Abstract
Despite remarkable progress in the reduction of under-five mortality, the rate of perinatal and neonatal mortality is still high especially in developing countries. The adverse outcome associated with preterm birth is one of the major public health challenges in Africa. However, there are limited and inconsistent studies conducted on the effect of preterm birth on adverse perinatal and neonatal outcomes in Ethiopia. Therefore, this systematic review and meta-analysis aimed to investigate the association between preterm birth and its adverse perinatal and neonatal outcomes in Ethiopia. We systematically searched several electronic databases like PubMed, Web of Science, SCOPUS, CINAHL, Google Scholar, African Journals Online databases and Science Direct. All identified observational studies were included. The
Background
In 2015, 2.8 million (44%) of the 6.3 million deaths in under-five children during the neonatal period and 4.5 million perinatal deaths (2.1 million stillbirths and 2.4 million early neonatal deaths) occurred globally. 2 Preterm birth is the leading cause of neonatal morbidity and mortality. It is the largest single condition in the Global Burden of Disease due to the high mortality and the risk of lifelong impairment among survivors.1,3 Preterm birth is the single leading direct cause of neonatal deaths resulting in 35% of the world’s deaths annually, cause of under-5 deaths and child death in all high- and middle-income countries.3,4 Neonatal and perinatal death associated with preterm birth is an important public health challenge across a range of countries mainly in Sub-Saharan Africa (SSA).5,6 It also imposes an economic burden on the health system due to the most common cause of readmission7–9 and increased length of hospital stay. 10
Preterm birth causes severe neonatal morbidity including the need for assisted ventilation (45.7%),10,11 respiratory distress, 12 sepsis, 10 need for phototherapy and newborn’s morbidity rate doubled in infants for each gestational week earlier than 38 weeks. 13 Premature birth was also associated with mortality during infancy10,14–16 and adulthood.15,17 Additionally, preterm birth affects the likelihood of parenthood; the decreased likelihood of parenthood,18,19 decrease romantic partnership and sexual life of partners.19,20 Preterm birth also increases the risk of malnutrition; underweight or wasted, more often screened positively for disability and neonatal mortality. 21
Different interventions were done in the perinatal and neonatal periods to reduce adverse perinatal and neonatal outcomes of preterm birth. 22 The Global strategy plans to reduce stillbirth at least 25 per 1000 live births and neonatal mortality at least 12 per 1000 live births in every country by 2030. The rate of morbidity and mortality associated with preterm birth was higher and varies in Ethiopia.23–28 There is growing national attention focused on neonatal mortality. Though, adverse perinatal and neonatal outcomes attributed to preterm birth remains high in Ethiopia. There are different studies conducted in Ethiopia on predictors of adverse perinatal and neonatal outcomes. Evidence on the effect of preterm birth on adverse outcomes is inconsistent and inconclusive for national-level health policy and managers across available epidemiologic studies. Unfortunately, there is no pooled study on the effect preterm birth on perinatal mortality, neonatal hypothermia and neonatal sepsis. Therefore, this systematic review and meta-analysis were conducted to estimate the effect of preterm birth on adverse perinatal and neonatal outcomes in Ethiopia.
Methods
Reporting of Systematic Review, Data Sources and Search Strategies
The findings of this systematic review and meta-analysis are reported based on the recommendation of the Preferred Reporting Items for Systematic Review and Meta-Analysis (PRISMA) 2009 statement checklist 29 (SupplementaryTable1). All published articles were searched from major international databases like PubMed, Web of Science, SCOPUS, CINAHL, Google Scholar, Science Direct, African Journals Online databases and Google hand searches. Additionally, a search was made for the reference list of studies already identified to retrieve additional articles.
For each of the selected components of adverse outcomes, electronic databases were searched using keyword search and the Medical Subject Heading [MeSH] words. The keywords include adverse perinatal or neonatal outcomes, perinatal mortality, stillbirth, sepsis, hypothermia OR neonatal mortality as well as Ethiopia. The search terms were combined by the Boolean operators ‘OR’ and ‘AND’.
