Abstract
Objectives
The Virginia Department of Health (VDH) identified an outbreak of Salmonella serotype Javiana infections in Virginia after a chili and chowder cook-off with 11 competitors and about 2500 attendees on September 30, 2017. The objectives of this study were to assess the extent of the outbreak and identify the most likely source of exposure.
Methods
To identify people with suspected Salmonella infection, VDH used press releases and social media posts to recruit event attendees to take an online survey about foods eaten at the cook-off and any gastrointestinal (GI) symptoms experienced. VDH defined a case as reported GI illness that occurred within 1 week after eating food from the cook-off. Confirmed cases required a clinical specimen culture positive for Salmonella. Probable cases reported diarrhea or related clinical symptoms. “Not ill” people did not report GI illness. Investigators calculated unadjusted relative risks of illness and performed stratified analysis to address potential confounding. Available food samples were tested for Salmonella. Environmental health specialists interviewed food handlers and inspected restaurants where 3 competitors had prepared food.
Results
Of 438 survey responses, 171 (39%) met the case definition. Of all chilies and chowders consumed, Chowder A was associated with the highest relative risk of illness (8.9; 95% CI, 5.7-13.7). A Chowder A sample tested positive for Salmonella serotype Javiana. The environmental investigation did not identify an original contamination source but did find deficiencies in maintaining safe cooking temperatures.
Conclusions
Epidemiologic and laboratory findings indicated that Chowder A was the most likely cause of outbreak. Recommendations to prevent future outbreaks include preparation of all food on-site to ensure safe temperatures during food preparation and service.
On September 30, 2017, a local volunteer fire company from the Eastern Shore region of Virginia hosted a chili and chowder cook-off attended by about 2500 people from multiple states. Accomack County Health Department (ACHD) received the first complaint of gastrointestinal (GI) illness on October 3, 2017. That same day, ACHD found more than a dozen reports of GI illness in a thread on a social media page (started on October 2, 2017) about the cook-off. Some ill attendees posting on the thread reported diagnoses of Salmonella infection (written communication).
The Virginia Department of Health (VDH) receives approximately 1000 reports of Salmonella infection annually. 1 Nationwide each year, salmonellosis is estimated to cause approximately 1.35 million illnesses, 26 500 hospitalizations, and 420 deaths. 2 Symptoms of infection typically appear 6-72 hours after exposure and can include diarrhea, abdominal pain, fever, dehydration, headache, nausea, or vomiting. 2
Approximately 94% of salmonellosis illnesses are foodborne, although salmonellosis can be transmitted directly to humans from animals (eg, handling chickens or turtles) or from person to person by the fecal-oral route. 3 Food can be contaminated by contact with feces of animals or humans carrying Salmonella at any stage of food production, including produce harvesting or animal slaughter, packaging, transportation, kitchen preparation, or food service.
VDH initiated a foodborne outbreak investigation after learning of the chili and chowder cook-off attendees who were ill. The investigation team included nurses, epidemiologists, and environmental health staff members from VDH, as well as laboratorians from the Division of Consolidated Laboratory Services (DCLS). Team goals were to assess the extent of the outbreak, identify the most likely source of exposure, prevent additional cases, and recommend steps to prevent similar outbreaks in the future.
Methods
Case Finding
ACHD interviewed the first people to report illness on October 3 by telephone using VDH’s Enteric Case Report Form or the Centers for Disease Control and Prevention’s (CDC’s) Environmental Health Specialists Network Foodborne Illness Complaint Form. 4 Because of the scale of the outbreak, VDH posted a report on October 4 to Epi-X, a secure data-sharing system managed by CDC, to spread awareness of the outbreak to public health professionals in other states (unpublished report, Epi-X, October 4, 2017).
To reduce the large amount of staff members and time required to conduct interviews by telephone, VDH created an online survey using REDCap electronic data capture tools. 5 VDH provided the survey link in a press release on October 5 and on local health department websites and social media to identify attendees. 6 Text included with the link encouraged all cook-off attendees to take the survey whether or not they were ill. VDH staff members entered the data from the first telephone calls (initially collected by paper form) into the online survey. The survey included questions about consumption of foods available at the cook-off and GI illness. For each food item available at the cook-off, the survey asked participants whether they had eaten that food (yes, no, or unsure). Additional questions asked respondents who reported illness when symptoms began, which symptoms were experienced, and whether health care treatment was sought. VDH personnel communicated with health departments of other states where illness was being reported in the survey. Parents or guardians answered survey questions for minors. This study was not subject to institutional review board review because it did not qualify as human subjects research.
