Abstract
Adenoid cystic carcinoma (AdCC) is a malignancy that most frequently originates in the salivary glands of the head and neck, though it may also rarely occur in other sites such as the trachea or breast. It is characterized by its slow-growing nature in the early stages, along with distinctive features of perineural invasion and a tendency for late metastasis, particularly to the lungs. Recurrence or metastasis can occur even years after the initial treatment. Currently, no standardized clinical protocol exists for long-term follow-up. The disease can recur or metastasize even years after initial treatment. At present, no uniform clinical protocol exists for long-term follow-up. To our knowledge, no documented cases of retrograde metastasis from primary pulmonary AdCC to the tongue have been reported. We describe the case of a male patient in his 40s with primary low-grade pulmonary AdCC who developed lingual metastasis after aggressive treatment. This case highlights an unusual metastatic pattern and underscores the need for vigilant, long-term monitoring of patients with AdCC.
Keywords
Introduction
Adenoid cystic carcinoma (AdCC) is the most common malignant tumor of the salivary glands, typically occurring at various sites within the head and neck region. 1 However, it can also originate in secretory glands outside the head and neck, such as those in the mammary gland, 2 tracheobronchial tree,3 or cervix. In the head and neck, primary AdCC often invades blood vessels and metastasizes hematogenously, most commonly to the lungs. 4 Some patients achieve long-term survival despite the presence of metastatic tumors. 5 In contrast, primary tracheobronchial adenoid cystic carcinoma (TAdCC) is rare, and retrograde metastasis to the tongue base has not been previously reported. This case report presents a unique instance of primary pulmonary AdCC with metastasis to the tongue base, providing a detailed account of this metastatic process and offering observations that may inform the understanding of AdCC progression.
Case report
A male patient in his 40s was referred to the Thoracic Surgery Department at The Affiliated Hospital of Qingdao University in October 2018. His symptoms included a cough with sputum and occasional hemoptysis. Chest CT revealed a space-occupying lesion in the right lung hilum (Figure 1(A)). Pathological examination following a biopsy of the middle stem of the right lung confirmed TAdCC (Figure 2(A)). An oral surgery consultation revealed no obvious abnormalities in the head and neck area (Figure 1(D) and (G)), leading to a diagnosis of primary TAdCC of the trachea and bronchi.

