Abstract
Compared with other members of the dendritic cell family, the antigen profile of the recently recognized vascular dendritic cells has received limited attention. This study demonstrates that vascular dendritic cells in the human aorta and carotid arteries express 55-kD actin-bundling protein (p55), a specific marker for blood dendritic cells and Langerhans cells. This finding will facilitate screening of dendritic cells during their isolation from the arterial wall, as well as other investigations.
Keywords
DENDRITIC CELLS are specialized antigen-presenting cells with a powerful capacity for initiating T-cell responses (Ricciardi-Castagnoli 1997; Banchereau and Steinman 1998). Earlier we reported that cells from the dendritic cell family reside in the arterial wall (Bobryshev and Lord 1995). These vascular dendritic cells are present in their immature form in the intima and adventitia of apparently normal nondiseased arteries and become activated during atherogenesis (Bobryshev and Lord 1995; Bobryshev et al. 1997a).
In the normal intima, dendritic cells have been proposed to be an element of vascular associated lymphoid tissue (VALT), which is probably analogous to the mucosa-associated lymphoid tissue (MALT) of the respiratory and gastrointestinal tracts (Wick et al. 1997). VALT consists of small numbers of immunocompetent and antigen-presenting cells disseminated throughout the subendothelial layer of the arterial intima (Wick et al. 1997; Waltner-Romen et al. 1998). VALT probably screens vascular tissue for potentially harmful antigens (Wick et al. 1997).
In atherosclerotic intima, the numbers of dendritic cells increase (Bobryshev and Lord 1995; Bobryshev et al. 1997a), with only a few dendritic cells transforming into foam cells (Bobryshev and Watanabe 1997). The functional significance of vascular dendritic cells in atherosclerosis is unknown, although it is most likely that vascular dendritic cells are involved in antigen processing and presentation, like dendritic cells in other tissues (Ricciardi-Castagnoli 1997; Steinman et al. 1997; Banchereau and Steinman 1998).
Unambiguous ultrastructural criteria are defined for identifying dendritic cells in the arterial wall (Bobryshev and Lord 1995; Bobryshev and Watanabe 1997; Bobryshev et al. 1997a,b). The tubulovesicular system and dense granules (Figures 1A-1C) are both unique to dendritic cells (Takahashi et al. 1996; Ricciardi-Castagnoli 1997; Steinman et al. 1997). Some of these dense granules transform to structures resembling Birbeck granules present in Langerhans cells (Figures 1B and 1C) (Bobryshev et al. 1997a). Both Birbeck granules present in Langerhans cells and Birbeck granule-like structures present in vascular dendritic cells are rod-shaped structures with a lamina through their center (Birbeck et al. 1961; Bobryshev et al. 1997a). However, in Birbeck granules present in Langerhans cells, the central lamina is intermittent (Birbeck et al. 1961), whereas in Birbeck granule-like structures present in vascular dendritic cells, the central lamina is continuous (Figure 1C) (Bobryshev et al. 1997a). In dendritic cells, the tubulovesicular system and Birbeck granules are cytoplasmic organelles involved in antigen processing and presentation (Hanau et al. 1987; Ricciardi-Castagnoli 1997). Ultrastructural peculiarities of the tubulovesicular system and dense granules (Bobryshev and Lord 1995; Bobryshev and Watanabe 1997; Bobryshev et al. 1997a,b) suggest that vascular dendritic cells represent a separate cell type within the dendritic cell family.
