Abstract
Objectives:
Studies have found an inverse relationship between community influenza vaccination rates and antibiotic use. This study examined the relationship between community-level influenza vaccination rates and facility-level antibiotic use in US nursing homes. We hypothesized that nursing homes in counties with high influenza vaccination rates would have low antibiotic prescribing rates.
Methods:
We linked data from the Centers for Medicare & Medicaid Services for adults aged ≥65 years in US nursing homes in 2019 at individual, facility, and county levels. We used linear mixed models to examine the association between county-level influenza vaccination rates and facility-level antibiotic prescribing rates. We generated maps to illustrate the overlap of facilities by quartiles of antibiotic prescribing and county-level influenza vaccination rates across the United States.
Results:
A 1% increase in county influenza vaccination rates was associated with a 0.03% decrease in the nursing home antibiotic prescribing rate after controlling for other factors (ß = −0.03; 95% CI, −0.03 to −0.02). As compared with other regions, the Midwest had a larger concentration of nursing homes in the upper quartile for antibiotic prescribing rates. When compared with nursing homes in the Midwest, nursing homes in the Northeast (ß = −0.98; 95% CI, −1.12 to −0.83), South (ß = −1.84; 95% CI, −1.95 to −1.73), and West (ß = −4.60; 95% CI, −4.79 to −4.41) showed a decrease in antibiotic prescribing rates.
Conclusions:
Modest improvements in community-level influenza vaccination rates can lead to decreased antibiotic prescribing rates in nursing homes.
Although antibiotics are needed to treat bacterial infections, the use and misuse of antibiotics contribute to antibiotic resistance. 1 In the United States, older adults (aged ≥65 y) residing in nursing homes are frequently prescribed antibiotics, which has led to a high prevalence of antibiotic-resistant infections in this population.2,3 When compared with the general population, nursing home residents are more vulnerable to other complications caused by the use of antibiotics, such as Clostridioides difficile infection and adverse drug reactions. 4 Therefore, understanding and preventing the overuse of antibiotics in the nursing home population is of public health importance.
It has been reported that nursing home facility-level prescribing rates may be influenced by factors other than the clinical indication for antibiotic use. 5 Emerging research shows a consistently inverse relationship between influenza vaccination rates and antibiotic prescribing rates. The reasons for this relationship are multifaceted and include the primary prevention of infectious disease, which reduces the need for antibiotics to treat secondary bacterial infections. Additionally, influenza vaccinations may reduce the inappropriate use of antibiotics for viral infections. 6 The World Health Organization recently published an action framework that prioritizes understanding the effect of vaccinations on antibiotic use. 7
The relationship between community-level influenza vaccination rates and antibiotic use in nursing homes is not well understood. However, previous studies of COVID-19–related health outcomes demonstrated that nursing homes are more vulnerable to their external environment than previously reported. For example, staff vaccination rates 8 and the prevalence of COVID-19 infection in the neighborhoods where staff reside 9 were associated with COVID-19 infection rates in the nursing homes where they work, after controlling for resident vaccination status. Furthermore, a systematic review of 16 randomized clinical trials and 19 observational studies found that higher rates of community-level influenza vaccination were associated with lower antibiotic use in the community setting. 6 To our knowledge, no studies have examined the relationship between community-level influenza vaccination rates and reductions in antibiotic use in the nursing home setting. This study examined the relationship between county-level influenza vaccination rates and facility-level antibiotic prescribing patterns in US nursing homes, controlling for individual-, facility-, and county-level factors. We hypothesized that higher community-level influenza vaccination rates would be associated with lower rates of antibiotic prescribing in nursing homes.
