Abstract
Immunoglobulin G4 (IgG4)-related disease is an immune-mediated disorder that commonly manifests in the salivary glands. As a recently described disorder, the description and classification of IgG4-related disease is an ongoing process. Diagnosis of IgG4-related disease requires integration of clinical history, histopathology, and radiographic findings, including ultrasonography and sialography. In this case report, we correlate parotid ultrasonographic and sialographic findings in a patient with proven IgG4-related disorder confirmed from analysis of previous submandibular gland resections. We aim to highlight the utility of multimodality imaging in the diagnosis of IgG4-related disease.
Introduction
Immunoglobulin G4 (IgG4)-related disease (IgG4-RD) was described in 2003 as an immune-mediated disorder that often involves multiple organs, presenting sub-acutely with tumor-like enlargement of the affected tissue. 1,2 It occurs commonly in salivary glands but has also been reported in nearly every organ system. As a recently described disorder, ongoing studies of its clinical presentation are actively directing revision of guidelines addressing evaluation and management.
The process of classifying salivary gland disease as IgG4-RD for research purposes differs from the process directing diagnosis for clinical management. 3 Wallace et al. 4 established the 2019 ACR/EULAR Classification Criteria for IgG4-Related Disease for enrollment in research studies. Their criteria sacrificed sensitivity (82.0%) to ensure high specificity (97.8%) with the goal to focus on exclusion of false positives. As a result, this ACR/EULAR classification scheme can be useful as a general guideline for clinical practice but should not be used to exclude patients if they do not completely fulfill criteria.
In a separate study, Wallace et al. 5 identified four distinct IgG4-RD phenotypes according to organ involvement and clinicopathologic similarities. Group 3 showed parotid involvement in only 22% of cases while Group 4 was associated with parotid involvement in 49% of cases. This heterogeneity in clinical presentation of IgG4-RD is further emphasized by the variability in reported findings in the radiographic analysis of salivary IgG4-RD.
Most reports identifying salivary gland IgG4-RD have shown the submandibular gland to be more commonly involved than the parotid gland and have identified a wide range of abnormal ultrasonic patterns. 6 -9 Reports of sialographic findings in patients with salivary gland IgG4-RD include glandular enlargement, ductal dilation, and slightly decreased secretory function without prominent sialectasis. 10,11
We describe bilateral parotid ultrasound and sialographic findings in a patient with IgG4-RD and symptomatic salivary swelling affecting all four glands to correlate imaging characteristics with histologic findings of previously resected submandibular glands.
Case Report
Clinical History
A 39-year-old woman presented to our otolaryngology clinic complaining of many years of painful bilateral parotid gland swelling, hardening, and itching with temporary improvement following sialadenoscopy with steroid and antibiotic insufflation. The patient’s left and right submandibular glands had been removed 4 and 2 years prior, respectively, for recurrent pain, itching, and swelling with limited response to oral antibiotics and immunosuppressive medications, including azathioprine, methotrexate, rituximab, and steroids. The patient reported symptomatic improvement with oral prednisone but experienced recurrence upon tapering the steroids. She denied any history of arthritis, xerophthalmia, or xerostomia. Laboratory testing revealed elevated ESR, slight anemia, and peripheral eosinophilia. Sjögren’s syndrome antibodies (SSA and SSB) were negative. Serum IgG4 levels were within normal limits.
