Abstract
Objectives:
Data from a longitudinal national cohort study was used to test associations between young caregiving and self-harming and suicidal behaviours.
Methods:
We used data from Waves 6–8 (2014–2018) of the Longitudinal Study of Australian Children to assess the effect of ‘core’ caregiving activities (e.g. personal care, assistance moving around) on suicidal and self-harming behaviours. Care activities at 16–17 years were classified as core caregiving, non-core caregiving and no caregiving. Five self-harming and suicidal measures, collected at age 18/19 years, were used to form two outcomes: thoughts (of self-harm or suicide, or plan to suicide) and behaviours (self-harm, suicide attempt), operationalised as binary variables. Analyses were carried out using augmented inverse probability treatment weighting, adjusting for potential confounders, on complete case data.
Results:
Core caregiving was associated with higher levels of suicidal and self-harming behaviours compared no caregiving, with an average treatment effect (ATE) of 0.07 (95% confidence interval [CI] = 0.02, 0.12), equating to a risk ratio of 1.86 (95% CI = [1.21, 2.45]). The ATE of core caregiving on thoughts of suicide or self-harm (compared to non-caregiving) was 0.05 (95% CI = [−0.00, 0.11]), equating to a risk ratio of 1.26 (95% CI = [0.97, 1.56]). There was no evidence of an association between non-core care and any outcomes tested. Sensitivity analyses confirmed main findings.
Discussion:
Core caregiving is associated with elevated risks of self-harm among young carers, underlining the crucial need to better identify and support young carers to mitigate these adverse outcomes.
Introduction
Young carers provide unpaid care to someone else, usually a family member with a disability, chronic or mental illness, or older person with care needs (Becker, 2007; Leu et al., 2022). Despite their significant contributions to social care needs, young carers are under-recognised by society, often delivering care with little support.
Who are young carers and what do they do?
Young carers are commonly considered to be young people aged 18 years and under who provide unpaid care (Becker, 2007). Pre-COVID estimates place the proportion of young carers in high income countries in the range of 5% to 10% of young people: 6.1% in Germany (Metzing-Blau and Schnepp, 2008), 7% in England (Joseph et al., 2019) and 7.9% in Switzerland (Leu et al., 2018). In Australia, the 2016 census found that 5.1% of those aged 15–19 years were young carers (Australian Bureau of Statistics, 2018) although this is considered an underestimate, with a recent nationally representative school-based study finding that 9% of children aged 8–14 years reported some care responsibilities (Hamilton and Redmond, 2019).
Young carers most commonly provide care to a parent (Cass et al., 2009), however care recipients may also be siblings, or other persons with a disability, chronic illness, poor mental health, a substance use disorder, or frailty due to old age. The tasks that young carers undertake vary in type, frequency and intensity. Becker proposed a ‘continuum’ upon which caregiving by children could be placed, with the activities that most young people carry out at the light end, and the activities of young carers at the high/intensive end (Becker, 2007). Activities at the intensive end of the continuum may be time intensive, regular, and often involve more intimate and personal care tasks, as well as other tasks such as shopping and housework (Becker, 2007). Another way of capturing care intensity is in terms of ‘core’ and ‘non-core’ domains (Australian Bureau of Statistics, 2016). Core domains include personal care (e.g. washing, dressing, eating, toileting), moving around (e.g. getting in/out of bed), and communicating, while non-core domains include health care (e.g. giving medication), transport (e.g. catching buses, trains), preparation of meals, housework, shopping, errands; house repairs or garden care; paperwork; and keeping company (Australian Bureau of Statistics, 2016).
Adverse outcomes of caregiving
Informal caregiving is associated with adverse outcomes among adults, including increased cardiovascular disease (Lambrias et al., 2023), poorer mental health (Ervin et al., 2022; King et al., 2024), poorer physical health outcomes, elevated stress hormones, and impaired immune responses (Vitaliano et al., 2003). While less research has investigated the health impacts of informal caregiving among young carers, there is growing evidence indicating adverse associations for this group. A census-based record linkage study in Northern Ireland found young carers had significantly higher mortality and poorer mental health than their peers (Tseliou et al., 2018). In Australia, a prospective study found young carers had poorer mental health than their non-caregiving peers, with this association evident 4 years after reporting their caregiving status (King et al., 2021). A longitudinal Australian study using 20 years of data found that young caring was associated with poorer mental health, particularly for those providing more than 20 hours/week of care (Fleitas Alfonzo et al., 2024). Two recent systematic reviews have also reported evidence that young carers are at increased risk of poorer mental (Fleitas Alfonzo et al., 2022; Lacey et al., 2022) and physical health (Lacey et al., 2022) than non-caregiving peers.
Poor mental health is a known risk factor for suicide ideation and behaviours (Arsenault-Lapierre et al., 2004; Li et al., 2011; Ribeiro et al., 2018). Therefore, it is plausible that informal carers may also have higher rates of suicide ideation than non-carers. Noting substantial variation in associations, studies have reported evidence of associations between caregiving and suicidal ideation among adult carers (O’Dwyer et al., 2016, 2021). In the United Kingdom, adolescents aged 17 years who were young carers in 2018-2019 had higher rates of suicide attempt 2–3 years later (Nakanishi et al., 2022).
