of Contraception. On the right side of this figure, we see that Some Form of Contraceptive Use is highest (19.7%) for women who make joint decisions with a spouse or partner on how their earnings are spent; followed by those who are the sole decision-makers on how their earnings are spent, and lowest (16.3%) for women whose husbands/partners make the decisions about how women’s earnings are spent.
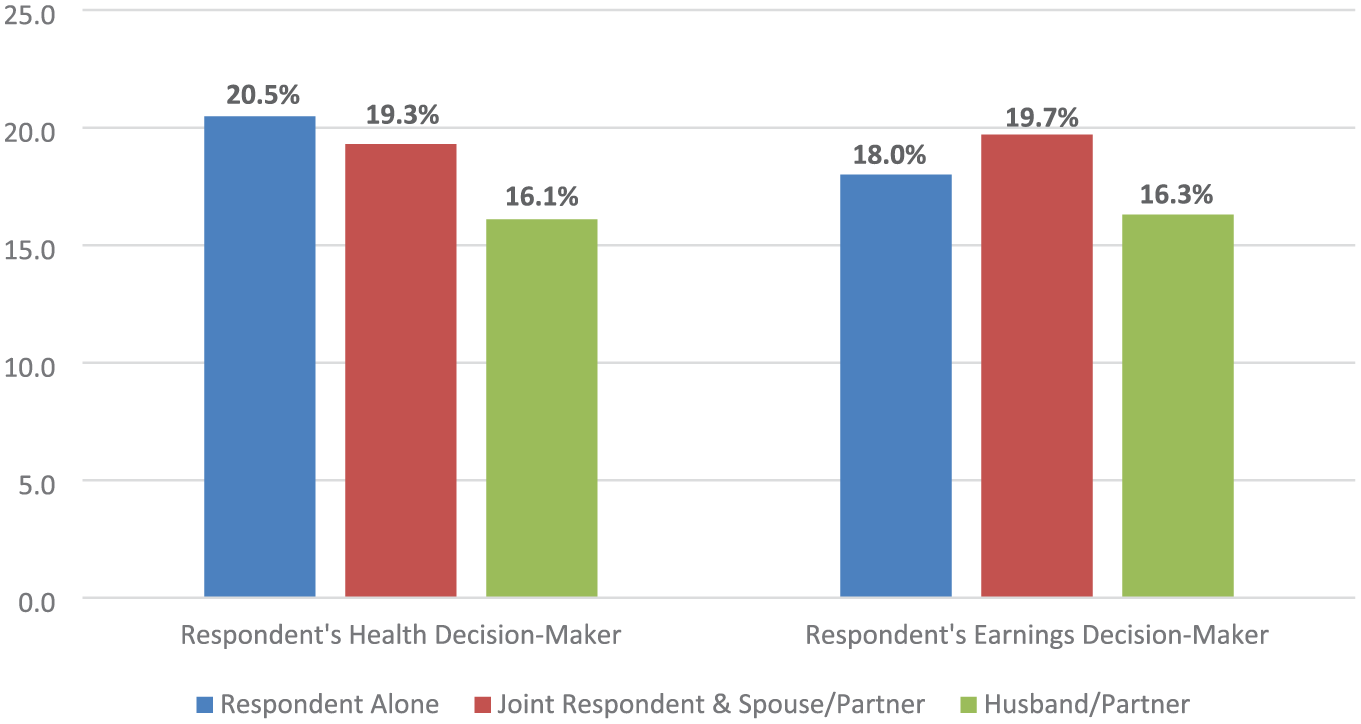
Predicted probabilities of contraceptive use by health and earnings decision-maker.
In terms of baseline relationships, the results in Model 4 of Table 1 show that as age increases, Nigerian women are more likely to use contraceptives. Christian and Catholic women are more likely than Muslim women, and Nigerian women living in urban areas are more likely than women in rural areas to use Some Form of Contraception. At each higher level of educational attainment, Nigerian women are more likely to use contraceptives. The wealth index indicates that women at higher quintiles are more likely to report using contraceptives compared with women in the lowest quintile. Model 4 of Table 1 also highlights the regional disparities in contraceptive use. We find that Nigerian women who live in the North East, North West, South East, and South–South regions are less likely to use contraceptives, compared with the North Central reference category, while controlling for underlying relationships. There is no significant relationship between Nigerian women living in the North Central, where the capital city of Abuja is located, and South West, where the largest city of Lagos is located. It is important to note that these logistic regression results include control variables for factors that have been shown to be related to both decision-making and contraceptive use in prior research. Other research (Abubakar and Abubakar, 2024) has shown using bivariate analysis that contraceptive use is higher in the Southern regions (25.5% in the South West, 18.4% in the South–South, and 15.8% in the South East), followed by the North Central region (14.5%), and then the North East and North West regions (with 8.1% and 6.2%, respectively). The low odds ratios for South East and South-–South in Model 4 of Table 1 reflect that the results are adjusted for religion and education.
