Abstract
Objective:
The objective of this study was to evaluate the graft success rate and hearing outcome of modified cartilage inlay graft technique for repairing large perforations under local anesthesia.
Study Design:
Prospective case series.
Methods and Materials:
We performed a prospective study in 31 patients with large perforations who underwent endoscopic local anesthesia-based modified cartilage inlay graft technique with no raising of the squamous epithelium and no rimming of the perforation margins. The graft outcomes and complications were evaluated at 6 and 24 months postoperatively.
Results:
Thirty-one patients (31 ears) were included in this study. The mean operation time was 42.3 ± 2.6 (ranged 36-51) minutes. The visual analog scale pain scores at intraoperative and 2 and 48 hours postoperatively were, respectively, 2.6 ± 0.6, 1.4 ± 0.2, and 0.6 ± 0.1. The graft success rate was 100.0% (31/31) at 6 months after surgery. However, only 25 (80.6%, 25/31) patients completed a 2-year follow-up and performed a temporal bone CT examination; re-perforation was seen in 2 patients, the graft success rate was 92.0% (23/25). CT revealed the well-developed pneumatization of the mastoids and middle ear in all the patients. Nevertheless, 1 (1/25, 8.0%) patient developed a graft epithelial inclusion cyst, which was removed by endoscope in the outpatient setting. The mean preoperative air bone gap (ABG) was 23.1 ± 4.3 dB, while the mean postoperative ABG after 6 months was 14.9 ± 2.6 dB; the difference between these values was significant (P < .05; Wilcoxon’s signed-rank test), and the functional success rate was 93.5% (29/31).
Conclusion:
Endoscopic modified cartilage “inlay” graft technique with no raising the squamous epithelium and no rimming the perforation is a minimally invasive technique with a short operative time and satisfying success rate for closure of large perforations under local anesthesia.
Introduction
An inpatient myringoplasty under general anesthesia remains the current gold standard of care for repairing chronic tympanic membrane (TM) perforations, especially for large perforations,1,2 which results in high medical costs and anesthesia risks. Thus, local anesthesia-based myringoplasty has been recommended by some scholars,1-3 which was defined as a transcanal procedure performed without sedation or general anesthesia and without creating a tympanomeatal flap.1-3 In the past, indications for local anesthesia-based myringoplasty were mainly small perforations, and the graft materials were platelet-rich plasma 4 and hyaluronic acid. 2 However, these materials were not readily available and expensive.2,4 Although underlay or bivalve cartilage inlay techniques were used in outpatient myringoplasty to repair small and medium perforations, these techniques had limitations, which required the removal of perforation margins and creating the groove of cartilage;5,6 the procedures undoubtedly increased the pain. We considered that local anesthesia-based myringoplasty should have no or minimal intraoperative pain, a short operation time, and be well tolerated during wakefulness. However, the middle ear is most sensitive to pain but least effective for local anesthetics. How to reduce the operating steps is vital for office-based myringoplasty. To date, no reports have been reported about local anesthesia-based myringoplasty for repairing large perforations because large perforations require the removal of more perforation margins and a high risk of graft failure.
Recently, we reported the perichondrium-cartilage double graft technique with no removal of the superficial layer, which did not increase the iatrogenic cholesteatoma and epithelial pearl in long-term follow-up.7,8 In addition, we performed underlay technique with preserving perforation margins and obtained similar graft outcome with excising perforation margins. 9 No removal of superficial layer and perforation margins reduced the local pain of patients during wakefulness. Based on previous studies, we performed a modified cartilage inlay graft technique with no raising of the tympanomeatal flap and squamous epithelium and no rimming of the perforation. The objective of this study was to evaluate the graft success rate and hearing outcome of this technique for repairing large perforations under local anesthesia.
Materials and Methods
Ethical Considerations
The study protocol was reviewed and approved by the Institutional Ethical Review Board of Yiwu Central Hospital. Informed consent was obtained from all participants.
