Abstract
Postmastectomy bras are essential for providing support and comfort to breast cancer survivors during recovery. However, existing designs primarily focus on functionality while often overlooking physiological comfort, which affects prolonged wearability. This study provides a comparative evaluation of mastectomy bras with different prosthetic materials, offering insights into their thermal and evaporative resistance measured using a thermal manikin under both dry and wet conditions. Results indicate that bras with silicone prostheses exhibit lower thermal resistance (Rcf = 0.051 ± 0.002 K m2/W) and evaporative resistance (Ref = 12.1 Pa m2/W) compared to foam prostheses, facilitating greater heat dissipation and moisture permeability. This research highlights the influence of prosthetic design, particularly the wavy back structure of silicone prostheses, in enhancing airflow and reducing heat buildup. In addition, the nonabsorbent nature of silicone contributes to moisture runoff, affecting weight retention in the bra. This study provides clinically relevant insights into how prosthetic material and design influence thermal regulation and overall physiological comfort, which can inform future advancements in mastectomy bra development. By addressing both material selection and structural design, these findings contribute to optimizing postmastectomy garments for improved patient comfort. Future research should incorporate wear trials to validate these results and refine prosthetic bra designs for broader clinical applications and user-centered improvements.
Breast cancer (BC) is a disease characterized by the uncontrolled growth of abnormal breast cells, leading to tumor formation. 1 According to the World Health Organization, 2.3 million women were diagnosed with BC in 2022, and by the end of that year, 7.8 million women were living with a BC diagnosis from the previous five years, making it the most common cancer worldwide. 2 In Saudi Arabia, 2459 BC cases were reported by the Saudi Cancer Registration report for 2020. 3 BC accounted for 17.8% of all cancers reported among Saudis and 31.4% of all cancers reported among women, with an age-specific rate (ASR) of 28.4 per 100,000 among the Saudi female population. 3 In the United States, the risk of developing BC increases with age: 1 in 69 in their 40s, 1 in 38 in their 50s, and 1 in 27 in their 60s. 5 Similarly, in Saudi Arabia, the risk is 1 in 2000 in the 40s, 1 in 1400 in the 50s, and 1 in 1100 in the 60s. 3 BC can be fatal if not treated promptly, as it may metastasize to other parts of the body.2,4,5
BC treatment often begins with a mastectomy, the surgical removal of one or both breasts, including lymphatic vessels and adjacent lymph nodes.2,6,7 Advances in treatment and population screening in recent years have reduced BC mortality rates despite increased diagnoses, 8 leading to a growing population of survivors. Following surgery, many women choose to wear mastectomy bras and breast prostheses to restore their physical appearance and boost confidence.9,10 The comfort of mastectomy bras is critical for postmastectomy patients, as conventional bras may cause discomfort due to sensitive skin irritation, band tightness, and rough seams.9,11–13 Moreover, conventional bras often lack the specific design features required to provide adequate support and stability for women using external breast prostheses (EBPs). 14
Several studies have sought to enhance the comfort of mastectomy bras and prostheses. Fleischman-Ament et al. 15 developed a bra with an inner lining and a prosthesis pocket to reduce irritation and maintain coolness, whereas Shin et al. 16 assessed the thermal and moisture control performance of mastectomy bras and EBPs, focusing on how different designs and materials affect comfort, with particular attention to thermal and evaporative resistance as key factors influencing physiological comfort. Van Dorp and Van Eijsden 17 designed a mastectomy garment focusing on comfort and support. In addition, Solomito et al. 18 used thermal manikins to evaluate the thermal comfort of prostheses. However, there is limited research on how mastectomy bras interact with various prostheses in terms of heat and moisture management.
The concept of comfort in mastectomy garments is multifaceted, encompassing aspects such as fit, support, and thermal regulation, all of which contribute to physiological comfort. Heat and moisture management are critical in ensuring postmastectomy bras provide sufficient comfort. Thermoregulation involves two key factors: thermal resistance (Rct), which represents the fabric’s ability to resist heat transfer, and evaporative resistance (Ret), which measures the resistance to moisture vapor transfer. High thermal resistance in a fabric can lead to heat buildup, while high evaporative resistance can trap moisture against the skin, leading to discomfort. Given that breast prostheses and mastectomy bras are worn close to the skin, their thermal and evaporative properties significantly impact overall physiological comfort.
EBPs are artificial breast forms designed to replace the natural breast after mastectomy, aiding in body symmetry and posture.19,20 Studies have shown that EBPs contribute to improved body image, confidence, and overall quality of life. 20 However, discomfort remains a major concern, particularly in relation to heat and sweat accumulation.20–24 Leung et al. 25 demonstrated that traditional silicone-based prostheses increase core body temperature due to their low breathability, highlighting the need for improved designs with better thermal regulation. Shin et al. 16 further explored the thermal and moisture control properties of different mastectomy bras and prostheses, concluding that heat-reduction designs improved comfort. In addition, McGhee et al. 26 investigated the effect of EBP mass on bra strap pressure, finding that while reducing prosthesis weight decreased pressure, it did not necessarily improve overall comfort.