The outbreak case definition included illness that occurred after eating food from the chili and chowder cook-off that occurred on September 30, 2017. Cases occurred from September 30 through October 7. Confirmed cases required a clinical specimen culture positive for Salmonella. Probable cases reported ≥3 episodes of diarrhea during a 24-hour period OR unquantified diarrhea and ≥1 other symptom that included nausea, vomiting, fever, chills, abdominal cramps, or dehydration. Investigators excluded from analysis surveys from people with GI illness not meeting the probable or confirmed case definition. The “not ill” group included all others who did not report GI illness.
Data Analysis
VDH staff members used R version 3.4.1 (R Foundation) for quality control, visualization, and analyses of survey data. Investigators excluded surveys that were incomplete because the respondents did not click the submit button in REDCap, surveys from respondents who did not eat food from the cook-off, surveys with comments mentioning illness onset only after close contact with an ill person (suggesting a secondary case of illness), and surveys with reported illness onset before the cook-off or after the date the survey was taken. For duplicate entries, investigators took the first survey response for analysis, except when a respondent had taken the online survey after VDH staff members had entered the paper case report information. In those instances, investigators retained the later online response.
Of 528 entries in the REDCap survey, investigators excluded 90 entries—57 were incomplete, 15 were duplicates, 10 reported illness that did not meet the case definition, 4 were likely secondary cases, 3 did not eat food from the cook-off, and 1 reported illness onset before the cook-off—leaving 438 surveys for data analysis.
Nine chilies and 5 chowders were available at the cook-off. One chili entry was entered under 2 separate names (the restaurant’s name and the restaurant bar’s name). For consistency with other food items, investigators used the entry under the restaurant’s name (Chili I) for analysis.
For each food item served, VDH staff members used the epitools 7 R package (version 0.5-9) to calculate relative risks (RRs) for illness, which compared exposed people with unexposed people. To determine exposures significantly associated with illness, staff members used the Fisher exact test to calculate P values and calculated 95% CIs for RRs using the epitools package. Investigators also calculated RRs for illness for the subgroup of survey respondents who reported eating only 1 chili or chowder and did not indicate “unsure” for any other food. P < .05 was considered significant.
The unstratified and single food analyses indicated a particular food item was most strongly associated with illness, and investigators calculated Mantel–Haenszel adjusted RRs to yield estimates of illness risk adjusted for exposure to the highest-risk food item.
Environmental Health Investigation
Eleven food vendors competed in the chili and chowder cook-off. Amateur competitors were required to cook food on-site, where VDH environmental health staff members provided oversight to ensure that foods were purchased from approved sources and that safe cooking practices were followed. Professional competitors (ie, people with VDH-permitted or Virginia Department of Agriculture and Consumer Services–inspected establishments) could prepare their food off-site. Eight of 11 competitors prepared their contest entries on-site, and environmental health staff members did not note any violations during on-site food preparations. Therefore, the environmental health investigation focused on competitors who cooked food off-site.
On October 5, a VDH environmental health specialist and foodborne illness investigation team member interviewed the 3 off-site food preparers about whether they had experienced GI symptoms around the time of the cook-off and how the food items were sourced, prepared, stored, transported, heated, and served. VDH staff members visited premises to assess the sanitary and physical conditions of the kitchen where food was prepared. Based on preliminary RR calculations, 1 restaurant was of particular interest, and VDH staff members interviewed food handlers from that restaurant again on October 13.
Laboratory Investigation
Diagnostic laboratories forwarded stool samples from ill attendees to public health laboratories in patients’ states of residency for confirmation of organism identity, serotyping, and molecular subtyping by pulsed-field gel electrophoresis (PFGE), according to standardized procedures developed by CDC. 8 Laboratory staff members posted the outbreak-associated PFGE patterns to the CDC PulseNet online forum (SharePoint) as soon as they were available to facilitate finding additional cases. Like Epi-X, PulseNet SharePoint is a secure system managed by CDC for data sharing among state laboratories and health departments. VDH provided the outbreak identification number to other states so that any out-of-state specimens associated with the outbreak could be easily identified.
