Abstract
Objective:
Better Access is a major Australian Government mental health initiative that provides rebates to people experiencing mental health problems so they can access psychological services at reduced or no cost. Currently, GPs, psychiatrists, clinical psychologists, psychologists, social workers, and occupational therapists provide referrals and/or treatment services under Better Access. This study sought to consult a broad range of stakeholders and identify their collective view on future reform priorities for Better Access.
Methods:
Consultations followed a three-phase process. In Phase 1, participants completed a brief online survey to identify priority topics. In Phase 2, participants took part in an online forum where they discussed and refined topic summary statements. In Phase 3, participants rated agreement with a revised set of statements and ranked topics in a second online survey.
Results:
Ninety stakeholders participated. Collective views emphasised the need to enhance access through improving affordability for consumers and increasing workforce capacity, particularly in rural/remote areas. Participants also identified a need to review the scope and rules of the programme to better accommodate the increasing use of Better Access by people with more complex mental health needs. Views varied on the best mechanisms to address these issues.
Conclusions:
Collective views emerged on key areas for reform for Better Access. While there were varying views on the best way to address these priority areas, stakeholders concurred that the programme's capacity needed to be expanded to meet the increasing levels of community demand for mental health care.
Introduction
Better Access is a large-scale mental health programme that commenced in 2006. It enables people with diagnosed mental disorders to receive care from eligible service providers (GPs, psychiatrists, clinical psychologists, psychologists, social workers and occupational therapists) who operate from private practices. Most commonly, a GP prepares a mental health treatment plan (MHTP) for a consumer and refers them for up to 10 treatment sessions with an allied health professional, reviewing the plan after the sixth session. Clinical psychologists provide ‘psychological treatment services’, and the remaining allied health professionals provide ‘focussed psychological strategies’. Services are available face-to-face or via telehealth. GPs can also provide focussed psychological strategies.
Better Access services are listed as items on the Medicare Benefits Schedule (MBS) and attract a rebate that is paid to consumers to offset the cost. Providers can bill Medicare directly and accept the Medicare benefit as the full payment for the service (‘bulk-billing’). Alternatively, they can charge above the rebate, and the consumer pays the difference (an ‘out-of-pocket cost’). Medicare has safety net thresholds, where if a consumer spends a certain amount on Medicare services in a given year, their subsequent rebates are higher. Rebates vary by service and provider type. For example, they are higher for psychological treatment services than for focussed psychological strategies. Social worker- and occupational therapist-delivered services attract the same rebate, which is lower than that of psychologists.
In 2021, Better Access provided services to one in ten Australians. It cost the Australian Government $1213 million in benefits paid (a 4% rise per year since 2018). Out-of-pocket costs were incurred for 47% of all Better Access services in 2021 (up from 36% in 2018), and the median copayment rose sharply from $74 in 2021 to $87 (a 17.5% increase) in the first half of 2022 (Tapp et al., 2026a, 2026b).
Since its inception, there have been divergent views on the general approach and parameters of Better Access, the level and distribution of funding, and the degree to which it has met or not met its aims (Dunbar et al., 2007; Jorm, 2011, 2018; Littlefield, 2008; Papadopoulos and Maylea, 2020; Rosenberg and Hickie, 2019). Criticisms include that the maldistribution of the Better Access workforce disadvantages those living in rural/remote and socioeconomically disadvantaged areas (Byles et al., 2011; Meadows et al., 2015), and that the programme operates on a fee-for-service model and outcome data are not systematically collected to monitor it (Rosenberg and Hickie, 2019).
As part of a broader evaluation of Better Access reported in this issue of the Australian and New Zealand Journal of Psychiatry (Arya et al., 2026; Chilver et al., 2026; Harris et al., 2026; Newton et al., 2026; Pirkis et al., 2026a, 2026b; Tapp et al., 2026a, 2026b), we undertook a structured consultation process with mental health sector stakeholders, seeking input on areas of the programme where reform is most urgently required and on the shape such reform might take.
Methods
Sampling and recruitment
We sought participation from providers who were eligible and ineligible to deliver Better Access services, First Nations service providers, consumers and people with lived experience, carers, advocacy organisation representatives, health system experts, and policy-makers. Most potential participants were approached via relevant professional associations or non-government organisations, which nominated or called for expressions of interest from 2-5 representatives based on their size, reach and level of Better Access involvement. The (then) Department of Health helped us identify health system experts and policy-makers.
