Abstract
Keywords
Introduction
Type 2 diabetes mellitus (T2DM) has become a major global health concern. The global burden of T2DM affected about 529 million in 2021, with projections rising to 1.3 billion by 2050 (Ong et al., 2023). The statistics from India are particularly alarming, with the burden of T2DM expected to surge from 77 million in 2019 to 134 million in 2045. This rapid rise in diabetes prevalence is associated with an increase in potentially life-threatening complications, including neuropathy, nephropathy and retinopathy. Diabetes, along with its complications, is the leading cause of mortality in India, with approximately 1 million deaths occurring annually (International Diabetes Federation, 2019). In addition to mortality, diabetic complications can also be associated with an increased financial burden and reduced quality of life.
Vitamin D is a fat-soluble secosteroid, predominantly produced in the skin upon exposure to ultraviolet B radiation from sunlight. While its role in calcium homeostasis and skeletal health has been established for decades (Cutolo et al., 2023), recent studies show a growing interest in its extra-skeletal effects. Emerging evidence suggests that vitamin D may play a role in immunomodulation; its deficiency has been implicated in the development and progression of various chronic disorders such as diabetes mellitus, asthma, thyroid disorders and rheumatoid arthritis (Sassi et al., 2018).
Several studies have demonstrated a higher prevalence of vitamin D deficiency among patients with altered glucose homeostasis and insulin resistance (Alharazy et al., 2021; Cӑtoi et al., 2021; Huu et al., 2021; Zhang et al., 2022). Although the exact mechanisms are not fully understood, the presence of vitamin D receptors in the pancreas is suggestive of their role in insulin secretion. They also postulated that vitamin D may indirectly influence insulin secretion by regulating calcium homeostasis. Additionally, vitamin D is hypothesised to enhance insulin sensitivity mechanisms such as increasing insulin receptors in peripheral tissues, improving phosphoinositide 3-kinase (PI3K)-dependent insulin signalling, and activating peroxisome proliferator-activated receptor delta (Ashraf and Alvarez, 2010; Mohd Ghozali et al., 2022).
Serum vitamin D levels could be a potential determinant of the presence of diabetic complications. Studies have revealed a strong correlation between vitamin D deficiency and an increased prevalence of cardiovascular complications in patients with diabetic (de la Guía-Galipienso et al., 2021). This could be attributed to the potential influence of vitamin D on endothelial dysfunction and atherosclerosis risk (Kim et al., 2020; Rodríguez et al., 2016). Experimental evidence from animal studies indicates that vitamin D deficiency might exacerbate the risk of oxidative stress, inflammation and ferroptosis, crucial factors in the pathogenesis of retinopathy and nephropathy (Kuhlmann et al., 2004; Tohari et al., 2020; Zhan et al., 2023). Additionally, some studies reported that vitamin D supplements may alleviate neuropathy (Chen et al., 2023). However, clinical evidence remained inconsistent and sometimes contradictory, highlighting the need for further research to draw definitive conclusions.
Considering the widespread health implications, vitamin D deficiency is a serious public health concern, even in countries with ample sun exposure, like India. It is estimated that vitamin D deficiency affects 47.9% of the global population (Cui et al., 2023). While national data are limited, studies indicate that vitamin D deficiency affects between 75% and 100% of the population in the Indian subcontinent (Ritu and Gupta, 2014). Contributing factors may include inadequate exposure to direct sunlight, dietary issues, skin pigmentation, and variation in body fat percentage. The higher prevalence of vitamin D deficiency, combined with its pathological implications, could be attributed to the rising prevalence of diabetic complications in India.
Numerous studies have investigated the association of vitamin D with various complications of T2DM. However, findings remain inconsistent due to heterogeneity of sample size, study design, population characteristics, adjustments for risk factors and variation in the vitamin D cut-off points (Alam et al., 2016; Jee et al., 2014; Usluogullari et al., 2015; Xiao et al., 2020; Zhao et al., 2021). Moreover, there is a paucity of research on this topic in our region, with only a handful of studies conducted in this regard (Adela et al., 2016; Ashinne et al., 2018; Bajaj et al., 2014). To address these gaps, we performed a retrospective study to determine the association between vitamin D deficiency and diabetic complications in T2DM. Our findings aim to provide more nuanced insights into the complex relationship between vitamin D and the aetiology of diabetic complications, offering insights that could potentially inform clinical guidelines and public health strategies.
Methods
Study design and setting
We conducted an unmatched case-control study retrospectively, from August 2023 to August 2024, at the Department of Medicine at a tertiary care hospital in south India. The present study was initiated after obtaining ethical clearance. Considering that the study was retrospective, informed consent was waived.
