Abstract
Introduction
Chronic pain, defined as pain that persists or recurs for more than 3 months (Treede et al., 2019), is a complex health issue that affects 30% of adults worldwide (Elzahaf et al., 2012), and represents a major human and economical burden (Campbell et al., 2019). A recent survey showed that 17% of Canadians aged 15 years and over experienced limitations in their daily activities because of constant or recurrent pain (Government of Canada, 2023). The influence and the need to address unfavourable lifestyle factors, such as physical (in)activity, stress, inadequate sleep and an unhealthy diet, are increasingly acknowledged to alleviate the impact of chronic pain (Nijs et al., 2024).
Living with chronic pain often implies a broad range of disruptions in daily routines and impacts on meaningful social and professional roles (Keponen & Kielhofner, 2006; Persson et al., 2013). Lifestyle-oriented interventions can help individuals reintegrate some of their roles through directly targeting effectiveness of activity pacing strategies in real-life daily routines (Nielsen et al., 2021; Uyeshiro Simon & Collins, 2017) which is an important factor of health-related quality of life in this population (Nielsen, Skou, Larsen, Søndergaard, & Christensen, 2022). Occupational therapy (OT) contributes to the management of chronic pain by identifying activities that are important and relevant to the individual living with chronic pain as a medium for therapy (Hesselstrand et al., 2015) and helping them use self-management strategies in their daily lives (Bouchard et al., 2025; Ochoa & Skubik-Peplaski, 2024). Yet, poor integration of this health profession within specialized chronic pain management multidisciplinary clinics has been documented (Lagueux et al., 2023; Slee et al., 2024).
OT driven lifestyle-oriented interventions, which focus on facilitating individualized development and implementation of healthy routines and habits, are increasingly being developed and showing promising therapeutic avenues to improve engagement in meaningful activities despite persistent pain (Lagueux et al., 2021; Shomer & Roll, 2022; Uyeshiro Simon & Collins, 2017). Among those, Lifestyle Redesign® provided initial impulse in research and clinical settings to promote health and well-being by reorchestration of daily activities in populations with or at risk of developing chronic conditions (Collins et al., 2025; Pyatak et al., 2022). In this context, Redesign your Everyday Activities and Lifestyle with Occupational Therapy (REVEAL(OT)) has been subsequently developed for adults living with chronic pain, and has undergone three iteration phases to improve delivery, outcomes, and fit within a specialized Danish pain clinic (Nielsen et al., 2024). It is a protocolized and manualized intervention led by two experienced and trained OTs that proposes a combination of two to four 1-hr individual sessions, four to eight 2-hr group sessions (maximum six patients) and daily guided-personal experience over the course of 12–15-weeks (Nielsen, Skou, Larsen, Bricca et al., 2022). The original version of this intervention included brief didactic presentations and discussions on various topics, skill training, personal experience, home visits, assistive devices loans, diary notes and wearing an activity tracker which detects daily physical activity, energy expenditure, and step counts. When added to usual care, REVEAL(OT) led to satisfaction and improvement in a range of occupational outcomes important to individuals living with chronic pain, such as more effective activity pacing, improved pain coping in everyday life (Nielsen et al., 2021; Nielsen et al., 2023), and positive change in occupational performance and satisfaction (Nielsen et al., 2024). Authors of this intervention also demonstrated its feasibility (Nielsen, Skou, Larsen, Polianskis et al., 2022) by showing satisfactory program adherence and patients’ self-perceived relevance, timing and mode of delivery.
It is increasingly recognized that it is more efficient to adapt an existing intervention than to create a new one, but also that this adaptation is necessary given that effectiveness of complex health intervention does not necessarily transfer to new contexts (Copeland et al., 2022; McKleroy et al., 2006). This adaptation process allows to balance the use of evidence-based practices with the practical aspect of delivering the intervention including the use of available resources. It also implies a tight collaboration with partners to optimize the intervention's suitability. Considering the REVEAL(OT)'s promising body of evidence, this project relies on rigorous guidelines to adapt it to a new context of delivery.