Data collection and analysis
Figure 1 provides details of the data collection and analysis process. We used a modified Delphi method with a three-phase design (Barnett et al., 2021). Phase 1 involved an online survey (Survey 1) where participants identified the most salient issues for Better Access going forward. The main topic areas were identified, and a set of ‘synthesis statements’ that captured these was drafted. In Phase 2, participants discussed the synthesis statements in an online forum using pseudonyms, after which they were further revised to reflect the discussion. In Phase 3, participants rated their level of agreement with the revised synthesis statements and ranked priorities for reform in a second online survey (Survey 2). Analysis focussed on the entire stakeholder group as other studies within our Better Access evaluation explored the perspectives of particular stakeholder sub-groups – e.g. consumers (Newton et al., 2026; Pirkis et al., 2026a, 2026b) and providers (Tapp et al., 2026a).
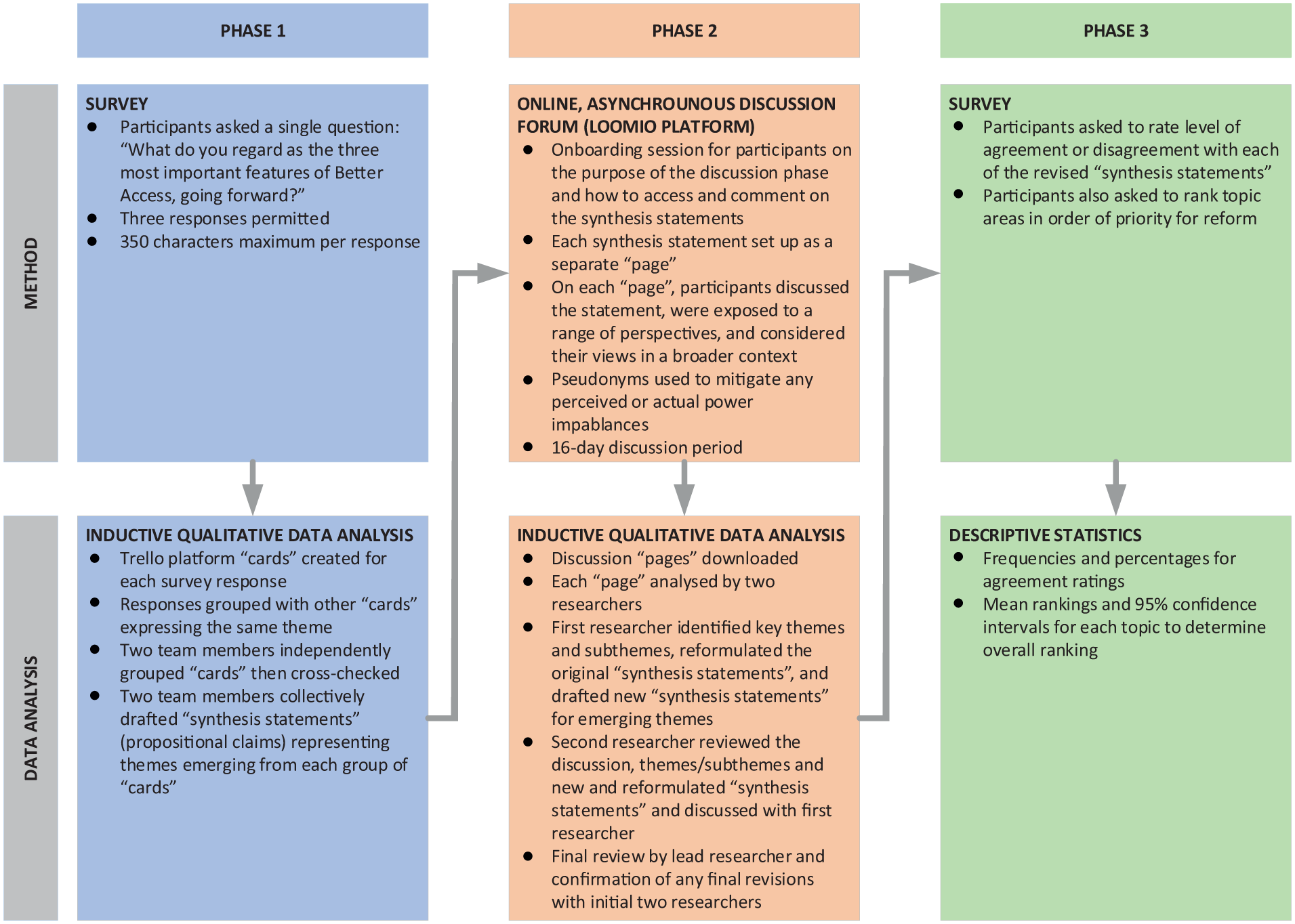
Data collection and analysis.