Comfort in mastectomy garments is complex and requires careful consideration of design, materials, and thermoregulation. Despite previous studies on mastectomy bras and EBPs, limited research has explored how prosthetic design elements influence the thermal and moisture properties in a mastectomy bra ensemble. This study aims to bridge this gap by evaluating the combined effect of material composition and prosthetic design on thermal comfort using a thermal manikin, which can simulate body surface heating, core temperature, body surface moisture, and the human breathing process, making it ideal for thermal comfort experiments. The findings will contribute to the development of improved postmastectomy garments that enhance wearer comfort through better heat and moisture control.
Aims and objectives
The physical properties of textile materials involve a complex interaction of heat and moisture transfer, which significantly impacts physiological comfort. This study aims to evaluate the thermal and evaporative resistance of a postsurgery bra, both independently and in combination with EBPs, under controlled steady-state conditions.
To measure thermal resistance (Rct). Assess the postsurgery bra’s ability to regulate dry heat transfer, both alone and in combination with EBPs, under a controlled temperature gradient. To determine evaporative resistance (Ret). Evaluate the garment assembly’s effectiveness in managing moisture by simulating controlled perspiration using a thermal manikin. To analyze comfort performance. Compare the thermal and evaporative properties of the postsurgery bra with and without prostheses to understand their combined impact on wearer comfort.
Materials and methods
A possible solution for replicating wear conditions more closely in the lab is to test garments on a thermal manikin and in a climate chamber. This approach allows factors such as garment fit, vent positioning, body movement, and variable climatic conditions to be accounted for. This method has the advantage of being controllable and repeatable, providing objective assessment data.
Postsurgery bra and prostheses
After surgery, women prefer to wear a soft, nonwired bra that is not too restrictive. In this study, the most widely used postsurgery bra with front closure was purchased online from Amoena Frances SB. The main fabric of the bra is 90% cotton and 10% spandex, while the pocket lining consists of 94% cotton and 6% spandex. The bra was tested under both dry and wet conditions on a female thermal manikin to assess the effect of metabolic heat and sweating on the transfer of heat and moisture to the environment. Furthermore, the postsurgery bra with two different prostheses (foam and silicone) was tested on a male manikin. The most frequently sold prostheses were selected for this study.
The EBPs tested included the following.
Foam prostheses: Amoena weighted leisure prostheses—132 N, made of polyurethane foam, size: 7. Silicone prostheses: Amoena essential 3 S breast prostheses—363, made of Polyurethane (PU) film, silicone, and phase-change material, size: 7.
These most commonly used prostheses were chosen to compare the impact of material composition on thermal comfort. The full bra assembly on the manikin with different prostheses is shown in Figures 1(a)–1(c).

(a) Postsurgery bra, (b) with foam prostheses, and (c) with silicone prostheses.
Thermal resistance
All the samples were preconditioned for 24 h in a standard climate-controlled room maintained at 20°C ±1°C and 65% ± 5% relative humidity before testing. The weights of the postsurgery bra, foam prostheses, and silicone prostheses were measured as 74, 360, and 880 g, respectively. The experimental setup followed the ASTM F1291-22 Standard Test Method for Measuring the Thermal Insulation of Clothing Using a Heated Manikin.
The test was conducted using a Thermetrics Newton thermal manikin, which is segmented and controlled to simulate body heat dissipation. For the dry thermal resistance measurements, the manikin was operated in passive (nonsweating) mode to assess insulation performance without moisture generation. The manikin was programmed to maintain a constant surface temperature of 35°C to replicate the average skin temperature. The lab conditions were kept stable with an ambient temperature of 20°C ± 1°C and relative humidity of 65% ± 5% according to the standard (Table 1).
Test parameters for dry test
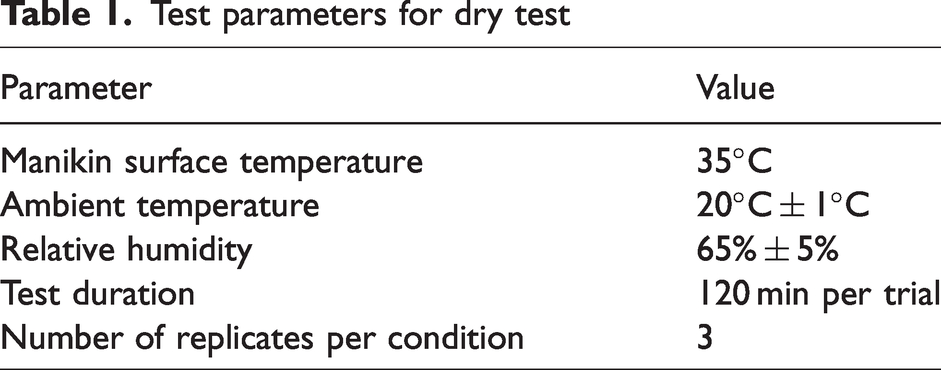
Although preconditioning was performed at 20°C in accordance with ASTM F1291-22, we acknowledge that this may result in additional equilibration time during testing, as the fabric adjusts to the elevated manikin surface temperature of 35°C. While this step ensures standardization and consistency with the test method, future protocol refinements could explore preconditioning at temperatures closer to the test condition to reduce test duration and enhance moisture equilibrium.