VDH provided stool collection kits to all 3 restaurant employees involved in preparing or serving the primary food item of interest to test whether any might have been Salmonella carriers. The restaurant provided 1 package of frozen raw clam strips, the same type but not the same package used in preparation of the food item, for testing at DCLS. One cook-off attendee called the health department to offer a container of the food item that had been taken home from the cook-off and not reopened or eaten. (The attendee had eaten a separate sample of the food item at the cook-off and was too ill to eat the take-home sample.) VDH sent this uneaten sample to DCLS for Salmonella testing in accordance with the US Food and Drug Administration’s Bacteriological Analytical Manual. 9
DCLS staff members incubated samples collected from food and Virginia patients overnight on tryptic soy blood agar at 37°C, then extracted genomic DNA from bacterial colonies using the Qiagen QIAamp DNA mini kit (Qiagen) and quantified with the Qubit dsDNA BR (broad-range) assay kit (Thermo Fisher Scientific). DCLS staff members completed sequencing library preparation for multiplexed paired-end libraries by following the manufacturer’s guidelines for the Nextera XT DNA sample prep kit (Illumina) and Nextera XT index kit (Illumina), with the modification that estimated genome size was used to normalize sample libraries before pooling for the sequencing run. Next, laboratory staff members performed sequencing using V2 chemistries on the Illumina MiSeq following standard FASTQ-only generation protocols to produce 250-base pair paired-end reads. DCLS staff members then analyzed sequencing reads using the LyveSET v1.1.4f pipeline with Salmonella enterica serotype Javiana str. CFSAN001992 as the reference strain for read mapping. 10
Results
Of the 438 included surveys, 267 survey respondents were not ill and 171 (39%) experienced illness that met the case definition (146 probable cases, 25 confirmed cases) (Table 1). An additional 12 attendees had a clinical specimen that tested positive for the outbreak strain Salmonella but no survey response to confirm attendance at the cook-off. Illness onset for 22 (13%) cases occurred within 6-12 hours of the cook-off on September 30 (Figure). Illness onset for most cases (n = 104, 61%) occurred on October 1, the day after exposure. Illness onset for 1 person with a confirmed case was reported as late as October 7.