Study participants
All patients with T2DM, according to the International Classification of Diseases, Tenth Revision (ICD-10 – coded E11), aged >18 years, who were admitted to the Department of General Medicine between January 2017 and December 2022, and whose vitamin D levels were recorded during the period of hospital stay, were included. Pregnant and lactating women, patients with type 1 or any other type of diabetes, patients with any type of malignancies or HIV infections, and patients who were already on vitamin D supplements or immunosuppressant were excluded. Patients with T2DM with complications were enrolled as cases. The control group included patients with T2DM without any complications. The sample size analysis was conducted using findings from a pilot study and was performed with the Epi Info programme developed by the Centers for Disease Control and Prevention, which is available at: https://www.cdc.gov/epiinfo/index.html. We used an alpha of 0.05, a power of 95%, a prevalence of vitamin D deficiency among controls of 57.14, and the expected odds ratio (OR) between cases and controls as 2. The minimum sample size was calculated to be 706–353 cases and 353 controls.
Data collection
A predesigned data collection form was used to extract data from medical records. Data, including demographic information such as, age, gender, place of residence, and type of occupation, was collected. The place of residence was then classified into four geographical regions: coasts, plains, plateaus, and ghats (ENVIS Centre, 2021). Their occupations were classified as indoor jobs, outdoor jobs, and unemployed or retired. The medical and medication history of the patients was collected, which included the duration of diabetes and the presence of comorbidities. Additionally, we collected information on laboratory parameters, including fasting blood glucose (FBS), random blood glucose (RBS), glycated haemoglobin (HbA1c), Red blood cells (RBC) indices, liver function tests such as alanine aminotransferase (ALT), aspartate aminotransferase, alkaline phosphatase and total bilirubin. Renal function tests such as serum creatinine, serum urea, sodium, potassium, serum albumin, total protein, and urine protein levels were also noted.
Determination of glycaemic control
HbA1c levels were estimated using high-performance liquid chromatography (HPLC). An HbA1c level of >7.0% was considered as uncontrolled diabetes, in accordance with the recommendations of the Research Society for the Study of Diabetes in India (RSSDI) – Endocrine Society of India (ESI) guidelines. These guidelines recommend <7.0% HbA1c as the target for minimising the risk of developing complications (Chawla et al., 2020).
Assessment and classification of serum vitamin D levels
Serum vitamin D levels of each patient were assessed during their hospital stay using the electrochemiluminescence immunoassay (ECLIA) method. Based on their vitamin D levels, patients were categorised as vitamin D deficient (<20 ng/mL), insufficient (20–30 ng/mL) and sufficient (>30 ng/mL) (Holick, 2009).
Assessment of diabetic complications
Clinical history and detailed physical examination were used to clinically diagnose diabetic neuropathy (ICD-10 E11.40–49). The diagnosis of diabetic retinopathy (ICD-10 E11.31–39) was confirmed based on fundus examination findings. According to the Kidney Disease Improving Global Outcome (KDIGO) (2022) clinical practice guidelines for the management of chronic kidney disease in diabetes, diabetic nephropathy (ICD-10 E11.21–29) is defined as an estimated glomerular filtration rate (eGFR) < 60 mL/min per 1.73 m2 and/or an albumin-creatinine ratio (ACR) > 300 mg/g (KDIGO, 2022). eGFR is calculated based on the Chronic Kidney Disease Epidemiology Collaboration (CKD-EPI) equation (Levey and Stevens, 2010).
Cerebrovascular (CVA) complications (ICD10-E11.51–59) of diabetes were diagnosed based on clinical evaluation and imaging studies. Ischaemic heart disease (IHD) (ICD10-E11.51–59) in diabetes was defined based on clinical evaluation and electrocardiogram. Diabetic foot disease (DFD) (ICD10-E11.621) was diagnosed based on clinical history and physical examination.
Statistical analysis
Since the Shapiro–Wilk test showed non-normal distribution, continuous variables were expressed as median [25th–75th quartile], and categorical variables were reported as numbers (percentage). The variables with missing data of more than 20% were omitted. Mann–Whitney test was employed to assess the difference in continuous variables, while the Chi-squared test was applied to evaluate differences in the distribution of categorical variables between groups and ascertain p-values. The relationship between serum vitamin D levels and various variables was analysed using Spearman rank correlation for continuous variables, the Mann–Whitney U test for categorical variables with two groups and the Kruskal–Wallis test for categorical variables with more than two groups.
Univariate analysis was performed using a generalised linear model with the presence of each diabetic complication as the dependent variable and other variables as independent variables. The significance was set as p < 0.2. To determine multicollinearity, the variance inflation factor (VIF) was calculated, and variables demonstrating a VIF higher than 5 were excluded to avoid overfitting.