Study timing
The study occurred in September-October 2022, when certain COVID-19 pandemic-related modifications to Better Access were in place that have since ceased (an additional 10 sessions) or been made permanent (telehealth). Other changes to Better Access rules have occurred since the evaluation, including some recent ones relating to services delivered by GPs (e.g. the review no longer has a specific item number and can be done under a general attendance item number) (Australian Government Department of Health, Disability and Ageing, 2025).
Ethics approval
The University of Melbourne Human Research Ethics Committee approved the study (2022-24221-32180-5).
Results
Sample description
One-hundred-and-four stakeholders were nominated, and 90 consented to participate. Table 1 details participation by stakeholder group. Eighty-six per cent of study participants completed Survey 1; 76% participated in the discussion, and 86% completed Survey 2. All participants indicated their consent by checking a consent box after reading a plain language statement.
Stakeholder groups, quotas and participation numbers.
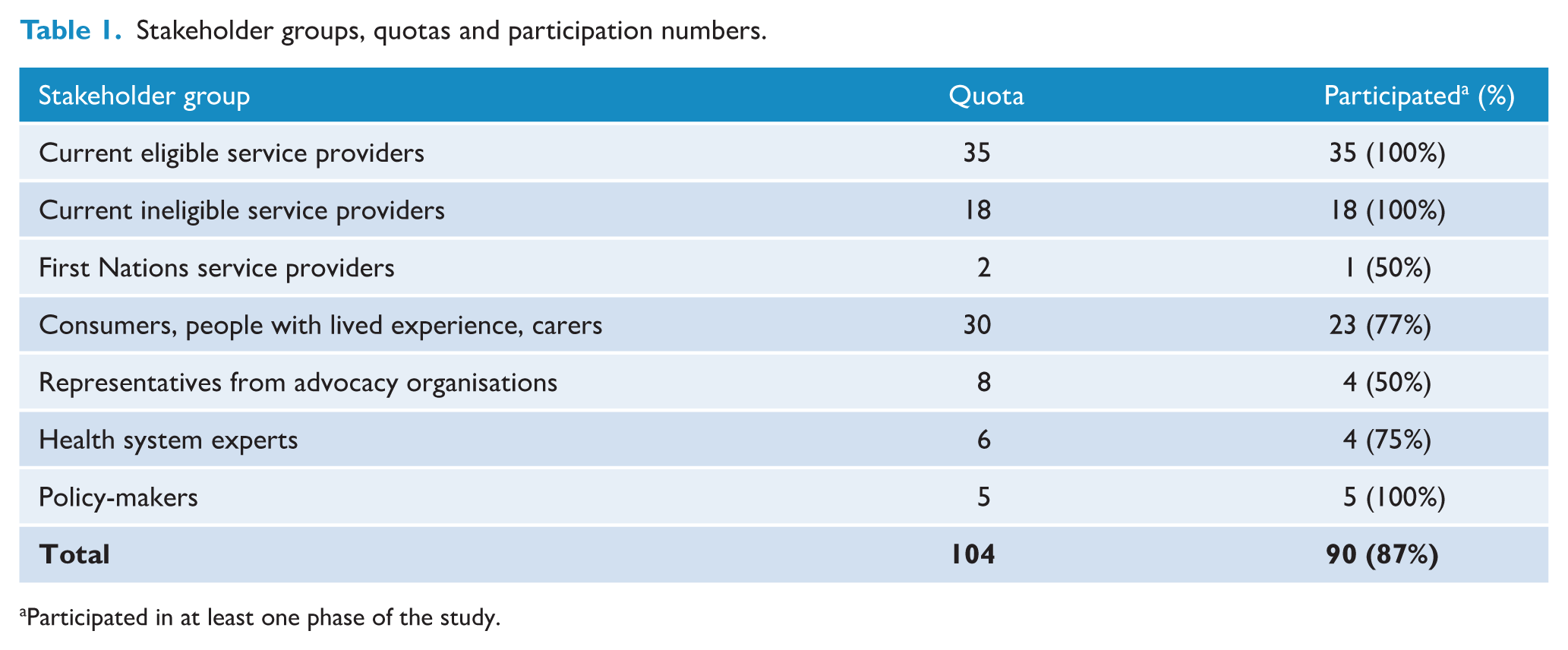
Participated in at least one phase of the study.