Methods
Data
We analyzed data from 4 linked files from the Centers for Medicare & Medicaid Services (CMS) for individual- and facility-level data from January 1 through December 31, 2019: 3.0 Minimum Dataset (MDS) for health status, 10 Medicare Part A for hospitalization and diagnoses, Medicare Part D for prescription drug data, 11 and the Long-term Care Focus in the United States database for nursing home characteristics. 12 These data sources are described elsewhere. 11 Briefly, the MDS is a federally mandated, standardized clinical assessment of every resident living in a CMS-certified nursing home. The MDS includes the CMS certification number, allowing the calculation of aggregate patient characteristics for each facility. Medicare claims provide detailed information on all health care services (Medicare Part A) and prescription drugs (Medicare Part D) provided to beneficiaries and paid for by Medicare. Long-term Care Focus in the United States is a web-based interactive database that includes information from the Certification and Survey Provider Enhanced Reports and aggregated MDS resident data from all certified nursing homes. 12 The CMS files were then linked to US Census Bureau county-level data, by county-level Federal Information Processing System codes. 13 County-level variables were lagged predictors based on the most recent year that these data were collected.
Study Population
Eligible participants included adults aged ≥65 years with continuous Medicare Part D coverage who were newly admitted to a nursing home from an acute care hospital in 2019. We identified antibiotic prescriptions in Medicare Part D by using the US Food and Drug Administration National Drug Codes for each prescription. Antibiotic prescriptions were filled within 7 days of the primary diagnostic claim date to maximize capture, account for lagged reporting, 14 and ensure that the prescribed antibiotic was associated with the primary diagnosis. All claims were deduplicated by the initial date of service and National Drug Code. We excluded nursing homes that were not located in the continental United States.
Variables of Interest
The dependent variable was the facility-level antibiotic prescribing rate, which we defined as the proportion of new nursing home residents who were prescribed at least 1 antibiotic in 2019. The primary exposure of interest was county-level influenza vaccination rates.
We aggregated individual-level covariates at the facility level due to the facility-level status of the dependent variable. These variables included average age, percentage female, percentage non-White, percentage dual eligibility (ie, covered by Medicare and Medicaid), average length of stay in days, and average risk adjustment score. We derived the risk adjustment score from the 2015 Diagnostic Cost Group and Hierarchical Condition Category (DCG/HCC) model. 15 The DCG/HCC model uses diagnoses and prescription claims data to infer health care problems, such as disability and morbidity, and predict the future health care costs of populations. 16 For example, a risk score of 2 means that a resident is likely to incur health care costs that are 2 times the health care costs for the average Medicare recipient. The algorithm for the DCG/HCC risk adjustment score has been validated by using claims data to accurately describe clinical profiles.
We selected facility-level factors on characteristics related to prescribing culture, 17 such as ownership status. 18 Facility-level covariates included the 2019 antibiotic case mix (described hereinafter), US Census region (Midwest, Northeast, South, West), location type (urban, rural), whether the facility has an on-site physician or nurse practitioner (yes, no), bed capacity (<50, 50-100, 101-250, >250 beds), profit status (for-profit, nonprofit), and ownership status (independent, chain). We created the facility-level antibiotic case mix by taking the count of 2 antibiotic recommendation categories, “always” and “sometimes,” and dividing by the total number of residents at each facility. The numerator included residents who were prescribed >1 antibiotic during the study period. We included the facility-level antibiotic case mix to control for the number of infections that may warrant antibiotic use. Categories for the recommended use of antibiotics were “always,” “sometimes,” and “never” and were based on codes from the International Classification of Diseases, Tenth Revision, Clinical Modification. 19
County-level factors included in this study were influenza vaccination rates, total population, percentage with some college education, and median household income. The influenza vaccination rates were derived from the 2016 Mapping Medicare Disparities Tool, 20 and the rates included all Medicare and Medicaid beneficiaries in a county. The 2016 influenza rate was the most recently available data at the county level for this variable. Based on Centers for Disease Control and Prevention estimates, the national influenza rate was relatively stable from 2016 through 2019. 21 The total population per county came from the 2017 US Census Bureau. 13 Median household income and education level came from the 5-year average of the American Community Survey for 2013-2017. 22 We selected median household income to represent county socioeconomic status based on prior reporting that showed income to be the most predictive socioeconomic status indicator of health outcomes.23,24
Statistical Analysis
We used descriptive statistics and data visualizations to examine data distributions and assess required assumptions for statistical modeling. Multivariable regression analyses via linear mixed models were used to examine the association between county-level influenza vaccination rates and facility-level antibiotic prescribing rates in a 2-level analysis (facility and county). We aggregated individual-level covariates to the facility level. We included county-level random intercepts to account for clustering of facilities within a county. We used a 4-stage model-building process and the Akaike information criterion to select the best fit and most parsimonious model (eTable 1 in Supplemental Material). We examined 2-way interactions for all facility-level covariates.