Clinical symptoms reported by survey respondents with salmonellosis after a chili and chowder cook-off, Virginia, 2017 a

aA total of 438 people responded to the online survey, of whom 171 experienced illness that met the case definition (ie, illness that occurred after eating food from the chili and chowder cook-off from September 30 to October 9). Confirmed cases were positive for Salmonella by culture. Probable cases reported ≥3 episodes of diarrhea in a 24-hour period OR unquantified diarrhea and ≥1 other symptom (nausea, vomiting, fever, chills, abdominal cramps, or dehydration).
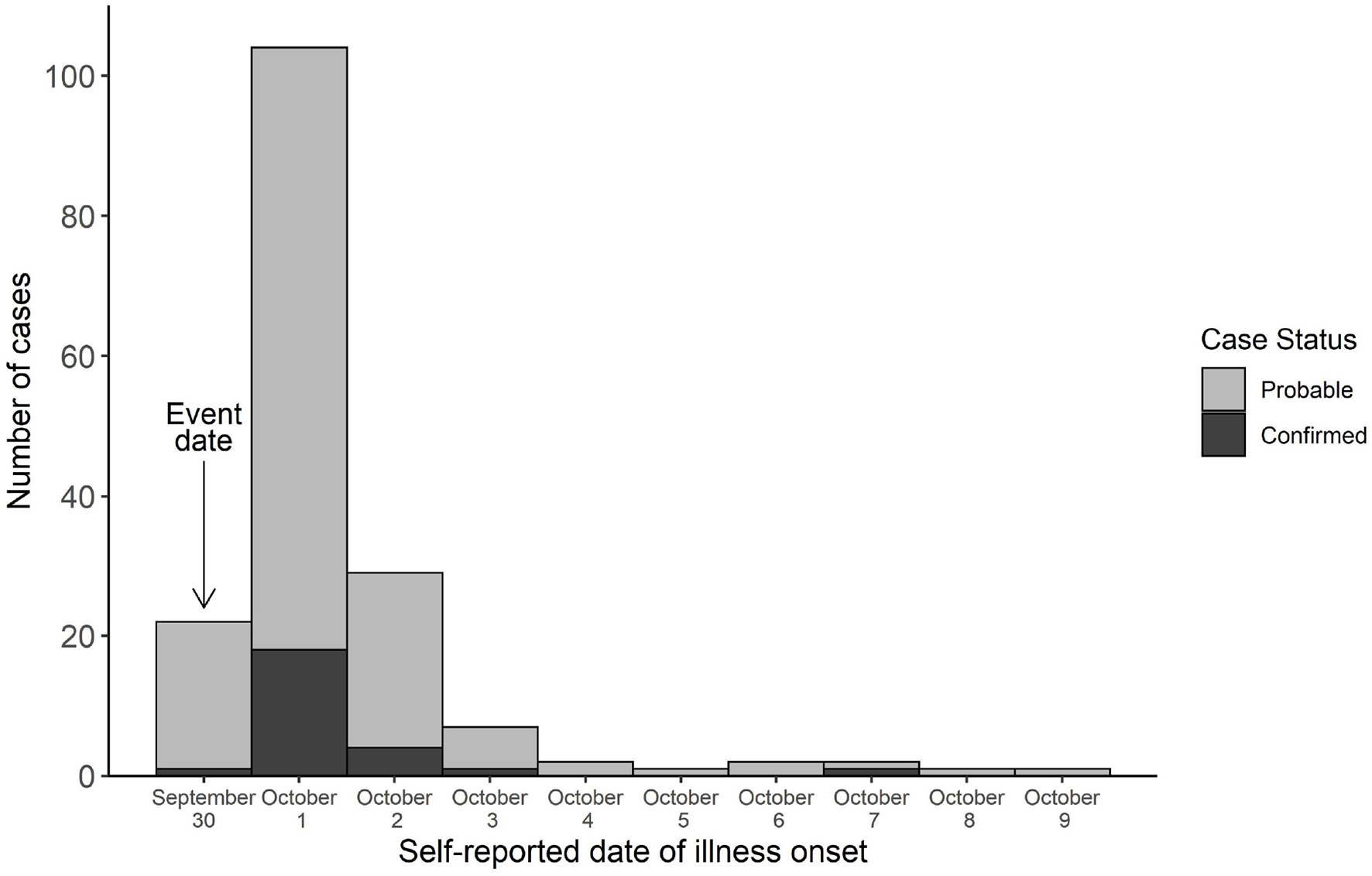
Illness onset date and case status for cases associated with a salmonellosis outbreak after a chili and chowder cook-off, Virginia, 2017. The outbreak case definition included illness that occurred after consuming food from the chili and chowder cook-off. Confirmed cases were positive for Salmonella by culture. Probable cases reported ≥3 episodes of diarrhea in a 24-hour period OR unquantified diarrhea and ≥1 other symptom (nausea, vomiting, fever, chills, abdominal cramps, or dehydration).
The most common reported symptoms were diarrhea (n = 171, 100%) and abdominal cramps (n = 142, 83%), followed by nausea (n = 111, 65%), fever (n = 108, 63%), chills (n = 106, 62%), and dehydration (n = 95, 56%) (Table 1). The median number of symptoms reported in addition to diarrhea was 4. More than half of respondents who were ill sought health care treatment; 32% (n = 55) were treated at an urgent care or physician’s office, and 21% (n = 36) reported treatment at a hospital emergency department. Eighteen people reported hospitalization overnight for illness; no deaths were reported.
The average age of ill respondents was 50 (SD, 17 years; range, 5-87 years), and the average age of respondents who were not ill was 53 (SD, 15 years; range, 6-81 years).
In addition to 52 Virginia residents who reported illness, attendees from 6 other states reported illness: Maryland (n = 50), Pennsylvania (n = 36), New Jersey (n = 16), Delaware (n = 13), West Virginia (n = 3), and North Carolina (n = 1).
