Abstract
Introduction
Establishing a supportive clinical environment is paramount for enhancing nursing students’ engagement in clinical practice, their clinical proficiencies, and satisfaction. The increase in nursing student enrollment at the Nursing College, driven by the collaborative efforts between Abu Dhabi Health Services Company (SEHA) and universities, has given rise to concerns regarding the quality of education and clinical instruction. These concerns are primarily due to the increased student-to-instructor ratio. Furthermore, the unsupportive clinical settings and learning tensions underscore the need to understand students’ learning experiences and address research gaps within the field of clinical learning in the United Arab Emirates (UAE).
Objectives
The purpose of this study is to investigate the undergraduate nursing students’ perceptions of their clinical learning environment, with a focus on perceived benefits and challenges.
Methods
This study used a cross-sectional survey design. The researchers administered a five-point Likert scale questionnaire, which had been adapted and contextualized, to a convenience sample of 217 third and fourth-year nursing students who willingly participated in this study.
Results
Despite the presence of positive aspects, such as diverse clinical experiences and strong support from both clinical instructors and peers, several challenges affect the students’ clinical learning. These challenges encompass disparate perceptions of supervision among staff nurses, learning tensions related to student academic workload, insufficient clinical supervision, and difficulties in finding assistance when needed.
Conclusion
There is a clear need to enhance the overall ward learning environment to optimize students’ academic motivation and clinical skills. Several measures can be taken to achieve this goal, including incentivizing and reducing the workload of staff nurses, investing in the professional development of clinical instructors, promoting peer interactions and group learning, and adopting a block pattern of education in years three and four for better clinical knowledge assimilation and reduced theoretical workload.
Introduction
Clinical learning holds a paramount position in nursing education. It serves as a cornerstone for preparing students to proficiently operate in their upcoming clinical endeavours. As outlined by WHO (2009), clinical learning is instrumental in providing nursing students with the indispensable skills, knowledge, and attitudes required to deliver good nursing care. One of the imperative catalysts for fostering clinical learning among students is the presence of a supportive clinical learning environment (CLE). CLE is an “interactive network of forces within the clinical setting that influence the students’ clinical learning outcomes” (Dunn & Burnett, 1995, p. 1166).
A supportive CLE distinguished by proficient and experienced clinical instructors (Niederriter et al., 2017), alongside thorough theoretical and practical preparation of students for real-world clinical scenarios (Ewertsson et al., 2015), has the potential to amplify students’ motivation, active participation (Thomas et al., 2018), self-confidence (Ford et al., 2016; Jonsén et al., 2013), and satisfaction (Jacob et al. 2023). This environment ought to cater to students’ educational needs and elevate their clinical proficiencies (Aboshaiqah et al., 2018; Hakimzadeh et al., 2013).
Nursing Education System
The Nursing College's program of the Bachelor of Science in Nursing aims to support the UAE's vision of achieving high-quality healthcare services. All four branches of the Nursing College (Abu Dhabi, Al Ain, Ajman, and Al Gharbia), where the study took place, follow a study plan that mandates 127 credit hours, 94 credits for theory courses, 9 credits for laboratory courses, and 24 credit hours for clinical courses, spanning three years and four months. Year one covers foundation courses; subsequent years focus on nursing theory, lab, and clinical courses.
Problem Statement
Due to the emergence of the COVID-19 pandemic, Abu Dhabi Health Services Company (SEHA), which is the UAE's largest health care provider, emphasized the important role that nurses could play to fight this infection (SEHA, 2020) or any other emerging pandemic. Moreover, the UAE government declared its commitment to achieving high-quality healthcare services, which is one of the Sustainable Development Goals that the UAE has reaffirmed through its support of the 2030 United Nations Agenda for Sustainable Development (United Nations in United Arab Emirates, 2023). As such, SEHA is collaborating with universities to encourage Emirati students to study nursing (Nowais, 2016). Furthermore, health authorities mandated Emirati High School to participate in an educational outreach program. It aimed at promoting nursing programs by creating a partnership between the communities, such as the Nursing College, and schools through school presentations and workshops to provide information about the nursing program to high school students. Health authorities also encouraged students to enrol in these programs by offering scholarships and stipends as incentives. This strategy led to a sudden influx of students at the nursing college. Moreover, the availability of qualified instructors and budget constraints highlight the potential challenges to seamless recruitment. As such, the class size increased, and the clinical instructor-student ratio jumped from one-to-nine to one-to-eighteen. This has significantly constrained the time allotted to each student, potentially impacting the provision of individualized feedback. According to the Texas Board of Nursing (n.d.), the ratio of faculty to students in the clinical setting is 1 to 10.