Topic areas and synthesis statements
In Phase 1, we derived 31 synthesis statements covering 21 topic areas, which expanded to 56 following the Phase 2 discussion. Table 2 presents the 21 topic areas (in alphabetical order) and indicates the levels of agreement/disagreement with the 56 synthesis statements. In Phase 3, participants indicated their level of agreement/disagreement with all 56 synthesis statements and ranked 18 of the 21 topic areas in order of priority for reform (two pairs of the original 21 topic areas were combined, and one was omitted as it did not address a reform target).
Participant agreement/disagreement with the final 56 synthesis statements (percentage).
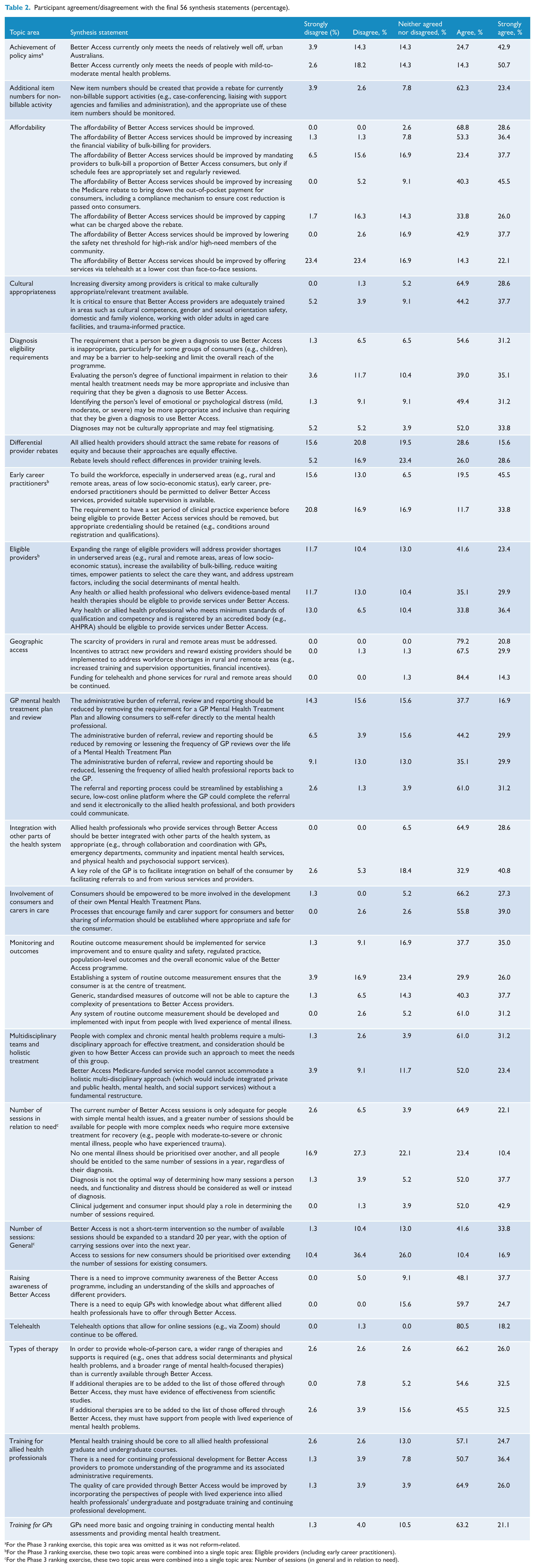
For the Phase 3 ranking exercise, this topic area was omitted as it was not reform-related.
For the Phase 3 ranking exercise, these two topic areas were combined into a single topic area: Eligible providers (including early career practitioners).
For the Phase 3 ranking exercise, these two topic areas were combined into a single topic area: Number of sessions (in general and in relation to need).
Below we provide a narrative overview of the key points of agreement and disagreement for the 18 ranked topics under four broad categories: improving Better Access for service users; expanding the scope of Better Access; current programme structures and rules; and quality improvement related activities.
Improving Better Access for service users
Affordability
There was consensus that the affordability of Better Access should be improved, but there were disparate views on how to achieve this. Suggestions that would increase affordability for consumers without impacting the financial viability of providers’ practices were particularly well endorsed, with 85% of participants supporting increases to the Medicare rebates and 81% supporting lowering the Medicare safety net threshold for high-need individuals. There was also consensus that mandating higher levels of bulk-billing would improve affordability; however, some thought these measures might detrimentally affect providers. There was some support for capping the out-of-pocket cost amount, however, concerns were expressed that caps might be anti-competitive and contravene consumer law and would probably not keep pace with inflation or service provision costs. The majority did not support improving affordability by offering telehealth as a lower-cost option, as it would position telehealth as a poorer quality offering and reduce consumer choice.
