Abstract
Spontaneous primary pleural mesotheliomas in Fischer 344 (F344) or other rat strains have rarely been reported. The objectives of this retrospective study were to develop historical incidence data and better characterize the light-microscopic morphology of these naturally occurring neoplasms in a large cohort of rats of several strains. A retrospective review was performed of National Toxicology Program (NTP) studies in rats conducted between 1980 and 2019 and comprising a total of 104,029 rats (51,326 males, 52,703 females), predominantly (90%) of the F344 strain. Of the 94,062 F344 rats surveyed, there were 30 cases of primary pleural mesotheliomas (22 males, 8 females). Of the 2998 Wistar Han rats surveyed, primary pleural mesotheliomas were present in 2 male rats. No primary pleural mesotheliomas were noted in male and female rats of other strains (6669 Sprague Dawley; 300 Osborne-Mendel). All primary pleural mesotheliomas in control and treated F344 and Wistar Han rats were considered spontaneous and unrelated to treatment. Based on light-microscopic evaluation of paraffin-embedded hematoxylin and eosin stained sections, only epithelioid and biphasic histologic subtypes were observed: 18 and 12 in F344 rats, respectively, and one each in Wistar Han rats. No sarcomatoid subtype cases were noted in any strain of rat.
Introduction
Mesotheliomas are neoplasms arising from the lining epithelium (mesothelium) of the body cavities (pleural, peritoneal, and pericardial). 1 In humans, malignant mesothelioma is a rare but devastating cancer for which the prognosis remains extremely poor. 1,2 The great majority of human mesotheliomas (up to 90%) are pleural (developing in the thoracic cavity) and the etiologic association between pleural mesothelioma and exposure to asbestos and asbestos-like fibers in people is supported by decades of research, with approximately 80% or more human pleural mesotheliomas attributed to such exposures. 1,3 –7 The predominance of pleural mesothelioma in men compared to women is at least partly attributable to men’s typically greater occupational exposure to asbestos/asbestos fibers. 5,7 However, some human mesotheliomas have no clear evidence of asbestos/asbestos-like fiber exposure or other known causative factors like radiation and their etiology remains undetermined. 3,5,6,8
In rats, intrathoracic pleural/pericardial mesotheliomas have been experimentally induced by exposure (usually via intrapleural, inhalation, or intratracheal instillation routes) to asbestos, erionite, and other naturally occurring and synthetic minerals; radionuclides; and carbon nanotubes. 9 –22 Induction of pleural mesotheliomas in rats by orthotopic implantation of syngeneic rat mesothelioma cells (II-45 cells) is a well-described animal model for human pleural mesothelioma. 23,24
On the other hand, spontaneous mesotheliomas in any intrathoracic or extrathoracic site are uncommon in rats. Male Fischer 344 (F344) rats have a demonstrated propensity for naturally arising mesotheliomas of the tunica vaginalis (the mesothelium lining the epididymis, testis, and mesorchium). 25 –27 These spontaneous tunic vaginalis mesotheliomas can disseminate widely throughout the peritoneal cavity although spread to thoracic cavity tissues appears to be rare. 25,28 Although well-described, spontaneous tunica vaginalis mesotheliomas in male F344 rats are nevertheless uncommon, with incidences ranging from 0.2% to 5.0%. 25,29 –31
Atriocaval mesothelioma is an intrathoracic neoplasm that can arise spontaneously in rats. Rat atriocaval mesotheliomas are also thought to develop from mesothelial or mesothelial-like cells but have a well-described distinct morphology, growth pattern, and localization (right atrial wall near the vena cava junction, or at the base of the interventricular septum) that distinguishes them from mesotheliomas arising elsewhere in the thoracic cavity. 32 –36 Incidences of atriocaval mesothelioma of up to 20% have been reported in NZR/gd inbred rats, 35 but in other rat strains these neoplasms appear to be rare, with incidences of less than 1.0% reported in F344 32 and Sprague Dawley rats. 33,36
In contrast, there is limited information about nonatriocaval pleural/pericardial mesotheliomas in rats. Such naturally occurring primary intrathoracic (pleural/pericardial) neoplasms are considered rare. 32,37,38 Single cases of spontaneous pleural/pericardial mesotheliomas have been described in detail in aging male F344/DuCrj 28 and Sprague Dawley (Crj: CD[SD]) rats. 39 One pericardial mesothelioma (in a male) was found in a review of 96 primary cardiac neoplasms in 79,971 F344 rats from National Toxicology Program (NTP) 2-year chronic toxicity and carcinogenicity studies. 32 In a review of spontaneous mesothelioma in a cohort of aging F344/DuCrj rats (1910 males, 1910 females), only 2 pleural mesotheliomas (in a male and female) and 1 pleural/pericardial mesothelioma (in a male) were identified, with no histologic descriptions included. 40 Several individual cases of intrathoracic mesothelioma in F344 rats were characterized by immunohistochemistry by Howroyd et al, 41 but did not distinguish between mesotheliomas that were primary intrathoracic versus potentially metastatic from the peritoneal cavity.
In addition, a few naturally occurring intrathoracic mesotheliomas have been cursorily listed in several general surveys of spontaneous neoplastic lesions in rats. These include mesotheliomas in the “mediastinum” of 1/98 Slc: Wistar male rats 42 and in the “pleura” of one of approximately 300 F344/DuCrj male rats. 43 Two cases of spontaneous “lung or pleura” mesothelioma in a cohort of 529 male F344 rats from NTP 2-year chronic toxicity and carcinogenicity studies were reported by Solleveld et al (these cases predate the period of the current review). 44 These general surveys did not include histologic descriptions so it is unclear if these cases were primary intrathoracic neoplasms versus possible metastases of tunica vaginalis mesotheliomas.
All of the above indicate a paucity of information about spontaneous primary intrathoracic mesotheliomas in rats. However, more detailed characterization of these rare spontaneous neoplasms is important to assist in accurate diagnosis and to provide meaningful historical data. Furthermore, spontaneous primary intrathoracic mesotheliomas in rats may serve as a useful model to better understand nonasbestos-related pleural mesotheliomas in people. The objective of this retrospective study was to better characterize rat spontaneous primary intrathoracic (pleural) mesothelioma by describing the light-microscopic morphology and assessing historical incidences of these neoplasms from a large cohort of rats from the NTP data base.