Population and Outcomes of the Study
The population of interest was all live births from 28 weeks of gestation to 7 days of postpartum period for perinatal outcomes and the first 28 days for neonatal outcomes respectively in Ethiopia. The exposure was preterm birth. Comparisons were defined for each perinatal and neonatal outcome of preterm delivery for each outcome.
The outcome lists were adverse perinatal and neonatal outcomes of preterm birth. The adverse perinatal outcomes included were perinatal mortality and stillbirth. However, neonatal sepsis, hypothermia and neonatal mortality were adverse neonatal outcomes.
Eligibility Criteria and Study Selection
This review included studies that reported adverse outcomes, which included perinatal mortality, neonatal sepsis, hypothermia and neonatal mortality. All studies published from inception to the end of our search, July 27, 2020 published in the English language were retrieved to assess eligibility for inclusion. Case reports of populations, abstracts of conferences, articles without full access and not reported outcomes of interest were excluded. The article selection process passed through different steps. Retrieved articles were screened using their title, abstract and full article review. Study screening and full review of the studies were conducted by two reviewers (MD and GMK). Any disagreement between the two reviewers regarding the selection and inclusion of the studies was resolved by consensus. There was then a full-text analysis of the studies that passed abstract review and whether or not the specified set of criteria had been met and for duplicated records.
Quality Assessment and Data Abstraction
The Newcastle-Ottawa Scale quality assessment tool was used to assess the quality of the included studies based on the 3 components; the selection of the study groups, comparability of the study groups and ascertainment of exposure or outcome. 30 The NOS has 3 categorical criteria with a maximum score of 9 points. The first component emphasized the methodological quality of primary studies, the second component was concerned with the comparability and the third component was used to evaluate the results and statistical analysis of each study. The quality of each study was assessed using the following scoring algorithm: ≥7 points were considered as ‘good’, 4 to 6 points were considered as ‘moderate’, and ≤3 points was considered as ‘poor’ quality studies. Additionally, to improve the validity of the results of this systematic review, only primary studies of fair to good quality were included in the final meta-analysis. Two reviewers (MD and NBY) independently assessed the quality and extracted data from these articles using a standardized data extraction format. The data extraction format included primary author, year of publication, geographic region of the study, sample size, the reported number of cases (live birth who develop the respective outcomes).
Publication Bias and Statistical Analysis
The publication bias was assessed using Egger’s
31
and Begg’s
32
tests with a
Results
Study Identification and Characteristics of Studies
This systematic review and meta-analysis included published studies on the pooled effect of preterm birth on adverse perinatal and neonatal outcomes in Ethiopia using published studies. A total of 375 studies were found from the review. Of these, 185 duplicated records were deleted and 142 articles were excluded by the screening of titles and abstracts. Subsequently, a total of 48 full-text papers were assessed for eligibility based on the inclusion and exclusion criteria. Thus, thirteen studies were excluded due to lack of the outcome of interest,22,35–46 population difference
47
and 1 article was excluded due to lack of access to the full text.
