Abstract
Objectives
To study changes in factors influencing doctors’ career specialty choices between one and five years after graduation.
Design
Questionnaire survey.
Setting
UK.
Participants
A total of 10,473 doctors who replied to our surveys both one and five years after graduating from all UK medical schools between 1993 and 2008.
Main outcome measures
The importance of each of 12 specified factors in influencing the doctors’ choice of future specialty ‘a great deal’.
Method
Questionnaires by post and email.
Results
Enthusiasm for and commitment to the specialty was the greatest influence on career choice at year 1 (66%) and year 5 (74%). Domestic circumstances increased in importance more than any other factor (from 22.5% to 41.3%); 26% of doctors rated this as important in year 5 but not in year 1. Other factors which increased in importance from year 1 to year 5 included hours/working conditions, experience of the job so far and self-appraisal of own skills. There was an increase in the importance of promotion/career prospects, self-appraisal of own skills, student experience of subject and enthusiasm/commitment for more recent cohorts compared with older cohorts. Between years 1 and 5, there was a greater increase in the importance of domestic circumstances, hours/working conditions and eventual financial prospects for intending General Practitioners than for other doctors.
Conclusions
Doctors remain committed to their specialty between years 1 and 5, but the influence of domestic circumstances and hours and working conditions grew stronger.
Introduction
Doctors choose their future career paths while considering a range of factors. Medical students are highly influenced by other people’s perceptions, the opportunity for patient contact and working hours.1,2 Junior doctors consider human interest, enthusiasm for the job and self-appraisal of skills to be important.3,4 In the UK, doctors who qualified recently place more importance on domestic circumstances and enthusiasm for their chosen specialty than their predecessors. 3
Previous research has found that burnout and job satisfaction vary by career stage, with junior doctors reporting the most work–home conflicts and middle career doctors being most likely to want to leave medicine for reasons other than retirement. 5 The relative importance of factors which influence career choice may also vary by career stage. In the UK, a study found that doctors who were aged over 30 years when they started medical school rated ‘inclination before medical school’, ‘wanting a career that fits my domestic situation’ and ‘enthusiasm/commitment’ as more important than doctors who had been under 21 years old on entry. 3 A study in which over half of the sample were trainee surgeons found that duration of training, lifestyle during training and working hours became less influential on career choice once training had finished. 6 There is, therefore, research evidence that the factors that influence career choice change in their importance as doctors increase in seniority, but these studies have been mainly cross-sectional in design. It is important to know how these factors change from year to year within the same cohort of doctors by using a longitudinal design.
The aim of this paper is to report changes in the strength of factors influencing doctors’ choices of career specialty between one and five years after graduation. We also report these factors in relation to gender, ethnicity, age at entry to medical school and the chosen career specialty.
Methods
The UK Medical Careers Research Group surveyed the UK medical graduates of 1993, 1996, 1999, 2000, 2002 and 2008. We sent postal questionnaires to all graduates in these cohorts one and five years after qualification, making 12 surveys in all. Up to four reminders were sent to non-respondents. Further details of the methodology are available elsewhere. 7 Each questionnaire contained a range of questions on career choice and employment, together with questions on factors affecting career choice. For four surveys (the year one surveys of the cohorts of 1993, 1999, 2002 and the year 5 survey of the cohort of 2008), a small number of respondents completed a short form questionnaire which did not contain factor questions.
One and five years after graduation, each doctor rated the influence of each of 12 factors on their career choice. These factors were based on an initial set used in our studies in the 1970s, modified when new themes were identified by us, as either arising in comments made to us by doctors or as recurring themes in the research literature.
The doctors were asked to indicate whether each factor had influenced their choice of specialty ‘not at all’, ‘a little’ or ‘a great deal’. The 12 factors were: ‘Wanting a career that fits my domestic situation’, ‘Wanting a career with acceptable hours/working conditions’, ‘Eventual financial prospects’, ‘Promotion/career prospects’, ‘Self-appraisal of own skills/aptitudes’, ‘Advice from others’, ‘Experience of chosen subject as student’, ‘A particular teacher/department’, ‘Inclinations before medical school’, ‘Experience of jobs so far’, ‘Enthusiasm/commitment: what I really want to do’, and ‘Other reasons’.
We report standard summary statistics. To test statistical significance, we used McNemar’s test for changes and χ2 statistics. Each response was classified according to the year of graduation (cohort) to which the doctor belonged (1993, 1996, 1999, 2000, 2002 or 2008); the number of years after graduation at which the response was collected (one or five); gender; ethnic group (grouped by us into Asian, white and other); age at entry to medical school (under 21 years, 21–30 years and over 30 years); and actual specialty of work of the doctor in year 5 (grouped by us for analysis into four classes: hospital medical specialties, surgical specialties, general practice (GP) and other hospital-based specialties).