The present study is anchored in a wider multimethod research (Creswell & Creswell, 2023) project that aims to adapt REVEAL(OT) intervention with partners in two Montreal (Canada) specialized pain clinics (Masse et al., 2023). The Obesity-Related Behavioural Intervention Trials (ORBIT) model for developing behavioural treatments to prevent and/or manage chronic disease (Czajkowski et al., 2015), provides methodological guidance for an overall flexible and iterative process, from intervention development to intervention testing. The present study carries out Phase Ia (Define the intervention) of the ORBIT model and aims to understand the perspectives of patients, clinicians and managers about REVEAL(OT) and identify format- and content-related modifications that are necessary to adapt to the Canadian context.
Method
Study Design
A multicentric (Das, 2022) qualitative design (Creswell & Creswell, 2023) has been used to provide contextualized insight and conduct a series of focus groups and individual semistructured interviews with partners: patients, clinicians and managers. Combining these two qualitative data collection methods enhanced data richness (Coenen et al., 2012; Lambert & Loiselle, 2008) and allowed participants’ preferences to be respected while facilitating a more effective research process (Baillie, 2019). All interviews were moderated by one member of the research teams (JM) who was an OT and a PhD Biomedical science candidate with more than 20-years combined clinical and academic experience. A experienced researcher (GP) and a research assistant were also involved as comoderators in three focus groups. Ethics approval was obtained from the research ethics board of the Research Center of the Centre Hospitalier de l’Université de Montréal (CHUM) (#MP-02-2024-11469) and authorization to conduct research from the Research Institute of the McGill University Health Center (RI-MUHC) (#MEO-02-2024-9703). Written consent was obtained electronically from participants who all received a monetary compensation (CAD$50) for the time invested in this study. The Consolidated criteria for reporting qualitative research (Tong et al., 2007) was used report our research.
Participants recruitment
A convenience sampling method was used to recruit participants at the CHUM and the MUHC. Patients were recruited via posters and from invitations sent electronically and in person by the health care teams. Clinicians and managers from both sites were invited via emails and posters. A member of the research team (JM) contacted interested individuals by phone to assess eligibility. A purposive maximum variation sampling strategy (Palinkas et al., 2015) was also used in order to include the diverse perspectives related to sex and gender (patients, clinicians, and managers), socioeconomic level (patients), urban/rural living (patients), care paths (patients) and healthcare disciplines (clinicians). Patients’ pain characteristics were also documented.
Inclusion/exclusion criteria
Eligible patients were those living with pain for more than 3 months who received treatments at one of the participating sites for chronic pain in the past 12 months and were speaking French or English. Eligible clinicians and managers were those working with individuals with chronic pain at participating sites for at least 12 months or officially involved in administrative/managerial tasks at participating clinics, and speaking French or English.
Sample size
Final sample size was guided by the concept of information power (Malterud et al., 2016) to ensure sufficient relevant information was obtained.
Data Collection
From June 2024 to February 2025, a total of eight focus groups and 12 individual interviews were held separately for patients and clinicians and managers at each site. Prior to those interviews, a brief sociodemographic questionnaire was completed by all participants using Research Electronic Data Capture (REDCap). The semistructured interview guide (Appendix 1) was developed based on Proctor et al.'s conceptual framework and taxonomy of implementation outcomes (Proctor et al., 2009, 2011). The first part of the interview guide focused on chronic pain-related daily challenges and how current treatments address them or not. The second part addressed partners’ appreciation of the intervention and ways to improve its implementation while complementary visual documents summarizing the intervention mapping and its hypothetical pathway were shared to feed the discussion (Masse et al., 2023). This included information about the topics covered in the intervention, as well as its proposed format (mix of individual and group sessions, their length, and time in between them). In-person interviews were audiorecorded, whereas online interviews were audiovisually recorded. Both were subsequently transcribed verbatim.
Data Analysis
A rapid qualitative analysis approach (Gale et al., 2019; Kowalski et al., 2024) was used to produce rigorous and rapid results that will inform the ongoing codevelopment of the adapted version of the intervention. This pragmatic deductive analytic approach consists of using summarized data to identify the key elements in alignment with the interview guide. Step 1.Verbatim transcripts were summarized in an MS Word table using a structured template based on Proctor et al.'s (2009) taxonomy. The template summary table was developed by one researcher (JM), tested and improved by the lead researcher (GP) with two transcripts, and subsequently used with all verbatims (JM). A review of the summaries was carried out during regular meetings with the lead researcher (GP). Step 2. Summaries were subsequently consolidated into a matrix (Averill, 2002; MS Excel document) by participant type (patients vs. clinicians vs. managers) to identify themes. Within each theme of the structure template (lines), subthemes (columns) summarized important aspects of the intervention which required no or minor adjustments to better fit the local context versus areas for important modifications, while allowing comparisons across groups. Finally, two researchers (JM and GP) revisited the data to identify broad themes aligned with the research question and select illustrative quotes.