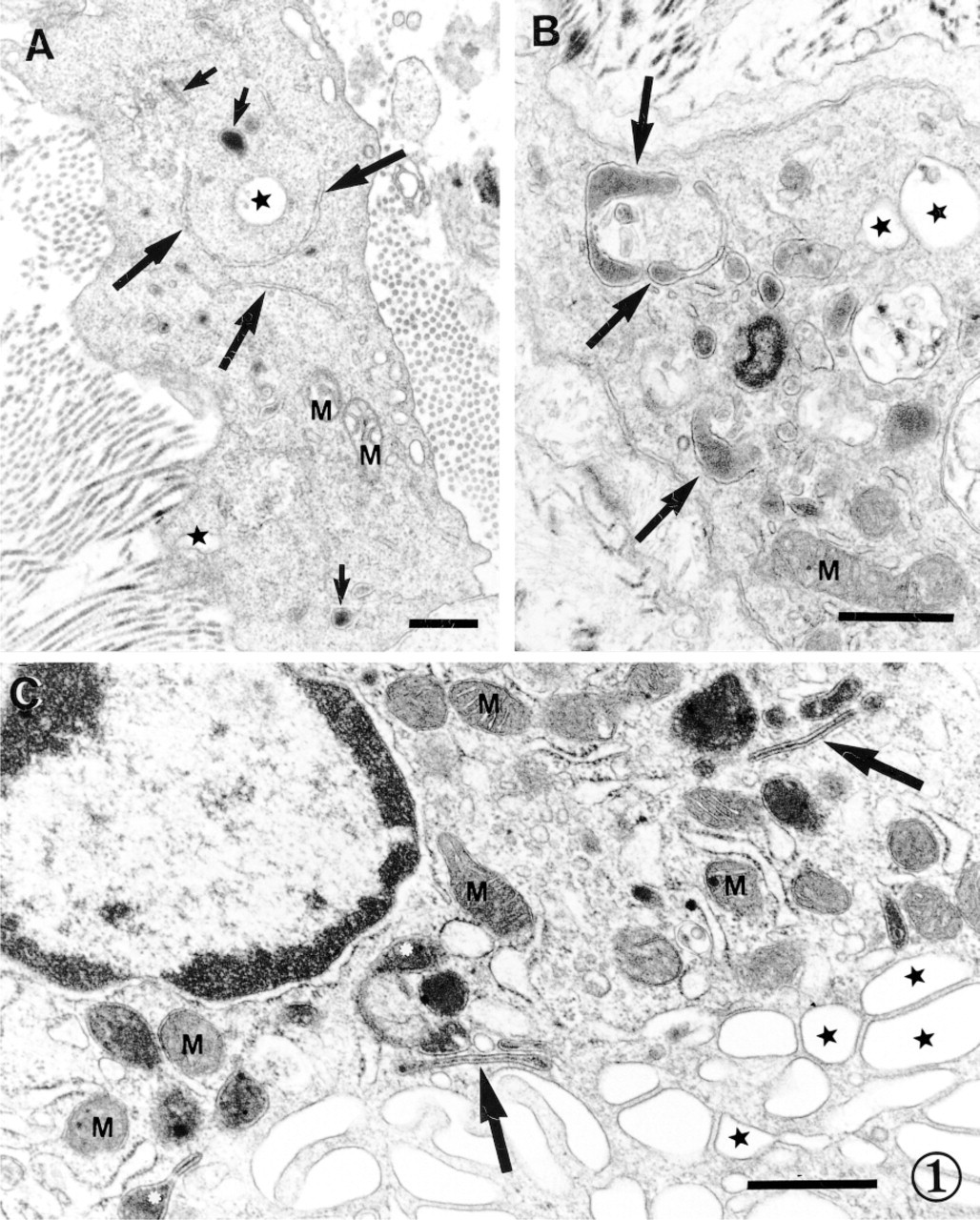
Ultrastructural criteria for identifying dendritic cells in the wall of human aorta. (A) Typical appearance of cisternae of the tubulovesicular system (large arrows). Dense granules are shown by small arrows. (B) Atypical dense granules (arrows). (C) Birbeck granule-like structures (arrows) and atypical dense granules transforming to Birbeck granule-like structures (asterisks). Caveolae are marked by stars. M, mitochondria. Bars = 0.5 μm.
