Abstract
This study examined the relationship between health and productivity management (H&PM) and inpatient health care efficiency in hospitals. This cross-sectional study is based on 1108 hospitals using data from the FY2021 Bed Function Report. The presence of Certified H&PM Organization was the proxy variable for H&PM implementation. The efficiency value obtained using the input-oriented Banker-Charners-Cooper model of data envelopment analysis was a proxy variable for inpatient health care efficiency. The input variables were the number of hospital beds, registered physicians, ward nurses, and other staff members in the ward. The output variable was the total number of patients in the ward per year. We conducted a Wilcoxon rank-sum test and compared certified and non-certified hospitals. The efficiency value was the objective variable, and certification presence was the explanatory variable. We used a stepwise method, including adjustment variables, to confirm whether the certification presence remained in the final multiple regression model. Efficiency was significantly higher in certified hospitals than non-certified hospitals. Certification presence remained in the final multiple regression model (β = .027, CI = −0.004 to 0.057, P = .085). Although not statistically significant, certified hospitals tended to have higher efficiency compared to non-certified hospitals. These findings suggested that hospitals that actively engage in H&PM may have higher efficiency in inpatient health care. However, further research is needed to establish the causal relationship.
Keywords
The concept of health and productivity management (H&PM) is widespread in Japan, and its implementation is expected to have effects such as improving the health of staff and improving organizational productivity. However, the relationship between H&PM and the efficiency of inpatient health care provided by hospitals remains unclear.
A positive correlation was observed between being a certified H&PM Organization and data envelopment analysis efficiency, which indicates the efficiency of inpatient health care. H&PM efforts could help provide efficient inpatient health care.
A greater number of medical institutions may engage in H&PM in the future. A greater number of medical institutions may engage in H&PM in the future. H&PM can be implemented even in hospitals that cannot be certified as specific function hospitals.
Introduction
Hospitals utilize many medical resources in treatment, and the efficiency of medical care is important for hospital managers.1,2 Improving the efficiency of medical care enables the provision of high-quality medical services. According to the World Health Organization (WHO), continuing to improve efficiency, quality, and equity in healthcare delivery is a challenge faced by high-income and upper-middle-income countries, including Japan. 3 Thus improvements in medical efficiency are attracting attention worldwide. The correlation between employee health and organizational productivity in various countries has increasingly attracted attention.4 -6 Poor employee health increases medical costs, adversely affects organizational survival, and decreases productivity, highlighting the importance of efforts to improve employee health and thus increase productivity.7,8
In Japan, the concept of health and productivity management (H&PM) is becoming widespread.9,10 H&PM refers to the “consideration of health management from a business perspective and its strategic implementation based on the belief that efforts to maintain and improve employee health are an investment that will increase profitability in the future.” 11 The Certified H&PM Organization system has been developed to create an environment that facilitates excellent corporations engaged in H&PM and allows them to receive social recognition. 12 To be a Certified H&PM Organization, it is necessary to undergo the Health and Productivity Survey Sheets which evaluates factors such as the dissemination of H&PM policies both within and outside the organization, the appointment of managerial personnel, the establishment of specific promotion plans (goals), the verification of the effectiveness of these initiatives, and compliance with laws and regulations. In the Health and Productivity Survey Sheets, a deviation value is calculated for each corporation. 13
Several studies have investigated the effects of H&PM. Certified H&PM Organizations have a better public image and recruitment results than non-certified companies, which may lead to lower turnover rates and improved productivity. 14 Furthermore, there is a greater prevalence of employees who are non-smokers, have a healthy BMI and good blood pressure control in organizations employing occupational health professionals than in those that do not. 15 Moreover, organizations that provide health education to managers have a higher proportion of non-smokers. 15 Research on H&PM in healthcare organizations shows that productivity decreases as employee health risk levels increase, and reducing employee health risks improves presenteeism. 16 Therefore, the implementation of H&PM has the potential to improve employee health and productivity, revitalize organizations, and enable health care staff to provide medical services to more patients. However, there are few studies that have examined how far the introduction of H&PM actually enhances health care efficiency.