As such, it is essential to assess the impact of these changes on students’ learning experiences.
Additional challenges that warrant exploration are more closely tied to students’ experiences in clinical settings. They often complain to their clinical instructors that some clinical settings are not conducive to learning, mainly because some preceptors are uncooperative and unsupportive (Aboshaiqah et al., 2018; Moghaddam et al., 2020; Thomas et al., 2018) and many patients reject them because they prefer to receive care from qualified nurses (Joolaee et al., 2015; Drateru, 2019). These issues may impact students’ self-esteem and motivation for clinical skill acquisition (Buthelezi et al., 2015).
Despite extensive exploration of facilitators and challenges to clinical learning environments (CLE) in international and regional literature (Amoo & Enyan, 2022; Aboshaiqah et al., 2018; Buthelezi et al., 2015; Chuan & Barnett, 2012; Happel & McAllister, 2015; Heidari & Mardani Hamooleh, 2016; Jamshidi et al., 2016; Moghaddam et al., 2020; Rozario et al., 2022; Yang & Chao, 2018), there is a significant gap in research specific to CLE in the UAE. Hence, gaining an understanding of students’ perceptions of their CLE becomes crucial. So, the primary purpose of this research is to explore the perceptions of undergraduate nursing students at the Nursing College about their CLE, with a focus on perceived benefits and challenges. The research questions that the researchers aim to answer are:
What are the undergraduate nursing students’ perceptions regarding their CLE? Are there any statistically significant differences between year three and year four students’ perspectives on their CLE factors?
Significance of the Study
This study is significant because it can provide valuable insights into students’ experiences, which can guide nursing educators, administrators, and policymakers in maintaining the facilitators of learning while also addressing any challenges encountered. Their perceptions may provide valuable guidance in shaping clinical policies, potentially prompting adjustments to the curriculum. These changes could involve modifications to the clinical practice model, teaching approaches, or clinical placements to meet students’ learning needs and improve the quality of their clinical learning. Effectively addressing these barriers can reduce student stress, improve educational outcomes (Papathanasiou et al., 2014), and boost satisfaction levels (Moghaddam et al., 2020).
Literature Review
One of the important factors that could influence the learning experiences of nursing students is the CLE. A positive CLE is characterized by well-oriented students, supportive staff (Mbakaya et al., 2020), cooperative preceptors (Ford et al., 2016), approachable and experienced clinical instructors (Jacobsen et al., 2019; Niederriter et al., 2017; Oermann et al., 2022), availability of resources, and the integration of theory and practice (Rozario et al., 2022). Such an environment could enhance the overall student's learning experiences (Ford et al., 2016), self-confidence, and motivation to learn (Jonsén et al., 2013).
Conversely, the clinical environment is not consistently regarded as a favourable learning environment for nursing students, and this is attributed to various challenges. These challenges include the heavy workload (Gemuhay et al., 2019) that leaves staff nurses unable to supervise, mentor, or provide feedback to students (Jacob et al., 2023, Mbakaya et al., 2020), coupled with uncooperative staff members (Thomas et al., 2018) who prevent student access to hospital learning resources like the library, internet, and training classes (Mamaghani et al., 2018). These challenges would also undermine students’ sense of belonging to the nursing team (Ford et al., 2016). Additionally, insufficient clinical equipment (Jacob et al., 2023), could hinder students’ practical learning and their achievement of clinical objectives (Gemuhay et al., 2019; Mbakaya et al., 2020; Rajeswaran, 2016). Moreover, the theory-practice gap may confuse students as they struggle to apply their knowledge in real-world settings (Bazrafkan & Kalyani, 2018; Jacob et al., 2023).
Additional challenges to CLE include mistreatment by patients, difficulties in managing patients from unfamiliar cultural backgrounds (Drateru, 2019), negative perceptions of the nursing profession, insufficient commitment of nurses to patient care, disrespect, student abuse, and a lack of appreciation (Moghaddam et al., 2020). Furthermore, students may face unpreparedness for clinical training when they grapple with anxiety stemming from concerns about making mistakes, uncertainty regarding patients, and confusion about the practical aspects of nursing (Günay & Kılınç, 2018; Joolaee et al., 2015), along with a fear of peer assessment and apprehension about receiving negative feedback from clinical instructors (Bazrafkan & Kalyani, 2018; Kalyani et al., 2018).
