Abstract
Chronic tonsillitis is a common otolaryngological disease worldwide. The treatment of choice is tonsillectomy, which is one of the most frequently performed procedures in Ear, Nose and Throat Departments. As with any surgical procedure, there are possible complications. Among them, rarely encountered and reported mainly in the pediatric population, is a short-term, transient facial nerve palsy resulting from local anesthetic administration. Here, we present a rare case of a 20-year-old woman with recurrent angina, who developed short-term, fully transient peripheral facial nerve palsy immediately after tonsillectomy under local anesthesia.
Introduction
Tonsillectomy is a routine surgical procedure often practiced by otolaryngologists in the treatment of recurrent tonsillitis. Between 2018 and 2022, we performed 230 tonsillectomies under local anesthesia in our clinic. There are 4 groups of indications for removing the tonsils: infections (eg, recurrent angina or recurrent intra- and peritonsillar abscesses), obstruction of the upper airways caused by hypertrophy of the tonsils (eg, sleep apnea or swallowing disorders), focal diseases (eg, rheumatic fever or inflammation of the heart or kidneys), and suspicion of neoplastic tonsillar processes.1,2 The most frequently observed postoperative complications are pain, early and late bleeding from the tonsillar bed, vomiting, dehydration, and swelling of the tongue and/or uvula. 3 The procedure can be performed under both general anesthesia and local anesthesia combined with sedation. Peritonsillar drug infiltration of a lignocaine–epinephrine solution during tonsillectomy is a common technique used by many otolaryngologists as an adjuvant therapy to reduce intraoperative bleeding and postoperative pain. Different local anesthetic doses have been described in the literature, but they are usually in the range of 4 to 10 mL per side of each tonsils’ niche.4 -6
In our clinic, due to observations of lower intraoperative bleeding, shorter hospitalization times, a tendency to avoid burdening the patient with general anesthesia drugs, and lower postoperative pain, we mostly perform tonsillectomy under local anesthesia. The routine dose of lignocaine is 10 mg, and that of epinephrine is 0.5 mg (10 mL volume of solution) per tonsil. An extremely rare complication of tonsillectomy is transient facial nerve palsy, which may result from infiltration of the parapharyngeal space with local anesthetics. Such a condition occurs most often in the pediatric population.7 -10 Thus far, this complication has not been reported in adults. Due to the rarity of this condition, in this article, we present the case of a 20-year-old woman with recurrent angina who developed short-term, fully transient peripheral facial nerve palsy immediately after tonsillectomy under local anesthesia.
Case Report
A 20-year-old patient with a long-term history of recurrent angina (up to 10 times a year) and severe symptoms over the past 2 years was admitted to the Department of Otolaryngology, Laryngological Oncology and Maxillofacial Surgery, University Hospital No. 2, 85-168 Bydgoszcz, Poland. Based on her medical history and clinical examination, she qualified for tonsillectomy under local anesthesia. The patient had no previous chronic illness and was not taking any medications on a regular basis.
On the day of admission to the clinic, the patient’s condition was good, and the required laboratory tests (ie, blood count and coagulogram) were performed. In the preoperative procedure, the patient received 2 g of cefazolin for antibiotic preoperative prophylaxis, 0.5 mg of atropine, and 20 mg of nalbufin. Immediately before the tonsillectomy, the patient received an additional 2 mg of midazolam and, for local anesthesia around the tonsils, a total of 20 mg of lignocaine and 1 mg of adrenaline (10 mg of lignocaine and 0.5 mg of adrenaline per tonsil). The course of the tonsillectomy was uncomplicated, and the patient did not report any disturbing symptoms. Immediately after returning to the hospital room, the patient reported the inability to close the eyelids of the right eye and the feeling that the corner of her mouth was falling down. The laryngological examination revealed peripheral nerve palsy of the VII nerve on the right side, or grade IV/V of the House–Brackmann scale (Figure 1-3). Intravenous steroid therapy with dexamethasone at a dose of 8 mg and subcutaneous injection of galantamine (5 mg) were immediately initiated. The patient was closely monitored, during which a gradual return of facial nerve function to normal was observed within 2 hours of the end of the procedure (Figure 4-6). During further hospitalization, facial nerve function was observed to be normal. The patient was discharged home on the first postoperative day, with normal local healing and full function of the right VII nerve.