Findings
Participants Characteristics
A total of 32 patients (P), 21 clinicians (C) and 4 managers (M) were appoached to discuss service gaps in chronic pain interventions regarding occupational needs, and comment on the proposed intervention content and format. Six patients declined mostly due to critical health problems preventing them from participating whereas four identified patients and two clinicians were not reachable. Therefore, a total of 45 participants (22 patients, 19 clinicians and four managers) were interviewed (Table 1). Patients (64%), clinicians (84%) and managers (75%) mostly participated in focus groups compared to individual interviews. The majority of the interviews were held online (65%). Median duration was 84 min (range 61–90 min) for focus groups and 58 min (range 38–91 min) for individual interviews. Focus group sizes ranged from two to seven participants.
Participants’ Clinical and Sociodemographic Characteristics (n = 45)
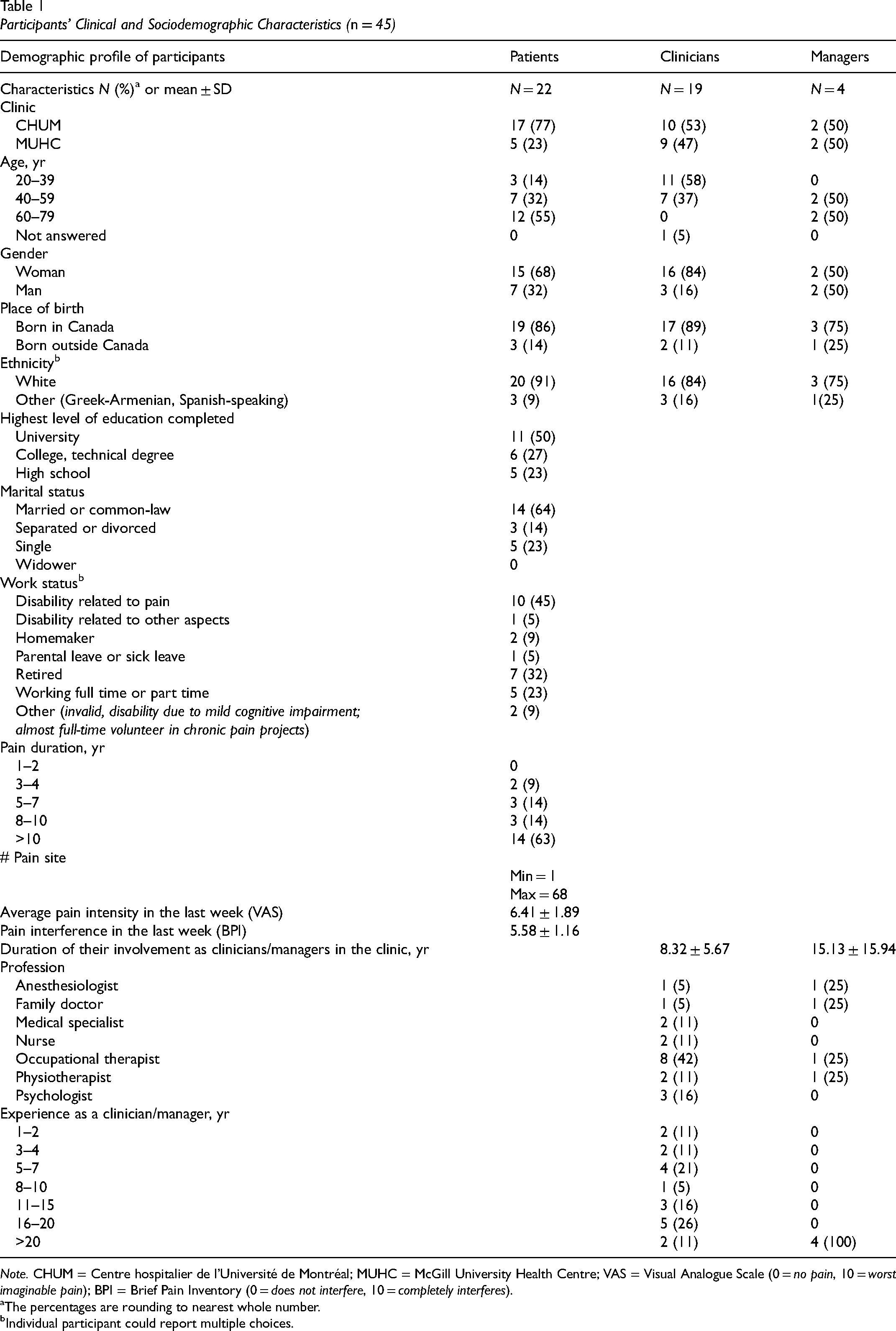

Note. CHUM = Centre hospitalier de l’Université de Montréal; MUHC = McGill University Health Centre; VAS = Visual Analogue Scale (0 = no pain, 10 = worst imaginable pain); BPI = Brief Pain Inventory (0 = does not interfere, 10 = completely interferes).
