Abstract
Objective:
The dual-factor model of mental health postulates a role for positive mental health, alongside mental illness, in determining mental health care needs. Informed by this model, the present study delineated profiles of social-emotional competencies and difficulties during middle childhood in a population-based sample of girls and boys and determined their association with adolescent mental disorder diagnoses.
Method:
Latent profile analyses were conducted across five indices of social-emotional competency and four indices of psychopathology that were measured by questionnaire self-report among 13,349 girls and 13,488 boys at age ~11 years. The association of the profiles with adolescent presentations to hospital or ambulatory services (ages ~12–17 years) were determined using logistic regression.
Results:
Analyses yielded five profiles in each sex:
Conclusion:
Combining information on social-emotional competencies and psychopathology in middle childhood may help refine the provision of mental health promotion and early intervention to alleviate adolescent mental disorder.
Keywords
With rates of youth mental disorders and psychological distress increasing globally (Brazel et al., 2023; Sacco et al., 2024; Slade et al., 2024; Tkacz and Brady, 2021), and adolescence marking the peak period of onset for many mental disorders (Solmi et al., 2022), school-based tiered mental health and wellbeing interventions have become a popular, evidence-based avenue of mitigating burden on mental health services (Grové and Laletas, 2020; Humphrey, 2023; Lee et al., 2023). These tiered interventions incorporate universal prevention for all students, alongside targeted interventions for students with emerging psychopathology, and individualised intensive interventions for students with established mental health difficulties. By universally fostering social-emotional wellbeing for all children, these approaches seek to prevent an increasing accumulation of need at the targeted and intensive intervention levels (de Bruin et al., 2023; Greenberg et al., 2017; Guest et al., 2024). They align well with growing evidence in support of a ‘dual-factor model of mental health’, wherein positive mental health and mental illness represent distinct (albeit correlated) factors rather than the extreme ends of a single dimension (Greenspoon and Saklofske, 2001; Suldo and