Abstract
Florid cemento-osseous dysplasia (FCOD) is a reactive bony lesion in which normal bone is replaced by fibrous and cementum like tissue. The differential diagnosis of this condition includes solitary bone cyst, solitary ossifying fibroma, and chronic diffuse osteomyelitis. It is often an incidental finding on a radiograph. Radiographically, it presents as a bilateral radiolucent lesion or lobulated radio-opaque masses with an affinity for tooth-bearing areas. Mostly, it progresses asymptomatically, usually diagnosed on a routine radiographic examination. Periodontal surgeries, extractions along with surgical invasive procedures have been determined to be a contraindication in these patients. There is a scarcity of literature to determine if patients with these lesions could be considered for prosthetic rehabilitative procedures like dental implants. The purpose of this literature review was to determine if dental implants could be considered as a treatment modality in patients with FCOD.
Methodology
An electronic search was done in PUBMED, SCOPUS, and a hand search was done in radiology, periodontology, and oral surgery journals. The search yielded 428 results, from which only 6 articles were selected for this literature review. Both prospective and retrospective studies were included. Clinical studies with information on the pre-implant condition of the site, detailed implant procedure, and follow-up after implant placement of more than 6 months were only considered for this review.
Results and conclusion
Limited clinical studies, shorter follow-up periods were the shortcomings of this review. However, it can be summarized that dental implants should not be placed at the site of FCOD, however can be placed at adjacent sites. Variations in implant type or the implant length had no bearing on the survival of implants at the sites of FCOD.
Introduction
Osseous dysplasia (OD) refers to a group of fibro-osseous conditions of the bone. Its etiology has been attributed to the bone superseding the fibrous connective tissue. 1 Based on the histopathologic spectrum and the extent of jaw involvement, osseous dysplasia has been further categorized into Florid, Fibrous, and Periapical dysplasia. FCOD was hitherto known as gigantiform cementum, multiple cemento-ossifying fibroma, sclerosing osteitis, multiple enostosis, and sclerotic cemental masses of the jaws. It was comprehensively described by Melrose et al. 2 Florid Cemento-osseous dysplasia (FCOD) is a rare benign fibro-osseous lesion predominantly seen in African American women, primarily in the posterior mandible region. 3 The pathogenesis of the disease involves the replacement of normal bone with fibroblasts, collagen fibers, and immature bone.1, 3
Radiographically evidenced early on with radiolucent lesions, the lesion on maturity can exhibit radiopacity. FCOD appears as diffuse, lobular, irregularly shaped radiopacities throughout the alveolar process of the maxilla and mandible. The lesion has been usually noted in the peri-apical alveolar area, but aggressive lesions have been noted more superiorly and inferiorly (Figure 1–5). 1 These lesions are usually asymptomatic, rarely causing pain and expansion and hence, are often diagnosed on routine radiographic examination.4–6 Panoramic radiographs have been found to be truly useful in the diagnosis of FCOD, owing to its multiple unilocular radiolucent appearance present in more than 1 sextant of the affected jaws as compared to solitary lesions.1, 2, 7 Clinical and radiographical features are deemed paramount for the diagnosis of this lesion. 8 A lot of conflicting data is available in the literature pertaining to dental treatment, in particular the invasive surgical procedures, in patients with Florid cemento-osseous dysplasia. The dental implant treatment in patients with osseous dysplasia poses a distinctive challenge. The pathologic and biological characteristics of osseous dysplasia's often coincide with structural changes in the bone, compromising its blood supply. Consequently, this can lead to potential issues in the process of successful osseointegration. 9 Poor vascularization, higher mineralization, and susceptibility to bone cavity formation are few of the roadblocks hindering the success of invasive surgical procedures in these patients. 10 The avascularity of the lesion has been reported as a contributing factor to secondary infections, which are considered one of the serious consequences. This infection, in turn, may lead to delayed sequestration and osteomyelitis. 11 With the growing demand for dental implants, it has become imperative to ascertain the potential success of implant therapy.

Reconstructed panoramic radiograph depicting florid osseous dysplasia in the mandible.

Reconstructed sagittal view of CBCT showing periapical osseous dysplasia near the apex of 30 and at the site of missing 31.