Methods
This was a prospective case series study performed between May 2020 and November 2020. The inclusion criteria were age >18 years with chronic large perforation occupying 2 quadrants of TM; at least 1 mm of remnant TM around the margin, which is not involved in the ossicular chain; dry ear for at least 3 months; an air bone gap (ABG) < 30 dB; and good pneumatization of the middle ear and mastoid region, as shown by temporal bone high-resolution computed tomography (HRCT). Prior to enrollment, HRCT was performed, and audiograms were recorded in all patients. The exclusion criteria were a marginal, subtotal, or total perforation; revision cases; cholesteatoma; visible ossicular chain abnormality; and fungal otitis externa. Dry ear was assessed based on patient history, but the assessment did not include ear monitoring for 3 months after enrollment per the study design.
The pure-tone average was calculated as the mean of behavioral thresholds at 500, 1000, 2000, and 3000 Hz. The ABG was determined as the mean of the differences between air conduction thresholds and bone conduction thresholds at 500, 1000, 2000, and 3000 Hz, both preoperatively and at 6 months postoperatively. For convenience, the ABGs in bins were grouped as follows: 0–10 dB, 11–20 dB, 21–30 dB, and >30 dB. The operative time was defined as the duration from the beginning of local anesthetic injection to the completion of the perichondrium-cartilage graft placement. Pain intensity was measured and recorded. All patients were asked to score their pain on a visual analog scale (VAS), comprising a 10-cm line with scores ranging from 1 (no pain) to 10 (severe pain), at intraoperatively and 2 and 48 hours postoperatively. In addition, only the deep pain of the ear reported by the patients was considered ear pain and scored the VAS scores, while the pain of the tragus area was not scored.
Surgical Technique
All patients underwent over-underlay myringoplasty under local anesthesia by a single surgeon in the operating room of the outpatient department. Patients were placed in a supine position with their head turned so that the ear with the perforation was up. A 0° endoscope with 4-mm diameter and 18 cm was used during the operation and a high-definition monitor. The patient’s ear was prepped with betadine and the periaural area and the ear canal are injected with 2 mL of 1% lidocaine with 1:100,000 epinephrine. Transcanal injections (1 cc) were administered in all 4 quadrants by using a 20-gage needle under direct endoscopic vision. Meanwhile, blanching of the canal skin was observed, and hemorrhagic bulbs were prevented by slowly and carefully injecting local anesthesia. The external auditory canal (EAC) and surface of TM were packed using small piece of gauze soaked with 2% lidocaine with 1:100,000 epinephrine for 10 minutes to ensure the blanching of TM. The painkillers of indomethacin enteric-coated tablets or acetaminophen were given to the patients during the surgery or after the surgery if the mild pain could not be tolerated by the patient.
A tragal cartilage with single side-perichondrium is harvested from the ipsilateral tragus. The lateral perichondrium was circumferentially elevated, but the pedicle attached the cartilage graft. The cartilage is fashioned to make it at least 1 mm larger than the circumferential margins, while the lateral perichondrium graft is also trimmed to make it wider than the cartilage graft.
The removal of the superficial layer and perforation margins were not performed and the myringosclerosis of TM remnant was reserved, while the mucosa underneath and around the perforation margins will be gently curetted to form minor bleeding. The tympanic cavity was slightly filled using a few biodegradable synthetic polyurethane foams through the perforation. The cartilage graft is placed trans-perforationally medial to the TM remnant, and the lateral perichondrium is placed on the superficial layer of the TM. The packing of EAC was not performed. The cartilaginous of EAC was packed with erythromycin ointment gauze, up to the tragus incision (Figure 1).
