Abstract
The necessity to routinely carry out histopathologic examinations of surgically removed polyps in patients with chronic rhinosinusitis with bilateral nasal polyps (CRSwNP) is uncertain. The aim of this study was to describe the histopathology of polyps from a large series of patients who underwent endoscopic sinus surgery for CRSwNP and the rate of neoplasms. This is a retrospective study of the histopathological result of all patients with CRSwNP who underwent functional endoscopic nasal surgery and in whom histologic examination was performed, from 2006 to 2015, in a tertiary medical center. Data on demographics and whether a nasal lesion was suspected for neoplasm prior to surgery were analyzed. Two hundred thirty-five patients underwent bilateral nasal polypectomy and histopathologic examinations of the surgical specimens. The rate of neoplasms in nonsuspicious cases was 2.3% (5 cases) and all were inverted papilloma. To conclude, inverted papilloma and other neoplasms are considered rare incidental findings in patients presenting with bilateral nasal polyps. This study demonstrated a higher rate of the latter than that reported in the literature. Our study further emphasizes that despite the low incidence of these pathologies, a histopathologic examination of every nasal polypectomy is warranted so as not to miss potential serious pathologies. We stress that a routine histopathological examination should be practiced at least in the elderly population.
Introduction
Chronic rhinosinusitis with bilateral nasal polyps (CRSwNP) affects from 0.5% to 4.3% of the population according to national population surveys. 1 It usually presents with nasal obstruction, smell impairment, and bilateral involvement. The disease significantly impairs quality of life and has the tendency to recur despite multiple medical and surgical interventions. It is associated with asthma, inhalant allergy, and aspirin sensitivity. 2 The diagnosis of CRSwNP is made according to clinical and imaging criteria, while histopathologic examination of nasal polyps contributes to disease classification according to the underlying inflammatory profile. It roughly differentiates between an eosinophilic or neutrophilic subtype, and it quantifies the eosinophilic burden of the disease, a factor that has a significant impact on treatment and disease recurrence. Pronounced eosinophilic infiltration is present in most CRSwNP cases in Western countries, while neutrophilic inflammation has been more commonly observed in polyps from patients with cystic fibrosis and in patients in Asian countries. 3 In essence, treatment is determined according to clinical phenotypes of the disease based on underlying conditions, such as aspirin-exacerbated respiratory disease, allergic fungal sinusitis, cystic fibrosis, primary ciliary dyskinesia, systemic disease, and immunodeficiency, as well as comorbidities, such as asthma and inhalant allergies. Current therapeutic approaches in the United States and European guidelines are oriented toward these phenotypes, while future therapies using monoclonal antibodies will be based on determining the specific pathophysiologic mechanism of the disease. 1,4
Since the treatment of CRSwNP is based upon clinical findings, the necessity for histopathologic examination of nasal polyps is uncertain, although tissue sampling may be important for excluding neoplastic disease. Inverted papilloma or other malignant neoplasms may also occur in apparently normal bilateral polyps. 5 -7 The consequences of an undiagnosed neoplasm are leading some authors to recommend routine histologic examination in bilateral nasal polyposis as well. 8 -13 The consequences of such a policy, however, are costly. In a meta-analysis that included 3772 patients, only 19 unexpected benign and 3 unexpected malignant diagnoses were identified (0.48% and 0.08%, respectively). The number needed to screen was 1258, and the pooled proportion for an unexpected malignant finding was 0.00107. The calculated cost to identify one unexpected malignant diagnosis was estimated at US$87 204.56 in that study. 14 We performed a retrospective chart study in order to review all the histopathologic results of nasal polyps taken from patients with bilateral nasal polyposis in order to extrapolate the rate of unexpected neoplastic results in our institution (Table 1).
Comparison of Unexpected Diagnosis of Neoplasms Among Patients With Chronic Rhinosinusitis With Bilateral Nasal Polyps Reported in the Literature and in the Current Study.
