Abstract
Parathyroid cyst is a rare entity that can closely mimic thyroid and brachial cleft cysts, particularly when located within the thyroid gland. Most commonly, the cysts are non-functional but can produce compressive symptoms. The cyst contains watery content with elevated PTH levels, specifying parathyroid origin 1 . Parathyroid cysts should be considered in the differential in patients with a neck mass. This study describes a rare case of a middle-aged woman with a history of a symptomatic intrathyroidal parathyroid cyst discovered intraoperatively.
Report of a Case
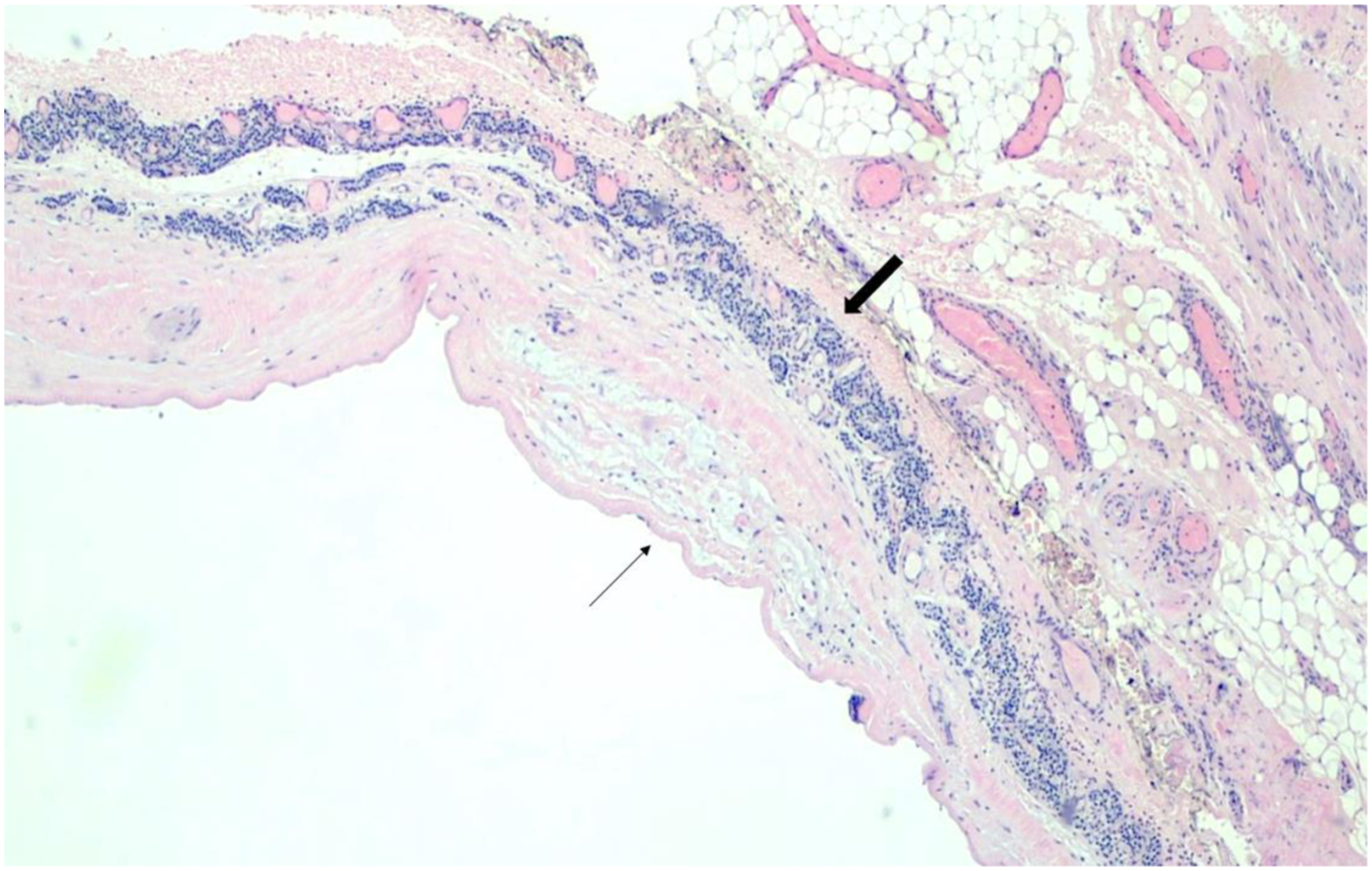
A 32-year-old female presented with a 1-year history of a left thyroid mass and worsening compressive symptoms. She described neck pain radiating to her left ear, labored breathing, and shortness of breath. She denied dysphagia, weight loss, and family history of thyroid cancer. Labs revealed low Thyroid Stimulating Hormone (TSH), normal Thyroid Stimulating Immunoglobulin (TSI), and normal free T4 and T3. Basic metabolic panel, CBC, and calcitonin were also within normal limits. An enlarged left thyroid lobe was appreciated on physical exam. Thyroid ultrasound confirmed the presence of a large, lobulated and partially septated cyst extending from the mid upper portion of the left thyroid lobe measuring 8.5 x 6.3 x 3.8 cm. Ultrasound also revealed a small right-sided solid nodule with mixed echogenicity and no microcalcifications, measuring 1.3 x 0.7 x 0.6 cm (Figure 1). Given the worsening compressive symptoms, the patient elected to a left hemithyroidectomy. Intraoperatively, the thin-walled large cystic nodule ruptured and released completely clear watery fluid. Histology of the left thyroid lobe showed Hashimoto’s thyroiditis and a large cyst with a thin fibrous wall containing foci of linear parathyroid tissue enriched with vessels and lacking adipocytes, consistent with a parathyroid cyst (Figure 2). Neck ultrasound demonstrating left intrathyroidal cyst. Representative H&E slide demonstrating cyst wall (thin black arrow) with hypercellular parathyroid tissue (thick black arrow).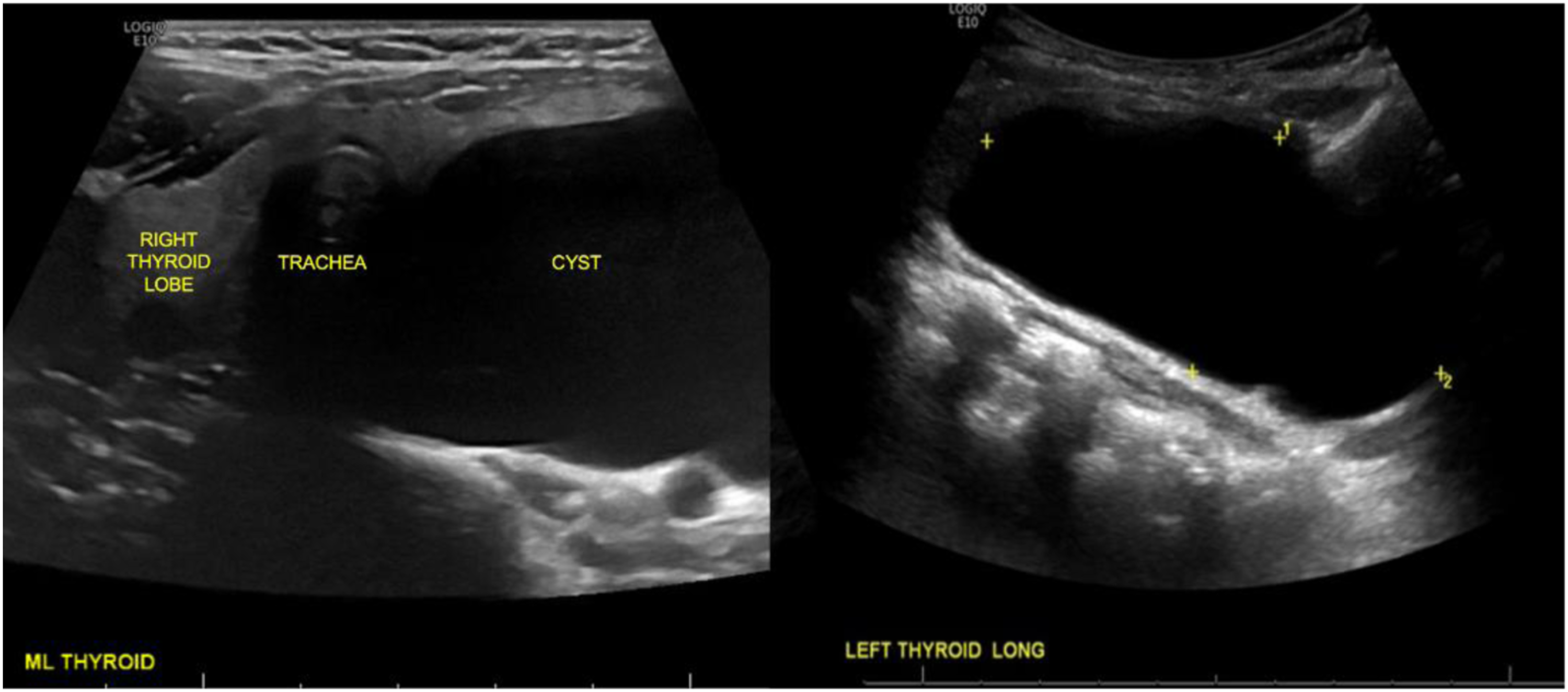
