Abstract
Objective:
People with different psychiatric diagnoses use certain suicide methods more frequently. These findings could have implications for reducing suicide. Therefore, the aim of this study was to assess associations between three severe mental illnesses (SMIs) and suicide methods, while adjusting for other confounding factors that could influence choice of suicide methods.
Methods:
We used information on all individuals dying by suicide in Queensland, Australia, from 1989 to 2021. Methods were compared to hanging, strangulation and suffocation for people with three different SMIs with adjusted risk ratios in multinomial logistic regression models.
Results:
People with psychotic disorders were over three times more likely to jump from a high place, jump or lie before a moving object, or use a sharp object. They were also more than twice as likely to use explosive material or smoke, fire and flames; or drowning and submersion and 60% more likely to use crashing of a motor vehicle. Poisoning by drugs was around 50% higher in those with psychotic disorders or depression. No other methods were substantially elevated relative to hanging, strangulation and suffocation (HSS). People with bipolar and depression had a lower risk ratios (RR) for several suicide methods.
Conclusion:
People with psychotic disorders were the most likely to use diverse methods and would benefit the most from means restriction interventions. Trialling interventions to ensure that people with psychotic disorders can avoid situations where they could use these methods may reduce suicides in this group. Further analysis of what drugs people with depression and bipolar might use is needed.
Introduction
In 2021, 746,000 deaths by suicide occurred worldwide (Weaver et al., 2025). Reducing suicide is a global public health imperative. Suicide arises from complex interactions between biological, psychological, clinical, social and environmental factors (Turecki et al., 2019). Thus, reducing suicide is difficult because it is unlikely that one algorithm will accurately predict suicidal thoughts and behaviours from existing risk factors (Franklin et al., 2017). Despite this, mental disorders are well-established risk factors for dying by suicide (Moitra et al., 2021), and suicide rates are especially high for people with severe mental illnesses (SMIs) compared to people with other or no known mental illnesses (Fu et al., 2023).
A necessary cause (Rothman, 1976) and effect measure modifier for suicide deaths is the lethality of the suicide method. A recent review found that firearms, hanging and drowning were the most lethal methods (Cai et al., 2022). Age and sex differences in suicide methods used, which affect suicide rates due to the methods having varying case-fatality rates (Cai et al., 2022; Conner et al., 2019; Fu et al., 2023). However, the relationship between SMI and suicide methods has not been extensively studied. Some studies have found that people with psychiatric diagnoses are more likely to use methods with higher case-fatality rates, like hanging and jumping (Chen et al., 2009; Kimura et al., 2013; Kõlves et al., 2018; Lopez-Morinigo et al., 2014), although they also use some with lower case-fatality rates, like poisoning with drugs (Kõlves et al., 2018).
A systematic review of population- and community-based interventions to prevent suicide concluded that reducing access to lethal means was one of four community-based interventions that may reduce suicide deaths (Linskens et al., 2023). Therefore, understanding whether people with different SMIs use suicide methods that are more common, predictable, or amenable to means restriction may help reduce their suicide rates. Since the suicide method used largely determines case-fatality rates (Cai et al., 2022), it is logical to study both psychiatric diagnoses and suicide methods together. Thus, our aim was to examine associations between SMI and suicide methods using data from a state-wide public health surveillance system, comprising the interim (iQSR) and final Queensland Suicide Register (QSR). We defined SMI as psychotic disorders, bipolar disorders, or depression, based on the three most common diagnostic groups cited as SMIs in a 2022 systematic review of 777 studies (Gonzales et al., 2022).
Several previous studies have found that having a psychotic disorder is associated with using a train (Huisman et al., 2010) and jumping (Huisman et al., 2010; Kim et al., 2021; Men et al., 2024; Park et al., 2013). People with depression have previously had odds of using jumping from height or poisoning 15% lower than hanging (Men et al., 2024). Based on this literature, we hypothesised that:
People with psychotic disorders would more frequently use suicide methods that involve jumping from a height or jumping before a moving object.
