Abstract
Keywords
Introduction
Tinnitus, the perception of a sound without an external auditory stimulus, 1 affects over 740 million adults worldwide, with 120 million people considering it a significant problem. 2 Tinnitus can also become chronic, 3 leading to an enormous burden on both the patient and the healthcare system. 4 The severity of tinnitus is closely associated with anxiety, depression, and a decline in the quality of life,5-7 highlighting the urgent need for accurate diagnosis.
Given the high prevalence of tinnitus, previous studies have shown that various factors, including gender, tinnitus loudness, and hearing loss, are associated with subjective tinnitus severity.8,9 Chen et al. 8 claimed that sleep status, anxiety levels, and changes in loudness in patients with chronic tinnitus are also significantly correlated with the severity tinnitus. There is evidence that the pathophysiology of tinnitus involves damage not only to peripheral and/or central auditory pathways but also to other brain networks. 10
Traditional methods (the use of questionnaires) for assessing tinnitus severity rely mainly on subjective judgments by doctors and results of hearing tests, which have some subjectivity and limitations. In recent years, with the development of machine learning and statistical methods, predictive models of tinnitus severity based on multiple factors have also been widely studied and applied. The nomogram is a visual tool based on statistical methods that can predict the tinnitus severity in patients by considering multiple factors.
A nomogram is an intuitive graphic prediction tool that simplifies complex regression equations into visual graphs, 11 allowing the integration of individualized risk factors and showing the numerical relationships between specific diseases and their risk factors. In this study, we use a nomogram to individually predict the severity of unilateral subjective tinnitus in patients and precisely identify individualized influencing factors. This predictive nomogram can help assess patient risk and facilitate clinical decision-making for planning personalized treatment.
Materials and Methods
Participants
We retrospectively collected clinical data of patients attending our outpatient clinic between January 2021 and June 2022 at Air Force Medical Center (Beijing, China). Patients were included in the study if they had “tinnitus” as the first complaint, unilateral subjective tinnitus, with or without hearing loss. Patients were excluded if they had treated tinnitus; bilateral subjective tinnitus; objective tinnitus or pulsatile tinnitus; tinnitus caused by otitis media and other secondary tinnitus (Ménière’s disease, acoustic neuroma); the state of anxiety and/or depression or history of depression or anxiety disorders; a combination of chronic serious systemic diseases; insomnia; chronic alcohol drinkers and smokers; or incapability to complete the scale or examination.
Based on the 2007 World Health Organization’s age group classification criteria, subjects included were classified into the youth group (<45 years), middle-aged group (45-59 years), and older group (≥60 years).
Clinical data were collected from medical records, including age, gender, tinnitus location (left or right), onset time, loudness and frequency of tinnitus, circumstances of worsening tinnitus (obvious in quiet environments or obvious in noisy environments), tinnitus severity, and hearing and otoscopic examinations. Tinnitus multielement integration sound therapy (T-MIST) platform was used to estimate loudness and frequency of tinnitus. Pure-tone audiometry (PTA) was used to assess hearing. Based on onset time, subjective tinnitus was classified as acute tinnitus (lasting <3 months), subacute tinnitus (lasting 3-6 months), and chronic tinnitus (lasting ≥6 months). 12
Pure-Tone Audiometry
The tests were conducted in a standard septal room within the department of otolaryngology head and neck surgery at the Air Force Medical Center. We used an ergometrics otometrics flex 100 sonotrope for tympanogram testing and an aurical pure-tone audiometer for air and bone conduction hearing threshold tests. The test equipment was calibrated by the general medical acoustical metrology and testing station of the Chinese People’s Liberation Army. Otoscopy and tympanometry were performed before audiometry to check the middle ear status of all participants. The assessment of hearing function was carried out using conventional PTA by study-certified audiologists, with hearing threshold measured at frequencies between 125 and 8 kHz. Normal hearing was defined as a hearing threshold less than or equal to 25 dB at any frequency in this range. Hearing loss in the tinnitus ear was defined as a threshold of 25 dB at any frequency between 125 and 8 kHz, characterized as mild for a PTA average of 26 to 40 dB and moderate for a PTA average of 41 dB or more.
Tinnitus Loudness and Pitch Matching
Tinnitus matching via the tinnitus platform test (T-MIST). A fine test with 1/24th of the tinnitus range is added to the traditional octave test. Using an acoustic stimulation interval of 0.3 ms, a pure tone of 5 dB higher than the threshold is emitted for 1.5 to 2.0 s in the range of 1/24 octave, allowing the patient to find the best-matched center frequency of their tinnitus sensation. Then, subsequent pure tons were presented in neighboring loudness of the threshold and frequency until a match was identified to determine the tinnitus’s exact pitch (frequency) and loudness. Classification of tinnitus frequency is based on <500 Hz, 500 to 3000 Hz, and >3000 Hz. The cutoff loudness of tinnitus was defined as 40 dB.