Initially, the thermal resistance of the nude female manikin (Rct0) was measured as a reference. The female attachment (breast) was used with the manikin to test the thermal resistance of the postsurgery bra alone. The manikin was then dressed in the bra, and the total thermal resistance of the system (Rct) was measured. The intrinsic thermal resistance of the bra (Rcf) was calculated using the following equation:
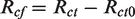
To minimize variability, only the zones covered by the bra (chest front/back) were selected in the software to calculate the group-weighted average thermal resistance, as shown in Figure 2.
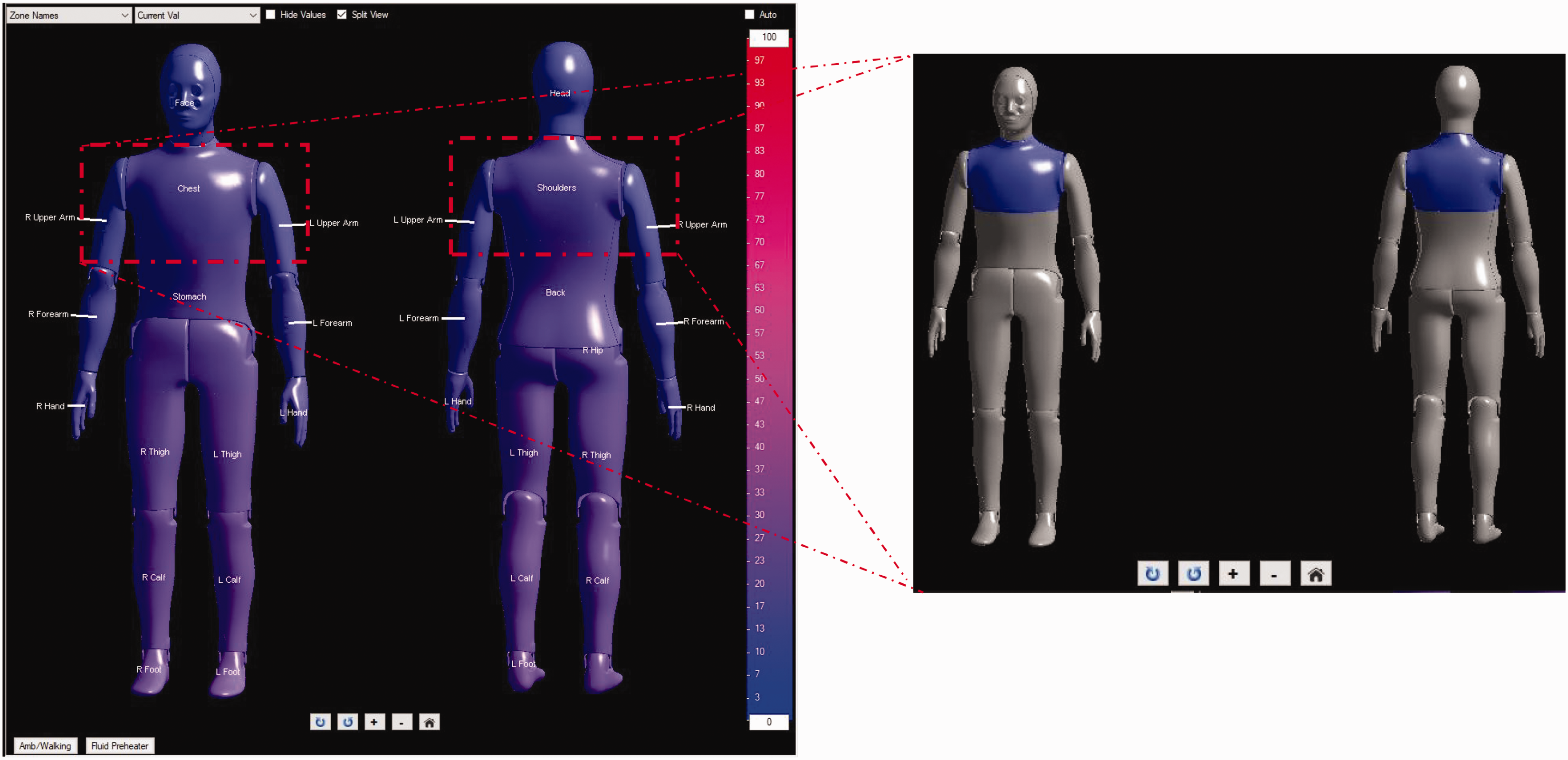
Screenshot from the ThermDAC software defining the group-weighted zone for the bra.
The female attachment (breast) was then removed, and the male manikin was used to assess the thermal resistance of the bra with the foam and silicone prostheses. Again, the nude male manikin was tested to establish Rct0, and then the thermal resistance of the full garment prosthesis system was measured.
Infrared thermal imaging analysis
Infrared (IR) thermography was used to visualize heat distribution across the bra and prostheses to complement the thermal resistance measurements. IR images were taken at the end of each test to assess temperature variation at different points on the bra surface. IR images were taken after approximately 2 h to allow sufficient time for thermal equilibrium to be reached between the manikin, the prostheses, and the surrounding environment. This duration was chosen based on preliminary tests, which showed that temperature stabilization occurred within this timeframe. While heat transfer rates may vary depending on the prosthetic material, the 2-h period ensures a stable temperature profile, minimizing transient effects that could influence the thermal resistance measurements. This approach aligns with standard practices in thermal manikin studies for assessing clothing insulation.
