Abstract
Background/Objectives:
The objective of this study was to determine the efficacy and effectiveness of video education in a neonatal intensive care (NICU) setting and examine family engagement and satisfaction with video interventions. Currently, the families of preterm infants in Aotearoa New Zealand receive verbal and written information during their NICU stay. Parental stress and low health information fluency can prevent family members from connecting with the resources. Educational videos have been successfully used in other patient care settings and could be used in NICU to support the provision of oral and written information.
Methods:
The PRISMA-ScR model was followed to conduct this review. A literature search was conducted using Scopus, Academic Search Complete, PubMed and Google Scholar. Studies that examined videos used in NICU settings for family education, published from 2009 to 2025 and available in English, were included.
Results:
Initially 9,422 studies were identified, and eight full-text studies met the inclusion criteria. The studies were published between 2012 and 2022 and were primarily conducted in North America. Four studies used qualitative methods, and four used quantitative methods. The eight studies had a variety of foci – breastfeeding, infant care and needle puncture procedures – and investigated the effects of educational videos on family knowledge, confidence, implementation of taught strategies and how they received the education. The results suggested that video education can be effective when used in an NICU setting.
Conclusion:
Video education interventions in NICU have the potential to increase family knowledge, family implementation of taught strategies and satisfaction. Further research is required however to determine the impact of video education on infant outcomes and ongoing engagement with healthcare systems. To maximise efficacy, creating resources that are culturally relevant is essential.
Introduction
Every year, approximately 13.4 million infants are born preterm worldwide (Huong, 2024). Preterm infants are fragile and face many health challenges throughout their hospital admission while they continue to grow and develop (Perinatal and Maternal Mortality Review Committee, 2024). Preterm infants often have to undergo often painful procedures and tests, under the watchful eye of their family, and sometimes family members are not fully informed about what is happening to their infant (Eissler et al., 2023). When families feel well supported by their care team, particularly nurses in the NICU, they are more satisfied with the care they receive (Eskandari et al., 2021).
According to the World Health Organization’s (2023) Code of Ethics, healthcare professionals should ensure that family are fully informed about the procedures their children are to undergo (World Health Organization, 2023). However, in times of stress or intense emotion, it may be difficult to retain and process new information (Caisip et al., 2025; Eskandari et al., 2021; Gibson et al., 2021, 2023). Family members are more likely to retain information that is valued by them, such as the names of health conditions and diagnoses, but they are less likely to remember related information such as further tests needed or treatment plans (Kessels, 2003).
Healthcare information is primarily given orally by the healthcare provider (Armstrong et al., 2011). In Aotearoa New Zealand (NZ), healthcare delivery is affected by institutional racism, and how providers choose to speak to patients reflects this (Talamaivao et al., 2020). Providers may make assumptions about patients based on the limited information they have about them, such as their ethnicity or clinical presentation (Talamaivao et al., 2020). In NZ, racism is a key determinant of health for Māori, and negative healthcare experiences contribute to reduced health outcomes (Talamaivao et al., 2020). Concerningly, this impact is intergenerational, as children whose family members experienced medical racism have reduced health outcomes regardless of their own healthcare experiences (Talamaivao et al., 2020).
Written information is more accessible to educated patients, but within colonised countries such as NZ, it is generally written from the prospective and experiences of European individuals (Coleman et al., 2023). Because people do not experience healthcare in the same way, Eurocentric information sheets are unlikely to be helpful for non-European populations (Caisip et al., 2025; Kremer et al., 2025; Talamaivao et al., 2020). Culturally tailored information is required to ensure that patients have accurate information that they can connect with, and this is particularly important to Māori (Coleman et al., 2023; Kremer et al., 2025).
Emerging research shows that preterm care pathways in Aotearoa can be culturally unsafe for Māori (Adcock et al., 2022). Families report that they sacrificed their own health and experienced severe stress to ensure their babies experienced the best care they could provide (Adcock et al., 2022; Reweti, 2023). This highlights significant inequities in NICU experiences for Māori, which could be lessened by educational tools that promote cultural safety and family empowerment.
