Abstract
Tumor cell-derived collagenase stimulatory factor (TCSF) stimulates in vitro the biosynthesis of various matrix metalloproteinases involved in tumor invasion, such as interstitial collagenase, gelatinase A, and stromelysin 1. The expression of TCSF mRNAs was studied in vivo, using in situ hybridization and Northern blotting analysis, in seven normal tissues and in 22 squamous cell carcinomas of the lung, and in seven benign proliferations and in 22 ductal carcinomas of the mammary gland. By in situ hybridization, TCSF mRNAs were detected in 40 of 44 carcinomas, in pre-invasive and invasive cancer cells of both lung and breast cancers. TCSF mRNAs and gelatinase A mRNAs were both visualized in the same areas in serial sections in breast cancers, and were expressed by different cells, tumor cells, and fibroblasts. The histological results were confirmed by Northern blot analysis, which showed a higher expression of TCSF mRNAs in cancers than in benign and normal tissues. These observations support the hypothesis that TCSF is an important factor in lung and breast tumor progression.
T
The specific detection of MMPs in peritumoral fibroblasts has led to the hypothesis that tumor cells might induce the synthesis of these enzymes implicated in cancer dissemination. In agreement with such an idea, several investigators have demonstrated cooperation between tumor cells and fibroblasts in vitro in the regulation of several MMPs, such as interstitial collagenase (Noël et al. 1993; Hernandez et al. 1985; Biswas 1984,1985; Bauer et al. 1979) and gelatinase A (Ito et al. 1995; Noël et al. 1994). Furthermore, a tumor cell-derived collagenase stimulatory factor (TCSF) also present in tumor cell-conditioned media, was isolated and purified from the plasma membranes of a human lung carcinoma cell line (Ellis et al. 1989). This factor is a glycoprotein of 58 kD and was recently identified as a member of the immunoglobulin super-family (Biswas et al. 1995). In addition to enhancing interstitial collagenase synthesis (Nabeshima et al. 1991), purified TCSF stimulates gelatinase A and stromelysin 1 expression by fibroblasts (Kataoka et al. 1993). Immunohistochemical studies employing a monoclonal antibody directed against TCSF have shown that TCSF is localized to the outer surface of cultured lung cancer cell lines (Ellis et al. 1989). The same distribution was seen in tumors of urinary bladder, in which TCSF was detected at the periphery of cancer cells but not in surrounding stromal cells (Muraoka et al. 1993). Furthermore, TCSF was also localized in tumor cells by immunohistochemistry in invasive and in situ ductal breast cancers (Zucker and Biswas 1994).
On the basis of limited information concerning TCSF localization in cancer tissue, the role of TCSF in tumor progression remains unclear. In the present study, to clarify the cell origin of TCSF and to study its role in cancer invasion, we performed in situ hybridization and Northern blot analysis on human lung and breast carcinomas as well as on normal tissues.
Materials and Methods
Source of Tissue
The tissue was obtained from 22 lungs resected for squamous cell carcinomas of Stages I (10 cases), II (eight cases), and III (four cases) according to the TMN classification, from seven normal lung samples, from 22 ductal breast cancers of Grade 1 (four cases), Grade 2 (14 cases), and Grade 3 (four cases) according to the Scarf and Bloom classification, and from seven benign breast proliferations (two fibrocystic disease and five fibroadenoma).
Tissue Preparation
Part of the samples were frozen in liquid nitrogen for Northern blot analysis and the remainder were fixed in formalin and embedded in paraffin for in situ hybridization.
In Situ Hybridization Localization
Tissue sections (5 μm) were deparaffinized, rehydrated, and treated with 0.2 M HCl for 20 min at room temperature, followed by 15 min in 1 μg/ml proteinase K (Sigma Chemical; St Louis, MO) in Tris-EDTA-NaCl, 37C, to remove basic proteins. The sections were washed in 2 X SSC (sodium saline citrate), acetylated in 0.25% acetic anhydride in 0.1 M triethanolamine for 10 min, and hybridized overnight with 35S-labeled (50C) anti-sense RNA transcripts. TCSF cDNA (1700
In Situ Hybridization Quantitation by Image Cytometry
Quantitation of the number of hybridization grains/μm2 was performed with the help of an automated image analyzer, the DISCOVERY system (Becton-Dickinson; Mountain View, CA). After thresholding, the number of grains are counted automatically on at least six fields at high magnification (× 500). At this magnification, one field measures 12,688 μm2. We performed these measurements on six different samples (three lung and three breast carcinomas) in which we found normal, in situ, and invasive areas on the same tissue section. Statistical analyses of TCSF mRNA expression levels were compared using the non-parametric Mann-Whitney U-test. Data were expressed as mean of dots/μm2 ± SEM. p values equal to or less than 0.05 were considered significant.