Tinnitus Handicap Inventory
The severity of unilateral subjective tinnitus was assessed by the tinnitus handicap inventory (THI), 13 which is the most commonly used self-rating scale for tinnitus. 13 The THI questionnaire consists of 25 items, which are further divided into the subscales of functional, emotional, and catastrophic. The total score of the questionnaire is 100. The Chinese version of the THI has been validated. A Chinese version of THI was completed in all patients, as described before. 14 All the patients with subjective tinnitus were divided into mild and severe groups according to THI scores, with a cutoff value of 38. 15
Construction and Validation of Nomogram
Patients were randomized according to a 7:3 ratio into the training cohort (104 patients) and the validation cohort (42 patients). In the training cohort, LASSO and binary logistic regression analysis mixed-effects models were employed to identify independent prognostic risk factors for unilateral subjective tinnitus. Based on the identified risk factors, generate a nomogram to predict the severity of unilateral subjective tinnitus.
The performance evaluation of the nomogram included discrimination. Internal verification was done using the bootstrapping method with 1000 resamplings. Internal verification was used to evaluate the performance of the model. The discriminative ability was measured by the concordance index (C-indices) and the area under the curve (AUC) of the receiver operating characteristic (ROC) curves.
This retrospective study was conducted in compliance with the principles of the Declaration of Helsinki and was approved by the Air Force Medical Center. Since the study did not involve exposing patients’ privacy and all procedures were part of routine care, the hospital ethics committee waived the requirement for written informed consent. The transparent reporting of a multivariable prediction model for individual prognosis or diagnosis (TRIPOD) statement was used as a reporting guideline for the model. 16
Statistical Analysis
All statistical analyses were conducted using R software version 3.6.1 (R Foundation for Statistical Computing, Vienna, Austria), with a significance level of
Results
Population Baseline Characteristics and Clinical Results
Among the 146 patients with unilateral subjective tinnitus included in the study (Figure 1), the average age was 45 years (SD = 17). Of these patients, 74 (50.7%) were male and 72 (49.3%) were female (Table 1). In terms of tinnitus duration, 96 (65.75%) had acute tinnitus, 13 (8.9%) had subacute tinnitus, and 37 (25.35%) had chronic tinnitus. Regarding tinnitus loudness, 74 (50.68%) had a loudness <40 dB, while 72 (49.32%) had a loudness ≥40 