Discussion:
Parathyroid cysts are a rare entity, representing <1% of neck masses and with an estimated incidence of 0.075%. 1 Most frequently, parathyroid cysts are positioned under the lower pole of the thyroid gland and are seen in the presence of additional thyroid nodules. 2 More than 90% of these cysts are non-functioning and appear to present more commonly in females between the ages of 40 and 60. Although rare, parathyroid cysts can produce compressive symptoms, as observed in this patient. 3
Intrathyroidal parathyroid cysts are even less common, as only eight cases have been reported in the literature. 4 The diagnosis proves to be a challenge as the cyst presents as a classic thyroid cyst on ultrasound, a well-defined homogenous nodule nestled within the lobe with no areas of calcification. Fine needle aspiration (FNA) and cytology of the cyst can help differentiate thyroid and parathyroid origin, with elevated PTH levels diagnostic for a parathyroid cyst. Color and consistency of the fluid expelled from the cyst can highly increase suspicion of etiology. Parathyroid cysts classically contain clear, watery, and crystalloid fluid, while thyroid cysts contain darker, brown, and possibly bloody fluid due to presence of colloid and sometimes hemorrhage. 3 In this patients’ case where an FNA was not performed, release of clear watery fluid from the cyst intraoperatively suggested parathyroid origin.
Conclusions
Parathyroid cysts, though rare, should be included in the differential in a patient with an asymptomatic or compressive thyroid mass. The appearance of clear watery fluid is highly suggestive of parathyroid origin and can distinguish the mass preoperatively by FNA or during surgical intervention.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed Consent
The patient provided both verbal and written informed consent.