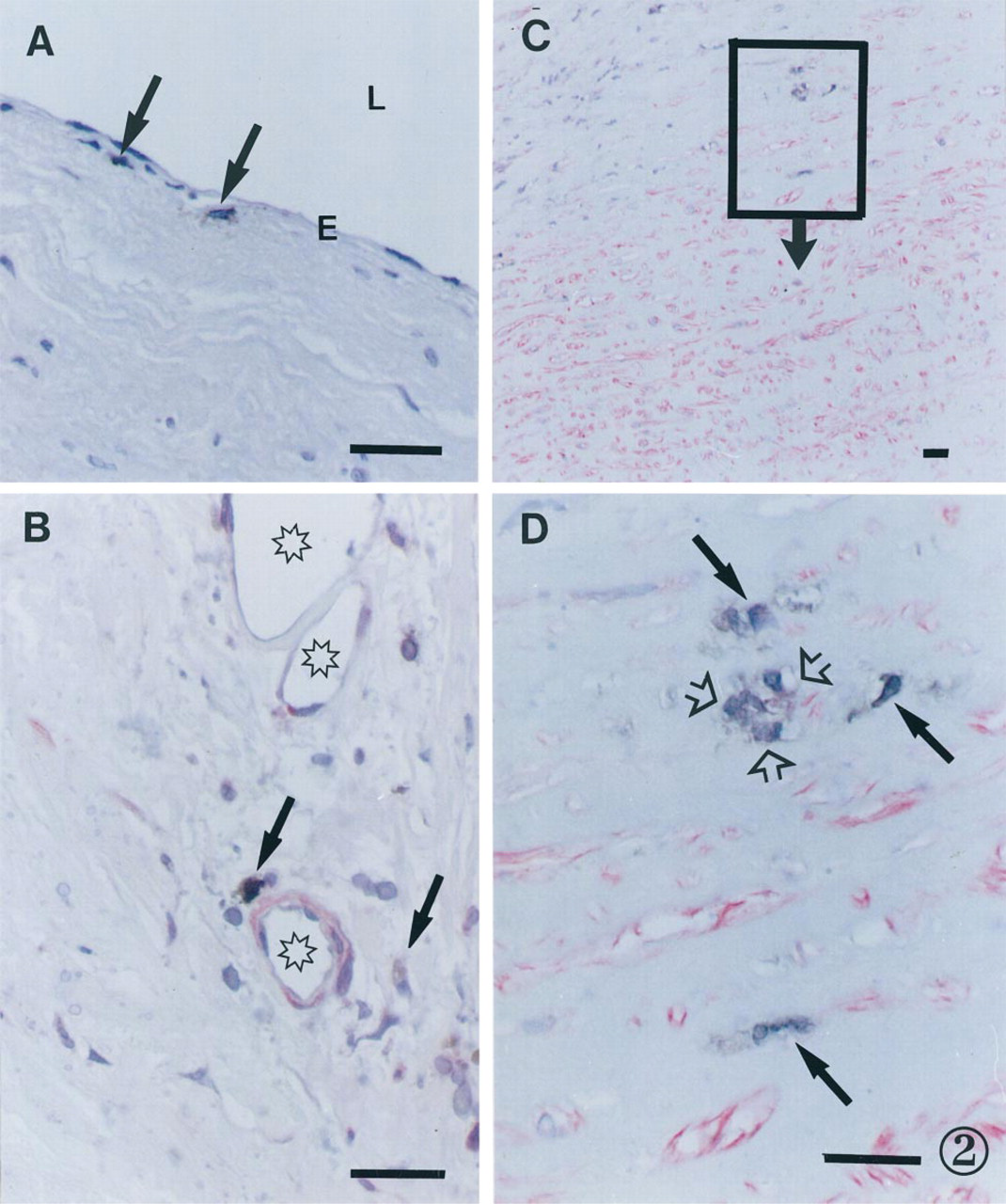
Patterns of distribution of p55+ cells in the arterial wall. (A) p55+ cells (arrows) in nondiseased aortic intima. p55+ cells were visualized by the ABC immunoperoxidase technique. E, endothelium; L, lumen of the aorta. (B) p55+ cells (arrows) in a neovascularization area in an atherosclerotic plaque in a carotid artery. Microvessels are marked by asterisks. (C) p55+ cells in the deep portion of aortic atherosclerotic intima on the border with the media. (D) Detail of C. A cluster of p55+ cells is shown by open arrows; separately located p55+ cells are shown by solid arrows. (B-D) Double immunostaining resulting in brown staining of p55+ cells (PAP technique) and rose staining of α-smooth muscle actin-positive cells (APPAP technique). Counterstaining with Mayer's hematoxylin. Bars = 100 μm.