Educational videos have been used to provide accessible, easy-to-understand information for patients in healthcare settings. Videos have also been used to deliver health information outside the neonatal intensive care unit (NICU) setting to ensure that patients and families receive the information they need to, regardless of their health information fluency 1 or stress (Ahmed et al., 2021; De Sousa et al., 2022; Hoe et al., 2024; Kinnane and Thompson, 2008). Previous research has demonstrated the utility of video education in increasing health education fluency; however, there is limited evidence for Māori, nor Māori families attending NICU (Galmarini et al., 2024).
Existing reviews of literature focus on mixed media education including written and oral education and training procedures (Dol et al., 2017, 2019; Galmarini et al., 2024). This scoping review aimed to investigate the use of educational videos in NICU settings and how family members respond to video resources compared to oral and/or written materials. A search for publications including reference to whānau (family, extended kinship group) Māori was conducted with the aim of examining the impact that educational videos have on family stress, knowledge and engagement with preterm infants’ healthcare in an NICU setting.
Methods
Search strategy
The PRISMA-ScR guidelines were followed to develop this review (Tricco et al., 2018). Three key concepts were utlised for the search: visual educational resources, whānau (family) and NICU. Within this review, the term whānau referred to the primary caregivers of an infant, as well as wider family perspectives such as grandparents and close family friends. Education here referred to any intervention or information provided to family about their infant’s care or how they could support their preterm infant. A variety of keywords were included for each concept to ensure more studies were identified. The search strategy was adjusted according to the demands and style of each database (see online supplementary Table 1 for an example of the search terms used).