We created maps by using ArcGIS Desktop version 10.8.2 (Environmental Systems Research Institute) to visualize nursing home facilities by quartiles of antibiotic prescribing rates and county-level influenza vaccination rates across the United States. We geocoded nursing home addresses onto US cartographic boundary files via county-level shapefiles, along with linked data. We performed all analyses in R studio version 9.0 (Posit PBC). The Northeastern University Institutional Review Board reviewed this study and determined it to be exempt from oversight because it involved the use of deidentified, publicly available data. The primary dataset for this study uses only a public use file from the CMS Research Data Assistance Center. This file contains no personally identifiable information.
Results
Our final dataset included 348 counties, 13 314 nursing homes, and 863 221 residents who newly resided in nursing homes in 2019 (eFigure 1 in Supplemental Material). The average 2019 antibiotic case mix was 30.9% and the average prescribing rate was 19%. The average age of residents was 80.6 years and the average length of stay was 31.3 days (Table 1). The average risk adjustment score was 1.8, meaning that the average resident in our study was expected to incur health care costs 1.8 times the average Medicare beneficiary. Most facilities had a large bed capacity (54.5%; 101-250 beds), had no physician or nurse practitioner working on-site (59.4%), were for-profit (62.3%), and were chains (55.8%). At the county level, the median influenza vaccination rate was 47.0%, the median population was 481 800, the median household income was $59 200, and the median percentage with some college education was 66.1%.
Characteristics of nursing homes and counties in the United States, 2019 (N = 863 221)