Suicide and self-harming thoughts and behaviours
Suicide and self-harm are key public health issues among adolescents (AIHW, 2023). The number of adolescents who think about self-harm or suicide significantly outnumbers those who go on to self-harm or attempt suicide (Hawton et al., 2002), leading to recognition of the importance of distinguishing between thoughts/ideation and behaviour (O’Connor et al., 2012). While most people expressing suicidal ideation do not attempt suicide, suicidal ideation is known to significantly increase risk of suicide (McHugh et al., 2019). For example, evidence using Northern Ireland registry data found greater risk of future self-harm and repeat presentation among those presenting to hospital with suicidal ideation (Griffin et al., 2020). The integrated motivational theory (IMV) (O’Connor, 2011; O’Connor and Kirtley, 2018) provides a theoretical framework for considering the distinct factors associated with each of these (thoughts/ideation and behaviours). The IMV model defines three phases across which suicidal behaviour may develop. In the pre-motivational phase, different background factors or certain life events set the context in which suicidal behaviour may arise. These factors lead to the motivational stage, in which the individual’s appraisal of circumstances and events–in particular appraisals of defeat and humiliation, and a sense of entrapment or no escape – can lead to thoughts and intentions to end one’s life. A series of volitional moderators are proposed to influence the extent to which thoughts and intent in the motivational stage proceed to behaviour (O’Connor et al., 2012; O’Connor and Kirtley, 2018). Experiences as a young carer may determine the extent to which individuals move beyond the motivational phase and to the volitional stage. For example, it is possible that for young carers, the perception of entrapment could support progression to the volitional stage. Alternatively, capability and access to means are key factors determining volitional moderators (O’Connor and Kirtley, 2018), and given that many young carers have adult responsibilities, it is possible that their capability for suicide and access to means are different to non-carers.
This study
Despite adverse associations observed between caregiving and health outcomes, very little is known about self-harming and suicidal behaviours among young carers. This study aimed to address these gaps in young carer research and compare the suicide and self-harming thoughts and behaviours of young carers to those of non-caregiving peers. It aimed to do this using a large cohort study and methods that account for bias due to confounding and maximise causal inference. Given that more intensive care is associated with poorer mental health outcomes (Fleitas Alfonzo et al., 2024; King et al., 2021), we sought to capture caregiving intensity. As ‘core’ care typically aligns with more intensive caregiving and is a common way of assessing caregiving demands in Australia, we operationalised caregiving by the extent to which it involved core or non-core tasks, with the following categories: ‘no caregiving’, ‘non-core caregiving’ and ‘core caregiving’.
Methods
Reporting of this study adhered to the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement.
Data Set
We drew on data from the Longitudinal Study of Australian Children (LSAC). LSAC is an ongoing cohort study that has been conducted since 2004 among two cohorts of children: Cohort B (birth cohort) aged 0–1 year at study commencement, and Cohort K (kindergarten) aged 4–5 years at study commencement (Soloff et al., 2005). Data collection has occurred biennially since 2004. Due to the collection of variables at specific ages, for this analysis we drew on Cohort K, Waves 6 (2014, aged 14–15 years) to Wave 8 (2018, aged 18–19 years); with the exposure (caregiving) measured in Wave 7, outcome (suicide and self-harming outcomes) measured in Wave 8, and covariates measured in Wave 6. We note that while an additional two waves of data collection have occurred beyond Wave 8, these two waves (Wave 9 C1 and 9 C2) did not collect information on self-harming and suicidal behaviours, thus the current analysis uses data from Waves 6–8.
The LSAC sampling approach has been documented elsewhere (Soloff et al., 2005) but involved sampling postcodes first, and then children within those postcodes were randomly selected using the Medicare Australia database (which captures 98% of Australian children). Data collected by LSAC are comprehensive across domains such as demographics; relationships; education; behaviour; development; and social, health, housing and financial characteristics. Data were collected from study children, as well as parents/carers and teachers. Wave 1 achieved a response rate of 50.4% (n = 4993, Cohort K) (Soloff et al., 2005), with strong retention for subsequent waves, noting some non-random attrition: 89.6% of the original sample in Wave 2, to 62.0% in Wave 7 and 49.4% in the latest wave (Wave 9 C2) (Australian Bureau of Statistics LSAC processing team and the Australian Bureau of Statistics Household Survey Methodology Team, 2022).
Variables
Exposure
We classified care in terms of ‘core activities’, adopting the Australian Bureau of Statistics (2016) definition whereby core activities are typically more intensive and may include personal care, assisting with communication and moving the person around (Warren and Edwards, 2016). Participants were asked whether they provided help to someone with a long-term health condition, a disability or who is elderly, with activities they would have trouble doing on their own. They were instructed to only consider ‘help you have given or are likely to give for at least 6 months’ and exclude paid or volunteer work.
Those providing care were then asked to indicate which of a range of care roles they engaged in. Core activities included personal care (e.g. washing, dressing, eating, toileting), moving around (e.g. getting in/out of bed), and communicating, while non-core caregiving roles included health care, transport, preparation of meals, housework, shopping, errands; house repairs or garden care; paperwork; and keeping company. We derived a three-category caregiving variable based on whether participants engaged in no caregiving, non-core caregiving and core caregiving activities. These categories were mutually exclusive, and those providing core care were categorised in the ‘core care’ category, irrespective of whether or not they also provided non-core care.