Shaffer, 2008). Positive mental health is defined by the World Health Organisation (2025) as ‘a state of mental well-being that enables people to cope with the stresses of life, realize their abilities, learn and work well, and contribute to their community’. The model postulates that consideration of indicators of social-emotional wellbeing alongside symptoms of ill health may better differentiate children’s need for interventions (Iasiello and Van Agteren, 2020) and help inform the level of intervention required. Informed by the model, the present study sought to examine population patterns in children’s co-presentation of social-emotional competencies and symptoms of psychopathology during middle childhood and determine how these patterns related to children’s subsequent presentations to health services with mental disorders during adolescence.
The dual-factor model of mental health proposes four different expressions (profiles) of social-emotional wellbeing and psychopathology in the population, namely: (1) ‘
Varying support for the four expressions in the dual-factor model has emerged from these analyses, conducted in child and adolescent community samples across a diversity of social-emotional wellbeing and psychopathology indicators, as summarised in Table 1. Across these studies, differing numbers of profiles emerged, including 3- (Clark and Malecki, 2022), 4- (Kim et al., 2018; Moore et al., 2019; Petersen et al., 2020) and 5-profile (Gregory et al., 2024) solutions. Multiple investigations were unable to detect a ‘
Summary of latent profile/class analyses conducted among children and adolescents and informed by the dual-factor model of mental health.
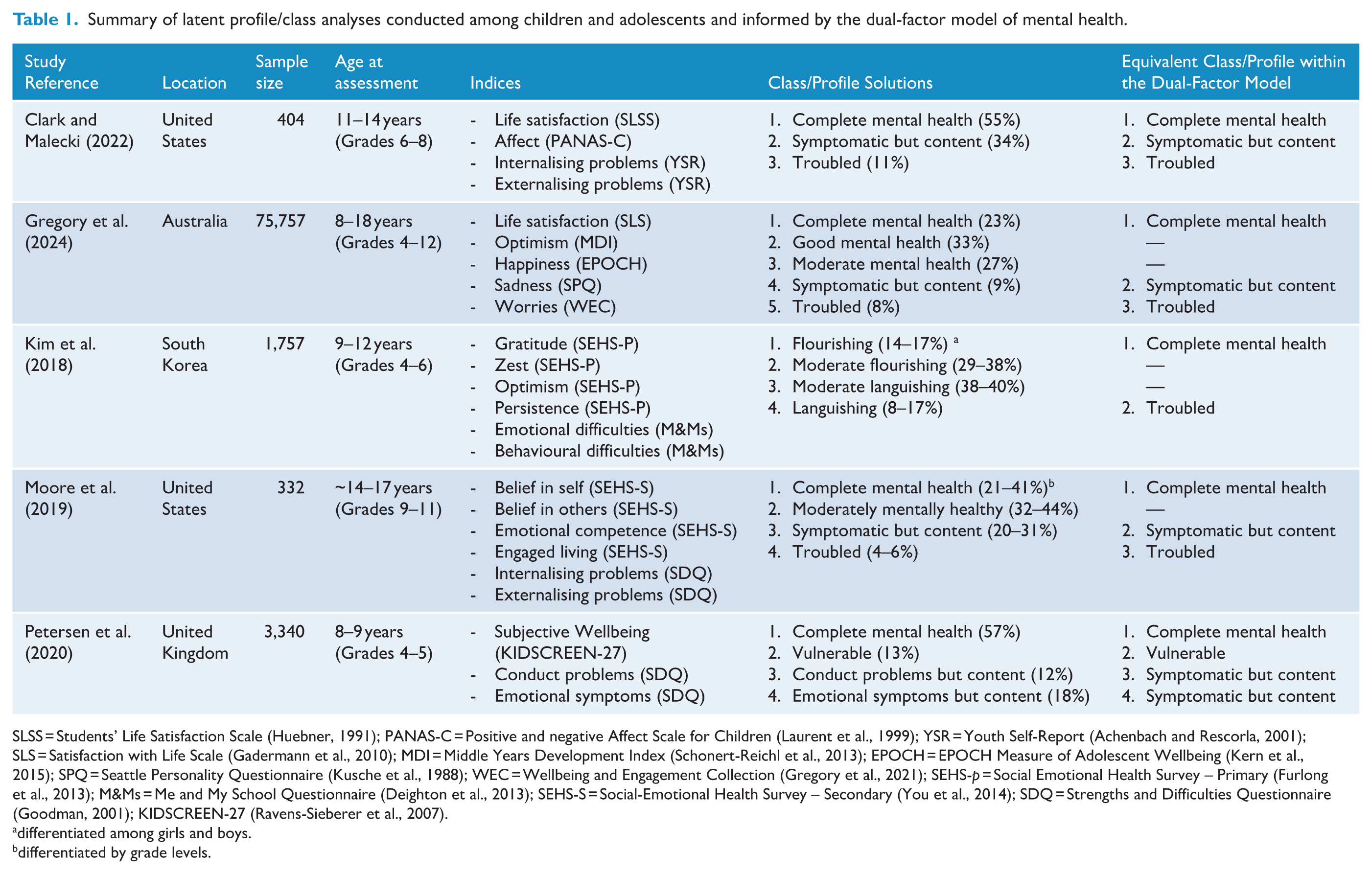
SLSS = Students’ Life Satisfaction Scale (Huebner, 1991); PANAS-C = Positive and negative Affect Scale for Children (Laurent et al., 1999); YSR = Youth Self-Report (Achenbach and Rescorla, 2001); SLS = Satisfaction with Life Scale (Gadermann et al., 2010); MDI = Middle Years Development Index (Schonert-Reichl et al., 2013); EPOCH = EPOCH Measure of Adolescent Wellbeing (Kern et al., 2015); SPQ = Seattle Personality Questionnaire (Kusche et al., 1988); WEC = Wellbeing and Engagement Collection (Gregory et al., 2021); SEHS-
differentiated among girls and boys.
differentiated by grade levels.