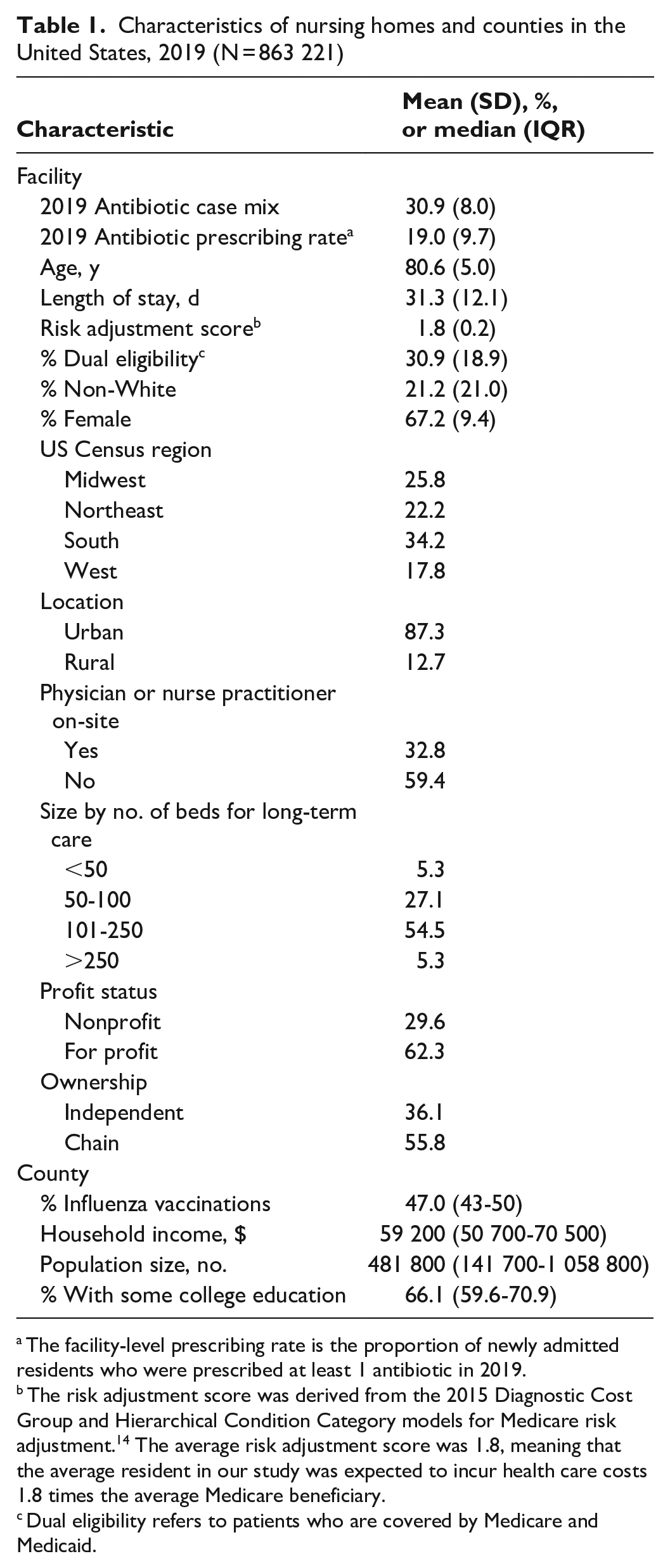
The facility-level prescribing rate is the proportion of newly admitted residents who were prescribed at least 1 antibiotic in 2019.
The risk adjustment score was derived from the 2015 Diagnostic Cost Group and Hierarchical Condition Category models for Medicare risk adjustment. 14 The average risk adjustment score was 1.8, meaning that the average resident in our study was expected to incur health care costs 1.8 times the average Medicare beneficiary.
Dual eligibility refers to patients who are covered by Medicare and Medicaid.
Unadjusted Analyses
In unadjusted analyses, a 1% increase in the facility antibiotic case mix was associated with a 0.3% increase in the antibiotic prescribing rate (ß = 0.26; 95% CI, 0.25-0.26) (Table 2). Every 1-day increase in length of stay was associated with a 0.4% increase in the prescribing rate (ß = 0.41; 95% CI, 0.41-0.41). For-profit status was associated with a 1.4% increase in the prescribing rate, while chain ownership was associated with a 0.4% increase in the prescribing rate. Larger bed capacity was associated with a 2.2% increase in the prescribing rate. Having a nurse practitioner or physician on-site was associated with a 0.4% increase in the antibiotic prescribing rate (ß = 0.43; 95% CI, 0.39-0.47). Nursing homes with higher average risk adjustment scores and a higher percentage of residents with dual eligibility were also associated with increases in the prescribing rate (Table 2). Nursing homes located in urban areas were associated with a 3.0% decrease in the antibiotic prescribing rate (ß = −3.04; 95% CI, −3.10 to −2.98). Nursing homes with a higher proportion of adults who were older, non-White, and female were associated with a decrease in the prescribing rate.