Evaporative resistance
All test samples were conditioned in the manikin lab at a controlled temperature of 35°C and relative humidity of 40% for 24 h prior to testing, as required by the ASTM F2370 Standard Test Method for Measuring the Evaporative Resistance of Clothing Using a Sweating Manikin. This ensured that the samples reached equilibrium under test conditions before measurement. A sweating thermal manikin with a controlled water supply system was used to simulate perspiration during testing. For the wet evaporative resistance tests, the manikin was set to active (sweating) mode with a controlled sweat flow rate of 200 g/(m2·h) to simulate perspiration.
Test parameters for wet test
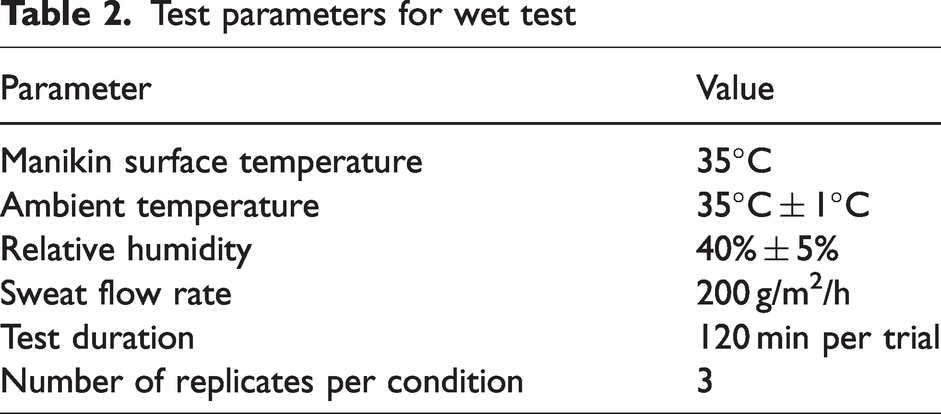
Table 2 presents the test parameters used for the wet tests to evaluate the evaporative resistance (Ret) of the samples.
Like the thermal resistance tests, a baseline measurement was obtained by conducting a nude manikin test (without a bra) to determine the evaporative resistance of the wet nude female manikin (Ret0). This value was used as a reference to calculate the intrinsic evaporative resistance (Ref) of the test samples using the equation
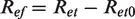
To assess the impact of the postsurgery bra on evaporative resistance, the female manikin was first dressed in the bra and subjected to wet testing under standard conditions. Following this, the evaporative resistance of the bra in combination with prosthetic inserts was tested. The female attachment (breast) was removed, and the male manikin was dressed in a bra with foam prostheses and silicone prostheses. Again, a wet nude male manikin test was conducted to determine the Ret0 before measuring the total evaporative resistance of the prosthetic ensembles.
The Thermetrics Newton thermal manikin is factory-calibrated and undergoes routine validation of its temperature and sweat flow sensors. Prior to testing, the calibration was verified using reference garments provided by Thermetrics, ensuring both temperature and sweat flow accuracy were within the tolerance limit in accordance with ASTM F1291-22 and ASTM F2370 standards.
Results and discussion
Thermal resistance
All tests were conducted in triplicate, and the mean values with standard deviations were reported. The average Rct values for different configurations were as follows:
bra, 0.045 ± 0.003 K m2/W; bra with foam prostheses, 0.063 ± 0.002 K m2/W; bra with silicone prostheses, 0.051 ± 0.002 K m2/W.
A one-way analysis of variance test was conducted to determine whether the differences in thermal resistance among the three ensembles were statistically significant. Figure 3 presents the thermal resistance results graphically.