Multivariate analysis was then performed with predicted variables and other desired variables. The association of vitamin D status with each diabetic complication was expressed as an adjusted odds ratio (AOR) with 95% confidence interval (CI). Vitamin D status was adjusted for factors such as age, gender, duration of diabetes and the presence of comorbidities such as hypertension and cardiovascular disease for each of the diabetic complications. For neuropathy, additional adjustments included residence, occupation, chronic kidney disease (CKD), osteoarthritis, HbA1c, glycaemic control, white blood cell (WBC) count, ALT, total bilirubin, serum urea and total protein. In retinopathy, further adjustments were made for residence, systolic blood pressure (SBP), diastolic blood pressure (DBP), CKD, HbA1c, mean cell haemoglobin, ALT, total bilirubin, serum creatinine, serum potassium and total protein. For nephropathy, the analysis additionally adjusted for season of assessment, residence, occupation, SBP, DBP, osteoarthritis, WBC, mean cell haemoglobin concentration (MCHC), serum creatinine, serum potassium and total protein.
In CVA, additionally adjusted factors for vitamin D status included season of assessment, SBP, DBP, dyslipidaemia, hypothyroidism, osteoarthritis, RBC, WBC, ALT, and serum sodium. For IHD, the vitamin D status was additionally adjusted for residence, occupation, SBP, DBP, dyslipidaemia, WBC, MCHC, serum creatinine, serum sodium, serum potassium and total protein. For DFD, further adjustments included HbA1c, glycaemic control, RBC, WBC, total bilirubin, serum creatinine, serum sodium and serum potassium.
All statistical analyses were performed using R software version 4.4.1. R Foundation for Statistical Computing, Vienna, Austria: https://www.R-project.org/.
Results
The data of 873 cases and 566 controls were analysed. The median age was 64 (55–71) years for cases and 59 (52–68) years for controls (p < 0.001). Regarding the geographical region of the residence, most participants resided in the coastal regions (46.51% vs. 43.11%, p = 0.273). Additionally, most of the patients were either unemployed or retired (58.19% vs. 56%, p = 0.193). Hypertension was the most prevalent complication in both the case and control groups (70.22% vs. 54.59%, p < 0.001), followed by hypothyroidism (12.71% vs. 11.66%, p = 0.552). Median HbA1c and RBS levels were higher in the case group [8.2% (6.8–10.4) vs. 7.8% (6.8–9.6), p = 0.012, and 202 mg/dL (140–280.25) vs. 191 mg/dL (136–272), p = 0.035, respectively] (Table 1).
