Abstract
Esophageal foreign bodies (FBs) are one of the common emergencies in otolaryngology, usually involving objects accidentally swallowed, and generally do not result in severe respiratory distress. This article presents an extremely rare case of an esophageal FB, where a 44-year-old man accidentally ingested an entire mantis shrimp while sucking its flavored tail, and was sent to the emergency department for severe throat pain and difficulty breathing. We immediately performed a laryngoscopy that revealed the FB that obstructs the entrance of the esophagus, obstructing the glottis due to the long shape of the shrimp. The mantis shrimp had barbs on its shell and trying to remove it intact would cause significant damage to the pharyngeal mucosa. Therefore, we extracted the mantis shrimp in segments under general anesthesia and applied electrocoagulation to stop bleeding from the damaged and bleeding posterior pharyngeal mucosa. As an esophagography was performed the following day, there were no signs of esophageal perforation. Through the detailed description and analysis of this case, our aim is to raise clinical awareness among physicians of such rare occurrences. Most important, appropriate examination and procedures of FBs should be performed based on the type, shape, and location of the FB.
Introduction
Ingestion of foreign bodies (FBs), including impaction in the esophagus, is a frequently encountered clinical problem in China, and the ingestion of esophageal FBs in adults is usually accidental. 1 The impaction of an esophageal FB depends on its size and shape. The typical clinical manifestations include dysphagia, odynophagia, or a sensation of a FB, while asphyxiation, stridor, and respiratory distress can occur in patients with airway obstruction or aspiration, although they are rare in cases of esophageal FB. 2 If the FB is a sharp object, an emergency endoscopy is required due to the high risk of esophageal perforation. 3 In rare cases, sharp FBs cause esophageal perforation and migrate to the soft tissue of the neck, requiring an external approach to remove. 4 In this article, we report a case of an esophageal FB caused by a mantis shrimp. The patient experienced difficulty breathing due to the long shape of the intact swallowed shrimp obstructing the glottis. The barbs on the mantis shrimp’s shell made removal difficult under local anesthesia, therefore it was emergency removed under general anesthesia. The patient’s respiratory distress was relieved after surgery, and fortunately there was no occurrence of esophageal perforation.
Case Presentation
A 44-year-old man accidentally swallowed a whole mantis shrimp while laughing during a meal and was sent to the emergency department for severe throat pain and difficulty breathing. We immediately performed a laryngoscopy, which revealed that the long shape of the shrimp had obstructed the glottis, leaving only a narrow gap (as shown in Figure 1). The barbs on the shell of the mantis shrimp caused the pain to the patient on attempting removal. Considering that removing intact mantis shrimp under local anesthesia could potentially cause severe injury to the esophageal and pharyngeal mucosa, emergency surgery was immediately ordered.
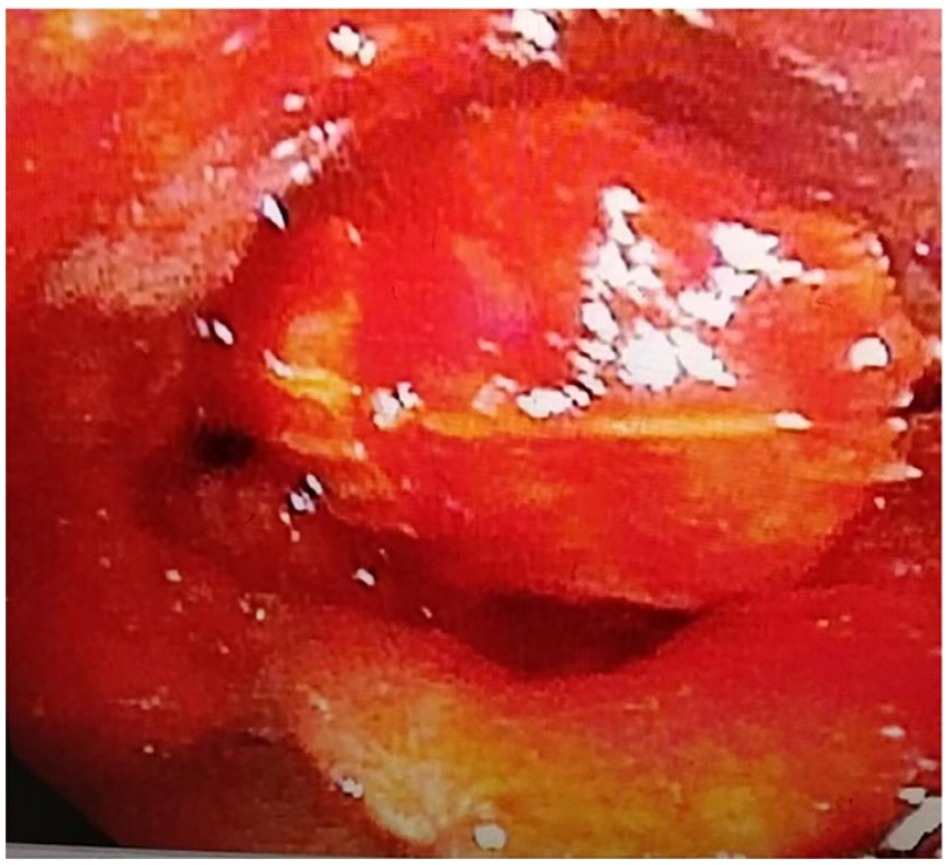
Laryngoscope image. The mantis shrimp is visible, blocking the glottis, leaving only a narrow gap.