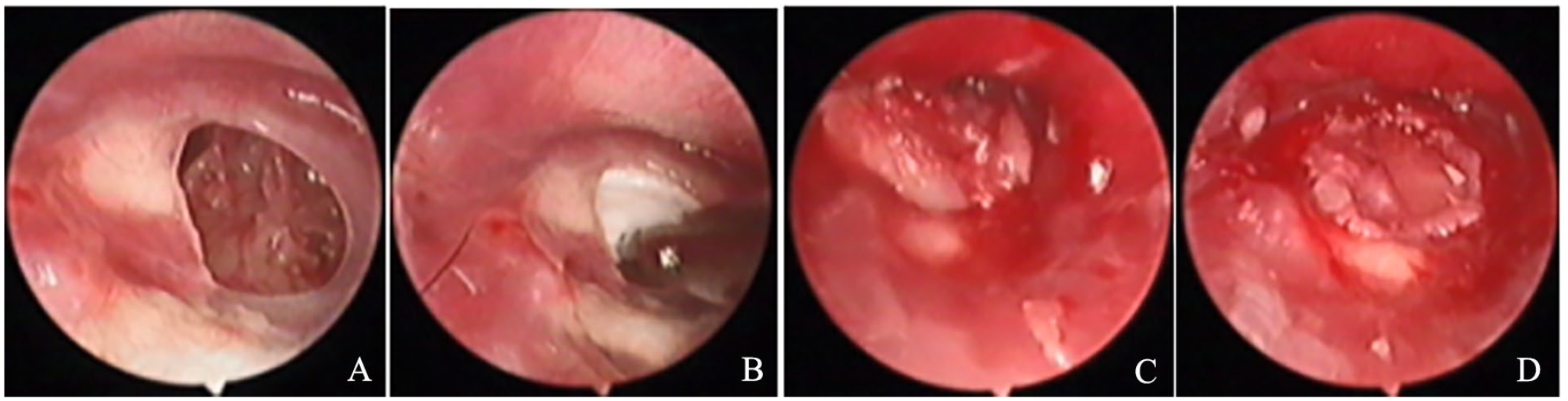
Preoperative perforation (A), middle ear packing (B), the cartilage-perichondrium graft was placed trans-perforationally (C), the cartilage medially to the TM remnant and the perichondrium laterally to the superficial layer of TM remnant (D).
Postoperative Follow-Up
All patients received a course of antibiotics (amoxicillin) after the surgery. Patients were discharged 2 hours after surgery. All patients were scheduled by endoscope for regular follow-up visits at 48 hours, 2 weeksand 4 weeks postoperatively, as well as at 3, 6, and 24 months postoperatively. Audiological testing was performed 6 months after surgery. In addition, the loss follow-up rate was evaluated at postoperative 24 months and postoperative HRCT was performed at last follow-up to evaluate the pneumatization of mastoids and middle ear. Graft success was defined as the presence of an intact graft; graft failure was defined as the presence of residual or re-perforation after surgery. Functional success was defined as an ABG ≤ 20 dB.
Statistical Analysis
Statistical analyses were performed using SPSS Statistics, version 20 (IBM Corp, Armonk, NY, USA). Data are expressed as means (standard deviations) and numbers (percentages). Differences between preoperative and postoperative ABGs were analyzed using the Wilcoxon signed-rank test. Differences with P < .05 were considered statistically significant.
Results
Thirty-one patients (31 ears) were included in this study. Of the 31 patients, 18 (58.1%) were female and 13 (41.9%) were male (mean age at surgery, 44.6 ± 2.7 years; range, 41-69 years), the duration of perforations was 20.4 ± 3.2 years. Left perforation was in 17 (54.8%) patients and right in 14 (45.2%) patients. The mean operation time was 42.3 ± 2.6 (ranged 36-51) minutes. The VAS pain scores at intraoperative and 2 and 48 hours postoperatively were, respectively, 2.6 ± 0.6, 1.4 ± 0.2, and 0.6 ± 0.1. Only 22.6% (7/31) patients accepted the painkillers during the surgery or after the surgery.
Graft Success Rate
Endoscopic observation showed abundant red blood vessels on the surfaces of the graft at postoperative 2 weeks and the complete survival of the graft at postoperative 4 weeks.The graft success rate was 100.0% (31/31) at postoperative 6 months (Figure 2). No residual perforation was seen.
