Abstract
Little is known about the treatment of bone pain in animal models of bone cancer. In the present study, the orthotopic 143-B human osteosarcoma xenotransplantation model was used to address the following questions: (1) Can repetitive analgesic treatment extend the experimental period by prolonging the time to reach humane endpoints and (2) Does repetitive analgesic treatment affect bone tumour development and metastasis? The analgesics, buprenorphine and meloxicam, were either applied individually or in combination at 12 h intervals as soon as the animals began to avoid using the tumour cell injected leg. While control mice treated with NaCl showed continuous body weight loss, the major criterion previously for terminating the experiments, animals treated with analgesic substances did not. The control mice had to be sacrificed 26 days after tumour cell injection, whereas the groups of animals with the different pain treatments were euthanized after an additional eight days. Importantly, primary intratibial tumour growth was not affected in any of the experimental groups by any of the pain treatment procedures. Between days 26 and 34 after tumour cell injection an increase of about 100% of the number of lung metastases was found for the groups treated with buprenorphine alone or together with meloxicam, but not for the group treated with meloxicam alone. In summary, the results indicated that both buprenorphine and meloxicam are suitable analgesics for prolonging the experimental periods in an experimental intratibial osteosarcoma mouse model.
Osteosarcoma (OS) is a primary malignant tumour of the bone. It is the most common bone tumour in children and young adults, with the lung and bone as the main sites of metastasis.1,2 Progress in combining primary tumour resection with systemic neoadjuvant chemotherapy has increased the five-year survival rate of patients over the past 30 years from 20% to 70%. 3 However, patients with metastatic disease continue to have a poor prognosis, with a five-year survival rate of only 20%. 4 Therefore, a more detailed understanding of the mechanisms in OS metastasis is of great importance in identifying novel tumour biomarkers and treatment targets for a precise diagnosis and a more specific and effective treatment, in order to finally improve the well-being and survival of OS patients.
Animal models of human cancers are very helpful for elucidating the complex mechanisms relevant for primary tumour development and metastasis that cannot be addressed in other systems. 5 Cancer promoting and cancer suppressing genes are being identified for the different stages of tumour progression as well as the mechanisms involved in dormancy and recurrence of primary tumours and metastases. 6 In addition, animal models are fundamental tools for the design and development of new diagnostic and treatment strategies in preclinical research. 7 Importantly, such animal tumour models should replicate the properties of the human disease as closely as possible. 6 Orthotopically growing tumours have therefore become more relevant compared with their subcutaneously or intraperitoneally generated counterparts because the orthotopic site offers the natural environment for the growing primary tumour.8,9
In recent studies, we used orthotopic injection of human OS cell lines into the tibia of SCID mice to investigate the functional properties of expression modified SAOS-2 (Cyr-61) and 143-B/LacZ (MMP-1) cells on OS primary tumour and metastases formation in comparison with control cells.10,11 These mice exhibited signs of significant discomfort (most often loss of more than 15% of body weight and sometimes ruffled fur) before they were euthanized. In the present study we introduced and tested different analgesic treatments in order to avoid pain-related side-effects in future studies in an attempt to refine our orthotopic tumour model and improve animal well-being. The analgesics, buprenorphine (an opioid) and meloxicam (a non-steroidal anti-inflammatory drug [NSAID]), were used alone or in combination.
Buprenorphine is a partial μ opiate agonist and, although interacting with other opioid receptors, its antinociceptive effect is primarily mediated by μ-opioid receptors. 12 The drug is now widely recognized as being extremely effective, with little of the addictive risk associated with pure μ agonists. 13 Buprenorphine has been shown to be an effective analgesic substance in mice, 14 rats, 15 humans, 16 and cancer pain in humans. 17
Meloxicam is a selective inhibitor of the cyclooxygenase-2 enzyme (COX-2) 18 and its high selectivity for COX-2 is thought to be responsible for its strong analgesic effects in rats, 19 mice, 18 and cats. 20 In addition, good gastrointestinal tolerance has been shown for meloxicam, an attribute also thought to be due to selective COX-2 inhibition. 21 Furthermore, meloxicam has been shown to be effective in ameliorating chronically painful conditions in rats, 22 mice, 23 and in humans 24 as well as bone cancer pain in rats.25,26
The aim of this study was to investigate whether analgesic treatment with meloxicam and/or buprenorphine can be used to extend the experimental time to reach humane endpoints for SCID mice which had received intratibial tumour cell injection without affecting primary tumour growth and lung metastasis.
Animals
Female 6–8-week-old immunosuppressed SCID mice (CB17/Icr-Prkdc scid/Crl) were purchased from Charles River Laboratories (Sulzfeld, Germany) and kept in individually ventilated cages (IVCs). Animal housing and experimental protocols were approved by the Cantonal Veterinary Department, Zurich, Switzerland, under licence no. 129/2009, and were in accordance with the Swiss Animal Protection Law.