Determining whether H&PM improves employee health and organizational productivity, and helps to provide efficient medical care is important to public health. Japan is experiencing a declining birth rate and aging population, and the burdens on the working generation are increasing. Securing and retaining staff is an issue at medical institutions due to harsh work environments, such as long working hours and night shifts. 17 Continuing to provide high-quality medical services in the future requires improving the working environment of medical institutions and efficiently using the limited resources. 17 Therefore, this study hypothesized that hospitals that are certified as Certified H&PM Organizations have higher inpatient health care efficiency than non-certified hospitals.
Methods
Research Subjects
This was a cross-sectional study. Data were obtained from publicly available sources, and an ethics committee approval was not required.
This study included hospitals from the FY2021 Bed Function Report published by the Ministry of Health, Labour and Welfare of Japan. 18 The Bed Function Report provides open data to prefectures on the medical functions of the beds owned by hospitals, ward equipment, medical staff assigned, medical practices, and other factors. 19 The FY2021 Bed Function Report included 7019 hospitals.
In another study, we selected 2000 hospitals from this data set 18 and conducted a questionnaire survey on the relationship between hospitals and health management; the results of the survey are being compiled. Additionally, to explore this association from multiple perspectives and not rely only on the survey results, we included similar hospitals in the present study.
The questionnaire survey excluded 403 hospitals based on the following criteria: all wards were closed; ≤1 patient in all wards; presence of a ward with ≥1 resident patients, inpatients, or discharged patients and zero licensed beds; presence of wards with both general and recuperative care beds; and presence of wards with the average length of stay <1 day (Exclusion Criteria 1). Subsequently, 6616 hospitals remained and were divided into certified and non-certified hospitals. Of the 6616 hospitals, 99 were certified and 6517 were non-certified. Certified hospitals were selected by extracting medical corporations, social welfare corporations, and health insurance associations (grouped as medical corporations) that were certified as Certified H&PM Organizations as of July 2023 by the Ministry of Economy, Trade and Industry of Japan. 20 A medical corporation is a non-profit organization whose purpose is to open and operate medical facilities. Next, for non-certified hospitals, 550 hospitals were excluded based on the following criteria: average length of stay that cannot be calculated, variables in the data envelopment analysis (DEA) containing zeros, having <1 registered physician, bed occupancy rates exceeding 100% (Exclusion Criteria 2). Moreover, 499 hospitals that could not be linked to addresses in the list of medical institutions created by local health and welfare bureaus across Japan as of October 2023 were excluded (Exclusion Criteria 3).21 -28 From the remaining 5468 hospitals, 1901 non-certified hospitals were randomly selected. After extraction, 6 hospitals that were not medical corporations and received certification were revised to certified hospitals. Therefore, 2000 hospitals were examined in the previous study, including 105 certified and 1895 non-certified hospitals.
Subsequently, we excluded 9 certified hospitals in which the average length of stay could not be calculated, the variables used for DEA included zeros, the number of registered physicians was <1, or the bed utilization rate exceeded 100% (Exclusion Criteria 2). Furthermore, we excluded 883 certified and non-certified hospitals with total annual number of patients in the ward in FY2021 <20% or ≥500% compared to the previous and following years or without general beds and bed classification not in the highly acute or acute stages (Exclusion Criteria 4). Consequently, 1108 hospitals were included. The bed classification was incorporated to ensure consistency in medical care and patient severity. Bed classification was divided into highly acute, acute, convalescent, and chronic stages. This classification is an indicator for appropriate medical care based on the condition of the patients. We summed the total number of beds in the hospital in each of the four categories and used the bed classification with the largest number of beds as the bed classification for that hospital. The final sample included 50 certified and 1058 non-certified hospitals (Figure 1). Furthermore, preliminary data processing, confirmed that there are no missing values.