Hierarchical generalized linear model of associations with facility-level antibiotic prescribing rate, 2019
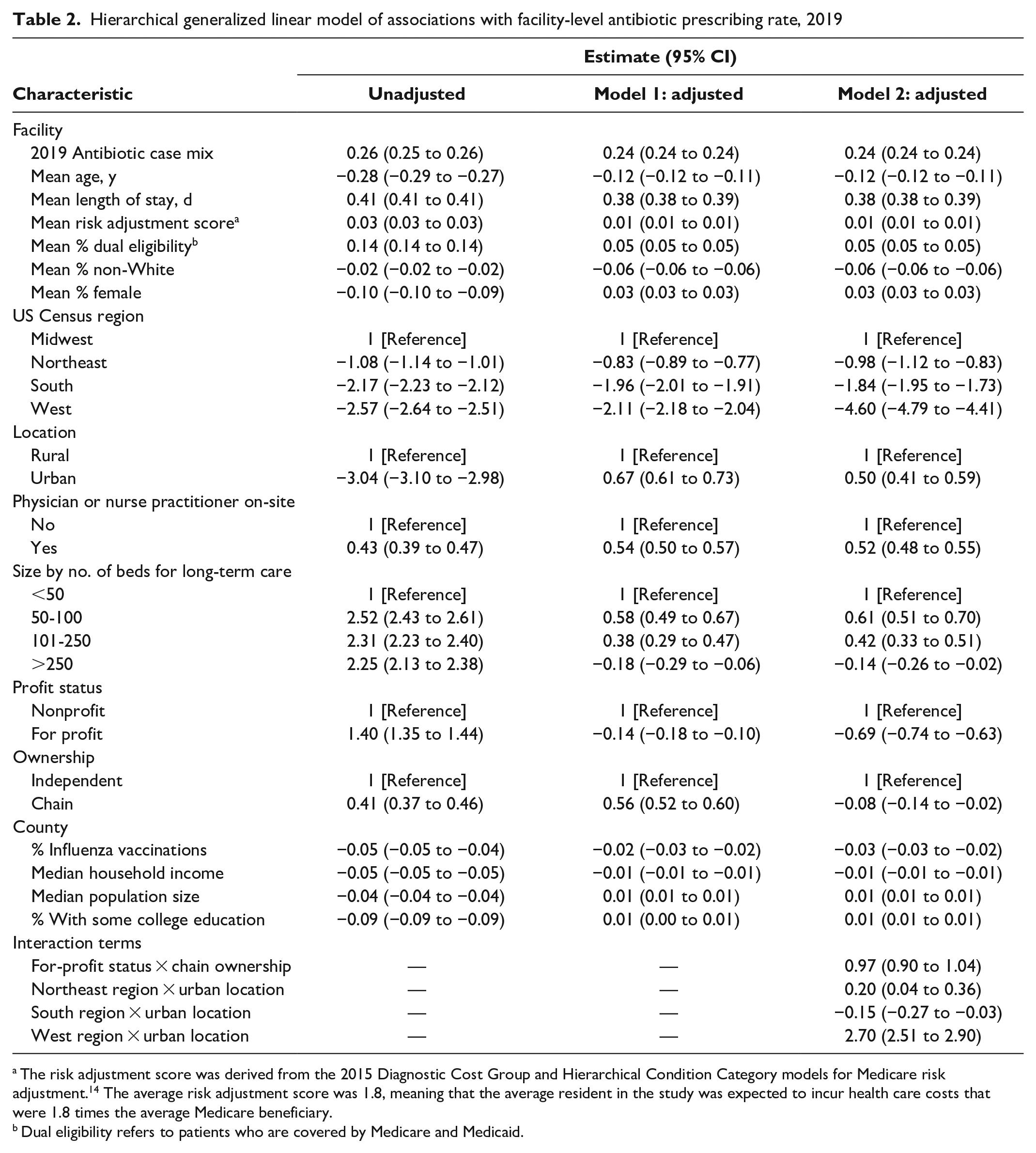
The risk adjustment score was derived from the 2015 Diagnostic Cost Group and Hierarchical Condition Category models for Medicare risk adjustment. 14 The average risk adjustment score was 1.8, meaning that the average resident in the study was expected to incur health care costs that were 1.8 times the average Medicare beneficiary.
Dual eligibility refers to patients who are covered by Medicare and Medicaid.
At the county level, in unadjusted analyses, a 1% increase in the county-level influenza vaccination rate was associated with a 0.1% decrease in the nursing home antibiotic prescribing rate (ß = −0.05; 95% CI, −0.05 to −0.04) (Table 2). In addition, a 1% increase in the proportion of county residents with some college education was associated with a 0.1% decrease in the nursing home antibiotic prescribing rate (ß = −0.09; 95% CI, −0.09 to −0.09).