Baseline characteristics.
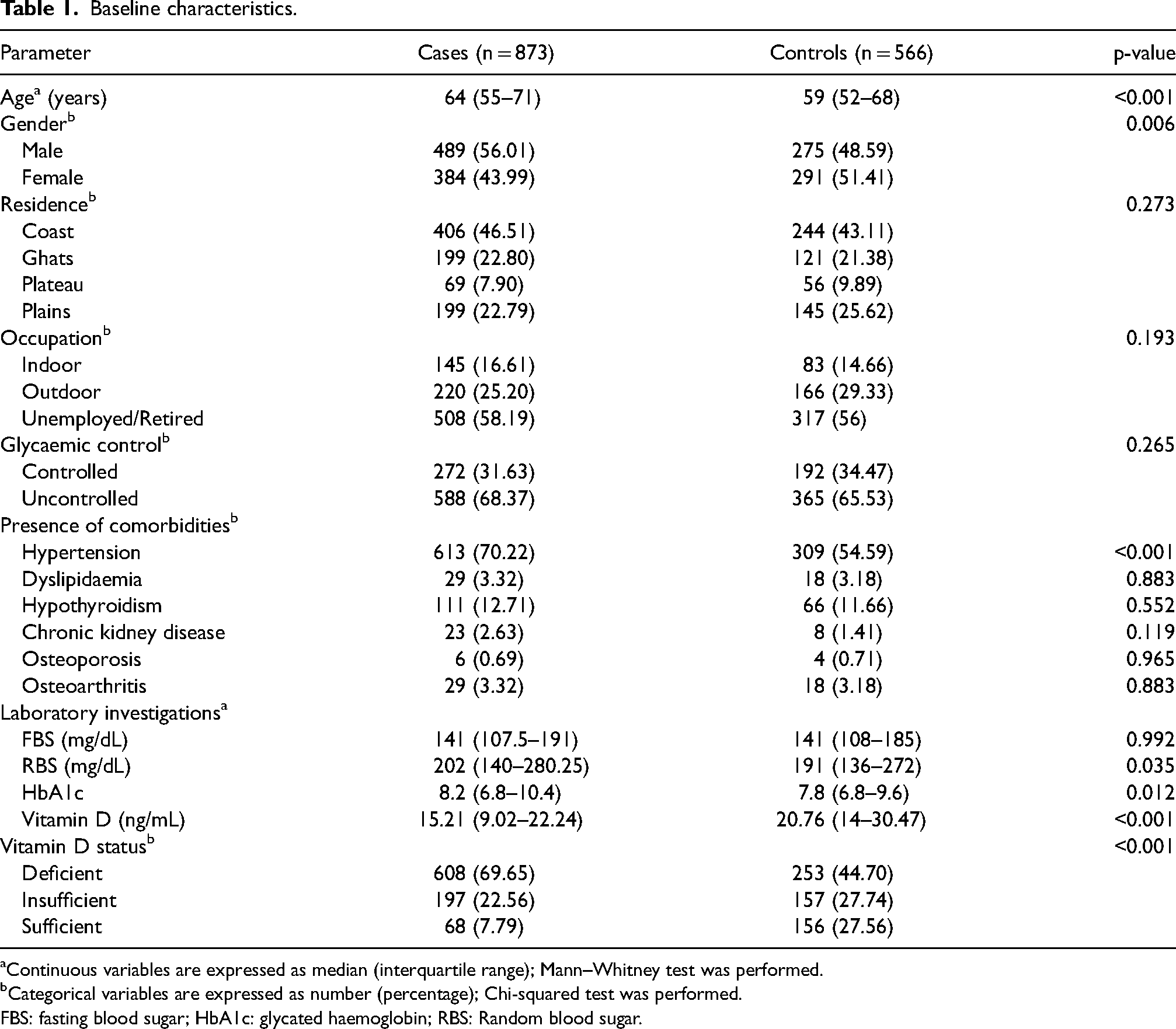
Continuous variables are expressed as median (interquartile range); Mann–Whitney test was performed.
Categorical variables are expressed as number (percentage); Chi-squared test was performed.
FBS: fasting blood sugar; HbA1c: glycated haemoglobin; RBS: Random blood sugar.
Effect of age, gender, residence, occupation and season on vitamin D levels
A weak positive correlation was observed between age and vitamin D levels (rho-0.11, p < 0.001). Males exhibited slightly higher vitamin D levels compared to females (p = 0.005). However, no significant difference in serum vitamin D levels was found across different seasons (p = 0.728). The analysis of vitamin D levels by place of residence revealed significantly lower levels in individuals living in ghats compared to those in coastal regions (p < 0.001). Furthermore, people with outdoor jobs had significantly higher vitamin D levels than those with indoor jobs (p = 0.006) and those who were unemployed or retired participants (p = 0.001).
Diabetic complications
Diabetic complications were present in 873 participants (60.67% of the study population), while 566 (39.33%) had no complications. Among those with complications, nephropathy was the most common (24.39%), followed by IHD (23.0%), neuropathy (21.95%), retinopathy (19.11%), DFD (11.81%) and CVA (11.61%). The vitamin D status across different combinations of complications is provided in Supplemental file S1.
Vitamin D levels
The median serum vitamin D concentration was significantly lower in cases as compared to controls [15.21 (9.02–22.24) vs. 20.76 (14–30.47), p < 0.001] (Figure 1). Vitamin D deficiency was observed in 69.65% of cases and 44.70% of controls, p < 0.001. Similarly, vitamin D insufficiency was more common among cases (22.56% vs. 27.74%, p = 0.026). In contrast, a higher proportion of controls had sufficient vitamin D levels compared to cases (27.56% vs. 7.79%, p < 0.001) (Table 2).