The percentages are rounding to nearest whole number.
Individual participant could report multiple choices.
Themes and subthemes are shown in Table 2 and explained below in details. The term “participants” will be used to refer to all categories of informants, that is, patients, clinicians and managers.
Themes and Subthemes
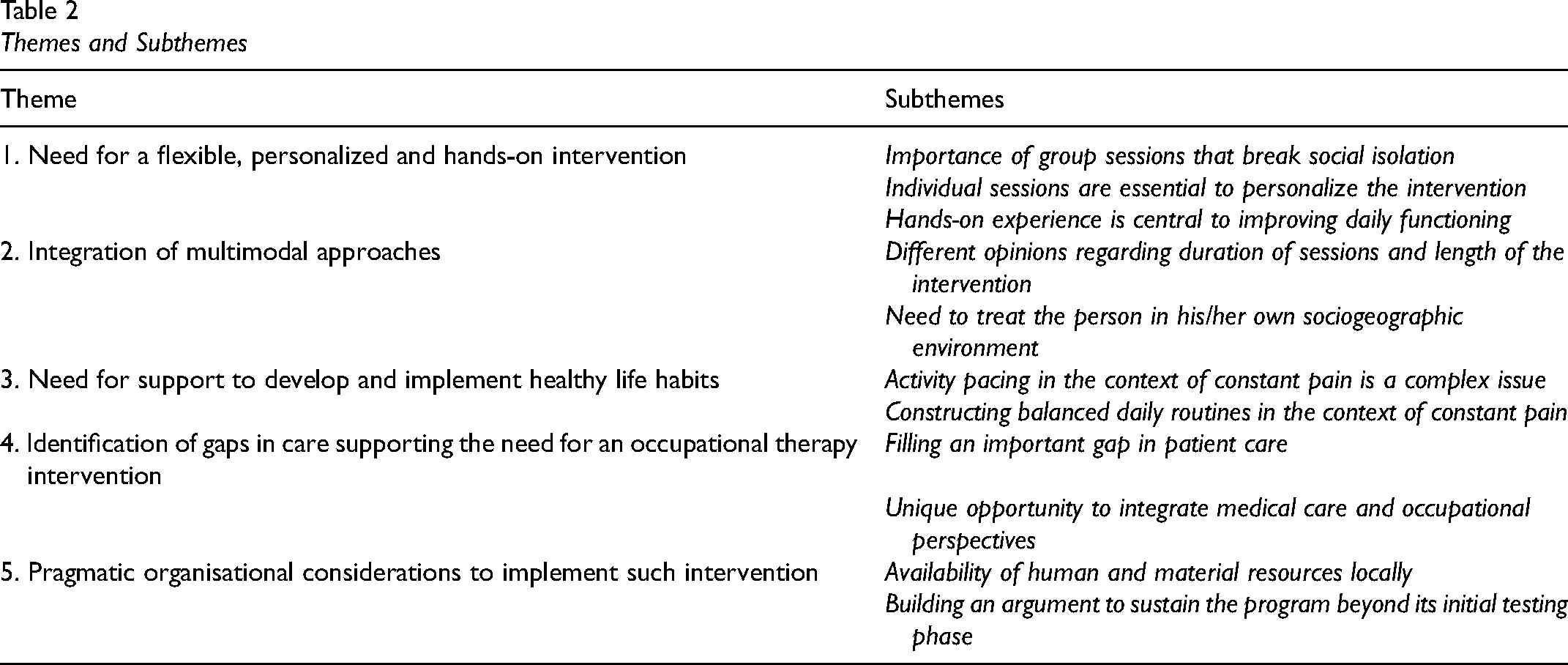
Need for a flexible, personalized and hands-on intervention
Participants expressed the need for an OT intervention that offers social interactions and yet is personalized. They valued the complementarity of group and individual sessions that each have a different purpose. Individual sessions were seen as essential to optimize the uptake and implemention of OT strategies. … there's a lot of different checkpoints where […] you can decide between you and the patient “what about your changes have not worked?”, then already […] restructure, make it fit […], that's the beauty of OT and tailoring to personal experience. (C19)
Clinicians also perceived benefits of group sessions, including a more efficient way to offer services to a larger number of patients: “I think group sessions are good […] especially if you have things that you can teach to a lot of people together … it's a waste of time to do one-on-one” (C14). Many patients emphasized the importance of group sessions that break social isolation. Although some of them expressed that there are risks in group settings that “… there will be one person that takes over and it takes away from other participants” (P20), they believed that feeling understood and sharing lived experience would help them find new ways to cope with chronic pain. Nevertheless, participants expressed that individual sessions are essential to personalize the intervention to each individual's daily experiences. A patient mentioned that “not everyone has the ability to adapt what we're shown” (P12).