Results – predicting modern and traditional contraceptive methods use
Analogous to the full Model 4 results in Table 1, the multinomial logistic results in Table 2 show that women whose husbands/partners make their healthcare decisions have a lower risk (or odds) of using both Traditional and Modern contraceptive methods, compared with women who make their own healthcare decisions. Similarly, women who make joint earnings decisions (with their husbands/partners) evidence a higher likelihood of using both Traditional and Modern contraceptive methods, compared with women who make their own decisions. Model 2 of Table 2 shows that these findings hold, net of other effects. This is a new finding which highlights how women’s uptake of Traditional contraceptive methods and Modern contraceptive methods works in the same way. Respondents with husbands/partners who make the respondent’s healthcare decisions are 45.7% less likely to use Traditional contraceptives and a 21.6% less likely to use Modern contraceptives, net of other effects, compared with women who make their own healthcare decisions.
Interpreting the relative risk (or odds) ratios in Model 2 of Table 2 for the control variables, the results for Modern Contraceptive Use are similar to the log odds results reported for Some Form of Contraceptive Use in Table 1. Age, Catholic, and Other Christian religion, and being urban are all associated with increased odds of Modern Contraceptive Use, compared with their reference group counterparts. Increased education and higher wealth status are also associated with a higher odds of using modern contraception over no method. When examining Traditional contraceptive use in Model 2 of Table 2, Catholic and Other Christian Religion, urban residence, educational attainment, and wealth status all indicate similar patterns of increased odds of Traditional contraceptive use (over no method), compared to their counterparts.
This research reveals that there are regional differences in contraceptive use when considering Modern and Traditional methods. First, the North Central region, containing the capital city of Abuja, demonstrates a higher odds of using Modern Contraception, compared with four of the five other regions. The fifth region, the South West region, which contains the megacity of Lagos, and is not distinguishably different in the odds of using Modern Contraception than the North Central region, which contains the capital city of Abuja. Turning to Traditional Contraceptive Method Use, the North East, North West, and South–South (i.e. South–South at the p < 0.10 level) regions evidence lower odds of Traditional contraceptive use compared with the North Central region (with the capital city of Abuja), and these relations are in the same directions as we found for Modern Contraceptive Use. In contrast to the results for Modern Contraceptive Use, the South East and South West coastal regions have higher odds of using Traditional Contraceptive Methods (over using No Method), compared with the North Central region, all else being equal. These regional differences when considering Modern and Traditional methods and the modeling of Traditional Methods Use separately provide novel findings on women’s contraceptive use in Nigeria.
Discussion of findings
Women’s decision-making power is a salient factor shaping contraceptive use in Nigeria. Women’s autonomy and empowerment make a difference for their reproductive health outcomes and their socioeconomic development, and together, this has implications for child and maternal welfare. We find that women’s health decision-making power influences contraceptive usage. Women whose husbands and partners made their healthcare decisions were found to be less likely to use Some Form of Contraceptives in Table 1 as well as less likely to use either Traditional or Modern Contraceptive Methods in Table 2. Prior scholarship (Do and Kurimoto, 2012) contends that when women lack decision-making power, this thwarts their capability to influence contraceptive usage, because the lack of autonomy affects their confidence to speak boldly and openly with their partners about it. Our findings complement the literature on the positive relationship between decision-making power and contraceptive use already noted for Ghana (Richards and Bass, 2018; Yaya et al., 2018), and further, provide evidence that this positive relationship between decision-making power and contraceptive use holds true for the Nigerian context, too.
We also provide evidence for joint decision-making in the earnings arena, which has a spillover effect on contraceptive use. Across our models, the joint decision on women’s earnings measure evidences a robust positive effect on women’s contraceptive use; we find that the likelihood of using contraceptives when a woman makes joint decisions with her partner on how her earnings are spent is even greater than for women who are the sole decision-makers on their earnings. This is an interesting finding, because historically, women in sub-Saharan Africa generally have exercised substantial control over their own earnings (Boserup, 1970). And while this finding seems curious or even counter to what one would expect in a Western context, we posit that women who share this decision-making on earnings with their husband or partner may be living in more egalitarian relationships to begin with, which allows them to voice their perspectives and to negotiate their fertility preferences with their husbands. Moreover, this points to the positive effect of decision-making power being shared within a more egalitarian relationship, and this is likely to have spillover effects on a woman’s quality of life and health outcomes. It also complements and is consistent with prior scholarship (e.g. Malhotra, 2012) showing that greater gender equality in decision-making in relationships is positively associated with contraceptive use. Our study underscores how increased gender equality within a couple’s relationship has great potential in the Nigerian society.
