Abstract
Clinical learning environment play a vital role in bridging theory with practice, equipping nursing students with essential skills for patient care and support their smooth transition into the nursing workforce. To assess Palestinian nursing students’ perceptions of clinical learning environment and supervision. A total of 308 undergraduate nursing students were conveniently recruited from Arab American University-Palestine for this descriptive cross-sectional study. Data collection utilized the Arabic version of the Clinical Learning Environment and Supervision plus Nurse Teacher scale. In general, nursing students expressed positive perceptions regarding their clinical learning environment (M = 130.56 ± 21.03), with the “supervisory relationship” and “role of nurse teacher” scoring highest (M = 3.85 ± 0.82 each). Conversely, the lowest rating was observed for “leadership style of the ward manager” (M = 3.8 ± 0.84). Fourth-year students and those trained in public hospitals showed significantly more positive perceptions (P < .001). Furthermore, students with higher professional satisfaction had more positive perceptions of the clinical learning environment (P < .001). The positive perceptions of Palestinian nursing students underscore the importance of the supervisory relationship and nurse teacher. However, finding suggest an area for improvement in the leadership style of the ward manager, emphasizing the necessity for strengthened partnership between nursing faculties and healthcare facilities. These insights expand our understanding of student perceptions and stress the importance of addressing these concerns to adequately prepare students for professional practice.
Clinical placement considers the central part of nursing education, providing students with valuable opportunities to employ theoretical knowledge in real-world practice
The study identifies areas for improvement within the clinical learning environment, informing future initiatives aimed at enhancing the overall learning experience for nursing students in Palestine.
Nursing educators should prioritize the cultivation of supportive supervisory relationships and improvement the role of nurse teachers within CLE.
Nursing faculties and Healthcare institutions need to collaborate closely to address the identified inadequacies in the leadership style of ward managers.
Introduction
In the ever-evolving environment of healthcare, nurse educators challenged to adequately preparing newly graduated nurses to fulfill the requirements of the profession. The integration of theory and practice is vital in nursing education, with clinical learning acting as a cornerstone of students’ educational experiences. 1 Clinical education not only equips nursing students with essential knowledge and skills required for patient care but also support their smooth transition into the nursing staff. 2
Clinical placement considers the central part of nursing education, providing students with valuable opportunities to employ theoretical knowledge in real-world practice. 3 Within clinical environments, students benefit from supervision and guidance from qualified healthcare professionals to support their skill development.3 -5 Additionally, hands-on engagement in direct patient care not only improves students’ clinical competency but also gains insight into the varied roles of nursing professionals. 6 However, the effectiveness of clinical placement relies significantly on the quality of the learning environment, which contributes to facilitate achieving student learning outcomes and competently qualifying them for nursing career.7 -9
As nursing education constantly changing to meet the healthcare requirements, the significance of the clinical learning environment for substantial learning experiences cannot be inflated. 2 The clinical environment serves as a vital arena in allowing students to link theory with practice, preparing them with competencies, positive attitudes, and critical thinking abilities essential for competent nursing practice.10,11 The favorable clinical learning environment not only shapes nursing students’ roles but also directly effects patient outcomes. Within this environment, students develop essential skills, confidence, and empathy under supportive mentorship, resulting in improved nursing care and ultimately leading to enhanced patient outcomes.