Materials and Methods
A total of 271 NTP studies that were started and completed, through technical report publication, 45 between 1980 to 2019 were retrospectively searched for the diagnosis of “mesothelioma” in one or more intrathoracic tissue sites (lung, heart, pleura, pericardium, blood vessel, thymus, lymph node [mediastinal or bronchial], mediastinum) using the Chemical Effects in Biological Systems database search engine software. 46 All but two were 2-year (24 month) carcinogenicity studies; the remaining two were lifetime studies (30 months). Details on the surveyed rat cohort are summarized in Supplementary Table 1.
For animals identified by this search, a light-microscopic review was performed on all available glass-slide sections of all intra- and extrathoracic (systemic) tissues, which had been previously paraffin-embedded, sectioned, and stained with hematoxylin and eosin (H&E). Intrathoracic mesotheliomas in these animals were categorized as: (1) nonatriocaval mesotheliomas which occurred within the thorax only (hereafter, “pleural mesothelioma”), (2) nonatriocaval mesotheliomas with involvement in the thorax and in one or more extrathoracic tissues (hereafter, “multicentric mesothelioma”), or (3) atriocaval mesotheliomas. Atriocaval mesothelioma and multicentric mesotheliomas were diagnosed based on established guidelines. 37,47,48
The NTP database search identified 82 cases of mesothelioma with involvement of one or more intrathoracic tissues: 41 multicentric (33 involving the tunica vaginalis), 9 atriocaval, and 32 pleural. All of these cases were in F344 rats with the exception of 2 multicentric mesotheliomas in Sprague Dawley (Hsd: Sprague Dawley SD) rats, and 1 multicentric and 2 pleural mesotheliomas in Wistar Han (CRL: WI[Han]) rats. All multicentric and atriocaval mesotheliomas were excluded from further review. The current review is based on the remaining 32 pleural mesotheliomas (Supplementary Table 2). Gross necropsy records for the pleural mesothelioma cases were also reviewed.
Results
Out of the 32 pleural mesotheliomas reviewed, 30 occurred in F344 rats, representing a 0.03% incidence in this strain (Table 1). Of the affected F344 rats, 22 (73%) were male and 8 (27%) were female. Almost all F344 cases (24) were single instances in given studies (Supplementary Table 2). Three studies had 2 cases of pleural mesothelioma each, with the neoplasms occurring sporadically in different dose groups in these studies. Overall incidences (for all F344 studies combined) were similar for control and treated F344 rats whether the sexes were compared separately or combined (Table 1). Because of their low, sporadic incidences, none of the F344 pleural mesotheliomas were considered treatment related.
Summary Incidence of Pleural Mesothelioma by Sex and Treatment Type in F344 and Wistar Han Rats.
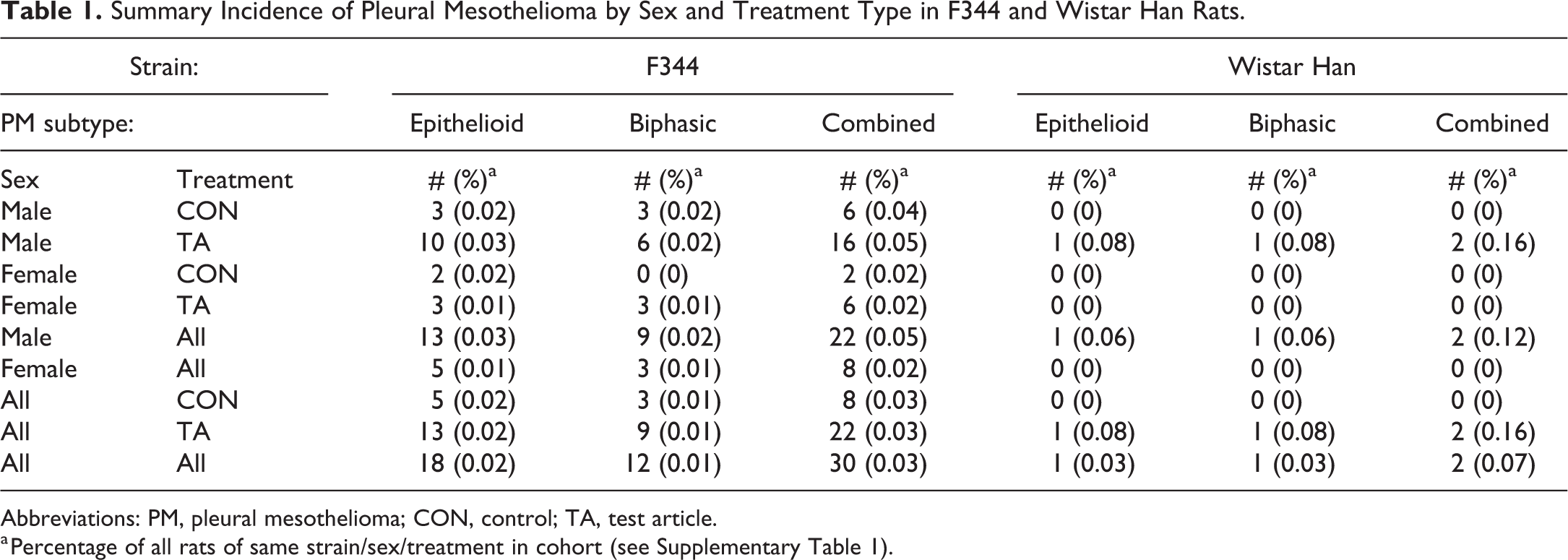
Abbreviations: PM, pleural mesothelioma; CON, control; TA, test article.
a Percentage of all rats of same strain/sex/treatment in cohort (see Supplementary Table 1).
When routes of administration were compared, overall incidences of pleura mesothelioma were higher in F344 rats subjected to whole body inhalation exposure (0.074%) compared to incidences in rats in studies with other administration routes (0.003%-0.041%), excluding the single study in which animals were given subcutaneous injections along with whole body inhalation (Table 2).
Summary Incidence of Pleural Mesothelioma by Exposure Route in F344 and Wistar Han Rats.