48
Finally, a total of 33 studies were included in the final quantitative meta-analysis (Figure 1). PRISMA flow diagram of the studies in the systematic review and meta-analysis.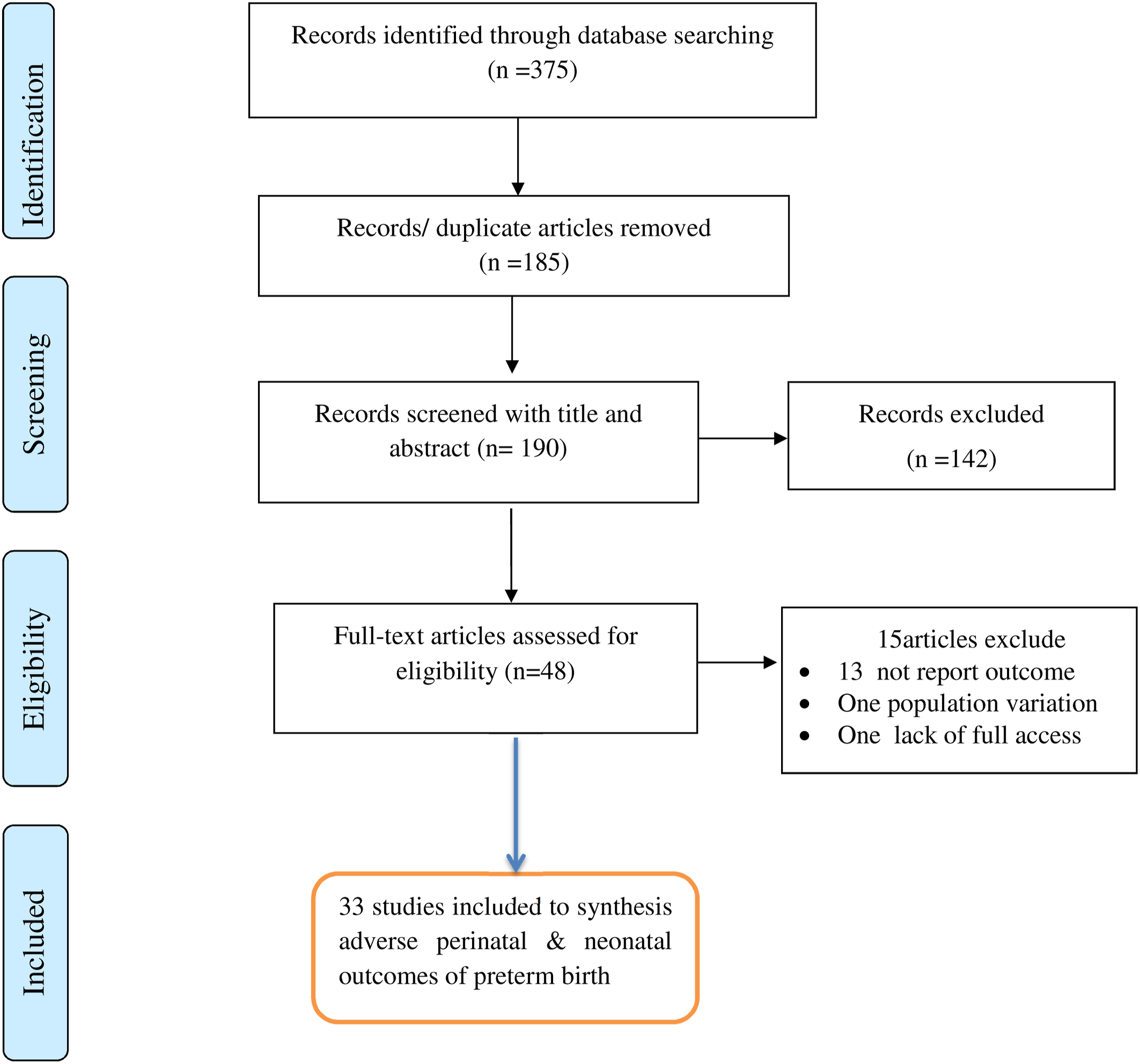
Characteristics of included studies on the effect of preterm birth adverse outcomes.

Impact of Preterm Birth on Adverse Perinatal Outcomes
The pooled random effect analysis of 8 studies showed that neonates born preterm were 10 times [ Forest pot of association of preterm birth and perinatal mortality: meta-analysis. Sub-group analysis of the impact of preterm birth on adverse outcomes by study design.

The pooled effect of 3 studies showed that the odds of stillbirth was 5.44 [ Forest pot of association of preterm birth and stillbirth in Ethiopia: meta-analysis.