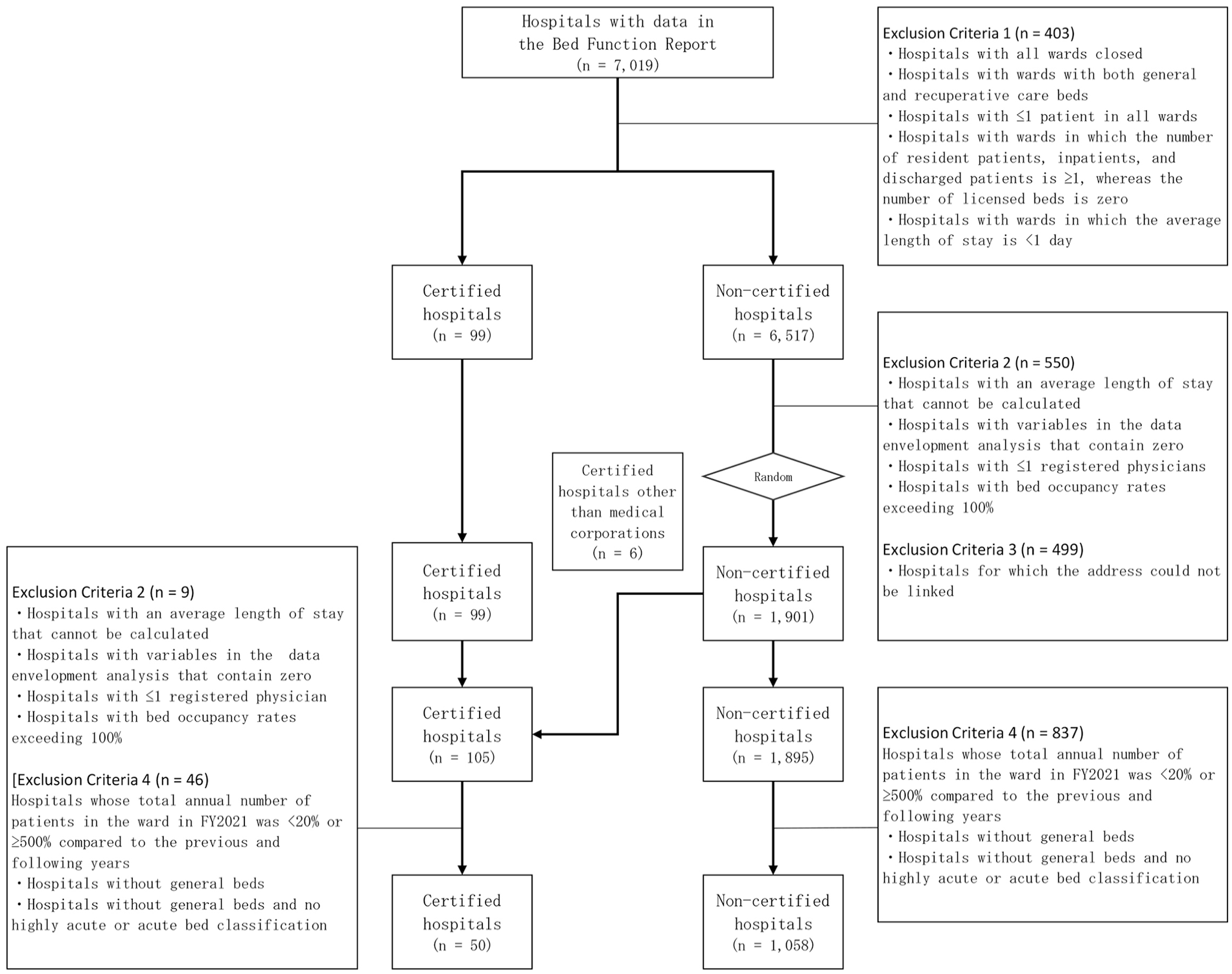
A flowchart of the hospitals.