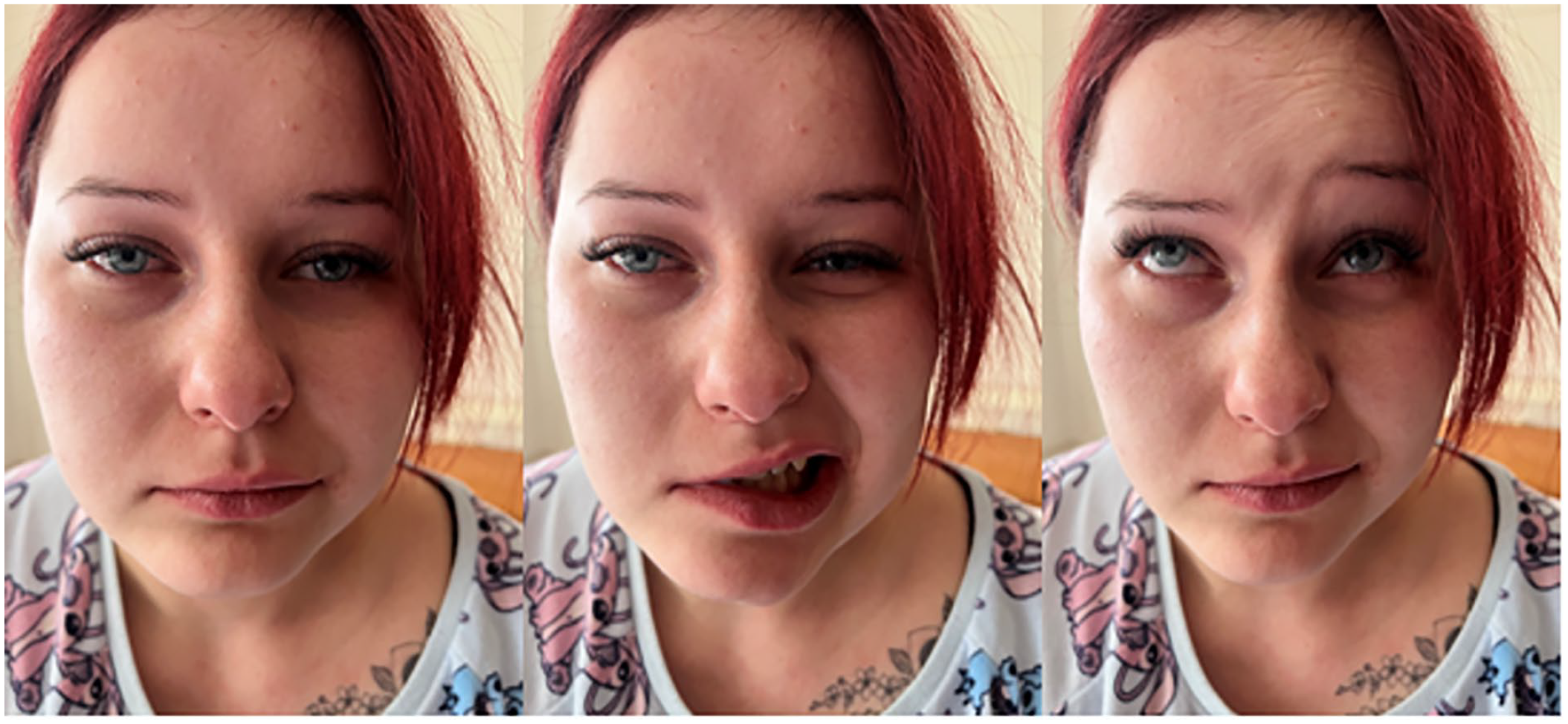
Patient directly after tonsilletomy—right facial nerve palsy.