Outcomes: self-harming and suicidal thoughts and behaviours
Outcome variables were derived from a series of questions from Wave 8 on suicidal and self-harming thoughts and behaviours over the past 12 months. Respondents were asked whether they had (1) considered suicide (consider suicide), (2) made a plan to attempt suicide (suicide plan), (3) attempted suicide (suicide attempt), (4) considered harming themselves (thought about self-harm); (5) self-harmed. In main models, responses were aggregated into two binary (yes/no) variables: (1) thoughts of suicide and self-harm (thought about self-harm or considered or planned suicide) and (2) behaviours (self-harmed or attempted suicide).
Covariates
We identified several covariates that could be potential prior causes of both caregiving and suicidal/self-harming behaviours. Specifically, the following variables could be considered confounders of the association between caregiving and self-harming and suicidal behaviours: gross household income (quintiled, based on the sample distribution); presence of someone with a disability/health condition in the household (no one with a disability/health condition, one or more people in household with disability or health condition); gender (male, female); household type (single parent; two parent household); number of siblings in household (continuous). Models also adjusted for parental country of birth, with three mutually exclusive categories: (1) both parents born in Australia; (2) one or more parents born in an English-speaking country; (3) one or more parents born in a non-English-speaking country (if a participant had one parent born in an English-speaking country, and one born in a non-English-speaking country, they were included in category 3). Parental educational attainment was also included as a confounder using the highest level of education of the primary parent respondent (primarily the respondent’s mother), with the following categories: did not complete Year 12, Year 12, certificate/trade, diploma, Bachelor’s degree or higher. See Supplementary Material S1 for information on the selection of covariates.
Missing data
The eligible sample was defined as those participating in Wave 7 of data collection with complete caregiving information (n = 2896, see Figure S1 in Supplementary Material). Of these, a total of 564 participants did not have complete data on the outcome measures, and a further n = 243 were missing information on one or more covariates, resulting in n = 2089 respondents with complete data on core caregiving, suicide and self-harming outcomes and covariates. Main analysis was conducted on the complete data set.
Imputation
While the main analysis was carried out on the complete data set, sensitivity analysis was conducted on an imputed data set. To obtain the imputed data set, we carried out multiple imputation (MI) using chained equations with 100 imputations. See Additional Material in Supplementary Material regarding variables, including choice of auxiliary variables.
Statistical analysis
Analysis utilised covariates measured in Wave 6, the exposure (caring) measured in Wave 7 (aged 16/17 years), and the outcome (suicidal behaviours) drawn from Wave 8 (aged 18/19 years). The selection of waves for data analysis was determined by the fact that suicidal behaviours were not measured in Wave 9.
Augmented inverse probability weighting (AIPW) methods were applied to estimate the risk differences or average treatment effects (ATE) of being a ‘core’ carer (‘treatment’) on suicide and self-harm outcomes (Funk et al., 2011). AIPW is a robust statistical method that optimises causal inference by addressing some of the key biases related to the use of observational data such as selection bias, confounding bias, as well as bias due to missing data or model mis-specification. It applies counterfactual reasoning to estimate what would have happened under alternative treatment scenarios and does this by combining two approaches to estimate causal effects from observational data: inverse probability weighting (IPW) and outcome regression modelling.
AIPW mimics the random treatment assignment of randomised controlled trials to correct for systematic differences between treated and untreated groups. To do this, it generates a pseudo-population where every respondent is exposed to each treatment group – that is, exposed (core carer or non-core carer), and unexposed (non-carer). This ensures that the effect of confounders on the exposure (caregiving) is blocked.
The AIPW estimation process involves first fitting a propensity score model by estimating the probability of treatment assignment conditional on Wave 6 characteristics. This is followed by fitting logistic regression models that estimate the outcomes (self-harm and suicide-related thoughts and behaviours), under all treatment conditions, weighting each outcome by the score derived in the propensity score model (Kurz, 2022). This provides an estimate of the effect of the exposure that can be interpreted as if all adolescents in the sample appear as both core carers and non-core carers. The AIPW estimator has a ‘doubly robust’ property, meaning that results are robust if one of the two fitted regression models is correctly specified (Funk et al., 2011; Kurz, 2022).
We estimated the potential outcome means (POMs) for each treatment group (non-carer, non-core carers and core carers), as well as the risk ratio. All analyses were conducted in Stata/SE version 16, using the teffects command (see StataCorp LLC manual for full details of the estimation procedure) (StataCorp, 2019), with the parameters of the outcome model estimated by the default maximum likelihood. Both the outcome and the treatment models were adjusted for the listed covariates, with main analysis conducted on the complete case sample (n = 2089) data. Risk ratios were calculated with the post-estimation lincom command.
Given that the provision of care is highly gendered among adults (International Labour Organization, 2018), we tested for interaction between gender and care on all outcomes and found no evidence of interaction for any outcomes. Longitudinal sample weights were applied to models to reduce risk of bias due to non-response and survey design.
Sensitivity analysis
Several sets of sensitivity analyses were conducted to assess the robustness of our findings. First, we ran models on an imputed data set. Second, we carried out logistic regression analyses. AIPW methods are robust methods but are computationally intensive and come with key assumptions including the assumption of exchangeability and no unobserved confounding, as well as the stable unit treatment value assumption that assumes that the treatment of one individual respondent does not affect the outcomes of others. We therefore also carried out analyses applying logistic regression models. These models also enabled us to model both the aggregated outcomes (as in main analyses) as well as each (non-aggregated) outcome measure. Third, we ran logistic regression models with a binary caregiving variable (no care vs any care). Fourth, we assessed cross-sectional associations between exposure and outcomes, and fifth, we carried out analyses with adjustment for baseline (Wave 6) outcomes.