dB. Based on the THI score, 76 (52.05%) patients fell into the mild tinnitus group and 70 (47.95%) patients were classified as having severe tinnitus. In terms of hearing, average hearing is in the same ear with unilateral tinnitus at 31 dB, 77 (52.73%) patients had normal hearing, 30 (20.54%) had mild hearing loss, and 39 (26.73%) had moderate hearing loss. Table 1 provides a summary of the baseline characteristics of the patients.
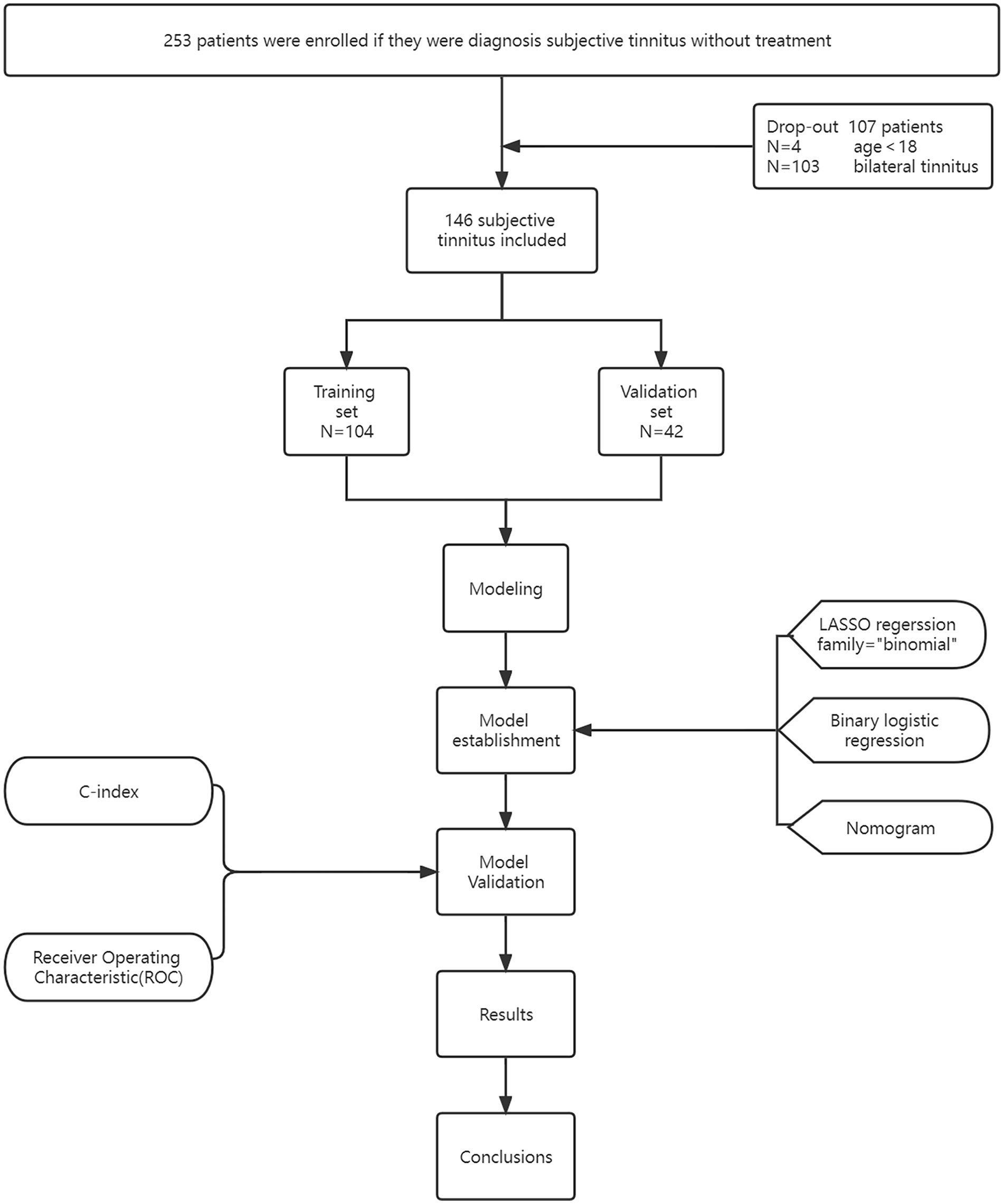
Study design flow chat.
Demographic Characteristics of the Training Cohort and Validation Cohort.
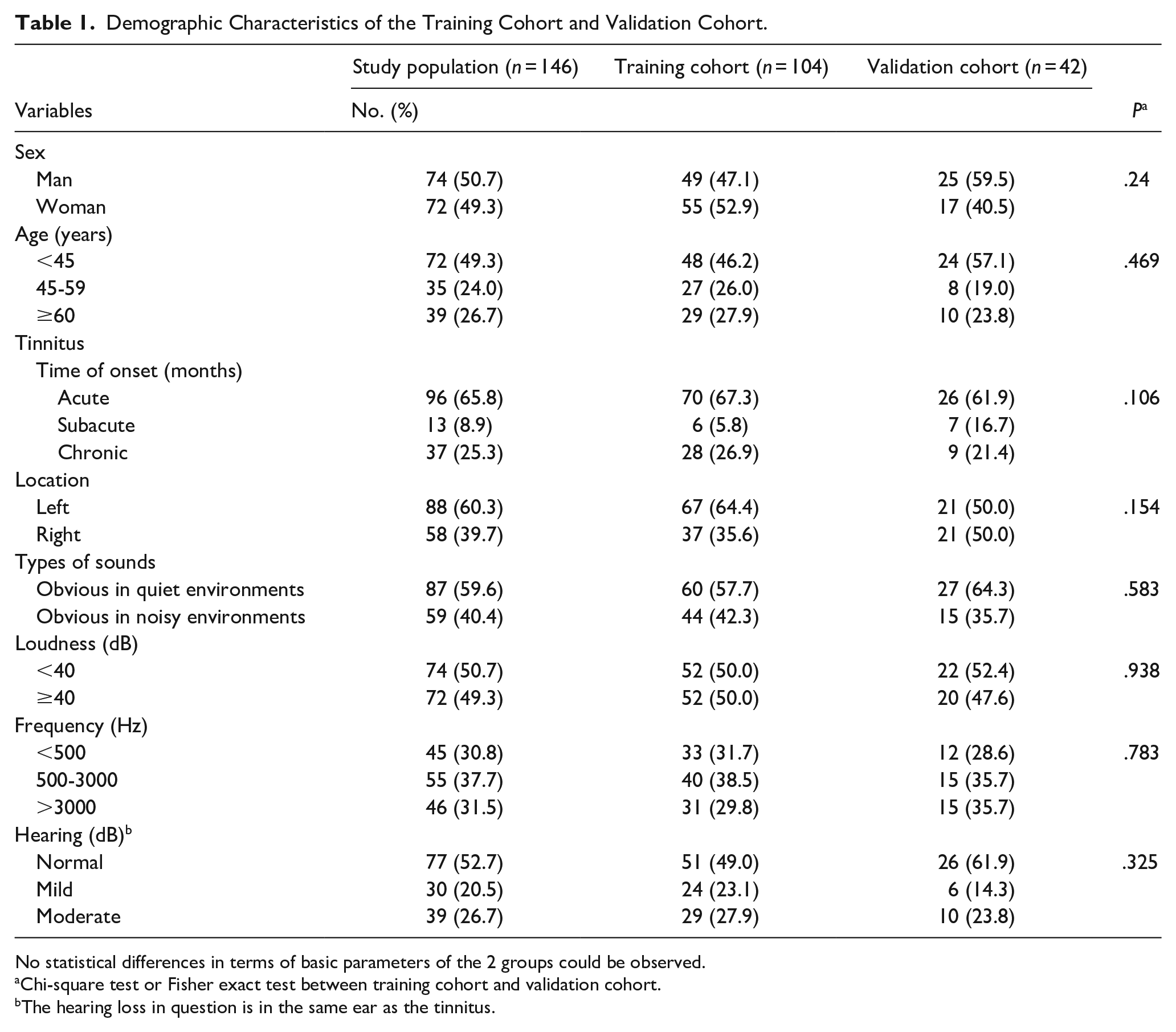
No statistical differences in terms of basic parameters of the 2 groups could be observed.
Chi-square test or Fisher exact test between training cohort and validation cohort.
The hearing loss in question is in the same ear as the tinnitus.
Development of the Nomogram
Based on 104 patients in the training cohort, by selecting features with nonzero coefficients in the LASSO regression model, 3 candidate variables were associated with the severity of unilateral subjective tinnitus, including sex, tinnitus loudness, and hearing loss (Figure 2A and B).
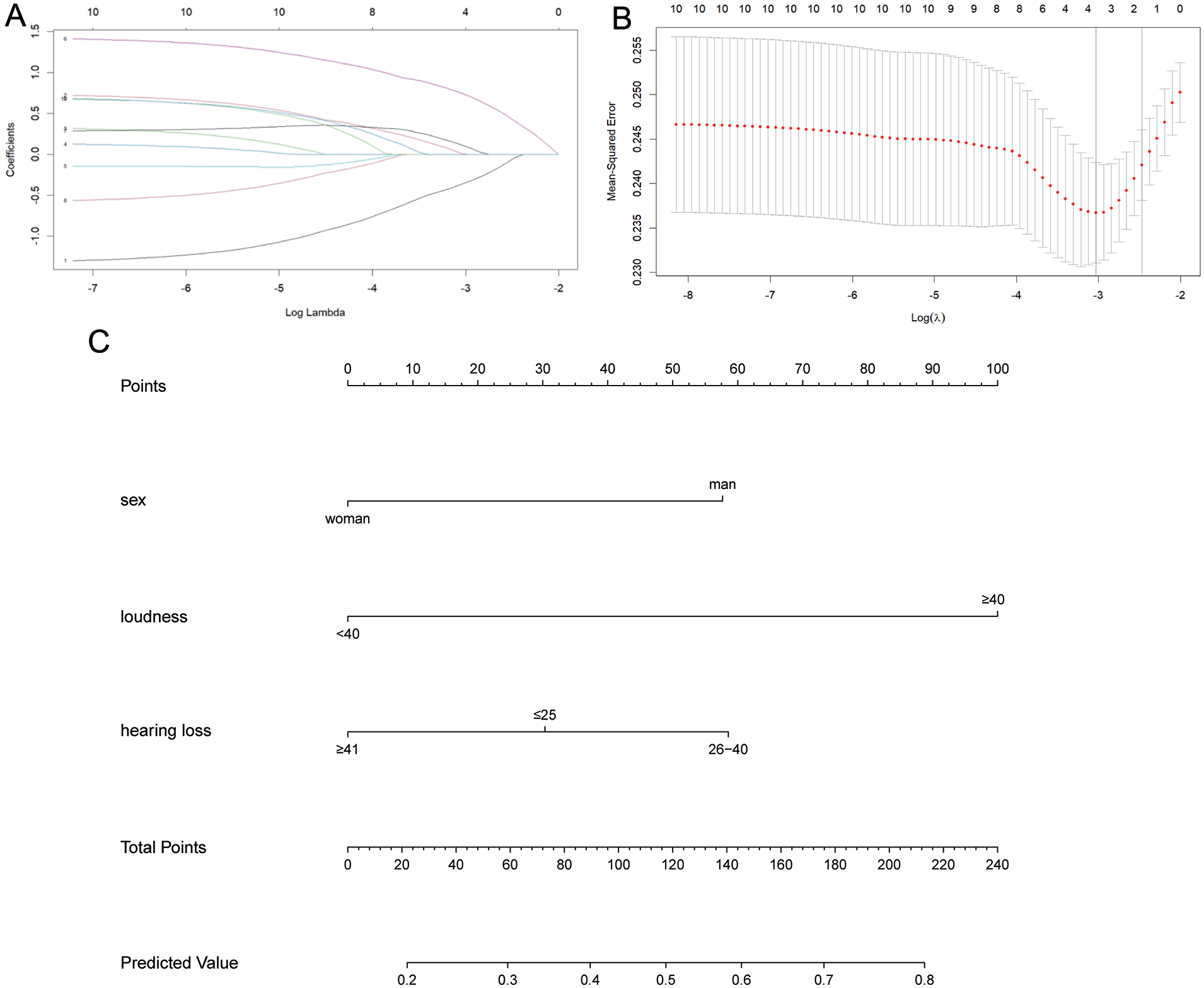
(A) By constructing a penalty function, the coefficients of the variables could be compressed so that some regression coefficients become 0. (B) Four variables were included with 1 standard error criterion. (C) Nomogram of factors affecting the severity for patients with subjective tinnitus.