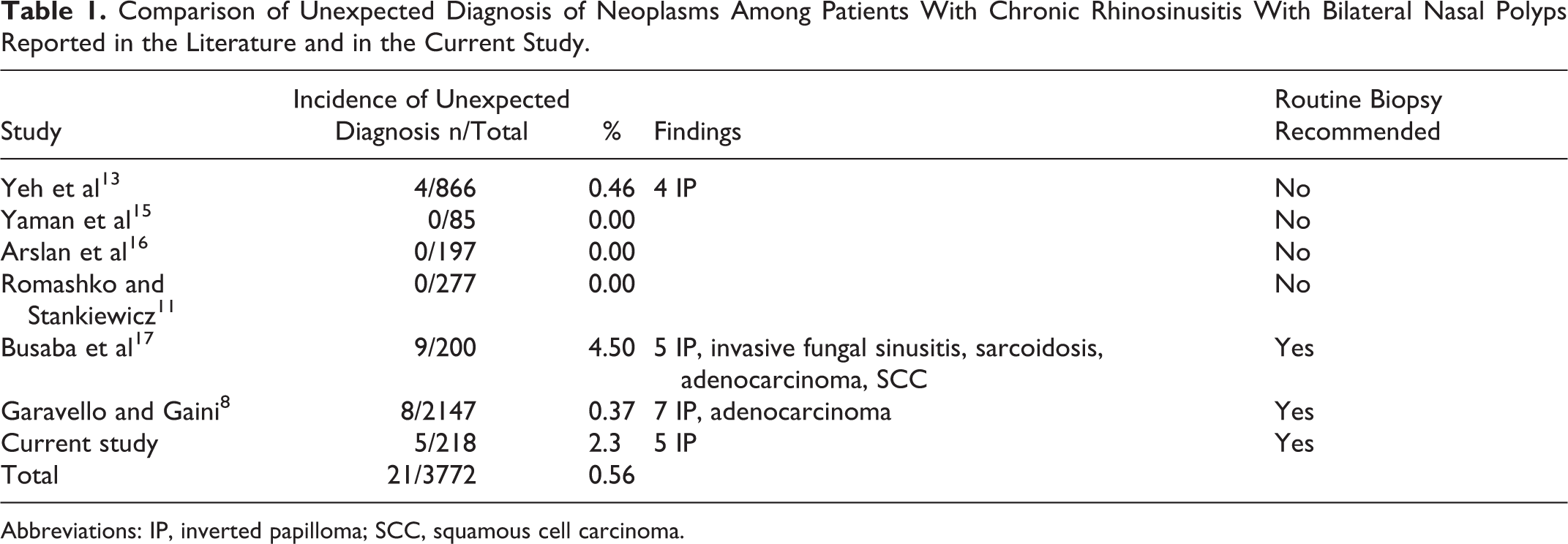

Abbreviations: IP, inverted papilloma; SCC, squamous cell carcinoma.
Materials and Methods
Retrospective Chart Study
The study was approved by the ethics board committee in TLVMC (0779-17 TLV).
Patient selection
The histopathologic results of all patients who underwent functional endoscopic sinus surgery (FESS) for chronic rhinosinusitis and bilateral polyposis, in which nasal polypectomy was performed from 2006 to 2015, were retrospectively reviewed.
Inclusion criteria were all adult patients with bilateral nasal polyps who underwent bilateral tissue sampling of the polyps during FESS. Patients with a preoperative diagnosis of neoplastic disease were excluded.
Data collection
Information on clinical and pathologic findings was extracted from the patients’ medical charts. Sources of data included operative reports, preoperative and postoperative physicians’ notes, and final histopathologic reports. According to departmental protocols, all patients processed preoperatively for FESS underwent a clinical evaluation by an expert rhinologist, including endoscopic evaluation and a computed tomographic imaging study of the sinonasal region. Criteria for surgical intervention were patients with symptoms of chronic rhinosinusitis without satisfactory response to medical therapy. Patients with unilateral polyposis were excluded from our study. Pathological sample was obtained from bilateral polyps and was performed on samples from both sides. Data on possible unanticipated risk factor for neoplastic disease were retrospectively retrieved from surgical notes; it included “suspicious” appearance according to intraoperative observations and polyp with erosion or vascular appearance. Patients were restratified as suspicious or nonsuspicious according to intraoperative findings, clinical presentation of epistaxis or imaging studies demonstrating bone erosion.
Statistical Analysis
Categorical variables, including gender, clinical suspicion, final pathology of neoplasm, and final pathology of inflammation, were described as frequency and percentage. For categorical variables, the λ2 test was used for comparisons. Age was reported by means and standard deviations, and Student t test was employed to compare the 2 study groups. Pearson correlation coefficient was performed to measure linear correlations between variables. The statistical analysis was performed using SPSS (IBM Corp. Released 2013. IBM SPSS Statistics for Windows, Version 22.0. Armonk, New York: IBM Corp). All reported P values were rounded off to 2 decimal places. All statistical tests and/or confidence intervals, as appropriate, were performed at α = .05 (2 sided).