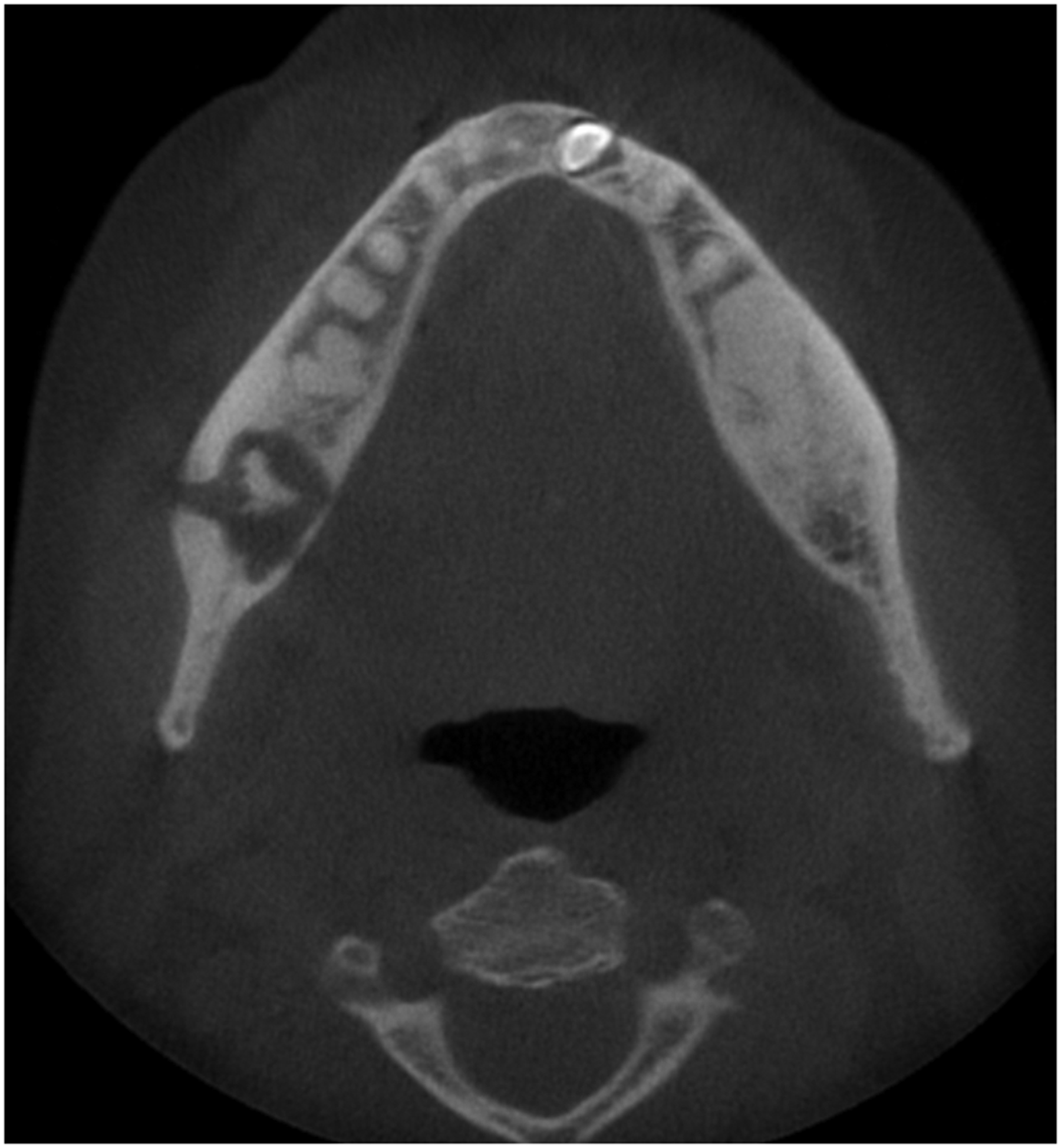
Reconstructed axial view of CBCT depicting florid osseous dysplasia in the mandible with disruption of the buccal cortical plate.

Reconstructed sagittal view of CBCT showing osseous dysplasia lesion at the site of missing tooth 19.

Periapical radiograph showing periapical osseous dysplasia near the apex of tooth 3.
The purpose of this literature review was to compare studies reporting success and failure rates after placing implants in patients with florid cemento-osseous dysplasia. The goal was to determine whether implants are a viable rehabilitative option for these patients.
