Abstract
Objectives:
In the United States, all men who have sex with men (MSM) were banned from donating blood from 1985 through 2015. In 2016, the guideline was amended such that men who had sexual contact with other men within the previous 12 months could not donate blood. We aimed to identify blood donation practices and their relationship with HIV risk and testing among young adult MSM (YMSM) at risk for having HIV.
Methods:
In 2014, we recruited HIV-negative non-Hispanic black, Hispanic, and non-Hispanic white YMSM aged 18-24 from across the United States through social media platforms to complete an online survey. Among these YMSM who previously donated blood, we conducted a secondary analysis examining the relationship between having donated blood within the past 12 months and sexual risk behavior from recent condomless anal intercourse (CAI), HIV testing, and self-perceived risk of having an undiagnosed HIV infection.
Results:
Of the 2261 YMSM surveyed, 1104 (48.8%) had ever previously donated blood and 305 (13.5%) had donated blood within the past 12 months. Of the 305 blood donors, 50 (16.4%) had ever had CAI before their most recent blood donation. Among YMSM who donated blood, past–12-month blood donation was more likely among YMSM who never had CAI (adjusted odds ratio [aOR] = 1.84; 95% confidence interval [CI], 1.24-2.73) than among YMSM who had CAI and more likely among YMSM who believed it was not possible at all that they had an undiagnosed HIV infection (aOR = 1.57; 95% CI, 1.14-2.16) than among YMSM who believed there was any possibility of having an undiagnosed HIV infection; it was not related to past–12-month HIV testing.
Conclusions:
YMSM donated blood frequently, suggesting that the deferral process in place did not prevent YMSM from donating blood. The current donor screening process should be reconsidered if it is to prevent YMSM from donating blood. Future research could identify screening questions that permit YMSM with a low risk of HIV infection to donate blood while maintaining the safety of the blood supply.
In 1985, the US Food and Drug Administration (FDA) enacted a guideline that excluded all men who had sexual contact (“sexual contact” was not defined) with another male after 1977 from donating blood because of concerns about transfusion-related HIV transmission. 1 –4 The FDA did not revise that guideline until December 2015, when it introduced a deferral period of 12 months after sexual contact with another man. 5 In May 2016, the FDA approved a revised blood donor screening questionnaire designed to exclude men who self-reported “sexual contact” (still not defined) with another man in the past 12 months from donating blood. 6,7 Critics of the revised guideline said that it was too restrictive and that it stigmatized sexual minority groups. 4,8,9 Some opponents noted that the blanket exclusion was excessively cautious because all blood products are screened for HIV, and modern diagnostic technology has substantially increased the sensitivity and specificity of HIV detection. 3,9 –11 The revised guideline’s effectiveness in excluding men who have sex with men (MSM) blood donors is unknown, although evidence suggests that donors might not answer blood donation screening questionnaires truthfully. 12 –21 Post–blood-donation surveys reveal that the proportion of male blood donors who self-reported sexual contact with other men in the post–blood-donation survey but not on the blood donor screening questionnaire increased over time, from 0.6% in 1993, 12 to 1.2% in 1998, 13 and to 2.6% in 2013. 14 Despite this increase in the percentage of MSM blood donors, the risk of HIV transmission via blood transfusion in the United States is small and has decreased over time. It was estimated at about 1 in 1.4-2.4 million transfusions in 2001. 22 The risk of donating HIV-infected blood during the period before the virus is detectable is also decreasing, estimated at 1 in 1.1 million donations in 2013-2014. 23
Most quantitative research on blood donation consists of post–blood-donation surveys, 12 –15,21 the findings of which are limited by small samples of MSM and probable underreporting of risk behaviors. Qualitative studies on this topic indicate that MSM blood donors are not unlike heterosexual donors: MSM donors value blood safety, share similar motivations for donating blood, 4,20 and tend to answer eligibility screening questions based on whether they consider their blood safe to donate. 20 Qualitative findings from Britain and the United States further suggest that MSM who donate blood do so because they practice safer sex or perceive themselves to be at low risk of having HIV. 4,16,20 However, self-perceived risk and reported risk behaviors have a complex interrelationship, 24 so it is unclear whether MSM who donate blood have fewer risk behaviors than MSM who do not donate blood. In addition, many MSM are unaware of their HIV status. In the United States, for example, an estimated 60% of HIV-infected teenagers and young adults aged 13-24 are unaware of their infection 25 and could pose a risk of HIV transmission if donating blood during the window period before the virus is detectable.
To better understand HIV risk factors among young adult MSM (YMSM) blood donors in the United States before the FDA deferral period was shortened to 1 year, we performed a secondary analysis of a national survey 26 on the blood donation history and sexual-risk behaviors of non-Hispanic black, Hispanic, and non-Hispanic white MSM aged 18-24 who use social media and believe themselves to be not infected by HIV. We examined the interrelationships of blood donation, HIV testing, self-perceived risk of having an undiagnosed HIV infection, and reported HIV risk behaviors. We were interested in whether their past–12-month blood donation behavior was associated with low self-perceived risk and reported risk behaviors or was cause for concern because of the possible risk of unknowingly donating HIV-infected blood.