Impact of Preterm Birth on Adverse Neonatal Outcomes
The pooled effect of this meta-analysis also showed that preterm birth was significantly associated with neonatal hypothermia and neonatal mortality. This meta-analysis also indicated that there was no significant association between preterm birth and neonatal sepsis (Figure 4). There was no publication bias (Supplementary file 4). The pooled effect of 4 studies revealed that preterm babies had 3.54 times higher odds of neonatal hypothermia than those delivered after 37 weeks of gestational age [ Forest pot of association of preterm birth and neonatal sepsis: meta-analysis. Pooled odds ratio of association of preterm birth and neonatal hypothermia. Forest plot of the impact of preterm birth on neonatal mortality: meta-analysis.
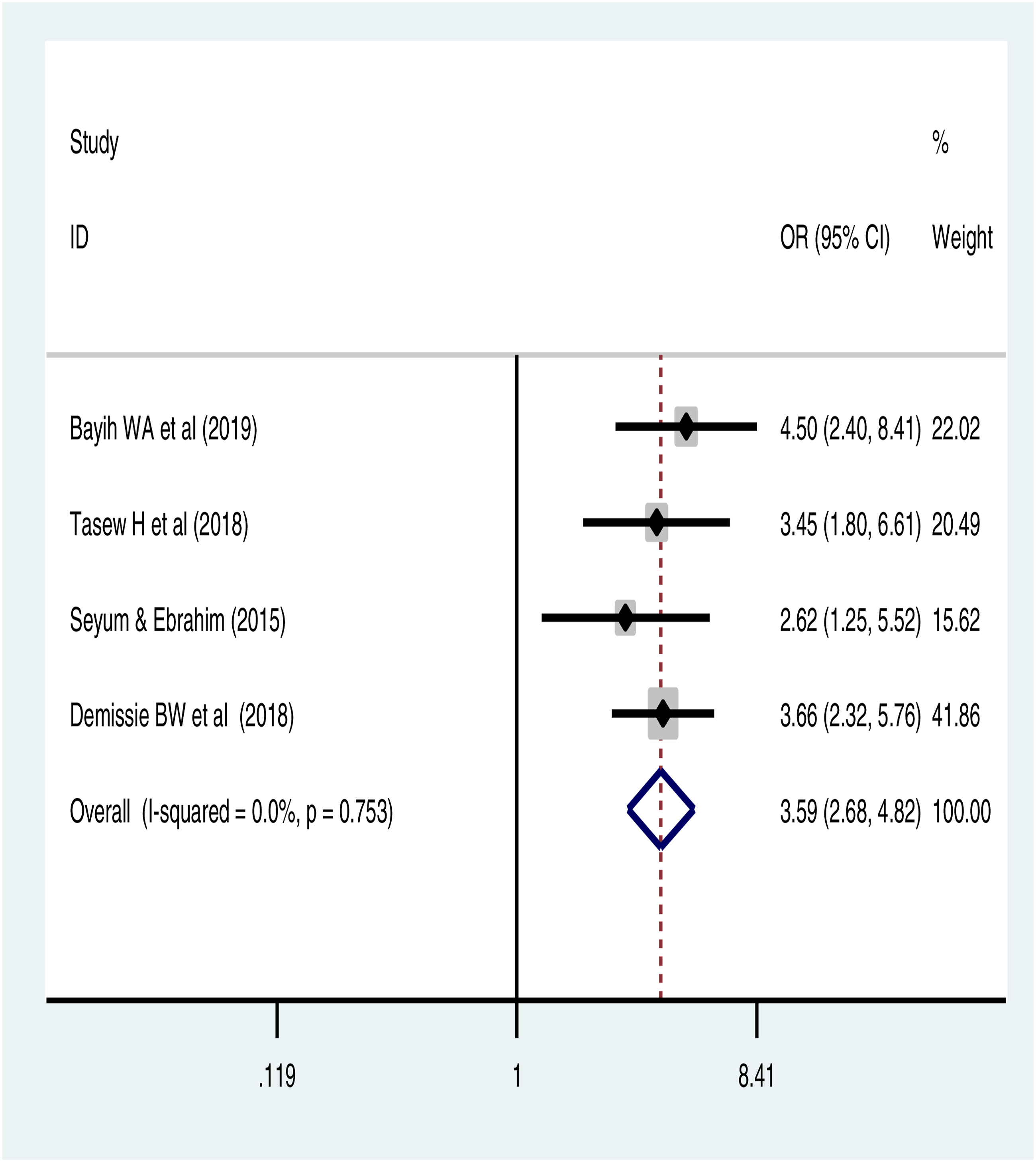
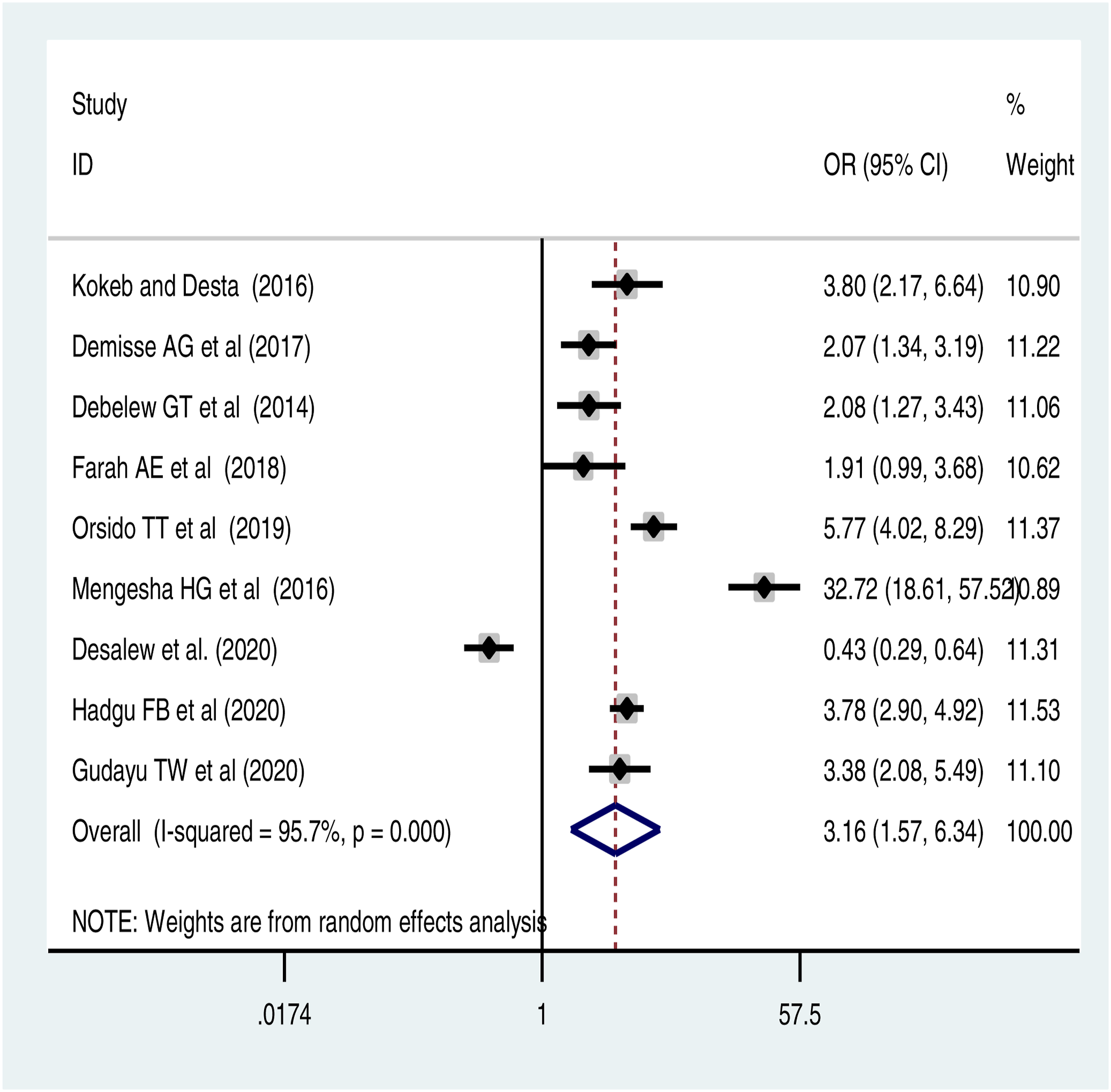
The sub-group analysis based on study design on the role of preterm birth on neonatal sepsis and neonatal mortality was investigated. The pooled effect of 3 case-control studies showed that preterm birth significantly increased the risk of neonatal sepsis by 2-folds [OR=2.33 (95%CI: 1.15, 4.71)] and neonatal mortality was significantly associated with preterm birth based on the sub-group analysis of 6 cohort studies [OR = 3.20 (95% CI: 1.01, 10.1)] and 3 cross-sectional studies [OR = 3.12 (95% CI: 2.10, 4.64)] (Table 2).