Limited research has explored longitudinal associations between these childhood/adolescent profiles and later mental illness. In their study of US students (Grades 9–11), Moore et al. (2019) indicated significantly higher later mean depression and anxiety symptoms in Grade 12 for the ‘
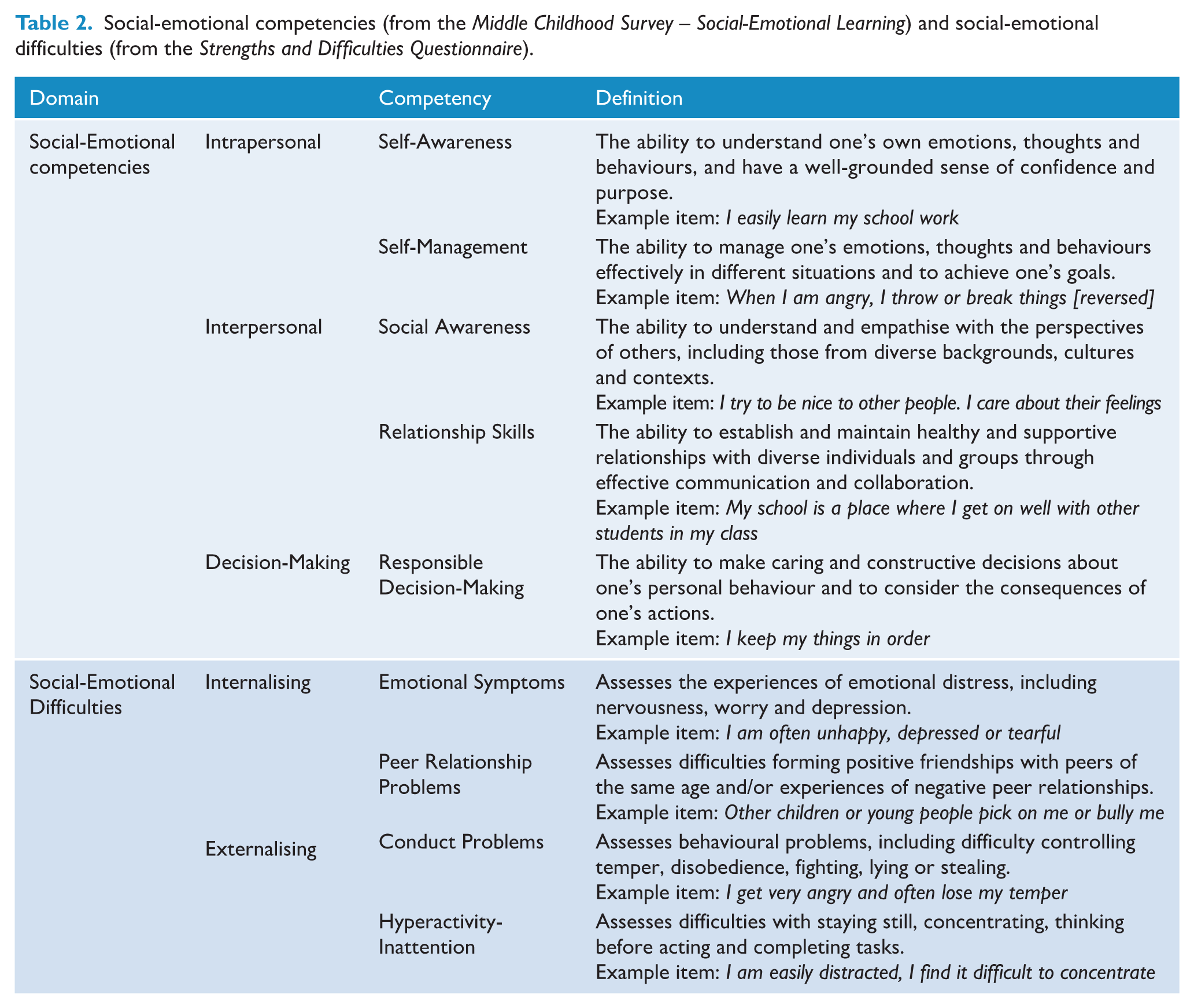
The present study examined these questions using data from a large population-based sample of ~27,000 children drawn from the New South Wales Child Development Study (NSW-CDS; Green et al., 2024). LPA analyses determined middle childhood mental health profiles, separately for girls and boys, according to nine indices (described in Table 2) of social-emotional competencies (
Social-emotional competencies (from the
Method
Participants and procedure
Participants in this study (
Ethical approval (HREC/18/CIPHS/49) for the linkage was provided by the NSW Population and Health Services (2019/ETH01571) and ACT Health Human Research Ethics Committees (2019.STE.00184), with relevant data custodian approvals. Probabilistic linkage of records was conducted by the Centre for Health and Record Linkage, managed by a third party under a waiver of consent process consistent with the Australian National Health and Medical Research Council’s (2007) National Statement of Ethical Conduct in Human Research. False linkage rate across all record sets was estimated at 0.5%.
Measures
Social-emotional competencies and difficulties
Children’s self-reports of five social-emotional competencies (as defined by the Collaborative for Academic, Social and Emotional Learning [CASEL], 2005, 2025) were assessed using the
Mental disorders
Health service contacts for mental disorder diagnoses were recorded in any of four record sets provided by the NSW Ministry of Health:
Four binary outcomes were explored: (1) any mental disorder diagnoses; (2) externalising disorders, including conduct disorder, mixed disorders of conduct and emotion, cluster B personality disorders and substance use disorders; (3) internalising disorders, including affective and anxiety disorders and (4) self-harm or suicidal ideation presentations (Supplementary Table S2 details the ICD-10-AM codes related to these outcomes). Presentation of these disorders from January 2016 (the year after Middle Childhood Survey completion in 2015) were coded 1. The reference group (coded 0) for all analyses was the group of children who had no recorded mental health diagnoses at any time.