Methods
Data
This secondary analysis used data the research team collected via an online survey, results of which have been published previously. 26 From August through December 2014, we invited YMSM aged 18-24 across the United States to participate in an anonymous online survey about HIV testing, HIV risk behaviors, and HIV testing preferences. 26 More details on the sites and sampling methods are published elsewhere. 26,27 Briefly, we recruited participants from social network and MSM-centric online dating sites including Bender, BGCLive, Facebook, Grindr, Growlr, Pinterest, and Reddit via targeted advertisements, pop-up advertisements, banner advertisements, emails, or referrals by other study participants. For sites with such capabilities, emails and advertisements were targeted at young adults aged 18-24 and men identifying as MSM. Potential participants viewing these advertisements were provided a brief introduction to the study and, if interested, were directed to the study website. The study website was accessible using both handheld and desktop devices and provided more information about the study. We followed recommended procedures to reduce multiple responses from the same individual and to maintain participant engagement. 28 Specifically, the survey blocked previously used internet addresses to prevent multiple responses. The survey used an inviting interface and included comical encouraging statements and eye-catching photos of attractive men to maintain participant engagement. English- and Spanish-language survey instruments underwent pilot testing evaluation and iterative revisions to ensure participant engagement and comprehension. The English-language questionnaire is available online. 29
The survey began with an eligibility screener to identify English- or Spanish-speaking YMSM who self-identified as non-Hispanic black, Hispanic (any race), or non-Hispanic white; were living in the United States; ever had anal sex with another man; and never had a positive HIV test (per self-report). We did not include YMSM who did not self-identify with any of these 3 racial/ethnic categories. The eligibility screener invited potential participants who were eligible and gave informed consent to participate in the study. YMSM who enrolled in the study were entered in a lottery for 1 of 6 $100 gift cards as an incentive for participation. The Lifespan-Rhode Island Hospital Institutional Review Board approved the study.
Analysis
Our analytic sample included men who had ever donated blood and excluded men who dropped out of the study before answering all questions of interest or who responded “refused” or “don’t know” to questions about blood donation, self-perceived risk of having an undiagnosed HIV infection, HIV testing history, or condom use history. We conducted all analyses by using Stata release 14. 30
We used the Pearson χ2 test, Fisher exact test, or Kruskal-Wallis rank test in bivariate analyses to compare demographic characteristics (age, education, race/ethnicity, geographic region), HIV testing history (testing not done at blood donation), self-perceived risk of having an undiagnosed HIV infection, and HIV risk behaviors of those who donated blood within the past 12 months and those who donated blood more than 12 months ago. We considered α = .05 to be significant. We determined self-perceived risk of having an undiagnosed HIV infection by asking, “How likely is it that you are infected with HIV (are HIV positive) but might not know it?” We dichotomized responses into “not possible at all” and “possible” (which included the responses of “not likely,” “somewhat likely,” “likely,” or “very likely”). We chose this separation between having no perceived likelihood of being infected with HIV and any perceived likelihood of being infected with HIV because the goal of blood donor screening is to identify potential donors who are not at risk of having transfusion-transmissible infections. We categorized participants further by how recently they had donated blood (<1 month ago, 1-6 months ago, 7-12 months ago, 1-2 years ago, >2 years ago, or never). Within each time interval, we calculated the proportion and 95% confidence intervals (CIs) of participants according to their most recent condomless anal intercourse (CAI) with another man and their self-perceived likelihood of having an undiagnosed HIV infection.
We used univariable logistic regression analysis to estimate the association between donating blood recently (within the past 12 months) and 4 factors: never having had CAI, no CAI within the past 12 months, no HIV testing within the past 12 months, and no self-perceived risk of having an undiagnosed HIV infection. Subsequent multivariable logistic regression models controlled for factors associated with recent blood donation in the aforementioned bivariate analyses: age, race/ethnicity, US region of residence, education (years), and having a primary care provider. We constructed additional models stratified by race/ethnicity, and we estimated odds ratios (ORs) and corresponding 95% CIs.
Results
Characteristics of the Study Sample
A total of 2772 YMSM aged 18-24 were eligible and chose to enroll in the study. Of those, 381 YMSM dropped out during the survey, and 130 had incomplete information on blood donation, self-perceived likelihood of an undiagnosed HIV infection, HIV testing, or condom use. Of the 2261 remaining YMSM, 1104 (48.8%; 95% CI, 45.9%-51.8%) had donated blood at least once in their lives, and the prevalence of donation was similar across racial/ethnic groups (Figure 1). Most of the 1104 YMSM blood donors had more than 12 years of formal education (n = 910, 82.4%) and had health insurance (n = 848; 76.8%); the largest proportion lived in the southern United States (n = 480, 43.5%; Table 1). All 50 states and the District of Columbia were represented in the sample. Of the 1104 participants, 949 (86.0%) self-perceived that it was not possible at all or not likely that they had an undiagnosed HIV infection, and 731 (66.2%) had been tested for HIV within the past 12 months.