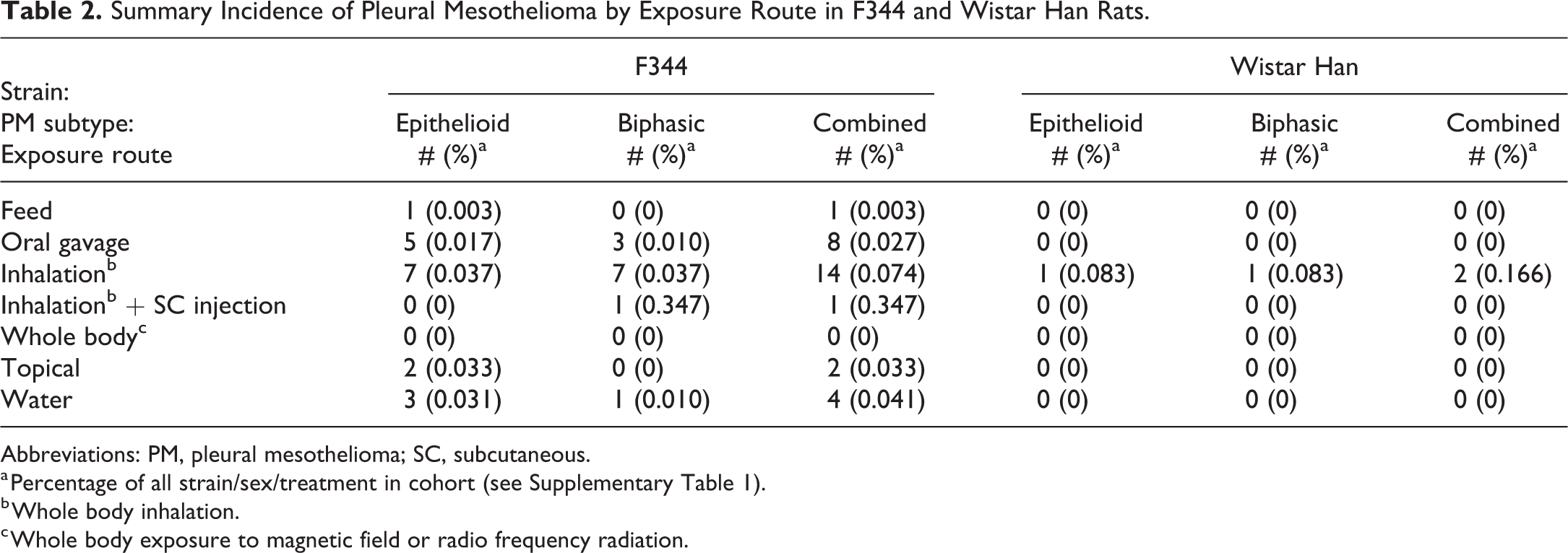
Abbreviations: PM, pleural mesothelioma; SC, subcutaneous.
a Percentage of all strain/sex/treatment in cohort (see Supplementary Table 1).
b Whole body inhalation.
c Whole body exposure to magnetic field or radio frequency radiation.
All F344 pleural mesotheliomas were noted in animals over 1 year of age. At the time of death or euthanasia, F344 rats with pleural mesothelioma had been on test an average of 667 days (range 413-735 days; median 681 days), including 8 rats that survived until terminal euthanasia. Of the 22 affected F344 rats that died or were euthanized early, 8 cases had pleural mesothelioma listed in data records as the primary cause of death; 10 cases had another diagnosis listed as the primary cause of death and 4 had no cause of death listed (Supplementary Table 2).
Out of a total of 2998 Wistar Han rats (1599 male, 1399 female) in the NTP cohort, 2 rats with primary pleural mesothelioma were identified, representing a 0.07% incidence in this strain. Both affected Wistar Han rats were males from a single study (Supplementary Table 2). One male was in the low dose treatment group and died naturally on study day 701; pleural mesothelioma was considered the cause of death. The second affected male was in the mid dose treatment group and survived until terminal euthanasia on study day 730. No other systemic or parenchymal neoplasms or space-occupying lesions of any type were concurrently present in the lungs or other intrathoracic tissues in these 2 animals. In this study, no relationship between test article administration and pleural mesothelioma was identified. The very low overall incidences precluded assessment of any possible sex predisposition in the Wistar Han cohort.
No pleural mesotheliomas were identified among the cohorts of Sprague Dawley rats (6669 rats) or Osborne-Mendel rats (300 rats) in the studies reviewed.
Gross necropsy records were available for all rats with pleural mesothelioma. In 14/29 F344 rats and 1/2 Wistar Han rats, gross lesions were identified in the thoracic cavity at necropsy and histologically associated with pleural mesothelioma. As noted at necropsy, the pleural mesotheliomas were typically described as multiple pale white to red nodules/masses affecting the lung, pleura, mediastinum, diaphragm, or intercostal muscles. Thickening of the pericardium and clear to red fluid within the thoracic cavity were also common necropsy findings in the rats with pleura mesothelioma.
As noted by light microscopy of H&E-stained sections, pleural mesotheliomas in F344 rats were expansile growths which characteristically grew along serosal surfaces of the lung and/or mediastinum (Figure 1A; case no. 32) with occasional extension to the pericardial and epicardial surfaces. The pulmonary pleural surface was most commonly affected (26/30 cases), but mesotheliomas confined to the mediastinum did occur (Supplementary Table 2). Mesotheliomas confined solely to the pericardial/epicardial surfaces were not observed. Compression of subjacent lung by the pleural neoplastic masses was sometimes prominent (Figure 1A) but local invasion into the subpleural parenchyma occurred in only one case (Case no. 20; Supplementary Table 2). However, extensive infiltration of mediastinal or pericardial fat was sometimes present. The light-microscopic morphology of the H&E-stained pleural mesotheliomas in Wistar Han rats was similar to that of the F344 cases.