Results
Two hundred thirty-five pathological samples were obtained from patients with chronic sinusitis and bilateral polyps, who underwent endoscopic sinus surgery in our institute. The median age of the patients was 52 years (interquartile range: 38-63) and 83 (35%) patients were females. Ten (4.3%) of our patients had inverted papilloma. There were no significant differences in gender distribution between the group of patients with neoplasms in the final pathology and the nonneoplastic group, but the patients with positive pathological findings were significantly older than those with negative findings (63.0 ± 13.11 years vs 50.12 ± 16.3 years, respectively; P = .015; Table 2).
Neoplasm Rates Among Patients Presenting With Bilateral Nasal Polyps Between 2006 and 2015.a

a N = 235.
The patients were further classified into suspicious and nonsuspicious for neoplastic involvement, and 220 (94%) were considered as having clinically nonsuspicious lesions during the preoperative and operative course. In the final pathology, 5 (2.3%) samples were found to have inverted papilloma and the remaining samples were diagnosed as inflammatory polyps (97.7%). Among the 15 (6%) suspicious lesions, 5 were found in final pathology to be inverted papilloma (33%) and the rest were inflammatory polyps (Table 2). No malignant lesions were detected in final pathology. Seven of the suspicious lesions were assessed as being asymmetric (the polyposis appeared to be much more extensive on one side), and 4 of them were diagnosed as inflammatory polyps on final pathology. Two lesions presented as bleeding lesions, and one of them was determined as being inflammatory polyps on final pathology. Two lesions were assessed as being firm, and 4 lesions were noted to have caused local bone thinning: All 6 of those lesions were eventually found to be inflammatory lesions on final pathology.
The patients whose final pathology was positive for neoplasm were significantly older than those whose final pathology was negative for neoplasm (63.0 ± 13.11 years vs 50.12 ± 16.3 years, P = .015; Table 3). There was only a weak positive correlation between age and final pathology positive for neoplasm among patients who presented with bilateral polyposis (Table 4). A logistic regression model based on age and gender for final pathology positive for neoplasm showed that the addition of every year in age in patients with bilateral polyposis increases the chance for final pathology positive for neoplasm by 6% (Table 5).
Demographics of the 235 Patients Who Presented With Bilateral Nasal Polyps.
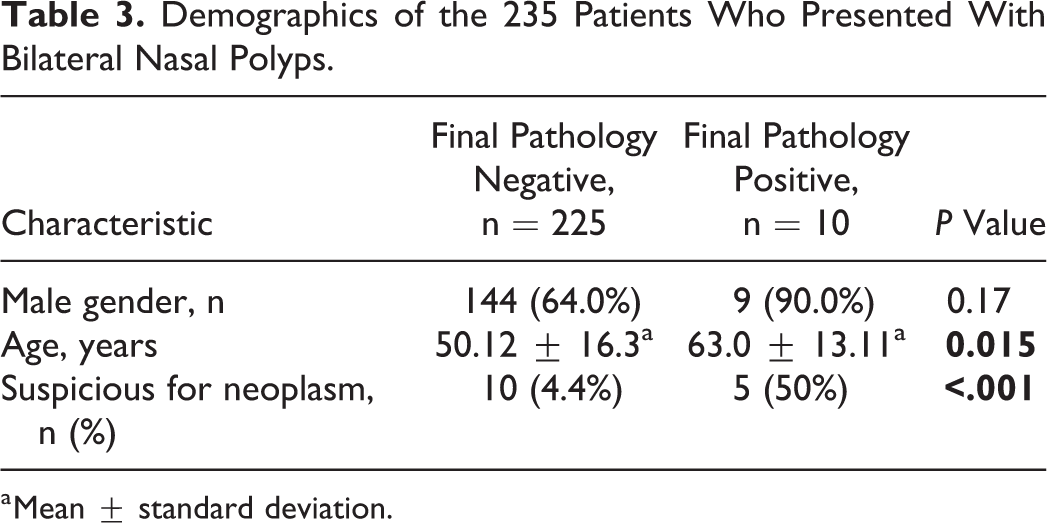
a Mean ± standard deviation.
Correlationsa Between Gender and Age and the Confirmation of Neoplasm Among Cases With Bilateral Nasal Polyps.