When the anesthesiologist prepares to perform awake tracheal intubation using a video laryngoscope, it was found that the mantis shrimp was obstructing most of the glottis, preventing the insertion of a standard adult-sized endotracheal tube. Therefore, the anesthesiologist chose a thinner pediatric endotracheal tube and carefully completed the tracheal intubation (as shown in Figure 2).
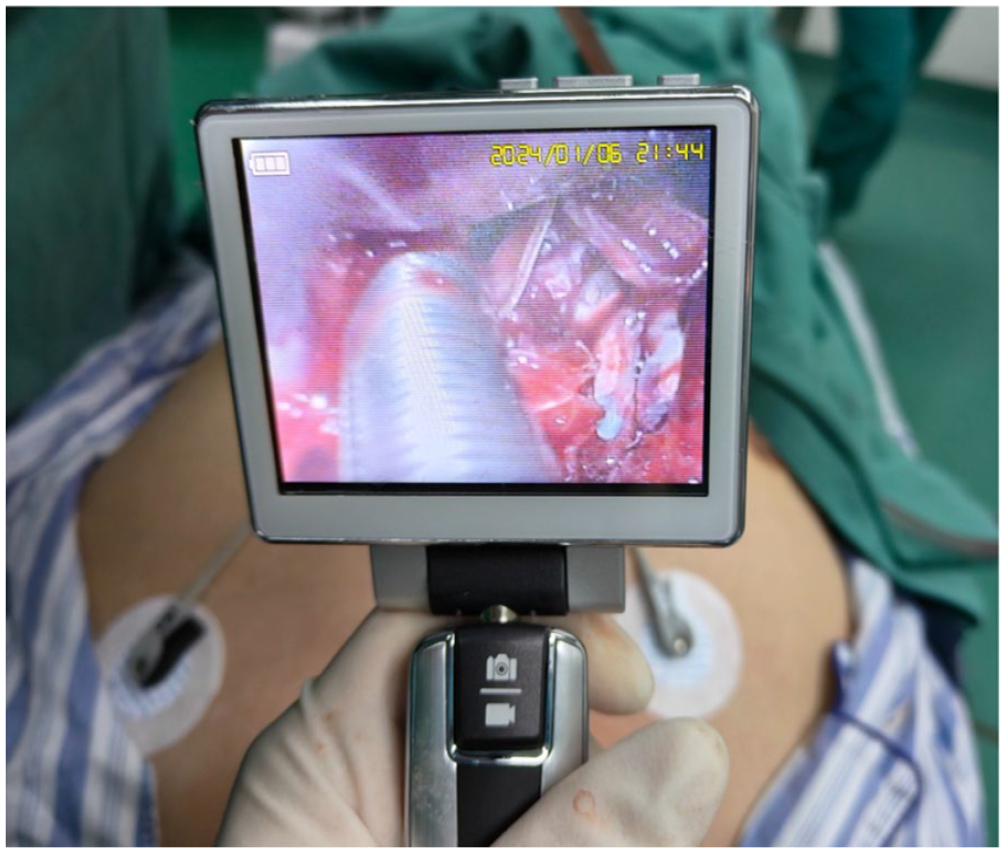
After gently pulling away the tail of the mantis shrimp, awake tracheal intubation was successfully completed.
