Abstract
A case of bilateral superior canine tooth pulp necrosis in an 18-year-old male
Introduction
Non-human primates (NHPs) are commonly used as laboratory animals for research purposes. Tooth fracture or excessive consumption may occur during the animal lifespan, and both conditions often result in exposure of the pulp cavity, commonly leading to root abscess.1,2
Due to their position and dimension, canines fracture more frequently than other teeth. In particular, it has been reported that superior canines are often affected by root abscesses in NHPs,3-5 resulting in periorbital swelling of the affected side and/or odontopathic fistula with drainage underneath the eye.1,4-6 The presence of abscess or fistula of the tooth root can be painful, gradually leading to reduced food consumption and weight loss, thus affecting the animal’s wellbeing. 1 Moreover, the animal may subsequently develop osteomyelitis and sepsis with associated systemic signs. 1 This condition may hinder the involvement of the subject in experimental trials. As in human dentistry, dental radiographs can provide conclusive information on dental condition, 1 and computed tomography (CT) may also be indicated when more detailed images of the infected tooth are required.
Treatment for dental abscesses consists of extraction of the affected tooth and drainage of purulent material, but also endodontic treatment should be considered.1,7-9
In NHPs, the extraction of the canine tooth has often been described as the method of choice for dental abscess, although this procedure is very invasive for the animal due to the anatomical conformation of the canine root.1,9,10 On the contrary, endodontic treatments, although more conservative and less traumatic for the animal, are scarcely reported in the literature.1,9,10
Here, we describe the clinical management of bilateral superior canine tooth pulp necrosis in a male cynomolgus monkey (