Northern Blot Analysis
Extraction of total RNA from tissues was performed by RNAzol treatment (Biogenesis; Bournemouth, UK). Ten μg of each RNA was analyzed by electrophoresis in 1% agarose gels containing 10% formaldehyde and transferred onto nylon membranes (Hybond-N; Amersham, Poole, UK). The membrane was hybridized with the cDNA probe encoding TCSF (1700
Results
Lung Lesions
By Northern blotting, TCSF transcripts were detected in 18 of 22 carcinomas. Quantitative analysis showed significantly higher (p<0.05) TCSF mRNA expression in lung carcinomas than in peritumoral lung tissues (Figures 1 and 2A). However, no significant differences between the TCSF mRNA levels were found in accordance with the TNM stage (Figure 2A).
With in situ hybridization, pre-invasive and invasive cancer cells were labeled in 18 of 22 tumors examined (the same positive samples as those found by Northern blot analysis). Stromal cells surrounding labeled invasive cancer cells, were always negative (Figure 3A). Normal (Figure 3C) or squamous metaplastic epithelium and bronchial glands did not express any TCSF transcripts. Moreover, in the normal or emphysematous adjacent lung, pulmonary alveolar macrophages identified by the CD68 monoclonal antibody (Dako; Carpinteria, CA) on serial sections (not shown) were particularly rich in TCSF mRNAs (Figure 3D). In the three cases analyzed by image cytometry, TCSF mRNAs were significantly expressed in tumor cell nests of both pre-invasive (1.68 ± 0.22 /μm2) and invasive areas (2.14 ± 0.35 /μm2) compared to the extracellular control compartment (0.19 ± 0.02 / μm2) and normal tissue (0.23 ± 0.04 /μm2) (p<0.05).
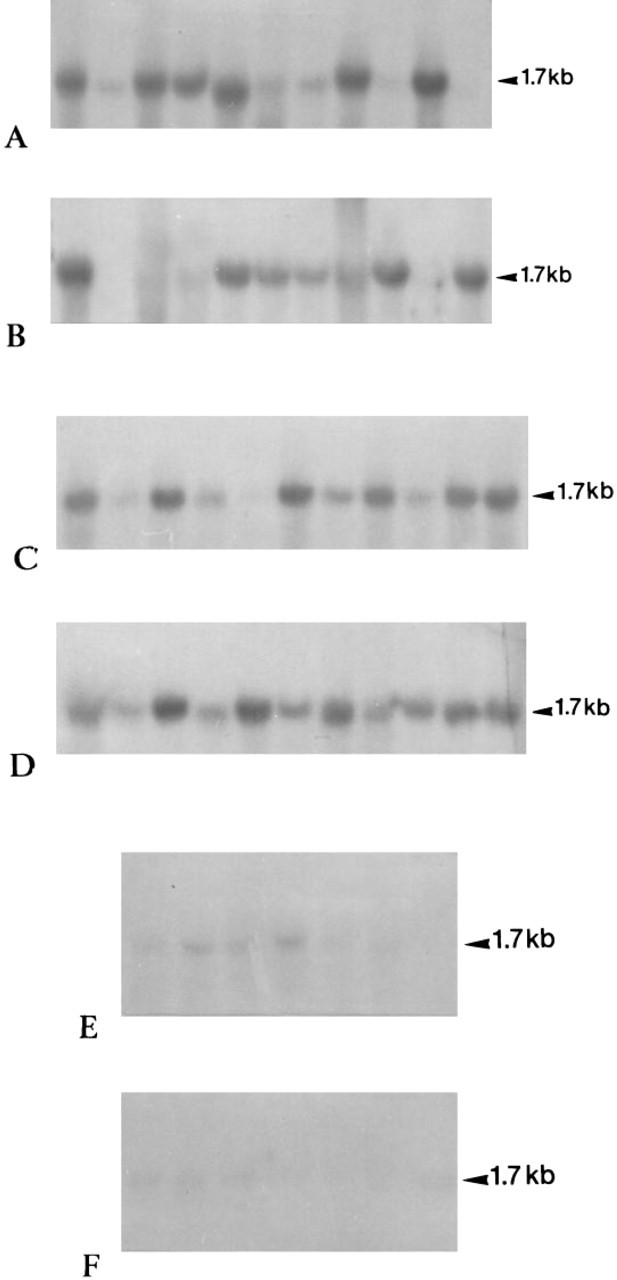
Northern blotting analysis of total RNA extracted from 22 lung carcinomas (
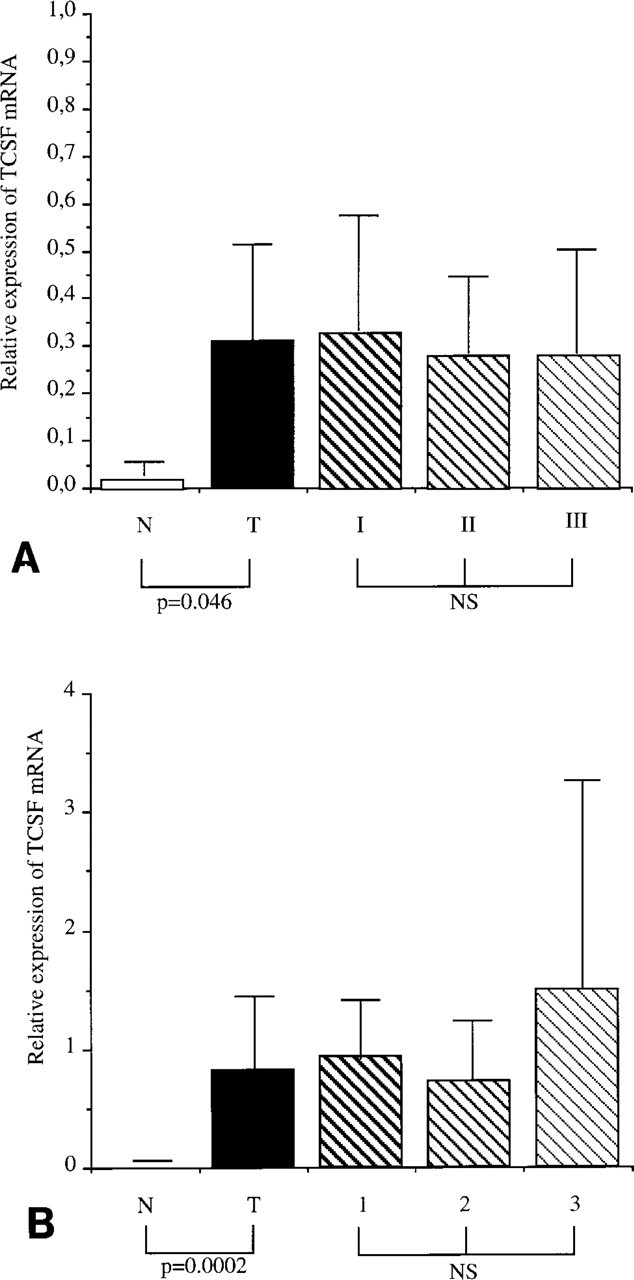
Comparison of TCSF mRNA levels (arbitrary units) according to tissue pathology and to the TNM stage and Scarf and Bloom grading in lung (
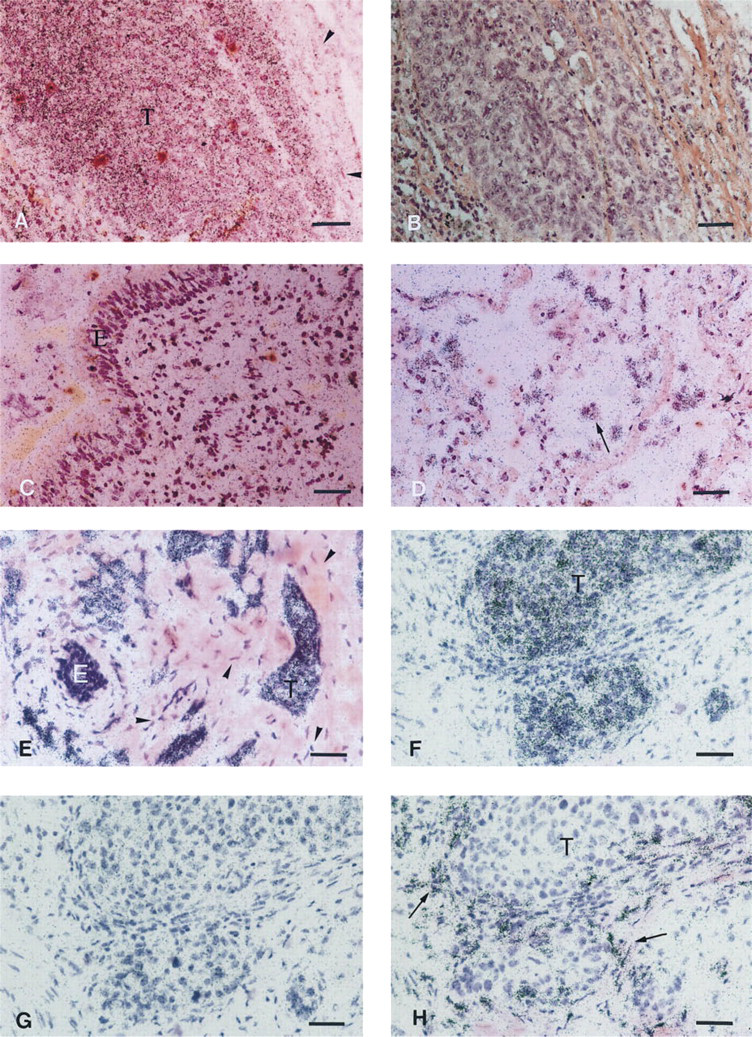
Localization of TCSF in lung cancers and breast cancers. (
Breast Lesions
By Northern blotting, TCSF mRNAs were detected in the 22 breast carcinomas. Quantitative analysis showed significantly higher (p<0.05) expression of TCSF mRNAs in breast carcinomas than in benign breast lesions (Figures 1 and 2B). No significant differences between the TCSF mRNA levels were found in accordance with the Scarf and Bloom staging (Figure 2B).
With in situ hybridization, benign proliferations and normal mammary areas mixed with cancer cells or adjacent to cancer areas did not show any hybridization grains (Figure 3E), whereas the TCSF mRNAs were detected in cancer cells in pre-invasive and invasive areas (Figure 3F) of all 22 tumors examined. Stromal cells did not contain any hybridization grains. In the three cases studied by quantification, the density of markers in both pre-invasive (2.14 ± 0.48/μm2) and invasive (2.95 ± 0.92/μm2) areas was significantly higher than in the extracellular control compartment (0.23 ± 0.12/μm2) and the normal areas (0.28 ± 0.10/μm2) (p<0.05). On serial sections, TCSF mRNAs were localized in cancer cells, whereas fibroblasts close to tumor clusters expressed mRNAs encoding gelatinase A (Figures 3F and 3H) in the same areas.