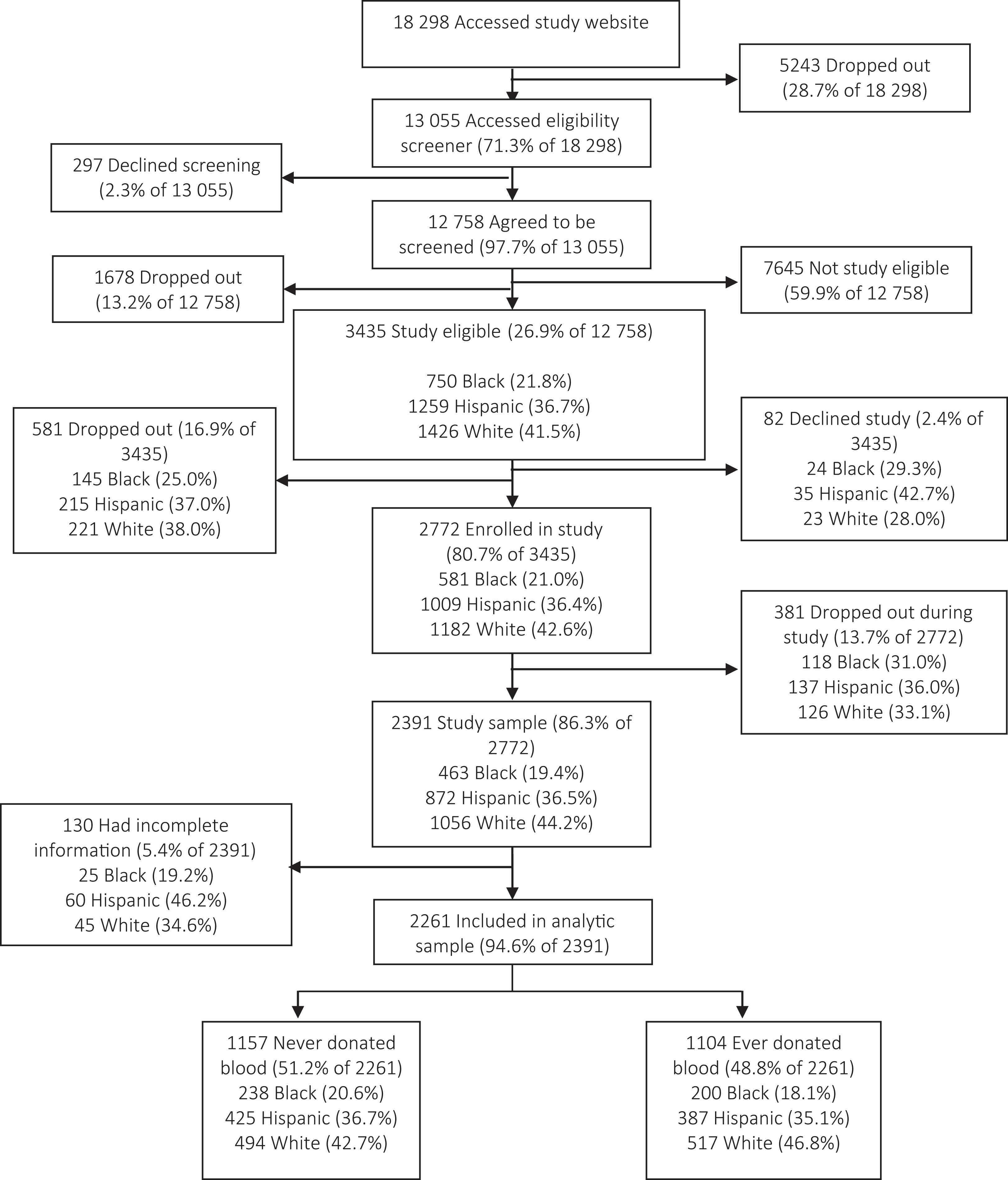
Study enrollment, retention, and prevalence of lifetime blood donation among men who have sex with men aged 18-24 who responded to an online survey from social media and online dating sites, United States, 2014. 27 Observations with “don’t know” or “refused” responses to a survey question on blood donation, possibility of being infected with HIV, HIV testing, or condom use were considered incomplete and were excluded from the analytic sample. Horizontal arrows represent men who were excluded or declined to participate. Black refers to non-Hispanic black, white refers to non-Hispanic white, and Hispanic refers to any race. Secondary analysis of previously published data.
Characteristics of men who have sex with men (MSM) aged 18-24 who had ever donated blood, by blood donation status within the past 12 months, online survey from social media and online dating sites, United States, 2014a,b
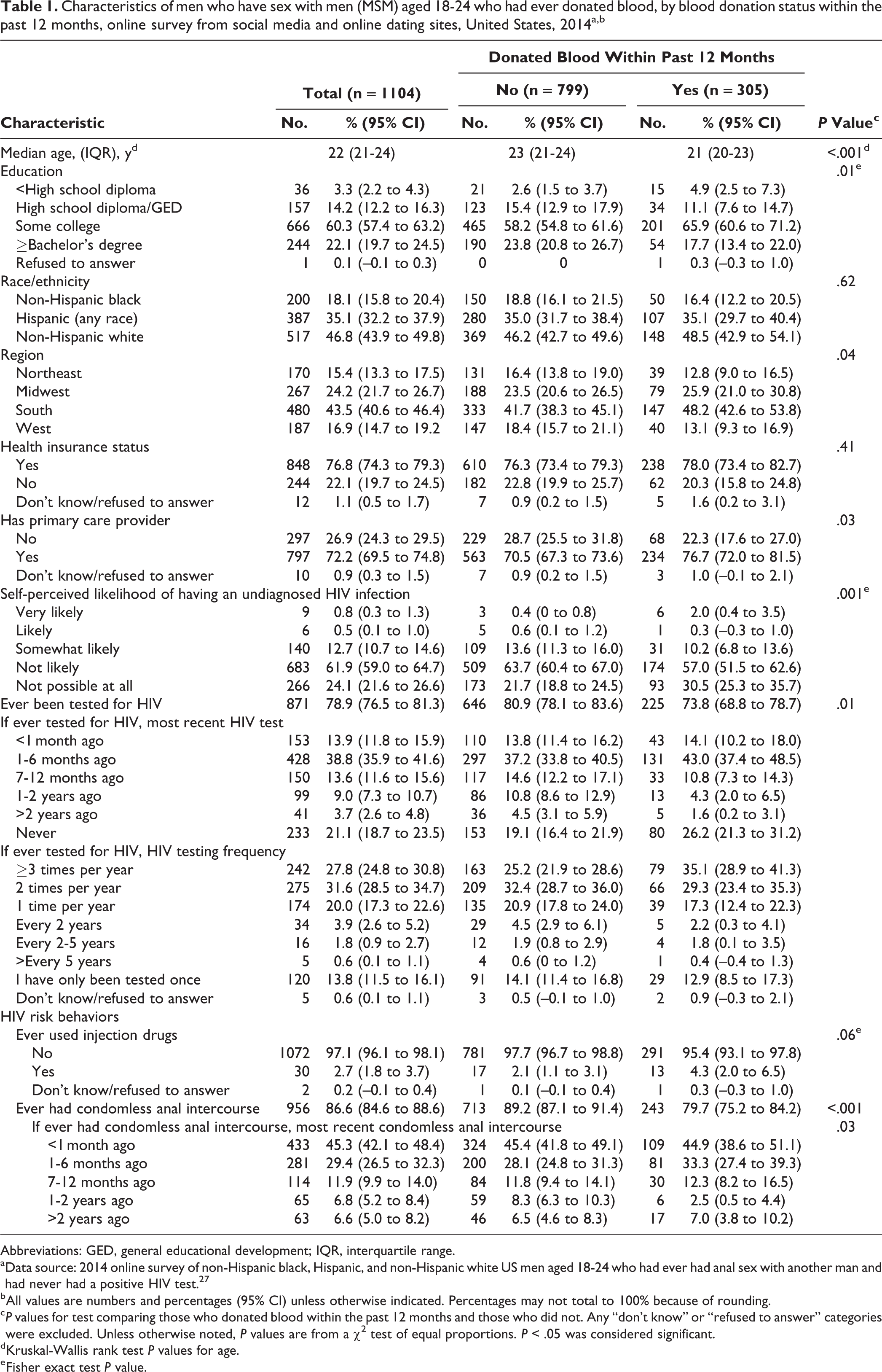
Abbreviations: GED, general educational development; IQR, interquartile range.
a Data source: 2014 online survey of non-Hispanic black, Hispanic, and non-Hispanic white US men aged 18-24 who had ever had anal sex with another man and had never had a positive HIV test. 27
b All values are numbers and percentages (95% CI) unless otherwise indicated. Percentages may not total to 100% because of rounding.
c P values for test comparing those who donated blood within the past 12 months and those who did not. Any “don’t know” or “refused to answer” categories were excluded. Unless otherwise noted, P values are from a χ2 test of equal proportions. P < .05 was considered significant.
d Kruskal-Wallis rank test P values for age.
e Fisher exact test P value.
Relationship of Past–12-Month Blood Donation With Participant Demographic Characteristics, HIV Testing History, Self-Perceived Undiagnosed HIV Risk, and Reported HIV Risk Behaviors