Results
Response rates
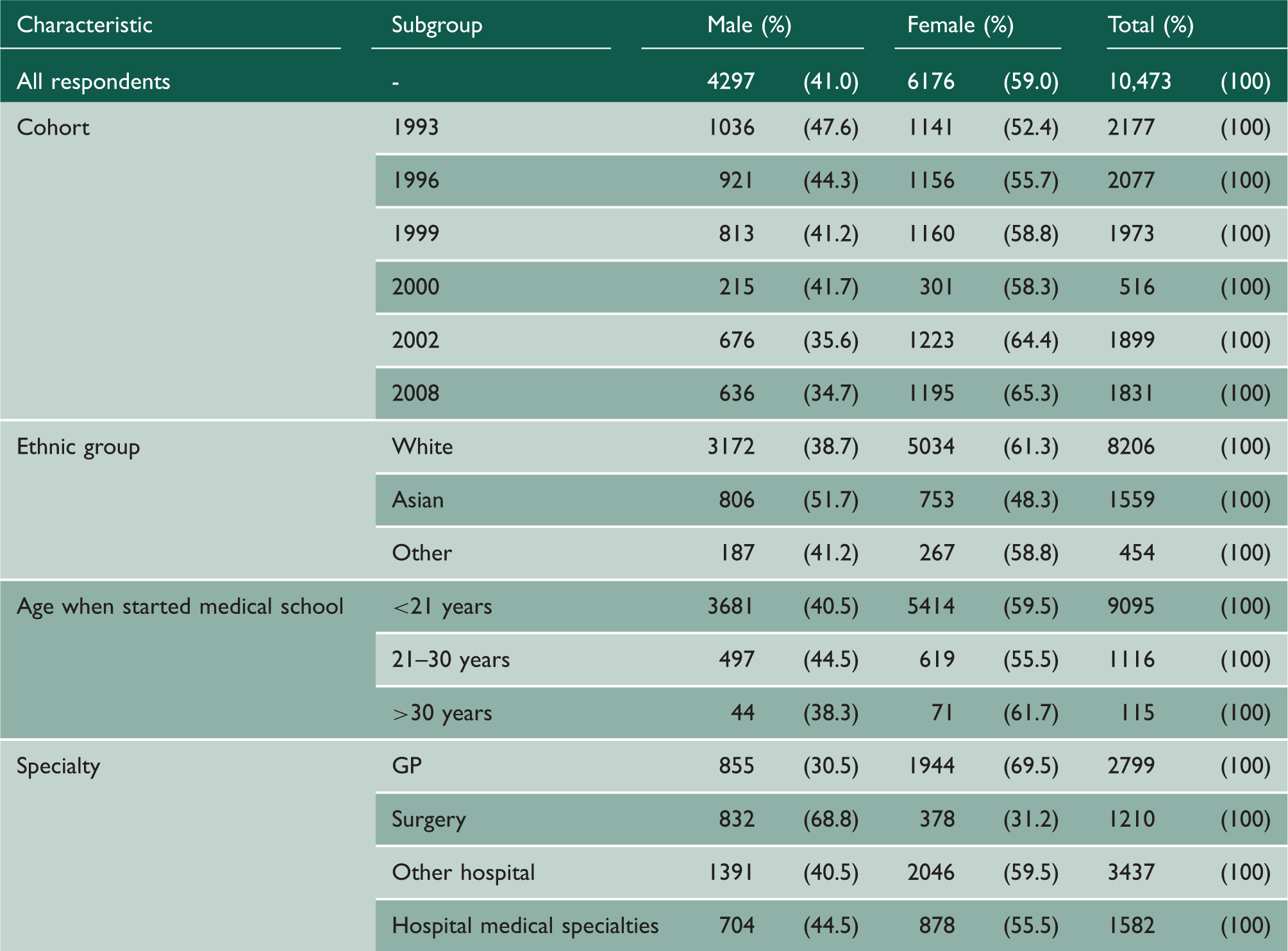
There were 27,403 UK medical graduates in the six cohorts. In year one, 17,332 doctors replied and in year five 15,533 doctors replied, respectively, 64.5% and 65.7% of the contactable populations, after excluding doctors who declined to participate, were known to have died or were untraceable. In all, 12,785 doctors replied on both occasions. However, 2312 of these doctors were excluded from our analysis because they completed short-form questionnaires which excluded factor questions (see ‘Methods’), reducing the number of useable responses to 10,473. Appendix 1 shows the demographics of the cohorts.
Factors influencing career choice in years 1 and 5
Factor changes from years 1 to 5 – percentage of respondents for which each factor had a great deal of influence on career choice.