Objective Variable
The objective variable was the efficiency of inpatient health care measured using the efficiency value based on the DEA. DEA has been used in research in various fields to evaluate organizational efficiency. 29 This model combines multiple endpoints with different units into 1 input and output, and the efficiency of each decision-making unit (DMU) is calculated. The efficiency value of the most efficient DMU is set to 1, and the efficiency value of each DMU is expressed as a value between 0 and 1 for relative evaluation. Understanding how well an organization such as a hospital is managed commonly involves comparisons with other hospitals; however, in some cases, hospital A may be better in 1 index, and hospital B in another. The advantage of DEA is the ability to evaluate hospitals with multiple indices and different units. 30
The DMU in this study was a hospital, and we assumed a model in which hospitals utilize capital and labor to treat patients. The inputs were the number of hospital beds as a proxy variable for capital and the number of registered physicians, ward nurses, and ward staff as proxy variables for labor force. The output was the total annual number of patients admitted to the ward as a proxy variable for the treatment outcome of inpatient health care. We used the FY2021 Bed Function Report to obtain data. 18 Analyses were conducted using DEA Solver Pro12.1 (Saitech, Inc., Tokyo, Japan). The analysis model was an input-oriented Banker-Charners-Cooper (BCC) type. Table 1 shows the input and output summary statistics.
Summary Statistics.

Note. For categorical variables, * indicates the use of Fisher’s exact test. The χ2 test was used for all other cases. For continuous variables, the Wilcoxon rank-sum test was used for input, output, and the number of general clinics, Welch’s t-test was used for the proportion of the population aged ≥65 years and the number of general hospitals.
Q1 = first quartile; Q3 = third quartile.
Explanatory Variables
Certified H&PM Organization is a Nippon Kenko Kaigi certification that indicates a corporation’s H&PM efforts above a certain level. 13 Nippon Kenko Kaigi is a private-sector initiative that brings together leaders from the business community, medical organizations, local governments, and insurers to increase healthy life expectancy and optimize medical costs. 13
We used this certification as an index to show that a hospital was actively engaged in H&PM efforts. Previous studies have also compared the effects of health management based on the certification status of Certified H&PM Organizations. 14 Additionally, there have been studies investigating the correlation between the deviation scores of Health and Productivity Survey Sheets and the implementation status of infection control measures in companies. 31
Both the deviation value of the Health and Productivity Survey Sheets and the certification status of Certified H&PM Organizations are used as indicators to represent the implementation status of initiatives. However, the deviation value of the Health and Productivity Survey Sheets targets all industries. On the contrary, this study targets medical institutions and thus uses the absolute evaluation of Certified H&PM Organizations. We selected the following types of hospitals from the list of certified corporations published by the Ministry of Economy, Trade and Industry of Japan in July 2023: corporations with an industry classification of medical corporation, social medical corporation, health insurance association; incorporated association, foundation, chamber of commerce, or industry; and professional, non-profit, public, special, and other corporations. 20 The hospitals owned by the extracted corporations were verified through each corporation’s website and designated as certified hospitals. Furthermore, for hospitals whose operating entity was a company according to the 2021 Bed Function Report data, 18 the operating company was identified from the hospitals’ websites. If the company’s name was listed in the 2023 list of certified corporations, 20 the hospital was designated as a certified hospital. Although the certification for Certified H&PM Organization is granted at the corporate level, the subject of analysis in this study is at the hospital level. Therefore, it was necessary to identify and verify hospitals operated by these corporations using their websites.