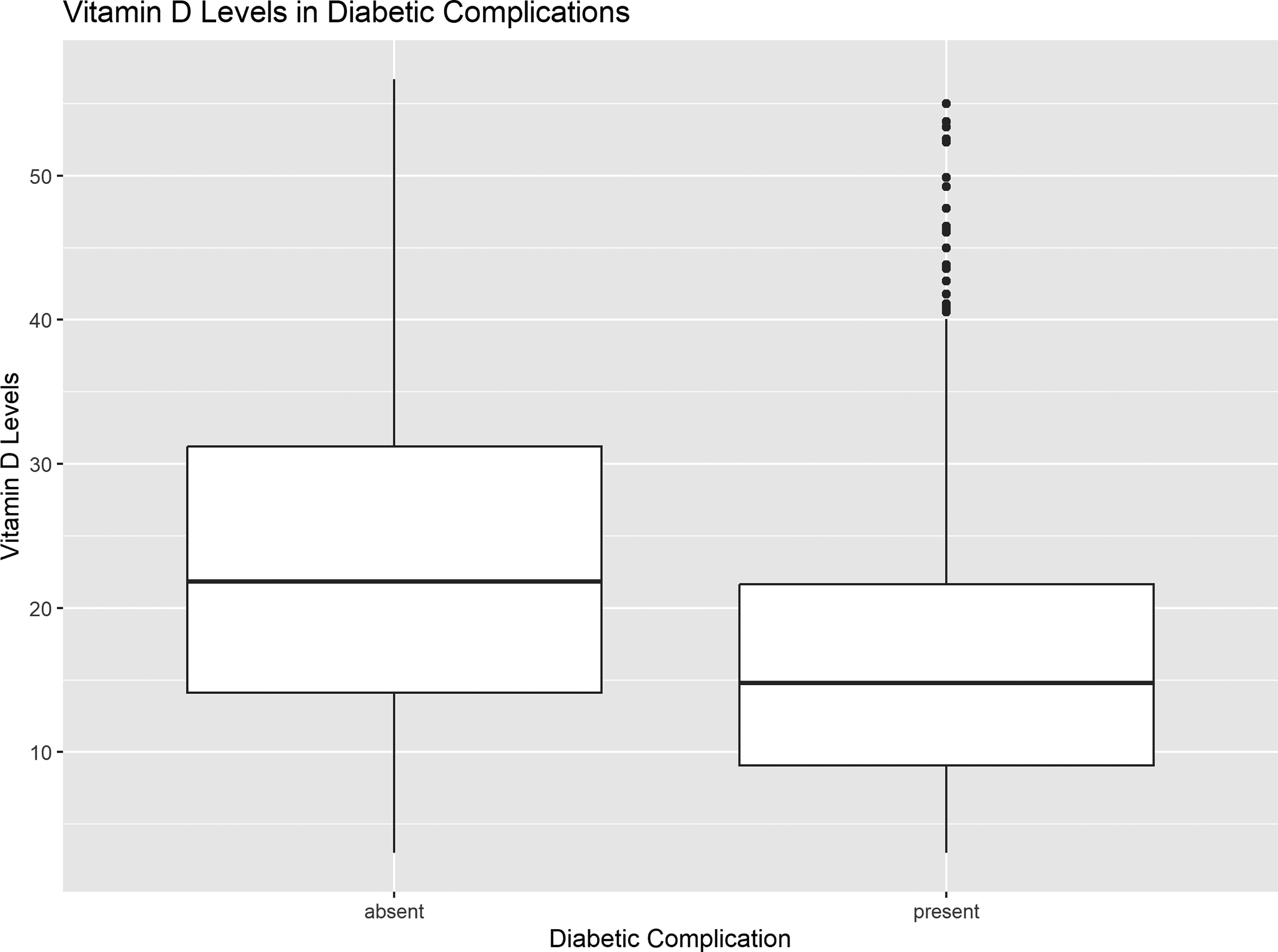
Serum vitamin D levels in cases and controls.
Vitamin D status among cases and controls.
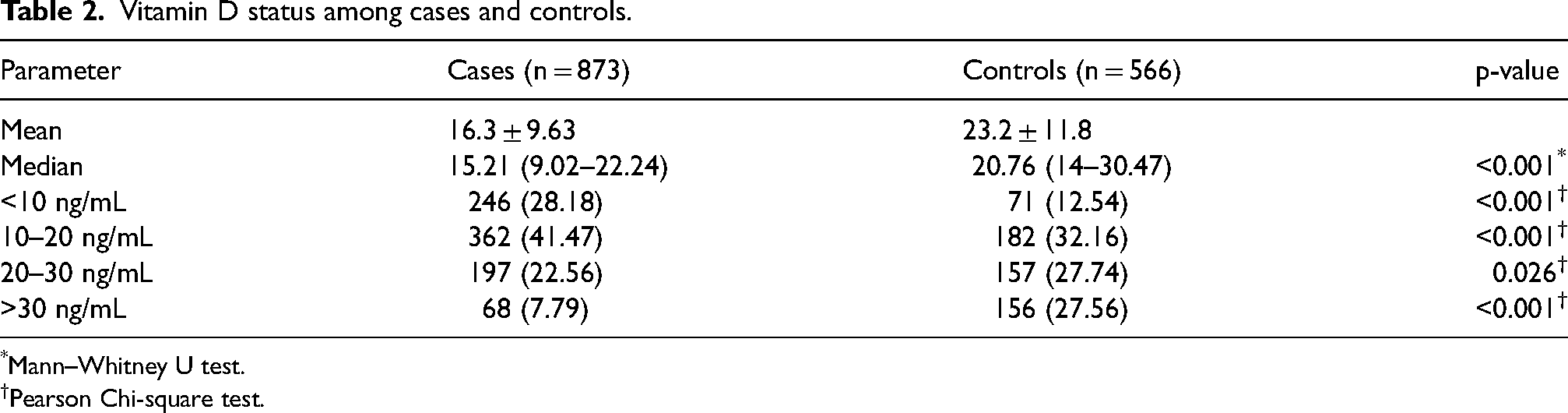
*Mann–Whitney U test.