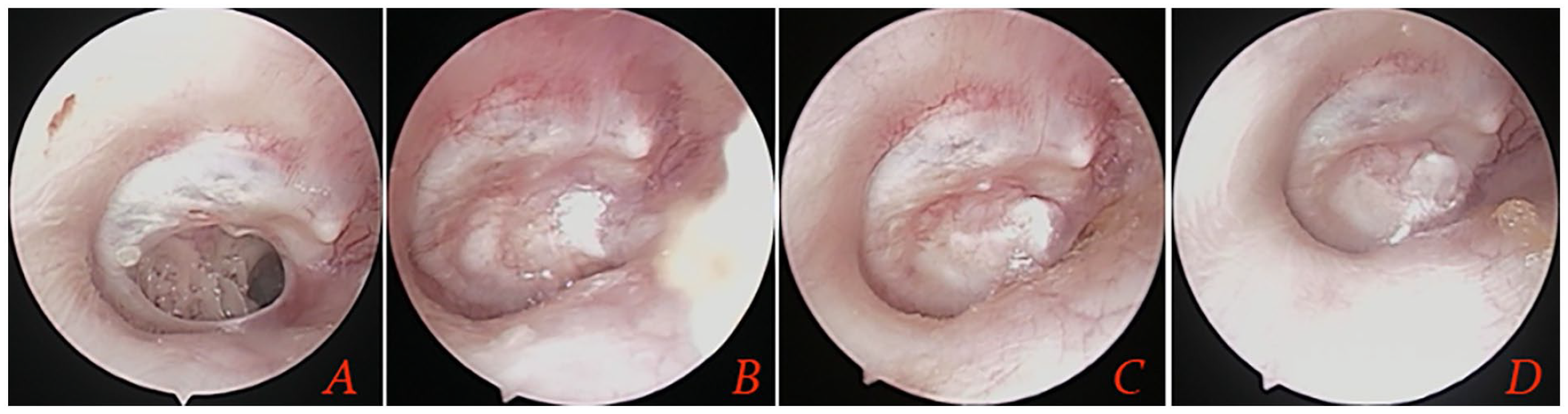
Preoperative perforation (A), 4 weeks after surgery (B), 8 weeks after surgery (C), and 12 months (D).
The loss follow-up rate was 19.4% (6/25) at postoperative 2 years. A total of 25 (80.6%, 25/31) patients completed 2 years of follow-up and performed temporal bone CT examination; the mean follow-up time was 25.1 ± 1.8 months (range 24-29 months). Re-perforations were seen in 2 patients, the graft success rate was 92.0% (23/25). CT revealed the well pneumatization of the mastoids and middle ear in all 25 patients. However, 1 (1/25, 4.0%) patient developed a graft epithelial inclusion cyst, which was removed by endoscope in the outpatient setting.
Hearing Outcome
Audiological testing was achieved in 31 patients at 6 months postoperatively, which showed that there is no sensorineural threshold shift. The mean preoperative ABG was 23.1 ± 4.3 dB, while the mean postoperative ABG after 6 months was 14.9 ± 2.6 dB; the difference between these values was significant (P < .05; Wilcoxon’s signed-rank test). For the individual ABG closure percentages, 67.7% (21/31) had ABG closure within 10 dB, 25.8% (8/31) had an ABG of >10 and <20 dB, and 6.5% (2/31) had an ABG closure more than 20 dB. The functional success rate was 93.5% (29/31). No graft-related complications (e.g., graft lateralization, significant blunting, graft medialization) were encountered during the follow-up period. None of the patients reported sensorineural hearing loss or intractable tinnitus.