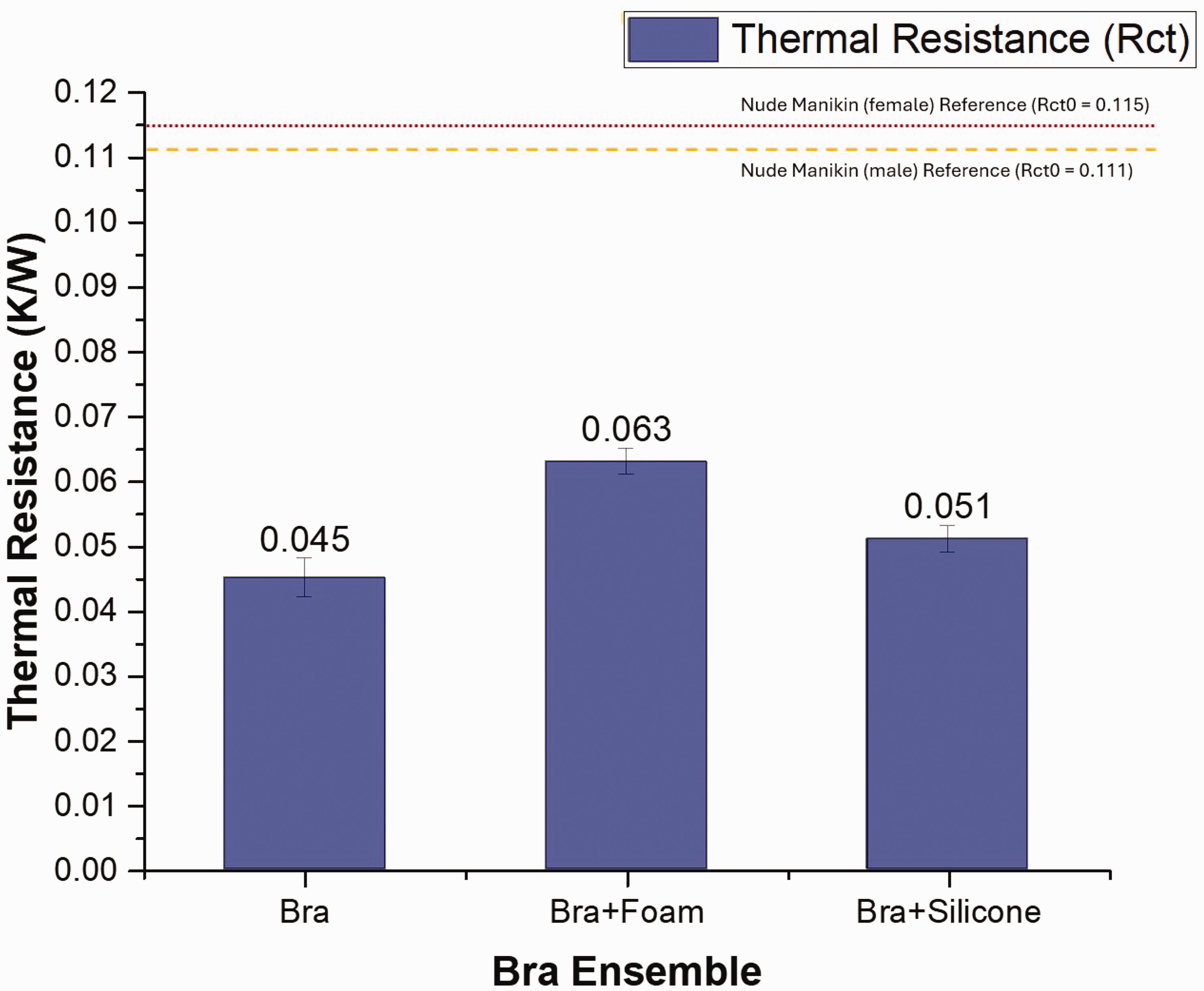
Thermal resistances (Rct) of bra ensembles.
IR images (Figures 4 and 5) illustrate the heat retention properties of foam and silicone prostheses.
Foam prostheses: The temperature at spot 1 was nearly equal to the ambient temperature, and the final temperature increase at this location was only 2.2°C. This suggests that the air pockets in the polyurethane foam structure (Figure 6) trapped body heat, reducing heat dissipation through the prostheses and bra.
Air pockets in foam prosthesis. Silicone prostheses: The final temperature rise was 3.1°C, indicating lower thermal resistance. The wavy back structure of the silicone prostheses (Figure 7) facilitated airflow through channels, enhancing heat dissipation.
Wavy back structure of silicone prosthesis.


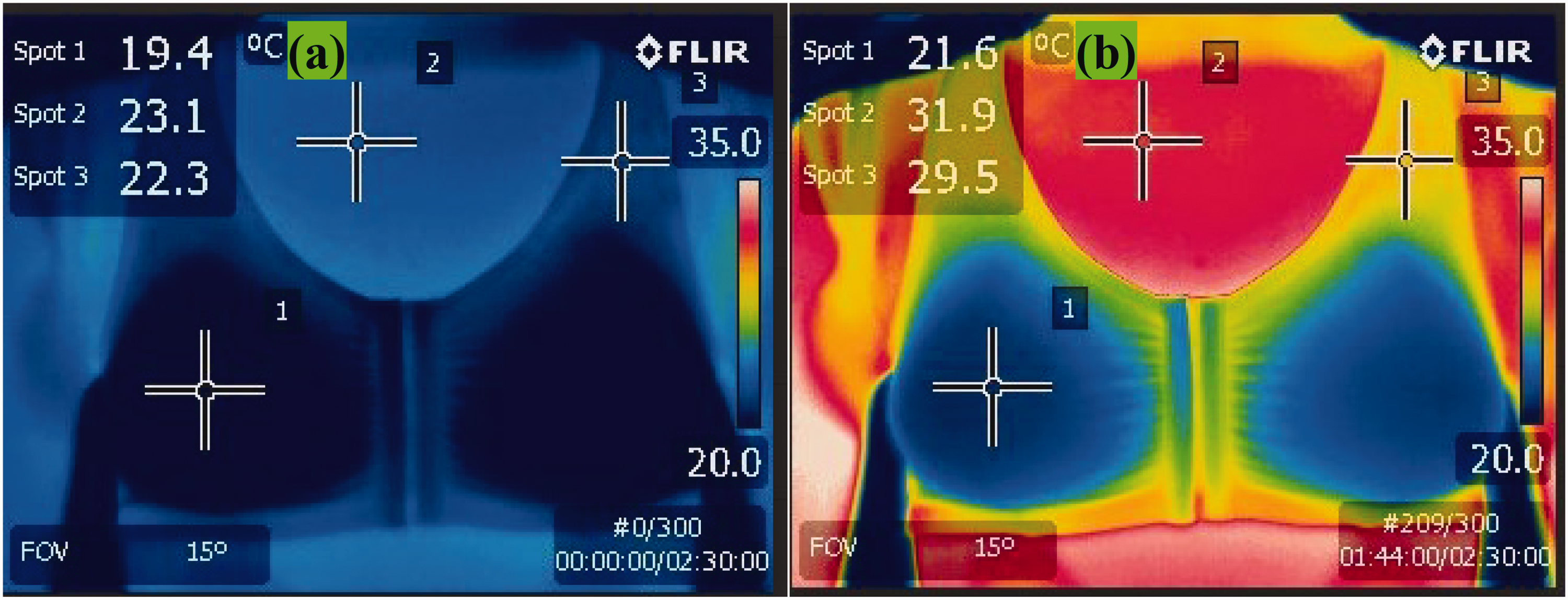
Infrared image of the bra with foam prostheses at (a) the start of the test and (b) the end of the test.