Imaging features of AdCC metastasis (tumor indicated by red arrow).
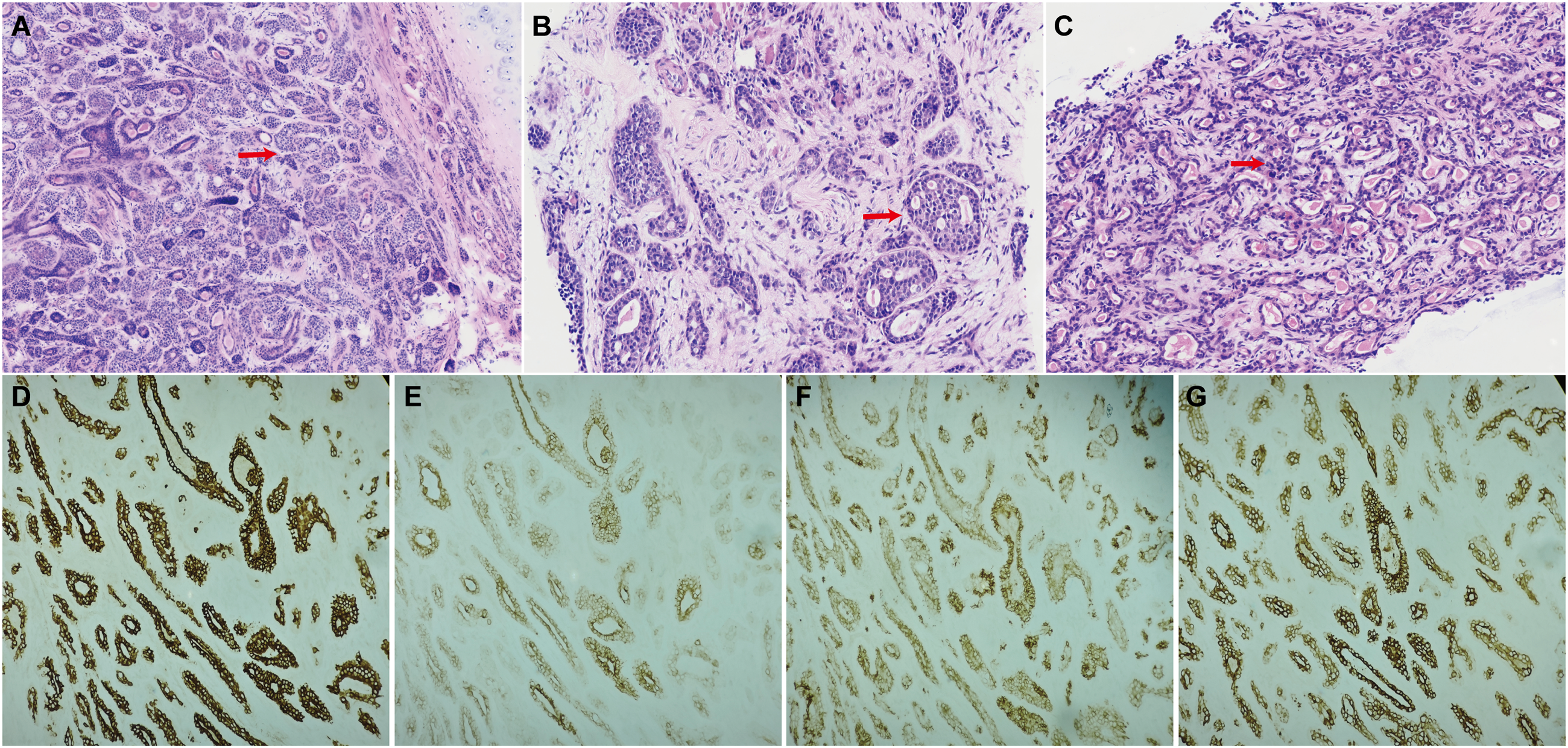
Histopathological examinations confirmed AdCC (the cribriform and tubular pattern in the tumor is indicated by the red arrow, ×80). (A) Primary pulmonary lesion. (B) Liver metastasis. (C) Tongue base metastasis. (D–G). Immunohistochemical profile of the primary lesion demonstrating positive staining for (D) CK8/18, (E) CK19, (F) CD117, and (G) CK7.
Written informed consent was obtained from the patient after a detailed explanation of the procedure. The patient subsequently underwent robot-assisted sleeve resection and regional lymph node dissection of the middle and lower lobes of the right lung, achieving R0 resection. Postoperative immunohistochemical analysis showed positive results for CK8/18, CK19, CD117, and CK7 (Figure 2(D) to (G)). Amplification Refractory Mutation System PCR (ARMS-PCR) testing revealed no mutations in EGFR, ALK, ROS, or BRAF. Following surgery, the patient underwent six cycles of pemetrexed (500 mg/m2) combined with nedaplatin (80 mg/m2) on day of a 21-day cycle, followed by 28 sessions of thoracic radiotherapy (Figure 1(B) and (C)).
Unfortunately, a reexamination in December 2020 revealed a suspicious liver lesion on routine chest CT (Figure 1(E)). Further PET-CT showed an irregular, low-density mass near the inferior vena cava in the upper segment of the right posterior lobe of the liver, with uneven metabolic uptake. No abnormal metabolic activity was observed in the lungs or head and neck (Figures 1(H) and 3). A biopsy confirmed metastatic AdCC in the liver (Figure 2(B)). The patient subsequently underwent laparoscopic partial hepatectomy at the hepatobiliary surgery department. The patient then received combination therapy with camrelizumab (200 mg, day1), nab-paclitaxel (300 mg, day1), and carboplatin (600 mg, day1) administered every 3 weeks for six cycles. Follow-up MR imaging revealed no further progression of the liver metastasis (Figure 1(F)).

PET-CT imaging characteristics two years after pulmonary surgery. Abnormal radioactive uptake in the liver (red arrow), and no abnormalities observed in the tongue.