Discussion
In this study we clearly showed the presence of mRNA encoding TCSF in epithelial tumor cells of lung and breast carcinomas. In agreement with our observations, previous immunohistochemical studies detected TCSF in cancer cells in breast (Zucker and Biswas 1994) and in bladder carcinoma (Muraoka et al. 1993). In the latter study, no staining was found in epithelial cells in non-neoplastic urothelium, except in superficial umbrella cells. However, Zucker and Biswas (1994) reported that TCSF is also present in normal breast ductules and lobules near in situ carcinoma areas, describing a more extensive distribution of TCSF compared with our data obtained by in situ hybridization (ISH). No TCSF transcripts were detected in normal epithelial cells in both nonneoplastic breast and lung lesions. It is therefore likely that normal epithelial cells express low levels of the TCSF mRNAs that we could not detect by ISH but that could produce amounts of the TCSF proteins detectable by immunohistochemistry. The presence of TCSF mRNAs in benign and normal tissues was confirmed by our Northern blot analysis, identifying weak expression of TCSF mRNAs in those samples. Furthermore, our Northern blot analysis strengthened our ISH data because a higher significant abundance of TCSF transcripts was found in both breast and lung carcinomas than in benign and normal samples. The detection of TCSF mRNAs in intraepithelial cancer areas of the lung and mammary gland indicates that TCSF mRNA overexpression is an early event in carcinogenesis. These data, taken together, suggest that the expression of TCSF mRNA can be correlated with tumor progression. However, despite its implication in cancer progression, TCSF might play a role in some other pathological processes, such as inflammation and emphysema, because it has also been detected in alveolar macrophages in our study and it has been proposed as a factor in arthritis (Karinrerk et al. 1992).
Even though the precise function of TCSF is not known, some recent in vitro studies have shown that TCSF is able to stimulate the production of several MMPs by fibroblasts. Recent experimental data have demonstrated that TCSF stimulates the production of interstitial collagenase, stromelysin 1 and gelatinase A but not stromelysin 3 in fibroblasts (Kataoka et al. 1993). However, stromelysin 3 is known to have a poor proteolytic activity against collagen-like substrates (Murphy et al. 1994). Moreover, these authors have also demonstrated that TCSF increases activation of gelatinase A. These results are of particular interest regarding the implication of TCSF in cancer progression, because in many carcinomas in vivo the stromal cells have been demonstrated to be the principal source of several MMPs. A variety of studies have indicated that fibroblasts adjacent to the malignant tumors clusters produce interstitial collagenase (Urbanski et al. 1992; Hewitt et al. 1991; Polette et al. 1991), stromelysins 1, 2, 3 (Polette et al. 1991; Basset et al. 1990), and MT-MMP1 (Polette et al. 1996; Okada et al. 1995). More precisely, in both lung and breast carcinomas, mRNAs encoding gelatinase A, which degrades basement membrane collagens (Tryggvason et al. 1993), have also been localized by ISH in the stromal cells surrounding invasive carcinomas (Polette et al. 1993,1994; Poulsom et al. 1992,1993; Soini et al. 1993). In addition to their specific localization at the tumor-stromal interface, MMPs were not or were only weakly found in normal tissues and benign lesions. These studies have therefore demonstrated an association between MMP expression and the invasive process in cancers. Using serial sections in breast carcinomas, we showed that there is an obvious expression of TCSF mRNAs by tumor cells and gelatinase A mRNAs by fibroblasts in the same areas.
It therefore appears that some MMPs, as well as TCSF, are expressed selectively in both pre-invasive and invasive carcinoma but by different cell types, peritumoral fibroblasts and tumor cells, respectively. Relating our in vivo data to the observation that TCSF enhances the production of some particular MMPs in fibroblasts in vitro, it can be postulated that the TCSF produced by tumor cells in vivo stimulates the expression of some MMPs by peritumoral fibroblasts. However, in vivo, interstitial collagenase and stromelysin 1, which are induced by TCSF in fibroblasts in vitro, are infrequently observed in stromal cells in breast carcinomas (Polette et al. 1991), whereas they are present at high levels in lung cancers (Muller et al. 1991), despite the presence of TCSF in both types of carcinoma. Moreover, in four of 22 of our lung carcinomas, we failed to detect any TCSF transcripts. These findings are consistent with the involvement of other factors in the regulation of those MMPs, such as the origin of the tissue, the extracellular matrix environment, and genetic rearrangements.
In conclusion, our observations on lung and breast cancers strongly support the hypothesis that TCSF is an important factor in tumor progression. More precisely, TCSF produced by tumor cells could play a role in the degradation of extracellular matrix associated with tumor invasion by stimulating the synthesis of some MMPs by peritumoral fibroblasts.
Acknowledgments
We gratefully thank Dr Gillian Murphy for the generous gift of gelatinase A probe.
This material is based on work supported by the US Army Medical Research administration under award no. DAMD 17-95-5017, the ARC no. 1096, and the Lyons Club of Soissons.