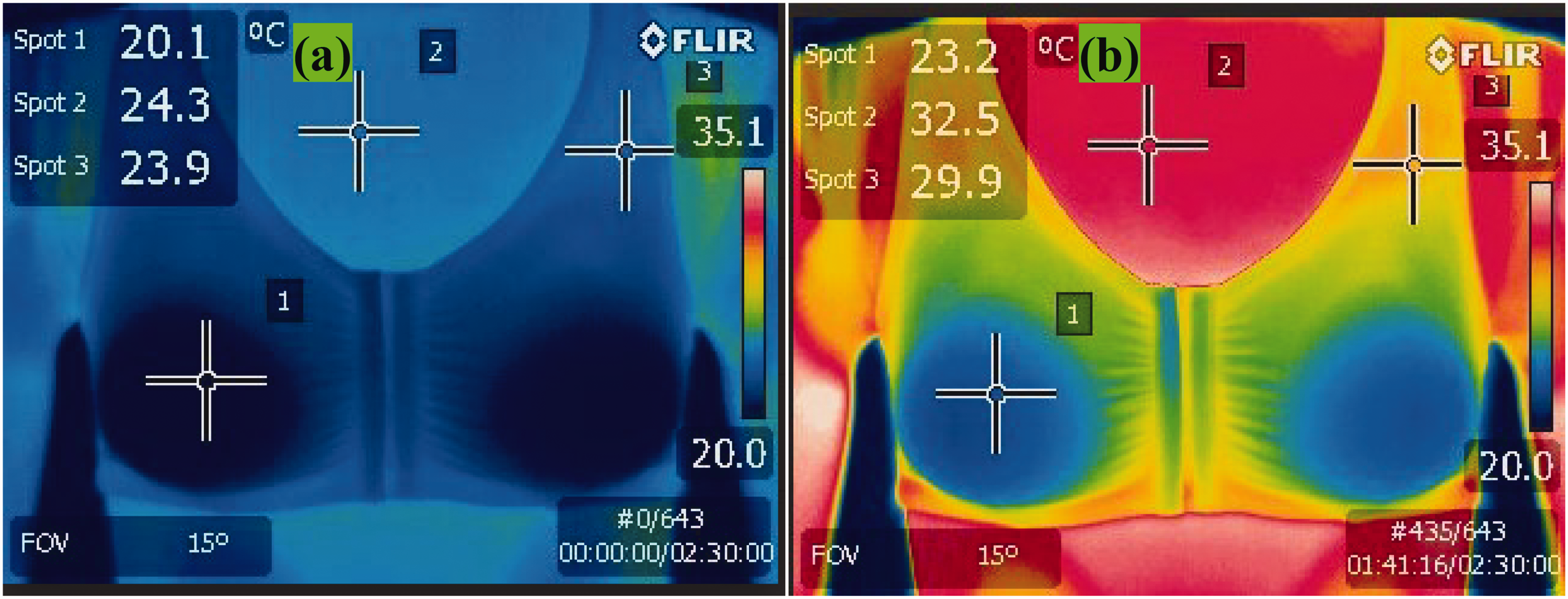
Infrared image of the bra with silicone prostheses at (a) the start of the test and (b) the end of the test.
These results indicate that while foam prostheses are lighter, they provide higher thermal resistance than silicone prostheses, affecting heat retention and wearer comfort.
The IR images in this study were used to observe relative temperature differences rather than absolute surface temperatures. Due to variations in fabric surface emissivity, reflectivity, and transmittivity, affected by characteristics such as color, moisture content, and texture, the reported temperatures should be interpreted qualitatively. As standard emissivity values were assumed, the thermal imaging results serve as approximate indicators of heat distribution across the bra ensembles.
Evaporative resistance
Three replicate tests were performed for each ensemble to ensure statistical reliability. The average Ret values were recorded as follows:
bra, 6.9 ± 1.0 Pa m2/W; bra with foam prostheses, 14.0 ± 2 Pa m2/W; bra with silicone prostheses, 12.1 ± 1.0 Pa m2/W.