Mice were housed in groups of five animals per cage for two weeks prior to tumour cell injection. Animals were kept in Eurostandard Type III clear transparent plastic (425 mm × 266 mm × 155 mm) IVCs (Tecniplast, Buguggiate, Italy) with autoclaved sawdust bedding (80–90 g per cage) and paper tissues as cage enrichment. They were fed with a pelleted and extruded mouse diet (Kliba No. 3436; Provimi Kliba, Kaiseraugst, Switzerland) ad libitum provided in a food hopper throughout the entire duration of the experiment, and had unrestricted access to sterilized drinking water. The light/dark cycle in the room was 12 h/12 h (lights off 19:00, lights on 07:00) with artificial light and a radio playing constantly at a low volume as background noise. The temperature was 21 ± 2℃, with a relative humidity of 50 ± 10%, and with 75 complete changes of filtered air per hour (HEPA H 14 filter). All manipulations were done under sterile conditions in a laminar flow hood.
Materials and methods
Cell lines and culture conditions
HEK293-T cells were purchased from the American Type Culture Collection (Rockville, MD, USA) and 143-B cells from the European Collection of Cell Cultures (Salisbury, UK). Cells were grown in Dulbecco’s modified Eagle medium (DMEM) (4.5 g/L glucose) and Ham F12 (F12) medium (1:1), supplemented with 10% fetal calf serum (FCS) (Life Technologies, Zug, Switzerland) in a humidified atmosphere of 95% air and 5% CO2 at 37℃.
Generation of modified cell line
Retroviral particles containing the lacZ gene (lacZ retrovirus) were produced in HEK293-T cells according to an optimized protocol of Mitta and coworkers. 27 Briefly, HEK293-T cells were transfected with the following three plasmids: the retroviral expression vector pQCLIN (Clontech Laboratories Inc, Mountain View, CA, USA), containing the lacZ and a neomycin resistance gene and the two helper plasmids pVSV-G (Clontech Laboratories Inc), encoding the G-glycoprotein of the vesicular stomatitis virus, and pHit60 (kindly provided by Dr Christian Buchholz, Paul-Ehrlich-Institut, Langen, Germany), coding for the retroviral gag and pol genes. Fourteen hours after transfection the medium was replaced with fresh transfection medium. The supernatant containing the respective recombinant retrovirus was collected 48 h after transfection, filtered through a 0.45 µm syringe filter, aliquoted and stored at –80℃.
Human 143-B OS cells stably transduced with the lacZ gene (143-B/LacZ) were generated with viral supernatant for 2 h in the presence of 8 µg/mL polybrene (Sigma-Aldrich, Buchs, Switzerland), and fresh cell culture medium was then added. After 48 h 143-B cells transduced with the lacZ gene were selected in cell culture medium containing 1200 µg/mL G418 (Merck Chemicals Ltd, Nottingham, UK) to select for neomycin resistant lacZ gene expressing cells.
In vivo experiments
143-B/LacZ cells were grown to subconfluency, detached with trypsin/ethylenediaminetetraacetic acid (EDTA)/phosphate-buffered saline (PBS) and prepared as a single cell suspension in PBS/0.05% EDTA at a density of 107 cells/mL. Tumour cells were intratibially injected in mice kept under general anaesthesia by intraperitoneal injection of 0.05 mg/kg fentanyl (Sintenyl; Sintetica, Mendrisio, Switzerland), 5 mg/kg midazolam (Dormicum; Roche Pharma, Basel, Switzerland), and 0.5 mg/kg medetomidine (Dorbene; Graeub Veterinary Products, Bern, Switzerland) in 0.9% NaCl. Ten microlitres of a cell suspension containing 105 cells were injected into the medullar cavity of the left proximal tibia of the mice under X-ray control with an MX-20 DC Digital Radiography System (Faxitron X-Ray Corporation, Lincolnshire, IL, USA). The injection was performed with a Hamilton syringe through an opening of the tibia plateau pre-drilled with a 26-gauge needle. After tumour cell inoculation, anaesthesia was antagonized by subcutaneous injection of 0.5 mg/kg flumazenil (Flumazenil Sintetica; Sintetica) and 2.5 mg/kg atipamezole (Alzane; Graeub Veterinary Products) in 0.9% NaCl. During anaesthesia (duration 15 to 20 min) and while recovering, mice were kept warm under a red heat lamp. To prevent the cornea from drying out, sterile eye ointment (Viscotears®; Novartis, Bern, Switzerland) was carefully applied to the eyes during all anaesthesia interventions. The health status of the mice was monitored at least three times a week.