Histopathological Findings of Submandibular Glands
Histopathologic re-examination of previously resected bilateral submandibular glands was performed by our institution with IgG and IgG4 immunohistochemistry. Both submandibular glands revealed chronic sialadenitis with periductal fibrosis and periacinar atrophy without storiform fibrosis or features of phlebitis (Figure 1(a)). Numerous eosinophils were present throughout the inflammatory infiltrate including some in ducts admixed with secretions and focally increased IgG4 plasma cells. Re-applied immunostaining identified 44 IgG4 plasma cells/hpf in the highest labeled area and an IgG4/IgG cell ratio of 46.8% (Figures 1(b) and (c)). Chronic sialadenitis (brackets) with periductal fibrosis (*) surrounding larger ducts (arrow) and acinar atrophy without storiform fibrosis or features of phlebitis (a). Immunohistochemistry for IgG (b) and IgG4 (c). IgG4, Immunoglobulin G4.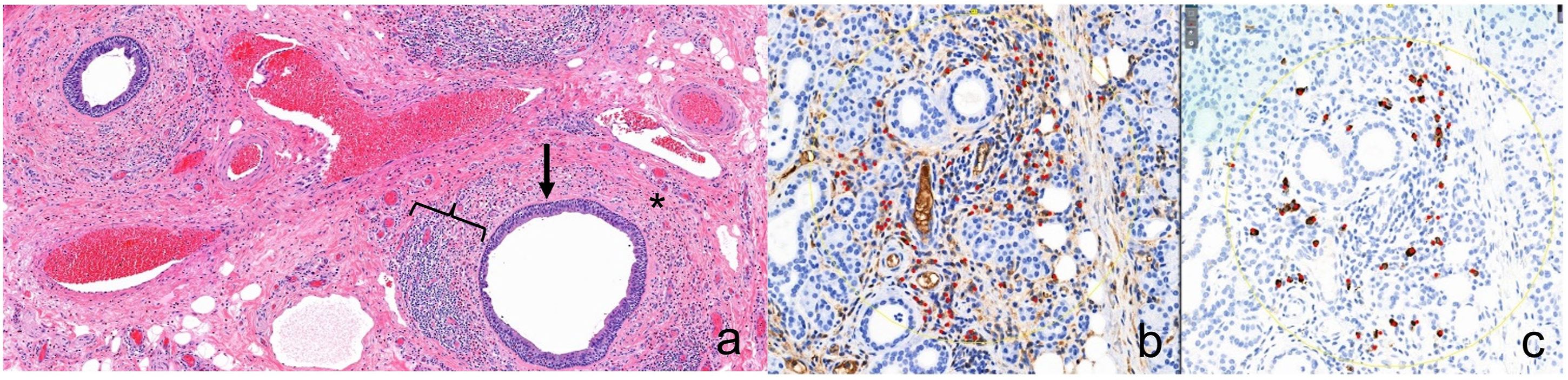
Parotid Sialography
Bilateral parotid sialography was performed with direct placement of a primed 22-gauge angiocatheter fixed to intravenous tubing through which Isovue 370® was instilled (3.5 mL on left; 3.0 mL on right), as described by Truong et al. 12 After adequate duct opacification was achieved, AP and lateral spot films were obtained. Removal of the cannulas permitted duct emptying with administration of lemon juice followed by post-void lateral imaging.
Normal primary and secondary ducts (per the Iowa Parotid Sialogram Classification System
13
) were identified on the left with mild narrowing of the mid main parotid duct on the right (Figure 2(a)). Intraglandular ductal irregularity was present bilaterally with post-void films showing adequate emptying with no contrast identifiable in the gland or duct system. Lateral view of right parotid sialogram showing mild narrowing of the main parotid duct (arrow) and normal secondary ducts (arrowheads) (a). Post-void films showing adequate emptying in bilateral parotid glands (arrows) with no residual contrast identified (b).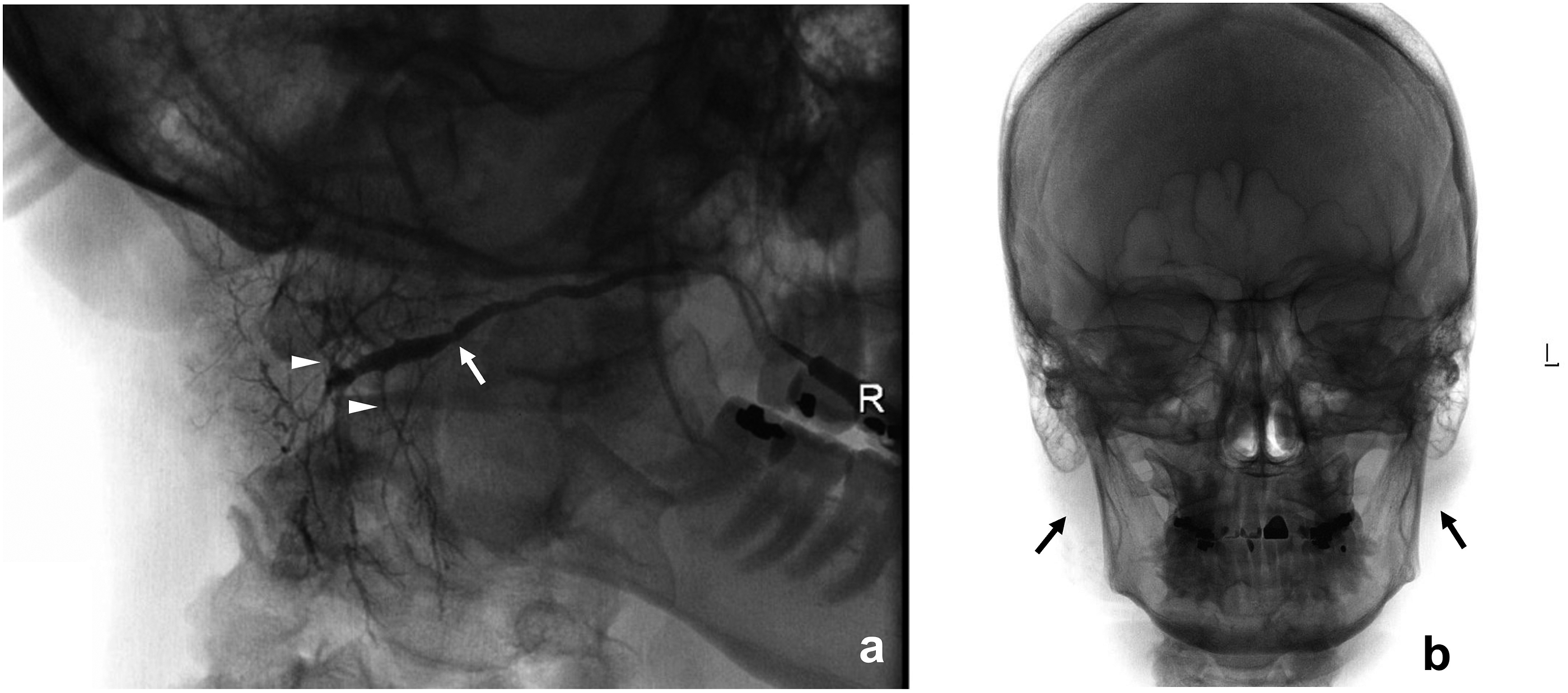
Ultrasound Evaluation
