Abstract
Keywords
Introduction
Schwannomas are generally benign, slow-growing tumors of Schwann cell origin and central, peripheral, or autonomic nervous system; approximately 25% to 45% of schwannomas are found in the head and neck region.1,2 Cervical sympathetic chain (CSC) schwannoma (CSCS) is a rare disease, with most cases reported in the literature as case reports.2-5
The superior cervical ganglion of CSC is the primary contributor to supplying post-ganglionic fibers to the head and neck region; ultimately, these sympathetic fibers serve critical roles in the “fight or flight” mechanisms of the autonomic nervous system through pupil dilation, inhibition of tear production, vasoconstriction of skin vasculature, and widening of the palpebral fissures. 6 If CSC could not be preserved during the CSCS surgery, which is frequently encountered as reported in the literature,7-9 Horner’s syndrome (HS) and first bite syndrome (FBS) could occur, and patients’ quality of life could be seriously affected, especially by the latter.10-12
Hence, successful intracapsular enucleation (ICE) of CSCS would significantly improve patients’ outcomes.13,14 As we have reported in our previous series of CSCS cases, intraoperative hemorrhage could be quite diffuse, making hemostasis rather difficult and time-consuming (sometimes even as long as the enucleation procedure itself). 14 We believe that postoperative HS could result from heat injury to CSC during the prolonged period of hemostasis. Therefore, we tried to achieve ICE and hemostasis with a different strategy, which significantly improved the patients’ surgical procedures and outcomes.
Patients and Methods
A retrospective review of CSCS cases treated at our tertiary medical institution was conducted between April 2018 and February 2024. The clinical and demographic data were retrieved from case records. The institutional review board approved the protocol of the research project, which conformed to the provisions of the Declaration of Helsinki. The patients signed a written consent form.
Diagnosis and Informed Consent
For an asymptomatic cervical lump, an ultrasound examination could reveal its proximity to the carotid sheath, indicating its possible nerve origin. Then, computed tomography scan or magnetic resonance imaging (preferred modality) with contrast would further reveal the relationship between the mass, common carotid artery (CCA), internal carotid artery (ICA), and internal jugular vein (IJV).
Furukawa’s criteria are quite useful for the differential diagnosis of this anatomic site. These criteria were proposed in 1996 and were based on 9 cases, 5 of which were vagal nerve schwannoma (VNS), and the remaining 4 were CSCS. For VNS, the schwannoma grew between CCA and IJV or between ICA and IJV, increasing the distance between the artery and vein (separation), whereas for CSCS, no separation was observed between IJV and CCA or ICA (Figure 1A). 15
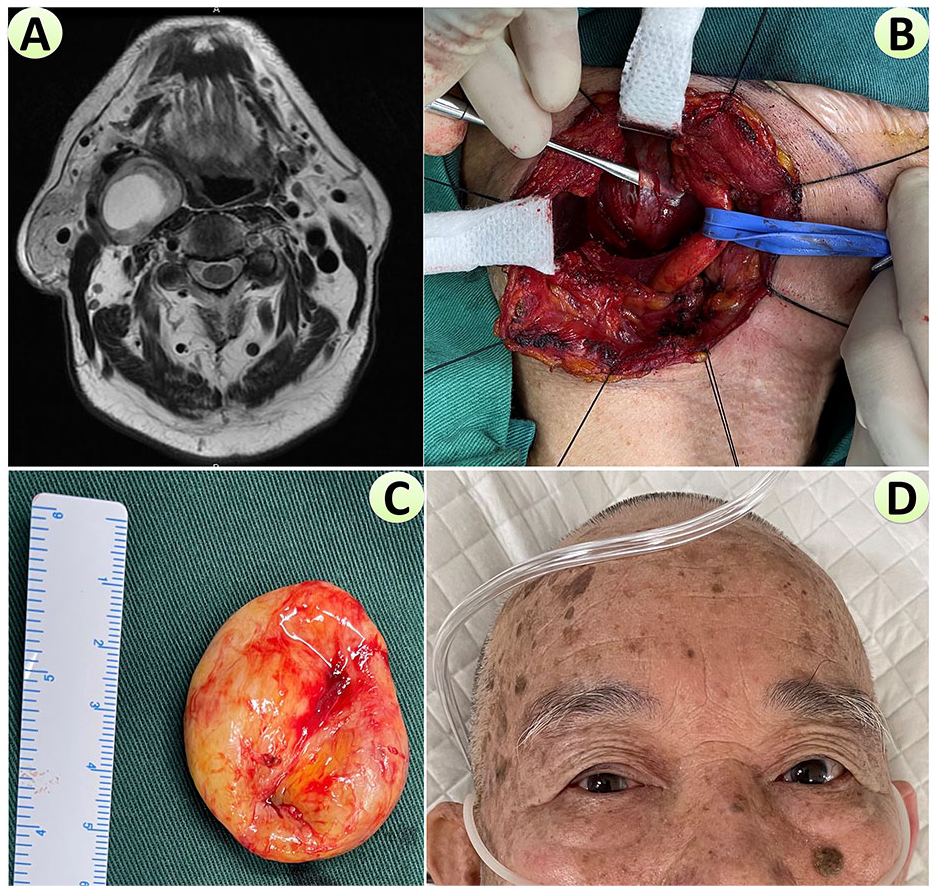