Compared with YMSM who donated blood more than 12 months ago (n = 799), YMSM who donated blood within the past 12 months (n = 305) were younger (median age 21 vs 23) and were less likely to ever have been tested for HIV (73.8% vs 80.9%) or had CAI (79.7% vs 89.2%; Table 1). YMSM who donated blood within the past 12 months were more likely to have a primary care provider (76.7%) than YMSM who had not donated blood within the past 12 months (70.5%). The 2 groups were distributed differently across geographic regions, by education, and in self-perceived likelihood of having an undiagnosed HIV infection. Although survey respondents did not report the first time they donated blood or had CAI, 14 participants who reported donating blood <1 month ago also reported their most recent CAI was between 1 month and 1 year ago and, therefore, had CAI before donating blood. Of the 32 YMSM who donated blood within the past month, 15 (47%) reported having CAI before donating blood (Table 2). Following the same logic, 50 (10 + 4 + 1 + 13 + 3 + 7 + 2 + 10 = 50) of the 305 (16.4%) YMSM who donated blood within the past 12 months reported having CAI in a time interval preceding their most recent blood donation.
Most recent condomless anal intercourse and recency of blood donation among men who have sex with men aged 18-24 who had ever donated blood, online survey from social media and online dating sites, United States, 2014a
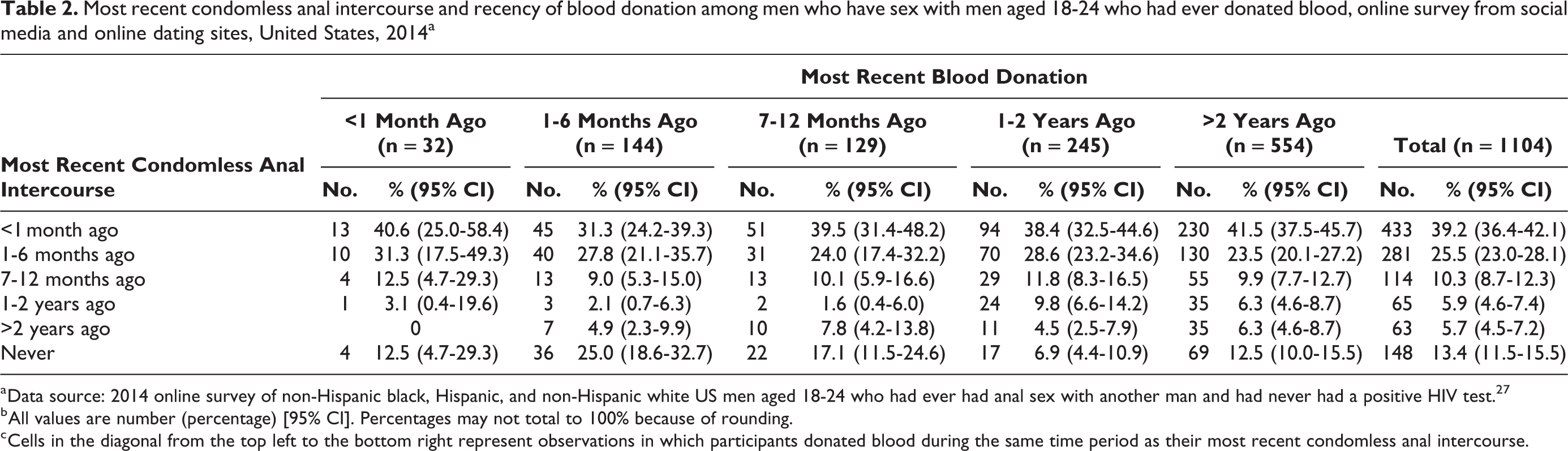
a Data source: 2014 online survey of non-Hispanic black, Hispanic, and non-Hispanic white US men aged 18-24 who had ever had anal sex with another man and had never had a positive HIV test. 27
b All values are number (percentage) [95% CI]. Percentages may not total to 100% because of rounding.