Discussion
Some scholars have been increasingly interested in local anesthesia for myringoplasty,1-6 which significantly reduces the medical costs, especially in developing countries. We believed that local anesthesia-based myringoplasty should have the following advantages: a short operation time, be well tolerating for local anesthesia, low cost, simple, and similar graft outcome with inpatient myringoplasty under general anesthesia. Previous local anesthesia-based myringoplasty was mainly limited to small-medium perforations,1-6 because the underlay technique was commonly used for the local anesthesia-based myringoplasty; larger perforations had a low graft success rate but required the overlay or over-underlay technique. The overlay or over-underlay technique involves raising the tympanomeatal flap and removing of the squamous epithelium, with the graft placed laterally on the fibrous layer of the TM remnant.10,11 These procedures increased the pain and are not suitable for local anesthesia-based surgery. We created local anesthesia-based modified cartilage “inlay” graft myringoplasty with no raising of the tympanomeatal flap and the squamous epithelium, no rimming of the perforation, and no packing of EAC, and applied this technique to repair large perforation for the first time. Compared with our previous technique, 7 the tissue of the perforation margins was not removed, and the perforation margin was not freshened in this study, but our previous study did. The removal of perforation margins increased the size of perforation and resulted in the absence of TM remnant in few areas. On the contrary, the preserving perforation margins increased the contact area of graft and TM remnant and reduced the residual perforation and thereby improved the graft success rate.
In this study, modified cartilage “inlay” graft myringoplasty reached a graft success rate of 100.0% at 6 months and 92.0% at 24 months under local anesthesia, which was comparable to the success rate using the inpatient over-underlay technique by other scholars.10,11 Babu et al. 10 reported the success rate of 84% (71/84) and 94.9% by Yigit et al. 11 Recently, Bao et al. 12 obtained a success rate of 96% and believed that the over-under technique is effective for repairing larger perforations or those with anterior extension. Zhang et al. 13 compared the graft success rate of over-underlay and medial technique and found over-under tympanoplasty is more suitable for large perforation. This technique is also superior to the success rate using other graft technique. Bedri et al. 14 reported the success rate of 90% using Double-Layer graft, 91% using lateral tympanoplasty by Angeli et al., 15 91% using butterfly technique, and 88% in the cartilage technique. 16 Nicholas Jungbauer et al. 17 reported the success rate of 85.3% for perforations greater than 50% in a systematic review. Kaleva et al. 18 performed the meta-analysis and showed no significant difference in the total closure rate of myringoplasty under general and local anesthesia (87% vs 91%).
Intraoperative pain intensity is the key to successfully complete myringoplasty in an office setting. Toulouie et al. 19 performed a systematic review and meta-analysis to compare postoperative pain after endoscopic versus microscopic otologic surgery and found that endoscopic ear surgery results in significantly less postoperative pain when compared with microscopic ear surgery.
In this study, the intraoperative pain scores were 2.6 ± 0.6, all the patients tolerated the procedures well, while the postoperative pain scores were 1.4 ± 0.2 and 0.6 ± 0.1 at 2 and 48 hours postoperatively, respectively, which resulted in significantly less postoperative pain compared with other myringoplasty.20,21 Chen et al. 20 reported that the pain score was 1.9 at postoperative day 3 using push-through technique. Similarly, Atchariyasathian et al. 21 reported 5.0 and 1.4 at postoperative 4 and 48 hours. Although raising of the tympanomeatal flap was not performed in their studies, rimming of the perforation, removal of thick sclerotic plaques, and EAC packing were applied. Our pain score at postoperative 4 hours was less than that of the overlay technique by Plodpai 22 who reported 3 of the pain score. The procedures for sensitizing to pain, including raising the tympanomeatal flap, rimming the perforation, and removal of squamous epithelium, had been neglected in this study; no EAC packing was applied. Aydil et al. 23 compared pain and safety in otologic procedures under local anesthesia, and myringoplasty was found to be less painful.