Methods
Design
The cross-sectional survey design was used to gain a general understanding of student's perceptions of their CLE. Surveys are useful tools to collect a wide range of unobservable data, including individuals’ preferences, traits, attitudes, beliefs, and behaviors (Gay et al., 2009).
Sample
The study population consists of four hundred year three and year four nursing students enrolled in the Bachelor of Nursing program in the four different campuses of the Nursing College in the UAE. A convenience sampling technique was used. Gay et al. (2009) recommend sampling 50% of the population in quantitative studies when the population size falls between 400 and 600 participants. The study's overall student population is 400. With a response rate of 53%, 217 year three and year four nursing students participated, and this sample is deemed sufficient, surpassing the recommended 50% threshold (Gay et al., 2009).
Inclusion/Exclusion criteria
The sample selection was guided by the following inclusion criteria: only students from the four campuses of the Nursing College were included. Additionally, only third- and fourth-year students were included, given their substantial clinical practice experience. The sample exclusively consisted of female students. As for the exclusion criteria, students from other colleges or universities in the UAE were not considered. Furthermore, first- and second-year nursing students were excluded due to their limited clinical experience, as the study plan does not mandate the completion of any clinical courses. Male students were also excluded, as no male students were enrolled in the program at the time of the study.
Instruments
This study used a questionnaire adapted from Chuan and Barnett (2012), specifically designed for the Malaysian context, with permission from the original authors. This questionnaire holds significance for our study as it delves into various factors that may either enhance or hinder the CLE of nursing students in the UAE. Its significance lies in its pivotal role in addressing the study's research questions.
The questionnaire has two parts. The first part is designed to gather demographic data concerning students’ nationality, age, year of study, and campus location. This data is intended for comparative analysis among students at various levels of study and across different campus locations. The second part consists of four subdivisions that measure the major factors related to clinical practice, and each factor is subdivided into several items, whose total number is 31. This part of the questionnaire is consistent with the first research question. These subdivisions include ward environment (13 items), supervision by clinical instructors (7 items), student satisfaction with clinical experience (4 items), peer support (2 items), and learning tensions (5 items). The first subdivision, ward environment, is divided into two dimensions that include the general ward environment (including 6 items) and supervision by staff nurses (incorporating 7 items).
The questionnaire's items were scored using a five-point Likert scale ranging from one (strongly disagree) to five (strongly agree). A high cumulative score for each statement indicates a more positive response. Item numbers 27 to 31, related to learning tensions, were negatively worded to mitigate response style bias. Researchers reversed these scores during analysis to enhance data validity (Baumgartner & Steenkamp, 2001; Paulhus, 1991).
To suit the UAE context, the researchers modified the Chuan and Barnett (2012) questionnaire by revising, adding, or removing items based on the literature review and their teaching experiences in the UAE. To establish the content, construct, and criterion validity of the questionnaire, it underwent expert review by three educational research specialists and two nursing research experts. Recommendations from these experts led to questionnaire amendments, including improved statement clarity.
Furthermore, the questionnaire was pilot-tested on 12 third-year and 13 fourth-year nursing students to identify and address ambiguities and confusion in the items. Based on their feedback, the researchers made changes to some statements. The researchers also used the responses from the pilot study to test the reliability by calculating Cronbach's alpha values in SPSS version 21. Cronbach's alpha value for the entire tool was found to be 0.82, while the coefficient for each factor ranged from 0.79 to 0.98. A Cronbach alpha test score ranges from zero to one, and a value of 0.7 is considered the minimum acceptable reliability score, and anything greater than 0.8 is good to excellent (Vogt et al. 2014).
Procedure
The researchers collaborated with instructors from four Nursing College campuses to invite third and fourth-year students to participate in the study. Upon securing consent from the students, the instructors provided guidance on meticulously completing the questionnaire without any omissions. Participants finished the questionnaire within approximately 15 minutes in the presence of the instructor.
Ethical Consideration
Ethical approval (Ref No.: FCEC-1-21-22-BSN-1-SF XYZ123) was granted by the Nursing College Ethics Committee. Participants were informed about the study's purpose and voluntary nature, with the option to withdraw anytime without consequences. Before collecting data, all participants signed informed consent forms, with assurance of anonymity and confidentiality throughout the study.