c Cells in the diagonal from the top left to the bottom right represent observations in which participants donated blood during the same time period as their most recent condomless anal intercourse.
In general, the self-perceived risk of having an undiagnosed HIV infection was similar across categories of time since most recent blood donation (Table 3). However, 30.5% (95% CI, 25.3%-35.7%) of YMSM who had donated blood within the past 12 months self-perceived no possible risk of an undiagnosed HIV infection, whereas 21.7% (95% CI, 18.8%-24.5%) of YMSM who had not donated blood within the past 12 months self-perceived no possible risk of an undiagnosed HIV infection (Table 1).
Self-perceived likelihood of having an undiagnosed HIV infection versus recency of blood donation among men who have sex with men aged 18-24 who have ever donated blood, online survey from social media and online dating sites, United States, 2014a,b
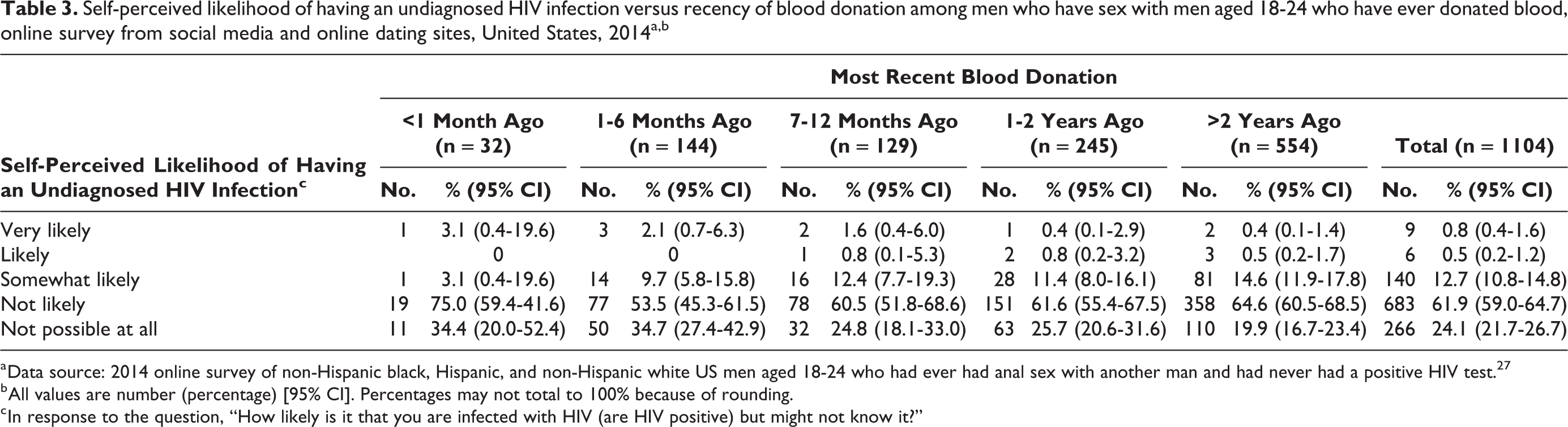
a Data source: 2014 online survey of non-Hispanic black, Hispanic, and non-Hispanic white US men aged 18-24 who had ever had anal sex with another man and had never had a positive HIV test. 27
b All values are number (percentage) [95% CI]. Percentages may not total to 100% because of rounding.
c In response to the question, “How likely is it that you are infected with HIV (are HIV positive) but might not know it?”