The Midwest had a larger concentration of nursing homes in the upper quartile for antibiotic prescribing as compared with other regions (Figure). In particular, states in the Midwest, such as areas around Wisconsin and Ohio, had counties in the lower quartiles for influenza vaccination rates (yellow dots, Figure A) and high concentrations of nursing homes in the upper quartile for antibiotic prescribing (red dots, Figure B). States in the South also had counties in the lower quartile for influenza vaccination rates and nursing homes in the upper quartile of antibiotic prescribing, such as Texas and West Virginia. However, other states in the South, such as Georgia and Florida, had counties in the highest quartile for influenza vaccination rates (dark blue dots, Figure A) and nursing homes in the lowest quartile of antibiotic prescribing (yellow dots in Florida, Figure B). Nursing homes in the South (ß = −2.17; 95% CI, −2.23 to −2.12) and West (ß = −2.57; 95% CI, −2.64 to −2.51) were associated with a >2% decrease in the prescribing rate when compared with nursing homes in the Midwest (Table 2). Nursing homes in the Northeast were associated with a decrease in the prescribing rate (ß = −1.08; 95% CI, −1.14 to −1.01) when compared with the Midwest. Bivariate associations between county influenza vaccination rates and nursing home antibiotic prescribing rates are also shown (Figure C).
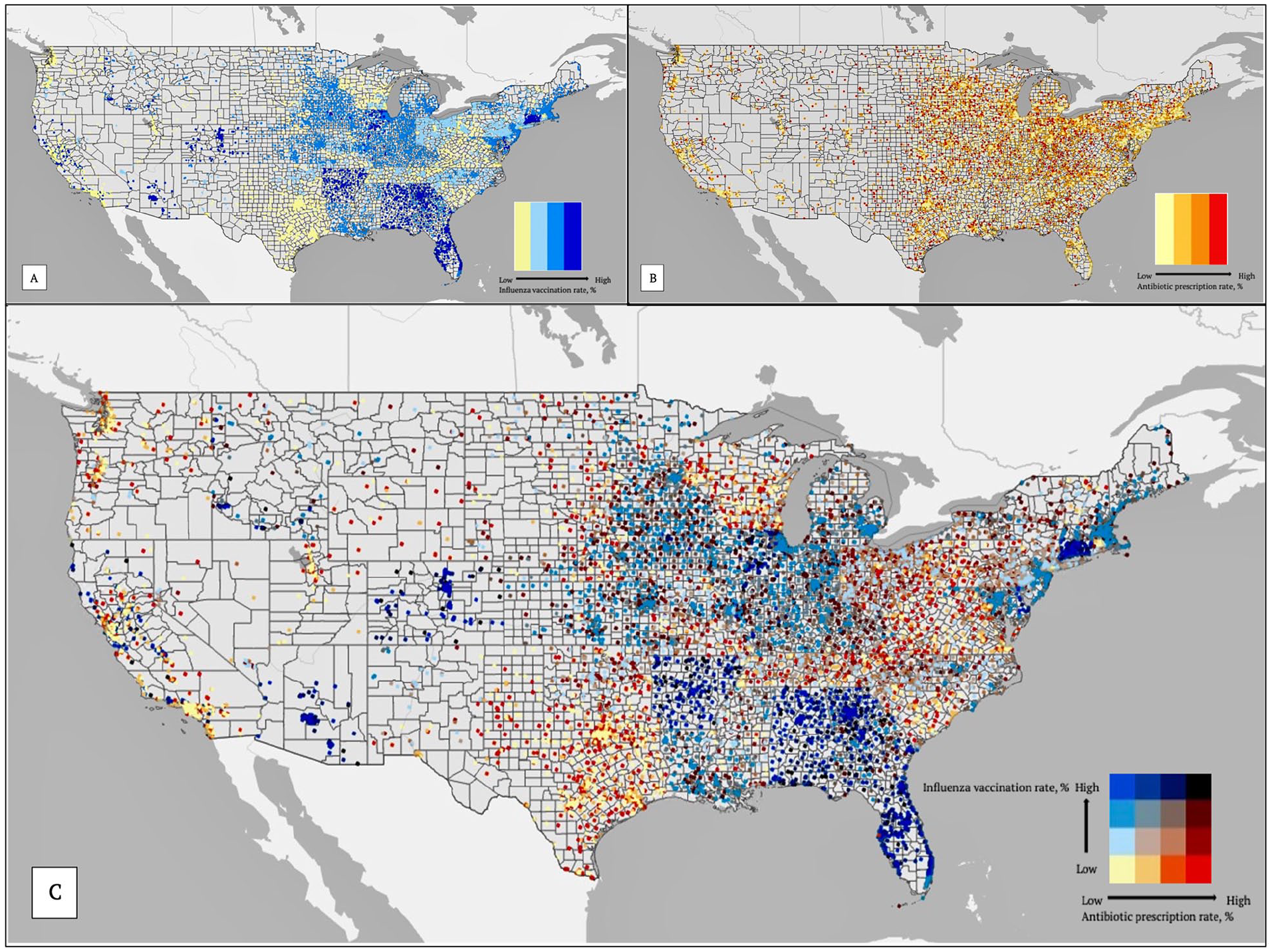
Facility-level antibiotic prescribing rates and county-level influenza vaccination rates at nursing homes in the United States, 2019. (A) County-level influenza vaccination rate quartiles (Q1 = 35%, Q2 = 42%, Q3 = 48%). (B) Facility-level antibiotic prescribing rate (Q1 = 12%, Q2 = 18%, Q3 = 27%). (C) County-level influenza vaccination rate and facility-level antibiotic prescribing rate.