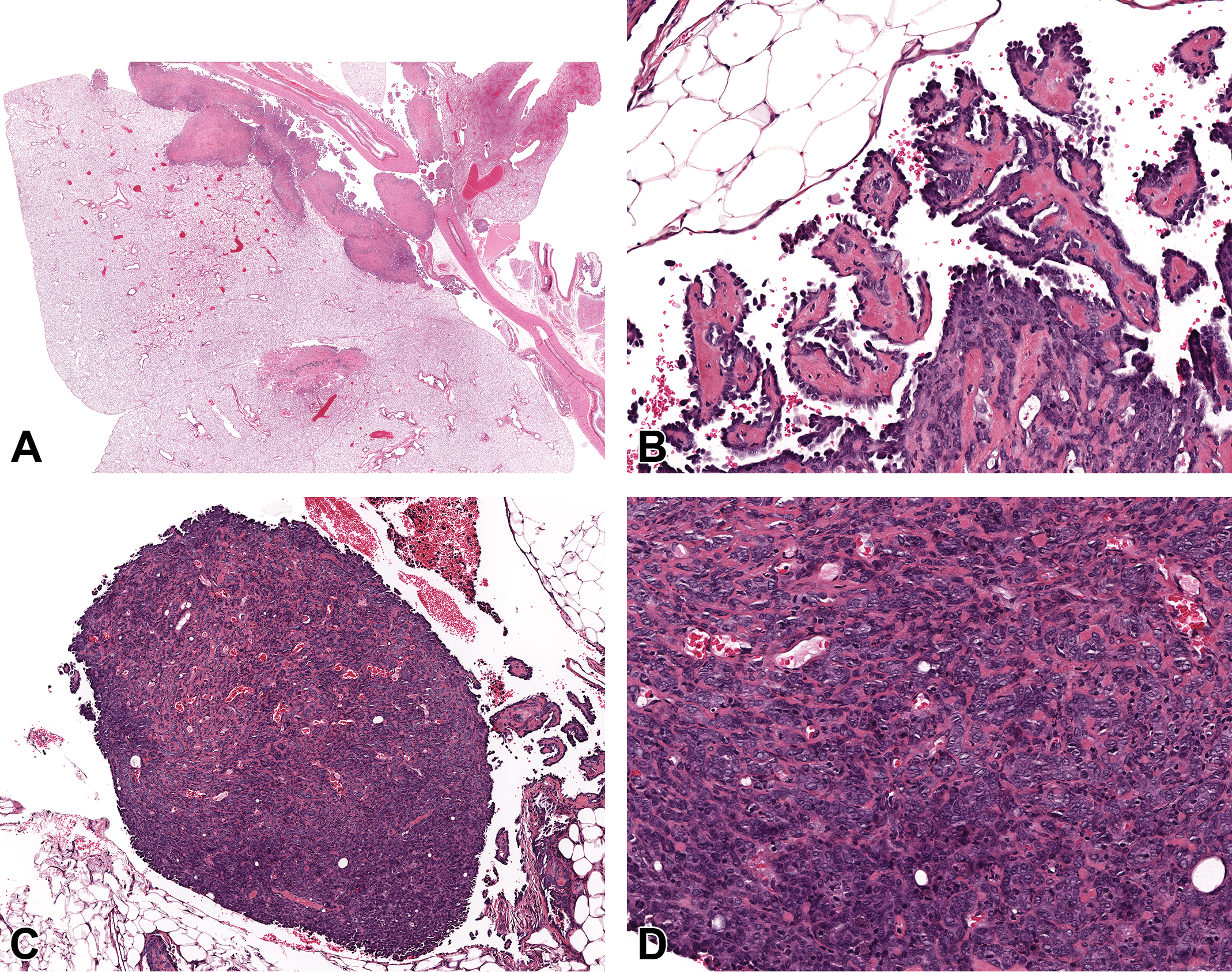
Epithelioid pleural mesothelioma in a male Wistar Han rat (case no. 32). A, Neoplastic masses extend along the pulmonary pleural surface with focal downward compression of the underlying pulmonary parenchyma. B-D, Higher magnification regions of the neoplasm shown in A. B, Multifocally the neoplasm forms papillary projections supported by homogenous, pale eosinophilic (hyalinized) collagenous stroma. C, Neoplastic cells also form solid, densely cellular nodules with scant connective tissue stroma. D, Higher magnification of solid nodule in C. Trabeculae composed of cuboidal neoplastic mesothelial cells are supported by scant collagenous stroma. Hematoxylin and eosin stain.
Pleural mesotheliomas were subdivided histomorphologically into epithelioid (epitheliomatous), biphasic (mixed), or sarcomatoid types based on published diagnostic criteria for rats and mice 37 and similar to the classification of human pleural mesotheliomas. 2,4,49 The majority of the F344 pleural mesotheliomas were classified as epithelioid (18/30), with the remaining 12 classified as biphasic (Table 1). The Wistar Han mesotheliomas were classified as one epithelioid and one biphasic (Table 1). Sarcomatoid types were not observed.
Component cells of epithelioid tumors had distinct cell borders, scant eosinophilic cytoplasm, a high nuclear to cytoplasmic ratio, and round to oval nuclei with large single central nucleoli. In some cases, the constituent cells were large and more pleomorphic with polygonal to elongated outlines. In epithelioid mesotheliomas, neoplastic cells formed papilliform and/or solid patterns. While one pattern typically predominated, both patterns could be identified within the same tumor (Figure 1B-D; case no. 32). Papilliform areas were composed of single to multiple, simple or branching connective tissue projections or trabeculae covered by a single layer of flattened to cuboidal epithelial-type cells (Figure 2A and B; case no. 2). Solid areas were composed of densely cellular sheets, nodules or broad trabeculae with scant connective tissue stroma (Figure 1C-D). In some solid neoplasms, mesothelial cells formed tubules, islands, and cords within the supporting stroma.