Analgesic treatment
Pain treatment was started individually 20 to 23 days after tumour cell injection when the mice began to avoid using the leg bearing the tumour. Occurrence of lameness or hobbling was assessed during the routine health checks. After starting analgesic treatment at day 20 all mice were assessed twice a day, at the same time point when the selected analgesic substances were injected intraperitoneally (every 12 h). We used either buprenorphine (Temgesic; Reckitt-Benckiser, Wallisellen, Switzerland) at a dose of 0.1 mg/kg body weight in 100 µL per injection or meloxicam (Metacam; Boehringer Ingelheim, Basel, Switzerland) at 5 mg/kg body weight in 100 µL per injection, or a combination of the two analgesics at the same dosage as described above. The dose rates for the two analgesic substances were obtained from the recommendations in 2010 of the committee for anaesthesia, analgesia and pain prophylaxis of GV–SOLAS. Mice in the control group received 100 µL 0.9% sterile NaCl solution by intraperitoneal injection. Mice were housed in groups of five animals per cage during the experiment. The animals were randomly selected in individual cages so that at least one mouse in each cage received one of the described analgesic treatments. Analgesia was applied until the animals were sacrificed (at 4 to 13 days).
Measurements
To assess the animals’ condition, clinical and behavioural signs that might indicate pain, discomfort or reduced general health condition were recorded once a week and twice a day after the start of analgesic treatment. According to our routinely used scoring system 28 abnormalities of body condition (e.g. sunken flanks or closed eyes), fur condition (e.g. ruffled coat), breathing (e.g. irregular) and posture (e.g. hunched back) were registered, and spontaneous behaviour and movement after manipulation or contact were assessed. The body weight of the mice was determined using a laboratory balance at least once a week and after the start of analgesic treatment every other day.
The endpoint criteria for removing the mice before finishing the study were listed on the score sheets and were approved by the Cantonal Veterinary Department, Zurich, Switzerland. If one of the endpoint criteria was observed the mouse had to be sacrificed. For our experiments we had the following endpoint criteria: (1) weight loss >15% from the initial weight; (2) ruffled fur, hunched back, closed eyes for more than one day; (3) immobilization/disability because of tumour size; (4) breathing difficulties; (5) no contact reactions; (6) no palm gripping reflex; (7) signs of infection.
During X-ray analysis and tumour volume measurements mice were kept under general anaesthesia by intraperitoneal injection of 5 mg/kg midazolam and 0.5 mg/kg medetomidine in 0.9% NaCl. Tumour growth and osteolysis were monitored by X-ray analysis once a week with a Faxitron® MX-20 Specimen Radiography System. The tumour volume (V) was calculated from the weekly measurements using a caliper rule with two perpendicular diameters of the tumour and the control leg according to the following formula: V = 0.5 × L × (S)2 (where L and S were the largest and smallest perpendicular tumour diameters, respectively); Tumour volume = Volume of injected leg – Volume of control leg. After the measurements anaesthesia was antagonized by subcutaneous injection of 0.5 mg/kg flumazenil and 2.5 mg/kg atipamezol in 0.9% NaCl.
Mouse lungs were prepared at sacrifice as described. 29 In brief, mice were anaesthetized with 112.5 mg/kg ketamine (Narketan 10; Vétoquinol AG, Bern, Switzerland), 16.5 mg/kg xylazine (Xylazin; Streuli Pharma AG, Uznach, Switzerland), and 15 mg/kg acepromazine (Prequilan; Fatro SpA, Ozzano Emilia, Italy) before the chest and the abdomen of the mice were opened. Blood was removed from the lung and the liver by perfusion with PBS that was injected into the right ventricle of the beating heart, after sectioning the vena cava intraabdominally. The lungs were then fixed under inflation for 10 min with 3% paraformaldehyde (PFA) injected into the right ventricle and into the trachea with subsequent pinch-off. PFA was then replaced by injection of PBS into the right ventricle and into the trachea. The left lobe of the lung was processed for X-gal staining as described in the next section.
Visualization of LacZ-transduced metastatic tumour cells in the lung
Mouse lungs were fixed with 2% formaldehyde in PBS at room temperature for 30 min, washed three times with PBS and stained at 37℃ for at least 3 h in 5-bromo-4-chloro-3-indolyl-β-D-galactoside staining solution (X-gal; Enzo Life Sciences, Lausen, Switzerland) as described. 29 For the quantification of the metastases, images of the surface of one lung lobe of each mouse were taken under a Nikon Eclipse E600 microscope with a Kappa PS 20 C digital camera (Kappa optronics GmbH, Gleichen, Germany) and imported as TIF files into Power Point© software. Indigo-blue stained foci on lung surfaces were counted as described recently. 11
Statistical analyses
The mice treated with analgesic substances were divided into two groups. At the time of euthanasia of the control mice (n = 10, treated with 0.9% NaCl) at day 26 after tumour cell injection, five mice from the experimental groups undergoing analgesic treatment were also euthanized to compare the influence of the substances on lung metastasis. The remaining animals (buprenorphine: n = 4; meloxicam: n = 6; buprenorphine and meloxicam: n = 5) were euthanized on day 34 after tumour cell injection to compare the effects of the analgesics after a prolonged time period.