Sociodemographic variables
Each child’s sex (as assigned at birth) and Aboriginal and Torres Strait Islander background (0 = non-Indigenous; 1 = Indigenous) was determined by consensus across NSW-CDS linked records. Area socioeconomic disadvantage was coded from the child’s residential postcode in 2015 (0 = bottom four quintiles, reflecting less disadvantage; 1 = highest quintile, reflecting greatest disadvantage), according to the Socio-Economic Indexes for Areas (SEIFA) Index of Relative Socio-Economic Disadvantage (IRSD) ratings (Australian Bureau of Statistics, 2011). Children’s geographical remoteness was coded according to children’s residential postcodes using ratings from the Accessibility and Remoteness Index of Australia (0 = major cities; 1 = inner regional, outer regional, remote and very remote areas; Department of Health and Aged Care, 2001).
Statistical analysis
Latent profile analyses
Latent profiles were specified in Mplus version 8 (Muthén and Muthén, 1998) for girls and boys, separately. Models were repeated, specifying two to
Profiles and later mental health service use
Once profile solutions for girls and boys were selected and the most likely profile memberships extracted for each child, a series of bivariate (unadjusted) logistic regressions were conducted to explore associations between the mental health profiles (relative to an average/moderate mental health profile) and mental health presentations, with children who had no presentations as the reference group. Analyses were repeated controlling for sociodemographic covariates (Aboriginal/Torres Strait Islander background, area-based socioeconomic disadvantage and geographical remoteness). The logistic regression analyses yielded odds ratios and their 95% confidence intervals (CIs), with significance denoted by CIs that did not cross 1.00. Odds ratios of 1.00–1.49 (or 1.00–0.67) were interpreted as small effects, 1.50–2.49 (or 0.66–0.40) as medium, 2.50–4.00 (or 0.39–0.25) as large and >4.00 (or <0.25) as very large effects (Rosenthal, 1996).