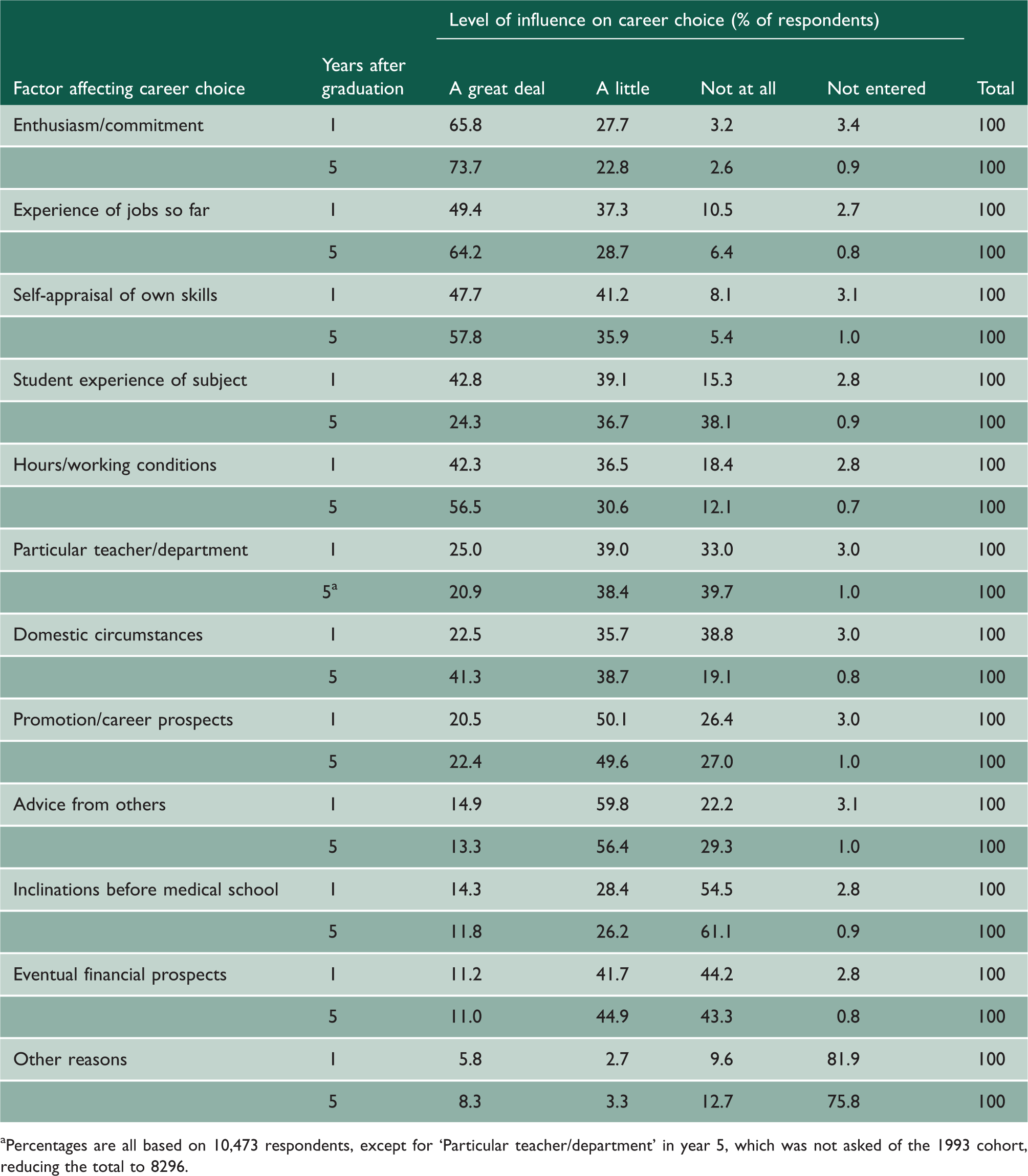
Percentages are all based on 10,473 respondents, except for ‘Particular teacher/department’ in year 5, which was not asked of the 1993 cohort, reducing the total to 8296.
In year 5, ‘Enthusiasm/commitment’ was still the most important factor and the percentage rating it as important had risen to 74%, followed by ‘Experience of jobs so far’ (increased from 49% to 64%) and ‘Self-appraisal of own skills/aptitudes’ (increased from 48% to 58%). ‘Domestic circumstances’ increased in importance more than any other factor (from 22.5% to 41.3%); Hours/working conditions’ also increased in importance from 42% to 57%. ‘Student experience of subject’ went down in importance (Table 1).
Changes in factors influencing career choice between years 1 and 5
Figure 1 summarises the percentages of doctors who held the same view from year 1 to year 5, and who rated each factor as more, or less, important in year 5 than in year 1. Numbers and statistical tests are given in Appendix 2, for which the categories ‘not entered’, ‘a little’ and ‘not at all’ have been combined as the category ‘unimportant’, and ‘a great deal’ has been described as ‘important’.