Studies were limited to those published from 2009 to 2025 and available in the English language. Data extraction and thematic analysis were conducted by the first author and reviewed by contributing authors. The search was carried out using PubMed, Scopus, Academic Search Complete (EBSCOhost) and Google Scholar. The initial search identified 9,422 studies (Figure 1), and eight papers were included in the final review. Publications were included if they were based in an NICU, used a video as their primary intervention and sought to educate the family. Publications were excluded if they targeted health professionals, if video was used for parent-provider communication such as via a tele-health intervention, if populations outside of NICU were examined or if parent health education fluency or mental wellbeing was not assessed. Publications were also excluded if they evaluated multiple interventions together, and it was not possible to determine the impact of the video education separately. Any type of literature review (e.g. systematic review) was also excluded.
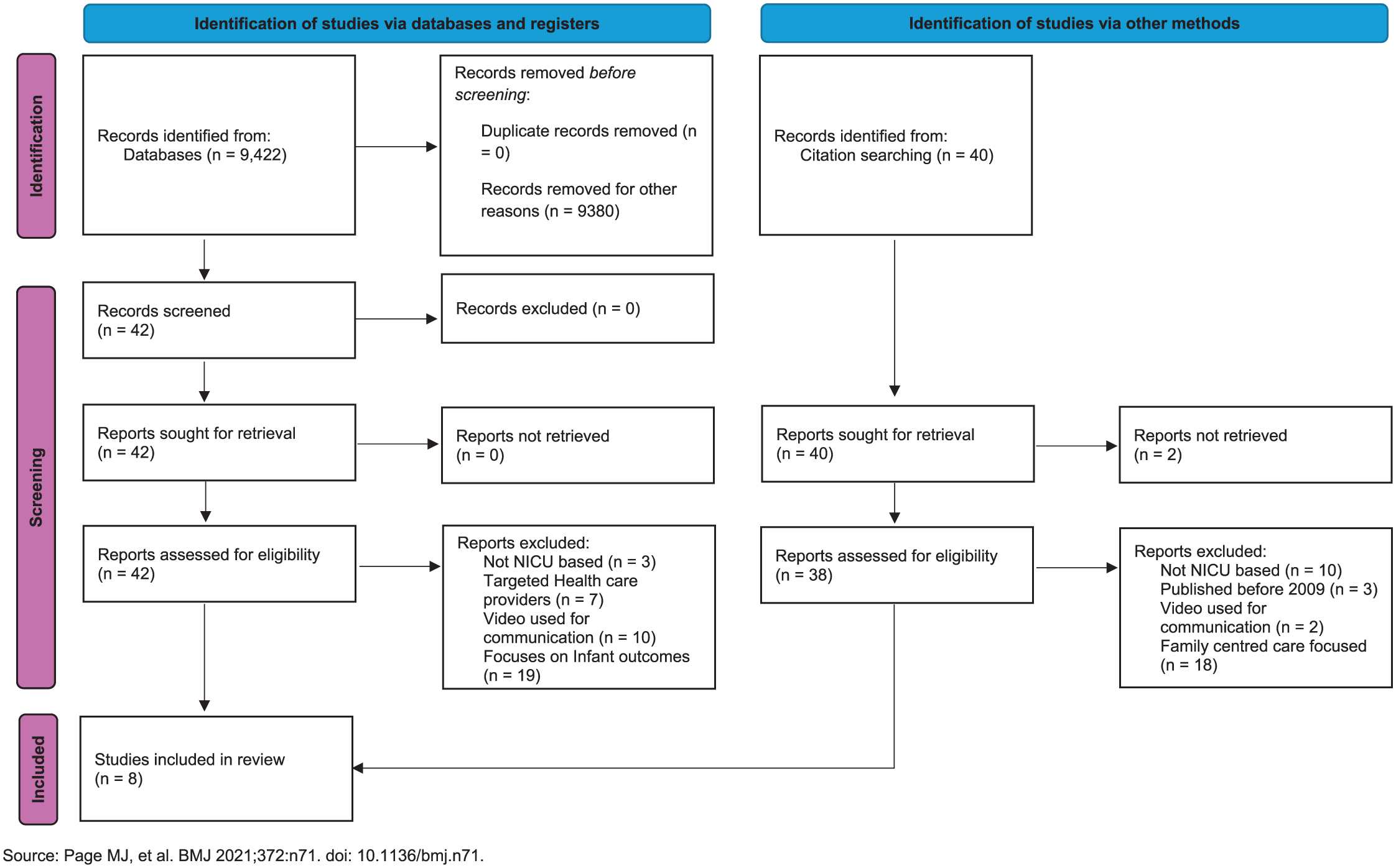
PRISMA-ScR diagram for the literature search.
Data synthesis was undertaken using a descriptive synthesis approach, inductively coding data to address the study aim (Pollock et al., 2024). The primary areas of interest were the knowledge and opinions of the family of preterm infants admitted to an NICU. Data concerning knowledge, stress and the application of learnt techniques were collected from the studies and analysed using qualitative content analysis (Pollock et al., 2024). The first author applied codes to the data, which were then arranged into themes. The codes and themes were then peer reviewed by the research team.
Results
Eight papers were included in the final analysis (Table 1). Each paper targeted the education of the family of NICU preterm infants. The incorporated studies used different methodologies and included quasi-experimental investigations, cross-sectional surveys, prospective non-randomised trials and non-randomised, non-blinded, pragmatic clinical trials. The video interventions referred to in the studies concerned a range of topics including diagnosed conditions and the examinations that might occur in preterm infants (intraventricular haemorrhage, retinopathy of prematurity, patent ductus arteriosus) and information about the NICU. Studies were heterogenous in their outcome measures, with five investigating parental knowledge, four investigating parental satisfaction with the video and two investigating intervention uptake post-video viewing. Some papers described a number of challenges the family faced during their infant’s admission such as breastfeeding, pain management or infant care.
Summary characteristics of included studies.