Power analysis was performed using G*Power 3.1.9.2 software. 31 Statistical analyses were performed using SPSS 20.0 software (IBM, Armonk, NY, USA). All data were tested for normal distribution. Mann–Whitney U-test was performed for percentages of body weight on injection day, tumour volumes and numbers of metastases (all groups at days 25, 23 or 26, respectively; analgesic treatment groups without NaCl group at day 34); post hoc testing was conducted with the Bonferroni test. P values < 0.05 were considered as significant.
Results
Analgesic effects of buprenorphine and meloxicam in the orthotopic 143-B OS tumour model
Forty-four SCID mice had human OS 143-B/LacZ cells injected into the proximal left tibia to investigate the effects of analgesic treatment by buprenorphine and meloxicam on primary tumour growth, lung metastasis and survival in our orthotopic OS tumour model. Three mice had to be euthanized within two days after tumour cell injection, one mouse from each of the three drug treatment groups. These animals became immobile and moribund unexpectedly early without any tumour growth, and were therefore not included in this study. One mouse of the group treated with meloxicam was excluded as an outlier, because the number of metastases was more than 10-fold higher than the mean value of the metastases for the mice of this group.
Analgesic treatment was initiated individually when the mice began to avoid using the tumour cell injected leg (lameness) between days 20 and 23 after tumour cell inoculation. After initiation of the analgesic treatment no lameness was observed in the mice. At this time point only 7 of 41 animals showed additional signs of discomfort, in most cases slightly reduced activity. The animals of the control group, treated with 0.9% NaCl solution, were euthanized 26 days after tumour cell injection because of progressive decrease in body weight between days 21 and 25 (Figure 1a) and indicative signs of pain such as ruffled fur and hunched back which were predefined humane endpoint criteria in this study. Even though the percentages of body weight on injection day did not show a statistical significant difference compared with the control group, no weight reduction or other humane endpoint criteria were observed in any of the animal groups receiving analgesic treatment (Figure 1a). Thirty-four days after tumour cell injection, the remaining mice in all groups were euthanized because ruffled fur, hunched back or closed eyes that might have been indicative of pain were observed despite analgesic treatment, or because of the large tumour size which