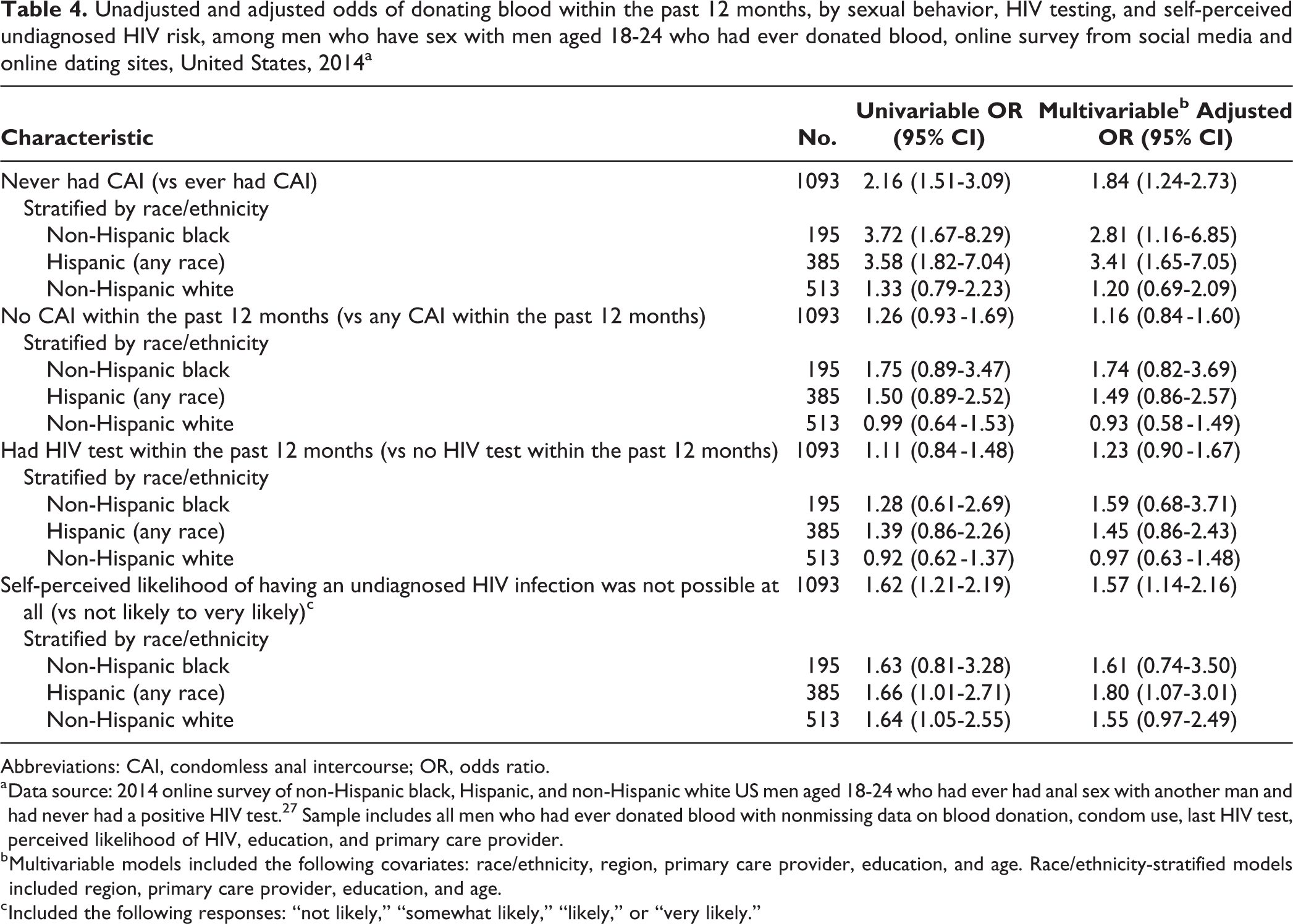
In multivariable analyses, YMSM who had never had CAI had higher odds of donating blood within the past 12 months than YMSM who had ever had CAI (aOR = 1.84; 95% CI, 1.24-2.73), as did YMSM reporting no self-perceived likelihood of an undiagnosed HIV infection compared with YMSM who reported any likelihood of an undiagnosed HIV infection (aOR = 1.57; 95% CI, 1.14-2.16; Table 4). Donating blood within the past 12 months was not associated with having had an HIV test within the past 12 months (aOR = 1.23; 95% CI, 0.90-1.67) or having had CAI within the past 12 months (aOR = 1.16; 95% CI, 0.84-1.60). The observed relationships generally were similar when stratified by racial/ethnic group, except for no previous CAI (no association for non-Hispanic white YMSM) and self-perceived likelihood of an undiagnosed HIV infection (no association for non-Hispanic white or non-Hispanic black YMSM).
Unadjusted and adjusted odds of donating blood within the past 12 months, by sexual behavior, HIV testing, and self-perceived undiagnosed HIV risk, among men who have sex with men aged 18-24 who had ever donated blood, online survey from social media and online dating sites, United States, 2014a
Abbreviations: CAI, condomless anal intercourse; OR, odds ratio.
a Data source: 2014 online survey of non-Hispanic black, Hispanic, and non-Hispanic white US men aged 18-24 who had ever had anal sex with another man and had never had a positive HIV test. 27 Sample includes all men who had ever donated blood with nonmissing data on blood donation, condom use, last HIV test, perceived likelihood of HIV, education, and primary care provider.
b Multivariable models included the following covariates: race/ethnicity, region, primary care provider, education, and age. Race/ethnicity-stratified models included region, primary care provider, education, and age.
c Included the following responses: “not likely,” “somewhat likely,” “likely,” or “very likely.”
HIV Testing History, CAI History, and Self-Perceived Risk of Undiagnosed HIV Infection
Two hundred twenty of 305 (72.1%) YMSM who donated blood within the past 12 months also reported having had CAI within the past 12 months. Having an HIV test within the past 12 months was more common among YMSM who had CAI within the past 12 months (157 of 220, 71.4%) than among YMSM who did not have CAI within the past 12 months (50 of 85, 58.8%). Self-perceived risk of undiagnosed HIV infection also tended to be lower among participants who had never had CAI than among participants who had had CAI, regardless of HIV testing status (Figure 2).