Statistical Analysis
Using SPSS version 21, the researchers measured the means, standard deviation, and percentages of each item. The percentage of agreement was calculated by adding the percentage of respondents who responded by ‘Strongly Agree’ to the percentage of respondents who responded by ‘Agree.’ The same applies to the percentage of disagreement. The means and SD were also calculated for the corresponding factors that affect the student's CLE. The independent sample t-test was used to compare differences between year three and year four students in terms of their perceptions related to the different factors affecting their CLE.
Results
Demographic data
A total of 217 female students completed the survey questionnaire. Many participants (30.3%) were 21 years old, 42.7% were 22 years of age or older, 14.4% were 20 years old, and 6.1% were 19 years old. Out of 217 responders, 193 (88.5%) were UAE nationals, while only 25 responders (11.5%) were expatriates. Concerning the study level, 78 (35.8%) students were from year three, and 140 (64.2%) were from year four. Concerning the campus location, Abu Dhabi = 20 students (9.2%), Ajman = 30 students (13.8%), Al Ain = 133 students (60%), and Al Dhafra = 37 students (17%). Due to the significant variation in response rates, the comparison between different campuses would not yield reliable results.
Descriptive Statistics of the Questionnaire
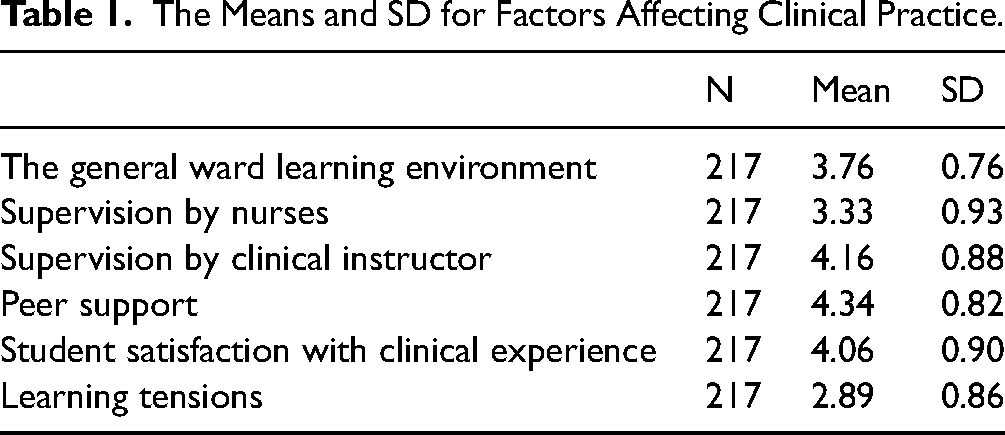
As seen in Table 1, the highest mean value was observed for “peer support” (M = 4.34, SD = 0.82), followed by “supervision by clinical instructor” (M = 4.16, SD = 0.88). The “learning tension” and “supervision by staff nurses” were rated the lowest with means of 2.80 (SD = 0.86) and 3.30 (SD = 0.93), respectively.
The Means and SD for Factors Affecting Clinical Practice.

As shown in Table 2, the overall percentage of agreement of the “general learning environment” was 71.7%, which is lower than that for “student satisfaction with clinical experience, “supervision by clinical instructor”, and “peer support”.
Means, SD, Percentages of Agreement and Disagreement of the General Ward Factor.