The clinical learning environment (CLE) is a complex atmosphere that involves an interactive network of several factors within clinical settings that impact learning outcomes.12,13 The CLE is instrumental in enabling students to attain learning objectives, acquisition of clinical competencies, development of professional identities, and immersion in professional socialization.14 -16
The complex nature of the CLE involves interactions between nursing students, clinical instructors, healthcare professionals, patients, and colleagues, which are vital for professional development and preparation for real-world practice.3,17,18 Creating a nurturing environment that supports effective communication between students and supervisors is imperative for successful clinical learning. 19 Furthermore, creating favorable pedagogical atmospheres within clinical settings encourage student engagement and facilitate open communication. 20 Additionally, the leadership styles of ward managers have a notable impact on CLE, with effective leadership improves students’ skill acquisition and critical thinking abilities.6,21 Similarly, the role of clinical instructor is vital in ensuring students achieve their learning outcomes, connecting the theoretical knowledge with practical application, and ultimately increasing student satisfaction with clinical placements. 3 Furthermore, the premises of care on the ward need to be clearly defined and supportive to timely sharing of patient care information to improve the quality of the CLE. 21
Considering the crucial role of clinical learning in nursing education, it is imperative to continually monitor and enhance the CLE. Extensive research has emphasized the relationship between the CLE’s quality and nursing students’ satisfaction and overall well-being.6,8,22 -24 However, negative experiences within the CLE can significantly hinder students’ attainment of clinical learning outcomes, thereby affecting their satisfaction with the nursing profession and potentially worsening the global nursing shortage.10,25 These negative experiences often originate from an unfavorable environment characterized by factors such as under-appreciation, negative feedback, pressure to meet high expectations, and inadequate clinical supervision.26 -30 Collectively, these findings underscore the critical role of a supportive environment in nurturing positive learning experiences and preparing nursing students for professional practice. Therefore, Assessing the CLE, particularly within the clinical placement, is crucial for evaluating the effectiveness of clinical education elements in nursing programs. 31 Understanding how nursing students view their environment is vital for tailoring approaches to support their learning and promote their overall clinical placement experiences. 32
Although there is robust empirical evidence from studies conducted in Arabic and Western countries emphasizing the significance of favorable CLE and their impact on the well-being of nursing students, research specifically focusing on the CLE and its effect on students’ outcomes in Palestine remains limited. Only 1 study conducted by Toqan et al 27 to investigate sources of stress and coping behaviors during first clinical training among nursing students, which is limited to first-year students. However, awareness of the importance of the CLE and the role of supervisors and teachers among Palestinian nursing students remains limited. Given the mandatory nature of clinical placements for all nursing students, exploring their perceptions of these environments is imperative. Therefore, the aim of this study to assess Palestinian nursing students’ perceptions of their CLE and supervision. These findings can inform nursing faculties and healthcare insinuation in creating a supportive CLE that addresses students’ learning and socializing needs.
Aim
The aim of this study was to assess Palestinian nursing students’ perceptions of their clinical learning environment and supervision.
Methodology
Design
The study employed a descriptive cross-sectional design. Due to the lack of clear findings on nursing students’ perceptions of the CLE in Palestine. Utilizing this design aims to establish foundational data on their perceptions within this setting. Additionally, cross-sectional studies offer efficiency and cost-effectiveness by collecting data at 1 point or over a brief period.
Setting
The study took place within the Nursing Faculty at Arab American University in Palestine (AAUP). This faculty offers a comprehensive 4-year undergraduate nursing program, culminating in the award of a baccalaureate degree in nursing. Clinical education commences at AAUP with the first clinical placement during the spring semester of the first year. The oversight of clinical nursing education is shared by both faculties and lecturers, collectively known as “nurse educators.” However, there exists a notable shortage of nurse educators relative to the student population. To address this shortfall, nurses employed in hospitals with bachelor’s or master’s degrees in nursing are recruited as part-time clinical educators, referred to as “clinical instructors.” These instructors play an essential role in delivering clinical education and training to students during their clinical practice placement. Each clinical instructor is tasked with supervising and evaluating a group of 6 students. 27
Participants
The study involved undergraduate nursing students enrolled at AAUP during the 2022 to 2023 academic year. Raosoft software was utilized to determined Sample size based on a population of 1500 students, with a confidence interval of 95% and a 5% margin of error, resulting in sample size of 306 students. To accommodate potential attrition, enrollment was increased to 340 students. Participants were recruited through convenience sampling to ensure a diverse representation across academic levels and clinical experiences. Inclusion criteria necessitated recent involvement in clinical practice, willingness to participate, and second, third, or fourth-year student status. Conversely, exclusion criteria comprised incomplete responses and a lack of willingness to participate. First-year students were excluded because they have limited experience in clinical settings, which could affect their ability to provide comprehensive perspectives on the CLE.
Instruments
The instrument consisted of 2 parts. The first part contained students’ characteristics, including gender, age, academic year, and professional satisfaction.