strongly inhibited the mobility of the mice. However, the mean values of body weight for all three analgesic treatment groups were above the values measured on the day of tumour cell injection. For the group treated with meloxicam, the mean body weight was 106.3 ± 0.7%, for the buprenorphine group 101.5 ± 1.3%, and for the animals treated with both meloxicam and buprenorphine 104.1 ± 1.8% (Figure 1b) of the body weight measured at the time of tumour cell injection. It was noticeable that the body weight growth chart of female SCID mice from Charles River also showed only a near stable plateau during the experimental period between 8 and 13 weeks. No significant differences in percentages of body weight on injection day between the different analgesic treatment groups were observed. Only 3 out of 15 mice from the three analgesic treatment groups had lower body weights than those measured on the day of tumour cell injection.
Changes in body weight over time in mice treated with saline or with the indicated analgesics. The development of body weight of vehicle- and analgesic-treated mice until day 26 (a) or of those mice in the analgesic groups which were kept until day 34 (b). Data are shown in percentages of the weight of the animals measured on the day of tumour cell injection. The data are presented as mean ± SEM for each group of animals receiving a specific analgesic treatment. The mice were treated with 0.9% NaCl (NaCl), meloxicam (Me), buprenorphine (Bu) or meloxicam and buprenorphine (Me + Bu).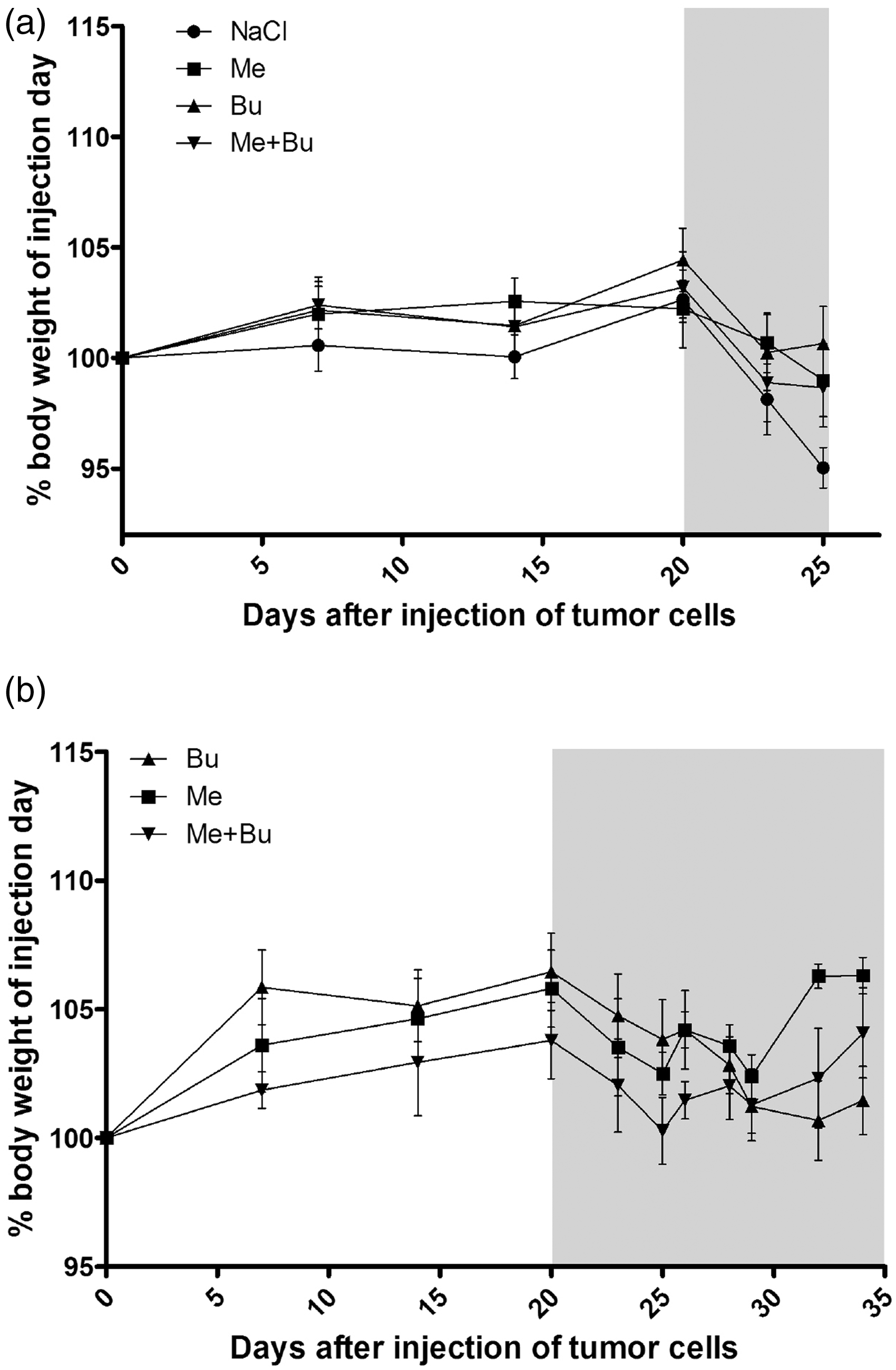
Effects of buprenorphine and meloxicam on primary tumour growth and lung metastasis
Analgesic treatment of the mice did not influence the growth of the primary tumour in the proximal tibia when compared with the control group treated with 0.9% NaCl solution (Figure 2a). Twenty-six days after tumour cell inoculation the mean tumour volumes in the different groups of mice were between 97 ± 22 mm3 and 120 ± 18 mm3. After prolonged analgesic treatments of the mice we did not observe any differences in primary tumour growth between the three drug treatment procedures. The mean volume of the primary tumour 34 days after tumour cell injection was 397 ± 41 mm3 in the group treated with meloxicam, 412 ± 116 mm3 in the group treated with buprenorphine, and 365 ± 99 mm3 in the group treated with both meloxicam and buprenorphine (Figure 2b). The serially taken X-ray images confirmed the caliper measurements. No differences were observed for the primary tumour volume (day 23 P = 0.774, day 34 P = 0.928) or for the osteolytic lesions (Figures 3a–c).