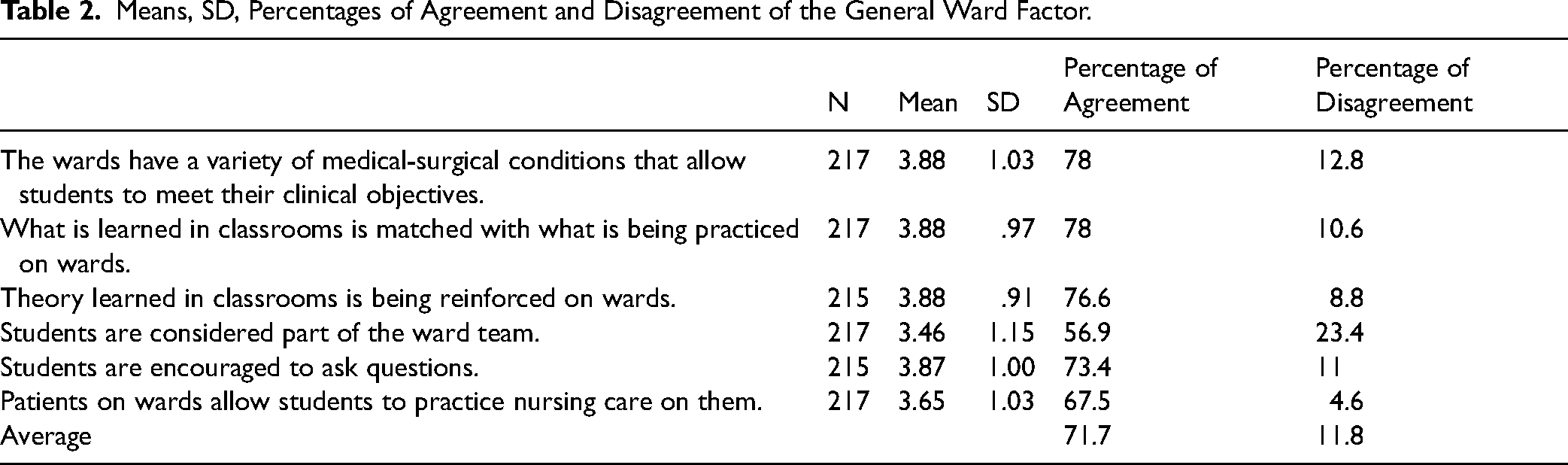
As shown in Table 3, the overall percentage agreement with the “supervision by staff nurses” factor was 49%, which is the lowest percentage when compared to other factors.
Means, SD, and Percentages of Agreement and Disagreement for Supervision by Staff Nurses.

As shown in Table 4, the “supervision by clinical instructor” factor had the second-highest overall percentage of agreement (84.2%)
The Means, SD, and Percentages of Agreement and Disagreement for Supervision by Clinical Instructors.

Table 5 shows the “peer support” factor had the highest overall percentage of agreement (90.15%).
The Means, SD, and Percentages of Agreement, and Disagreement for Peer Support.

Table 6 shows that the overall percentage of agreement with student “satisfaction with clinical experience” was 78.42%, which is lower than that obtained by “peer support” and “supervision by instructor”.
The Means, SD, and Percentages of Agreement and Disagreement for Student Satisfaction with clinical experience.

Table 7 shows that the “learning tensions” factor had the lowest overall percentage of agreement, with a percentage of 44.7%.
The Means, SD, and Percentage of Agreement and Disagreement for Learning Tensions.

Parametric Statistic of the Questionnaire
Parametric Statistic of the Questionnaire
Table 8 indicates that, aside from “peer support” (significance level 0.02 < 0.05), all other factors had significance levels surpassing 0.05. This implies a noteworthy distinction in “peer support” between third-year and fourth-year students at a 95% confidence level, with year four students exhibiting superior peer support (4.49) compared to year three students (4.08).
Independent Sample T-test.

Discussion
Discussion of the Descriptive Statistics
This discussion aims to answer the first research question. This question is: What are the undergraduate nursing students’ perceptions regarding their clinical learning experiences?
The general ward learning environment obtained the third-lowest ranking among factors influencing CLE. The score, close to neutral on the Likert scale, suggests a mixed response. Most students found their assigned hospital wards to align with their clinical learning goals (Thomas et al., 2018) by offering a diverse range of medical and surgical cases that provide ample opportunities for skill development through repetition (Bandura, 1977).
Additionally, most students noted the alignment between classroom learning and practical application, a finding consistent with Victor et al. (2016) in Pakistan. In contrast, studies in Saudi Arabia (Aboshaiqah et al., 2018), India (Thomas et al., 2018), Ghana (Amoo & Enyan, 2022), and Iran (Bazrafkan & Kalyani, 2018) reported different results, reflecting contextual variations in nursing care quality influenced by factors like nurse competence, healthcare policies, and resource availability. In the UAE, public healthcare facilities prioritize skilled, licensed nurses, with many organizations emphasizing accreditation, professional development, and the provision of necessary resources for high-quality patient care.