The second part introduced the Clinical Learning Environment, Supervision, and Nurse Teacher Scale (CLES + T), originally developed by Saarikoski et al 12 and translated into Arabic by Guejdad et al 33 These variables were selected based on literature review and their relevance to understanding nursing students’ perceptions of the CLE, focusing on individual characters and main aspects of the educational experience. The Arabic version of CLES + T consist of 34 items across 5 subscales, each reflecting vital aspects of the CLE: “Supervisory relationship,” “Pedagogical atmosphere on the ward,” “Role of the nurse teacher,” “Leadership style of the ward manager,” and “Premises of nursing on the ward.” Responses were collected utilizing a 5-point Likert scale, ranging from totally disagree (1) to totally agree (5). A higher score indicating a more positive CLE and supervision. Both the original and Arabic version of the CLES + T scale displayed satisfactory validity and reliability.12,33 The reliability of the Arabic version of CLES + T was evaluated using Cronbach’s alpha, yielding a coefficient of .93 for the total scale and ranging from .71 to .92 for the subscales. 33 In this study, it was 0.94 for total scale and ranging from 0.87 to 0.94 for subscale.
Data Collection and Ethical Consideration
Prior to data collection, ethical approval was obtained from AAUP. Data collection took place at the end of the fall semester—2022/2023, with participants filling out questionnaires in lecture rooms following classes. Data collection spanned 4 weeks in December 2022, facilitated by 2 trained volunteers to minimize researcher bias. Prior to participation, the study’s objectives were thoroughly explained by principal investigator, ensuring students were fully aware of their right to withdraw from study at any point without facing any sequences. Students who agreed to participate were requested to sign an informed consent, and were assured that their voluntary involvement would not impact their educational experience. Data were collected and stored in compliance with data protection regulations. Permission to use Arabic version of the CLES + T was obtained from author.
Statistical Analysis
Data were analyzed using SPSS version 26. Skewness and kurtosis were assessed to determine the normality and distribution of the data. Descriptive statistics were utilized to summarize the students’ characteristics and the CLES + T subscales. inferential statistic including ANOVA and independent t-test was employed to explore the relationship between student characteristics and the CLES + T subscales. A P-value of <.05 was considered statistically significant.
Result
Out of the 340 distributed questionnaires, 317 were returned, yielding a response rate of 93.2%. After excluding 9 questionnaires with significant missing data, 308 questionnaires were suitable for analysis.
Students’ Characteristics
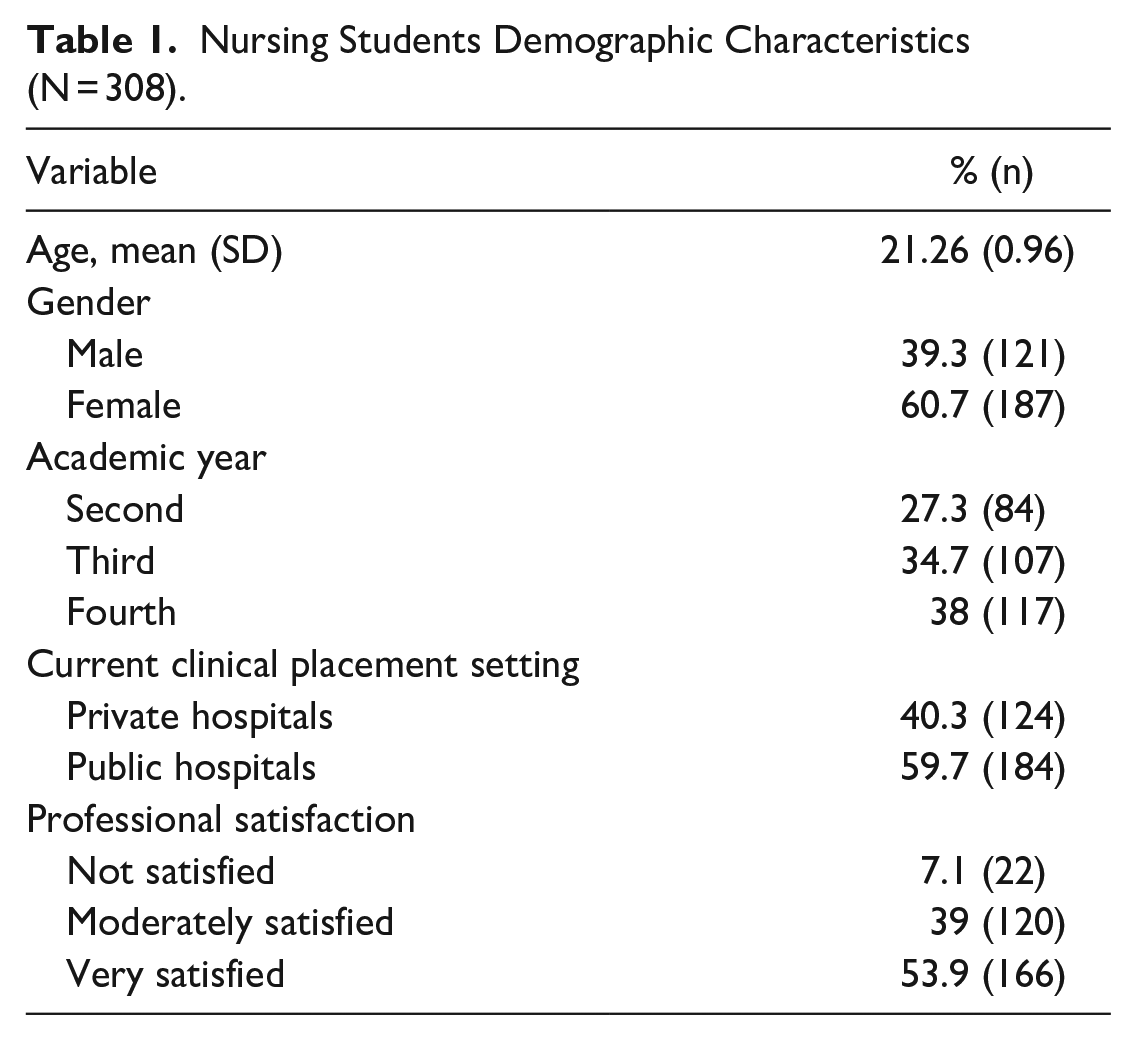