Ultrasound reports from 2 years prior (actual images not available for review) identified enlargement of the right submandibular gland with hypoechoic and heterogeneous echotexture. The left submandibular gland had been removed. Also reported was the presence of multiple small cysts noted in bilateral parotid glands, with regions of ductal dilation measuring up to 2.6 mm in the right Stenson’s duct. Ultrasound of the right parotid the following year, performed 2 months following right sialography with steroid insufflation, revealed that the gland, while still enlarged, had slightly decreased in size, as had the degree of ductal dilation (measuring 2.2 mm). Ultrasound (unstimulated) performed at our institution immediately before sialography revealed enlarged ducts without obstruction of the right parotid main duct (Figure 3(a)) and gland parenchyma including secondary ducts (Figure 3(b)), with dilated secondary and tertiary ducts without obstruction (Figure 3(c)). Transverse ultrasound images showing enlarged ducts without obstruction of right parotid main duct (arrows; a, b) and gland parenchyma including secondary ducts (arrowheads; b, c). Longitudinal image of left parotid parenchyma identifies dilated secondary and tertiary ducts without obstruction (arrowheads; c).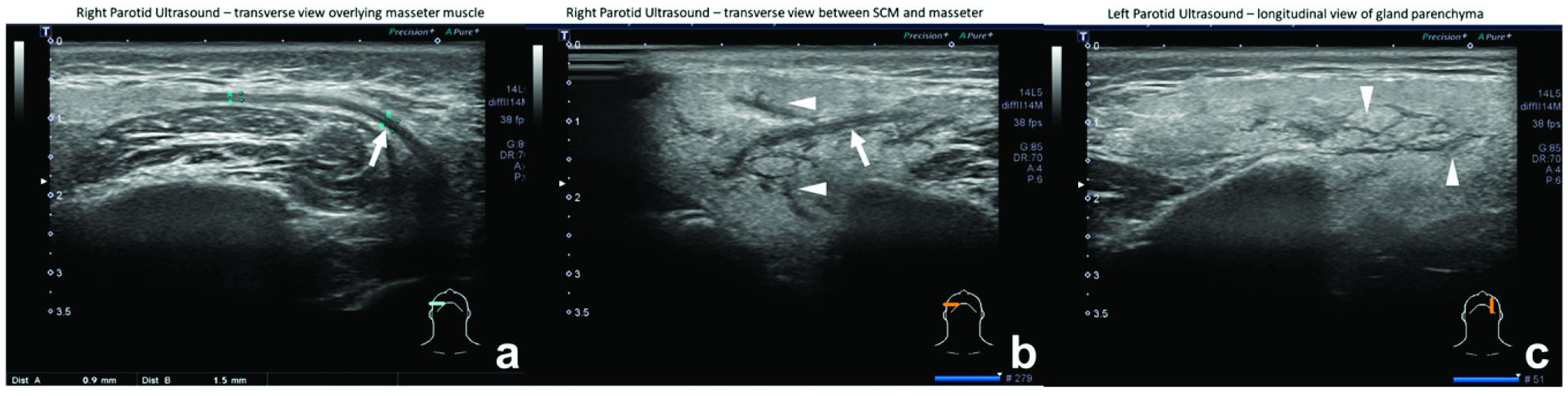
Discussion
The differential diagnosis of salivary gland enlargement is broad and includes neoplasia, infection, obstruction, and immune-mediated conditions such as IgG4-related disease (IgG4-RD) or Sjögren’s syndrome. 1,14,15 A retrospective comparison by Hong et al. revealed overlapping clinical, laboratory, radiographic, and histopathologic findings for IgG4-RD, Sjögren’s syndrome, and obstructive submandibular sialadenitis. 11 The therapeutic principles guiding management of each of these conditions are different, and therefore, thoughtful diagnostic workup is needed to optimize management. The 2019 ACR/EULAR Classification Criteria for IgG4-RD identifies that the classification of IgG4-RD requires the integration of clinical, serologic, radiological, and histopathologic features—stating that none of these findings in isolation are sufficient to clinically diagnose the disease. 4