Adjusted Analyses
In the final adjusted model, a 1% increase in county influenza vaccination rates was associated with a 0.03% decrease in the nursing home antibiotic prescribing rate after controlling for facility- and county-level factors (ß = −0.03; 95% CI, −0.03 to −0.02) (Table 2). Nursing homes in the Northeast (ß = −0.98; 95% CI, −1.12 to −0.83), South (ß = −1.84; 95% CI, −1.95 to −1.73), and West (ß = −4.60; 95% CI, −4.79 to −4.41) were associated with a decrease in the prescribing rate when compared with nursing homes in the Midwest. Facilities with a physician or nurse practitioner on-site and urban location were positively associated with the antibiotic prescribing rate. We explored interaction terms and found some effect modification by nursing home bed capacity, but this effect diminished once we examined the interaction between profit status and chain ownership. On average, for-profit and chain nursing homes were negatively associated with the antibiotic prescribing rate; however, for-profit chain nursing homes were associated with a 1.0% increase in the antibiotic prescribing rate (ß = 0.97; 95% CI, 0.90-1.04). Nursing homes in urban areas of the Northeast and West were positively associated with the antibiotic prescribing rate, while we observed the inverse in the South.
Discussion
In this nationwide, multilevel, ecological study, we found an association between county-level influenza vaccination rates and nursing home antibiotic prescribing rates. A 1% increase in county influenza vaccination rates was associated with a 0.03% decrease in nursing home antibiotic prescribing rates after controlling for facility and county factors. For example, in a population of 500 000 county residents and 1000 antibiotic prescriptions in a nursing home of 200 residents, for every 5000 county residents who were vaccinated against influenza, we saw a reduction of 15 antibiotic prescriptions in the nursing home after controlling for facility- and county-level factors. To our knowledge, this study is the first to explore the association between community influenza vaccination levels and antibiotic prescribing in the nursing home setting. Although our observed relationships were modest in magnitude, even small individual-level effects in a rapidly growing older adult population could lead to substantial aggregate effects. These findings are consistent with previous studies reporting that higher population-level vaccination rates were associated with lower antibiotic use.6,25,26 Our study supports research indicating that nursing home residents are more susceptible to external community factors than previously thought, such as COVID-19 prevalence and vaccinations, that may be introduced through staff and visitors. 8
Despite finding an association between county-level influenza vaccinations and nursing home antibiotic prescribing rates, the factor most strongly associated with nursing home antibiotic prescribing rates was geographic region after controlling for other variables. Furthermore, the relationship between region and antibiotic rates was modified by whether a nursing home was located in an urban or rural area. For example, on average, nursing homes in the West had 4.6% lower antibiotic prescribing rates than those in the Midwest. However, nursing homes in urban areas of the West had 2.7% higher antibiotic prescribing rates than nursing homes in the Midwest. Regional variations in antibiotic prescribing rates are well documented and may result from a complex interplay of clinical practices and policy-level factors. 27 Differences in prescribing behaviors can reflect variations in local health care infrastructure, health care provider education, and patient demographic characteristics, as well as the prevalence of infectious diseases in certain areas. Additionally, regional policies, such as antibiotic stewardship programs, substantially influence prescribing patterns. 28
We found that for-profit chain nursing homes had higher antibiotic prescribing rates than nonprofit chain nursing homes. These findings may point to differences in quality of care by ownership status, which is consistent with other studies. For example, deficiencies in staffing levels, infection control practices, and individualized care—common indicators of reduced quality of care—may contribute to the higher use of antibiotics. 29 It has been reported that for-profit nursing homes, particularly those owned by large chains, tend to perform worse than nonprofit or independently owned facilities on various quality indicators, including higher rates of avoidable hospitalizations and pressure ulcers. 30 However, further research is needed to elucidate these associations.