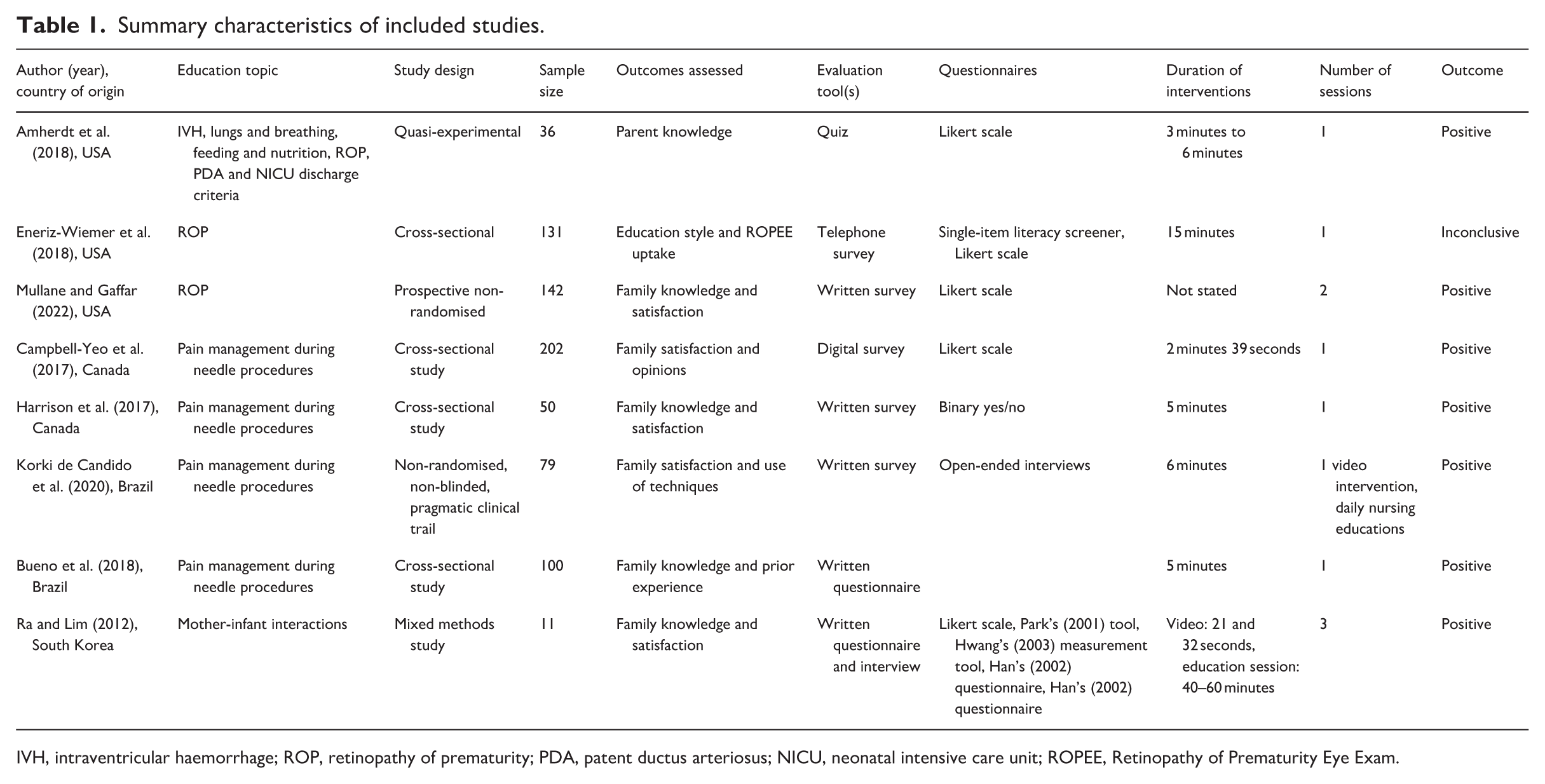
IVH, intraventricular haemorrhage; ROP, retinopathy of prematurity; PDA, patent ductus arteriosus; NICU, neonatal intensive care unit; ROPEE, Retinopathy of Prematurity Eye Exam.