Results
Latent profile analysis
For girls and boys, solutions are reported up to nine profiles (Table 3), beyond which the LMR-LRT was consistently non-significant, indicating no improvement in fit. With each increase in the number of profiles specified, small improvements were observed in AIC and BIC. For both samples, LMR-LRT was non-significant at the six-profile solution, indicating six profiles did not significantly improve fit above the five-profile model. In both samples, a five-profile solution was the last model before the smallest profiles consistently comprised less than 5% of children and before posterior probabilities fell below 80%. Accordingly, the most likely profile memberships from the five-profile solutions for girls and boys were extracted for each child.
Model fit comparison of latent profile analysis of social-emotional competencies and psychopathology among girls and boys.
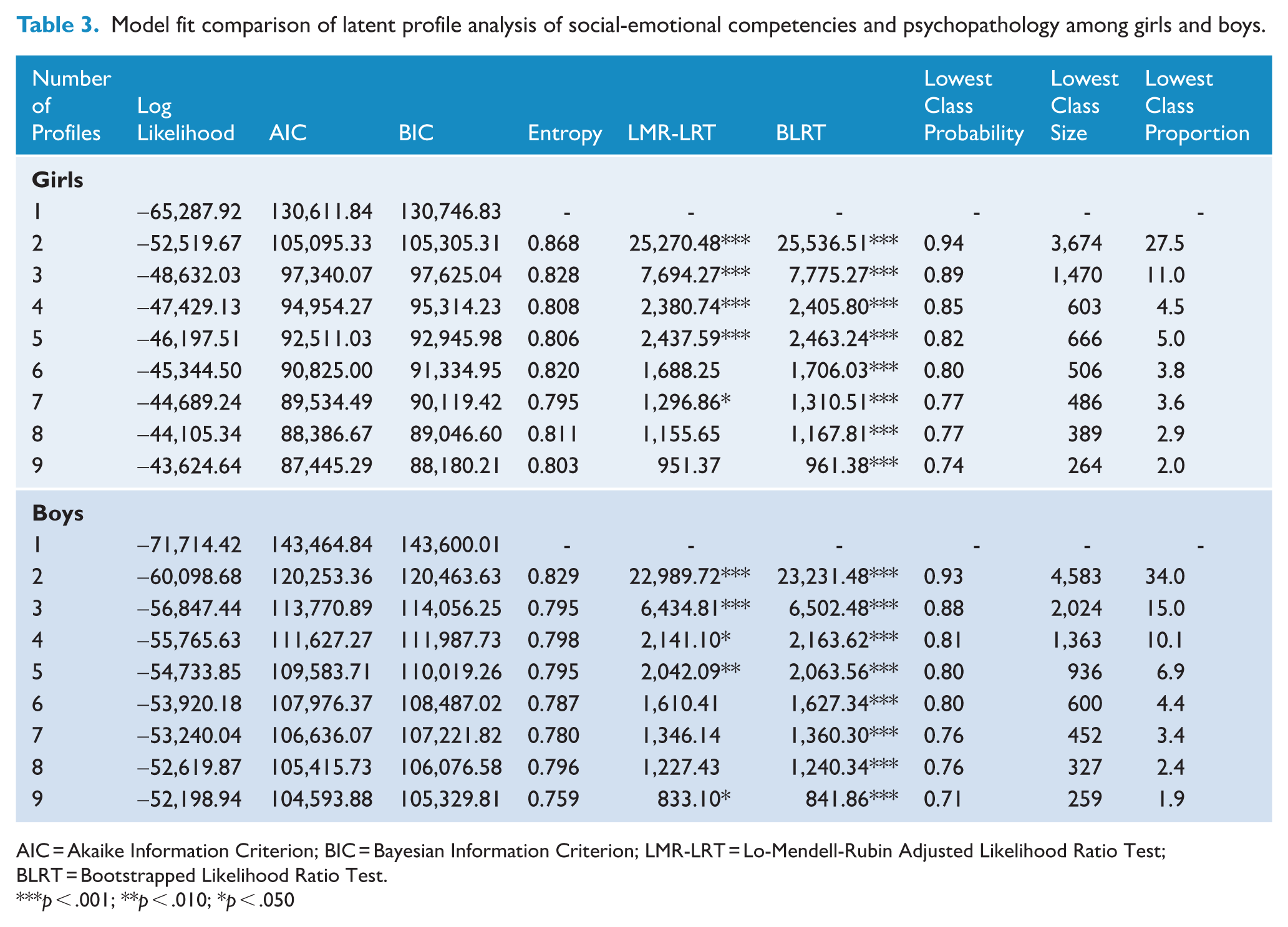
AIC = Akaike Information Criterion; BIC = Bayesian Information Criterion; LMR-LRT = Lo-Mendell-Rubin Adjusted Likelihood Ratio Test; BLRT = Bootstrapped Likelihood Ratio Test.
Mean values of the nine constructs for children in each of the five profiles are displayed in Figure 1 (and detailed in Supplementary Table S3). Profile patterns were sufficiently comparable for girls and boys to support consistent naming, albeit cross-tabulation analyses revealed small but significantly different prevalence distributions by sex for each of the five profiles. Prevalences for girls and boys in each profile were:
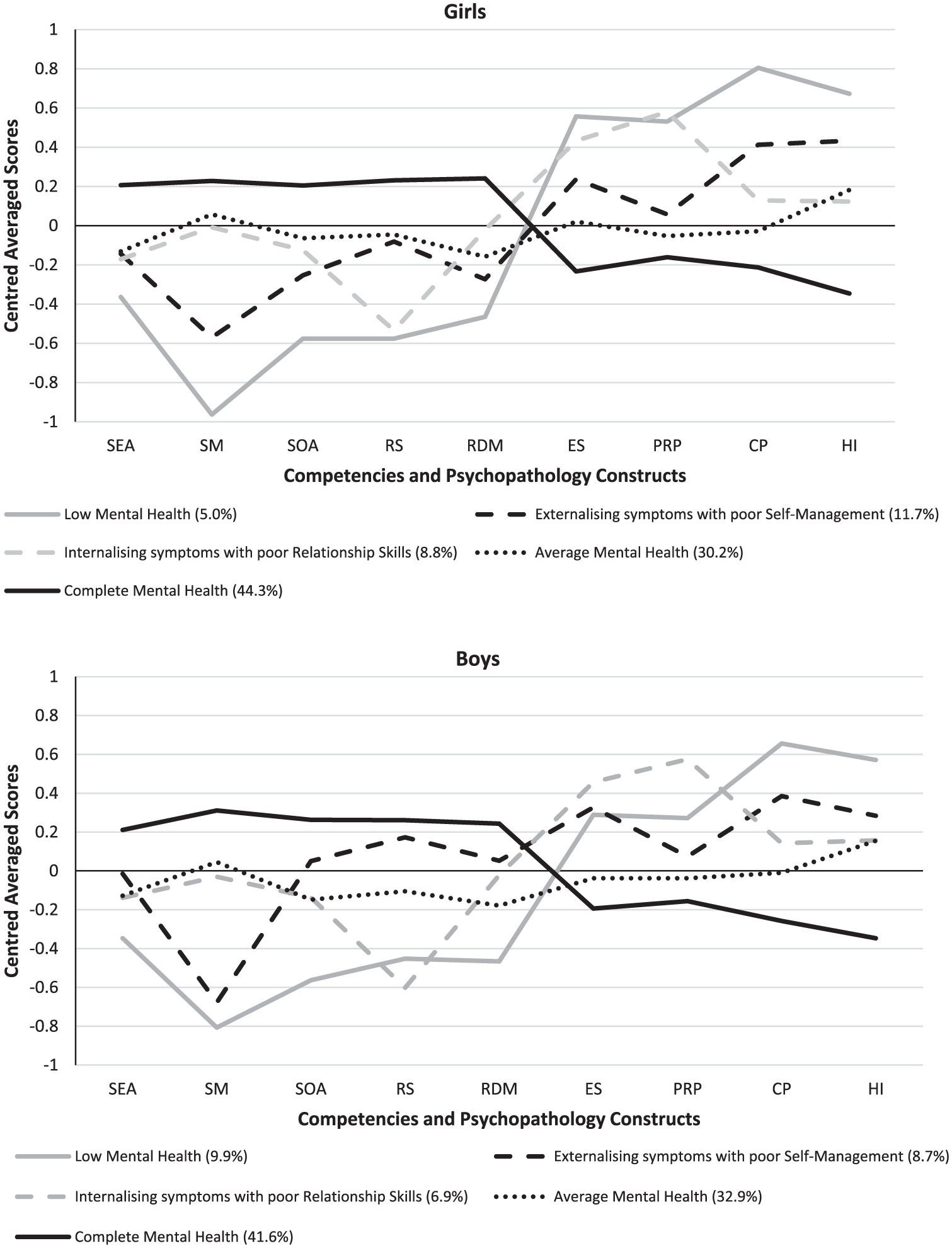
Latent profile analysis solutions evidencing five profiles for girls and boys.