The study sample comprised 308 nursing students, aged between 20 and 23 years, with an average age of 21.26 years. Among these students, 60.7% (n = 187) were female, and 38% were belonged to the fourth year. They were undergoing clinical placements in both public (n = 184; 53.7%) and private (n = 124; 40.3%) hospitals. The majority of students expressed high professional satisfaction, with 66.1% (n = 166) being very satisfied. Detailed demographics are presented in Table 1.
Nursing Students Demographic Characteristics (N = 308).
Descriptive Results of the CLES+T and Subscale
The findings showed that nursing students generally had a moderately positive view of their CLE, as indicated by an overall mean score of 3.84 (130.56 out of 170) on the CLES + T scale. The mean scores across the 5 CLES + T subscales ranged from 3.8 to 3.85 (Table 2), indicating moderately positive perceptions among the students. Specifically, the “Pedagogical atmosphere on the ward” subscale received a mean score of 3.84, suggesting a moderate level of satisfaction with the CLE. The “Supervisory relationship” and “Role of the nurse teacher in clinical practice” subscales achieved the highest mean scores of 3.85, indicating higher satisfaction levels. Conversely, the “Leadership style of the ward manager” and “Premises of nursing on the ward” subscales obtained lower mean scores of 3.80 and 3.83, respectively, indicating areas for improvement (Table 2).
Clinical Learning Environment Scale and Its Sub-Dimensions Mean Scores Based on Demographic Characteristic.

M = Mean; SD = standard deviation.
P < .001.
The findings also revealed significant differences in nursing students’ perceptions of the CLE based on their year of education (P < .001), current clinical placement settings (P < .001), and professional satisfaction (P < .001. However, no statistically significant differences were found based on gender (P = .71; Table 3).
Comparison Between the Clinical Learning Environment and Students’ Characteristics. (N = 308).

M = Mean; SD = standard deviation.
P < .001.
The Supervisory Relationship
Regarding to supervisory relationship subscale, the study showed that nursing students generally satisfied with the supervisory relationship. The average scores for individual items ranged from 3.72 to 3.94. Notably, the item “Mutual respect and approval prevailed in the supervisory relationship” received the highest score of 3.94, suggesting a strong sense of mutual respect between students and their supervisors. Similarly, “My supervisor showed a positive attitude toward supervision” and “There was mutual interaction in the supervisory relationship” obtained high scores of 3.93 and 3.91, respectively, indicating positive dynamics between students and supervisors. However, the item “I continuously received feedback from my supervisor” received the lowest score of 3.72, suggesting that there is room for improvement in the provision of continuous feedback by supervisors.