The graphical results of evaporative resistance for all three bra ensembles are presented in Figure 8.
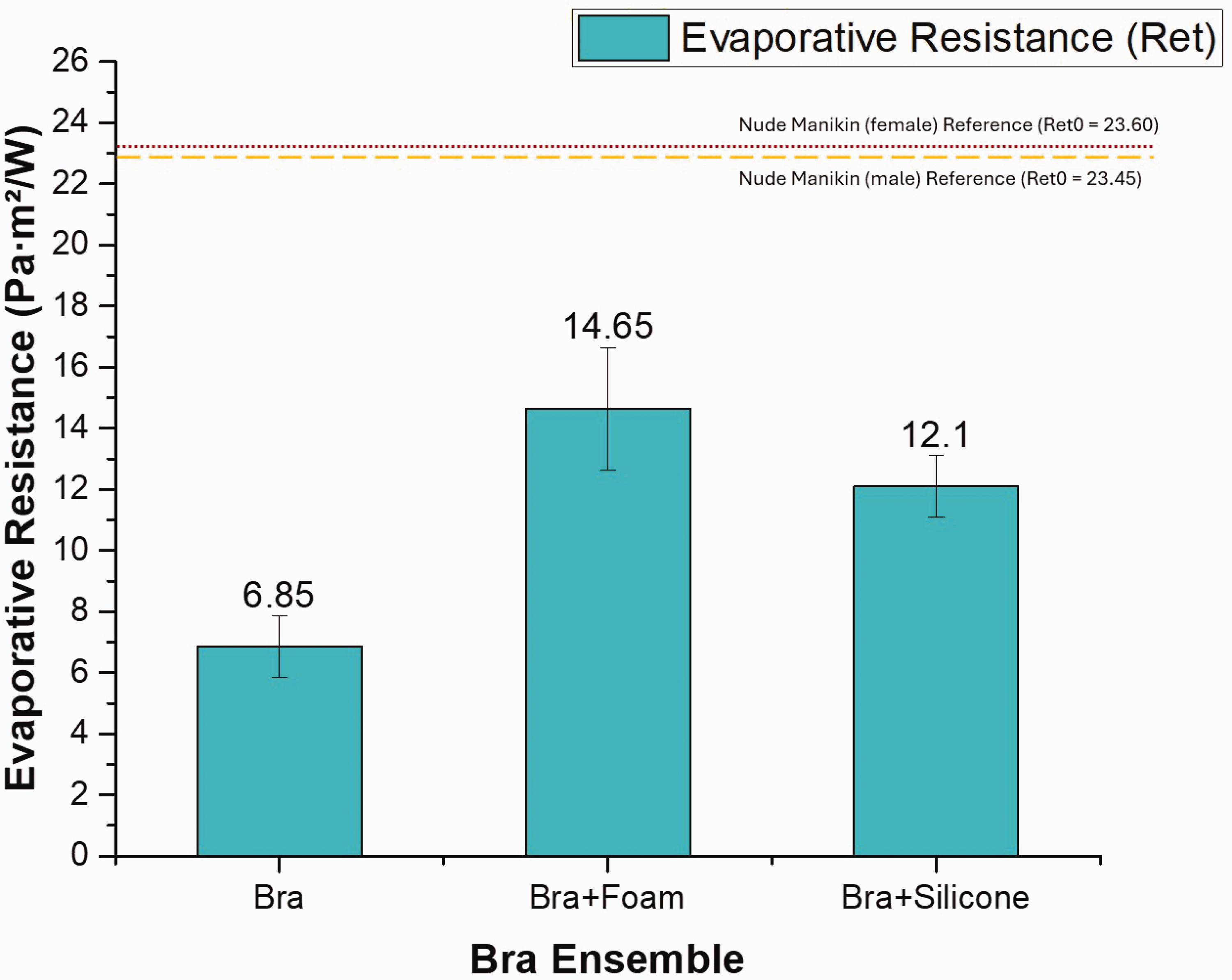
Evaporative resistances (Ret) of bra ensembles
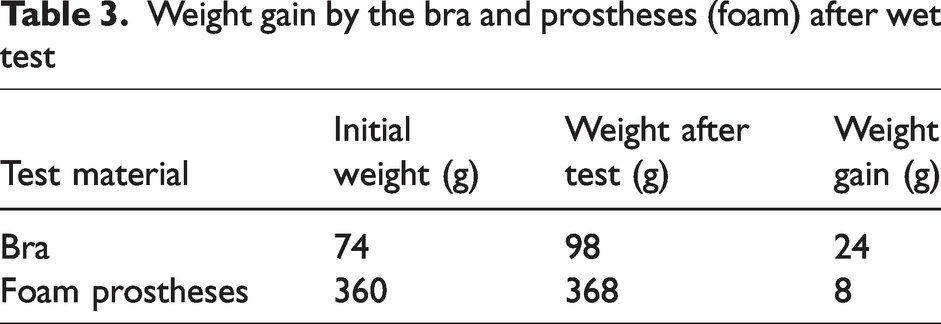
Weight measurements were taken at the start and end of each test to quantify the moisture retention in the bra and prosthetic inserts. The weight gain results are detailed in Tables 3 and 4.