While most students felt encouraged to ask questions, some were hesitant due to unfamiliarity with staff members or shyness, especially with male staff nurses. The UAE culture is conservative, and women in this culture may feel shy in group communication, and they may either be silent or prefer to find a female to talk to (Ahmad, 2014). Moreover, feeling unintegrated into ward teams was a hindrance to clinical learning, and this could be attributed to students’ temporary assignments to these wards or the nurses’ demanding schedules and their inability to provide adequate support (Ford et al., 2016; Thomas et al., 2018). However, patients’ openness to receiving care from students provides valuable opportunities for students to enhance their skills (Aboshaiqah et al., 2018; Hansbrough et al., 2020). Some patients prefer care from Emirati or Arab nursing students due to shared language and cultural understanding as well as their tendency to display more caring behaviours, while busy staff nurses may lack time for meaningful communication. Unfortunately, such enriching experiences were not uniformly distributed among all students, as some patients could be concerned about receiving nursing care from students because they may think that students are incompetent.
The staff nurse's supervision factor had the second-lowest score among the five factors affecting CLE. Students had different experiences. Most students view staff nurses as good role models, and this is consistent with Vizcaya-Moreno et al. (2018) in Spain and is different from the findings of Thomas et al. (2018) study in India. This suggests that UAE nursing students generally have a more favourable view of their staff nurses, potentially influenced by stringent licensing procedures and ongoing efforts by the Department of Health to elevate nursing care standards.
Students also hold conflicting perspectives with the idea that staff nurses were willing to invest time in teaching, offer learning opportunities, guide students while they performed new tasks, and provide feedback (Günay & Kılınç's, 2018). The heavy workload and staff shortage may hinder nurses from mentoring or providing feedback to students (Gemuhay et al., 2019; Mbakaya et al., 2020). Moreover, nurses’ patient care responsibilities may limit their availability for student teaching, as neglecting these responsibilities could lead to reprimands from nurse managers.
Students generally had a positive perception of their clinical instructors, and this is consistent with the study of Jacobsen et al. (2019) in Norway. They viewed instructors as role models, especially when instructors displayed professionalism, systematic approaches to their work, familiarity with clinical settings, and effective management of student clinical practice (Niederriter et al., 2017; Rozario et al., 2022). Students indicated that their clinical instructors effectively communicated expectations for clinical practice (Bazrafkan & Kalyani, 2018). This may be attributed to the Nursing College's proactive measures in preparing students, including pre-placement orientation sessions led by clinical instructors, a practice recommended by Oermann et al. (2022).
While most students were satisfied with the time clinical instructors dedicated to their learning support, which is expected since instructors are mandated to spend eight hours with their assigned students in clinical settings, a few students held a contrasting view. The decrease in time allocated to each student can be attributed to both a sudden increase in student enrollment (Jacob et al., 2023) and the practice of assigning instructors to multiple students across various clinical areas with diverse geographical locations.
Clinical instructors are not just responsible for supervising students in clinical settings but are also expected to actively contribute to students’ learning (Günay & Kılınç, 2018) by effectively guiding students, using thought-provoking questions and diverse teaching approaches, and providing constructive feedback (Bandura, 1997; Clapper, 2015; Gaberson et al., 2015). Most students also acknowledged their clinical instructors’ role in enhancing their clinical knowledge and skills, in contrast to studies conducted in Iran (Bazrafkan and Kalyani, 2018), India (Thomas et al., 2018), Tanzania (Gemuhay et al., 2019), and Uganda (Drateru, 2019). The Nursing College maintains high-quality clinical instructors through stringent recruitment and mandatory regular professional development for knowledge and teaching skill enhancement. However, some opposed it, possibly due to challenges in supervising larger student numbers.
Most students were satisfied with the peer support. Most of them agreed that their classmates both contributed to their learning and helped them perform their assigned tasks. Similar findings were reported by Ädel et al. (2021). Engaging in collaborative discussions fosters the students’ cultivation of novel ways of thinking and enhances their learning experiences (Yaacob et al., 2021). However, around 10 students (5%) disagreed that their peers were helpful. This attitude may stem from students’ inclination to keep information to themselves or being overly focused on activities to achieve individual learning goals rather than engaging in peer support (Ädel et al., 2021).