Pedagogical Atmosphere
The students generally expressed a positive perception of the pedagogical atmosphere on the ward, with an average score of 3.84. Notably, they viewed that the ward as conducive place for learning, with a mean score of 3.92. The item “There were sufficient meaningful learning situations on the ward” received the highest mean score. However, students’ responses were less favorable about items such as “The staff were easy to approach” (3.80), “The staff were generally interested in student supervision” (3.78), and particularly “During staff meetings, I felt comfortable taking part in the discussions” (3.74).
The Role of the Nurse Teacher
The evaluation of the “Role of the Nurse Teacher” subscale showed average scores ranging from 3.78 to 4.92, with an overall mean of 3.85. The items “In our common meetings, I felt we were colleagues” received the highest mean score of 3.92, indicating a strong sense of collaboration. However, the items “The nurse teacher was like a member of the nursing team” and “Focus on the meetings was on my learning needs” received the lowest scores of 3.78.
Additionally, items such as “The nurse teacher was able to provide expertise to the nursing team,” “The nurse teacher and the clinical team worked together to support my learning,” and “The common meetings between myself, mentor, and NT were a comfortable experience” received slightly lower scores of 3.86, 3.85, and 3.85, respectively.
Overall, the “Role of the Nurse Teacher” subscale scored high among all subscales. Items like “The nurse teacher was capable of operationalizing the learning goals of this placement” (3.87) and “In my opinion, the nurse teacher was capable of integrating theoretical knowledge and everyday practice of nursing” (3.89) receiving the highest mean scores. However, the item “The nurse teacher helped me to reduce the theory-practice gap” had a slightly lower mean score of 3.88, indicating a more varied response from the students.
Leadership Style of the Ward Manager
The “Leadership style of the ward manager” subscale received the lowest scores among all subscales based on student responses. The item “The ward manager was a team member” had the lowest mean score of 3.78, while “The ward manager regarded the staff on his/her ward as a key resource” had the highest mean score of 3.82. This suggests a need for further exploration into the dynamics of leadership within clinical settings.
Premises of Nursing on the Ward
The “Premises of nursing on the ward” subscale receive somewhat low score. The mean scores for the items related to "Premises of nursing on the ward" ranged from 3.71 to 3.98, with an overall mean of 3.83. The item “The ward’s nursing philosophy was clearly defined” received the lowest mean score of 3.71, while “Documentation of nursing (eg, nursing plans, daily recording of nursing procedures, etc.) was clear” obtained the highest mean score of 3.98.
The analysis of nursing students’ perceptions across various subscales of the CLES + T revealed statistically significant differences based on their current clinical placement settings (P < .001), year of education (P < .001), and professional satisfaction (P < .00). However, gender did not show any statistically significant differences in the mean scores of CLES + T subscales (P > .05; Table 2).
Discussion
Assessing nursing students’ perspectives on their CLE, supervision, and interactions with nurse teachers is essential for nursing administrators to ensure the effectiveness and satisfaction of educational programs. The aim of this study was to assess Palestinian nursing students’ perceptions of their clinical learning environment and supervision.
The findings of the present study showed that Palestinian nursing students expressed a favorable perception of their CLE, consistent with previous research.6,7,22,23,34 -38 These findings underscore the supportive role of the CLE in nurturing nursing students’ confidence, facilitate clinical skill development, and improving critical thinking abilities.10,11
Specifically, our results revealed that the majority of nursing students had a positive perception of their CLE, with an average CLES + T score of 3.84. This score exceeds those reported in comparable studies conducted in Saudi Arabia, China, Spain, and Ghana.7,22,23,35,36,39 -41 However, Strandell-Laine et al 37 reported a higher mean score of 4.01 among graduate nursing students across European countries. This variation emphasizes the potential diversity in CLE, influenced by cultural norms, healthcare system frameworks, and educational methodologies.