Weight gain by the bra and prostheses (foam) after wet test
Weight gain by the bra and prostheses (silicone) after wet test
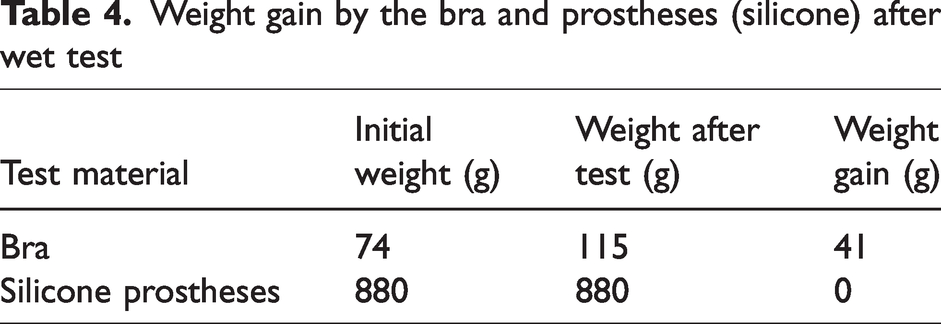
When the bra alone was tested, the weight gain after the wet test was approximately 45 g. This can be attributed to cotton fabric’s ability to absorb moisture without feeling damp, as previously reported by Leung et al.25 However, when the silicone prostheses were included, all absorbed moisture was retained within the bra, as silicone is water-resistant and does not absorb sweat. This resulted in a higher post-test weight compared to the initial measurement. These findings align with previous studies, which reported that women wearing silicone-based EBPs experienced sweat and heat buildup between their skin and the prostheses.
In contrast, when the foam prostheses were used, most of the sweat was absorbed by the foam itself, with only a small portion passing through to the bra. This is reflected in the evaporative resistance results, where the foam prosthesis ensemble exhibited the highest resistance (14.7 Pa m2/W), while the bra alone showed the lowest (6.9 Pa m2/W). The higher Ret value of the foam prosthesis ensemble indicates limited moisture transfer and reduced heat dissipation due to trapped sweat.
Conversely, the lower Ret value of the silicone prosthesis ensemble (12.1 Pa m2/W) suggests greater moisture permeability, not because silicone absorbs moisture, but due to its inability to retain sweat, leading to runoff rather than accumulation. In addition, the wavy back structure of the prosthesis may have contributed to improved airflow and heat dissipation, further preventing excessive moisture buildup (see Figure 7). Despite their superior heat dissipation and moisture permeability, the significantly higher weight of silicone prostheses may influence wearer preference, particularly for extended use. Future investigations should consider the trade-off between thermal comfort and overall wearability.
In light of the above findings, future mastectomy bra designs should carefully balance prosthesis material and weight, leveraging silicone’s wavy‐back channels to promote airflow and moisture runoff, while also considering lighter alternatives that reduce overall mass without compromising stability. Fabric selection is equally important, with moisture-wicking inner linings combined with breathable outer layers to efficiently manage sweat and enhance wearer comfort.
Conclusion
This study has used a thermal manikin to evaluate the thermal and evaporative resistance of a mastectomy bra paired with different breast prostheses under both dry and wet conditions. The results have shown that the bra with silicone prostheses exhibited lower thermal and evaporative resistance compared to the bra with foam prostheses. This difference can be attributed to the inability of silicone to absorb moisture, leading to sweat runoff rather than retention, as well as the wavy back structure of the silicone prostheses, which may facilitate some airflow and heat dissipation. In contrast, the foam prostheses absorbed moisture, increasing their overall thermal resistance and evaporative resistance due to moisture retention within the material. This highlights the importance of prosthetic material properties in moisture management and heat dissipation, which directly impact wearer comfort.
This study underscores the role of prosthetic design in influencing heat dissipation and moisture management. While silicone prostheses demonstrated better thermal and moisture management, their increased weight must be considered in the overall comfort assessment. Further investigations should explore material innovations that balance thermal performance with weight reduction.
The findings highlight the potential for future developments in mastectomy bras that integrate improved ventilation structures, adaptive materials, and ergonomic design considerations. Such advancements could offer better comfort and wearability for postmastectomy patients. Given that comfort perception and pressure distribution were not directly measured, future research should focus on human trials to assess these factors in real-world conditions. In addition, the development of high-performance materials, such as moisture-wicking textiles, breathable foams, or adaptive smart fabrics, could further improve prosthetic bra designs, ensuring that they effectively meet the diverse needs of BC survivors.
Footnotes
Acknowledgment
The authors, acknowledge with thanks WEFT (Research Centre), RMIT University, Australia and Deanship of Scientific Research (DSR) at King Abdulaziz University, Jeddah for technical and financial support.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
This project was funded by the Deanship of Scientific Research (DSR) at King Abdulaziz University, Jeddah, under grant no. J: 72-253-1442. The research was also supported by the Australian Research Council (ARC) through Linkage Project LP190101294, in collaboration with Hunting Lady Pty Ltd, trading as Ventou Garment Technology.