Percentages of doctors by factor ratings at one year and five years.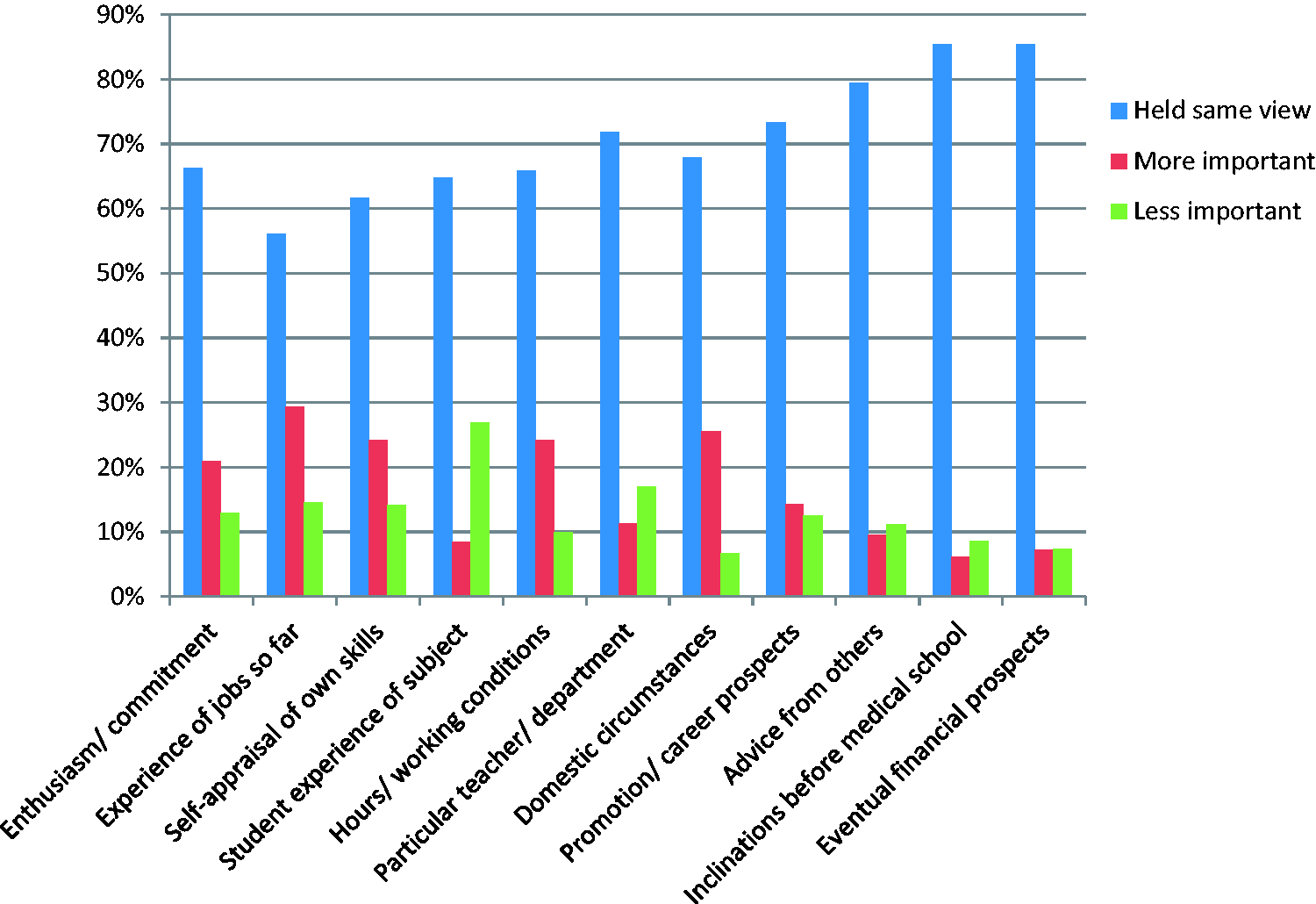
All factors changed significantly in importance from years 1 to 5, with the exception of ‘Eventual financial prospects’, but some generated larger test statistics (Appendix 2) reflecting larger percentage changes from years 1 to 5. Of the factors, ‘Domestic circumstances’ gained in importance most notably in year 5: 25.5% of doctors rated this as important in year 5, but not in year 1, and only 6.6% rated this factor as important in year 1, but not in year 5. ‘Student experience of subject’ decreased considerably in importance in year 5. ‘Hours/working conditions’, ‘Experience of the job so far’, ‘Self-appraisal of own skills’ and ‘Enthusiasm/commitment’ also increased in importance from year 1 to year 5. Changes in the importance of other factors were more modest.
Characteristics of doctors whose views of each factor changed between year 1 and year 5
The views of many doctors stayed the same in both years 1 and 5 (Figure 1). We decided to focus on doctors whose views of each factor changed between year 1 and year 5, and to investigate how, for those whose views changed, the likelihood of a positive rather than negative change of view varied by gender, cohort, ethnicity, age and specialty (in year 5).
A binary variable for changes in factors influencing career choice between years 1 and 5 was created by omitting cases where there had been no change between years 1 and 5. Each factor had either ‘increased in importance’ or ‘decreased in importance’ by year 5. Therefore, the following analysis, undertaken separately for each factor in turn, only includes doctors whose ratings of the factor changed between years 1 and 5.