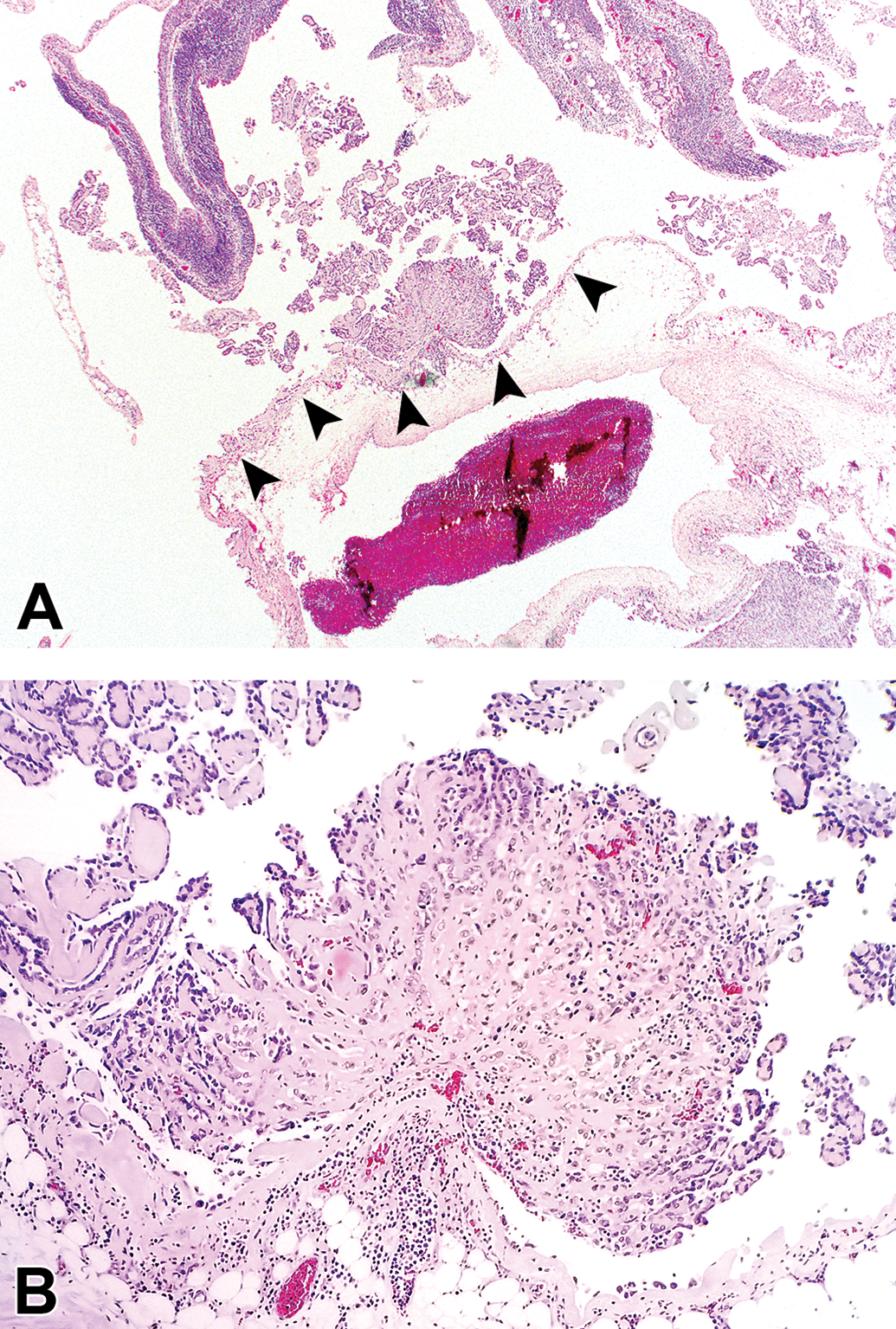
Papillary epithelioid pleural mesothelioma in a male F344 rat (case no. 2). A, Multiple frond-like projections extend from the mesothelial surface (arrowheads) of the mediastinal tissue. B, Higher magnification of A. A characteristic papilliform projection is composed of multiple branching connective tissue trabeculae covered by a single layer of flattened to cuboidal epithelial-type neoplastic mesothelial cells. Hematoxylin and eosin stain.
Biphasic mesotheliomas had papillary and/or solid epithelioid components (similar to those described for epithelioid neoplasms) but also exhibited prominent mesenchyme consisting of variable combinations of dense connective tissue and poorly differentiated spindle cells resembling sarcoma (Figure 3A and B; case no. 28).
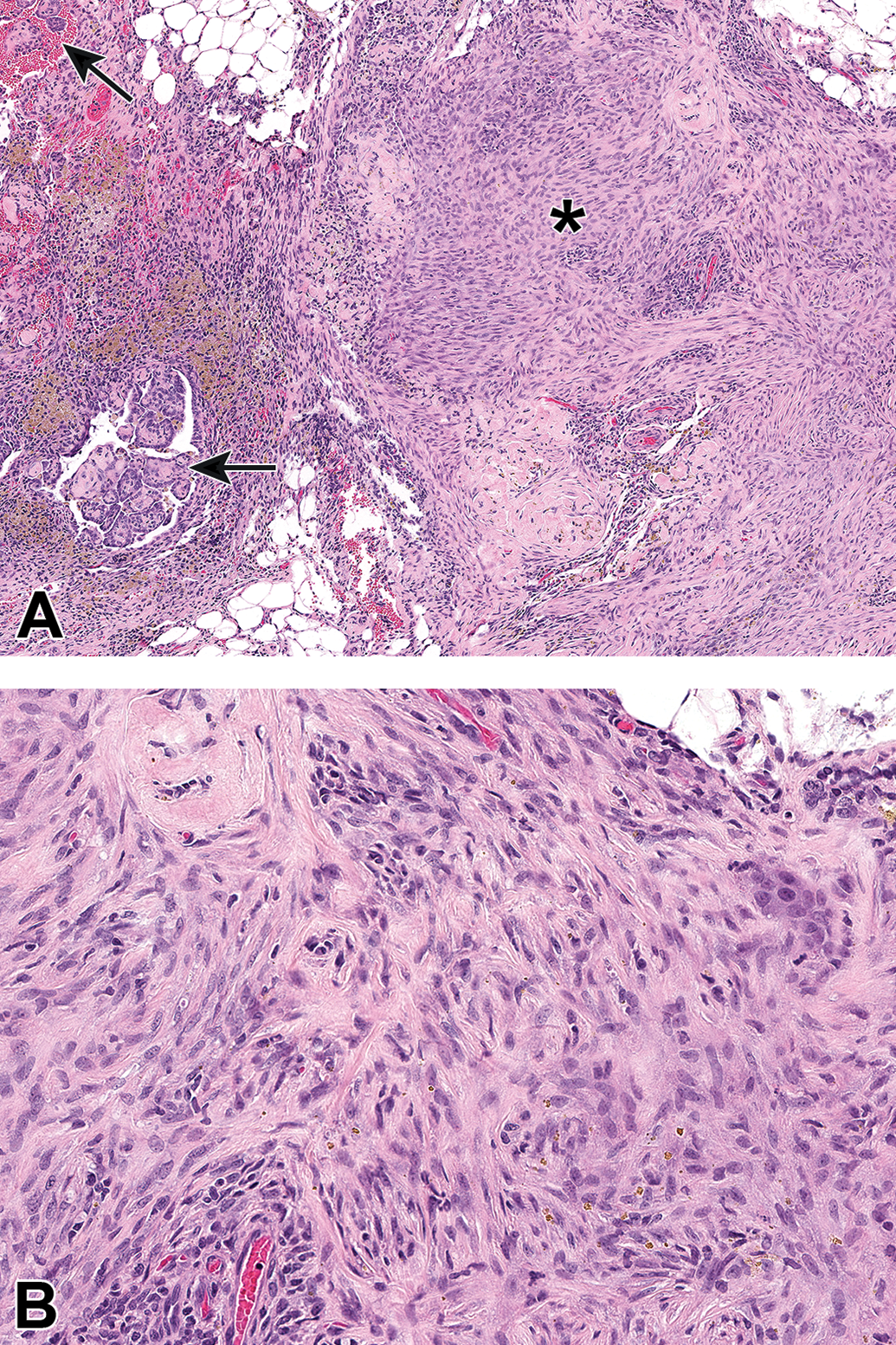
Biphasic pleural mesothelioma in a male F344 rat (case no. 28). A, This biphasic mesothelioma contains both papillary epithelioid projections (arrows) and sarcoma-like regions (asterisk). B, Higher magnification of the sarcoma-like region in A. Spindle-shaped neoplastic mesothelial cells with indistinct cell borders form streams and bundles supported by moderate amounts of collagenous stroma. Hematoxylin and eosin stain.
In all types of pleural mesothelioma, the connective tissue stroma typically had a homogenous, pale eosinophilic (hyalinized) appearance (Figure 1B). Histologic features observed in only a few of the pleural mesotheliomas included erythrophagocytosis; intracytoplasmic eosinophilic globular material