Strengths and Limitations
This study had several strengths and limitations. Strengths of our study included the use of a large national sample of nursing home residents; a multilevel design to control for county and nursing home factors; and aggregated individual-level predictors, such as comorbidities, category of recommended use of antibiotics, and age. The generation of maps is a novel use of these data to examine the bivariate associations between county-level influenza vaccination rates and antibiotic prescribing rates in nursing homes across the nation.
This study also had several limitations. First, we assumed that staff and visitors were located in the same county. However, in a 2013 study by Pesis-Katz et al, distance to a nursing home was the strongest predictor of nursing home choice, and the average distance was equivalent to the size of a county. 31 Furthermore, nursing home staff may hold second jobs in the same county. 32 Second, the county-level influenza vaccination rate used in this study was from 2016 because that was the most recently available year for these data. Yet, this rate did not differ substantially from the Centers for Disease Control and Prevention’s 2019 InfluenzaVaxView estimates, 21 which rely on national survey data, and the average nursing home 3.0 MDS facility-level influenza vaccination rates for 2019 in our dataset (54.8%). We did not include the nursing home facility-level vaccination rate in the model because it overlapped with county-level estimates.
Conclusion
Vaccines prevent infections and can reduce the use of antibiotics; therefore, vaccinations could play a large role in reducing antimicrobial resistance. This study addresses a gap in our understanding of how community-level vaccinations may protect against antibiotic use among older nursing home residents in the United States. Our study showed that modest improvements in community-level influenza vaccination rates can improve antibiotic prescribing in nursing homes. These study findings are specific to vaccinations against a respiratory virus and do not reflect the effect of vaccinations for nonrespiratory viruses and bacterial infections, which may be weaker or stronger, respectively. We hope that these findings will strengthen the evidence base for the importance of influenza vaccination efforts, underscoring the need for policy initiatives that promote widespread influenza vaccination to improve the care and health outcomes of adults in nursing homes.
Supplemental Material
sj-docx-1-phr-10.1177_00333549251342746 – Supplemental material for County Influenza Vaccination Rates and Antibiotic Prescribing Rates in US Nursing Homes
Supplemental material, sj-docx-1-phr-10.1177_00333549251342746 for County Influenza Vaccination Rates and Antibiotic Prescribing Rates in US Nursing Homes by Quynh T. Vo, Farzad Noubary, Brandon Dionne, Shira Doron and Becky A. Briesacher in Public Health Reports®
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work is funded by the National Institute on Aging of the National Institutes of Health under awards R21AG057979 and R33AG057979.
Data Availability Statement
The data used in this study are from public use files obtained from the Centers for Medicare & Medicaid Services (CMS). These data are available to researchers through the CMS website and can be accessed upon request. Use of these files requires compliance with CMS data use policies, including data security and privacy standards. Publicly available facility-level data are available at https://ltcfocus.org. Publicly available county-level data are available at ![]() .
.
Supplemental Material
Supplemental material for this article is available online. The authors have provided these supplemental materials to give readers additional information about their work. These materials have not been edited or formatted by Public Health Reports’s scientific editors and, thus, may not conform to the guidelines of the AMA Manual of Style, 11th Edition.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