Materials and methods
An electronic literature search was performed in the following electronic databases like PubMed/MEDLINE, Google Scholar, Scopus, and Science Direct from the year 2010 to 2023 to identify clinical studies reporting success and/or failure of dental implant placement at the site of FCOD. These databases are one of the biggest sources to find articles from all over the world. Boolean keywords AND/OR were used with keywords like osseous dysplasia, florid cemento-osseous dysplasia, implants success, implant survival, and implant failure. Furthermore, hand search was also done in the Journal of Oral radiology, British Journal of Oral and maxillofacial surgery, Journal of dental research, Journal of Periodontology, and Journal of Clinical Periodontology. Hand search was done in Periodontology, radiology and implantology journals to find any relevant article that might have been missed in our electronic search.
Inclusion criteria:
Patients with Florid cemento-osseous dysplasia (FCOD) who have received dental implants at one or more sites, Clinical prospective and retrospective studies, Retrospective studies were included if details of the implant's dimensions, and procedure details were mentioned, Studies with at least a 6-month follow-up. Studies with no details on dental implants dimensions or the procedure, Studies with less than a 3 month follow up as more time follow up is needed to determine implant survival, Studies with no clinical or radiographic evidence of FCOD.
Exclusion criteria:
Results and discussion
The electronic search from 2010–2020 yielded 428 results. These publications were further screened based on their titles and abstracts. 52 studies remained after further application of exclusion criteria and removal of duplicate articles. Eleven studies were considered for the literature review. Out of eleven articles included in the study, six articles described the successful placement of implant placement in cases with florid cemento-osseous dysplasia and five articles demonstrated a failure of dental implants. However, on detailed screening, only 6 articles remained for discussion in the literature review (Table 1). Few studies discussing the failure of dental implants were excluded due to the incomplete data presentation with regards to the dental implant specifications, pre-implant site details, and the implant placement procedure. Five studies1, 11–14 discuss the success of dental implants and 1 study 15 describe the failure in FCOD patients.
Summary of studies.

As reported in the literature, most patients reporting FCOD are women in the age range of 30 and above. The same could be observed from the case studies included in this review.1, 11–15 Study by Esfahanizadeh N, Yousefi H, 2018 1 have highlighted the importance of CBCT in implant planning for patients with FCOD. In their study, CBCT was done prior and then OPG was done after the implants were placed. The OPG was repeated at 2,4,6 months after implant placement to determine implant osseointegration at various intervals. After loading the implants, OPG was taken again at 12, and 18 months to determine the functional integration. The authors reported no changes in the size of the FCOD lesion nor in the implant integration. However, there were different views presented in studies by Bencharit et al. 11 and Shaheen, 13 who suggested that implant placement should be avoided in the region of the FCOD lesion. In study by Bencharit et al., 11 FCOD radioopacities were present in the mandibular posterior region. Five anterior mandibular implants were placed to construct an implant retained denture and the patient was seen at 1,2, and 3 years where they did not see any bone loss around implants or any change in the size of the FCOD lesion. Similarly, in study by Shaheen et al. 13 FCOD lesion was found in the region of mandibular #24, hence the implants were placed in the region of #23,25. They followed up for 3 months after T1 and performed histological analysis to determine the type of bone around the implants. Both studies suggest that they found features of normal alveolar bone on H&E staining. After the second stage implant placement, no bone loss was found. Both the studies suggested that for rehabilitation, an implant can be placed in an adjacent area or the site of FCOD lesion could be restored with pontics, while using the adjacent sites as implant supported abutments. In both these studies, implants were placed either in the adjacent region or the opposite side of the same jaw. Case report by Perez et al., 2021 14 discusses techniques to place implants in the region of FCOD. The author stresses the importance of implant placement atraumatically and with copious cooling measures to reduce the risk of implant failure. Authors had placed implants in the region of #31,41 which were adjacent to the sites of FCOD (#32,42). Two stage implant protocols were followed to determine the progress or stability of implants. At few months after the first stage, bone loss was observed around the necks of implants, and connective tissue graft procedure was performed to cover the defect. At 6 months follow up, the radiographic lesions were found to be mature on periapical radiograph and no further bone loss was observed. The authors loaded the implants after 6 months of implant placement. A follow-up of 6 months showed osseointegrated functional implants. Similarly, studies by Shadid and Kujan 12 stress on infection control with antibiotics for implant placement at sites of FCOD. In their case report, patient has generalized FCOD lesions. After confirming with OPG, two posterior implants were placed, and the patient was asked to have antibiotic coverage. This study has the longest follow up time of 8 years and they noticed implant osseointegration at follow up intervals.