Geographic access
Addressing workforce shortages in rural/remote areas was raised as a priority for reform. Participants cautioned that this must not result in reduced quality of service and emphasised that the focus should be on growing the permanent workforce rather than encouraging short-term transient providers. Incentives to attract and retain providers were strongly supported, with suggestions including scholarships for residents and improved training/supervision opportunities for the existing regional workforce.
Cultural appropriateness
A broad range of cultural competencies was identified as desirable for Better Access providers, including gender and sexual orientation safety, domestic and family violence, working with older adults in aged care facilities, and trauma-informed practice. While almost all participants supported improving cultural competency, concerns were raised that it may not be possible for all providers to attain such competencies. Some participants expressed the view that ensuring providers are culturally competent is the responsibility of universities and other training institutions.
Raising awareness of Better Access
Gaps in awareness of Better Access among the general community and referring GPs were cited as limiting the number of consumers accessing the programme and as a barrier to providing optimal care. Awareness-raising encompassed increasing understanding about what different providers have to offer in order to better match providers’ expertise and consumers’ needs.
Involvement of consumers and families/carers in care
There was widespread support for consumers being empowered to be more involved in the development of their own MHTPs, encouraging family/carer support, and better information sharing with families/carers where safe and appropriate. To realise these goals, there were suggestions that increasing consumers’ mental health knowledge would aid them in making decisions about their care, and that introducing an MBS item number for GPs to consult with families/carers could be beneficial. There was also discussion about the need to assess family/carer involvement in light of the needs and wishes of consumers.
Expanding the scope of Better Access
Number of sessions
Participants emphasised that session number limits mean that Better Access is not ideal for people with complex needs, and most proposed that more sessions should be available. It was acknowledged, however, that Better Access was not designed to provide long-term psychosocial support for those needing lengthier or more intensive treatment for recovery. Many participants did not think diagnosis was the appropriate way to assess need and that levels of functioning and distress should be considered, and 95% of participants considered that decisions about session numbers should be based on clinical judgement and discussions with the consumer.
As noted, an additional 10 sessions per year were temporarily introduced during the pandemic. Seventy-five per cent of participants supported retaining this measure, although others observed that offering 20 sessions to all would benefit existing consumers but exacerbate access problems for new consumers.
Types of therapy
In their discussion of permissible therapies, participants emphasised the interrelatedness of mental and physical health and the influence of social determinants on both. For participants, the corollary of this was that for Better Access to provide whole-of-person care, a wider range of therapies and supports is required. Participants acknowledged that additional therapies must be evidence-based, although there were different views about what constituted evidence, with some emphasising scientific evidence and others preferencing the views of people with lived experience about what works.
Eligible providers
Two-thirds of participants considered that expanding the range of eligible providers would increase accessibility and increase consumers’ choices. Others argued that expanding Better Access to include providers without foundational mental health training would be inappropriate. Credentialing and appropriate oversight from registering bodies were seen as essential for ensuring practitioners meet minimum standards for quality practice.
The majority of participants supported including early-career practitioners as eligible providers to address workforce shortages, but thought that this should be done cautiously, noting significant risks. Permitting early-career practitioners to deliver Better Access as a workforce solution in regional and underserved communities raised concerns about those communities being staffed by underqualified practitioners, a transient workforce, and service quality issues.
Multidisciplinary teams and holistic treatment
It was generally acknowledged that Better Access is increasingly serving people with complex needs that are only likely to be met by multidisciplinary teams. Participants discussed the kinds of providers needed for multidisciplinary teams, and how such teams might operate and be recompensed. Peer workers were promoted, as were additional MBS item numbers to expand options for conferencing and care coordination, additional training for providers, and shared care between Better Access providers and public sector providers. There were concerns that a multidisciplinary approach could not be accommodated within the current Better Access service model, with three-quarters of participants agreeing that a major programme restructure or alternative models of care would be required.
Integration with other parts of the health system
Improved integration of Better Access with other parts of the health system was raised as a priority. Most participants believed that GPs had a pivotal role to play in supporting integration by facilitating referrals to and from other services and providers. Barriers to establishing new systems and processes of integration were recognised, including issues of privacy and informed consent. It was also noted that better integration would require financial investment and the development of overarching, cross-service platforms.