There was a strong consensus about the idea that hands-on experience is central to improving daily functioning. Indeed, experienced OTs stressed the importance of in-vivo experimentation as the patients implement changes in their daily routines and suggested to advise patients from the beginning that “most of the work isn’t done in the clinic with us, it is done at home in your things” (C7). Patients expressed the need to explore new ways of performing daily occupations including the use of assistive devices while performing challenging activities under the supervision of a competent health professional. According to an OT manager, it also improves clinical outcomes. I think it's way better than just making a recommendation and never following up on it […] you have to practice with that activity for an X amount of time for it to become any kind of habitual tasks. (M4)
Integration of multimodal approaches
Results showed that while combining those approaches, the intervention format should be flexible. In fact, participants had different opinions regarding duration of sessions and length of the intervention. They generally approved the total duration of 12–15 weeks. A session every week or two was judged to be sufficient: “because we need time to change our habits […] I think it's important to do it at least once a week because you can forget, you can let yourself go” (P16). Although there was no clear consensus about the dosage of group versus individual sessions even within categories of participants, patients and clinicians agreed that a few booster sessions would be beneficial because “after discharge, they go back to their normal life […] and once we let them go, they're back to square one” (C14). Starting with higher treatment intensity and gradually decreasing sessions frequency has also been suggested by a clinician who proposed “in the beginning […] more frequent sessions would make sense and then […] there could be more time, more space so that they can do trial and error themselves” (C18).
In addition, participants stressed the importance of treating the person in his/her own sociogeographic environment. Although “it's good for both parties to come [home] and see in which environment we have to live with our condition” (P5), home visits are currently not possible due to the geographical remoteness and the impossibility to free up OTs involved in a hospital setting to travel to patients’ homes: “From a management point of view, with the resources we currently have […] it's impossible” (M2). Participants agreed that virtual therapy sessions could be an interesting alternative to gather useful information from the patient's home environment. These virtual sessions were also perceived as a way to remove barriers to attending in-person sessions in the context of disabilities, time constraints and financial issues. Nevertheless, patients, clinicians and managers insisted that in-person sessions are especially important at the beginning to foster the therapeutic alliance and that they enhance the level of attention and commitment given to the intervention. I feel more attentive when I'm there. […] I don't know why … maybe it's because I'm from a different background, and […] as I have an accent, if I ask questions, I like them to be well understood. (P16)
Clinicians and managers insisted that vigilance is required to find the right balance between in-person and group sessions in order to meet targeted clinical outcomes: “When we give patients the choice, often the patients who choose the virtual are precisely the ones who need help to get organized, to get moving and to get into action […] It's a paradox, because part of learning how to deal with your pain is managing your energy so that you can come to these appointments” (C10).