Moderator Variables
We used the following 17 moderator variables for hospital characteristics: regional classification (metropolitan type, regional city type, depopulated area type), implementing body, being a diagnosis procedure combination (DPC) target hospital, being a specific function hospital, being a community medical support hospital, presence of comprehensive hospitalization system premium, being an at-home recuperative care support hospital, being an at-home recuperative care and logistic support hospital, being a tertiary emergency medical facility, being a secondary emergency medical facility, being an emergency notification hospital, presence of discharge coordination department, general bed classification, general bed care department, recuperative bed classification, recuperative bed care department, and number of beds. In the regional classification, the metropolitan type was defined as an area with a population of ≥1 million in the secondary medical area or a population density of ≥2000 people/km2. The regional city type was defined as an area with a population of ≥200 000 in the secondary medical area or a population of 100 000 to 200 000 and a population density of ≥200 people/km2. The depopulated area type was defined as an area that did not belong to either the metropolitan or regional city types. 32 DPC target hospital were those that had fixed-rate payment systems for inpatient medical expenses. Special function hospitals were those certified as providing advanced medical care. Community medical support hospitals were those that aimed to secure community medical care through support for family physicians. A comprehensive hospitalization system premium indicates having sufficient personnel and equipment and being able to provide acute care 24 h per day. At-home recuperative care support hospitals were those that had a system that allowed for house calls or home-visit long-term care 24 h per day. At-home recuperative care and logistic support hospitals were registered as hospitals in which patients receiving at-home care could be admitted for emergencies. Tertiary emergency medical facilities treat critically ill patients when a primary or secondary emergency response cannot be provided. Secondary emergency medical facilities treat critically ill patients who require hospitalization or surgery. Emergency notification hospitals treat patients who are more seriously ill than those who can be treated at general acute care hospitals. A discharge coordination department considers the discharge destination of hospitalized patients and includes necessary services. Recuperative beds are used when patients who required long-term recuperation are hospitalized.
Moreover, we set the number of general hospitals and general clinics per 100 000 people in the secondary medical area to which the hospital belongs as variables representing medical resources in the vicinity of the hospital. Furthermore, we set the proportion of the population aged ≥65 years in the secondary medical care to which the hospital belongs as a variable representing patient characteristics in the vicinity of the hospital. The secondary medical area was set as regional units that provide inpatient health care based on geographical and traffic conditions. 33
For the data for each variable, we calculated regional classification and proportion of the population ≥65 years using the Secondary Medical Area Basic Data Professional Version 12.0.2. 34 The data were created by Wellness Co, Ltd. and provided free of charge, including medical welfare provision system data and basic statistical information for each secondary medical area across Japan. We used the FY2021 Bed Function Report to obtain data on the implementing body, presence of DPC, being a specific function hospital, being a local medical support hospital, presence of comprehensive hospitalization system premium, being an at-home recuperative care support hospital, being an at-home recuperative care and logistic support hospital, being a tertiary emergency medical facility, being a secondary emergency medical facility, being an emergency notification hospital, presence of discharge coordination department, general bed classification, general bed care department, recuperative bed classification, recuperative bed care department, and number of beds. 18 We used the FY2021 Medical Facility Survey to obtain the number of general hospitals and general clinics per 100 000 people.35,36 We used the metropolitan type as a reference for the regional classification, with other regions being the regional classification dummy variables. We used medical corporation as a reference for the implementing entity, with other corporations used as a dummy variable. The general bed classification was a binary variable of highly acute stage and acute stage, with the highly acute stage used as a reference. We used the internal medicine department was used as a reference for the general medical care department, and multiple medical and other medical departments were used as dummy variables. We used hospitals without recuperative beds as a reference for the recuperative bed classification, and hospitals with recuperative beds were used as a dummy variable. We used hospitals with no departments (ie, no long-term care beds were present) as a reference for the long-term bed care department. Internal medicine department, multiple medical departments, and other medical departments were used as dummy variables. The number of beds was classified as a categorical variable, with categories of <50 beds, 50 to 99 beds, 100 to 149 beds, 150 to 159 beds, and ≥200 beds.