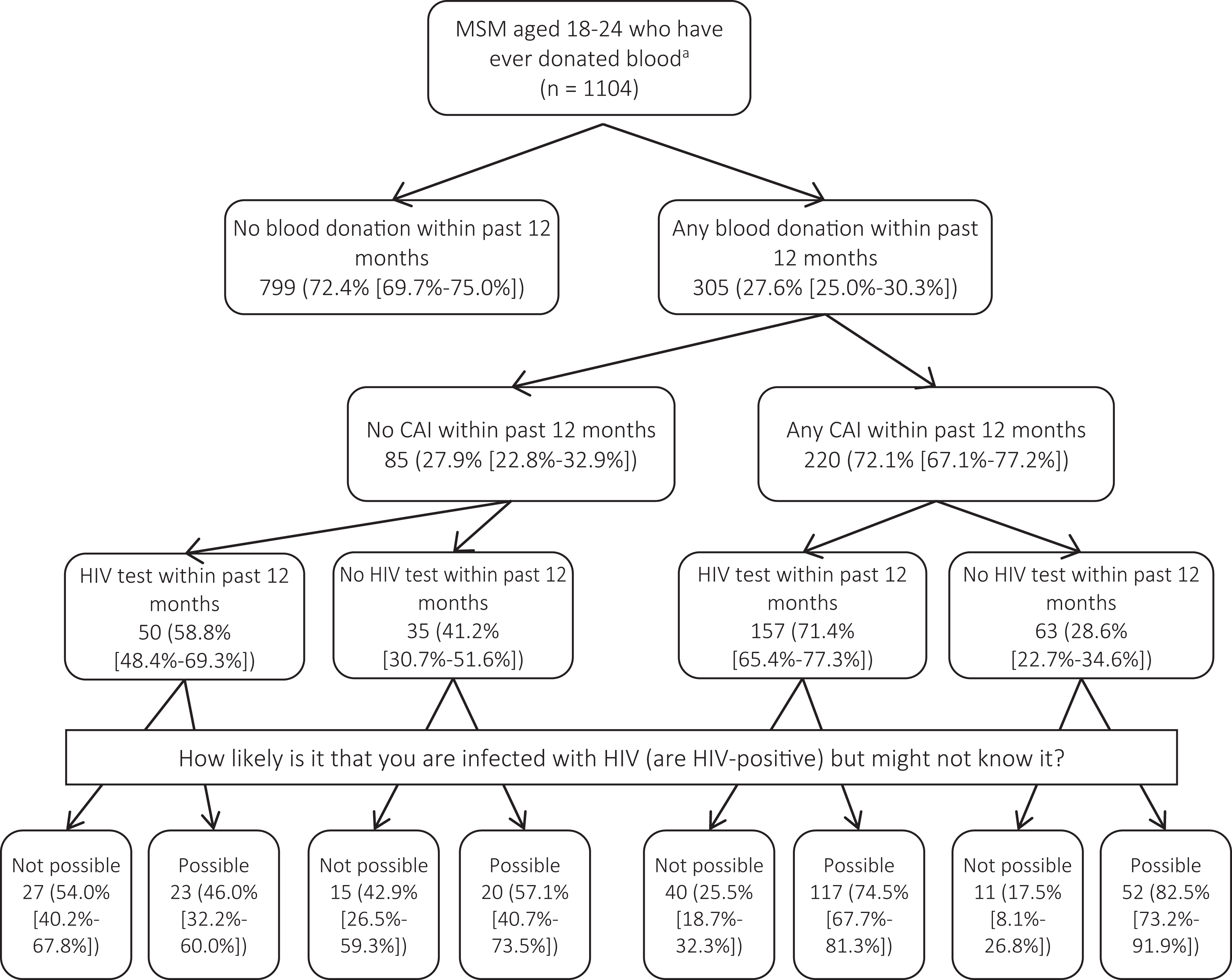
Blood donation history, condom use, HIV testing history, and self-perceived likelihood of having an undiagnosed HIV infection among men who have sex with men (MSM) aged 18-24 who responded to an online survey from social media and online dating sites, United States, 2014. 27 The sample includes US men who had ever had anal sex with another man, had never had a positive HIV test, and had ever donated blood. Likert-type scale responses to the question about likelihood of HIV infection were combined for simplicity. “Not possible” encompasses “not possible at all” and “possible” encompasses “not likely,” “somewhat likely,” “likely,” and “very likely.” Data are presented as number (percentage) [binomial 95% confidence interval of proportion]. Percentages were calculated by using the number in the box immediately above as the denominator. Secondary analysis of previously published data. Abbreviation: CAI, condomless anal intercourse.
Discussion
Among YMSM aged 18-24 surveyed, nearly half had ever donated blood despite the 1985 FDA blood donation ban in effect at the time of the study. Although the survey did not provide data on what proportion of YMSM donated blood before ever having sex with other men and ceased doing so afterward, these data can be used to approximate an upper bound and lower bound on compliance had the 2016 FDA guideline been in effect. If we assume that CAI occurred before blood donation when the most recent episode of both behaviors was reported in the same time frame, up to 220 (72.1%) YMSM who had donated blood within the past 12 months would have been noncompliant with the revised guideline because of CAI during the previous 12 months. At a minimum, 50 of 305 (16.4%; 95% CI, 6.1%-26.7%) recent donors reported that their most recent CAI occurred before their most recent blood donation.
The prevalence of blood donation was 48.8% in this sample of YMSM. Few studies of blood donation among YMSM are available with which to compare these results. Of the weighted sample of 14 631 600 men aged 18-24 in the 2010 National Health Interview Survey (not restricted to YMSM), 4 408 257 (30.1%; 95% CI, 26.8%-33.5%) had donated blood since 1985 and 1 582 316 (10.8%; 95% CI, 8.5%-13.1%) had donated blood in the past year. 31 The percentage of YMSM who had ever donated blood was 48% in a 2012 online survey in Hong Kong (advertised as a blood donation study), 18 76% in a 2014 online survey in Israel (excluding HIV-infected participants), 19 29% in a population-based survey in Britain (2009-2010), 16 and 50% of bisexual or homosexual Boston-area men surveyed in 1984. 32 In a 2011 survey of MSM in San Francisco, 23% of MSM had donated blood since 1977. 33 In the San Francisco survey, 25.2% of MSM blood donors were determined to be noncompliant with the ban based on their age at first intercourse with another man and their age when the ban went into effect. 33 Most MSM donors in the Israel study (63%) denied their sexual orientation in screening, 19 and 39.7% of MSM blood donors in Britain reported donating blood while they were ineligible under similar criteria as in the United States. 16 The prevalence of lifetime donation in our study is comparable with estimates reported in previous studies but near the higher end of the range of reported estimates. This result is surprising given that this population should have been turned away at screening. However, only one definitively published case of transfusion-transmission of HIV in the United States has occurred since 2002. 34 Knowing that MSM donate blood suggests that MSM who elect to donate blood are not at higher risk of HIV infection than other blood donors or that testing procedures for donated blood are working well.