In May 2022, the patient developed an odynophagia and presented to the oral and maxillofacial surgery department. A hard lump was identified at the base of the tongue (Figure 1(I)). A biopsy confirmed the presence of AdCC (Figure 2(C)). Following the diagnosis of lingual AdCC metastasis, the patient provided informed consent for both the publication of this case report and subsequent treatment. Due to the patient's inability to tolerate surgery, radiotherapy was administered to the head and neck tumor region (6000 cGy/24F). Unfortunately, the patient ultimately succumbed to drug-induced liver damage and bone marrow suppression following chemotherapy and radiotherapy. We have de-identified all patient details. The reporting of this study conforms to CARE guidelines. 6
Discussion
AdCC is one of the most unpredictable tumors of the head and neck. Primary TAdCC exhibits biological behaviors similar to those of salivary gland adenoid cystic carcinoma (SAdCC), with common metastatic sites including the liver, bones, brain, and kidneys. 7 In this case, clinical and radiological evaluations during the initial treatment phase excluded the possibility of a primary oral AdCC, and the tumor was confined to the lung. After active treatment, there was no significant recurrence of the lung lesion. However, metastasis was observed in the liver and tongue, with no positive lymph nodes detected in the neck. This is likely due to the hematogenous metastatic route of AdCC, similar to liver cancer, in which tumor cells initially involve the liver and subsequently spread via the bloodstream to distant sites.
The most frequent sites of metastasis in TAdCC are the lung, bone, liver, and brain. 5 However, our case represents an unusual instance of metastasis to the tongue base.
AdCC is histologically classified into cribriform, tubular, and solid types. A higher proportion of solid patterns is typically associated with a higher histological grade and a poorer prognosis. 8 In SAdCC, larger tumor sizes and higher pathological grades are more likely to result in distant metastasis. 9 However, primary TAdCC is rare, and few systematic reports are available. In our case, tumor samples from three different anatomical sites exhibited a combination of cribriform and tubular patterns, along with a rare solid pattern, and were classified as histologic grade I. Despite the lower histologic grade, these features contributed to earlier distant metastasis and a poorer prognosis. Metastasis in SAdCC can occur 10–30 years after treatment, underscoring the importance of long-term follow-up for AdCC patients. Common follow-up sites include the lungs, liver, and brain, but we recommend that the head and neck regions also be monitored, especially when metastasis occurs at other primary sites.
Although AdCC patients often have a chance for long-term survival following lung metastasis, liver metastasis generally indicates a much poorer prognosis. Treatment of AdCC remains challenging, as systemic treatments employing cytotoxic chemotherapy or targeted molecular therapies have not yet led to a cure for locally recurrent or metastatic AdCC.10 At best, temporary partial disease response or stabilization may be achieved. In this case, radical resection of the pulmonary lesions was performed, followed by postoperative radiotherapy and chemotherapy. A combination of immunotherapy and a TP regimen was also used to inhibit tumor progression. While local lesions did not progress, metastasis to the tongue occurred. Ultimately, the patient succumbed to severe liver dysfunction caused by chemotherapy, highlighting the ongoing challenge of distant metastasis in the treatment of AdCC. To our knowledge, this is the first reported case of primary TAdCC metastasizing to the tongue base. However, this report is limited by the patient's premature death, which precluded a comprehensive assessment of the impact of this unusual metastasis on long-term prognosis and treatment response.
Conclusion
Although patients with AdCC may achieve long-term survival even after lung metastasis, metastasis to uncommon sites is generally associated with a significantly worse prognosis. Establishing systematic long-term follow-up protocols is essential to optimize disease management outcomes. In this context, retrograde metastasis patterns involving oral minor salivary glands also warrant careful clinical attention.
Footnotes
Acknowledgements
This work was supported by the National Natural Science Foundation of China [grant number 82203418]. I confirmed that all authors have viewed and agreed to the submission.
Ethical considerations
Ethics approval for this case report was not required according to the guidelines stated by the Research Ethics Board of Qingdao University.
Consent to participate
We have obtained the written informed consent form signed by the patient.
Consent for publication
Informed consent for publication was signed by the patient, and we have de-identified all patient details.
Author contributions
Yu Zhang: conceptualization, methodology, software. Jiaqi Zhu: data curation, writing—original draft preparation. Wei Shang: supervision, software, validation. Zongxuan He: writing—reviewing and editing.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the National Natural Science Foundation of China [grant number 81502340].
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Declarations
This material contained in the manuscript has not been previously published and is not being concurrently submitted elsewhere.
Data availability
The authors confirm that the data supporting the findings of this study are available within the article.