The inclusion of caregivers has also been raised frequently by participants. Many patients shared struggles associated with stigma and invalidation of chronic pain: “I've been living for 50 years with someone who keeps telling you “I don’t see the pain” (P17). At the same time, others expressed willingness to minimize the burden on their relatives and improve their ability to communicate their needs and limits. It's hard to “hold the boat” because they don't have any tools, then they want to understand us, but sometimes they're overloaded. (P3)
They mentioned that family members are sometimes “overprotective or not understanding” (M3) and highlighted the worthiness to include them at some point of the intervention: “because a household task […] is shared with family members, [so] to understand the capabilities and then how to share, that would be really relevant” (C12). Clinicians and managers also highlighted barriers associated with including relatives in interventions, including time constraints and that “there's such a large range of what you can have in terms of caregiver support or family dynamic” (C16).
Need for support to develop and implement healthy life habits
Patients expressed a deep concern about their daily functioning in the context of chronic pain and their explanations of their functional difficulties were often emotionally charged. For me it's a real ordeal […]. I'd say my whole day is pain management, sitting in my armchair, putting on ice every hour and a half […] it's depressing […]. (P14)
Activity pacing in the context of constant pain is a complex issue that seems to be the cornerstone of living well with chronic pain: “we have to learn to live with it, then dose our things” (P6). Clinicians and managers acknowledged that chronic pain “affects all aspects of daily life” (M3) and appreciated the pertinence of all of the nine topics addressed in the intervention (i.e., occupation for health and well-being, benefits of daily physical activity, meals and eating habits, occupational balance and time management, productivity/domestic and out-of-home activities, energy conservation, ergonomics at home and work, flow experience and leisure, and hobbies). They highlighted the necessity to address them given how they influence each other: “our patients suffer from a daily basis of problem in doing almost everything. […] the pain can be kind of a little snowball, around it there's so many things that keep collecting, […] if we can take this big snowball and make it a little bit smaller by this intervention, I think that would be great” (C14).
Concomitantly, patients expressed a great need for support to live better despite chronic pain. Practical adjustments to manage my energy, adapt my environment so I don't hurt myself, regain strength without hurting myself […] make me more independent, more functional. I need it, because I don't do anything at home anymore. (P21)
They recognize that constructing balanced daily routines in the context of constant pain requires a global overview of their daily routines to help them find space and energy not only for self-care and productivity, but also to accomplish “… hobbies, because we exhaust ourselves doing things, feeling useful, and we forget the things we love because we lack time, or energy, in the end” (P16). Patients expressed a need to add opportunities to be creative.
Identified gaps in care supporting the need for an OT intervention
All participants argued that adding REVEAL(OT) to usual care offered would be filling an important gap in patient care. In fact, no OTs are involved in those clinics and patients don’t have access to OT services in a timely manner. … the needs are significant and I think it's unfortunate right now that it appears to be only through rehabilitation centers that patients get these services and the wait lists are very long and only few patients qualify, when in reality many more could benefit even just from […] a brief intervention that may be not in a context of rehabilitation. (C13)
Most patients and clinicians had already heard about OT in various health care settings (e.g., hand therapy, acute care, vocational rehabilitation). While some participants across all categories said they wanted to know more about OT's concrete contribution to chronic pain management, those who had experienced it expressed great satisfaction. Clinicians and managers argued that adding such an OT service would be an unique opportunity to integrate medical care and occupational perspectives. We all talk to our patients about their daily activities, but I think most of us don't go into detail. We tell them that, yes, the aim of our interventions is to increase your functional capacity […], but it's clear that we don't have the skills or the time to do so. […] In my opinion, we're missing a player who can really put into practice what we're trying to do. (C1)
Pragmatic organisational considerations to implement such intervention
For participants, implementing the interventions appeared relatively straightforward, however some were concerned about its sustainability. Availability of human and material resources locally already supports the implementation of the intervention. The fact that OTs are working in both institutions but not directly in the pain units, raises the issue of staff mobility and financial resources. A rehabilitation manager stated that it would be preferable to involve two clinicians to avoid service breakdowns and promote the exchange of information and expertise. There were also concerns about long-term feasibility and sustainability of the intervention delivery in the current organisational structure and limited financial resources. The real “yes” is the funding of it. Taking away resources from another area to service this area, it's not a viable option. (M4)
Communication between OTs and other health professionals involved is a key aspect of the intervention. Our findings confirmed that OTs would be welcome to be actively involved in regular teams meetings and to contact other clinicians when needed: “… it would be very valuable information for us to share” (C13).