The patient we present identified recurrent swelling of bilateral submandibular and parotid glands responsive to steroid insufflation. Serology was negative for Sjögren’s syndrome antibodies and there was no elevation in serum IgG4 concentration. Normal serum IgG4 concentrations, despite classic histopathological and immunohistochemical findings, have been reported previously in up to nearly 50% of patients with biopsy-proven, clinically active IgG4-RD. 1,4,16 In our patient, histopathologic re-examination of excised submandibular tissue revealed elevated IgG4-positive plasma cells and an increased IgG4-/IgG-positive plasma cell ratio, periductal fibrosis, and prominent eosinophilia—features consistent with a diagnosis of IgG4-related disease. However, it should be noted that the presence of increased IgG4-positive plasma cell infiltrates alone is not specific to IgG4-RD and has also been observed in malignancy, vasculitis, and other inflammatory diseases. 1,14 This case highlights the importance of correlating all clinical findings, and, specifically, the utility of multimodality imaging, in the diagnosis of IgG4-RD. The classification criteria established by Wallace et al. identify clinical features, including radiographic support and serology, may be sufficient to diagnose IgG4-RD in the absence of histopathology. 4
Narayan et al. reported sonographic features of salivary gland IgG4-RD to include hypoechoic lesions with variable patterns (reticular/nodal, irregular, net-like, heterogeneous echotexture, and diffuse hypoechogenicity). 7 Ultrasound of our patient’s parotid glands revealed a range of findings, including small cysts (hypoechoic regions) and hyperechoic echo-regions throughout the parotid parenchyma—features common to both IgG4-RD and Sjögren’s syndrome. 6,7 Narayan et al. also note the significant overlap of ultrasound findings between IgG4-RD and Sjögren’s syndrome that may confound differentiation using ultrasound imaging alone. 7 Although ultrasound and sialogram findings in IgG4-RD may be non-specific in isolation, these imaging modalities may increase diagnostic accuracy in patients with suspected IgG4-RD of the salivary glands.