Preoperative, intraoperative, and postoperative images of Case 5. (A) Preoperative T2-weighted MRI image demonstrated a heterogeneous mass (with possible central cystic degeneration and accumulation of fluid content), pushing the carotid arteries and internal jugular vein antero-laterally, without obviously separating them. (B) Intraoperative image showed the common carotid artery medially retracted by the blue vascular band. The fibrous capsule of the CSCS has been incised longitudinally and away from the CSC nerve fiber. Blunt dissection with a cold instrument between the capsule and tumor parenchyma was performed. (C) ICE of the CSCS was achieved, and the complete mass measuring about 5 cm in diameter was demonstrated. During the ICE procedure, some internal fluid had burst out under the retraction tension, rendering the mass smaller. (D) Partial ptosis of the right upper eyelid presented 2 hours after surgery. MRI, magnetic resonance imaging; CSCS, cervical sympathetic chain schwannoma; CSC, cervical sympathetic chain; ICE, intracapsular enucleation.
However, the situation here could be more complicated than just Furukawa’s criteria. In 2017, based on 20 cases (9 VNS and 11 CSCS cases), Graffeo et al demonstrated (through multivariate modeling) a 75% probability of VNS if both ICA/IJV splaying and medial ICA displacement were observed and an 87% probability of CSCS if no ICA/IJV splaying with lateral ICA displacement was observed. 16 According to these predictions, surgeons should be more careful in preoperative counseling because postoperative neurological deficits could differ from preoperative predictions (eg, hoarseness vs ptosis) based on a judgment of the nerve of origin. Moreover, we had already encountered such a discrepancy 3 times. Fortunately, our informed consent was comprehensive, and no patient complained.
Surgical Procedures
Incision, flap elevation, and identification of anatomical landmarks were identical to our previous work. 14 After longitudinal incision of the fibrous capsule, blunt dissection with cold instruments could usually separate tumor parenchyma from the fibrous capsule (Figure 1B). However, the main change regarding the strategy of enucleation of CSCS was that whenever we encountered a connection between capsule and tumor parenchyma, we would not divide it until it was managed securely under loupe magnification: when a nourishing vessel was apparent, it was ligated with knots near tumor parenchyma, and away from the capsule. However, even if the connection appeared to be a ligament with no apparent vessel, we still dissected it away from the capsule and divided it with bipolar coagulation near tumor parenchyma. After complete enucleation (Figure 1C), the inner surface of the capsule was irrigated with normal saline solution with a coagulation agent (eg, Hemocoagulase Bothrops Atrox). After secure hemostasis, a negative pressure drain was placed and the incision was closed.
Patients were observed closely for onset of HS every 2 hours after surgery. The drain was removed when daily drainage was less than 10 mL, and the patient was discharged.
Follow-Up
Patients were routinely followed up every month in the outpatient clinic for the outcome of postoperative complications, especially concerning the dynamic changes of HS. After recovery from HS, the patients were followed up every 3 months.
Statistical Analysis
The differences in continuous data were assessed for significance using the Student’s t test. A 2-tailed P value of <.05 was considered significant. All statistical analyses were performed using SPSS 26.0 (IBM Corp., Armonk, NY, USA).
Results
A total of 8 cases were included, with 4 male and 4 female patients. The patients’ ages ranged from 23 to 77 years, with average and median ages of 48.5 and 49.5 years, respectively. The presenting symptom was a neck mass in all the cases, with 4 on the left and 4 on the right side (Table 1).
Clinical Data of Our Patients With Cervical Sympathetic Chain Schwannoma.