Profiles’ associations with adolescent mental health service presentations
Table 4 presents the distribution of children within each profile according to adolescent health services presentations with mental disorder diagnoses (aged ~12–17 years). Table 5 displays the odds of children in each profile presenting with mental disorders, each relative to
Mental health presentations post-2015 (ages ~12–17 years) according to mental health profiles in middle childhood.
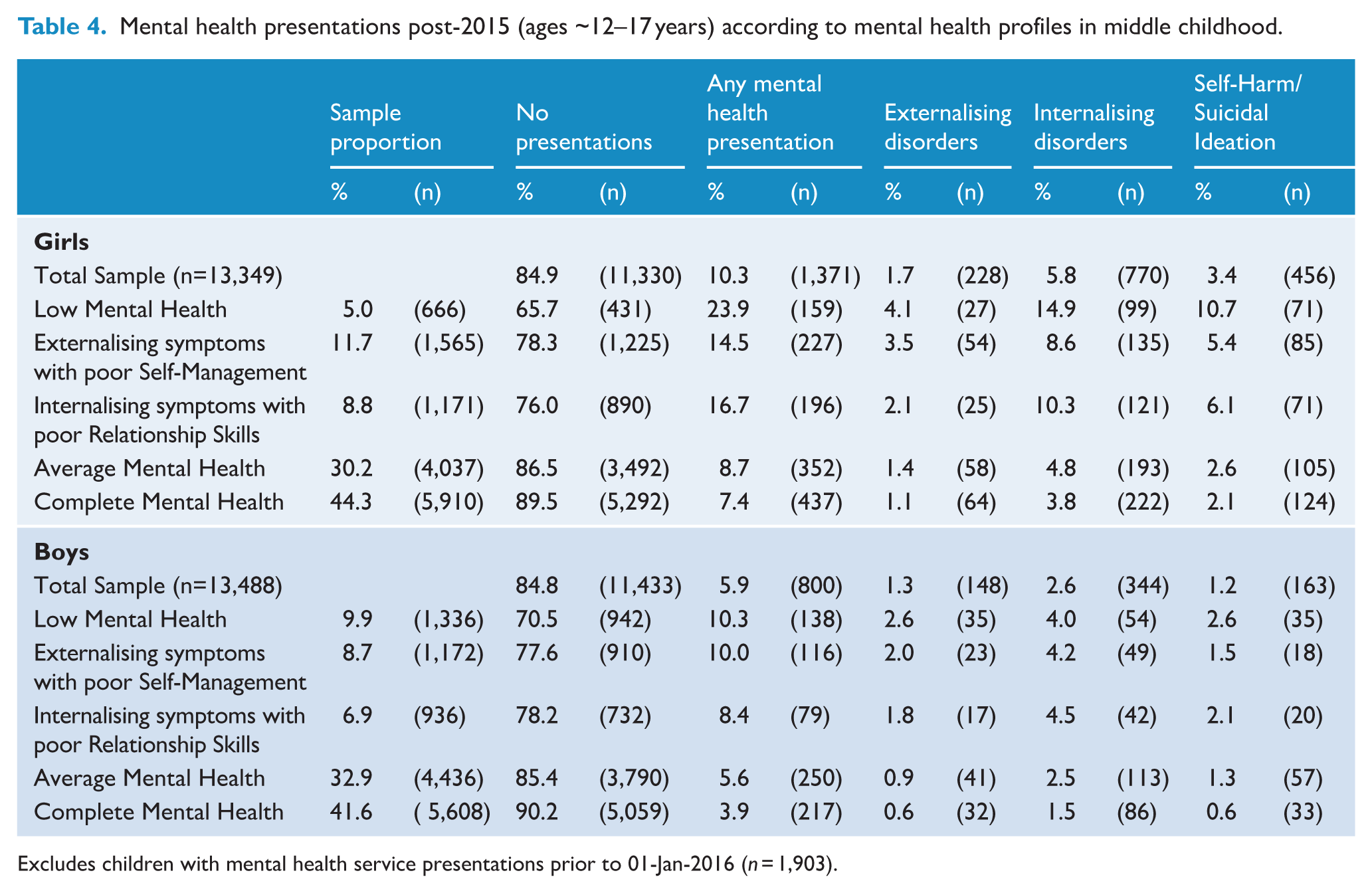
Excludes children with mental health service presentations prior to 01-Jan-2016 (
Logistic regression results for mental health presentations according to mental health profile.