Percentages of doctors whose views changed between years 1 and 5, for whom each factor became more important.
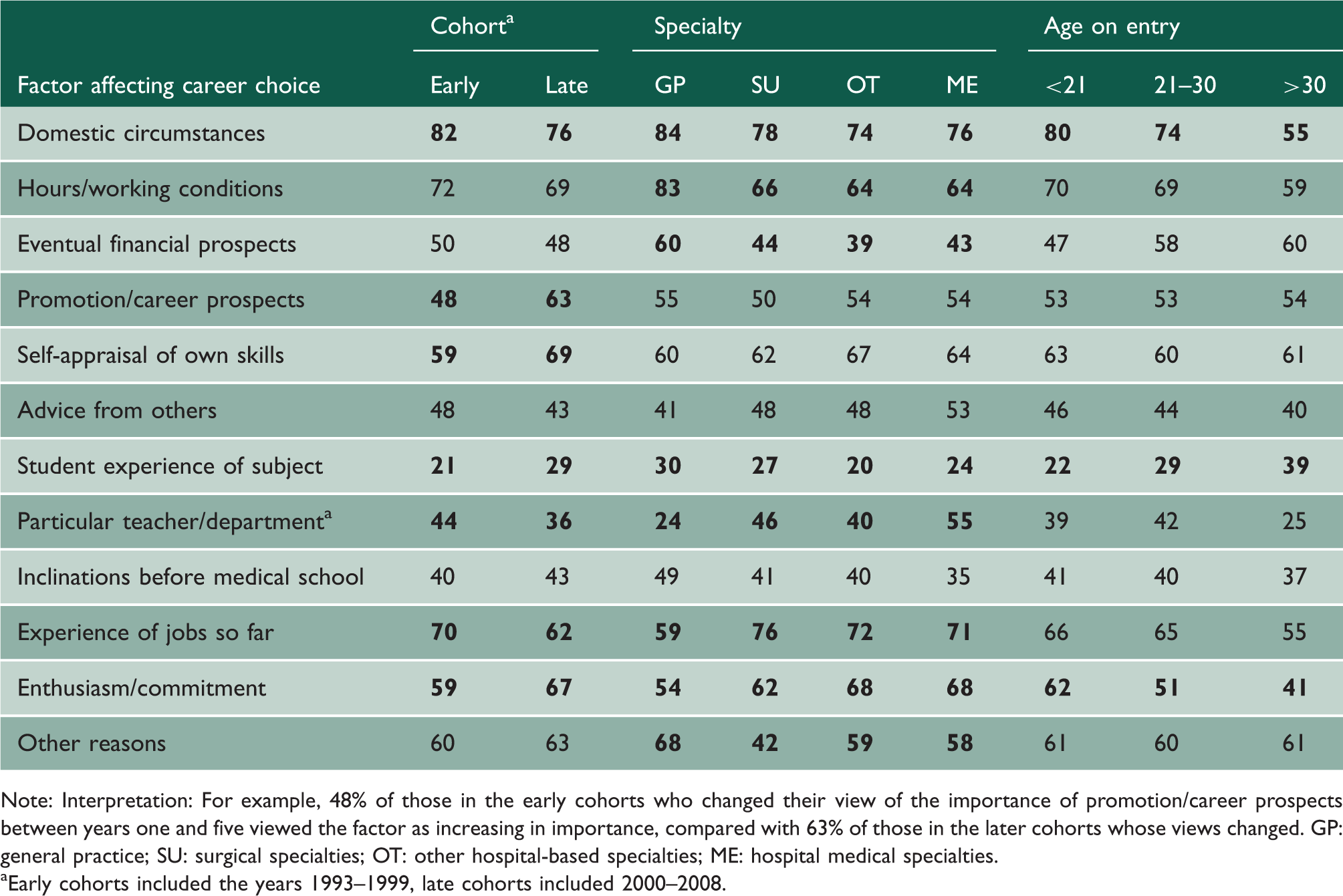
Note: Interpretation: For example, 48% of those in the early cohorts who changed their view of the importance of promotion/career prospects between years one and five viewed the factor as increasing in importance, compared with 63% of those in the later cohorts whose views changed. GP: general practice; SU: surgical specialties; OT: other hospital-based specialties; ME: hospital medical specialties.
Early cohorts included the years 1993–1999, late cohorts included 2000–2008.
Cohort
‘Promotion/career prospects’, ‘self-appraisal of own skills’, ‘student experience of subject’ and ‘enthusiasm/commitment’ became more important between years 1 and 5 for the later cohorts (i.e. those qualifying between 2000 and 2008) than for the earlier cohorts (i.e. those qualifying between 1993 and 1999). ‘Domestic circumstances’, ‘experience of jobs so far’, and ‘a particular teacher/department’ became more important between years 1 and 5 for the early cohorts than for the later cohorts.