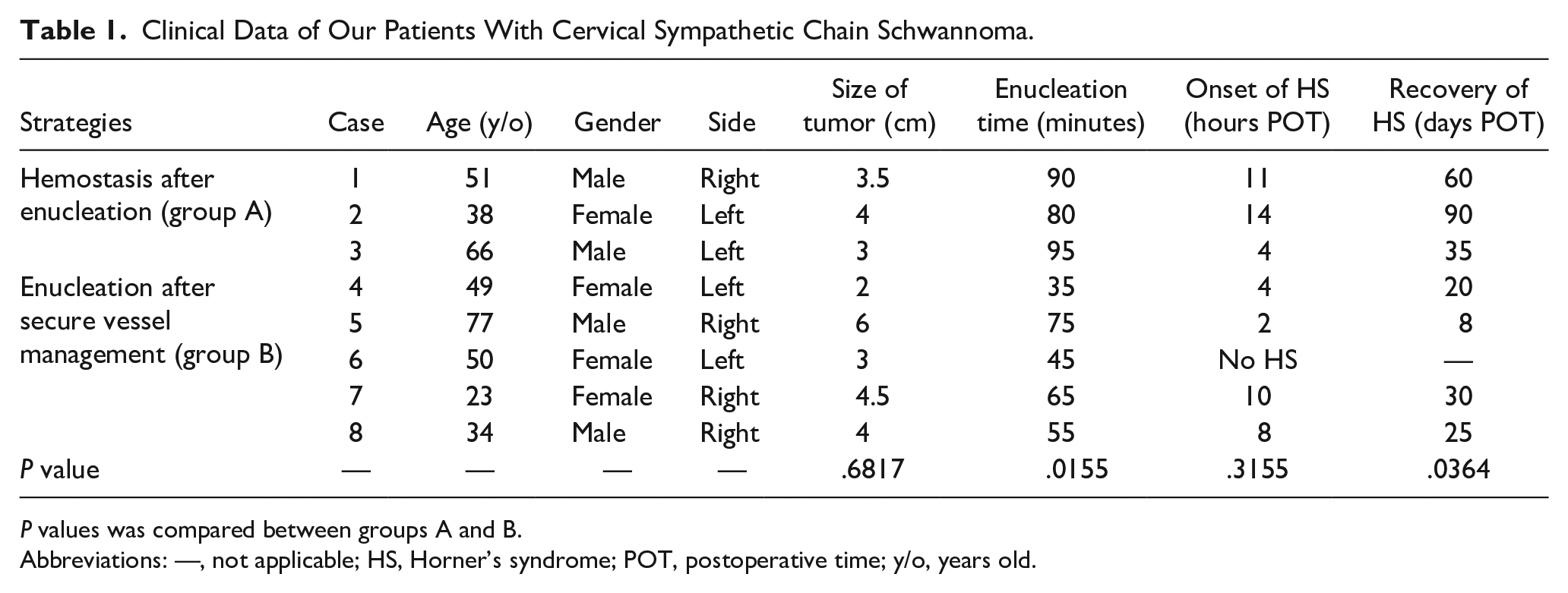
P values was compared between groups A and B.
Abbreviations: —, not applicable; HS, Horner’s syndrome; POT, postoperative time; y/o, years old.
Enucleation was first undertaken for the first 3 cases (Cases 1-3, between April 2018 and March 2022, group A), followed by hemostasis. However, this strategy was quite difficult and relatively time-consuming (80-95 minutes; Table 1). For the remaining 5 cases (Cases 4-8, between March 2022 and February 2024, group B), a novel strategy was developed to preemptively manage any potential nourishing vessel between the capsule and tumor parenchyma. This strategy significantly decreased operation time (35-75 minutes, P = .0155). The greatest diameters of tumors of the 2 groups were not significantly different (P = .6817). Furthermore, the hemorrhage was much less difficult to control. We assumed that the advantage of this new strategy was that the managed small vessels could no longer retract into the capsule, facilitating hemostasis in group B.
FBS was avoided in all cases. Postoperative HS was avoided in 1 patient (Case 6, new strategy), but it occurred in 7 patients, taking 8 days to 1 month to resolve with the new strategy (4 patients in group B), significantly shorter than before (3 patients in group A, 1-3 months; Table 1; P = .0364). The onset of postoperative HS (Figure 1D) occurred between 2 and 14 hours after surgery, with no significant difference between the 2 strategies (P = .3155). Recovery of all 8 patients was otherwise uneventful.
The average and median duration of follow-up was 22.5 and 20 months, respectively. No recurrence was documented.