In contrast to the above-mentioned studies favoring the implant placement at sites of FCOD, Gerlach et al. 15 reported implant failure at the site of FCOD in the region of #30 after 26 months of function. The authors had placed implants in the region of teeth #14, 15 too. These teeth exhibited no signs of FCOD and showed no signs of failure at follow up. They suggested that implant in the region of FCOD is bound to fail as fibrous tissue and woven bone replaces the normal bone, thereby not letting osseointegration occur at the site of implants. The study emphasizes the importance of longer follow up for implants placed at sites of FCOD as recurrence of these lesions is common after 3 years. Similar behavior of bone loss and eventually implant failure is discussed in an intensive case report by Oliveira et al. 9 In their case report and literature review, the authors have suggested that FCOD should be considered a “restrictive risk factor”. In their case report, they detail the presence of dysplastic tissue can compromise the bone remodelling at the site of implant placement, thereby limiting the osseointegration. This could lead to implant mobility at an early stage and implant failure. Literature also suggests that due to the hypovascularity and buildup of cementoid and osseous calcifications, these regions are more prone to osteomyelitis, and abscesses.16–18 Therefore, invasive surgical procedures like extractions, periodontal surgeries, implant rehabilitation are contraindicated at these sites.
Another important consideration while placing implants in the region of FCOD is to place implants in a two-stage procedure in a very sterile environment. Submerged two-stage surgery has been proposed to avoid any premature loading during the process of healing and to minimize the risk of infection. 12 Inflammation and secondary infection increase the chances of the progression of COD. Step by step implant placement also lets a clinician perform a routine check at intervals to determine the progress of the lesion after implant placement.1, 11, 19 There was no ideal time suggested between the first and second phase of the implant placement, however, the studies included loaded the fixed prosthesis after 3 months or longer. Failure of dental implants could be attributed to technical and surgical complications too, but those factors have not been taken into consideration in the present literature review due to the presence of pathological lesions at implant sites. Limited case reports are a limitation of this literature review.
Conclusion
Bone remodeling is a complex phenomenon and although FCOD could be a stable lesion, studies have suggested that it shows unpredictable behavior which could cause expansion of the same lesion or spread to nearby areas, thereby causing cysts or osteomyelitis. It has been demonstrated through the case reports that if the implants are to be considered at sites of FCOD, patients should be informed about possible grafting, chances of recurrence as well as longer follow up times for the implant. A thorough radiographic and clinical follow-up is required for these patients to determine the progression of the lesion. Within the limitations of the present review, it can be determined that though patients with FCOD are not ideal patients for receiving implants, it cannot be concluded that implants are an absolute contraindication. Implants can be considered at adjacent sites or the opposite regions of the same jaw, but any surgical procedure at sites of the lesion should be avoided. The authors suggest that more prospective, randomized long-term studies are needed to determine the status of implant survival and success in such patients.
Footnotes
Author's contribution
Dr Rohan Jagtap: Conceptual research and project design, writing the introduction and methodology, final approval of the manuscript.
Dr Swati Gupta: Researching articles, designing the tables and figures and making final edits to the manuscript.
Dr Mythili Bhat: writing the introduction and literature review.
Dr Neeta Mehta: Writing the discussion and editing the draft of the manuscript.
Dr Sumit Gupta: Writing the discussion and conclusion, and implementing significant changes to the manuscript based on reviewer suggestions.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethics approval
Our institution does not require ethical approval for reporting review article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Informed consent
Not applicable.
Author biographies
Rohan Jagtap is the Director of the Division of Oral and Maxillofacial Radiology and an Assistant Professor in the Department of Care Planning and Restorative Sciences at the School of Dentistry, with a dual appointment in the Department of Radiology at the School of Medicine at the University of Mississippi Medical Center, Jackson, Mississippi, USA.
Swati Gupta is internationally trained Periodontist and implantologist. She has DMD from Boston university and is currently practicing as general dentist and Implantologist. She has authored more than 30 research publications and has nationally acclaimed research grants.
Mythili Bhat is a AEGD resident in the department of Advanced Education General Dentistry at the University of Mississippi Medical Center School of Dentistry. She completed her DDS from University of Michigan School of Dentistry.
Neeta Mehta is associate professor in the department of Advanced Education General Dentistry at the University of Mississippi Medical Center School of Dentistry, Jackson, MS, USA.
Sumit Gupta is a general dentist, practicing in India. He is the director of Muffin healthcare limited which is a startup funded by the Govt of India. He is the coauthor of a book on clinical periodontology. He has 2 patents in his name and nationally acclaimed grants.