Specialty chosen
For 8 of the 12 factors, there were differences by specialty group (Table 2). ‘Domestic circumstances’, ‘hours/working conditions’ and ‘eventual financial prospects’ grew in importance more for GPs than for other doctors. ‘Experience of jobs so far’ and ‘enthusiasm/commitment’ became less important for GPs than for other doctors. ‘Particular teacher/department’ became more important between years 1 and 5 for doctors working in the hospital medical specialties (54.6%) compared with other specialties.
Age
‘Domestic circumstances’ increased in importance between years 1 and 5 more for doctors who had started medical school aged under 21 years than for doctors who started aged 21–30 years or those who started over 30 years. Similarly, ‘Enthusiasm/commitment’ became more important for doctors who had started medical school aged less than 21 years than for doctors who started at an older age.
Multivariable modelling
For each factor, multivariable modelling was undertaken using only those characteristics (from cohort, age and specialty) which were shown as significant in Table 2. The results are shown in Appendix 4. In the multivariable models, all characteristics which were found to be significant in the univariable analysis in Table 2 remained significant. Odds ratios and 95% confidence intervals are shown in Appendix 4.
Discussion
Main findings
Enthusiasm/commitment had the greatest influence on doctors’ career choice in year one. Other important factors included experience of jobs so far, self-appraisal of own skills/aptitudes, student experience of subject and hours/working conditions. Enthusiasm/commitment was still the most important influence in year 5. Domestic circumstances and working hours increased in importance between years 1 and 5 more than any other factor.
Concentrating only on those doctors whose view changed between years 1 and 5, ‘domestic circumstances’ was rated as important in year five but not in year one by one-quarter of doctors. Other factors which increased in importance included hours/working conditions, experience of the job so far, self-appraisal of own skills and enthusiasm/commitment.
Between years 1 and 5, there was a rise in the importance of promotion/career prospects, self-appraisal of own skills, student experience of subject and enthusiasm/commitment among later cohorts (those who qualified in the 2000s) compared with earlier cohorts (those who qualified in the 1990s). GPs, when compared with other doctors, attached more importance to domestic circumstances, hours/working conditions and eventual financial prospects by year five, and less importance to experience of jobs so far and enthusiasm/commitment.
Strengths and weaknesses of the study
Other studies which have researched factors affecting career choice have been mainly cross-sectional. This study’s key strength is its longitudinal design. This enables us to understand how factors change from year to year at the level of the individual. Alongside data on perceptions, we also collected data on doctors’ actual jobs. We could therefore compare doctors by specialty group five years after graduation. This is a large study, which covers all of the UK’s medical schools, and spans a wide breadth of cohorts from 1993 to 2008. Response rates were good. As with all surveys, there is the possibility of responder bias.
Comparison with existing literature
Our finding that enthusiasm for the job is the greatest influence upon career choice at both years 1 and 5 is consistent with other studies.3,4 We found that domestic circumstances and working hours increased in importance during the early postgraduate years. This fits with other findings that junior doctors report the most work–home conflicts, and middle career doctors are most likely to want to leave medicine: junior doctors, unhappy with their work–life balance, are surely more likely to increase the importance they place on domestic factors. 5 Other research found lifestyle and working hours to become less important to doctors with more than four years of clinical experience. 6 However, over three-quarters of the study’s participants had decided upon a surgical career, and 64% were male doctors and so the samples were quite different.
We found that GPs increase the importance they place on domestic circumstances, hours/working conditions and eventual financial prospects between years 1 and 5. In Switzerland, a study which looked at interventions to promote primary care found that primary care physicians indicated the highest acceptance with an increase in reimbursement. 8
Implications
Demographics of responding doctors in the study.
Numbers and percentages rating each factor ‘a great deal’ in years 1 and 5.