Discussion
This systematic review and meta-analysis estimated the association between preterm birth and adverse perinatal and neonatal outcomes using studies conducted in Ethiopia. The current review underscored the significant association between preterm birth and adverse birth outcomes in Ethiopia. The findings of this study showed that the odds of perinatal mortality were higher among preterm babies than those with normal gestational age. This finding is in line with findings reported in Low and Middle-Income Countries (LMICs).75,76 This could be because those neonates born before 37 weeks of gestation might be more likely to have perinatal morbidities mainly due to the high burden of maternal near miss mainly hypertensive disorders and antepartum haemorrhage. Hence, hypertension disorders and antepartum haemorrhage are significantly associated with preterm birth and are known to decrease the feto-maternal perfusion that reduces blood supply to the foetus, asphyxiated and ultimately resulting in death in the perinatal period. This can be also explained because the health services delivery system and a health care system to improve the survival of preterm neonates is limited in the setting 77 including poor uptake of maternity waiting home in the health facility.78–80 Since a systematic review and meta-analysis were done in Africa revealed that maternity waiting for home utilization significantly reduced the risk of perinatal mortality.81,82
This study found that a significant higher odd of stillbirth among preterm babies. This may indicate the preterm newborns might be due to low birth weight and growth-restricted 83 and the poor quality of care in the peripartum period, lack of skilled health personnel, and increased unassisted births and a lack of timely provision of life-saving emergency perinatal services leading to an increased risk of stillbirth. 84 Hence, an improved antepartum care 85 and intrapartum care interventions can reduce stillbirths by 46%. 86 Therefore, the improved survival of preterm babies and the reduction of perinatal mortality rate by providing appropriate care and improvements in the quality of care offered by the health facilities during pregnancy, during labour and after birth are needed.
The present systematic review and meta-analysis also found that preterm birth significantly increased the odds of neonatal hypothermia. This was following with other studies done in Eastern Africa. 87 This finding can be explained by the fact that preterm babies have lower brown body tissue or fat, decrease the potential to maintain body temperature and are easily exposed for hypothermia.88,89 The narrative review of this study also showed higher odds of neonatal near misses among preterm babies than their counterparts. This finding was supported by a study conducted in Brazil.90,91 The neonatal near miss rate was almost 8 times higher than the neonatal mortality rate based on the findings of the systematic review done by Santos JP and his collaborators. 92 Thus, a strategy to reduce the burden of hypothermia and neonatal sepsis among preterm neonates should be scaled up by governmental and non-governmental institutions.