Primary tumour growth in the absence or presence of analgesic treatment. Primary tumour volume was measured at indicated time points as described in Materials and methods. (a) Shows the increase in tumour volume during the first 26 days in all mice investigated. (b) Shows the tumour growth in the groups of mice that were euthanized after 34 days. The data are presented as mean ± SEM for each individual group of animals receiving a specific analgesic treatment. The mice were treated with 0.9% NaCl (NaCl), meloxicam (Me), buprenorphine (Bu) or meloxicam and buprenorphine (Me + Bu). The grey shaded areas indicate the time period of pain treatment. X-ray monitoring of primary tumour growth and tibia osteolysis. X-ray images taken at indicated days after tumour cell injection of representative mice treated with meloxicam (a), buprenorphine (b) or meloxicam and buprenorphine (c) are shown.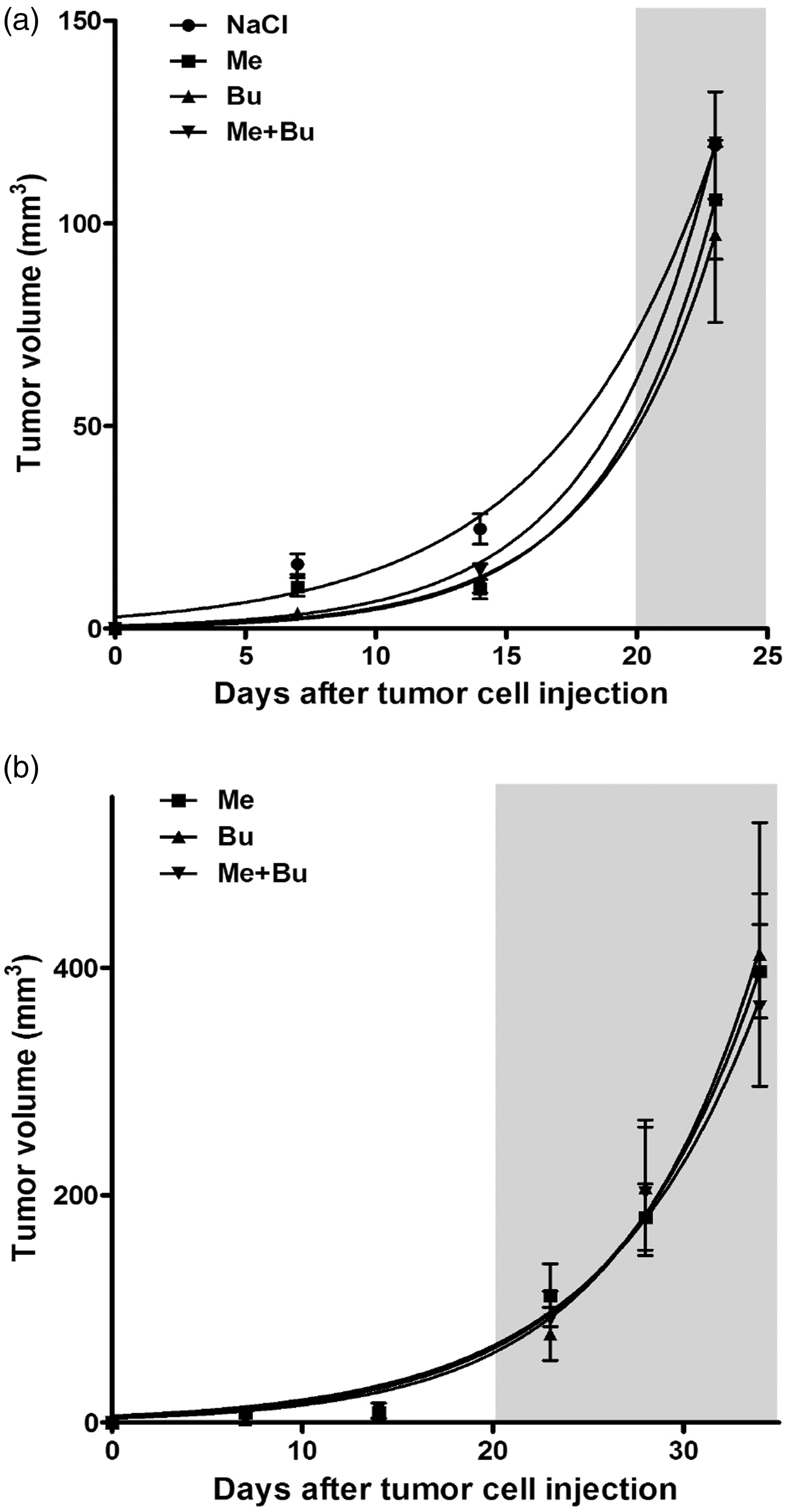

The second important quantitatively measurable effect for this established OS tumour model was the number of metastases made visible after euthanasia of the mice by X-gal staining on lung surfaces and after being counted. In the present study the number of lung metastases 26 days after tumour cell injection was similar for both the control group (222 ± 34) and the group treated with buprenorphine (215 ± 32) (Figure 4a). Interestingly, for the mice treated with either meloxicam alone (109 ± 36) or with meloxicam and buprenorphine together (138 ± 33) a lower number of metastases was found than in the other animal groups (Figures 4a and b). The number of lung metastases increased between day 26 and day 34 after tumour cell injection in the group of mice treated with either buprenorphine alone (431 ± 181) or with buprenorphine and meloxicam (333 ± 49), which is a doubling of the number of metastases within eight days. However, in the group treated with meloxicam alone (122 ± 42) the number of lung metastases only slightly increased during this time period (Figures 4a and b). Nevertheless, differences between groups were not significant (day 26 P = 0.086, day 34 P = 0.082).