Statistical Analysis
Statistical analyses were conducted using R version 4.1.3. First, we classified the study target hospitals into certified and non-certified and confirmed the summary statistics. Continuous variables were analyzed using the Wilcoxon rank-sum test and Welch’s t-test. Categorical variables were analyzed using the chi-square test and Fisher’s exact test. Next, we used DEA to determine the efficiency value and evaluated the difference between certified and non-certified hospitals. The Wilcoxon rank-sum test was used for the analysis. Subsequently, we analyzed the correlation between efficiency and the presence of Certified H&PM Organization using a simple regression analysis. Finally, we conducted a multiple regression analysis with the moderator variables. The moderator variables with a difference at a significance level of 20% were extracted from the simple regression analysis. We determined the final moderator variables using a stepwise method, with the presence of Certified H&PM Organization added to the extracted moderator variables. The significance level for variables other than variable selection was set at 5% on both sides. Additionally, during the regression analysis, the normality of the residuals was confirmed.
Results
Target Hospital Background
Hospital information is presented in Table 1. Significant differences were seen in the following 6 out of 20 variables: implementing entity, presence of comprehensive hospitalization system premium, being an at-home recuperative care and logistic support hospital, presence of discharge adjustment department, recuperative bed classification, and number of general clinics per 100 000 people. More certified than non-certified medical corporations had implementing entities. Fewer certified than non-certified hospitals had a comprehensive hospitalization system premium. Certified hospitals included more at-home recuperative care and logistic support hospitals than non-certified ones. More certified than non-certified hospitals had discharge coordination departments. More certified than non-certified hospitals had a recuperative bed classification. Secondary medical areas in certified hospitals had a larger number of general clinics per 100 000 people than those in non-certified hospitals.
DEA
DEA results are presented in Table 1. The median efficiency values were 0.86 (0.81, 0.92) and 0.83 (0.76, 0.89) for certified and non-certified hospitals, respectively. A Wilcoxon rank-sum test was conducted on the difference in the median efficiency value, and a significant difference was observed (P = .019).
Regression Analysis
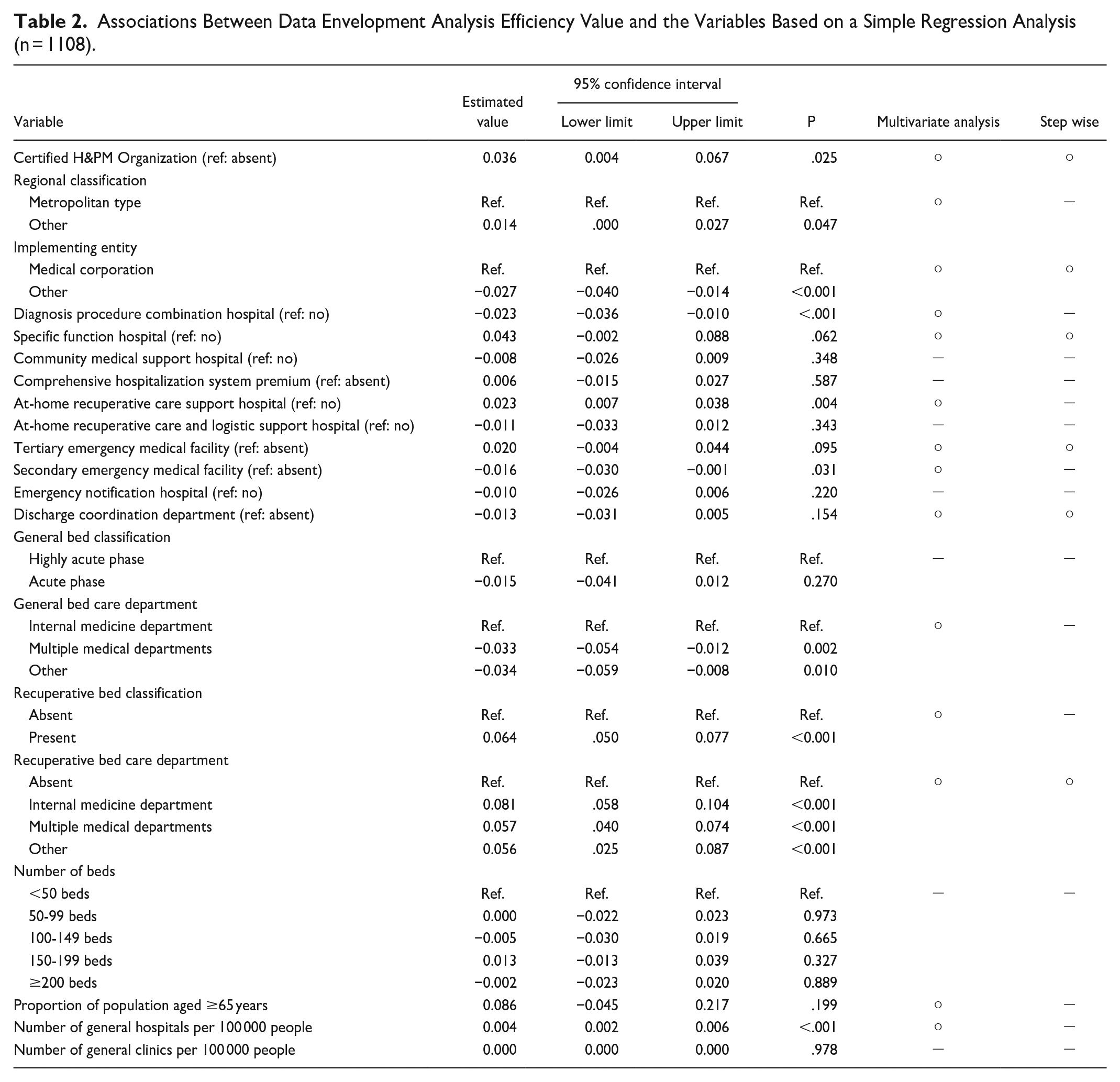