Discussion
Asymptomatic, painless, progressive, upper lateral neck swelling is the usual mode of presentation of CSCS, while other symptoms might include dysphagia, voice changes, or other cranial nerve deficits. 17 Tumor expansion occurs in the plane of least resistance, medially toward the tonsil and lateral pharyngeal wall, and posteriorly into the retromandibular area, presenting as a medial displacement of the tonsil, soft palate, and pharynx, or as a mass near the angle of the mandible. 18 Very rarely, CSCS might cause neuropathic pain of the ipsilateral face and shoulder, accompanied by ipsilateral hyperhidrosis, lacrimation, and nasal congestion, refractory to analgesic and antimigraine medications, which might resolve following the surgical resection of the CSCS. 19 Symptoms of paralysis of various nerves, such as hoarseness or HS, might aid in differentiating VNS from CSCS, but only a few patients exhibit preoperative paralysis. 20
A meta-analysis based on 89 CSCS cases revealed an age range of 18 to 74 years (with an average age of 42.6), and 69.7% were asymptomatic. Unfortunately, extracapsular resection involving nerve sacrifice, rather than ICE with nerve preservation, was the most frequently performed surgical procedure (87.6% vs 12.4%, respectively), irrespective of mass size. 21 According to some authors, the mass could not be resected without sacrificing a portion of the chain. 7 Other authors reported they could not preserve sympathetic nerves in all cases due to the tumor’s large size, 9 while sometimes the reason for sacrificing CSC was not elucidated. 8 Therefore, it seems reasonable to schedule an ICE procedure when a CSCS is discovered, especially when the CSCS is still not very large (<4 cm) and could potentially be separated from CSC.
However, during our first 3 ICE attempts, ICE proved quite challenging. On one hand, we were fortunate that, in none of the 3 cases did we encounter adhesion between CSCS and CSC nerve fiber. On the other hand, we used cold instruments for enucleation because we were afraid to cause heat injury to the CSC nerve fiber that was immediately outside the tumor capsule. However, the hemorrhage within the capsule was very diffuse, and the responsible vessels were difficult to find (some tiny vessels might have been hidden within the ligaments between the capsule and tumor). Furthermore, hemostasis could be rather difficult to achieve. We had to stop enucleation constantly and use bipolar coagulation to control hemorrhage with saline irrigation to prevent heat injury to the CSC nerve fiber immediately outside the capsule. This strategy increased the operation time and might have caused heat injury to the CSC nerve fiber. Although postoperative HS recovered in all 3 patients, the recovery time was longer (Table 1).
Therefore, we held several group discussions, proposing that since the responsible vessel for the diffuse hemorrhage could not be easily identified and hemostasis was so time-consuming, it was advisable to control potential vessel damage preemptively. Hence, a revised strategy was adopted: whenever a connection between the capsule and tumor parenchyma was discovered, we would not divide it until it was securely managed. The connection could be gently lifted away from the capsule by traction on the tumor parenchyma and divided near the tumor parenchyma. This way, we could decrease vessel damage and experience less hemorrhage. Moreover, significantly less time was needed for the ICE process because hemorrhage was controlled better, even in a large mass (Case 5, Table 1). The duration of recovery of postoperative HS with the new strategy (Cases 4-8, group B) was also significantly shorter than that with the old strategy (Cases 1-3, group A). In one female patient (Case 6), HS did not present postoperatively, although she did not consent for her masked photo to be published.
Furthermore, malignant triton tumors could arise from CSC. 22 Hence, when a CSC tumor is discovered, we would not recommend observation; instead, we recommend intervention.
The main limitation of this study is the small sample size. Hence, the management algorithm we proposed needs validation using more cases. However, it is our great joy that we could develop a better strategy to improve the ICE process for CSCS and achieve better outcomes for such patients.
Conclusion
ICE could be achieved for CSCS surgeries, especially with our newly developed strategy to preemptively and securely manage potential nourishing vessels. Operation time could be significantly shortened. When CSC is preserved, postoperative FBS can be avoided; although postoperative HS could still occur, the duration of recovery could also be shorter with the novel strategy.
Footnotes
Acknowledgements
Not applicable.
Author Contributions
Shan-Shan Zhu and Hui Zhang reviewed medical records, analyzed data, and participated in patient follow-up. Yan-Bo Dong participated in treatment of patients and figure configuration. Yu-He Liu made contributions to revising manuscripts. Cheng Lu participated in treatment of patients, and made contributions to revising multiple versions of manuscripts. Wan-Xin Li participated in treatment of patients, reviewed literature, and wrote multiple versions of manuscripts.
Availability of Data and Materials
All data, models, and code generated or used during the study appear in the submitted article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by Beijing Hospitals Authority’s Ascent Plan (grant number DFL20220102), National Natural Science Foundation of China for Young Scholars (grant number 82303642), and Beijing Friendship Hospital Seed Project, Capital Medical University (grant number YYZZ202125).
Ethics Approval
The protocol for the research project has been approved by Bioethics Committee of Beijing Friendship Hospital, Capital Medical University.
Statement of Informed Consent
Written informed consent was obtained from the patients for their anonymized information to be published in this article.
Statement of Human and Animal Rights
All procedures in this study were conducted in accordance with the institutional review board’s approved protocols (2023-P2-015-01).