The learning tension factor score falls within the neutral range on the Likert scale. Agreement percentages highlight specific stressors experienced by students during clinical training, stemming from workload expectations on assigned wards, responsibilities without sufficient supervision, and difficulties in seeking assistance. This may be attributed to a potential lack of support and encouragement from staff nurses (Zamanzadeh et al., 2015), fear of evaluation and negative feedback from the clinical instructor (Bazrafkan & Kalyani, 2018; Kalyani et al., 2018), perceived lack of competency (Gemuhay et al., 2019), or a shortage of clinical instructors (Jacob et al., 2023). The students’ learning tension is also attributed to the heavy workload of theoretical classes, negatively impacting their preparation for clinical practice (Thomas et al., 2018). Adequate preparation is crucial, as it empowers students to apply theoretical knowledge by performing procedures during clinical placements (Bandura, 1997; Nabavi, 2012).
Despite concerns raised by some nursing students at the Nursing College about supervision and stress during clinical placements, many express a positive sentiment toward their CLE. This aligns with a study by Jacobsen et al. (2019) in Norway. This positivity could be attributed to their favourable views on aspects like effective guidance from clinical instructors, peer support, and available learning opportunities. Such an outlook can enhance students’ contentment with clinical practice, thereby enhancing their clinical performance and sense of self-efficacy (Bandura, 1997; Nabavi, 2012).
Discussion of the Parametric Analysis
The independent T-test answers the second question: Are there any statistically significant differences between year three and year four students’ perspectives on their CLE factors? The T-test results reveal a statistically significant difference in terms of peer support, with year four students demonstrating better peer support than year three students. This distinction may be attributed to the greater knowledge and skills of fourth-year students, stemming from the completion of more theory courses and increased clinical experience. However, there is no statistically significant difference between year three and year four students regarding their perceptions of the other five factors. This lack of difference could be explained by both groups undergoing clinical practice in the same clinical areas and exposing them to the same clinical environment.
Strengths and Limitations
The study has notable strengths contributing to its credibility. Firstly, well-defined research questions provide a clear investigation focus. Secondly, a comprehensive literature review shows a thorough understanding of the subject's existing knowledge. The research methodology is well-designed and employs a robust approach to data collection and analysis. The use of reliable and validated data enhances methodological integrity, and a sufficiently large sample size supports result generalizability. Notably, it addresses a literature gap regarding the CLE in the UAE.
However, a significant limitation is the sample composition, consisting solely of undergraduate nursing students from one college with branches in four different Emirates. This may restrict generalizing findings to the broader population of nursing students in the UAE. Another limitation is the exclusion of male participants due to cultural norms discouraging males from pursuing nursing in Emirati culture. Additionally, challenges in drawing meaningful campus comparisons arise from the significant variation in response rates. Despite these limitations, the study's strengths and contributions provide valuable insights into the CLE in the UAE.
Implications for Practice
The UAE government is dedicated to achieving excellence in healthcare services, aligning with Sustainable Development Goal 3. According to Bandura (1977), learning is influenced by cognitive, environmental, and behavioural factors, implying that the learning environment can impact a student's learning. Improving the CLE is crucial for enhancing students’ academic motivation and clinical skills (Gemuhay et al., 2019) and, consequently, for preparing competent future nurses. Understanding undergraduate nursing students’ perceptions of their CLE experiences is essential. These perceptions can provide insights into the need for maintaining positive aspects and addressing areas that require careful attention at various levels, from the government to individual nursing students.
The government has to allocate a generous budget for hospitals to recruit qualified nurses and for the Nursing College to prioritize hiring nursing instructors and continue supporting them in providing professional development activities. Emphasizing the accreditation of healthcare providers and nursing colleges, along with providing necessary resources, is crucial for ensuring high-quality patient care.
Hospitals should enhance the integration of students’ clinical learning into nurses’ duties while concurrently reducing the workload demands on their preceptors. Applying Vygotsky's theory, staff nurses should involve students in tasks and independent execution under supervision to foster skill development, as a shortage of such opportunities hampers clinical practice (Sarker, 2019). Dedicated staff nurses committed to teaching and offering individual feedback and support could facilitate the learning process (Mbakaya et al., 2020, Rozario et al., 2022; Vizcaya-Moreno et al., 2018). Moreover, encouraging staff nurses to serve as role models for students, fostering positive interpersonal relationships, and providing ample support to enhance their sense of belonging within the hospital team are essential steps. This sense of belonging acts as a powerful motivator for students to ask questions and seek guidance (Ford et al., 2016). Additionally, to ensure sustained motivation and commitment among nurses, it is advisable to acknowledge staff nurses for their contributions to student education (Gaberson et al., 2010). This recognition can take the form of benefits such as free tuition for their children's education or access to college facilities like libraries, gyms, or swimming pools.