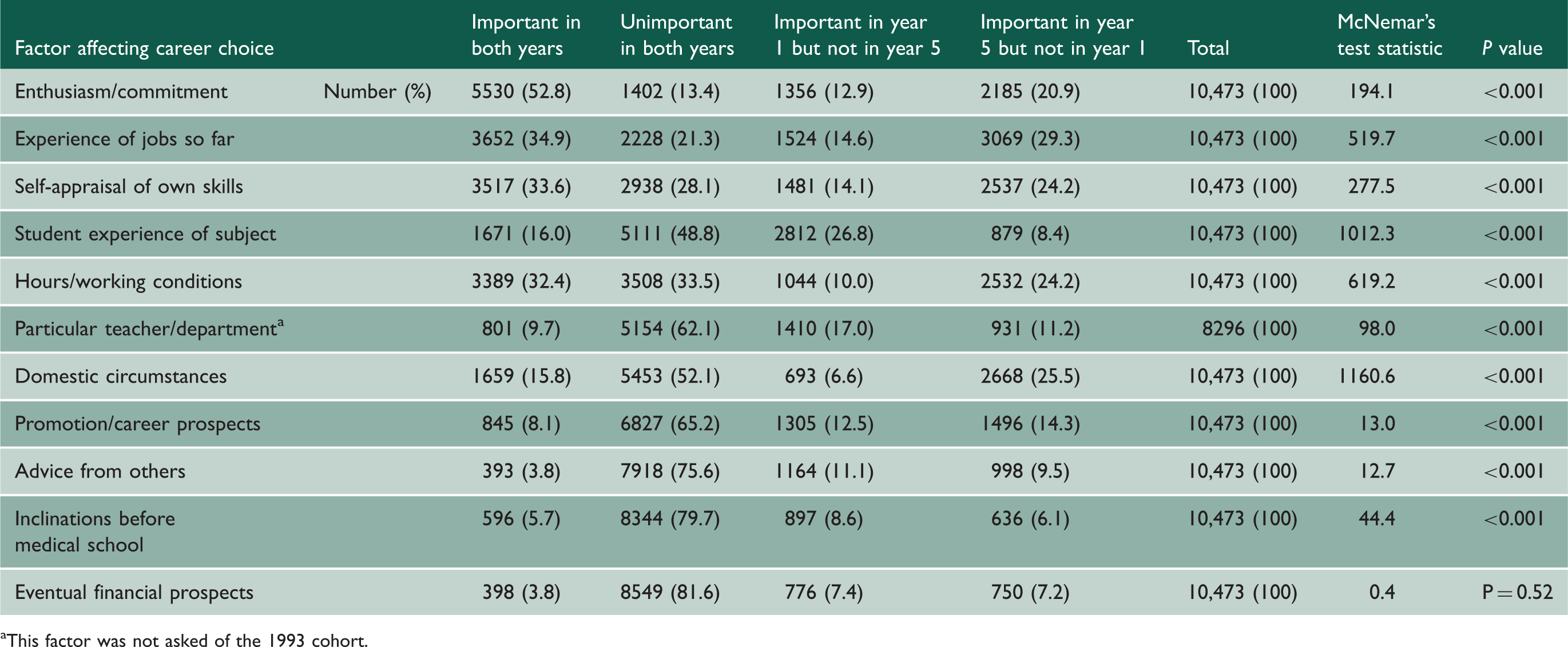
This factor was not asked of the 1993 cohort.
Numbers of doctors whose views changed between years 1 and 5, who became more positive about each factor.
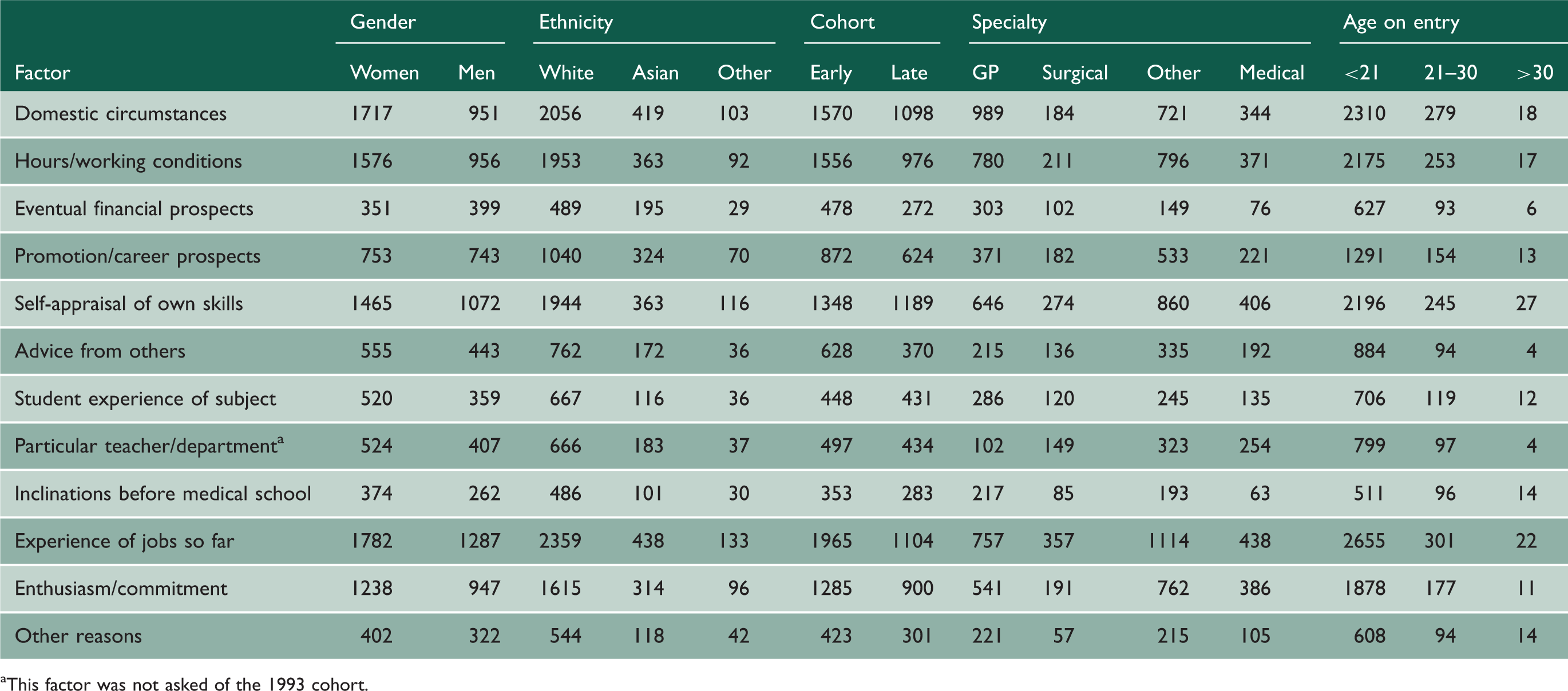
This factor was not asked of the 1993 cohort.