Moreover, the results of our systematic review and meta-analysis also found increased odds of neonatal mortality among preterm babies. This finding is in line with other studies done in Eastern Africa 93 and Europe. 94 This can be explained by the fact that preterm babies have immature lungs and other vital organs, which exposed them to respiratory problems including infections, facing difficulty to adapt the extra-uterine life. Premature newborns are at risk for death during the neonatal period 21 due to higher rates of associated neonatal morbidities such as neonatal sepsis, 95 neonatal near miss and foetal malformations, 96 leukaemia, 97 retinopathy of prematurity,12,21 respiratory distress, feed intolerance and jaundice 98 and neonatal sepsis.98–100
A recent study conducted in Ethiopia also showed the highest rate of preterm mortality was attributed to respiratory problems distress syndrome (45%), infections (30%) and asphyxia (14%). 101 Thus, to reduce morbidity and mortality of preterm neonates improving the interventions during the antenatal, intrapartum and postpartum period for the women and the newborn like optimal care in temperature maintenance, adequate feeding, hygienic cord and skincare, and early detection is needed. Also, treatment of morbidities including respiratory distress syndrome and infections associated with preterm birth is paramount. The observed strong association between preterm birth and adverse perinatal and neonatal outcomes might be linked with an increased risk of ill-health and negative feelings about their baby 102 including anxiety and postpartum depression.103–106 This because depression and anxiety are known factors to reduce caring for themselves and neonates, reduce health care service utilization for the sick newborn, absence of breastfeeding, increase febrile illnesses and malnutrition 107 and increases the risk of near miss, ultimately to mortality.
Therefore, an integrated interdisciplinary approach and interventions on the maternal continuum of care and neonatal care is needed. Scale-up of such interventions to prevent adverse outcomes and long-term impacts of the offspring associated with preterm birth are also recommended. However, the multiple clinical and research disciplines are not practically integrated significantly, mainly obstetricians are more concerned with labour and delivery complications and mental health experts are concerned with mental health problems like antenatal and postnatal depression. A narrative review on the reported outcomes that were unable to do a meta-analysis was conducted, the review showed that preterm birth significantly increased neonatal jaundice, 108 respiratory distress syndrome and neonatal near miss. 109
The current systematic review and meta-analysis are not without limitations. The highest heterogeneity among studies might be explained by the heterogeneity in the characteristics of the studies and may have led to insufficient statistical power to detect statistically significant association. However, a meta-regression analysis was conducted to identify the source of heterogeneity, and, it revealed that there was no variation due to sample size and publication year. The studies were conducted only on the 7 regions which may reduce the representativeness of the country. Future researchers should address the main predictors of preterm neonatal mortality to develop a package of interventions to reduce mortality.
Conclusions
This systematic review and meta-analysis indicated that preterm birth was significantly associated with perinatal mortality, stillbirth, neonatal hypothermia and neonatal mortality. Therefore, improving the quality of intervention programs during antenatal care, intrapartum and neonatal period are essential to reduce preterm birth and its adverse outcomes. The Federal Ministry of Health and other stakeholders should also work towards reduction of adverse perinatal and neonatal outcomes associated with preterm birth.
Availability of Data and Materials
Data will be available from the corresponding author upon reasonable request.
Supplemental Material
sj-pdf-1-inq-10.1177_00469580211064125 – Supplemental Material for Effect of Preterm Birth on the Risk of Adverse Perinatal and Neonatal Outcomes in Ethiopia: A Systematic Review and Meta-Analysis