Our study revealed interesting insights into nursing students’ perceptions of their CLE across CLES + T subscales. Notably, the “Supervisory relationship” and “the role of nurse teacher” received the highest scores, followed closely by the “pedagogical atmosphere on the ward.” Conversely, students evaluated the “Premises of nursing on the ward” and “Leadership style of the ward manager” as the lowest scored subscales. In a Saudi Arabian context, Al-Anazi et al 39 reported opposing findings, with high scores recorded for the “Leadership style of the ward manager” and “premises of nursing on the ward,” while the “pedagogical atmosphere on the ward” and “role of nurse teacher” received lower scores. Similarly, Aljohni et al 35 found different results among Saudi internship nursing students, where the “role of nurse teacher” and “leadership style of the ward manager” rated the highest, while the “supervisory relationship” and “Premises of nursing on the ward” scored the lowest.
These findings resonate with those reported by Rodríguez-García et al 23 in Spain, where nursing students evaluated the “supervisory relationship” and “pedagogical atmosphere on the ward” highest and the “role of nurse teacher” lowest. In Ghana, Abuosi et al 36 observed a different trend, with nursing students score the “leadership style of the ward manager” highest, followed by the “role of nurse teacher,” while the “pedagogical atmosphere” and “Premises of nursing on the ward” obtained lower scores. Moreover, study by Strandell-Laine et al 37 involving nursing students from 6 European nations consistently reported high ratings for the “pedagogical atmosphere” and “supervisory relationship,” while “leadership style of the ward manager” and “Premises of nursing on the ward” obtained lowest scores.
The lower mean scores for the “Leadership style of the ward manager” and “Premises of nursing on the ward” subscales pinpoint areas necessitating improvement from nursing students’ perspectives. Effective leadership in the CLE involves clear communication, student involvement in decision-making, and robust mentorship. Improving these aspects through structured communication, participative leadership, and strong mentorship programs will improve the CLE and better prepare nursing students for their professional roles. Additionally, the physical environment of the wards is vital; issues like outdated layouts, equipment shortages, and inadequate safety and comfort can hinder learning and increase student stress. Addressing these factors requires a thorough assessment of the physical environment, ensuring necessary supplies, and enhancing safety and comfort, ultimately improving the overall CLE.
Additional exploration into these findings, it becomes evident that nursing students’ perceptions of their CLE are shaped by a variety of circumstantial factors, including cultural norms, educational systems, and specific clinical settings. For instance, in Saudi Arabia, studies by Al-Anazi et al 39 and Aljohni et al 35 exhibited higher ratings for aspects related to leadership and premises of nursing, potentially representing cultural and organizational norms within Saudi Arabian healthcare settings.
In contrast, studies in Spain, Ghana, and European countries23,36,37 showed diverse forms, where “supervisory relationship” and “pedagogical atmosphere” received higher ratings, while “leadership style of the ward manager” and “Premises of nursing on the ward” were rated lower. These differences emphasize the necessity for tailored strategies to enhance nursing education and enhance students’ learning experiences, taking into consideration the unique contextual factors shaping their perspective. Further investigation into the factors contributing to these differences could yield valuable insights for both nursing education and practice.
The comparison of mean scores with students’ characteristics provides valuable observation into the various factors influencing students’ perceptions. These factors encompass the student’s year of education, professional satisfaction, and clinical placement settings. In this study, fourth-year nursing students indicated a more positive perception of their CLE in comparison to other students. This finding is consistent with previous research indicating that students with increased clinical exposure tend to view their environment more positively.8,22,34,39 This positive perception may be due to several factors. By their fourth year, students have become more familiar with the clinical setting, enabling them to navigate and utilize resources more effectively. They have also established stronger relationships with the clinical staff, which can lead to better support and mentorship. Additionally, the advanced stage of their education means they have improved their clinical skills and confidence, making them more comfortable and competent in the clinical environment. However, inconsistent to these findings, previous studies have showed that senior nursing students were less satisfied with the CLE.23,30,41 -43
In terms of professional satisfaction, our study confirms a significant association between professional satisfaction and nursing students’ perceptions of the CLE. Specifically, those who reported high satisfaction with their profession inclined to view their CLE more positively. This finding aligns with prior research,3,43 highlighting the influence of students’ knowledge, motivation, and professional perception on their adaptation and success in clinical practice.3,44 Additionally, maintaining a positive perspective has been related to decreased stress and increased satisfaction with the clinical experience.3,30 Our study emphasizes the importance of considering students’ professional satisfaction in shaping their perceptions of the CLE, which in turn affects their overall clinical experience and success. It is important to address the factors contributing to professional satisfaction among nursing students, as they carry significant implications for their educational outcomes and well-being.