Quantification of lung metastases in mice treated with saline or different analgesics. (a) The total numbers of metastases per lung were quantified by counting the indigo-blue stained spots on the lung surface from mice euthanized after 26 or 34 days. The bars represent the mean value ± SEM of the number of metastases per lung in the different groups of mice. (b) Representative images show X-gal stained lung metastases from the different groups of mice. Images in the top row were taken from lungs of animals euthanized after 26 days and images in the bottom row from animals euthanized after 34 days. Animals were treated with saline without analgesic (NaCl, control), with meloxicam (Me), buprenorphine (Bu), or with meloxicam and buprenorphine together (Me + Bu). Bar: 1 mm.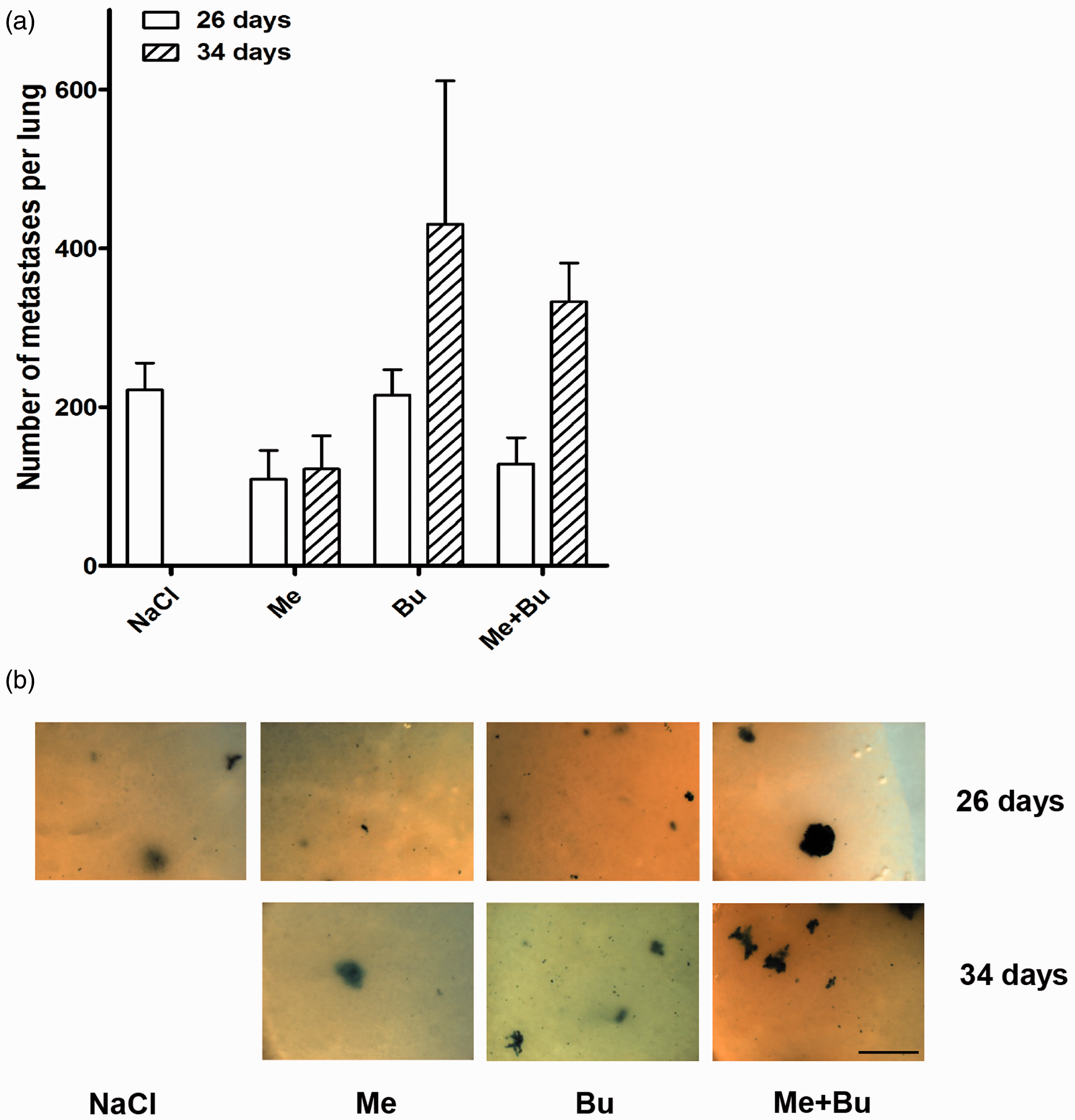
Discussion
Ethical concerns as well as animal welfare regulations both require the use of appropriate analgesics for procedures that may cause discomfort or pain to a laboratory animal. The present study compared the analgesic and tumour model interfering effects of buprenorphine and meloxicam when used as analgesics in an intratibial human xenograft OS model. The purpose of these experiments was to determine (1) whether meloxicam or buprenorphine or a combination of both can influence the general condition of the animals or prolong the time period to reach humane endpoint criteria during the experiment, and (2) whether these analgesics influence intratibial primary tumour growth and/or lung metastasis in our established OS model with SCID mice.