Materials and methods
An 18-year-old male Right parasagittal image of the skull obtained from the multiplanar reconstruction of the pre-contrast CT series before treatment. Image shows periapical bone lysis of the right upper canine tooth along with the corresponding root canal measurement.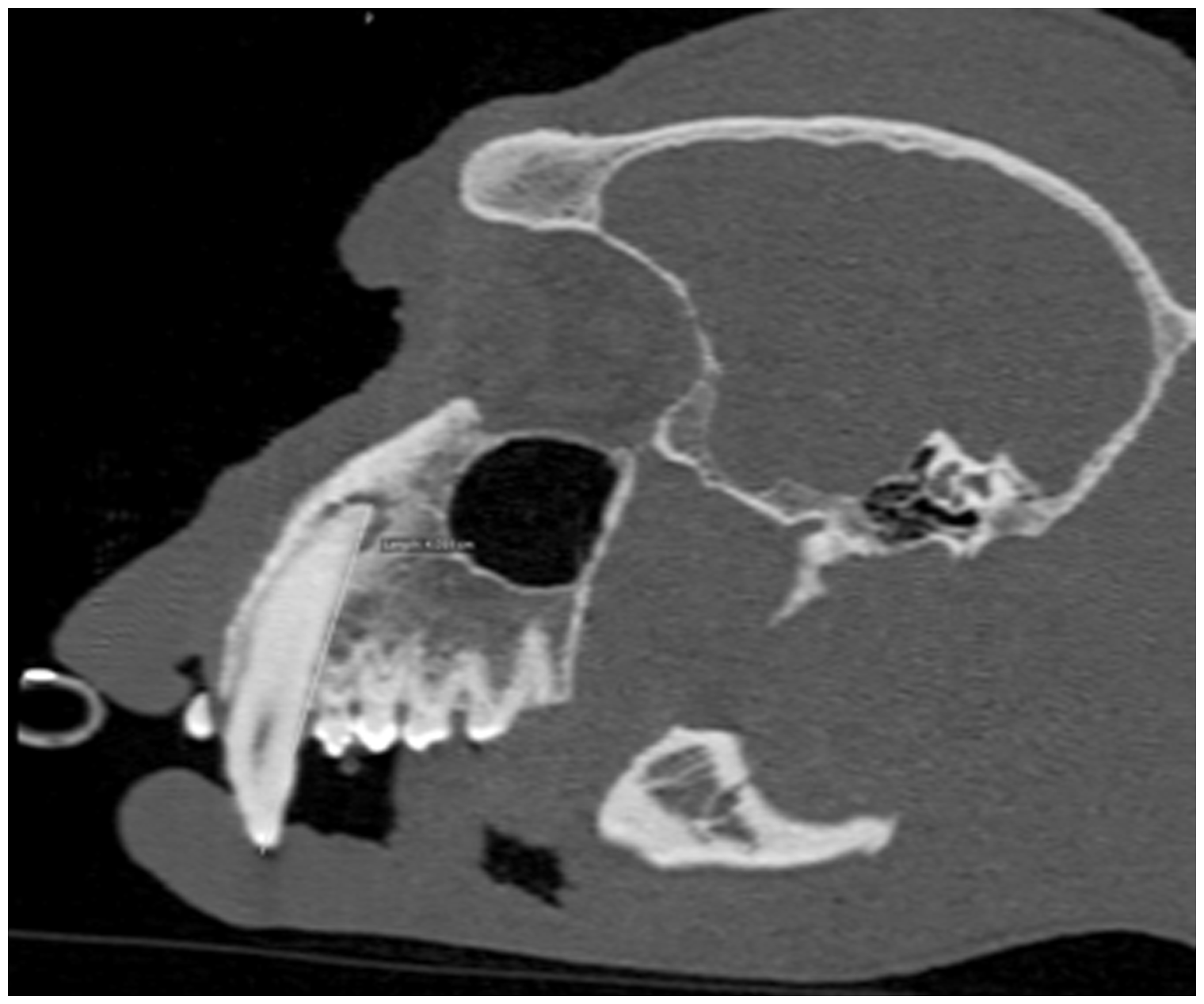
On the basis of the antibiogram test result, the macaque received a systemic antibiotic (12.5 mg/kg of spiramycin and metronidazole (Spiroxan; Ceva Salute Animale spa, Agrate Brianza, Italy)), orally every 12 hours for 7 days, to treat
After 10 days, foam rubber and temporary sealant were removed from the anaesthetized macaque. The root canal was irrigated to remove the iodoform paste residuals and sealed with gutta percha points (ISO 80) and endodontic cement (Sealapex, KerrHawe S.A., Via Strecce, 4-CH-6934 Bioggio, Switzerland) using a plugger to compact them to the root wall. A System-B Heat Source was adopted to heat the abovementioned materials. The residual coronal portion of the root canal was filled with gutta percha, melted by means of an obtura syringe and then compacted with a plugger. Finally, the pulp canal was sealed with Relyx Unicem 3 M® (3M Deutschland GmbH) cured using an LED lamp (Led.E Wireless Curing Light, Giorgio De Carli, Italy). The coronal portion of the canine was restored with an adhesive technique and composite (Scotchbond universal adhesive 3M, Deutschland GmbH; ∑ Quick, Tokuyama Dental Corporation 38-9, Taitou 1-chome, Taitou-ku, Tokyo, Japan).
At the end of the procedure, radiographs of the treated tooth were taken to verify the success of the procedure (Figure 2). The anti-inflammatory therapy described above was then repeated for two days.