Telehealth
There was almost universal support for the continuation of telehealth sessions, although some participants cautioned that telehealth should be seen as an adjunct to, not a replacement for, face-to-face care.
Current programme structures and rules
Diagnosis eligibility requirements
It was generally considered that the requirement that people have a diagnosed mental disorder to be able to access Better Access was inappropriate and created barriers. Many believed that diagnoses could be culturally inappropriate, stigmatising and/or overly pathologising. Some suggested that a focus on emotional or psychological distress or functional impairment was preferable. Participants believed that treating providers should be able make their own assessment of consumers’ need for Better Access care. Despite these concerns, some participants expressed reservations about removing the diagnosis requirement and considered that some criteria should remain in place to ensure that Better Access did not become a panacea for all things related to mental health in lieu of other services and supports that may be more appropriate.
GP mental health treatment plan and review
Many participants recognised communication and collaboration between GPs and allied health professionals as important. However, there was little support for the current MHTP preparation and review arrangements as the best mechanism for achieving this. Perceived shortcomings included doubts about GPs’ ability to diagnose mental health problems, variable plan quality, and consumer difficulty accessing GPs. Many thought that a simple GP referral would be sufficient or that consumers should have the option of self-referral, although risks were identified with the latter, including a potential conflict of interest for allied health professionals when determining consumer eligibility. The GP review process was described as overly burdensome for consumers and providers, an administrative hurdle with little clinical value, and doing little to facilitate collaborative care between GPs and other providers.
Differential provider rebates
There was no majority view on the proposition that allied health professionals should attract the same rebate, and just over half the participants considered that rebate levels should reflect differences in provider training. Those favouring the same rebate for all said that the differential rebates were outdated, divisive, unjust, not reflective of evidence of differences in provider effectiveness, and based on a false distinction between focussed psychological strategies and psychological therapy services. Those favouring differential rebates believed that there should be a financial acknowledgement of advanced training and competencies, and that without this, there would be a disincentive for new practitioners to complete higher-level training.
Additional item numbers for non-billable activity
There was general agreement that non-billable work was a considerable burden on providers, particularly for complex cases. Participants considered that where additional work was required, it should be recompensed, although concerns were expressed that such item numbers might be open to rorting and that compliance checking or auditing would be required.
Quality improvement-related activities
Monitoring and outcomes
Approximately 75% of participants indicated that they valued routine monitoring and outcome measurement for service improvement, but fewer agreed that routine outcome measurement ensured the consumer was at the centre of treatment. In general, participants considered it important that the purpose of both monitoring and outcome measurement be clearly articulated (e.g. service improvement, accountability in terms of government spending, and providing feedback to providers on how consumers were progressing). Participants raised concerns about the feasibility of introducing routine outcome measurement, identifying additional burden for providers and technical issues.
Training for allied health professionals
Continuing professional development around Better Access was considered by most as helpful. There was support for including mental health training in undergraduate and graduate allied health programmes, although some considered investing in postgraduate mental health training for those pursuing clinical careers preferable. There was strong agreement on the value of incorporating the perspectives of people with lived experience into training and continuing education.
Training for GPs
Eighty-four per cent of participants considered that GPs needed more training in mental health assessment and treatment. However, participants also acknowledged that the current training GPs undertake to access higher rebates for preparing MHTPs was useful. Some participants considered that regular professional development in mental health should be mandatory, while others indicated that this would not be feasible given the range of presenting issues managed by GPs.
Ranking of priorities for reform
Figure 2 shows the overall ranking, based on mean rank, of priorities for reform. The top three priorities concerned improving access to Better Access for service users: affordability, involvement of consumers and carers in care, and geographic access. Topics related to the scope and delivery modes of Better Access were the next most highly ranked (4-11), followed by rules and processes (12-15) and quality improvement topics ranked lowest (16-18).