Pain is a common and unbearable symptom of cancer in humans and animal tumour models that often influence the general condition of both. Tumour growth is often accompanied by compression of peripheral nerves as well as by the release of inflammatory and tumorigenic components. These factors contribute to the generation of both chronic and movement-evoked pain. 30 Bone cancer pain has a complex nature, and due to its multifactor origin it is difficult to manage. 32
One main observation in the present study was that for the animals receiving analgesic treatment the time period until they reached one of the humane endpoint criteria was longer in comparison to that of the saline controls, which suggests that all three analgesic procedures tested were effective in alleviating the discomfort of the animals. The time period from tumour cell injection to euthanasia, which was 26 days for the control group treated with 0.9% NaCl, increased by one week to 34 days for the groups treated with analgesia until one of the predefined humane endpoints was fulfilled. Consequently, the prolonged period of survival of analgesia-treated animals after tumour cell injection improves the quality of the experiments, because primary tumour formation and, more importantly, lung metastasis can be analysed in more detail and over a longer period of time. Interestingly, in a syngeneic mouse lymphoma model a beneficial, discomfort-relieving effect of buprenorphine for the animals was not observed. 33 The distinct tumour models (syngeneic lymphoma versus orthotopic OS) and different methods of application of buprenorphine (application as food gel or intraperitoneal injection) could be the reasons for these contrary results.
In this study, saline-injected controls lost body weight, which was predefined as a major criterion for the termination of the experiment if the loss reached 15%. The loss of body weight was probably due to pain caused by progressive tumour growth and avoidance of using the tumour-bearing leg. Guarding of the affected limb, resulting in changes to weight bearing and gait, is a known sign of pain,34,35 and in our study may have led to a reduction in performance of behaviours that require straighten up like eating and drinking. Therefore, in our OS animal model, loss of body weight is an important indicator of tumour-induced discomfort and pain for saline-treated animals, whereas for the analgesic-treated mice other humane endpoint criteria like ruffled fur and hunched back were relevant.
A second important observation was that none of the three analgesic treatment procedures influenced primary tumour growth in the tibia in comparison to the saline control. In addition, after prolonged analgesic treatment (days 26–34) primary tumour growth was very similar for the three different groups. To our knowledge the influence of buprenorphine on tumour growth has not been analysed until now. On the other hand, meloxicam-dependent inhibition of primary tumor growth has been described for different tumour types. For hepatocellular carcinoma meloxicam-dependent inhibition of primary tumour growth has been shown in two different subcutaneous in vivo systems.36,37 In an ovarian cancer system, where OVCAR-3 cells were subcutaneously inoculated into nude mice, meloxicam use alone suppressed primary tumour growth and prolonged the survival of the mice with intraperitoneal DISS tumours in comparison to a control group. 38 Interestingly, Naruse and coworkers found a significant inhibition of primary tumour formation for OS. 39 However, they transplanted the mouse LM8 OS tumour cells subcutaneously rather than orthotopically and effectively applied meloxicam once, at a high dose (40 mg/kg). Whether repetitive meloxicam treatment is more effective than a single administration remains to be investigated. It is noteworthy that meloxicam inhibited primary tumour growth only when the tumour cells were inoculated subcutaneously, and not orthotopically as was done in this study. This suggests that, at least for meloxicam, the location of tumour cell inoculation may influence the anti-tumour activity of the drug in in vivo cancer models.
In conclusion, the use of buprenorphine or meloxicam has improved the quality of our in vivo experiments by enabling us to monitor tumour progression and metastasis over a longer time period. Both analgesics markedly delayed occurrence of signs of reduced animal well-being, especially pain-related body weight-loss of the mice, and avoided early termination of the experiment due to this endpoint criterion. However, the prolonged use of meloxicam revealed an anti-metastatic effect in our OS tumour model, and similar results have been described in the literature for other tumour types.36,40 Consequently, the use of meloxicam as an analgesia in cancer studies may be used with caution, but conversely its promising potential of influencing OS lung metastases formation has to be further investigated.
Footnotes
Acknowledgements
The authors thank Dr Emanuel E Strehler (Department of Biochemistry and Molecular Biology, Mayo Clinic College of Medicine, Rochester, USA) for critical reading of this manuscript.
Conflict of interest
None declared.
Funding
This study was supported by the Swiss National Science Foundation SNF, the Schweizerischer Verein Balgrist, the University of Zurich, the Krebsliga Zurich, a grant from the Walter L and Johanna Wolf Foundation, Zurich, Switzerland, and the HSM program for Muskuloskeletal Oncology of the Kanton Zurich.