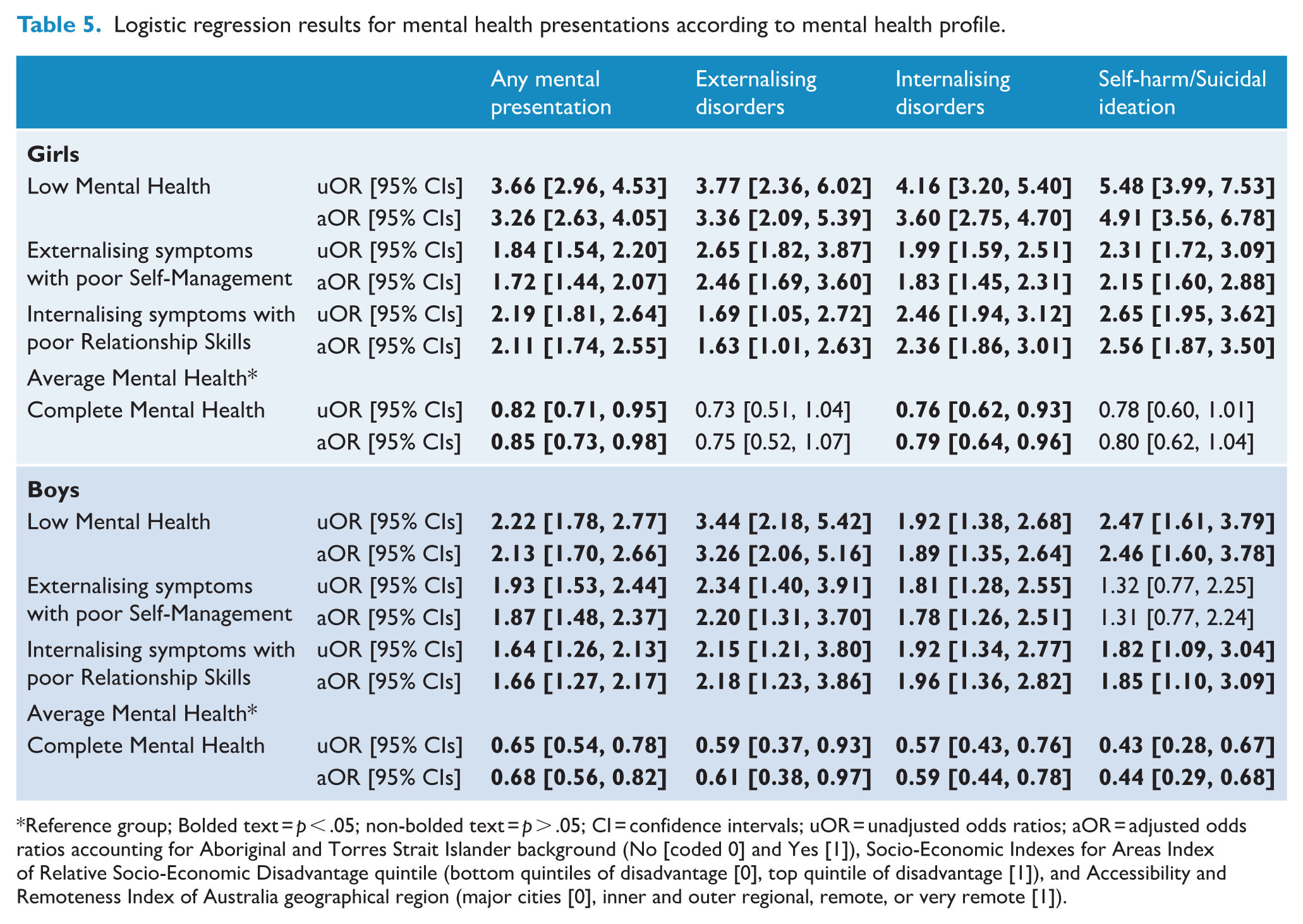
Reference group; Bolded text =
Discussion
Latent profile analyses of middle childhood (age ~11 years) social-emotional competencies and difficulties yielded a five-profile solution for girls and boys, and these profiles differentially related to health service presentations for mental disorders during adolescence (ages ~12–17 years). Between 42–44% of girls and boys were classified as demonstrating
This comprehensive exploration of patterns of middle childhood interpersonal and intrapersonal competencies and internalising and externalising psychopathology identified an
This study demonstrated longitudinal associations between middle childhood mental health profiles and adolescent mental disorders. The
A strength of this study was the use of a large, representative sample of Australian young people followed over time, but several limitations are notable. Non-significant differences in odds of mental disorders could be a result of the small number of individuals with mental disorders among some of the profiles (e.g. 1.5% of
Future longitudinal research could explore potential predictors of membership in each of the profiles, such as early childhood mental disorders, parental mental illness or adverse childhood experiences. Continued follow-up of the sample into early adulthood would capture more mental health presentations, particularly for disorders that peak in onset during adulthood (e.g. substance use, mood and personality disorders and schizophrenia; Solmi et al., 2022). Where this study was limited to self-report assessment of children’s perceived social-emotional competencies and difficulties at age ~11 years, future research could determine whether these profiles are replicated among different age groups and using teacher- and/or parent-report data.
This study demonstrates the utility of middle childhood mental health profiles that account for both social-emotional competencies and difficulties in indexing risk for mental disorders in adolescence (ages ~12–17 years). Middle childhood represents an opportune time for prevention and early intervention, prior to the difficult transition to adolescence – the peak period of onset for many mental disorders (McGrath et al., 2023; Solmi et al., 2022). Social-emotional competencies are teachable and can be promoted in schools via effective, evidence-based programming (Carpendale et al., 2025; Durlak et al., 2022). Further research is required to determine the effectiveness of these programmes for averting mental health difficulties and to inform where the provision of targeted and intensive supports – tailored to students’ social-emotional needs and emerging/established psychopathology – may be required in addition to the whole-school teaching of all competencies.
Supplemental Material
sj-docx-1-anp-10.1177_00048674261426776 – Supplemental material for Middle childhood profiles of social-emotional competencies and difficulties differentiate risk of health service presentations with adolescent mental disorders