Next, this analysis considered the use of Modern and Traditional Contraceptive Methods simultaneously as separate outcomes for the first time and found that the same factors shape women’s use of Modern and Traditional Contraceptive Methods in similar ways, yet the relationships for Modern Methods are more robust. The models presented in Table 3 fill a gap in our knowledge and provide novel findings on women’s use of Traditional Contraceptive Methods. Our findings provide specificity to prior research that examined any form of contraceptive (i.e. Yaya et al., 2018 who modeled Modern and Traditional Methods as one outcome) and extend the findings from prior research on Modern Contraceptive Methods (i.e. see Abubakar and Abubakar, 2024; OlaOlorun and Hindin, 2014; Viswan et al., 2017) to those women who desire to control their fertility with Traditional Methods. Indeed, whether using Traditional, Modern, or Some (i.e. any) Form of contraception, these women are similar in their intent to control their fertility. Our modeling of women’s use of traditional contraceptive methods as a separate category effectively broadens our understanding women’s reproductive behavior in Nigeria.
Women who live in rural areas are less likely to use Some Form of Contraception, and specifically, both Traditional and Modern Methods of Contraception, compared with their urban counterparts. This rural–urban schism also patterns and may be related to lower access to family planning and reproductive health care in rural areas, lower incomes and educational levels in rural areas, and fewer life opportunities in rural areas of Nigeria. It is striking that the magnitude of the urban effect is higher for Modern Contraceptive Methods Use than for Traditional Contraceptive Methods Use.
Considering the effect of religion, we find that Muslim women have the lowest propensity to use Some Form, Modern, and Traditional Methods compared with their Christian counterparts, which adds support for the Muslim finding of prior research (Lumor et al., 2023; Obasohan, 2015). However, as Kana et al. (2017) found in the North East region, disentangling the cultural effects of residing in a rural area and being Muslim is complex, because rurality and Muslim religion may overlap culturally through patriarchal social norms that reinforce women’s diminished autonomy and likelihood that they will use contraceptives.
Education is also an important driver of contraceptive use in Nigeria. Our finding that increased educational attainment is positively associated with the likelihood of using contraception validates other research (see Fadeyibi et al., 2022; Yaya et al., 2018) on this positive relationship between education and contraceptive use for Nigeria. Women who are educated are more likely to have autonomy and more likely to use contraceptives (i.e. when we tested Some Form, Modern, and Traditional Methods). Similarly, wealth is related to higher contraceptive use. Moreover, we find that the magnitudes of the education and wealth effects are larger than the effects of the focal variables, healthcare decision-maker and earnings decision-maker, across all models, which suggests possible underlying positive relationships across education and wealth on one hand and both decision-making power and contraceptive use, on the other. While disentangling the directions of these effects is beyond the scope of this analysis, we find that higher socioeconomic status (i.e. measured with educational attainment and higher wealth status) translates into a higher likelihood of using any form of contraception (i.e. Some Form, Traditional, and Modern Methods that we tested).
In addition, we offer new results on regional disparities that operate independently of rural/urban context on women’s propensity to use Some Form of Contraceptive (i.e. considering both Modern and Traditional Methods together) in Nigeria. Those in the North Central region (i.e. where the capital city of Abuja is located) are more likely to use contraceptives compared with all other regions but the South West region (i.e. where Lagos is located), net of other effects. Nigerian women who live in the North East, North West, South East, and South-–South regions are less likely to use contraception in general, all else being equal, compared with women who live in the North Central region, which also has the capital city of Abuja. It is striking that respondents from the urbanized region of the South West, where the megacity of Lagos is located, are not significantly different in their likelihood to use contraceptives than the capital city region, North Central. This highlights the importance of living near an urban area with its more developed reproductive health infrastructure, as a possible explanation. Our finding on the differential use of contraceptives by region of residence is consistent and updates with what earlier studies have found (Babalola and Oyenubi, 2018; Sekoni and Oladoyin, 2016). Another explanation for this regional difference in contraceptive use is educational levels; indeed, we find that women residing in regions most likely to use contraceptives (i.e. North Central and South West regions) also have the highest levels of education in the country.