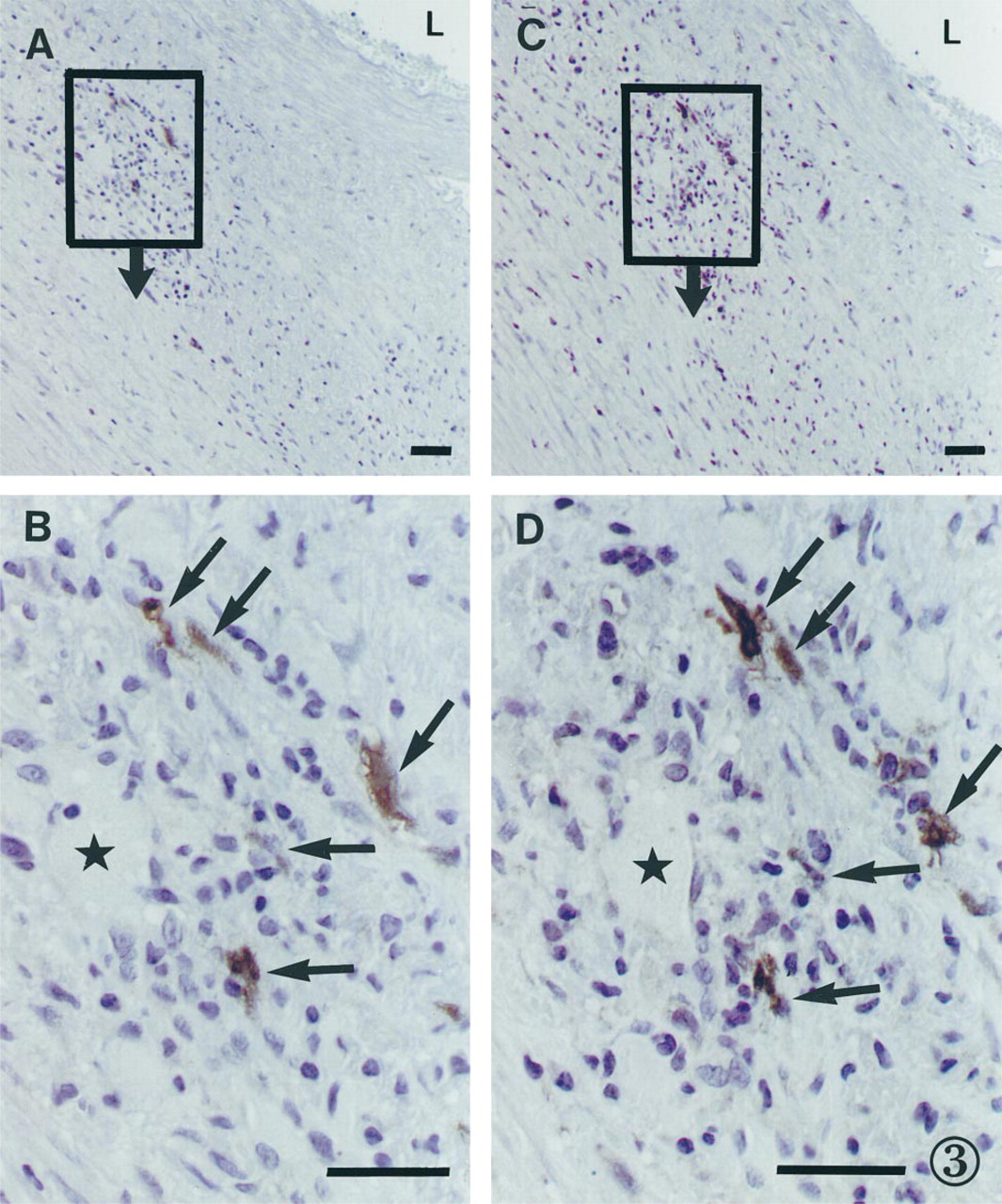
A group of p55+ (A)/CD1a+ cells (C) in an area of neovascularization in an aortic atherosclerotic plaque seen in consecutive sections. L, lumen of the aorta. (B) Detail of A. (D) Detail of C. (B,D) p55+/CD1a+ cells are shown by arrows and a microvessel is marked by stars. ABC immunoperoxidase technique. Counterstaining with Mayer's hematoxylin. Bar = 100 μm.
Unlike the ultrastructural characteristics, thus far the antigen profile of vascular dendritic cells has been poorly studied. Vascular dendritic cells express CD1a (Bobryshev and Lord 1995,1998), S-100 protein (Bobryshev and Lord 1995,1998; Bobryshev and Watanabe 1997), and Lag-antigen (Bobryshev et al. 1997a), which are markers for their immunohistochemical identification in the arterial wall. At present, CD1a is the most reliable marker for identifying vascular dendritic cells in the arterial wall because CD1a expression is restricted to thymocytes and dendritic cells (Ricciardi-Castagnoli 1997). S-100 antigen is expressed by a variety of cell types, including glial cells, Schwann cells, and ependyma, but none of these are present in the intima, making S-100 a convenient marker for dendritic cells in this location (Bobryshev and Lord 1995, 1998). Lag-antigen is specifically expressed by vascular dendritic cells but its expression is restricted to only a small proportion of these cells (Bobryshev et al. 1997a).