The regression analysis revealed a significantly positive correlation between efficiency and certification presence (with β = .036, CI = 0.004-0.067, P = .025; Table 2). The following moderator variables were significant at the 20% level: regional classification, implementing body, presence of DPC, being a specific function hospital, being an at-home recuperative care support hospital, being a tertiary emergency medical facility, being a secondary emergency medical facility, presence of discharge coordination department, general bed care department, recuperative bed classification, recuperative bed care department, proportion of population aged ≥65 years, and number of general hospitals per 100 000 people. We conducted a stepwise analysis that included certification presence. However, as the recuperative bed classification and recuperative bed care department overlapped in that the absence of recuperative beds was a reference for both, we used the recuperative bed care department as a variable in the stepwise analysis. The following variables remained significant in the final analysis: certification presence, implementing entity, being a specific function hospital, tertiary emergency medical facilities, presence of discharge coordination department, recuperative bed care department, and number of general hospitals per 100 000 people. The results of the multiple regression analysis showed a positive correlation between efficiency and certification presence (β = .027, CI = -0.004–0.057, P = .085; Table 3). The coefficient of determination of the multiple regression model was 0.108, and the adjusted coefficient of determination was 0.101.
Associations Between Data Envelopment Analysis Efficiency Value and the Variables Based on a Simple Regression Analysis (n = 1108).
Association Between Data Envelopment Analysis Efficiency Value and Certified H&PM Organization Based on a Multiple Regression Analysis (n = 1108).

Note. AIC = −1,834.7; R2 = .108; adjusted R2 = .101.
Discussion
This study examined the relationship between H&PM and the efficiency of inpatient health care in hospitals. Certification presence remained in the final multiple regression model. Although not statistically significant, certified hospitals tended to have higher efficiency compared to non-certified hospitals, and the former had an efficiency that was 0.027 points higher. The input variables in this study are the numbers of the following: beds, physicians, nurses in the wards, and other staff in the wards. Certified hospitals suggest more efficient use of medical resources to manage inpatients compared to non-certified hospitals. These results suggest that actively engaging in H&PM may improve staff health and hospital productivity and enable hospitals to treat a greater number of inpatients, thereby increasing the efficiency of inpatient health care. Previous studies have argued that providing incentives to management is necessary for promoting H&PM, 37 and this study’s results may contribute to improving health care management and increasing the efficiency of inpatient health care.