Food Item Exposure Analysis
Unstratified analysis
All chowders and all but 1 chili (Chili I) eaten at the cook-off were significantly associated with illness (Table 2). Consumption of Chowder A was associated with the largest RR for illness (8.9; 95% CI, 5.7-13.7), and consumption of Chowder B was associated with the next-largest RR for illness (2.9; 95% CI, 2.2-3.7).
Associations between salmonellosis and chilies and chowders available at a cook-off, by whether or not the food item was consumed, a Virginia, 2017
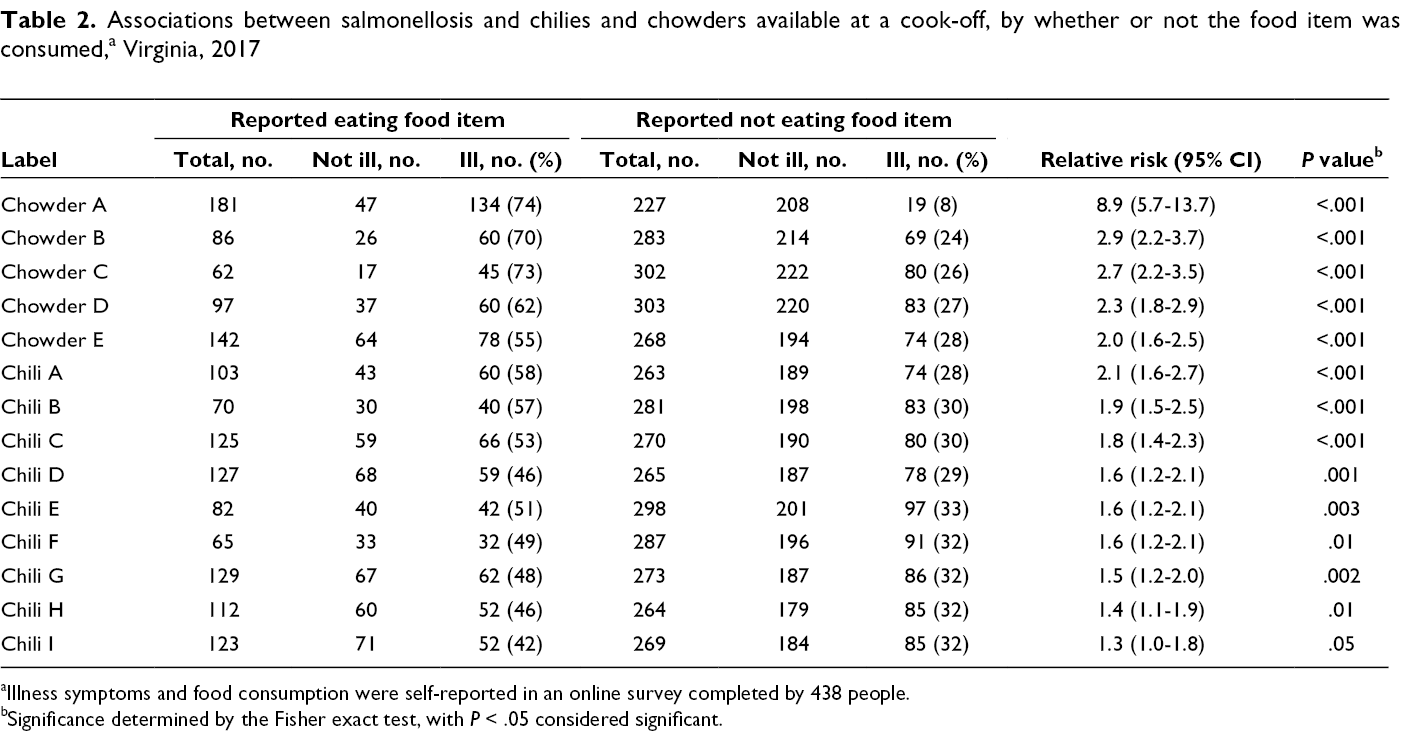
aIllness symptoms and food consumption were self-reported in an online survey completed by 438 people.
bSignificance determined by the Fisher exact test, with P < .05 considered significant.