After successful anesthesia, the surgeon used a self-retaining laryngoscope, lifted the epiglottis, and exposed the laryngeal vestibule and the postcricoid region, where mantis shrimp was seen blocking the entrance to the esophagus and obscuring the glottis. After carefully removing the mantis shrimp in segments, it was observed that the posterior pharyngeal wall was significantly injured with a small amount of blood oozing. Electrocoagulation was applied to stop the bleeding, and a detailed examination was again performed, which revealed no significant bleeding except swelling of the mucosa in the postcricoid region of the hypopharynx and at the entrance of the esophagus.
The segments of the mantis shrimp that were removed were pieced together. It is necessary to confirm the integrity of the segmented mantis shrimp, as its red shell has a good concealment function in bloody secretions of the throat. It could be seen that its length exceeded 20 cm and that the shell was covered with barbs (as shown in Figure 3).
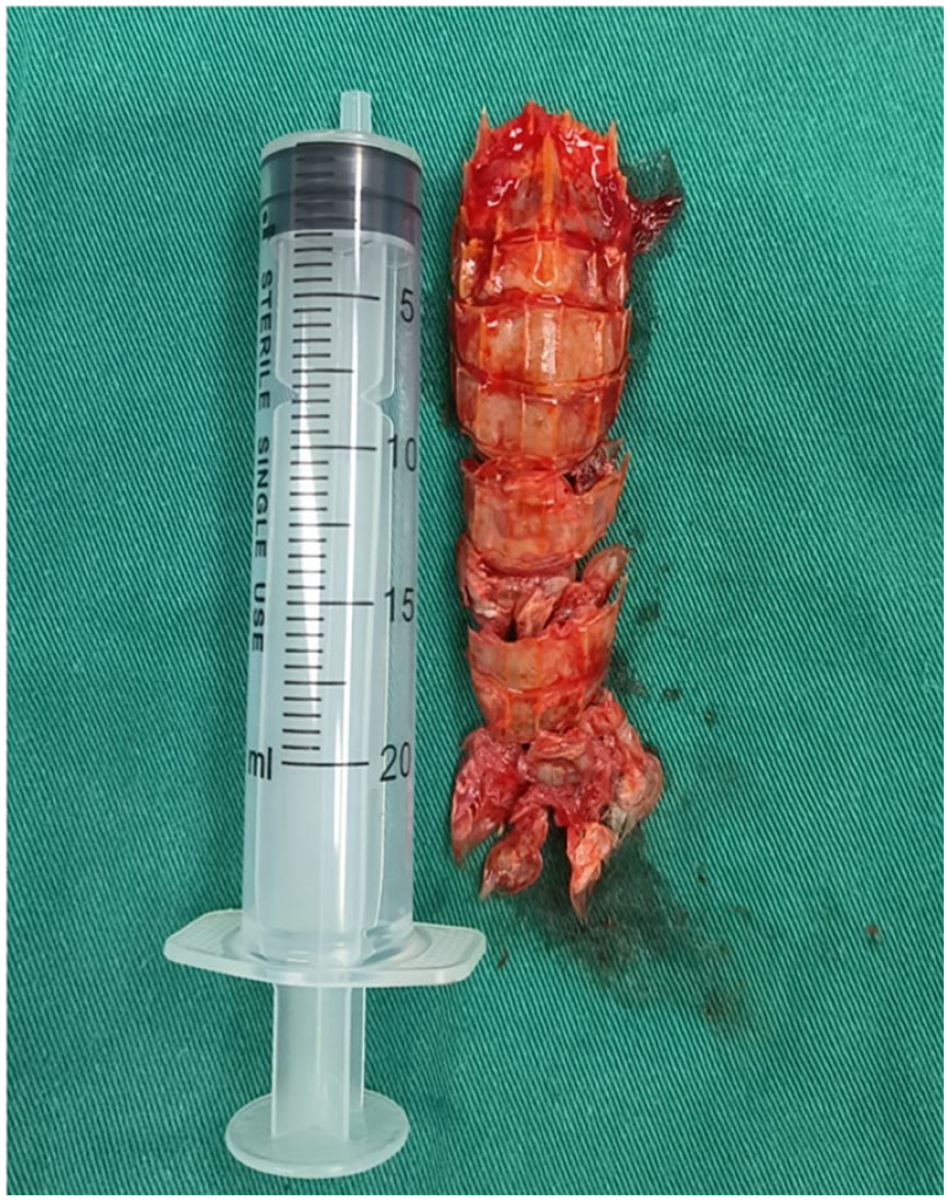
Complete mantis shrimp after splicing, with a length exceeding 20 cm.