Supplemental Material, sj-pdf-1-inq-10.1177_00469580211064125 for Effect of Preterm Birth on the Risk of Adverse Perinatal and Neonatal Outcomes in Ethiopia: A Systematic Review and Meta-Analysis by Melaku Desta, Melaku Admas, Yordanos Yeshitila, Belsity Meselu, Keralem Bishaw, Moges Assemie, Nigus Yimer and GetachewKassa Kassa in INQUIRY: The Journal of Health Care Organization, Provision, and Financing
Supplemental Material
sj-pdf-2-inq-10.1177_00469580211064125 – Supplemental Material for Effect of Preterm Birth on the Risk of Adverse Perinatal and Neonatal Outcomes in Ethiopia: A Systematic Review and Meta-Analysis
Supplemental Material, sj-pdf-2-inq-10.1177_00469580211064125 for Effect of Preterm Birth on the Risk of Adverse Perinatal and Neonatal Outcomes in Ethiopia: A Systematic Review and Meta-Analysis by Melaku Desta, Melaku Admas, Yordanos Yeshitila, Belsity Meselu, Keralem Bishaw, Moges Assemie, Nigus Yimer and GetachewKassa Kassa in INQUIRY: The Journal of Health Care Organization, Provision, and Financing
Supplemental Material
sj-pdf-3-inq-10.1177_00469580211064125 – Supplemental Material for Effect of Preterm Birth on the Risk of Adverse Perinatal and Neonatal Outcomes in Ethiopia: A Systematic Review and Meta-Analysis
Supplemental Material, sj-pdf-3-inq-10.1177_00469580211064125 for Effect of Preterm Birth on the Risk of Adverse Perinatal and Neonatal Outcomes in Ethiopia: A Systematic Review and Meta-Analysis by Melaku Desta, Melaku Admas, Yordanos Yeshitila, Belsity Meselu, Keralem Bishaw, Moges Assemie, Nigus Yimer and GetachewKassa Kassa in INQUIRY: The Journal of Health Care Organization, Provision, and Financing
Supplemental Material
sj-pdf-4-inq-10.1177_00469580211064125 – Supplemental Material for Effect of Preterm Birth on the Risk of Adverse Perinatal and Neonatal Outcomes in Ethiopia: A Systematic Review and Meta-Analysis
Supplemental Material, sj-pdf-4-inq-10.1177_00469580211064125 for Effect of Preterm Birth on the Risk of Adverse Perinatal and Neonatal Outcomes in Ethiopia: A Systematic Review and Meta-Analysis by Melaku Desta, Melaku Admas, Yordanos Yeshitila, Belsity Meselu, Keralem Bishaw, Moges Assemie, Nigus Yimer and GetachewKassa Kassa in INQUIRY: The Journal of Health Care Organization, Provision, and Financing
Supplemental Material
sj-pdf-5-inq-10.1177_00469580211064125 – Supplemental Material for Effect of Preterm Birth on the Risk of Adverse Perinatal and Neonatal Outcomes in Ethiopia: A Systematic Review and Meta-Analysis
Supplemental Material, sj-pdf-5-inq-10.1177_00469580211064125 for Effect of Preterm Birth on the Risk of Adverse Perinatal and Neonatal Outcomes in Ethiopia: A Systematic Review and Meta-Analysis by Melaku Desta, Melaku Admas, Yordanos Yeshitila, Belsity Meselu, Keralem Bishaw, Moges Assemie, Nigus Yimer and GetachewKassa Kassa in INQUIRY: The Journal of Health Care Organization, Provision, and Financing
Supplemental Material
sj-pdf-6-inq-10.1177_00469580211064125 – Supplemental Material for Effect of Preterm Birth on the Risk of Adverse Perinatal and Neonatal Outcomes in Ethiopia: A Systematic Review and Meta-Analysis
Supplemental Material, sj-pdf-6-inq-10.1177_00469580211064125 for Effect of Preterm Birth on the Risk of Adverse Perinatal and Neonatal Outcomes in Ethiopia: A Systematic Review and Meta-Analysis by Melaku Desta, Melaku Admas, Yordanos Yeshitila, Belsity Meselu, Keralem Bishaw, Moges Assemie, Nigus Yimer and GetachewKassa Kassa in INQUIRY: The Journal of Health Care Organization, Provision, and Financing
Footnotes
Author Contributions
MD: conceived and designed the study protocol, literature review, data extraction, data analysis, interpretation and wrote up the manuscript.
YGY, BTM, KA, MA and MAA have extracted and analysis data.
GMK and NBY have review and edit the manuscript.
All authors read and approved the final manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
Supplementary files
Supplementary file 1 (S1): Effect of preterm birth on the risk of adverse perinatal and neonatal outcomes in Ethiopia: a systematic review and meta-analysis
Supplementary file 2: The Newcastle – Ottawa Scale (NOS) quality assessment of studies
Supplementary file 3: funnel plot on the association of preterm birth and perinatal mortality
Supplementary file 4: funnel plot on the association of preterm birth and neonatal sepsis
Supplementary file 5: funnel plot on the association of preterm birth and neonatal hypothermia
Supplementary file 6: funnel plot on the association of preterm birth and neonatal mortality
Appendix A
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