Supplemental material, sj-docx-1-anp-10.1177_00048674261426776 for Middle childhood profiles of social-emotional competencies and difficulties differentiate risk of health service presentations with adolescent mental disorders by Emma J Carpendale, Melissa J Green, Oliver J Watkeys, Stacy Tzoumakis, Vaughan J Carr and Kristin R Laurens in Australian & New Zealand Journal of Psychiatry
Footnotes
Acknowledgements
This research used population data owned and managed by the NSW Ministry of Health, ACT Health, the Australian Coordinating Registry (on behalf of Australian Registries of Births, Deaths and Marriages, Australian Coroners and the National Coronial Information System) and the University of New South Wales. The findings and views reported are those of the authors and should not be attributed to these Departments and Agencies, or the NSW or Australian Governments. Record linkages were conducted by the NSW Centre for Health Record Linkage (CHeReL).
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was conducted by the University of New South Wales with financial support from National Health and Medical Research Council Project Grants (APP1058652 and APP1148055), an Australian Research Council Future Fellowship (FT170100294 awarded to KRL) and Discovery Early Career Researcher Award (DE210100113 awarded to ST), a Department of Health and Aged Care Medical Research Future Fund Million Minds Mental Health Grant (APP2006436) and Suicide Prevention Australia (Postdoctoral Fellowship awarded to OJW) with funding provided by the Australian Department of Health, Disability and Ageing.
Ethical approval and informed consent
Ethics approval was provided by the NSW Population and Health Services and ACT Health Human Research Ethics Committees (HREC/18/CIPHS/49).
Consent for a school to participate in the Middle Childhood Survey (MCS) was provided in online (electronic) form by the school Principal (school leader). Child recruitment for the MCS within participating schools followed a child and parent opt-out consent procedure using online forms, written instruction and verbal instruction. The use of opt-out consent procedures (for parents and children) was guided by the Australian National Health and Medical Research Council National Statement of Ethical Conduct in Human Research (chapter 2.3), which specifies conditions under which these procedures are appropriate.
Data availability statement
Data used in this project has been provided by government agencies for the research purposes of the NSW Child Development Study and are unable to be shared with third parties or deposited into data repositories. Collaborative research activities may be possible depending on scope and resources; alternatively, data can be accessed by applications to relevant data custodians.
Supplemental material
Supplemental material for this article is available online.