Ethics approval
Ethics approval for this analysis was granted by the University of Melbourne Human Research Ethics Committee (#20333). The Longitudinal Study of Australian Children (LSAC) was approved by the Australian Institute of Family Studies Ethics Committee, a Human Research Ethics Committee registered with the National Health and Medical Research Council (NHMRC). LSAC meets the ethical standards outlined in the National Statement on Ethical Conduct in Research Involving Humans, and conforms with the ethical requirements defined in the Declaration of Helsinki. Written informed consent was obtained from all participants. Parental consent was obtained for children/adolescents aged under 18 years and verbal consent was obtained from study children/adolescents.
Results
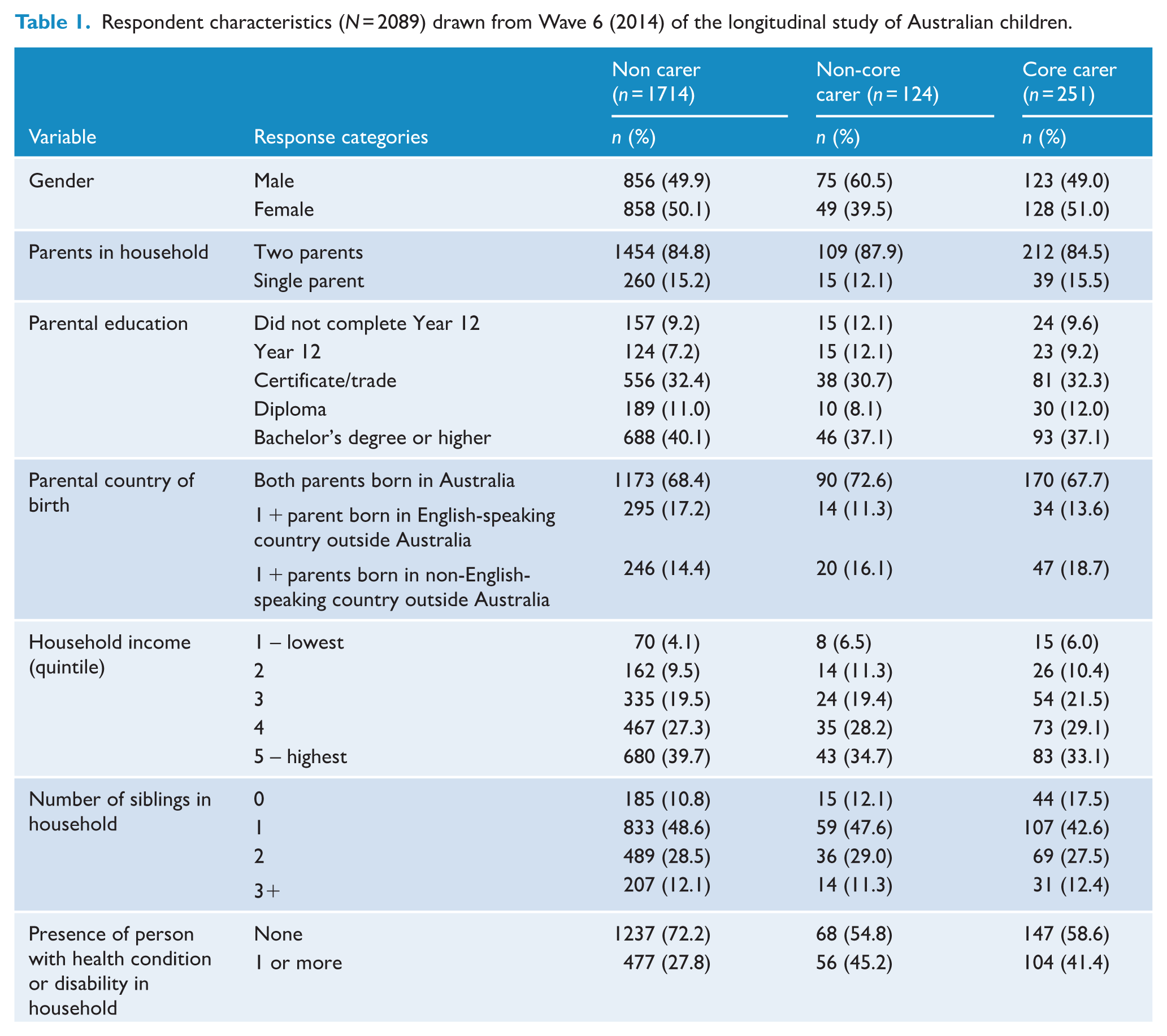
Sample descriptive statistics are presented in Table 1. A higher proportion of non-core carers were males. Most participants lived in two parent households, with a slightly higher proportion of non-core carers living with two parents (87.9%). Parental education was slightly lower for non-core carers relative to the other groups; almost one quarter (24.2%) of non-core carers did not have a parent who completed Year 12, compared to 16.4% of non-carers and 18.8% of core carers. Relative to non-carers, a higher proportion of core carers had at least one parent born in a non-English-speaking country. Relative to the other care categories, a higher proportion of core carers had no siblings in the house (17.5%, compared to 10.8% and 12.1%). A higher proportion of non-carers were living in households in the highest income quintile (39.7%, relative to 34.7% and 33.1% for non-core and core carers, respectively); and households where there was no one with a disability/health condition (72.2% compared to 54.8% and 58.6% for non-core and core carers, respectively).