All candidate variables were included in the binary logistic regression analysis presented in Table 2. The results showed that gender (OR: 0.76; 95% CI: 0.6-0.95;
Binary Logistic Regression Analysis of Risk Factors Associated With Unilateral Subjective Tinnitus.
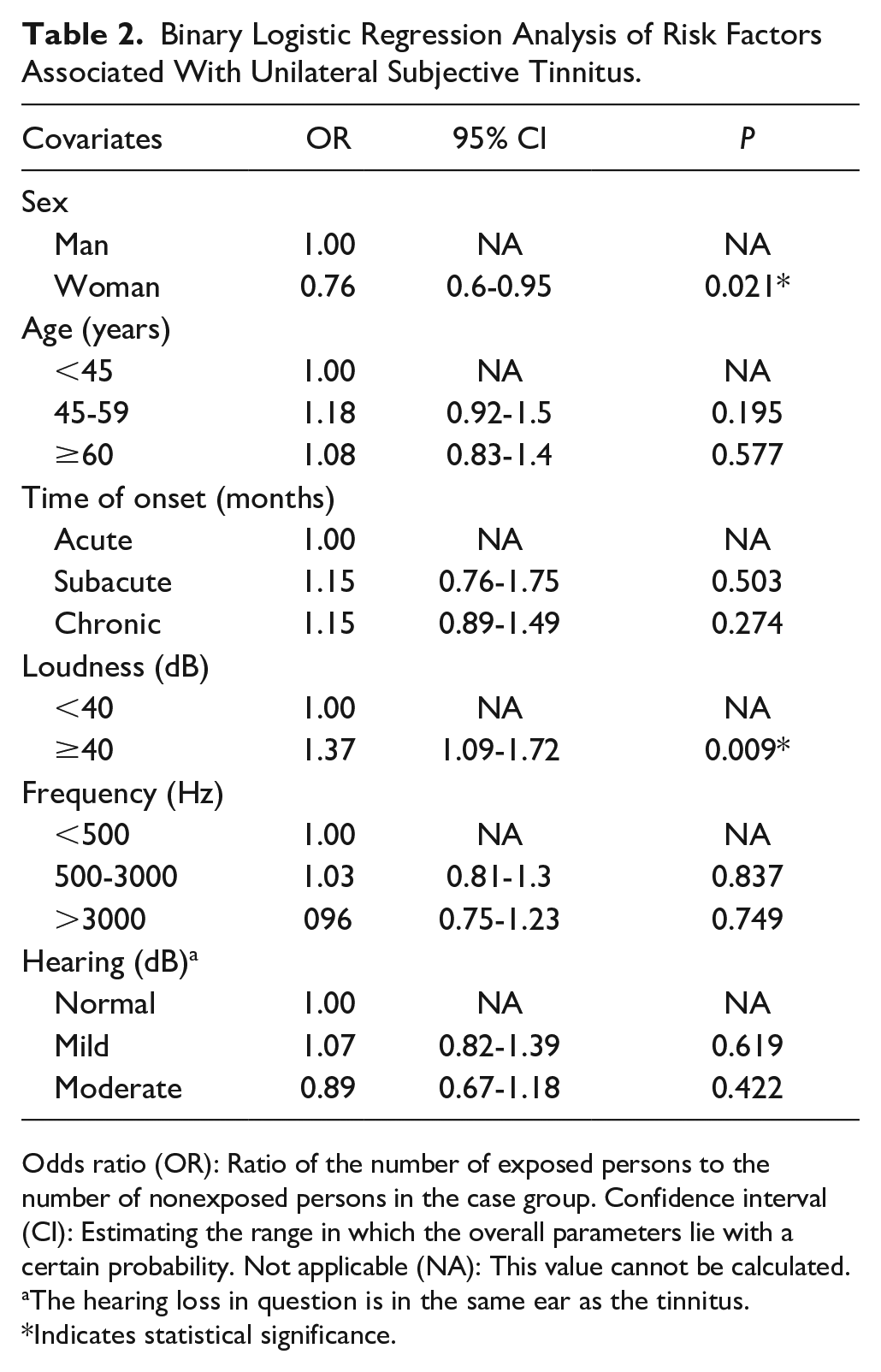
Odds ratio (OR): Ratio of the number of exposed persons to the number of nonexposed persons in the case group. Confidence interval (CI): Estimating the range in which the overall parameters lie with a certain probability. Not applicable (NA): This value cannot be calculated.
The hearing loss in question is in the same ear as the tinnitus.
Indicates statistical significance.
Validation of Nomogram
The performance of the nomogram was internally validated by estimating the discriminative ability of the novel model. We used the C-index to determine the discrimination of the predictive model. The C-index was 0.707 (95% CI: 0.607-0.806) for the training cohort and 0.706 (95% CI: 0.548-0.863) for the validation cohort, indicating that the prediction model had a powerful ability to discriminate. Similarly, in the training and the validation cohorts, the ROC curves of our nomogram were 0.692 and 0.705 (Figure 3), respectively. These results showed that the model had good accuracy.