†Pearson Chi-square test.
Association of vitamin D status with diabetic complications
Univariate and multivariate logistic regression were performed with each diabetic complication as the dependent variables, and vitamin D status and other relevant clinical variables as the independent variables. Variables that showed a significant association in the univariate analysis and had a VIF <5 were considered for multivariate analysis. After adjusting for other relevant variables, vitamin D deficiency was a significant independent predictor for neuropathy [AOR 4.09 (2.34, 7.63), p < 0.001], nephropathy [AOR 5.23 (2.72, 10.85), p < 0.001], retinopathy [(AOR 2.52 (1.44, 4.69), p < 0.001], IHD [AOR 2.19 (1.33, 3.76), p = 0.003)] and DFD [AOR 2.66 (1.34, 5.91), p = 0.030] (Table 3). The detailed univariate and multivariate analysis is provided in Supplemental file S2.
OR for vitamin D status in diabetic complications.
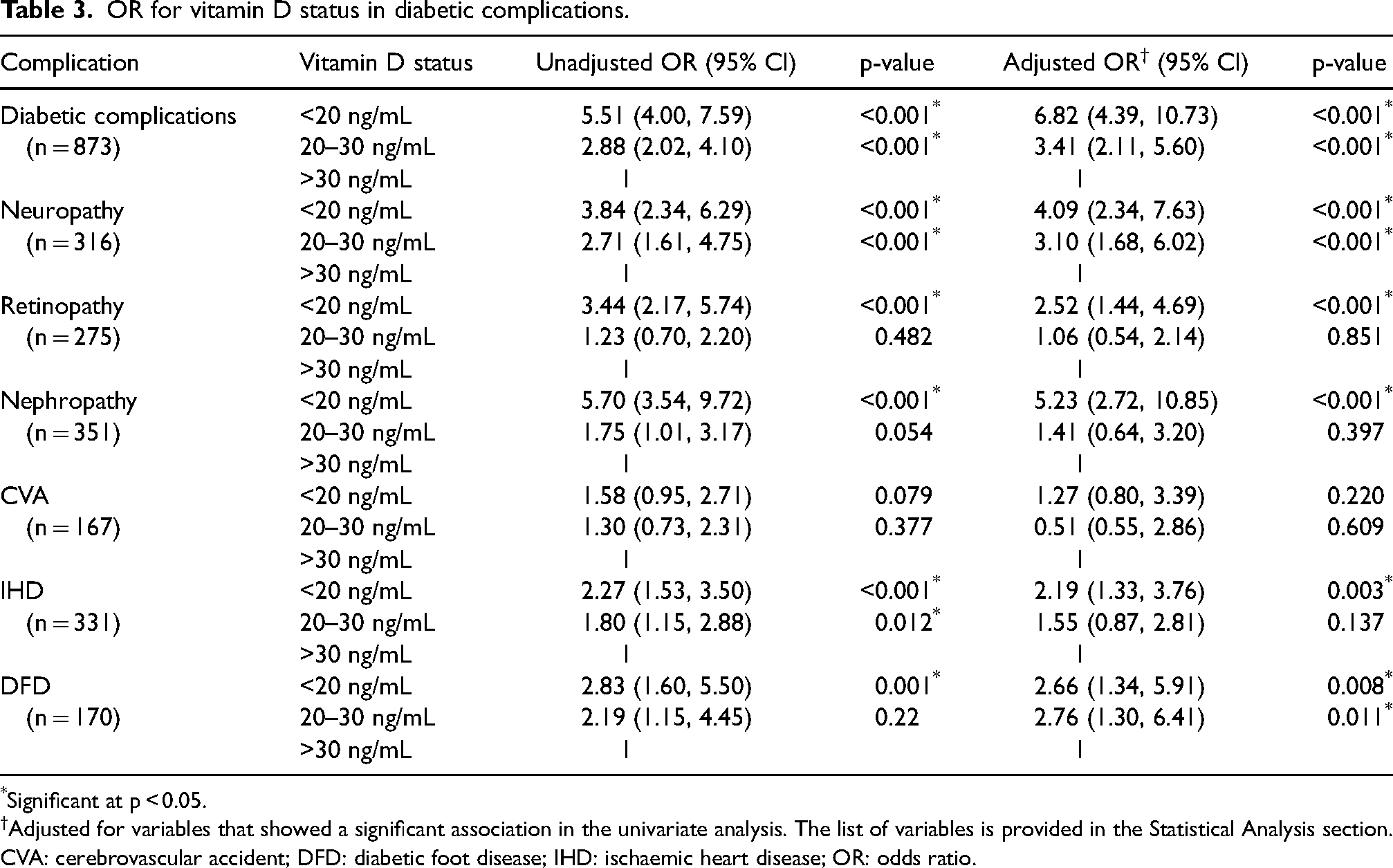
*Significant at p < 0.05.