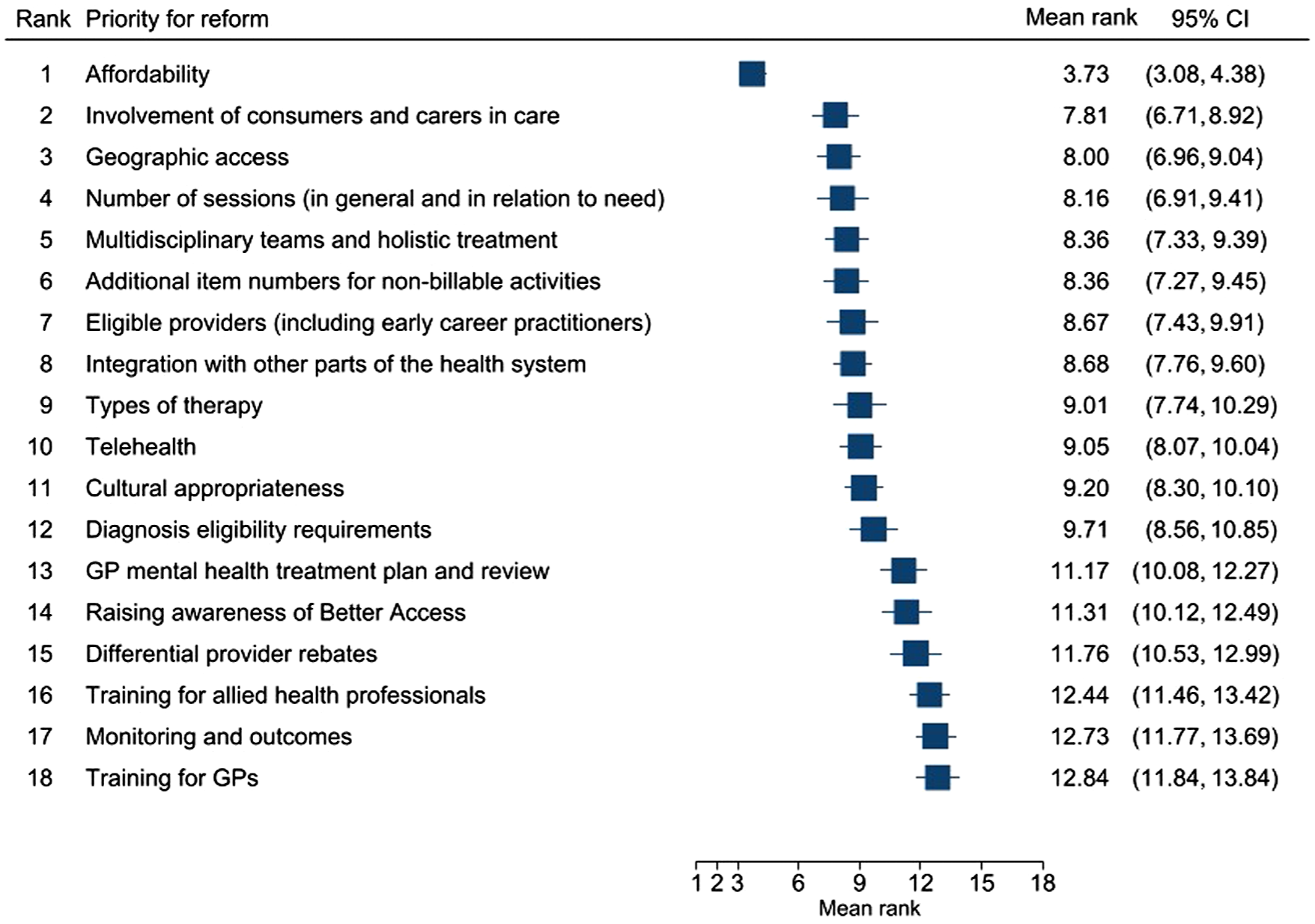
Priorities for reform by mean ranking.
Discussion
This study aimed to glean a collective view from stakeholders across the mental health sector on reform priorities for Better Access. As would be expected, there was diversity in the views expressed, but there was broad agreement on a number of reform priorities, and many of the divergent views related to specific mechanisms through which these priorities might be achieved.
Consistent with findings from Better Access consumer and provider studies conducted as part of our Better Access evaluation (Newton et al., 2026; Pirkis et al., 2026a, 2026b; Tapp et al., 2026a), there was a collective view that it is increasingly difficult for consumers to access Better Access, particularly those with relatively fewer economic resources and those in rural/remote areas. There was consensus that addressing affordability and geographic access was important to maintain the intent of the programme and for equity reasons. Affordability was ranked as the number one priority. Although Better Access has greatly increased access to mental health treatment across the population, inequality in access is a long-standing issue (Byles et al., 2011; Meadows et al., 2015). A number of reforms mooted by participants potentially address these issues, including proposals for higher rebates, bulk-billing incentives, and expanding the range of eligible providers and types of permissible therapies. However, there was no consensus on these approaches; all attracted dissenting views and concerns.