Right lateral (oblique) projection of the skull after the definitive endodontic upper right canine tooth treatment. Radiopaque material within the right canine root canal is evident. Single asterisk shows the endotracheal tube; double asterisk shows the pulsossimetry probe.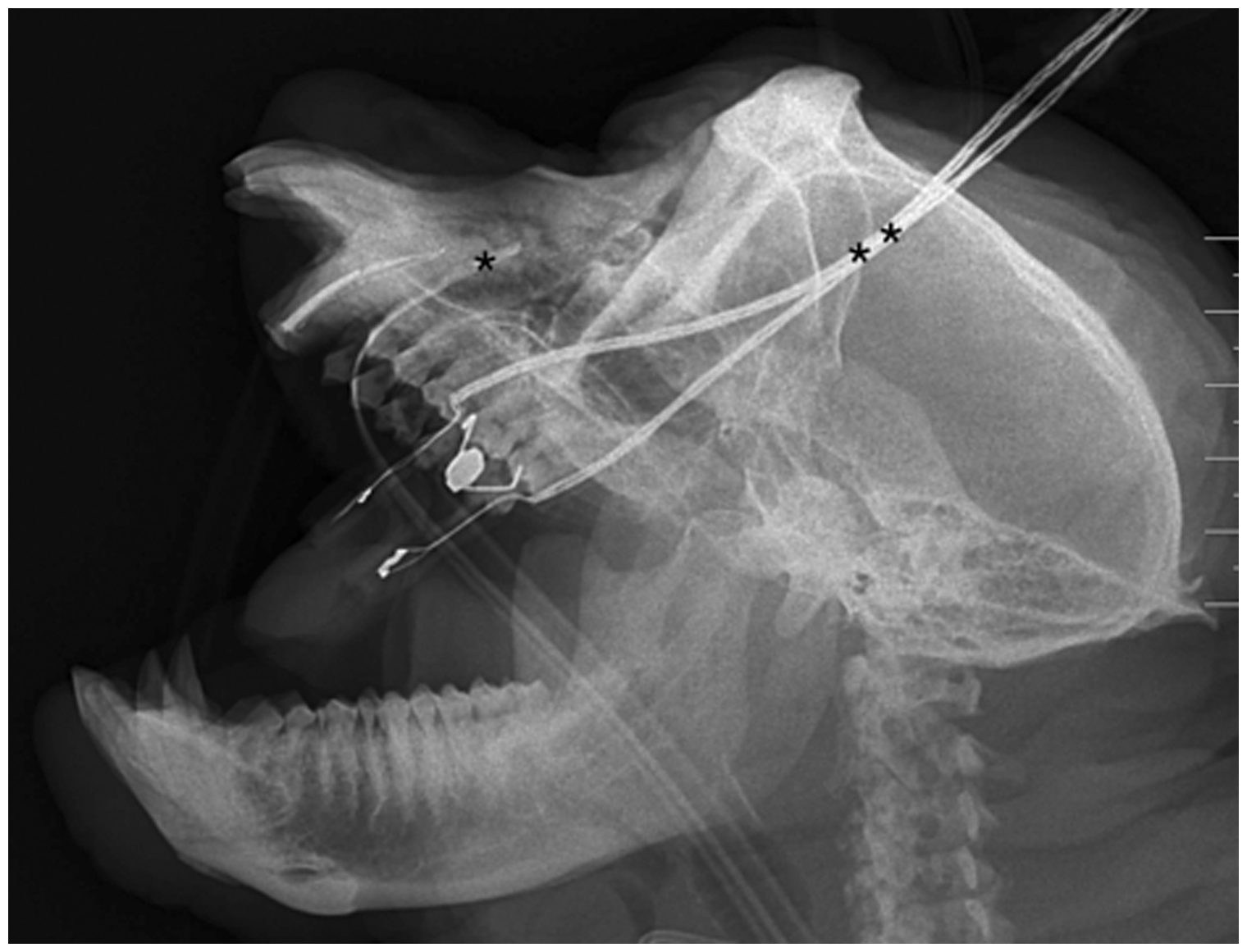
No relapse on the treated tooth occurred during the following months. However, seven months later, the monkey presented a swelling on the left suborbital area of the skull. For this reason, a prompt and accurate diagnostic, including clinical evaluation and a non-contrast-enhanced CT study, was provided under general anaesthesia to allow surgical procedures if the swelling was due to a dental root abscess. A non-contrast-enhanced CT scan of the skull was performed to assess the status of the left upper canine tooth and simultaneously evaluate follow-up of the contralateral tooth treatment. A left upper canine root abscess was diagnosed, and its treatment followed the same procedure as had been applied to the right canine tooth.
Results
Intraoral clinical examination performed before surgery revealed relevant wear and tear of canine teeth of both sides. The first contrast-enhanced CT scan confirmed the presence of periapical abscess on the right tooth, pointing out periapical alveolar bone reaction and osteolysis. No abnormalities were revealed in the other teeth or at the regional lymph nodes (mandibular and retropharyngeal).
The second non-contrast-enhanced CT scan revealed a left upper canine tooth root periapical reaction along with a moderate thickening of the mucosa in the rostral-most ipsilateral nasal cavity. The same diagnostic procedure demonstrated the efficacy of the treatment on the right tooth performed 7 months earlier and the correct positioning of the sealant (Figure 3). The successful treatment of the right canine tooth prompted application of the same techniques when a similar pathology was diagnosed in the contralateral canine.