Single food exposure analysis
The median number of chilies and chowders tasted was 3 overall, with a median of 2 chilies and chowders tasted among people who were not ill and 4 among people who were ill. Although 294 (67%) survey respondents reported tasting >1 chili or chowder at the cook-off, 32 (7%) survey respondents reported eating only 1 chili or chowder, with no food exposures marked as “unsure.” Of the 32 respondents who reported only 1 exposure, 7 reported GI illness. Six of 7 ill respondents with GI illness identified Chowder A as their only exposure, for an RR of 13.2 (95% CI, 1.8-95.7).
Stratified analysis
Nineteen people who were ill did not report eating Chowder A. The percentage of respondents who were ill was 3-16 times higher among people who also ate Chowder A than among people who did not eat Chowder A (Table 3).
Associations between salmonellosis and chilies and chowders available at a cook-off, stratified by exposure to Chowder A, a Virginia, 2017
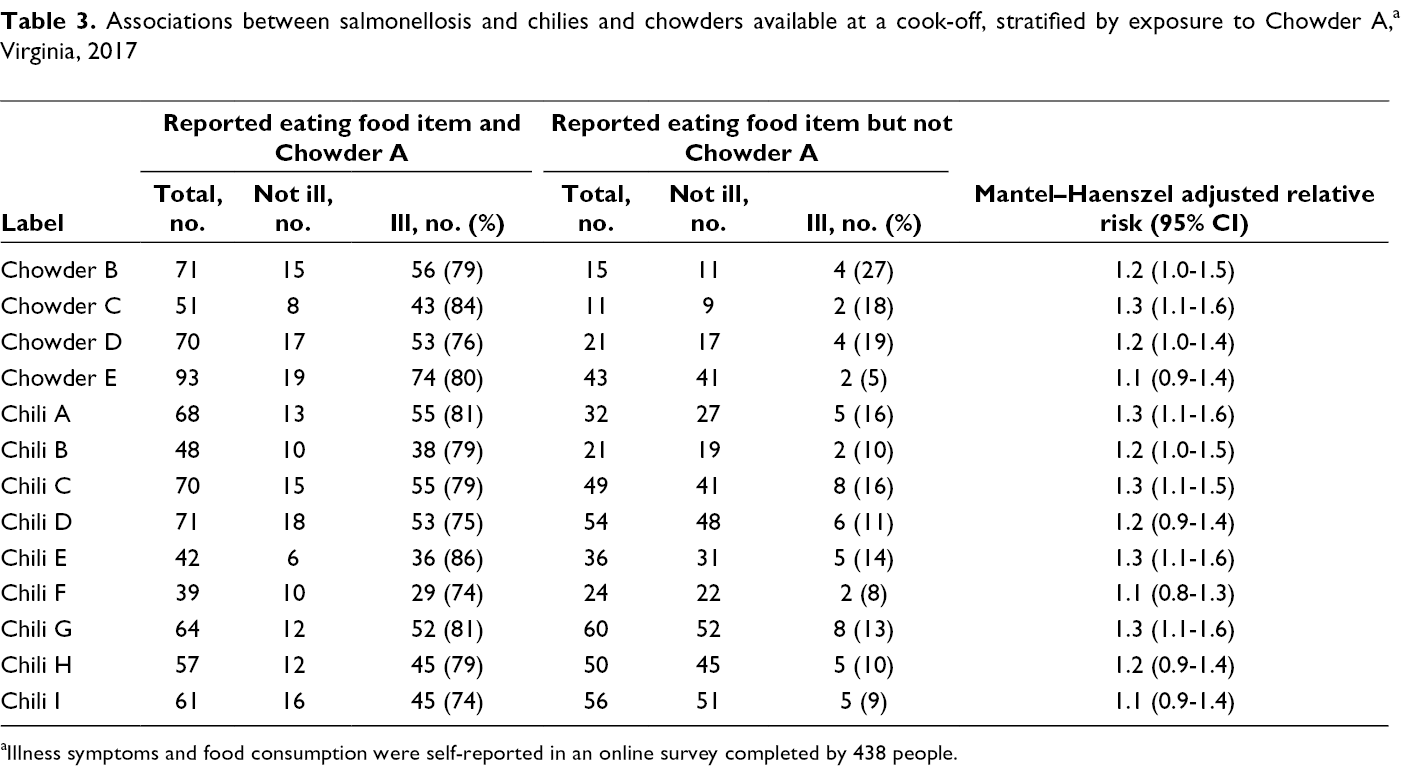
aIllness symptoms and food consumption were self-reported in an online survey completed by 438 people.