Vascular dendritic cells also express HLA-DR (Bobryshev and Lord 1998), E-cadherin (Bobryshev et al. 1998), intercellular cell adhesion molecule-1 (ICAM-1) (Bobryshev and Lord 1998), vascular cell adhesion molecule-1 (VCAM-1) (Bobryshev and Lord 1998), and CD40 (unpublished data), but these molecules are widely expressed by different cell types in atherosclerotic lesions. These plasmalemmal markers will probably be useful for isolation of vascular dendritic cells from the arterial wall but do not allow specific immunohistochemical identification.
The 55-kD actin-bundling protein (p55) was recently shown to be expressed specifically by dendritic cells (Mosialos et al. 1996). Actin-bundling proteins regulate cytoskeletal rearrangements and the interaction between the cytoskeleton and membranes in response to extra- or intracellular signals (Stossel 1993). Actin-bundling proteins direct the three-dimensional polymerization of actin filaments in migrating cells (Stossel 1993). Related to cell motility is also the ability to process and present antigen (Stossel 1993). p55 is now widely used for detecting different types of dendritic cells (Ricciardi-Castagnoli 1997; Steinman et al. 1997).
To determine whether vascular dendritic cells express p55, we examined aortic and carotid artery specimens collected as previously reported (Bobryshev and Lord 1998). For immunohistochemical examination, the unfixed specimens were immediately embedded in OCT compound, rapidly frozen in liquid nitrogen, and stored at −70C until cryostat sectioning. For the present study, frozen sections were obtained from seven aortic arteries and seven carotid arteries containing both atherosclerotic lesions and adjacent normal-appearing arterial wall. Consecutive sections were stained with antibodies to p55 (ascites fluid obtained by IP injection of the K-2 hybridoma into BALB/c mice (Mosialos et al. 1996; a gift of Professor Langhoff; diluted 1:500), anti-CD1a (Dako, Glostrup, Denmark; 1:50), S-100 (Dako; 1:700), E-cadherin (Transduction Laboratories, Lexington, KY; 1:50), CD68 (Dako; 1:50), CD3 (Dako; 1:100), α-smooth muscle actin (Dako; 1:25) and von Willebrand factor (Dacle Behring, Gladesville, Australia; 1:500) using the avidin-biotin (ABC) immunoperoxidase method as previously described (Bobryshev and Lord 1995, 1998). Double immunostaining included a combination of peroxidase-anti-peroxidase (PAP) and alkaline phosphatase-anti-alkaline phosphatase (APAAP) techniques (Bobryshev and Lord 1998).
Immunohistochemical examination demonstrated the presence of p55+ cells in the nondiseased intima as well as in atherosclerotic lesions in both the aorta and the carotid artery. In the nondiseased intima, p55+ cells were mostly located in the subendothelial layer (Figure 2A), whereas in atherosclerotic lesions p55+ cells were distributed irregularly throughout and often formed cell clusters (Figures 2B-2D, 3A-3D). In atherosclerotic plaques, p55+ cells located most frequently in areas of neovascularisation (Figures 2B, 3A-3D). p55+ cells were also present around vasa vasorum in the adventitia in both the nondiseased and the diseased segments of the arterial wall. Comparing consecutive sections stained with different antibodies demonstrated that p55+ cells were negative for CD3, CD68, α-smooth muscle actin, and von Willebrand factor but were consistently positive for CD1a (Figures 3A-3D), S-100, and E-cadherin.
The present observations demonstrate that, in the arterial wall, 55-kD actin-bundling protein (p55) is expressed by dendritic cells and that its expression is restricted to dendritic cells. This finding will assist in further investigation of vascular dendritic cells, particularly, in screening dendritic cells during their isolation from the arterial wall.
In contrast to all other cell types populating the arterial wall, vascular dendritic cells appear to be the only cell type restricted to the arterial tissue. Isolation of vascular dendritic cells might allow the identification of a unique antigen(s) on their surface and thus ultimately lead to new strategies for the target delivery of biologically active substances to atherosclerotic lesions.
Footnotes
Acknowledgements
Supported by the St. Vincent's Clinic Foundation, Sydney. We thank Professor E. Langhoff (Department of Medicine/Nephrology, Pennsylvania State University, Hershey) for the kind gift of anti-p55 antibody.