Respondent characteristics (N = 2089) drawn from Wave 6 (2014) of the longitudinal study of Australian children.
The outcome measures of self-harm and suicidal thoughts and behaviours are presented in Table 2. Looking first at the aggregate measures, a higher proportion of those providing core care reported thoughts of self-harm or suicide (26.3% compared to 19.4% of non-core carers and 19.8% of non-carers) and behaviours (15.1% compared to 8.1% of non-carers and 12.1% of non-core carers).
Proportion of respondents reporting suicidal and self-harming outcomes in 2018 (N = 2089).
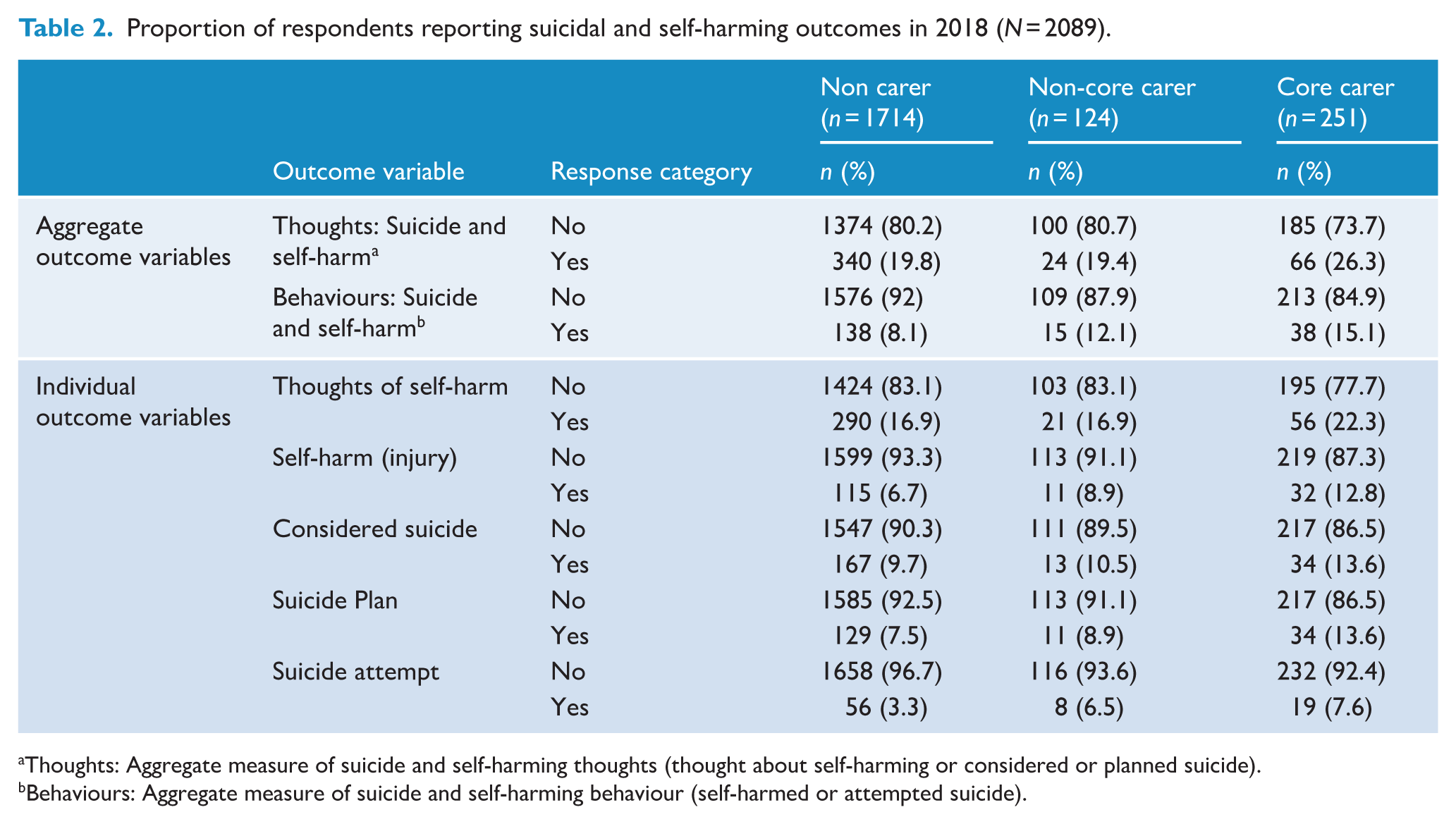
Thoughts: Aggregate measure of suicide and self-harming thoughts (thought about self-harming or considered or planned suicide).
Behaviours: Aggregate measure of suicide and self-harming behaviour (self-harmed or attempted suicide).
In terms of the single outcome measures (tested in supplementary analyses), a higher proportion of core and non-core carers reported a previous suicide attempt (7.6% and 6.5%, respectively, compared to 3.3% for non-carers). Investigation of other specific outcome measures consistently showed that a higher proportion of core carers reported thoughts of self-harm, self-harm injury, thoughts of suicide and making a suicide plan, while non-carers and non-core carers did not differ substantially on these measures.