Regarding clinical placement settings in Palestine, nursing students underwent clinical training in both private and public hospitals. Our result shows that students in public hospitals perceive a more positive CLE compared to their colleagues in private hospitals, consistent with findings by Aljohni et al 35 who also reported variation in perceptions among internship nursing students across diverse clinical sites. This implies that specific factors within public hospitals contribute to this perception. Public hospitals typically offer designed training programs, abundant resources, and a larger patient population, which could improve the clinical learning experience for students. Additionally, the collaborative environment and exposure to a various range of cases in public hospitals may contribute to the positive perception informed by students. This highlights the importance of considering the clinical placement setting in shaping nursing students’ experiences and perceptions during their clinical placement.
As far as we know, As the first study conduct to assess Palestinian nursing students’ perceptions of their CLE. The insights gained are helpful for educational institutions, healthcare providers, and policymakers alike, as they endeavor to improve the quality of nursing education and training programs. Educational institutions can utilize these findings to tailor their curricula and clinical placements to more effectively meet the need and expectations of nursing students. Similarly, healthcare providers stand to benefit from understanding students’ perceptions to improve the CLE and enhance the training experience. Policymakers can employ the result of this study to inform policies and regulations pertaining to nursing education and clinical practice, guaranteeing they align with the needs and experiences of students. However, it’s critical to acknowledge the study’s limitations, including its exclusive focus on a single university and employ a convenience sampling method, which may limit generalizability. Future research should aim to overcome these limitations by employing random samples from multiple universities, thereby improving the study’s generalizability. Overall, this study establishes a foundation for future research into Palestinian nursing students’ perceptions of the CLE, and it is recommended that replication studies with larger, more representative samples from various universities be conducted to further expand these initial findings.
Implication for Practice
The findings of this study have numerous implications for nursing education and clinical practice. Initially, nursing educators should prioritize the cultivation of supportive supervisory relationships and improvement the role of nurse teachers within CLE. This can be accomplished through mentorship programs, continuous professional development opportunities for clinical instructors, and the establishment of regular feedback mechanisms to ensure effective supervision and mentorship.
Additionally, healthcare institutions and nursing schools need to collaborate closely to address the identified inadequacies in the leadership style of ward managers. This may involve providing leadership training programs for ward managers, facilitating open communication channels between nursing staff and students, and promoting a culture of mutual respect and collaboration within clinical settings.
Finally, nursing programs should consider incorporating strategies to increase students’ satisfaction with their profession, as this was found to be positively associated with their perceptions of the CLE. This could involve career counseling services, opportunities for professional growth and progression, and initiatives to encourage a sense of fulfillment and purpose in the nursing profession.
Conclusion
Creating positive supervisory relationship and fostering interaction with nurse teacher are essential for successful leaning environment for nursing student throughout their clinical placements. The study indicated that Palestinian nursing students exhibited positive perceptions of their CLE, influenced by their academic level, clinical placement settings, and professional satisfaction. The supervisory relationship and the role of the nurse teacher were the most positively perceived by students, emphasizing the importance of ongoing support and guidance in nurturing CLE. Collaboration among nursing administrators, educators, and healthcare institutions is essential to implement targeted strategies for fostering a supportive CLE. Through continually evaluation and improvement of the clinical learning experience, we can ensure that nursing students receive the necessary education and support to become competent healthcare professionals, thereby improving healthcare outcomes in Palestine and beyond. Additionally, this study lays a vital foundation for future research into Palestinian nursing students’ perceptions of the CLE, and it is recommended that replication studies with larger, more representative samples from various universities be conducted to build upon and strengthen these initial findings.
Footnotes
Acknowledgements
The authors extend their appreciation to the nursing students whose participation was integral to the successful completion of this study.
Author Contributions
BH and FE designed the study. FE, IF, BS, and AA collected the collected the data. BH, and AA summarized data, and performed the statistical analysis. BH, FE, AA, BS, and IF interpreted the data, and drafted the manuscript. All the authors have accepted responsibility for the entire content of this submitted manuscript and approved submission.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