There has been criticism of the escalating cost to the government of Better Access (Rosenberg and Hickie, 2019), but participants in this study collectively considered that the scope of Better Access required expansion, particularly because consumers with complex needs are increasingly using Better Access. Better Access was originally designed to provide short-term care for people experiencing mild-to-moderate mental illness, and, in isolation, the model of care is not optimal for those with more complex needs. There were suggestions about how to make Better Access more comprehensive, as well as cautions about expecting Better Access to be the sole avenue for publicly-funded mental health care. Some commentators have suggested that the fee-for-service model of Better Access may itself need reconsidering, and that blended funding or other options may be more suitable for providing multidisciplinary, holistic care (Rosenberg and Hickie, 2019). However, our participants strongly advocated for reforming the existing Better Access programme to better accommodate the expanded needs of those seeking treatment.
In terms of programme rules and processes, there was a collective view that basing eligibility on a mental illness diagnosis was undesirable and that session number limits were incompatible with best practice. Providers who completed a survey in a complementary part of our evaluation also strongly endorsed this view (Tapp et al., 2026a). Forum participants also broadly concurred that the current Better Access referral and review processes need improvement. Overall, participants agreed that GPs had an important role in the programme, but there were different views on the ideal scope of that role, ranging from providing a simple referral to continuing to complete MHTPs, to acting as de facto care coordinators. It is not clear whether the fact that GPs can now undertake reviews using general attendance item numbers (Australian Government Department of Health Disability and Ageing, 2025) would address any of these issues.
Many participants indicated that, in principle, routine outcome measurement could provide useful data for quality improvement of Better Access. However, it was not universally endorsed and was ranked as the second to last priority. Concerns were expressed about the practicalities of implementation, relevance and utility for clinical practice, and the potential use of data for compliance monitoring. There are precedents for routine outcome measurement elsewhere in the Australian mental health sector, including in specialist mental health inpatient and community services (Australian Mental Health Outcomes and Classification Network, 2022) and primary mental health care (Australian Government Department of Health, 2022). Implementing routine outcome measurement at scale in a system where providers operate individually is likely more difficult.
Finally, there was a collective view across multiple priority areas that consumers should be more involved in their own care and that the voice of people with lived experience should be included in programme reform initiatives. People with lived experience interviewed in another component of our Better Access evaluation shared this view (Newton et al., 2026). Although forum participants expressed support for these general principles, they did not offer suggestions for how they might be achieved. Resources and strategies for inclusive programme design and delivery are increasingly available (Arblaster et al., 2023).
Strengths and limitations
Strengths of this study were the large number of stakeholders with different relationships to Better Access, high participation rates, a study design that allowed collective views to emerge while accommodating dissenting views, and the use of pseudonyms in the discussion to encourage participation and mitigate power imbalances. Limitations included the predominance of service provider stakeholders. This was necessary and desirable to accommodate both eligible and ineligible provider groups, but may have over-emphasised the technical and administrative aspects of Better Access. There was also potential for the most engaged participants to dominate and disproportionately influence the discussion, although the three-phase design and the analysis methods likely attenuated this. Only one Aboriginal and Torres Strait Islander Service Provider Organisation was represented.
Conclusions
We explored the views of 90 stakeholders with involvement in, or knowledge of, Better Access and/or the broader mental health system. Collective views emerged on several areas for future reform, emphasising the need to improve access through making the programme more affordable to consumers and increasing workforce capacity, particularly in rural/remote areas. There was also a focus on the scope and rules of the programme, often in the context that Better Access now increasingly serves people with more complex mental health needs, and the original design and rules are not optimal to meet their needs. While there were varying views on how to address these priorities, stakeholders concurred that the programme's capacity needed to be expanded to meet increasing levels of community demand for mental health care.
Footnotes
Acknowledgements
This study was funded by the Australian Government Department of Health, Disability and Ageing as part of the broader evaluation of Better Access. We would like to thank the two groups that were constituted to advise on the evaluation, the Clinical Advisory Group and the Stakeholder Engagement Group.
We would like to acknowledge stakeholder organisations for assisting with recruitment and participants for their time and contribution.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclose receipt of the following financial support for the research, authorship, and/or publication of this article: The evaluation of Better Access was funded by the Australian Government Department of Health, Disability and Ageing.
ORCID iDs
Data Accessibility Statement
The datasets generated and analysed for the current study are not available.