Table 3 presents the marginal potential outcome means (POMs), ATEs (average treatment effects) and risk ratios for self-harm and suicidal thoughts and behaviours for core carers, non-core carers and non-carers. Compared to non-carers, a higher proportion of those providing core caregiving at age 16–17 years reported suicide and self-harming behaviours (suicide attempt and self-harm) at age 18–19 years, ATE = 0.07 (95% confidence interval [CI] = 0.02, 0.12). Calculated on the relative scale, this equates to a risk ratio of 1.86 (95% CI = [1.21, 2.45]). There was some evidence of increased suicide and self-harming thoughts among those providing core caregiving (compared to non-carers), however this was not statistically significant (risk ratio 1.26, 95% CI = [0.97, 1.56]). There was no evidence that either thoughts or behaviours (suicide and self-harm) among those providing non-core care differed to that of those providing no caregiving.
Average treatment effect of core caregiving (2016) on suicidal behaviours (2018): complete case analyses (N = 2089). a
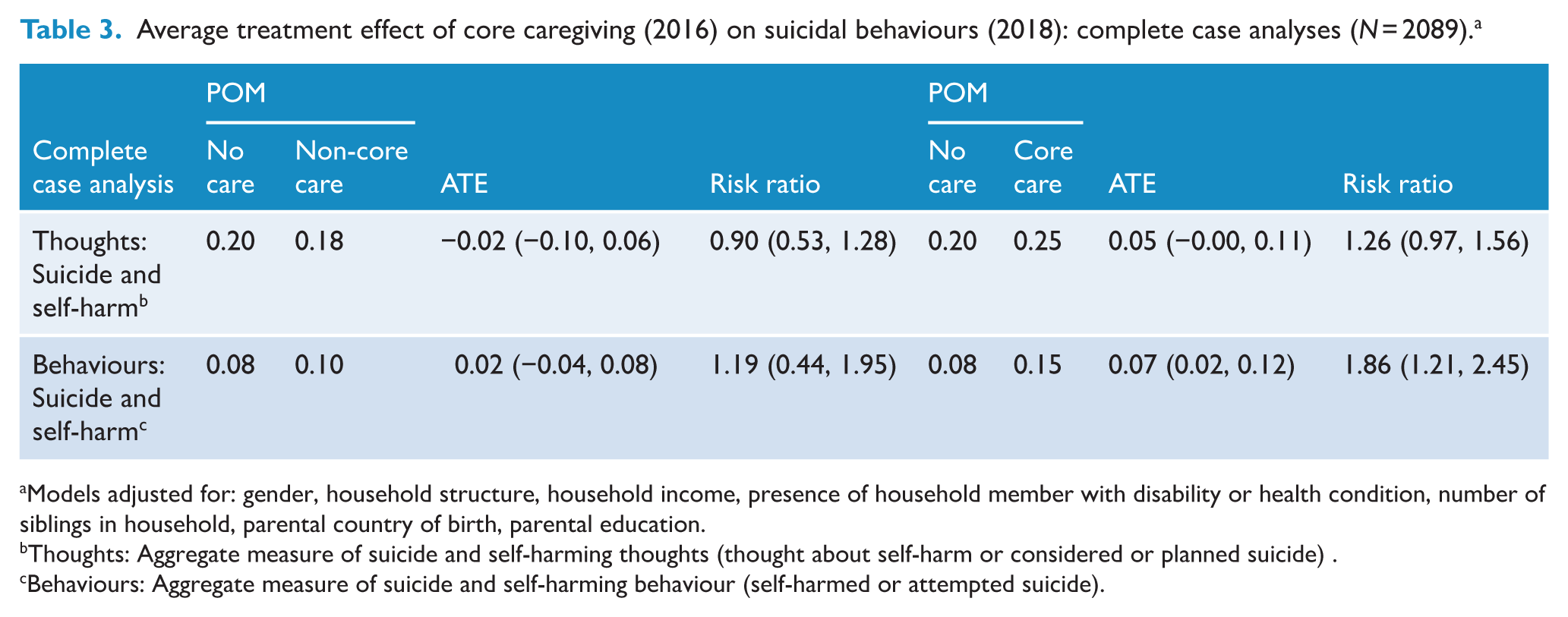
Models adjusted for: gender, household structure, household income, presence of household member with disability or health condition, number of siblings in household, parental country of birth, parental education.
Thoughts: Aggregate measure of suicide and self-harming thoughts (thought about self-harm or considered or planned suicide) .
Behaviours: Aggregate measure of suicide and self-harming behaviour (self-harmed or attempted suicide).
Sensitivity analysis using the imputed data set produced results that were highly concordant with those of the main analyses (see Table S2 in Supplementary Material), showing an elevated risk of suicide and self-harming behaviours among young carers. Logistic regression models (see Table S3 in Supplementary Material) applied to each single (non-aggregated) outcome measure also supported main findings, indicating increased odds of self-harm, suicide attempt and making a suicide plan among those providing core care (relative to non-carers). No associations between non-core care provision and self-harming or suicidal thoughts or behaviours were apparent. These logistic regression models also tested associations for the aggregate outcomes and found increased odds of both behaviours and thoughts for core carers relative to non-carers. Analysis using a binary care variable (any care vs no care) supported the main findings, with associations observed between caregiving and self-harm, making a suicide plan, and suicide attempt assessed as individual outcomes, and the aggregated behaviours measure (see Table S4 in Supplementary Material). In analysis of cross-sectional associations between exposures and outcomes (Table S5 in Supplementary Material), there was some attenuation of estimates, however associations remained signficant for suicide attempt and making a suicide plan. Models in which we adjusted for Wave 6 outcomes (Table S6 in Supplementary Material) were highly aligned with those in Table S3 in Supplementary Material.