Finally, in a societal context of uncertainty in regard to chronic pain continuum of care transformation and budget restrictions, building an argument to sustain the program beyond its initial testing phase is essential: “we need to put this together in terms of human resources and in the right way” (M4). Although managers expressed clear commitment to the project, implementation of a new OT intervention still needs to be argued in terms of feasibility and clinical outcomes: “… if you have important results it can help to justify positions” (M1). The importance of avoiding redundancies with other levels of care that offer similar interventions such as rehabilitation centres has also been brought up from a managerial perspective.
Discussion
Our findings from interviews with patients, clinicians and managers showed that REVEAL(OT) is consensually perceived as a needed intervention that could fulfill an important clinical care gap, and could be implemented in both Canadian specialized pain clinics with minimal adjustments. The following discussion will stress the necessity and suggest avenues to best meet the occupational needs of patients, while considering barriers and facilitators to the optimization of the adapted intervention's implementation and suitability within its new context of delivery.
Avenues to Adapt the Intervention Content and Format
Translating OT evidence-based practices into new clinical settings requires strong collaborations between clinicians and researchers to identify efficient implementation strategies (Juckett et al., 2019). As shown in Table 1, our sample mostly consisted of patients with long-lasting (>10 years) diffuse (up to 68 pain sites) moderate to severe pain intensity (average 6/10 on VAS), clinicians from varied disciplines (OTs, medical practitioners, psychologists, physiotherapists and nurses) where OTs were in majority (42%), as well as balanced representation of medical and rehabilitation managers. Our data from all categories of participants suggest that group-based pain management programs have benefits in terms of providing social support and opportunities to be understood and share inspiring coping strategies which is consistent with a recent meta-analysis that shows that they improve quality of life and other pain outcome measures in patients with chronic musculoskeletal pain (Romm et al., 2021). On the other hand, individual sessions offer the advantage to personalize the treatment toward specific challenges and solutions (Bruce et al., 2023; Nijs et al., 2024). There was a general consensus among participants that adapting REVEAL(OT) to its new Canadian context requires the combination of group and individual sessions with a strong focus being put on hands-on experience. They emphasized that therapeutic activities shouldn’t only occur in the clinical setting, but first and foremost within the individual's own environment including their relatives. This is highly supported by recent evidence about the influence of social support on the experience of chronic pain (Gong et al., 2024; Huntsman & Bulaj, 2025).
Unlike the original intervention Danish context, home visits cannot be carried out by OTs working in targeted Canadian hospitals. This observation, as well as the geographical remoteness and preferences of many patients led to consider the use of telerehabilitation to some extent throughout the intervention. Although it can help align the rehabilitation process with people's daily environment and activities, all types of participants included in our study mentioned that it could and should not be used as an alternative to in-person treatment. They expressed concerns about its limited effect on patients’ engagement in the therapeutic process which may reduce its impact. These findings are consistent with a recent qualitative evidence synthesis (Velez et al., 2023) that demonstrated that online service delivery should be recommended not only as a solution to accessibility barriers, but as a complement to the usual in-person inpatient rehabilitation. From an OT point of view, it might also limit the establishment of the therapeutic alliance, hands-on experience and logistical difficulties for inexperienced patients that would need further assistance (Almog & Gilboa, 2022).
The Need for a Personalized Support to Manage Pain From a Lifestyle-Oriented Perspective
Our study corroborates the importance of addressing the complexity of the daily experience of living with chronic pain (Campbell et al., 2020). This involves understanding and addressing patients’ occupational needs in a personalized manner to create sustainable lifestyles that will support successful real-life pain management. It is increasingly well-known that modifiable lifestyle factors such as lower levels of physical activity, poor eating habits and sleep disturbances must be addressed to help break the vicious cycle of physical symptoms, poor functioning, and psychological distress in the context of chronic pain (Senba & Kami, 2017; van Hecke et al., 2013). We noted a strong consensus among interviewed participants about the complementarity of REVEAL(OT) with currently available treatments, which is inline with evidence about OT's unique contribution to interdisciplinary chronic pain management programs (Goodall & Brown, 2022; Kallhed & Mårtensson, 2018).