Furthermore, hospitals whose implementing entity was a medical corporation tended to have higher efficiency values. Medical institutions managed by the national government and public institutions may struggle to improve efficiency due to their involvement in medical care in remote areas as well as unprofitable medical care that the private sector cannot incorporate. Specific function hospitals tended to have higher efficiency. Specific function hospitals differ from general hospitals in that they provide more advanced medical care, and their certification requirements include the percentage of patients referred from other medical institutions and those referred to other medical institutions; therefore, plans for increasing efficiency may have been in place. Tertiary emergency medical facilities tended to have higher efficiency. Tertiary emergency medical facilities have a high level of staffing and treat patients who require serious emergency medical care. Efficiency may have been higher in these hospitals because they handle critically ill patients who cannot be treated at other medical facilities, resulting in a larger number of patients and higher efficiency. Hospitals without discharge coordination departments tended to have higher efficiency. Previous research has shown that the efficiency of secondary medical areas was positively correlated with hospital discharge coordination 38 ; however, efficiency was low in the present study. Unlike previous research, the present study used health care workers as input and the number of patients in the ward as output. Other values, such as revenue, were not used. Therefore, in this DEA model, the results produced by health care workers working in a discharge coordination department may not be fully reflected in the output. Hospitals with recuperative beds tended to have higher efficiency. This could have been because recuperative beds were used by patients whose symptoms were relatively stable, and the required medical resources were fewer than for general beds. Hospitals with a greater number of other hospitals located in the secondary medical area tended to result in higher efficiency values. Functional differentiation may have been planned by providing medical care in cooperation with surrounding medical institutions, thereby increasing efficiency value.
This study had several limitations. First, this study targeted hospitals that were listed in the Bed Function Report, and hospitals that were not reported were not included in the study, which may have led to selection bias. However, the number of hospitals in Japan as of October 2023 was 8125, 39 of which 7019 hospitals were listed in the Bed Function Report, indicating that many hospitals were reported. Second, hospitals in this study were grouped based on whether they held Certified H&PM Organization; therefore, hospitals that were not certified but implemented H&PM and hospitals that were not at all engaged in H&PM were included in the non-certified group. Future studies should analyze hospitals based on whether H&PM was implemented to verify whether similar results can be obtained. Third, as this study was cross-sectional, causal relationships could not be identified. This study could not determine whether implementing H&PM increased the efficiency of inpatient health care, or if hospitals with high efficiency of inpatient health care were able to engage in H&PM. Therefore, the health issues of staff in hospitals engaging in H&PM should be accurately identified, and appropriate efforts should be determined.
H&PM can be implemented even in hospitals that cannot be certified as specific function hospitals. Considering the importance of improving employee health and productivity, implementing H&PM is valuable regardless of the magnitude of increase in efficiency. Research on the effectiveness of H&PM in medical institutions is limited, and evidence needs to be accumulated through further research.
Conclusion
It was revealed that there is a positive correlation between the certification status of hospitals as Certified H&PM Organizations and the efficiency values of inpatient care derived from DEA. This suggests that hospitals actively engaging in H&PM may provide more efficient inpatient care. The efficiency of health care is a critical concern for hospital administrators. As the burden on hospital staff increases, initiatives to maintain and enhance the health of the staff are essential. Therefore, the findings obtained in this study are valuable. However, further research is needed to elucidate nuances of the causal relationship.
Footnotes
Author Contributions
All authors were involved in study design, data interpretation, and data analysis. HW wrote the manuscript. SM, SK, and YN helped prepare the manuscript. All authors revised and approved the final manuscript.
Data Availability
The data underlying this article will be shared on reasonable request to the corresponding author.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Deanonymized Ethical Considerations
Data were obtained from publicly available sources, and an ethics committee approval was not required.
Consent to Participate
Not applicable.
Consent for Publication
Not applicable.