The short operation time is also crucial during wakefulness. The mean operation time was 42.3 ± 2.6 minutes in this study, which was shorter compared with the endoscopic transtympanic technique with no raising of the tympanomeatal flap by other scholars,20,21 who reported a mean operation time of 50 minutes 20 and 60 ± 17 minutes, respectively. 21 Plodpai 22 reported that the mean operating time was 101.6 minutes using overlay technique. Also, Saraf et al. 24 reported the mean operation time was longer in overlay than underlay techniques; this was due to raising the tympanomeatal flap and removal of squamous epithelium in overlay technique but not in underlay techniques. Atchariyasathian et al. 21 believed that adequate hemostasis is important in endoscopic ear surgery since bleeding may lead to an obscured surgical view through the blood smeared lens of the endoscope, thereby prolong the operation time. In previous study, raising the tympanomeatal flap, rimming the perforation, and removal of squamous epithelium were performed,20-23 but this technique only involved middle ear packing and graft placement, and thus does not cause substantial bleeding, which is obviously beneficial for office-based myringoplasty.
Compared with myringoplasty under general anesthesia, myringoplasty under local anesthesia significantly lowers medical costs. Kaleva et al. 18 analyzed that although general and local anesthesia had similar graft outcomes, local anesthetic surgery may minimize anesthetic risks, reduce costs, and reduce environmental impacts. In addition, no packing of EAC was beneficial to endoscopic observation and correcting the graft mismatch in the early stage, although it did not occur in this study. No packing of EAC has been widely used by some scholars; they did not report the graft lateralization and extrusion. 25
Similar to previous studies,5-9 this study showed that postoperative ABG had significant improvement compared with preoperative ABG. Usually, improvement of postoperative ABG is incontrovertible only if the procedure does not injure the middle ear structure and ossicular chain for the patients with no abnormal ossicular chain. The major concern for using the present technique where the graft is set over intact epithelium surrounding a perforation edge is the development of an intratympanic iatrogenic cholesteatoma/epithelial inclusion cyst. Previous views believed that the scar tissue of perforation margins and the squamous epithelium may induce the iatrogenic cholesteatoma.26,27 But, iatrogenic cholesteatomas and epithelial pearls can occur even in edges and squamous epitheliums that have been removed.14,15,28 On the contrary, previous studies found that the lateral perichondrium became necrosis and crust but didn’t develop the long-term iatrogenic cholesteatoma.7,8 In this study, 80.6% patients completed 2 years of follow-up and performed HRCT examination, which revealed well pneumatization of the mastoids and the middle ear. Although 4.0% patients developed a graft epithelial inclusion cyst, it could be simply removed by endoscope in the outpatient setting. It follows that worry about the development of an iatrogenic cholesteatoma is unnecessary for a modified cartilage “inlay” graft. Thus, we defined local anesthesia-based myringoplasty as a transcanal procedure performed without a sedation or general anesthesia and without creating a tympanomeatal flap, removing the squamous epithelium, rimming the perforation, packing of EAC with or without packing of the middle ear, being well tolerated, and reaching similar graft outcomes as inpatient myringoplasty. The drawback of this study was small sample size, short follow-up, and the absence of control group. Theoretically, it is not sufficient for 2 years of follow-up postoperatively for the assessment of middle ear cholesteatoma. Thus, long-term follow-up of large sample should be encouraged in future.
Conclusion
Endoscopic modified cartilage “inlay” graft technique with no raising of the squamous epithelium and no rimming of the perforation is a minimally invasive technique and has short operative time and satisfying success rate for closure of large perforations under local anesthesia.
Footnotes
Author’s Contributions
Meixia Wu: Interpretation of data for the work, design of the work, analysis of data for the work, drafting the work, agreement to be accountable for all aspects of the work, final approval of the version to be published; Zhengcai Lou: Interpretation of data for the work, design of the work, final approval of the version to be published.
Data Availability Statement
All data generated or analyzed during this study are included in the published article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by Health Commission of Zhejiang province, China (Grants#2021KY1186), Technology Agency of Jinhua city, China (Grants#2022-3-042).