Pre-contrast CT transverse image at the level of the plane passing through the tips of bilateral upper canine teeth roots. Asterisk shows the abscess of the left canine tooth root, whereas the long arrow indicates thickening of the ipsilateral nasal cavity mucosa. The short arrow points to the dorsal-most portion of the right upper endocanalar sealant; residual periapical bone lysis is still evident.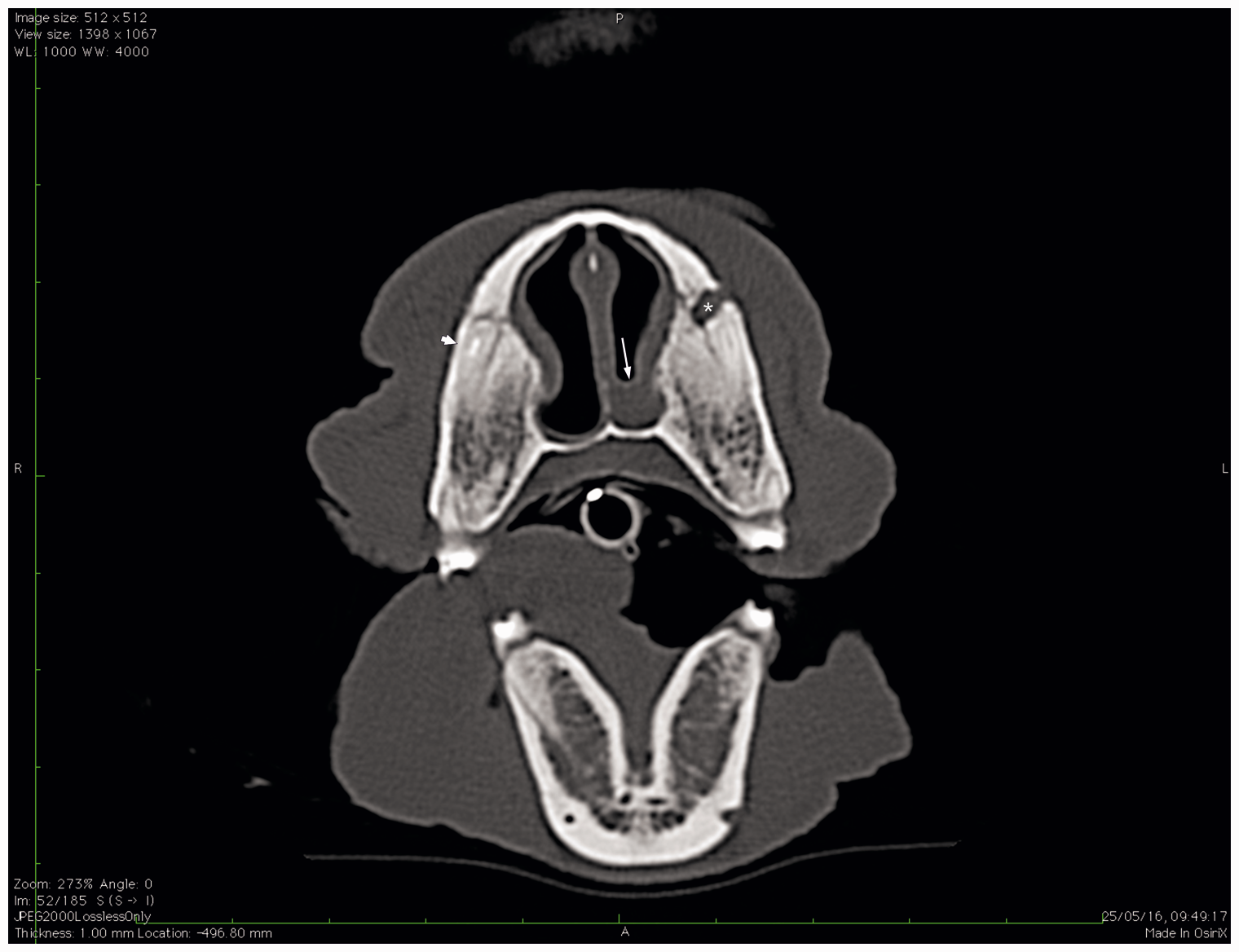
The endodontic surgical procedures allowed, in both cases, rapid healing of the infection. The macaque returned to normal eating behaviour (considering both mastication and appetite) within 24 hours after each treatment. Facial expressions became normal. Relationship with conspecifics was not influenced by the coronotomy.
Radiographic examination performed after both surgeries showed a correct positioning of the sealant. The root canals were perfectly filled for the whole of their lengths. Radiographic and CT examination are valuable diagnostic tools to be used before and after endodontic surgery. However, the use of both contrast and non-contrast-enhanced CT scans allowed a rapid and more detailed examination of bilateral abnormalities of both hard and soft tissues.
Clinical follow-up at 24 months after the first surgery highlighted the success of the treatment adopted in both teeth. In fact, body weight, fur quality, social behaviour and appetite demonstrated the animal’s good health and welfare.