Patient after 2 hours after tonsillectomy—full recovery of function of facial nerve.
Discussion
To explain the mechanism of facial nerve palsy after tonsillectomy, it is important to discuss 2 aspects: the effect of lignocaine on nerve transmission and the anatomical course of the facial nerve after exiting the stylomastoid foramen.
Lidocaine is a sodium channel blocker, whose main mechanism of action is blocking voltage-gated Na+ channels. The drug can reduce the peak currents of Na+ channels and accelerate the deactivation process to reduce the excitability of neurons, thus preventing or reducing the sensation of pain. 11 Lidocaine is known to have an onset of less than 2 minutes and a duration of 1 to 2 hours. 12 If epinephrine is supplemented, a prolongation of this action occurs as a consequence of vasoconstriction, which delays the clearance of the local anesthetic from the surgical site. 13
The facial nerve is the seventh cranial nerve, which leaves the cranial cavity through the stylomastoid foramen and exists on the outer surface of the base of the skull. Then, it divides and separates in 3 directions: downwards, branching into the posterior belly of the digastric muscle; posteriorly, into the posterior auricular nerve; and anteriorly, bending and penetrating almost horizontally into the parotid gland, just below the external auditory opening and lateral to the posterior belly of the digastric muscle, which lies on the lateral surface of the mandibular branch. 14 Generally, all facial expression muscles receive their innervation via the facial nerve. 15
Peritonsillar administration of local anesthetics, especially when the injection is administered too deeply, may cause the drug to pass through the superior pharyngeal sphincter muscle, thereby affecting the facial nerve trunk and its branches.7 -10 This is manifested by peripheral paralysis of the facial nerve; the patient is unable to close their eyelids, the philtrum smoothes out, and the corner of the mouth drops down. 16 To assess the severity of symptoms, the House–Brackmann scale is used, 17 which in the case of our patient indicated a stage of IV/V facial nerve palsy.
Facial nerve dysfunction may result from both the pharmacokinetics of local anesthetics and the compression caused by the volume of the administered solution. The pathogenesis of palsy presents as retrograde epineurial compression edema with ischemia of the facial nerve caused by vasospasm. 18 Peripheral nerves rely on their blood supply to maintain the structural and functional requirements of the vasa nervorum. 19 In the case of our patient, the agents used for local anesthesia, after moving into the area of the facial nerve fibers, were able to directly affect nerve transmission (lidocaine) and the contraction of the vasa nervorum, which nourishes the nerve (epinephrine). With the passage of time and a decrease in the local concentration of the drug, a gradual regression of the symptoms of facial nerve palsy is observed until a complete return to function, which in this case took about 2 hours.
To minimize the risk of facial nerve palsy as a complication of tonsillectomy, the surgeon should inject local anesthetics directly into the peritonsillar space and avoid an overdose of drugs and repeated injections.
Conclusion
Tonsillectomy is a basic laryngological procedure performed in everyday medical practice. Local anesthesia during the procedure reduces the risk of early bleeding, as well as postoperative pain. Like any surgical procedure, there is a risk of complications. Among them, peripheral facial nerve palsy resulting from the local administration of anesthetics is extremely rare and may occur in both children and adults. Fortunately, this complication usually disappears within a few hours after the end of the procedure, does not leave any permanent consequences, and does not affect the patient’s recovery.
Footnotes
Data Availability Statement
No public database has been created. All data are available from the authors of the work.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethic Statement
Our institution does not require ethical approval for reporting individual cases or case series.
Statement of Informed Consent
Verbal informed consent was obtained from the patient(s) for their anonymized information to be published in this article.