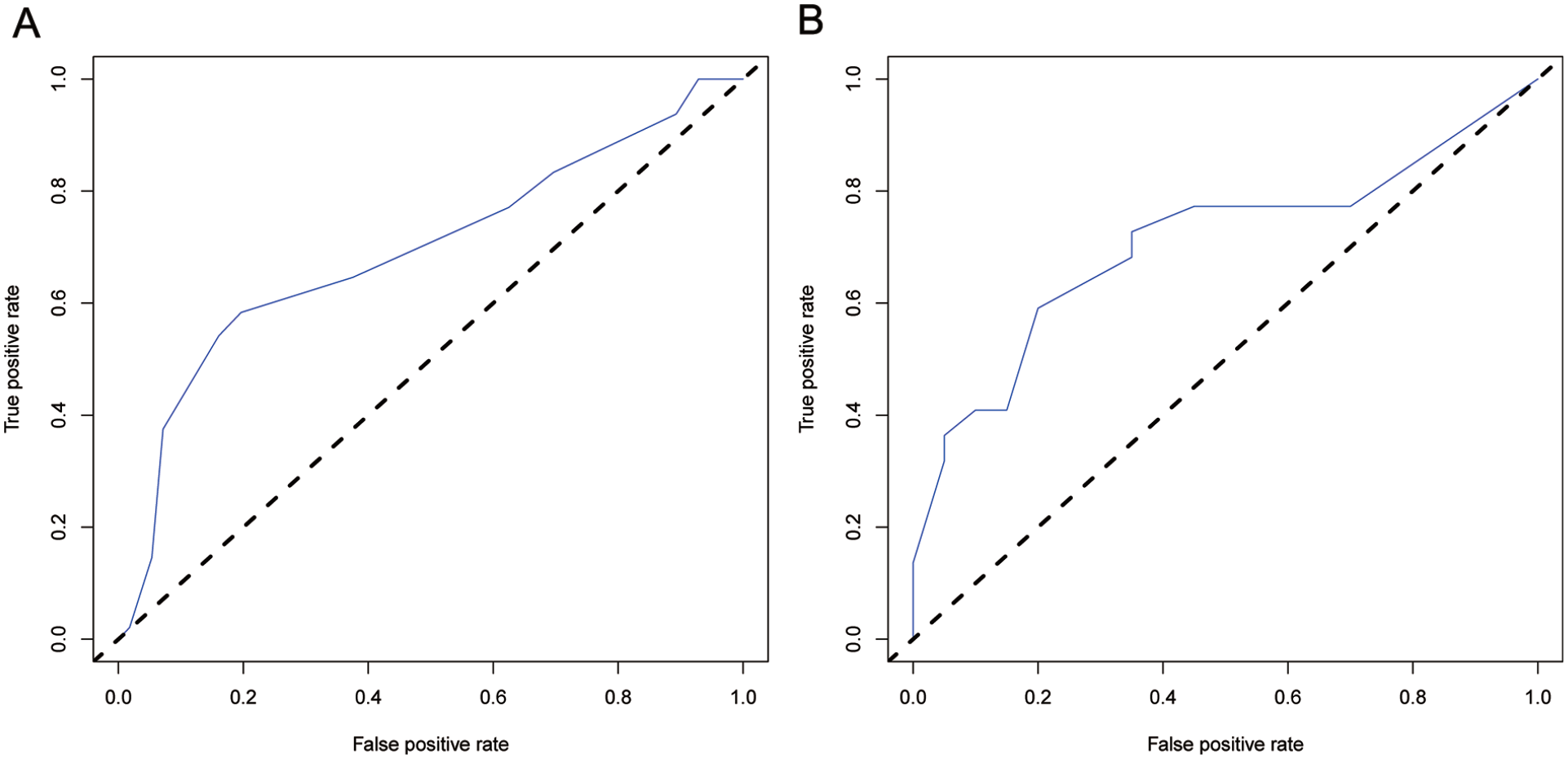
The AUC of ROC curve for predicting severity of unilateral subjective tinnitus. (A) The training set; (B) the validation set.
Clinical Application of Nomogram
The total score for each patient can be calculated by adding up the scores for each of the variables listed in Figure 3. The probability of unilateral tinnitus severity occurring in unilateral subjective tinnitus can then be predicted from the nomogram, using the total score as a reference. For example, as shown in the legend, a male patient with a tinnitus loudness of less than 40 dB and a hearing loss between 26 and 40 dB would have a cumulative score of approximately 115 points. The corresponding risk of patients developing unilateral severe tinnitus is approximately 40% to 50%. Therefore, it is strongly recommended that this patient undergo further tinnitus testing, and interventions are strongly recommended to prevent the progression of the condition.
Discussion
To our knowledge, this is the first study to establish a nomogram to estimate the predicted risk probability of tinnitus severity in patients with unilateral subjective tinnitus.
In this study, we developed and validated a nomogram based on clinical indicators to predict the risk of patients developing unilateral severe subjective tinnitus. The nomogram provides clinicians with a fully visualized, evidence-based tool to standardize clinical decision-making. Our model includes gender, tinnitus loudness, and hearing loss as predictors of patients with unilateral severe subjective tinnitus. Furthermore, the validation results demonstrate good discrimination accuracy of the nomogram.
Compared to traditional methods for assessing tinnitus severity, the nomogram has several advantages. Firstly, traditional methods, such as subjective self-report questionnaires or audiometric measurements, may be limited by their subjectivity or lack of sensitivity to individual differences. In contrast, the nomogram model can incorporate multiple variables, including demographic and clinical factors, to provide a more comprehensive and personalized assessment of tinnitus severity. Secondly, the nomogram model can generate a visual representation of the predicted tinnitus severity score based on the input variables, which can facilitate communication between healthcare providers and patients. This can help patients better understand their condition and make informed decisions regarding treatment options. Thirdly, the nomogram model can be updated and refined as new data becomes available, allowing for ongoing improvements in its predictive accuracy and clinical utility.