The Mantel–Haenszel adjusted RRs and 95% CIs for 4 chilies (A, C, E, and G) and 2 chowders (B and C) were >1, indicating increased risk for illness adjusting for Chowder A (Table 3).
Environmental Health Investigation
The food preparer reported cooking approximately 32 gallons of Chowder A early in the morning on the day of the cook-off. Ingredients included bacon, butter, flour, potatoes, onions, carrots, frozen raw clam strips, chicken broth, and cream that were purchased from a national restaurant supplier. The food preparer reported excessive cooking was avoided to prevent separation of the cream, but he reportedly measured the temperature at 185°F during cooking. The food preparer placed the chowder in plastic containers set in metal trays filled with ice until it was cool enough to move to a walk-in refrigerator. As needed during the cook-off, the food preparer removed portions of the chowder from the walk-in refrigerator, reheated it in pots on the stove, and transported it in plastic containers by vehicle approximately 1 mile to the cook-off.
At the cook-off, the chowder in the plastic containers was poured into metal chafing dishes, with lit methanol gel chafing fuel candles underneath to maintain heat. The food handler also wrapped aluminum foil around the base to prevent the candles from being blown out because of windy conditions that day. The food handler at the event reported she had no time to measure temperatures during the event. The investigation team received comments by telephone and online surveys that Chowder A was lukewarm or cold. No chowder was left over after the event. Neither the food handlers directly involved in the event nor any other kitchen staff members reported GI symptoms or illness before, during, or after the event.
During the October 13 re-interview of Chowder A food handlers, the establishment owners mentioned that chowder served at the event was actually from 2 batches; 1 was cooked 1 day before the event (September 29), and 1 was cooked on the morning of the event, as previously described.
Laboratory Investigation
Of 37 isolates received by state laboratories, 14 were from Virginia, 11 from Maryland, and 12 from Pennsylvania. All tested positive for Salmonella serotype Javiana. Twenty-five isolates were from survey respondents; 12 patients had not completed the survey. Of the 25 people who completed surveys, 22 reported exposure to Chowder A, including 2 people who reported Chowder A was the only item they ate at the cook-off. The next most common exposure was Chowder E, eaten by 12 people, all of whom also reported Chowder A exposure.
One isolate was from a Virginia resident who was not included in the data analysis because he did not attend or eat food from the cook-off. However, he reported eating steamed clams and steamed shrimp at the restaurant where Chowder A was prepared a day after the event. Salmonella was not identified in any food handler specimens or the sample of frozen raw clam strips that was the same type as those used in Chowder A. However, an uneaten sample of Chowder A that had been taken home by an event attendee tested positive for Salmonella serotype Javiana.
Three PFGE pattern types emerged among outbreak-related samples. The chowder sample and 21 clinical specimens belonged to pattern JGGX01.0349, a total of 15 clinical specimens belonged to pattern JGGX01.1197, and 1 specimen belonged to pattern JGGX01.3103, relative to historical serotype Javiana isolates typed by PFGE in the United States. According to higher-resolution genetic analysis using whole genome sequencing, the 14 Salmonella isolates from event attendees and the uneaten Chowder A sample were highly genetically related, with no single nucleotide polymorphism differences among isolates in the genomic regions compared. The Salmonella isolate from the patient who visited the restaurant after the event and became ill also had no single nucleotide polymorphisms different from the outbreak clade.
Discussion
Large-scale food events (eg, chili and chowder cook-offs) can make outbreak investigation challenging, from gathering information from event attendees to finding associations between food items and subsequent illness. In this outbreak, use of an online survey that was publicized in press releases and social media allowed investigators to quickly gather large amounts of data from ill and not ill attendees from multiple states. Many people at large-scale food events are exposed to multiple food items, confounding statistical associations. In the initial chili and chowder cook-off data analysis, 8 chilies and 5 chowders were significantly associated with illness.