of undetermined identity; and extracellular mineralized structures that were either irregularly shaped or concentrically lamellated (psammoma bodies) 39 (Figure 4; case no. 10). Though typically scant, aggregates of pigmented macrophages, mast cells, and lymphocytes were prominent in some cases. Mitotic figures were typically scattered through the neoplasms in low numbers, however, rare tumors contained regions of high mitotic activity. Areas of hemorrhage (both acute and chronic) and necrosis were often present but were not major features. Osseous or cartilaginous differentiation was not observed. 4,15,18,50
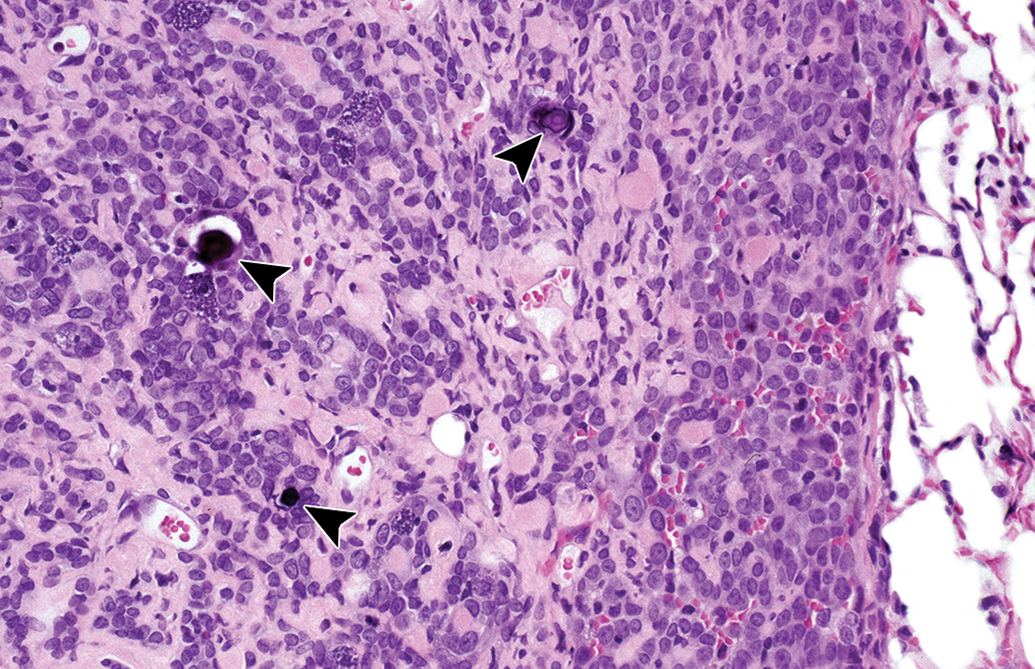
Epithelioid mesothelioma in a male F344 rat (case no. 10). Psammoma bodies (arrowheads) are scattered within a solid tumor region. Hematoxylin and eosin stain.
Five F344 rats with pleural mesotheliomas had concurrent mononuclear cell leukemia in the lungs and intrathoracic lymph nodes (bronchial and/or mediastinal) (Supplementary Table 2). In these 5 cases, the leukemic mononuclear cell infiltrates were diffuse accumulations in vascular lumens and/or tissue parenchyma with no formation of large space-occupying masses. In addition, one rat with mononuclear cell leukemia had a concurrent alveolar-bronchiolar adenoma, measuring approximately 1.5 mm diameter, in one lung lobe. No other systemic or parenchymal neoplasms or large space-occupying lesions of any type were concurrently present in the lungs or other intrathoracic tissues in these 5 animals or any of the other F344 rats with pleural mesothelioma.