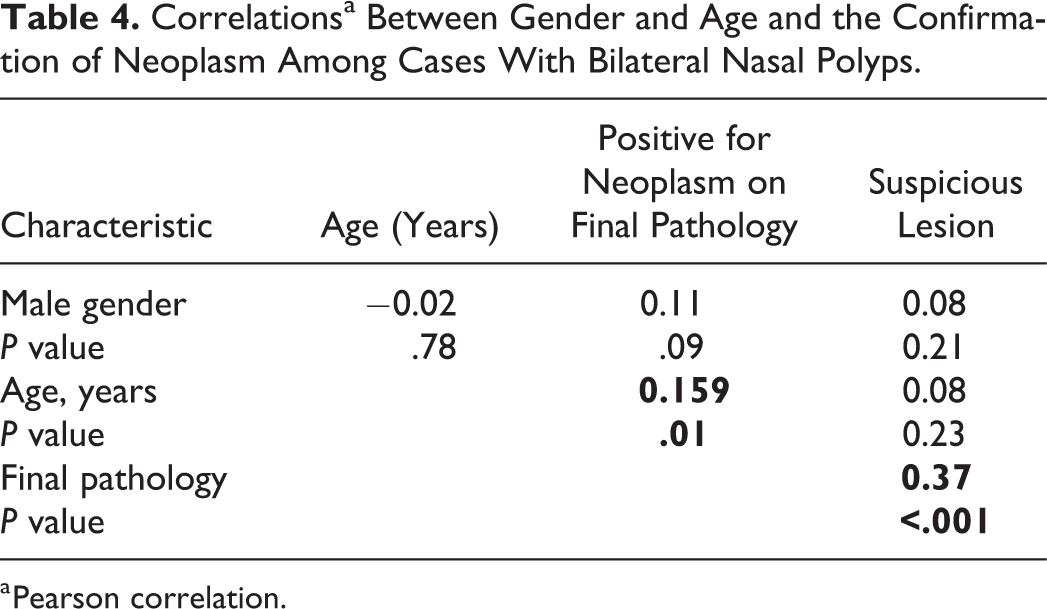
a Pearson correlation.
Multivariant Analysis.a
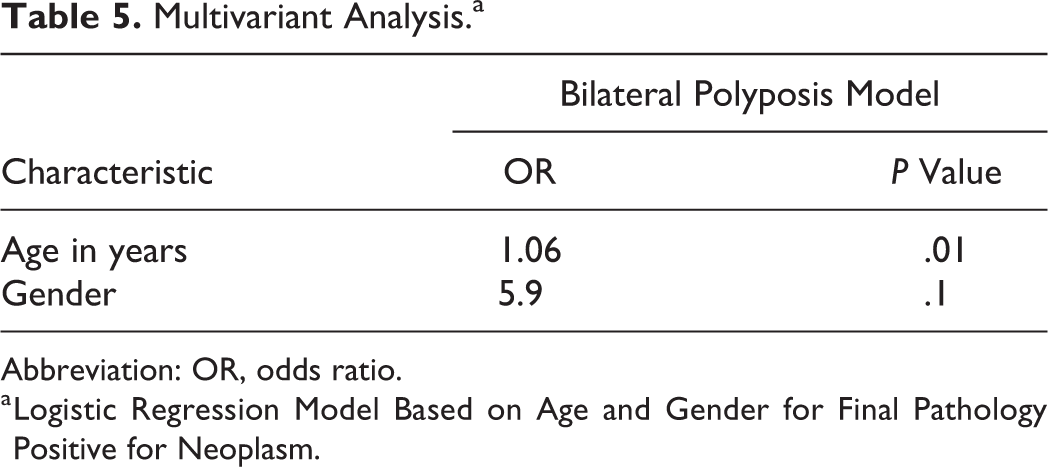
Abbreviation: OR, odds ratio.
a Logistic Regression Model Based on Age and Gender for Final Pathology Positive for Neoplasm.
Discussion
The final histopathological results obtained from 235 patients who presented with bilateral polyposis had a rate of 4.3% neoplasms, all of which were inverted papilloma. This is a surprisingly high rate of neoplastic disease among patients who were diagnosed with having chronic rhinosinusitis with bilateral nasal polyposis, and much higher than those reported in the literature (<1%). 8,14 Our search of the literature yielded only one study with results similar to ours. Busaba et al 17 reported that 3.5% of the polyps among 200 patients with bilateral nasal polyps were neoplasms, of which 2.5% were diagnosed with inverted papilloma.