†Adjusted for variables that showed a significant association in the univariate analysis. The list of variables is provided in the Statistical Analysis section.
CVA: cerebrovascular accident; DFD: diabetic foot disease; IHD: ischaemic heart disease; OR: odds ratio.
Discussion
Vitamin D deficiency could be considered a plausible modifiable risk factor for diabetic complications, yet its role remains poorly defined. This investigation sought to assess serum vitamin D levels in patients with diabetic complications and compare them to those without complications to ascertain whether vitamin D deficiency could be a potential risk factor for these complications. Our findings indicate a significant association between vitamin D deficiency and the presence of diabetic complications, with deficient individuals showing a 6.8-fold higher risk compared to those with insufficient or sufficient vitamin D levels. Notably, vitamin D deficiency was strongly associated with neuropathy, retinopathy, nephropathy, IHD and DFD, but not with CVA. Our findings are consistent with the previous studies (Bajaj et al., 2014; Castillo-Otí et al., 2022; Kurian et al., 2024; Zahedi et al., 2024; Zhuang et al., 2024), which showed a significant association of vitamin D levels with microvascular complications of diabetes. However, they contrast with studies by Girard et al. (2021) and Usluogullari et al. (2015), which found significant associations only with nephropathy. Similarly, Priyanto et al. (2023) could not find an association between vitamin D levels and DFD.
Current guidelines do not clearly establish the role of vitamin D in diabetic complications or define the exact levels associated with their development in T2DM (Amrein et al., 2020; Bleizgys, 2021; Demay et al., 2024). The findings from this study indicate that not just vitamin D deficiency (<20 ng/mL), but also vitamin D insufficiency (20–30 ng/mL) could be a potential risk factor for developing complications like neuropathy. This suggests that the threshold for optimal vitamin D levels in preventing complications may need re-evaluation.
The biological plausibility of our findings is supported by the multifaceted role of vitamin D in glucose metabolism, inflammation and vascular health. Vitamin D receptors are widely expressed throughout the body in pancreatic beta cells, immune cells and vascular endothelium, suggesting the potential mechanisms through which deficiency could exacerbate diabetic complications (Bikle, 2014; Hossein-Nezhad and Holick, 2013). The effect of vitamin D receptors on immune cells and vascular endothelium, along with its anti-inflammatory and anti-angiogenic properties, could explain its association with complications like neuropathy, nephropathy and IHD (Contreras-Bolívar et al., 2021; Usluogullari et al., 2015). However, the lack of association with CVA remains puzzling and may reflect differences in the pathophysiology of macrovascular complications or the influence of unmeasured confounders.
One possible explanation for the lack of association between vitamin D levels and CVA is that our study did not differentiate between ischaemic and haemorrhagic stroke. Evidence suggests that vitamin D deficiency is strongly associated with ischaemic stroke, likely due to its role in endothelial dysfunction and inflammation (Cui et al., 2024). In contrast, haemorrhagic stroke, which often occurs due to factors like hypertension and vascular malformations, may not show the same association with vitamin D levels (Kuriakose and Xiao, 2020). Since our study grouped all CVA cases together, the inclusion of haemorrhagic stroke may have diluted the observed association. Further studies should stratify CVA by subtype to examine the relationship between vitamin D deficiency and CVA in diabetics.
Vitamin D is a steroid hormone primarily synthesised in the skin through exposure to sunlight, making adequate sun exposure a crucial factor in preventing vitamin D deficiency (Bleizgys, 2021; Holick et al., 2011). Our study tried to assess the impact of various factors that could potentially influence sunlight exposure in the target population. Participants from coastal areas and those with outdoor occupations had significantly higher vitamin D levels, underscoring the importance of sun exposure in maintaining adequate levels. The guidelines also suggest that vitamin D levels could alter based on the variation in sun exposure (Bleizgys, 2021; Pludowski et al., 2018). However, we observed no significant seasonal variation in vitamin D levels. This could be due to the low interannual variability in various regions of India, especially in South India, reducing the effects of seasonal variations in sunlight exposure (Dubey et al., 2021). Males had significantly higher vitamin D levels as compared to females. Similar results were observed in a systematic review of the factors affecting vitamin D levels in the South Asian population (Siddiqee et al., 2021). This difference may be due to cultural factors, as females tend to stay indoors more as compared to their male counterparts, and the clothing style among Indian women restricts sunlight absorption as compared to men. Therefore, further studies are needed in which additional covariates affecting vitamin D are adjusted for to further reduce the risk of bias.