When considering Modern and Traditional Contraceptive Methods as distinct outcomes, we find that the same factors that are associated with Some Form of Contraceptive Method also shape women’s use of Modern Methods and in similar directions and magnitudes. Next, while most of these relationships hold in similar directions for Traditional Methods, this research reveals novel regional differences in Traditional Contraceptive Use. Specifically, the South East and South West regions are more likely than the North Central region to use Traditional Contraceptive Methods compared with using no method. It is curious that the two coastal regions of South East and South West evidence higher odds of Traditional Contraceptive Use compared with the North Central (i.e. capital city) region. We believe that these results may be explained by considering the composition of these two southern regions as largely Catholic (especially the South East) or Christian, while the North Central region is roughly split between Christian and Muslim. Also, it could be related to educational attainment, as the South East and South West regions have relatively high educational levels, and therefore Catholic women who wish to control their fertility with natural methods encouraged by Catholic leadership in Nigeria. Future research should test for underlying relationships across education, being Catholic, and living in the South East and South West regions as three-way interactions.
Adding to this, the rural regions of North East and North West are less likely than the North Central region to report using Traditional Methods of contraception. This finding agrees with prior research findings for these two regions (Kana et al., 2017; Abubakar and Abubakar, 2024). These results can be explained by considering the largely Muslim composition in these two northern regions, compared with the evenly split religious composition of the North Central region. To disentangle the religion and region effects, we tested for an interaction between region and religion, and we found that although there is a region effect, religion is a more robust predictor of Some Form of Contraceptive Use, net of other effects. As background, there are marked differences in religious affiliation patterned by region of residence, with Islam being the dominant religion in the North West and North East regions, and Muslims and Christians in equal numbers in the North Central (i.e. capital city of Abuja) region, and Christian denominations predominate in the southern regions (South East, South–South, and South West). Breaking it down by region and religion, we found that Muslim women are less likely to use Some Form of Contraceptive (i.e. with a 17.9% predicted probability), compared with Other Christian and Catholic women (23.8% and 23.2% predicted probabilities, respectively). Muslim women who live in the North West and North East regions (with 10.9% and 12.4% predicted probabilities, respectively) are the overall least likely to use Some Form of Contraceptive, and Catholic and Christian women in the North West region having the highest likelihoods of using contraceptives (40.3% and 32.7% predicted probabilities, respectively), while controlling for the baseline variables of interest in this analysis.
Implications and conclusions
Our findings inform contraceptive programming in Nigeria and efforts to address UN Sustainable Development Goal 5 to empower women and achieve gender equality. First, Government of Nigeria policies and other family planning programs need to invest in strategies to improve women’s educational attainment and decision-making power in Nigeria. As discussed earlier, our research clearly highlights how improving women’s educational attainment and decision-making power both share independent relationships with contraceptive use. From this, making these gains in female educational attainment in rural areas could serve as a pivotal event that would improve women’s autonomy and decision-making, which could allow them more say in negotiating and controlling their reproductive decisions. Education also has a positive effect on wealth status, another factor that we find associated with contraceptive use, as women in the lowest wealth quintile are least likely to use contraceptives. Programs should aim to improve educational enrollment levels, and in particular, higher education for women and girls in Nigeria. Women’s status is inextricably linked to increasing educational opportunities, which enhances women’s say in decisions vis-à-vis their partners and is associated with increased contraceptive use.
Another implication of our findings is that religious leaders need to be involved if family planning and reproductive health programs are to be effective. We provide evidence that religion influences contraceptive use, and that it is a more robust predictor than region or rural/urban residence. We find that Muslim women in Nigeria are less likely to use either Some Form of Contraceptives in Table 1 and both Traditional and Modern Methods of Contraception in Table 2. However, there are other predominantly Muslim countries, like Egypt and Indonesia, that have had successful, nationwide contraceptive government programs and interventions (Babalola and Oyenubi, 2018; Roudi-Fahimi, 2004). Because we know that being Muslim is associated with lower contraceptive uptake in Nigeria, family planning programs should work with religious leaders to encourage contraceptive uptake.
One limitation of this study is that it uses only the women’s Nigeria DHS sample for analysis. Findings from other research have shown that men’s attitudes toward contraceptives can also serve as an important driver of contraceptive use. Findings from this research indicate that couple dynamics matter in terms of how decisions are made for contraceptive use, yet there is much to be understood. In a society like Nigeria, understanding the reproductive attitudes and preferences of male partners and their implications for contraceptive use could prove useful and complement our understanding, so future research needs to Nigerian men’s preferences into the analysis.
Moreover, we show that women’s decision-making power translates into a positive influence on contraceptive use (i.e. any method, modern methods, and traditional methods). Next, our findings show that women’s agency and autonomy matter; when women have power, either jointly with their partners or alone, to make decisions about their healthcare and earnings, they are also more likely to exercise control over their reproduction with contraceptive use. This has positive implications for women’s reproductive health and their overall well-being.
Footnotes
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Financial support for this research was provided by the University of Oklahoma Libraries’ Open Access Fund.