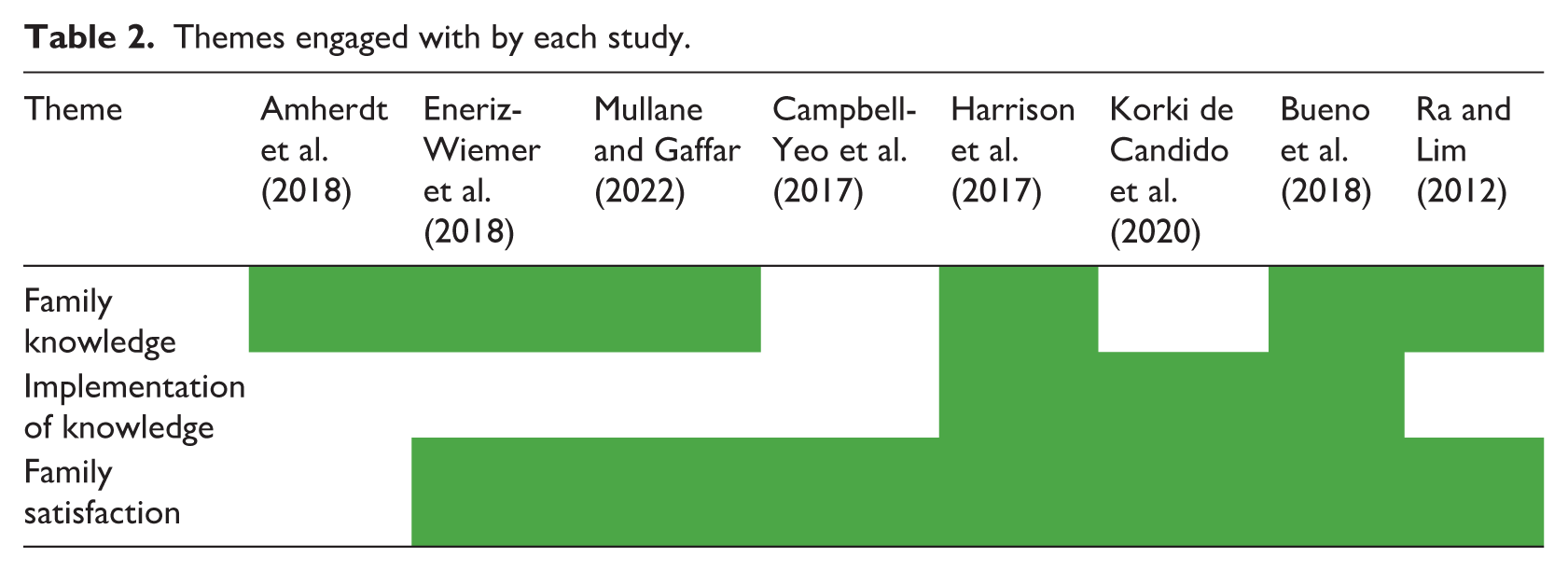
Thematic analysis of the eight papers included identified three main themes: family knowledge, family implementation of taught strategies and family satisfaction (Table 2). Family knowledge focused on the ability of the family to learn, retain and share information acquired from resources. Family implementation of taught strategies focused on the use of the techniques and information family members had been taught about in real-life situations, including their intention to use the strategies. Family satisfaction focused on family opinions about the resource, including aspects they would want to improve.
Themes engaged with by each study.
Family knowledge of medical information
In the studies selected, families in the video intervention groups had a better understanding of their infant’s diagnosis, treatment and how they could provide support during these procedures (Amherdt et al., 2018; Bueno et al., 2018; Eneriz-Wiemer et al., 2018; Harrison et al., 2017; Mullane and Gaffar, 2022; Ra and Lim, 2012). Amherdt et al. (2018), for example, found that 83% of participants were able to correctly answer 100% of the topic-specific questions following a single viewing of the video intervention (Amherdt et al., 2018).
The NICU environment is stressful and generally not considered well suited for learning. Video interventions were often coupled with educational seminars or written information. These interventions were effective in developing longer-term memory beyond the stressful environments (Tarchi et al., 2021).
Family implementation of taught strategies
Families that viewed educational videos were more likely to report using the strategies they had been taught (Bueno et al., 2018; Harrison et al., 2017; Korki de Candido et al., 2020). Bueno et al. (2018), and Korki de Candido et al. (2020) reported on the effects of videos educating about neonatal pain management and found that 96%–100% of parents intended to ask healthcare professionals to use pain-management strategies during future needle procedures (Bueno et al., 2018; Korki de Candido et al., 2020). Harrison et al. (2017) found that 40% of the intervention group parents asked healthcare professionals to use the taught pain-management strategies during needle procedures compared to 24% of the control group parents (Harrison et al., 2017).
Families reported that they found educational videos easier to follow as the relevant behaviours was modelled in a familiar context, for example, when interacting with an infant (Amherdt et al., 2018). A video intervention was also seen as more relatable to the family as they could see what was happening to the infant and how the infant responded, giving them behavioural cues to look for when they themselves used the strategy (Bueno et al., 2018; Harrison et al., 2017; Korki de Candido et al., 2020). Parents expressed that knowing what to expect during a needle-based procedure, and how to adjust their technique during, it helped the family feel more comfortable and encouraged them to engage with the healthcare system (Bueno et al., 2018; Harrison et al., 2017; Korki de Candido et al., 2020). Participants in the study by Ra et al. (2012) highlighted how ‘the content on mother-infant interaction . . ., and maternal role confidence was especially beneficial’ since it reinforced the value of behavioural modelling (Ra and Lim, 2012). In another study, a video intervention gave the family the confidence they needed to become more involved in their infant’s care and advocate for their infant’s comfort and safety with health care professionals (Harrison et al., 2017).