Inverted papilloma is the most common benign epithelial tumor of the sinonasal tract. In spite of its benign histology, it behaves aggressively, with local destruction, a high recurrence rate, and malignant transformation. Tumor recurrence is thought to be related either to incomplete surgical excision or predisposed mucosa, and its rate is estimated to be as high as 53%. 18 Moreover, inverted papilloma is associated with malignancy in about 11% of the cases, either synchronously (7.1%) or metachronously (3.6%) 19 . Early diagnosis and surgical excision of inverted papilloma will result in better clinical outcome.
Clinical presentation (ie, unilateral polyposis or epistasis) has a major role in operative patient management. Considering the group of patients with nonsuspicious bilateral lesions (ie, following exclusion of atypical appearing polyps, such as vascular polyps, patients with a history of epistaxis, and any signs of bone erosion or soft tissue involvement in preoperative imaging), the importance of routine biopsy is further emphasized. In our study, an innocent-looking lesion was not a good predictor for inflammatory pathology since one-half of the neoplastic lesions had not originally been suspected of being neoplastic. Moreover, two-thirds of the lesions suspicious by the surgeon for neoplasm were found to be inflammatory. Therefore, surgeon assessment of a lesion based on appearance and imaging was not found to be a reliable tool for screening for lesions that should undergo a pathological examination.
Patients with neoplastic samples were significantly older than those with benign samples. Age was also weakly correlated with neoplasm, while gender was neither correlated nor significantly different between patients with neoplasms and those with inflammatory lesions. These findings are in contradiction to those of previous cohorts 8,11 in which neoplasms were not correlated with age or gender.
There is still no consensus about the necessity of referring samples from patients with bilateral polyposis to histologic evaluation. Sinonasal tumors are considered rare, comprising only 3% of all head and neck cancers and 1% of all malignancies, with a peak incidence in the fifth to seventh decades and with a male preponderance. However, the literature does not show any correlation in bilateral polyposis cohorts with age or gender. No guidelines for referral to histopathology have been established, and only 38% of otolaryngologists in the United Kingdom routinely send all nasal polyps for histologic examination. 5 The high price of performing a routine histopathological examination of each specimen is an important consideration, given that routine histopathologic examination of endoscopic material has little clinical value. Van den Boer et al 19 examined 1695 polyp samples of which 18 were inverted papillomas. In their results, all the neoplastic diseases were suspected, and the total cost of finding 2 unsuspected inverted papillomas was close to €80 000. Garavello et al reviewed 2147 8 cases and came to the same conclusion. 8 In a meta-analysis of 3772 patients, 14 only 18 unexpected benign (of which 16 were inverted papillomas) and 3 unexpected malignant diagnoses were identified, representing a proportion of 0.48% (0.42% of which were inverted papillomas) and 0.08%, respectively. The number needed to screen was 1258, and the pooled proportion for unexpected malignant finding was 0.00107. The cost of detecting one unexpected malignant diagnosis was estimated as being US$87 204.56 in that study. 14 In our cohort, 235 patients were biopsied, of which 10 had 10 suspected neoplasms. The estimated surgical cost calculated for routine histopathology biopsy for all patients and 10 patients requiring functional endoscopic sinus surgeries was estimated as €81 718.8. However, the calculated cost of late detection, reflected by a more complexed intraoperative course, increased surgical risk, and a higher likelihood for craniotomy, was estimated at €143 463.6. This resulted in estimated benefit in surgical costs of €61 745.
It is important to emphasize that information regarding the incidence of unexpected clinically significant diseases identified at routine nasal polyp histology is still very limited and controversial.
Our study has several limitations that bear mention. First, pathology sample was obtained from the prominent mass of polyps in the nasal cavity, and not all polyps resected were sent to final pathologic examination. Second, the number of neoplastic cases is small compared to other studies. However, even after exclusion of suspected lesions, we still have a high rate of neoplasms.
In conclusion, the findings of this study demonstrated that the rate of unexpected diagnosis in nonsuspicious bilateral nasal polyposis, although low, is higher than previously reported in the literature with IP as the most common pathology. Further demonstrated in this study was a positive correlation between an unexpected diagnosis and increasing patient age. Even though we are able to identify the nature of these lesions by means of clinical assessment and imaging studies, we believe the rate of unexpected neoplastic disease warrants a routine histopathologic examination for CRSwNP, especially in the elderly population.
Footnotes
Authors’ Note
Ahmad Safadi and Narin N. Carmel-Neiderman are joint first authors.
Acknowledgment
The authors kindly thank Esther Eshkol for her editorial support.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