Discussion
This longitudinal study of a sample of Australian adolescents found that those providing ‘core’ care were at increased risk of reporting suicide and self-harming behaviours 2 years later, relative to same age peers who were not carers. Specifically, performing core caregiving activities, for at least 6 months at age 16–17 years was associated with an 86% increase in the rate of reporting suicide or self-harming behaviour at 18–19 years of age, compared to peers who carried out no caregiving. Weaker evidence indicated that core carers were at elevated risk of self-harming and suicidal thoughts relative to non-carers, but there was no evidence that those providing non-core care were at elevated risk of either suicide and self-harming thoughts or behaviours.
These results align with, and extend, research in the United Kingdom over the COVID-19 pandemic indicating that young carers had higher rates of suicide attempt than non-carers (Nakanishi et al., 2022). The results are also consistent with evidence that caregiving is associated with poorer mental health among young people (Fleitas Alfonzo et al., 2022, 2023, 2024; King et al., 2021), as well as research among adults indicating that thoughts that life is not worth living (O’Dwyer et al., 2014) and suicide ideation (O’Dwyer et al., 2016) are higher among adult carers relative to adult non-carers.
Core care activities address essential needs of recipients and typically indicate greater dependence of the care recipient on the carer. Our findings suggest that it is this high-dependency caregiving such as personal care (e.g. washing, dressing, eating, toileting), moving around (e.g. getting in/out of bed), and communicating that is associated with elevated risk of self-harm and suicide behaviour (and possibly thoughts and ideation) in young people, rather than all forms of caregiving. Less intensive non-core caregiving activities showed no observable association with self-harm and suicidal thoughts and behaviours relative to no caregiving.
Further research into the mechanisms underpinning the associations observed in this analysis is needed, and it is possible that the associations do not reflect a causal relationship between young caregiving and suicide and self-harming outcomes. However, we note that there are some factors that may elevate suicide and self-harm risks among young core carers. More intensive caregiving activities may be associated with higher expenditure of time and emotional energy and greater levels of isolation and loneliness–known risk factors for suicide. Some young carers report intensely conflicting emotions (Blake-Holmes and McGowan, 2022), and sometimes experience guilt and stigma (Moore and McArthur, 2007) and these may be exacerbated in the case of intense core caregiving, resulting in poorer mental health. It is notable that among adults, intensive caregiving is associated with higher levels of stress (Lyons et al., 2015), CVD incidence (Lambrias et al., 2023), and poor mental health (Ervin et al., 2022). The mental health impacts of caregiving have led to a recent position statement by Suicide Prevention Australia calling for greater protections and support for carers (Suicide Prevention Australia, 2022).
Young carers who provide core care may also be less likely to receive sufficient support, leading to an intensification of the isolation and stress of caregiving. Relative to those providing non-core care, it is plausible that support needs may be greater for those providing more intensive core care. Many young carers are highly protective of the care recipient and are reluctant to complain or seek support and may sometimes perceive help-seeking as a form of complaint or criticism (Blake-Holmes and McGowan, 2022). Many parents are determined to ensure that young carers are not disadvantaged by their caring role, but achieving this may be dependent on them feeling safe enough to disclose their caregiving–to service providers or others in a position to assist–without judgement and stigma (Blake-Holmes and McGowan, 2022). This can place young carers and their families in a difficult position of needing assistance, but being reluctant to seek help. Lack of awareness among peers, gatekeepers such as teachers and service providers, and stigma can compound a sense of isolation and contribute to young carers’ reluctance to seek help (Moore and McArthur, 2007; Watt et al., 2017).
In the United Kingdom, where local authorities are obliged to identify the needs of young carers, an estimated 80% of young carers receive no assistance from their local authority (Children’s Commissioner, 2016). This points to a key need to improve awareness of the prevalence and support needs of young carers, especially those providing core care, and where young carers are identified, to improve linkage to support and services. Further research is also needed to identify the best ways to support young carers.
Young caregiving often intersects with other forms of disadvantage (Pautz et al., 2021) which may heighten risk of self-harm and suicide among young carers. One study in Scotland identified that many young carers came from economically disadvantaged households and found they were aware of, concerned about, and sometimes responsible for managing their household’s finances. Proportionately fewer core and non-core carers were in the top income quintile in this research, relative to young people providing no caregiving. As well as potentially having a lower household income, it is possible that the demands of core caregiving may further impede earning capacity and exacerbate finance-related stress for the young person.
Core caregiving likely indicates poorer health of the care recipient, as well as higher likelihood of disability and/or increased vulnerability (relative to non-core care). For young people, having a family member who is ill is associated with increased risk of mental health difficulties (Pakenham and Cox, 2014). Outcomes observed in this analysis may therefore be partially due to young carers emotional responses and concerns about the disability or health condition of the person requiring care, independent of the demands of caregiving. Finally, the apparent lack of association between non-core caregiving and suicidal behaviours may indicate a lack of statistical power. It is important to ensure that the needs of this group are also prioritised. Given that young carers may shift between types of caregiving, it is possible that over time, young people providing non-core caregiving will transition to providing more intensive core caregiving.