Family satisfaction of resources
The video interventions were more positively viewed by family members than the oral and written interventions (Bueno et al., 2018; Campbell-Yeo et al., 2017; Eneriz-Wiemer et al., 2018; Harrison et al., 2017; Korki de Candido et al., 2020; Mullane and Gaffar, 2022; Ra and Lim, 2012). In several studies, family members who were shown a video said they would recommend the video to other families, were more engaged with the material and found it easier to use and understand than written and oral interventions (Bueno et al., 2018; Harrison et al., 2017; Ra and Lim, 2012). For example, patients who viewed videos on retinopathy of prematurity were more likely to be ‘very satisfied’ with the treatment they received from providers than those who only received written information (Eneriz-Wiemer et al., 2018).
Video interventions were also preferred to other sources of information for using less jargon and less complex language (Bueno et al., 2018; Harrison et al., 2017; Ra and Lim, 2012). In one study, the use of video gave family members the necessary information to build their confidence to help their infant during needle-based procedures (Harrison et al., 2017). This confidence meant that family members could initiate discussions about pain-management strategies with the healthcare team (Harrison et al., 2017). In another study, being confident enabled family members to become more engaged with healthcare services in relation to premature infant discharge from hospital (Chen et al., 2016).
Discussion
Educational videos are a relatively recent addition to healthcare patient and family education. As a result, there is currently limited research on responses to patient and family education videos. Despite this, the limited literature in the NICU setting indicates that educational videos have the potential to reduce parent stress, increase parental engagement and improve family understanding of their infant’s condition (Amherdt et al., 2018; Bueno et al., 2018; Campbell-Yeo et al., 2017; Eneriz-Wiemer et al., 2018; Harrison et al., 2017; Korki de Candido et al., 2020; Mullane and Gaffar, 2022; Ra and Lim, 2012).
Because of this, it is important for family education to be included within clinical practice guidelines and equally important for these guidelines to be implemented within an equity framework (Gustafson et al., 2024; Rogers et al., 2025). Within an NZ context, Te Hā o Whānau (whānau voices leading maternity care) is a model of care that is based on Māori values (Stevenson et al., 2020) and can be used within a neonatal setting to increase cultural safety for Māori (Stevenson et al., 2020). A practice example provided within the model is for healthcare professionals to engage in meaningful communication that is comprehensible and allows participation by all, aligning with the findings of this scoping review (Stevenson et al., 2020). Its use is supported by research indicating that Māori families and parents want the very best health outcomes for their infant and to be active in the care of their infant (Adcock et al., 2021; Rogers et al., 2025).
Family knowledge of medical information
Krouse (2001) and Kinnane and Thompson (2008) demonstrated that family members retained more information from video education than from traditional oral or written methods, particularly at stressful times (Kinnane and Thompson, 2008; Krouse, 2001). Krouse (2001) demonstrated that the video modelling of behaviours improved patients’ understanding and consultation efficiency, especially when the patient could relate to the model (Krouse, 2001). Kinnane and Thompson (2008) found that patients who viewed videos concerning medical interventions and conditions had better recall than patients who experienced other methods (Kinnane and Thompson, 2008). Hoe et al. (2024) and De Sousa et al. (2022) identified that video education could be more effective at conveying complex information at stressful time as it supported formation of short-term knowledge (De Sousa et al., 2022; Hoe et al., 2024). Together, these findings indicate that there is a place for video education alongside written and oral face-to-face education in the NICU environment; however, research suggests that for maximum efficacy, context and time need to be taken into account (Eskandari et al., 2021; Gibson et al., 2023). Māori often prefer to be treated and make decisions as a collective, and in many families, there may be more than one person caring for an infant; therefore, educational resources such as video resources should be offered to multiple members of the family (Rogers et al., 2025).