Logistic regression models for the factors: odds ratios with 95% confidence intervals.
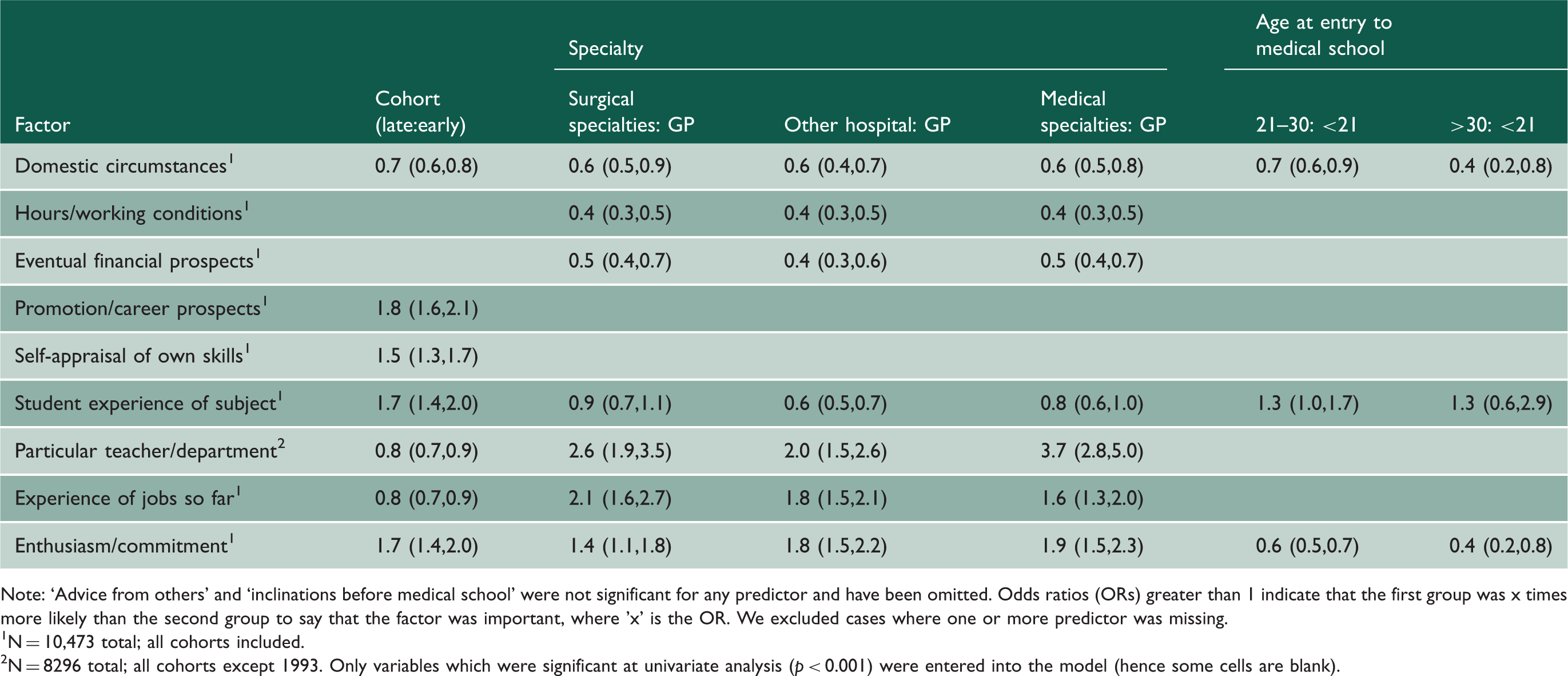
Note: ‘Advice from others’ and ‘inclinations before medical school’ were not significant for any predictor and have been omitted. Odds ratios (ORs) greater than 1 indicate that the first group was x times more likely than the second group to say that the factor was important, where 'x' is the OR. We excluded cases where one or more predictor was missing. 1N = 10,473 total; all cohorts included. 2N = 8296 total; all cohorts except 1993. Only variables which were significant at univariate analysis (p < 0.001) were entered into the model (hence some cells are blank).