Policymakers at the nursing college level have to develop a comprehensive strategy addressing staffing needs and financial constraints to reduce the workload on clinical instructors and enhance students’ satisfaction. This involves allocating a sufficient budget and implementing effective advertising strategies to recruit more clinical instructors for the Nursing College.
Furthermore, policymakers should address the heavy academic workloads faced by students in preparing for clinical practice by emphasizing the importance of efficient curriculum planning, as poor performance stemming from inadequate preparation could lead to diminished self-efficacy among students (Bandura, 1997; Nabavi, 2012). Currently, the Nursing College employs a concurrent course pattern that integrates theory with practice and promotes critical reflection. However, considering the benefits of the block pattern for “assimilation,” “consolidation,” and “socialization” (Rohatinsky et al., 2017, p. 156), policymakers should explore its adoption. Emphasizing clinical practice within the block pattern can alleviate concerns about theory course workload, provide a more realistic perception of work, enrich students’ clinical knowledge, and encourage a concentrated focus on clinical placement (Birks et al., 2017). The block pattern may be particularly suitable for senior students with strong clinical skills and self-confidence, while the concurrent pattern could be more appropriate for first- and second-year students who need additional time to acclimate to the clinical environment (Birks et al., 2017). Therefore, it is recommended to adopt a combination of these patterns (Iwasiw et al., 2020).
The students’ perception of clinical instructors as role models and mentors underscores their crucial role in enhancing the CLE. Investing in the professional development of clinical instructors and actively involving them in student learning can have a positive impact on clinical learning. Instructors should assist students in managing stress, demonstrate enthusiasm, acknowledge mistakes, and judiciously employ humour (Gaberson et al., 2015; Oermann et al., 2022). Furthermore, instructors should consistently provide diverse clinical experiences, address various student concerns, and emphasize a dynamic connection between theory and practice through reflective sessions at the end of each clinical day. These sessions help students overcome challenges in clinical settings (Thomas & Asselin, 2018), and enhance their overall learning experience (Ford et al., 2016) and critical thinking skills (Ardian et al., 2019).
Nursing students express a high level of satisfaction with peer assistance, underscoring the significance of group learning in easing the stress associated with managing assigned tasks. This, in turn, contributes to an improved overall learning environment (Ädel et al., 2021). Therefore, it becomes the responsibility of clinical instructors to capitalize on this positive aspect and encourage students to engage in collaborative learning and mutual support, emphasizing cooperation over competition for learning opportunities (Oermann et al., 2022).
Conclusion
Nursing students had mixed reactions to the overall CLE, suggesting room for improvement in satisfaction and motivation. They found opportunities for diverse clinical experiences and alignment with theoretical knowledge. The students’ perceptions of the staff nurses’ supervision varied; some regarded them as mentors, while others voiced concerns about the lack of encouragement and feedback. Students generally had a positive view of clinical instructors as role models but expressed concerns about effective facilitation, possibly due to student-instructor ratios. Peer support was strong, and most students anticipated a positive clinical practice experience, which could boost self-efficacy. However, students reported stress due to workload, limited supervision, and difficulties seeking assistance.
The researchers suggest expanding the study to include students from all UAE nursing colleges for more robust findings. They also propose researching clinical instructors’ views on factors affecting students CLE and preceptors’ views regarding their role in supporting the clinical learning of undergraduate nursing students.
Footnotes
Acknowledgements
Special thanks to the nursing students in the Nursing College who answered the survey questions.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
The Ethics Review Committee at Fatima College approved our study (Approval: FCEC-1-21-22-BSN-1-SF XYZ123) on September 19, 2021. A consent form was signed by the college of nursing student before starting the survey.
Both authors actively and significantly contributed to various aspects of the research, including the conceptualization and design, literature review, data analysis, and discussion section. Both authors also played a critical role in revising the article.
However, Dr. Imad obtained ethical approval from his college and distributed the survey, utilizing his access to faculty members and students. Dr. Wafaa was more involved in the manuscript's writing process. These contributions justify their legitimate claims to authorship.
Funding
The authors received no financial support from any funding agency in the public, commercial, or not-for-profit sectors.