Implementation of taught strategies
Video modelling, when presented in a relatable and culturally familiar way, has been shown to increase the likelihood of family members using the strategies they have been taught (De Sousa et al., 2022; Hoe et al., 2024; Krouse, 2001). Viewing real-life scenarios helps families feel better prepared to be more involved in infant care (De Sousa et al., 2022; Hoe et al., 2024; Krouse, 2001). Having resources that a family can connect to and identify with makes them more likely to engage with healthcare providers, helps them understand medical procedures and assists them to take steps to improve their own and their family’s health (De Sousa et al., 2022; Hoe et al., 2024; Maleki et al., 2022). For Māori, having resources and illustrations that reflect their cultural identity increases engagement with health education resources (Kremer et al., 2025).
Family satisfaction of resources
In a wide range of studies, families preferred video interventions to written or oral (Ahmed et al., 2021; Hoe et al., 2024; Kinnane and Thompson, 2008). Patients typically describe videos being more accessible, less intimidating and easier to understand, particularly when tailored to a lay audience using less jargon and real life. There is strong evidence that left to their own, patients seek out video education about health issues on platforms such as YouTube, whether they are recommended to do so or not (Ahmed et al., 2021). Gibson et al. (2023) and Eskandari et al. (2021) identified that the demands of caring for a sick child alongside the lack of knowledge of relevant procedures can cause severe parental distress (Eskandari et al., 2021; Gibson et al., 2023). Gibson et al. (2023) argue that parents want more information that they can easily engage with while caring for an infant to help make decisions about their care. To satisfy this interest and demand, healthcare providers need to provide information in a form that is engaging and easy to understand. One way of doing this is through up-to-date, culturally appropriate educational videos.
Blended education approaches
Despite family preferring video education and being able to retain information from them in a short period of time, video education alone does not promote the long-term retention of information (Deshpande et al., 2023; Krouse, 2001). The NICU is a high-stress environment. Stress inhibits the formation of long-term memories; therefore, relatively passive education forms such as videos need to be complemented by other approaches (De Sousa et al., 2022; Eskandari et al., 2021; Gibson et al., 2023; Hoe et al., 2024). Maleki et al. (2022) showed that in-person education is critical for some infant care tasks such as skin-to-skin care, indicating that video education should be a tool to assist not replace more family-centred and holistic forms of care (Maleki et al., 2022). Eskandari et al. (2021) also highlighted the important role that face-to-face nursing care can provide, giving new parents the emotional and practical support to build their confidence in infant cares. Face-to-face communication is likely to be preferred by Māori families, alongside access to written and visual education resources (Mead, 2016).
Limitations
This study had a number of limitations including the absence of a control group in many of the experimental studies. It is also important to note that there were no Indigenous participants in the included studies, signalling an important research gap. In NZ, future research that engages with Māori preferences for health education is essential to contribute equitable healthcare (Te Whatu Ora, 2024). Beyond this, only publications written in the English language were included, and further research using non-English language sources is required.
Proposed future research
Future research priorities include randomised controlled trials and mixed methods studies investigating the efficacy of traditional oral and written information techniques when offered alongside video education.
Conclusion
Educational videos are an underutilised resource in NICU settings. Having a preterm infant is stressful, and family are exposed to numerous challenges and receive large amounts of information in a short period of time. Providing written information alongside can result in family members having a backlog of information to cope with. Well-designed educational videos can provide viewers with complex information in an accessible way, enhancing health education literacy in a short amount of time. Creating resources that are culturally relevant is essential to maximise acceptability, engagement and efficacy.
Supplemental Material
sj-docx-1-hej-10.1177_00178969261419457 – Supplemental material for Are families attending a neonatal intensive care unit engaged and satisfied with video education? A scoping review
Supplemental material, sj-docx-1-hej-10.1177_00178969261419457 for Are families attending a neonatal intensive care unit engaged and satisfied with video education? A scoping review by Brynn McBurney, Amber Young and Lisa J Kremer in Health Education Journal
Footnotes
Acknowledgements
We thank Thelma Fisher, subject librarian at Ōtākou Whakaihu Waka (the University of Otago), for support in upskilling a member (BMcB) of the research group in literature searching.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: BMcB was in receipt of a Research Summer Studentship from He Rau Kawakawa (School of Pharmacy) (Reference SC403446).
Disclaimer
The views expressed in the submitted article are our own and not the official position of any of the institutions the authors are affiliated with.
Supplemental material
Supplemental material for this article is available online.