To prevent future outbreaks, VDH recommendations for event organizers include requiring all competitors to prepare food items on-site, where the process can be monitored by environmental health specialists, and ensuring all competitors have sufficient heating equipment (eg, propane gas burners) that can withstand windy conditions for the duration of food service. Recommendations for chili and chowder cooks and other food preparers included following all recommended hand hygiene and surface cleaning practices to prevent any cross-contamination between foods, monitoring food temperatures to ensure the thresholds required to kill harmful bacteria are met (155 °F for fresh or 165 °F for reheated chili and chowder according to VDH Food Regulations) and maintained (≥135 °F for food service), with repeated trips through the “danger zone” for bacterial growth (41 °F to <135 °F) avoided as much as possible.
Multiple ingredients in the chowder and in the restaurant environment could, according to the literature, harbor Salmonella. For example, plant-derived food commodities (eg, fruits, leafy vegetables) are responsible for more than half of serotype Javiana outbreaks, 11 and Salmonella can also be found in seafood such as raw clams 12 and raw shrimp. 13 The environment of the Eastern Shore of Virginia itself is another potential contamination source. Samples from water, sediment from creeks, 14 and wildlife such as turtles, snakes, and birds 15 from that area have tested positive for Salmonella serotype Javiana, including 1 of the outbreak PFGE patterns. 14 Investigators were unable to determine whether cross-contamination occurred in the kitchen or from a local environmental source that resulted in introduction of Salmonella into the chowder.
Regardless of the initial source of contamination, time and temperature conditions of the chowder on the day of the cook-off could have promoted bacterial growth. The large volume of chowder (about 32 gallons), the need for transport to the fairgrounds, and windy conditions would have made reaching and maintaining a safe temperature difficult. Cross-contamination at the festival was unlikely because all contestants used their own serving equipment, and samples were eaten out of disposable containers with disposable utensils.
This outbreak illustrates the potential for large numbers of people to be infected with Salmonella from a contaminated food item at a large-scale event. The findings of this outbreak investigation led to recommendations that helped lead to a foodborne illness–free return of the chili and chowder cook-off in 2018.
Limitations
This study had several limitations. First, although it would have been ideal to interview all event attendees, no attendance list or contact information was available. ACHD recruited as many people as possible to complete the survey, and all press releases reflected a desire to inform all attendees whether or not they were ill, but limited enrollment may have resulted in a biased sample and misapplication of cohort analyses. Second, a map of vendors at the cook-off was not available until after the survey was deployed; inclusion of this map in the survey could have assisted with respondent recall. Finally, laboratory evidence from the original chowder ingredients and restaurant environment was not available; as such, the initial contamination source was unknown.
Conclusions
Consumption of Chowder A at the chili and chowder cook-off had the highest RR of salmonellosis, and Salmonella isolated from an uneaten sample of Chowder A was closely genetically related to clinical isolates from ill attendees. The substantial quantities of food required, the necessity of transporting food, and the lack of typical restaurant cooking equipment at food events can present unique challenges, and on-site oversight by environmental health specialists is a valuable tool to ensure food safety.
Footnotes
Acknowledgments
The authors thank the following agencies and people who assisted with the investigation: VDH Eastern Shore Health District: David Matson, William Pfeiffer, Kenneth “Wes” Greene, Iravon Ashby, Cynthia Bull, Scott Chandler, Nancy Decker, Teressa Downing, Jennifer “JJ” Justis, Patrina Keyes, Ann Lawson, Cheryl Revell, Jonathan Richardson, Chris Taylor, Ramona Kellam, and Mickey Kellam; VDH Division of Surveillance and Investigation: Stephanie Campbell; VDH Office of Environmental Health Services: Peri Pearson, Julie Henderson, and Shannon Macika; Division of Consolidated Laboratory Services: Chris Waggener, K Libuit, Stephanie De la Cruz, Elaine McCaffery, Sean Kelly, Tim Horseman, Daksha Patel, Mary Scoble, Francis Tannor, Shannon Levesque, Robert Barnes, Olga Hallum, Michelle Hodges, Arian Nassiri, Patricia Crosscut, Leigh Emma Lion, Mary Katherine Dickinson, Mona Johnson, Marc Carpenter, Wes Folston, Lauren Sawtelle, and Jessica Maitland.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors declared no financial support with respect to the research, authorship, and/or publication of this article.