Although many YMSM in our study did not comply with blood donation policies, these data support qualitative data that MSM donate blood under the belief that their blood is safe because of their self-perceived low-risk behavior, such as frequent HIV testing or being in a monogamous relationship. 4,16,20 Supporting this theory, one post–blood-donation survey found a substantially lower prevalence of HIV among MSM blood donors (0.3%) than among the general MSM population (approximately 11%-12%). 5 YMSM in our study who donated blood within the past 12 months were less likely than YMSM who donated blood more than 12 months ago to have ever had CAI and more likely to have a lower self-perceived likelihood of undiagnosed HIV infection. Multivariable analysis indicated that YMSM who had never had CAI were more likely than YMSM who had had CAI to have donated blood within the past 12 months; however, in stratified analysis, we observed this relationship among non-Hispanic black and Hispanic YMSM but not among non-Hispanic white YMSM. More research aimed at understanding the reasons for these racial/ethnic differences may better inform blood donation policies.
HIV testing within the past 12 months was not associated with donating blood. One explanation for this finding is that HIV testing was common among the study population and all participants who had been tested for HIV reported a negative result (per study eligibility criteria), which might have reduced the ability to assess the relationship between HIV testing and blood donation. In an ideal scenario, potential MSM blood donors would obtain a negative HIV test result before donating blood. HIV RNA testing shrinks the period between infection virus detection and increases the likelihood of a true-negative test result. 9,10 Objective data on the value of recent HIV testing as a marker of blood donation eligibility for MSM are not now available.
Current FDA blood donor screening guidelines attempt to prevent blood donation by men who have had sex with another man within the past 12 months. 7 Nearly three-quarters (n = 220, 72.1%) of YMSM in our sample who donated blood within the past 12 months also had CAI within the previous 12 months, and many more-recent donors had also had CAI recently. These observations undermine faith in the usefulness of screening by self-report of any sex with another man after 1977, and it is unknown whether these men would have had different blood donation behavior under the updated guideline. Screening that is designed according to HIV risk behaviors and that has waiting periods based on current detection abilities, regardless of MSM status, is generally viewed as more acceptable than screening that targets MSM and is standard in several developed countries. 4,19,35 Future work might compare the screening effectiveness of sensitive questions (eg, risk behaviors, such as CAI) with questions that may be perceived as discriminatory, such as the current screening strategy.
Limitations and Strengths
Our study had 3 main limitations. First, the sample was not necessarily representative of the underlying population of non-Hispanic black, Hispanic, and non-Hispanic white YMSM (whether or not they use the social media outlets used to recruit participants for this study). As such, our results may not be generalizable to the population of YMSM in the United States. Also, because we included only non-Hispanic black, Hispanic, and non-Hispanic white YMSM in our study, our findings may not be generalizable to MSM from other racial/ethnic backgrounds or transgender populations. Second, the survey was not specific enough to determine how many YMSM donated blood before ever having sex with other men and ceased blood donation afterward or if any YMSM donated blood during the window period between initial infection and virus detection. However, our data indicate recent CAI among many young blood donors. Third, because of limits of the cross-sectional questionnaire, we do not know if blood donation behavior changed over time.
This study also had 2 strengths. First, anonymity may have increased the likelihood of veracity of the self-reported data. Second, our extensive survey development processes indicated high levels of comprehension of study questions among participants. Participants had a high level of understanding of the blood donation question and were able to distinguish blood donation as separate from phlebotomy for medical testing.
Conclusion
Young adult MSM participating in this study donated blood frequently despite the ban in effect in the United States at the time of the study. A high proportion of YMSM who donated blood within the past 12 months also had CAI within the past 12 months, which is in opposition to current FDA guidelines. Although the choice to donate blood for some YMSM was congruent with perceived HIV risk (ie, recent blood donors had a low self-perceived risk of having an undiagnosed HIV infection), we found that this association between self-perceived risk and recent blood donation was not consistent across racial/ethnic groups. Although the current screening questions apply a 12-month deferral instead of permanent deferral, it is unknown if YMSM are more likely to comply with current guidelines than with the permanent deferral. The current screening questions for excluding blood donations should be reconsidered if YMSM are to be prevented from donating blood. In addition, future research is needed to identify better options to permit YMSM who are at low risk of HIV infection to donate blood while maintaining the safety of the blood supply.
Footnotes
Acknowledgments
The authors gratefully recognize the assistance of Ian Donaghy and Justin Romanoff in the execution of this study.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Disclaimer
Preliminary findings from this research were presented at the 9th International AIDS Society Conference on HIV Science (IAS 2017) in Paris, France, July 24-26, 2017.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was supported by grants from the National Institute of Nursing Research (R21 NR023869, ![]() Identifier: NCT02369627) and the National Institute of Mental Health (4T32MH078788-09).
Identifier: NCT02369627) and the National Institute of Mental Health (4T32MH078788-09).