Discussion
Previous reports indicate that spontaneous primary mesotheliomas originating in the pleural/pericardial cavities are rare in F344 rats. 32,40,43,44 Incidences of pleural mesotheliomas in F344 rats (0.03% total; 0.05% in males and 0.02% in females) in the present study were also low and thus consistent with these previous surveys (Table 1). It is possible that some of the multicentric mesotheliomas identified but not further characterized in F344 and Wistar Han rats in the current study may have originated from primary pleural mesotheliomas, making the pleural mesothelioma incidences minimum estimates. Nevertheless, these overall incidences indicate that spontaneous primary pleural mesotheliomas are rare in F344, Wistar Han, and Sprague Dawley rats and most likely rare in Osborne Mendel rats.
Determination of test article–related effects often relies on comparison to concurrent control incidences; however in the case of rare neoplasms, such as pleural mesothelioma, historical control rates, among other factors, are useful in determining whether a positive signal is present for the test article. Of the 30 F344 pleural mesotheliomas, 8 occurred in controls and 22 in treated animals (males and females combined), representing similar combined-sex incidences of 0.03% each in control and treated F344 rats (Table 1). Control and treated cases were noted in studies with a variety of test materials. In most instances, only one pleural mesothelioma was present in a given study. In those studies with more than one (up to 2) pleural mesotheliomas, all neoplasms were in different dose groups. For all of these reasons, all pleural mesotheliomas in control and treated F344 rats in the present study were considered spontaneous and unrelated to treatment. It is notable that the only 2 cases in Wistar Han rats occurred in a single study in test article–treated males: 1/50 (2%) low dose males and 1/50 (2%) mid-dose males. Based on the NTP study report, 51 these mesotheliomas were not considered related to the tested compound. The incidence of mesothelioma at any site in males in this study was 1/50, 2/50, 1/50, and 2/50 in control, low dose, mid dose, and high dose groups, respectively. The historical control rate for mesothelioma, at any site, in Wistar Han rats in NTP studies averages 1.71% (range 0%-4%). 52 There were no incidences of intrathoracic mesothelial hyperplasia diagnosed in any group in this study. Taken together, these factors support a spontaneous nature for these pleural mesotheliomas. However, consideration should be given to distinguishing between pleural mesotheliomas and mesotheliomas arising elsewhere when evaluating incidence rates, particularly in strains such as F344 that are predisposed to tunica vaginalis mesotheliomas.
In previous reports and surveys of F344 and other rat strains, most or all of the pleural/pericardial mesotheliomas occurred in males compared to females, 28,32,39 –43 suggesting a possible male sex predisposition for these neoplasms. Likewise, in the present study, 2.5 times as many neoplasms were noted in F344 males (22/30) compared to females (8/30) (Table 1). Although not definitive, these results support the premise that primary pleural mesotheliomas in F344 rats may also have a male sex-predisposition similar to the unequivocal F344 male predisposition for peritoneal (tunica vaginalis) mesotheliomas. 25,26 Although there were too few cases in the Wistar Han strain to evaluate possible sex predisposition, it is notable that both cases identified occurred in male rats as well. There were no clear morphologic differences in the pleural mesotheliomas among male and female rats in this cohort. In people, the predominance of pleural mesothelioma in men is partly attributable to greater occupational exposure to asbestos or similar fibers. 5,7 Such exogenous exposures cannot account for the apparent male sex predisposition in this retrospective review, suggesting endogenous, sex-related factors may play a role. Sex differences in epigenetics, metabolism, response to cellular stress, and immunity have all been postulated to play a role in cancer development. 53
Histologically, human mesotheliomas are classified into 3 broad categories (with many subtypes): epithelioid (epitheliomatous), sarcomatoid, or biphasic (mixed), 2,4,49 and this general histological classification is also recommended for the classification of mesothelioma in all sites in rats and mice. 25 –27,37 Using these established criteria for rat mesothelioma, all primary spontaneous pleural mesotheliomas in the present study were categorized as epithelioid (18 in F344 rats; 1 in Wistar Han) or biphasic (12 in F344; 1 in Wistar Han). No sarcomatoid cases were observed. These results are consistent with the general observation that epithelioid-type neoplasms are the most common type of spontaneous peritoneal/pleural mesotheliomas in rats. 27 Many reports of experimentally induced pleural mesotheliomas in rats either do not histologically subtype the neoplasms; consist of very low numbers of cases; and/or vary in whether epithelioid or sarcomatoid subtypes had the higher incidences. 9 –15,17,18,21,40 These methodological disparities preclude plausible comparison of subtype incidences in the present series versus incidences in previous reports of induced pleural mesotheliomas.
In rats, pleural mesothelioma must be differentiated from mesothelial hyperplasia and other intrathoracic neoplasms. 27,37,54 Mesothelial hyperplasia, which is considered by many authors to have the potential to progress to mesothelioma, can precede or be concurrent with peritoneal/pleural mesotheliomas in rats. 9,12,15,20,50,55 The light microscopic diagnostic criteria for hyperplasia include focal or papillary proliferation of mesothelial cells with little or no connective tissue stroma or extension/invasion into adjacent tissues. 27,37 Because mesothelial cells can contain hyaluronan (hyaluronic acid), stains suggestive of hyaluronan, like hyaluronidase-sensitive Alcian blue, and colloid-iron stains have been used in humans and occasionally in rats to help distinguish mesothelial proliferations from other types of neoplasms. 28,39 Invasion of the lung, diaphragm, myocardium, and other thoracic cavity tissues can occur in spontaneous and induced pleural mesotheliomas in rats. 13,14,39 In the present series, infiltration of mediastinal and pericardial fat occurred commonly to varying degrees; however, infiltration of the lung parenchyma was seen in only one case in which shallow infiltration of subpleural lung parenchyma occurred. This may be another useful feature in discerning pleural mesothelioma from bronchioloalveolar carcinomas in rats. Mediastinum-only bronchioloalveolar carcinomas rarely occur in rats but can also pose a differential diagnostic challenge, especially distinguishing them from epithelioid mesotheliomas. Howroyd et al 41 found that mediastinal-only bronchioloalveolar carcinomas were negative for WT-1 (Wilm’s tumor susceptibility gene product) and positive for CCSP (club-cell secretory protein) while several pleural mesotheliomas had opposite results (WT-1 positive; CCSP negative).