This case-control study is one of the few from this region to identify a potential association between vitamin D and diabetic complications. A major strength of this study lies in its large sample size of real-world data. Moreover, we accounted for residual confounding factors for vitamin D deficiency, such as age, place of residence, gender, assessment season and occupation type.
Despite these strengths, our findings must be interpreted with caution due to certain limitations. A major limitation of the study was its retrospective nature, which restricted us from collecting data on additional variables that might have influenced vitamin D levels, such as dietary intake, bone mineral density, alcohol consumption, smoking status, degree of physical activity and socioeconomic status of the sample. Whilst we did not match age and sex for the cases and controls, we adjusted these factors in our regression models. Furthermore, although our study identified a significant association between vitamin D and diabetic complications, it does not establish causality. Additionally, we were unable to assess the effect of vitamin D levels on the progression of these complications.
The clinical implications of our findings are significant. Routine screening of vitamin D levels in the diabetic population may be clinically warranted, given the strength of observed associations with diabetic complications. Maintaining vitamin D levels above 30 ng/mL could potentially reduce the risk of complications, although this hypothesis requires further validation. Prospective cohort studies would help better understand how vitamin D deficiency influences the progression of diabetic complications. Additionally, a large, randomised controlled trial (RCT) would be particularly valuable in assessing the clinical benefits of vitamin D supplementation for the prevention and management of diabetic complications, considering the plausible mechanisms and limited supporting evidence available from previous trials.
Conclusion
This study demonstrated a significant association between vitamin D deficiency and increased risk of diabetic complications. Our findings indicate that patients with T2DM and lower vitamin D levels are at a higher risk of developing complications such as neuropathy, retinopathy, nephropathy, IHD and DFD. However, no such association was observed between vitamin D and CVA. The study emphasises the need for further research to establish the causality and define the optimal vitamin D threshold for further prevention and management. Prospective cohort studies and RCTs are essential to translate these findings into clinical practice and improve outcomes for patients with diabetes and its complications.
Supplemental Material
sj-docx-1-nah-10.1177_02601060251359708 - Supplemental material for Vitamin D status and its association with diabetic complications in type 2 diabetes mellitus: A case-control study
Supplemental material, sj-docx-1-nah-10.1177_02601060251359708 for Vitamin D status and its association with diabetic complications in type 2 diabetes mellitus: A case-control study by Ashna Chackochan, Swetha R Reghunath, Vasudeva Guddattu, Girish Thunga, Shivashankara Kaniyoor Nagri, Revathi P Shenoy, Vishnu Prasad Shenoy and Leelavathi D Acharya in Nutrition and Health
Supplemental Material
sj-docx-2-nah-10.1177_02601060251359708 - Supplemental material for Vitamin D status and its association with diabetic complications in type 2 diabetes mellitus: A case-control study
Supplemental material, sj-docx-2-nah-10.1177_02601060251359708 for Vitamin D status and its association with diabetic complications in type 2 diabetes mellitus: A case-control study by Ashna Chackochan, Swetha R Reghunath, Vasudeva Guddattu, Girish Thunga, Shivashankara Kaniyoor Nagri, Revathi P Shenoy, Vishnu Prasad Shenoy and Leelavathi D Acharya in Nutrition and Health
Footnotes
Acknowledgements
The authors would like to acknowledge Manipal Academy of Higher Education, Manipal College of Pharmaceutical Sciences, Department of Pharmacy Practice, Manipal, India, and the Medical Superintendent, Kasturba Hospital, Manipal, India, for providing all the support and facilities for the best possible completion of this work.
Authors’ contribution
AC was involved in conceptualisation, data curation, formal analysis, investigation, project administration, visualisation and writing – original draft; SRR in writing – review & editing; VG in formal analysis, validation and writing – review & editing; GT in conceptualisation, supervision and writing – review & editing; SKN in supervision and writing – review & editing; RPS and VPS in writing – review & editing; and LDA in conceptualisation, funding acquisition, supervision and writing – review & editing. All authors have read and approved the manuscript.
Availability of data and materials
Data described in the manuscript will be made available upon request.
Consent to participate
Informed consent was waived off due to the retrospective nature of the study.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical statement
This study was conducted in accordance with the guidelines of the Declaration of Helsinki, and the research protocol was reviewed and approved by the Institutional Ethics Committee of Kasturba Medical College and Kasturba Hospital, Manipal, India (IEC1: 4-2023).
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by the Manipal Academy of Higher Education Intra mural Fund.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