Habits and routines are complex by nature and fundamental to understand satisfaction, wellness and quality of life of people with disabilities (Clark, 2000) including chronic pain (Ochoa & Skubik-Peplaski, 2024). Nevertheless, lifestyle habits changes are huge challenges in the chronic pain population (Roose et al., 2023). Nijs et al. (2023) suggest a paradigm shift from a tissue- and disease-based approach toward individually tailored multimodal lifestyle interventions, arguing that it is much more coherent with the biopsychosocial nature of chronic pain and that further studies are needed to explore its effects. Our study embodies these principles and shows that capitalizing on OTs’ expertise in analysing and enabling occupation was perceived by both patients and clinicians/managers as an asset that would strengthen the impact of multidisciplinary specialized care already offered in both clinics.
Pragmatic Considerations
Implementing evidence-informed clinical programs requires careful consideration of contextual factors (Ernstzen & Louw, 2024). In the present study, availability of human and material resources was discussed with partners and informed the adaptation of the intervention. Partners’ point of views confirmed that all topics addressed in the original version of REVEAL(OT) intervention were relevant. However, they recommended a preponderance of group sessions over individual sessions, contrary to the original intervention, to increase effectiveness. Clinicians and managers mentioned that in a context of healthcare transformations and budgetary restrictions, long-term remuneration of clinicians beyond research funding could be challenging. Efforts will be required to set up optimal conditions to ensure the sustainability of the intervention beyond its initial testing phase. Iterative cycles of development with partners’ input are recommended to manage pragmatic realities of healthcare innovations (Kosiol et al., 2024; O"Cathain et al., 2019). Demonstrating OT intervention's clinical effectiveness from an economic perspective (Freeman et al., 2025; Ho & Argáez, 2017) is also an important avenue for future research to increase the likelihood of integrating the healthcare service offerings for chronic pain.
Study Limitations
Our sample is representative of pain population in terms of gender (two-thirds were women) (Keogh, 2022) but lacks heterogeneity in terms of age (more than half were over 60 years old), and life-course characteristics (a vast majority identified with white ethnicity, were born in Canada, maried and highly educated). Knowing that sociodemographic characteristics might influence the magnitude and severity of the impact of chronic pain (Campbell et al., 2019) and considering participants were recruited from only two pain clinics, it limits the tranferability of our results. The fact that the main interviewer was an OT and most of the clinicians were OTs as well provided a solid basis for discussing the adaptation process but may also induce bias in favour of such an intervention.
Conclusion
Chronic pain patients have unmet needs related to their daily functioning. According to the patient, clinician and manager's perspectives, the Danish lifestyle-oriented intervention REVEAL(OT) could improve functional outcomes in complementarity with multidisciplinary treatments currently offered in two Canadian specialized pain clinics. The importance that has been attributed to addressing occupational functioning and the necessity of individual and group sessions while allowing space for hands-on experience, face-to-face contact and caregiver involvement have been identified as essential elements in the process of its adaptation. Our study also suggests that optimizing its implementation and suitability within its new context of delivery requires that special attention be accorded to organizational constraints in relation to long-term allocation of resources.
Key Messages
Patients receiving pain clinic treatments report difficulties carrying out many lifestyle habits that are not directly adressed by current care.
Patients, clinicians and managers involved in two Canadian multidisciplinairy pain clinics agree that REVEAL(OT) fills an important gap by targeting functional outcomes using an OT intervnetion in complementarity with other interventions delivered by healthcare professionals.
Adapting this lifestyle-oriented intervention involves balancing multiple approches while personalizing the intervention and taking pragmatic considerations into account.
Footnotes
Acknowledgments
The research team warmly thanks all research participants for sharing their knowledge and lived experience.
Declaration of Conflicts of Interest and Funding Disclosure
The authors declare that there is no conflict of interest.
Funding
This study is funded by the Canadian Institutes of Health Research (Grant No. 486429). JM is supported by doctoral scholarships awarded by the Canadian Institutes of Health Research, Research Center of the Centre hospitalier de l’Université de Montréal, Université de Montréal’s Faculty of Medicine and Faculty of Graduate and Postdoctoral Studies and Ordre des ergothérapeutes du Québec. MGP is a Junior 2 research scholar from the Fonds de recherche du Québec—santé. SSN and STS are funded by the Exercise First research and implementation program, Region Zealand, Denmark. JRC is funded by the two Research Units for General Practice Aarhus and Odense, Denmark. The Danish version of the REVEAL(OT) intervention was supported by grants from Region Zealand Health Research Fund (Reg. SJ-703); The University of Southern Denmark (Reg. principal investigator S. S. Nielsen); and The Danish OT Association (Reg. FF1-18-R76-A1690).
Author biographies