Strengths and limitations
There are some important strengths of this analysis. First, the longitudinal design and the use of data from a national study of Australian Children strengthens both the validity and generalisability of findings. The use of AIPW is a robust method that reduces bias related to confounding and maximises causal inference. Second, five sets of sensitivity analyses including that conducted on an imputed data set and single (non-aggregated) outcome measures corroborated the main findings. Third, to avoid capturing everyday tasks in our caregiving measure, and mitigate misclassification of caregiving, we focussed on core caregiving. Fourth, we were able to specify the temporal ordering of variables to give greater confidence in the theorised causality between caregiving and the outcomes (exposure collected in Wave 7, outcomes collected in Wave 8, and confounders being mostly parent-level information and collected in Wave 6). Fifth, adjustment for a household member with a disability or health condition (including a mental health condition) also mitigated the risk of residual confounding due to either familial clustering of mental illness, or due to the distress related to having an ill household member (that may arise independent of caregiving).
We acknowledge some limitations of this study. The statistical analysis may have been underpowered with the number of core carers in the sample relatively low. While any level of suicidal or self-harming behaviour is too high, the fact that these outcome behaviours are relatively rare in absolute terms means that the combination of this, with a relatively rare exposure (caregiving), may have weakened our ability to detect differences between treatment groups (that is, between no care, non-core care and core care groups). Related to sample size, our classification of carers is necessarily blunt, and does not capture variations in intensity or duration of caregiving, nor the care needs of the care recipient – all factors which may impact on the way young carers experience caregiving. Further, ‘core’ care may not capture emotional care or care for someone with a mental illness or substance use disorder – forms of care that are likely to impact on young carers but that are sometimes missed by data collection as well as service providers–both of which may contribute to distress among young carers. It is also possible that the relationship between the young carer and the care recipient impacts on the young carer in a way that is distinct from the impact of caregiving itself. For example, the relationship between a young carer and a care recipient who is a parent is likely to be different to that of a care recipient who is a sibling, and this relationship may affect the stress, mental health and suicide risk of young carers. Not adjusting for these relationship-related factors may have introduced some bias into our analyses.
Given sample size restrictions we aggregated outcomes into thoughts (thoughts of suicide, thoughts of self-harm, made a suicide plan) and behaviours (suicide attempt and self-harm). While this distinction is theoretically grounded (O’Connor, 2011; O’Connor et al., 2012; O’Connor and Kirtley, 2018). It may also conceal some differences in the expression and experience of different types of behaviours or thoughts (noting that we mitigated this by carrying out sensitivity analyses on non-aggregated outcomes). In addition, while the temporal ordering of variables is a key strength of this analysis, it is possible that other events occurred across this period and may have impacted on outcomes. For example, the care recipient may have died between Waves 7 and 8, thus leading to distress and contributing to associations observed here.
We also acknowledge that our results may have been impacted by selection bias due to missing data. There were some differences between the characteristics of those included in the analytic sample, and those participating in Wave 1 but not included in the analysis due to missing data or sample attrition. Those participating in Wave 1 but excluded due to loss to follow up or missing data were more likely to be in the lowest income quintile, live in a single parent household, have a primary parent respondent who had not completed year 12, have at least one parent from a non-English-speaking household, have 3 or more siblings. Given evidence that young carers are disproportionately from households that are low-income or with a single parent, and identify as culturally and linguistically diverse (Cass et al., 2009), it is likely that selection bias arising from this missing data would have resulted in underestimation of treatment effects and risk ratios. We also note that we applied longitudinal survey weights to mitigate any selection bias due to non-response and survey attrition.
Conclusion
This study provides evidence that young carers who provide core care are at increased risk of suicidal and self-harming behaviours. While there is some evidence of increased risk of suicidal and self-harming thoughts among those providing core care, further research using larger data sets is needed. What is clear is that young core carers represent a group of young people who need increased awareness, recognition and system supports to help mitigate their heightened risk of suicidal and self-harming behaviours.
Supplemental Material
sj-docx-1-anp-10.1177_00048674251391993 – Supplemental material for A prospective study of suicide and self-harm among young carers using an Australian cohort
Supplemental material, sj-docx-1-anp-10.1177_00048674251391993 for A prospective study of suicide and self-harm among young carers using an Australian cohort by Tania King, Gerry Redmond, Nicola Reavley, Myra Hamilton and Alison Barr in Australian & New Zealand Journal of Psychiatry
Footnotes
Acknowledgements
In this study, we use unit record data from Growing Up in Australia, the Longitudinal Study of Australian Children (LSAC). The study is conducted in partnership between the Department of Social Services (DSS), the Australian Institute of Family Studies (AIFS) and the Australian Bureau of Statistics (ABS). The findings and views reported in this paper are the those of the authors and should not be attributed to AIFS, DSS or ABS. We are grateful to the survey participants of LSAC.
Contributorship statement
TK conceptualised the study, acquired the funding, carried out the analysis, and wrote the paper. All authors contributed to analytical design, interpretation of findings, review and revision of drafts.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Ethics approval statement
Ethics approval for this analysis was granted by the University of Melbourne Human Research Ethics Committee (#20333). The LSAC study was granted ethics approval by the Australian Institute of Family Studies Ethics Committee, a Human Research Ethics Committee registered with the National Health and Medical Research Council (NHMRC).
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by an Australian Research Council Discovery Early Career Award (TK, DE200100607) and a Suicide Prevention Australia Innovation Grant.
Data availability statement
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