Discussion
Any condition that causes exposure of the pulp cavity and/or tooth root can result in pulp necrosis. 1 Such conditions include excessive dental wear, caries, dental trauma, tooth fracture or periodontal disease. 1
In our patient, the oral clinical examination performed revealed worn teeth. This condition probably led to pulp canal exposure, bacterial contamination and abscess formation.
Radiographic examination and CT scans proved to be essential in determining which tooth was actually involved, the exact location of the lesion, and the condition of the alveolar bones. Moreover, contrast-enhanced CT examination enabled concurrent evaluation of regional lymph nodes. X-rays were also important to assess the correct positioning of the sealant and the accuracy of the treatment performed.
A few studies indicate that tooth extraction is an efficient technique for canine tooth treatment in NHPs.7,11-13 However, we considered that canine tooth extraction might be risky and too invasive for the animal’s health and welfare. For this reason, endodontics was performed instead. The use of endodontic techniques in NHPs was described by Templeton and Smith 8 and Wiggs and Hall. 9 By selecting an endodontic approach, we avoided the side effects of canine tooth extraction, including teeth drifting, 10 malocclusion, osteomyelitis, skull fracture and infection of a large open alveolus. 1 Since the pulps of both canines were non-vital, the one-step approach was replaced by a two-step surgery.
No automated rotary Ni-Ti instruments are available on the market for veterinary dentistry, thus prompting us to use automated human equipment. Unfortunately, the instrument tip for human use was not long enough to reach the canine root apexes of the macaque and perform accurate root canal treatments. For this reason, coronotomy could not have been avoided. Additionally, the rotary instrument was preferred to the manual one because its tip can bend and better adapt to the tooth root, thus avoiding root apex stripping and consequently allowing better debridement.
To the best of our knowledge, the use of iodoform paste in NHP endodontics has never been documented previously. In our patient, no adverse reaction followed the treatment despite iodoform being known to be algogenic in humans. 14 The recovery of the macaque was immediate; the subject started to eat from the day following the surgical procedures and showed no pain signs. The absence of post-operative pain is most likely due to the administration of anti-inflammatory drugs and accurate cleaning of the root canal.
Following endodontics, the canine tooth is devitalized and therefore dehydrated, thus increasing the risk of fracture. Nevertheless, the coronotomy applied reduces the risk of fracture relapse, because shortened canines are less subject to mastication stress.
Other techniques used in the past, such as crown amputation with vital pulpotomy, have shown high failure rates and a negative impact on the animal’s health and welfare. 15 In our patient, the pulp was necrotic. The clinical situation therefore prompted us to perform a total pulpectomy to properly clean the root canal. Lommer and Verstraete 15 also reported that some rhesus monkeys who underwent partial pulpectomy subsequently showed clinical (e.g. cutaneous draining and discoloured teeth) and radiographic manifestation of relapse starting at 3 months after surgery, during a follow-up period lasting 24 months. In our case, the macaque had no clinical manifestation of relapse in the 2 years that followed dental surgery. During the follow-up period, we decided to skip any X-ray examination that was not warranted by a clinical sign, thus avoiding unnecessary anaesthesia. However, a long-term CT scan may be recommended to improve the accuracy of collateral diagnostics.
Since the contralateral canine tooth, although already showing signs of wear, was not infected at the time of the first CT scan, we decided not to perform surgery on a healthy and intact tooth. Our decision was based on ethical concerns: preventive treatment of a worn canine could eventually have reduced the number of future anaesthetic procedures on the macaque, but it would also have led to devitalization and weakening of a healthy, although worn, tooth.
In fact, the choice to proceed with the amputation of the crown of the canine tooth would have eventually led to changes in social behaviour, and the root canal treatment could have caused chronic pain. Since both conditions might potentially have influenced the macaque’s welfare, thus leading to an impairment of behaviour- or nociception-focused experimental trials, we believe that the macaque should have been removed from any further experimental cohort. On the other hand, our procedure was much more conservative, painless in the short and long run, and led to no modification of social behaviour. Therefore, in our case, the decision to remove the macaque from any further experimental procedure would have been ethical but not medical, as the animal is physically fit.
In conclusion, endodontic treatment of NHP canine abscesses could preserve the affected teeth and avoid short- and long-term complications due to extraction. The techniques described here and the instrumentations proposed in this clinical case may contribute to the application of endodontics in the macaque and other NHPs, with special regard to the considerable reduction of invasive treatment and consequent significant improvement of animal welfare.
Footnotes
Acknowledgements
The authors would like to thank Mr Daniele Ramon and Mr Andrea Barzon for their invaluable contribution and technical support.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