Our model revealed tinnitus loudness as an independent predictor for patients with unilateral severe subjective tinnitus, which is consistent with previous observations linking tinnitus loudness to tinnitus severity based on the THI scale. 17 High THI scores associated with increased loudness of tinnitus suggest that perceived tinnitus strength could exacerbate tinnitus symptoms and lead to significant adverse effects. 18 Moreover, strategies aimed at reducing tinnitus loudness have been effective in treating tinnitus. 19
Our study identified sex as an independent predictor of unilateral severe subjective tinnitus. However, our findings differ from earlier research that suggested tinnitus is more likely to worsen in women than men. 9 Instead, our results indicated that tinnitus is generally more severe in men. This finding may be attributed to certain male patients experiencing more tinnitus and stress. It is worth noting that responses to tinnitus can vary significantly among individuals. 20 Additionally, gender differences in the form and function of auditory system processing exist due to the interplay between genetic susceptibility and hormones. 21 When discussing the measurement of subjective tinnitus loudness, it is important to acknowledge the subjectivity and potential biases involved in the measurement process. Despite the use of certain objective techniques, such as psychoacoustic tests, there is still a reliance on patients’ subjective judgments. This can lead to biases in patients’ responses regarding the loudness of their tinnitus during testing. To address this issue, a multi-method approach that combines subjective and objective measurements is necessary to obtain a more comprehensive assessment of tinnitus. Furthermore, ongoing research is needed to develop more objective and reliable measures for tinnitus assessment, enhancing the accuracy and reliability of evaluations.
In our study, we found no direct link between hearing loss and tinnitus. However, we did include hearing loss as a factor in evaluating subjective tinnitus severity due to its clinical relevance and its potential to increase patient discomfort. Indeed, previous studies find high-frequency hearing loss linked to tinnitus. 22 This is because hearing loss is frequently observed alongside tinnitus, which can cause additional discomfort for patients. Moreover, hearing loss may be caused by damage or dysfunction of the peripheral or central auditory system, which is a critical component of all current theories on the pathophysiology of tinnitus. 10 One widely accepted theory proposes that compensatory changes in homeostasis of the central structures occur as a result of hearing loss to maintain auditory nerve activity. 23 This process may lead to tinnitus as a maladaptive consequence. 24
Several studies have aimed to identify different factors that influence subjective perceptions of tinnitus severity8,9 and to create a phenotypic profile of subjective tinnitus patients. 25 However, there is a need for a user-friendly tool that integrates these risk factors to make better clinical decisions. Nomograms can integrate risk factors associated with outcomes. 26 In recent years, nomograms have been introduced because of their convenient interface and strong statistical ability to predict individualized outcomes. 26 Our nomogram would provide accurate, and personalized risk predictions for each individual, enabling clinicians to effectively screen high-risk patients and provide timely interventions. The parameters in the nomogram are easily accessible, providing a straightforward interface without the need for a computer software. Overall, our study builds upon previous research and highlights the potential of using nomograms in clinical decision-making and treatment planning for tinnitus patients.
There are several significant limitations. First, this single-center nature of the study limits its generalizability, and further external validation in larger and more diverse populations is needed. Additionally, the retrospective design of the study raises the possibility of selection bias, which should be considered when interpreting the results. Moreover, our study did not evaluate extended high-frequency hearing levels in tinnitus patients who may still experience hidden high-frequency hearing loss despite having normal conventional PTA. Our future research will incorporate extended high-frequency hearing tests for these patients to elucidate the predictive value of hearing loss within the nomogram. Nonetheless, the development of a prediction nomogram for subjective tinnitus is a significant achievement, and this tool has the potential to help clinicians make more informed decisions about screening and interventions for their patients. Future research should aim to address these limitations and further refine the predictive accuracy of the nomogram.
Conclusions
In conclusion, we developed and internally validated a nomogram that accurately predicts tinnitus severity in patients with unilateral subjective tinnitus using gender, tinnitus loudness, and hearing loss as predictors. This user-friendly tool could prove valuable for clinicians in their decision-making regarding risk assessment and personalized treatment for patients with unilateral subjective tinnitus.
Footnotes
Publisher’s Note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organization, or those of the publisher, the editors, and the reviewers.
Authors’ Contributions
Xiao-Min Zhai had full access to all of the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. Study conception and design: Rui Guo, Jia-Jia Dong, Hong-Lei Zhang, and Jun Yuan. Acquisition, analysis, or interpretation of data: All authors. Drafting of the article: Xiao-Min Zhai and Jia-Jia Dong. Critical revision of the article for important intellectual content: Rui Guo, Jia-Jia Dong, Hong-Lei Zhang, Jun Yuan, and Xue-Jing Hao. Statistical analysis: Xiao-Min Zhai. Obtained funding: Rui Guo. Administrative, technical, or material support: Rui Guo, Hong-Lei Zhang, and Jun Yuan. Study supervision: Rui Guo and Hong-Lei Zhang. All authors have read and agreed to the published version of the article.
Data Availability
Data will be made available on request.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by Air Force Medical Central (No. 2021LC017 and No. 2021LC007).
Ethical/Consent Statement
I certify that this article is original and has not been published and will not be submitted elsewhere for publication while being considered by