Sialography has been considered the optimal imaging technique to identify salivary ductal changes. 6 It is most commonly used in concert with other salivary gland imaging modalities, with these combined evaluations thought to increase diagnostic accuracy. 6,12 Hong et al. showed distinct differences in sialography findings between the sialadenitis associated with IgG4-related disease (IgG4-RD), Sjögren’s syndrome (SS), and chronic obstructive submandibular sialadenitis. Sialography in patients with IgG4-RD showed glandular enlargement and ductal dilation in contrast to those with SS which was associated with prominent sialectasis. 11
Sialography in our patient revealed glandular enlargement and normal ductal structure with minimal irregularities and narrowing, without sialectasia or decreased secretory function, findings favoring the diagnosis of IgG4-RD over Sjögren’s syndrome. The parotid sialographic findings likely reflect periductal fibrosis and chronic inflammatory infiltrate with peripheral sparing noted in the previously excised submandibular glands. Further, the dilation of the secondary and tertiary ducts noted by parotid ultrasound may be secondary to the stenosis of the primary duct detected sialographically. This composite imaging analysis incorporating histopathology, sialography, and ultrasonography provides powerful supportive evidence for the diagnosis of IgG4-RD.
Accurate and early diagnosis of active, symptomatic IgG4-RD is necessary for the initiation of treatment to prevent potentially permanent tissue damage. 1,14,15 Glucocorticoids are utilized as first-line treatment for the disease with reports of excellent treatment response. 9 Our patient underwent several steroid and antibiotic insufflations and was prescribed multiple oral immunosuppressive medications throughout her clinical course. On comparison of the reports of the patient’s right parotid ultrasounds performed successively over 3 years, the degree of ductal dilation appears to have decreased over time, which may reflect a response to treatment that correlates to the patient’s reported temporary symptomatic relief following steroid insufflation. Wang et al. observed that response to steroid treatment may decrease with time, due to the extensive fibrosis and loss of regenerative ability of acinar cells. 9 Accordingly, long-term maintenance with regularly scheduled steroid insufflation, as was initiated for our patient, may be indicated for symptomatic management and prevention of irreversible glandular damage.
Conclusion
We present parotid sialographic and sonographic analogs of histopathologically proven IgG4-RD of the submandibular salivary glands. We also note the dynamic disease pattern of IgG4-RD demonstrated by the temporal changes observed in recording of successive parotid ultrasounds. Further, we highlight the role of multimodality imaging using both ultrasonography and sialography, along with histopathology and clinical history, for diagnosis and treatment of salivary gland IgG4-RD.
Footnotes
Author’s Note
Dr Hoffman is a research consultant for COOK Medical and author for Up To Date.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Abstract Presentations
Combined Otolaryngology Spring Meeting 2020, TRIO, Virtual Poster Presentation, May 15–June 15, 2020.