A variety of factors have been implicated in the pathogenesis of mesothelioma in humans and rodents, including environmental exposures, genetic mutations, inflammation, and mechanical forces. In the present survey, there were no known extraneous exposures to asbestos, other mineral fibers, radionuclides, or other known causes of pleural mesotheliomas in humans and experimental animals. 1,3,4,19,56 In humans, genetic factors, including germline mutations, may play a role in the development of pleural mesothelioma with or without exposure to asbestos or other mineral fibers. 3,4,56 –60 Genomic alterations (deletion of CDKN2A/2B and amplification of ERBB2, a receptor-type tyrosine kinase involved in cell proliferation) have been associated with experimental iron-induced peritoneal mesotheliomas in rats. 61 Thus, it is possible that sporadic genetic alterations might play a role in development of naturally occurring pleural mesotheliomas in rats. Some evidence suggests that chronic serosal inflammation may be a risk factor for development of nonasbestos-related mesothelioma in humans. 4,62 However, inflammation of intrathoracic tissues was not a prominent histologic feature in most of the rat pleural mesotheliomas in this survey, so any possible role in development of pleural mesotheliomas in these cases remains undetermined.
In the present survey, overall incidences of pleural mesothelioma (0.074%) were higher in rats subjected to inhalation exposure (whole-body) compared to incidences (0.003%-0.041%) in rats subjected to other administration routes (Table 2). It remains undetermined if this distribution was fortuitous and random or possibly related to the inhalation route. Prior studies have identified different rates of testicular adenomas and pituitary gland neoplasms between feeding study and inhalation study control F344 rats. 30 Stress related to individual housing, used in inhalation studies, versus group housing, used in feed studies, was postulated for this difference. Which factors, if any, related to inhalation administration (eg, increased general stress, increased inflammation or irritation of intrathoracic tissues) that may play a role in pleural mesothelioma development remains undetermined. Such data further supports assessing historical control rates by administration route when possible.
One hypothesis for the prevalence of tunica vaginalis mesotheliomas in male F344 rats is that enlargement of the testes by frequently-occurring Leydig cell tumors exert physical forces on the tunica vaginalis that stimulate mesothelial proliferation. 28 In the present series, five F344 rats with pleural mesothelioma had mononuclear cell leukemia, a very common spontaneous systemic neoplasm in F344 rats, 25,30 in the lungs and intrathoracic lymph nodes, but these infiltrates did not coalesce into space-occupying masses. One F344 rat had a small (1.5 mm diameter) concurrent alveolar-bronchiolar adenoma. Neither these 5 animals nor any of the other rats with pleural mesothelioma had other space-occupying lesions in any intrathoracic tissue. Thus, there is no evidence that any such proposed “physical forces” were a potential causative factor in the pleural mesotheliomas in this series.
In conclusion, the pathogenesis of the spontaneous primary pleural mesotheliomas in this series remains undetermined. However, the results of the present survey do indicate that naturally occurring primary pleural mesotheliomas are rare in F344, Wistar Han (CRL: WI(Han), and Sprague Dawley (Hsd: Sprague Dawley SD) rats and may also be rare in Osborne-Mendel rats. In the F344 rat subcohort in the present study, primary pleural mesotheliomas appeared to have a male sex-predisposition similar to that for peritoneal (tunica vaginalis) mesotheliomas in this strain. There were too few cases in the Wistar Han strain to evaluate possible sex predisposition. The light microscopic features of these rat pleural mesotheliomas were generally similar to those of human pleural mesothelioma and rat peritoneal/pleural mesotheliomas, so in accordance with histologic diagnostic criteria for mesothelioma in rats and humans, the pleural mesotheliomas in this survey were classified as epithelioid and biphasic; no sarcomatoid types were noted in this series. Some of the morphologic features described in this report might be useful in differentiating epithelioid pleural mesotheliomas from other intrathoracic neoplasms in rats such as metastatic carcinomas in the lung and mediastinum-specific bronchioloalveolar carcinomas. Future studies to characterize the genetic profiles, particularly for tumor suppressor genes, of spontaneous primary pleural mesotheliomas in rats may be useful in elucidating the pathogenesis of these tumors and their comparative potential for spontaneous pleural mesothelioma in humans.
Supplemental Material
Supplemental Material, sj-docx-1-tpx-10.1177_01926233211053631 - Spontaneous Primary Pleural Mesothelioma in Fischer 344 (F344) and Other Rat Strains: A Retrospective Review
Supplemental Material, sj-docx-1-tpx-10.1177_01926233211053631 for Spontaneous Primary Pleural Mesothelioma in Fischer 344 (F344) and Other Rat Strains: A Retrospective Review by Debra A. Tokarz, Margarita M. Gruebbel, Gabrielle A. Willson, Jerry F. Hardisty, Gail Pearse and Mark F. Cesta in Toxicologic Pathology
Supplemental Material
Supplemental Material, sj-pdf-1-tpx-10.1177_01926233211053631 - Spontaneous Primary Pleural Mesothelioma in Fischer 344 (F344) and Other Rat Strains: A Retrospective Review
Supplemental Material, sj-pdf-1-tpx-10.1177_01926233211053631 for Spontaneous Primary Pleural Mesothelioma in Fischer 344 (F344) and Other Rat Strains: A Retrospective Review by Debra A. Tokarz, Margarita M. Gruebbel, Gabrielle A. Willson, Jerry F. Hardisty, Gail Pearse and Mark F. Cesta in Toxicologic Pathology
Supplemental Material
Supplemental Material, sj-xlsx-1-tpx-10.1177_01926233211053631 - Spontaneous Primary Pleural Mesothelioma in Fischer 344 (F344) and Other Rat Strains: A Retrospective Review
Supplemental Material, sj-xlsx-1-tpx-10.1177_01926233211053631 for Spontaneous Primary Pleural Mesothelioma in Fischer 344 (F344) and Other Rat Strains: A Retrospective Review by Debra A. Tokarz, Margarita M. Gruebbel, Gabrielle A. Willson, Jerry F. Hardisty, Gail Pearse and Mark F. Cesta in Toxicologic Pathology
Footnotes
Acknowledgments
The authors thank Michelle McCrimmon, Emily Singletary, Maureen Puccini, and Dr Karen Cimon of Experimental Pathology Laboratories, Inc. for their excellent technical and editorial assistance.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was supported by the Intramural Research Program of the NIH, National Institute of Environmental Health Sciences, contract no. HHSN273201500014C.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