Taking into account the patient’s severe pharyngeal injury and the large amounts of bloody secretions swallowed before surgery, a nasogastric tube was placed intraoperatively for gastrointestinal decompression. Since the patient had not fasted before undergoing general anesthesia, he was transferred to the intensive care unit for close observation after surgery. As an esophagography was performed the following day, there were no signs of esophageal perforation. On the sixth day after surgery, when the patient came to the outpatient clinic for follow-up, the laryngoscopy did not reveal any specific signs of the larynx and pharynx.
Discussion
FB ingestion can be divided into nonfood ingestion and food bolus impaction. In normal adults, most cases of FB ingestion belong to food bolus impaction, which is usually accidental. The most common esophageal FBs are animal bones, toothpicks, and fish bones. 5 It is ideal to remove esophageal FB within 24 hours. For patients with sharp objects, button batteries, and complete obstruction, emergency examination and removal should be performed in 2 to 6 hours, 6 because complications can arise more frequently afterward, such as esophageal perforation, obstruction, and ulcers. 7
Radiographic identification plays a crucial role in the diagnosis of esophageal FB, especially in the recognition of FB embedded in soft tissue. 8 However, for patients with clear principal complaints, accompanied by obvious pain, FB sensation, and respiratory distress symptoms, radiographic identification is not mandatory and emergency endoscopic examinations should not be delayed. In cases where the properties and location of the FB can be seen and determined by endoscopy, emergency surgery should first be performed to remove the FB, followed by relevant radiographic identification to help determine the occurrence of complications such as esophageal perforation.
Most adults can provide reliable information about FB, 9 including what was swallowed, when it was swallowed, what are the current symptoms, and so on. Physicians must integrate this information with the findings of the physical examination and any additional diagnostic tests necessary, such as esophagoscopy, to evaluate the presence, location, and size of FB. 10 In our case, the patient exhibited obvious symptoms of esophageal FB, including obvious sore throat, marked dysphagia, and drooling. But more important, the patient showed symptoms of difficulty breathing, which led emergency physicians to first suspect that it was FB in the trachea. After combining the information provided by a friend who came with the patient that the FB was a whole mantis shrimp, the emergency doctor first decided to perform an electronic laryngoscopy to determine the approximate condition of the FB. Electronic laryngoscopy examination found that a FB obstructs the entrance to the esophagus. Due to the long shape of the mantis shrimp, it also blocked the glottis, causing difficulty breathing for the patient. The problem is that there are barbs on the shell of mantis shrimp and attempting to remove them directly can cause serious damage to the esophageal and pharyngeal mucosa. Therefore, we extracted the mantis shrimp in segments under general anesthesia and applied electrocoagulation to stop bleeding of the damaged pharyngeal mucosa. And pieced together, the mantis shrimp fragments to ensure that there was no residue. The esophageal angiography performed the next day revealed no esophageal perforation nor did any other complications occur.
To our knowledge, this is the first reported case of esophageal FB caused by swallowing a whole mantis shrimp, accompanied by symptoms of respiratory distress, which is different from most cases of esophageal FBs that do not present with respiratory difficulties. The situation is very urgent. Therefore, it is imperative to immediately assess and remove the FB lodged in the esophagus. This tests the doctor’s calm personality and superb surgical skills in the face of danger and motivates them to always remain calm, but quickly handle problems.
Footnotes
Data Availability
The image data used to support the findings of this study are included within the article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics Approval
The studies involving human participants were reviewed and approved by the ethics committee of The Second Affiliated Hospital of Xiamen Medical College.
Informed Consent
Written informed consent was obtained from the patient for the publication of this case report.