Compared to hanging, strangulation and suffocation (HSS), people with depression would use other methods less frequently.
Methods
Reporting statements
We reported according to the STrengthening the Reporting of OBservational studies in Epidemiology guidelines (Vandenbroucke et al., 2007) and the REporting of studies Conducted using Observational Routinely-collected Data (Benchimol et al., 2015) guidelines (see populated checklists in Supplementary Table 1).
Study design
Population-based consecutive case series.
Setting
Queensland.
Study subjects
This study included all individuals who died by suicide in Queensland from late 1989 (partial year) to 2021. A small number of deaths occurring in 1989 were included in the database and were thus included. Although the data for 2020 and 2021 were incomplete, they were retained as the date of death was a continuous variable, and we anticipated that the relationship between suicide methods and psychiatric diagnoses would not vary significantly within parts of a year.
Codes or algorithms used to select subjects
Two reviewers used a decision tree to probabilistically code each death received into a ‘possible’, ‘probable’, or ‘confirmed’ suicide (Leske et al., 2022: 44). Study subjects included had deaths classified as ‘probable’ or ‘confirmed’ suicides.
Validation studies of codes
To establish the direction and magnitude of misclassification bias that might affect studies using routinely collected health data such as this one, QSR coding was evaluated against a psychological autopsy (PA) interview method in a quality control study using a sample of 130 suicides from December 2005 to December 2007 (De Leo and Sveticic, 2007). For each death by suicide coded into the QSR, a PA interview also occurred to establish if the QSR underreported or overreported several factors. The PA interview, conducted by a clinical interviewer with the deceased’s next-of-kin, provides a detailed assessment of the circumstances of a suicide 6 to 24 months after the death (De Leo and Sveticic, 2007). The average duration of a PA interview is 2 hours and covers demographics, recent life events, history of suicidal behaviour, medical history and psychiatric illness as assessed via the Structured Clinical Interview for Diagnostic and Statistical Manual Disorders (Spitzer et al., 1994). This study identified some underreporting of suicide intent in the past 12 months, lifetime and 12-month suicide attempts, several life events and some psychiatric diagnoses, indicating determinations of suicide were based on incomplete information. However, it is unfeasible to conduct PA interviews with all next-of-kin, which is a well-known limitation of suicide surveillance data internationally.
Variables
Supplementary Table 2 lists all codes used to classify exposures, outcomes and confounders.
Outcomes
The outcome variable was suicide methods coded according to the International Classification of Diseases, 10th Revision (ICD-10) by different data entry staff across the period of 1989 to 2021. We treated this as a multinomial variable, comparing each suicide method against HSS, the most frequently occurring group of suicide methods in Queensland, to avoid confounding in the base outcome and to enable a parsimonious approach to analysis by conducting one multinomial logistic regression instead of multiple binary logistic regressions. Similar previous studies (Huisman et al., 2010) have also chosen hanging as the reference group because it was the most common method. It therefore served as a meaningful reference point for the other categories, and using the method with a larger number of events as the base outcome provided more stability in each comparison. Moreover, means restriction for HSS is difficult, so we were more interested in the other suicide methods relative to it. QSR coders determined the suicide method used based on what forensic pathologists reported as the medical cause of death in post-mortem autopsies. In the event of multiple apparent methods, such as plastic bag suffocation and gas or poisoning, coders are instructed to code gas or poisoning as additional suicide methods (there are three variables for suicide methods in the QSR), but may determine the suicide method responsible for death, coding this as the first suicide method, based on the post-mortem.
Exposures
The exposure variables included psychotic disorders, depression and bipolar disorders coded by QSR data entry staff based on information from police reports and coronial findings or inquests. Data sources do not report whether someone had a primary or secondary diagnosis of these disorders. We considered that depression or bipolar disorder could overlap with psychotic disorders, yet people with bipolar disorder were coded as not having depression when this occurred (148 instances), with the understanding that some staff may have confused unipolar and bipolar depression.
Confounders
Confounding variables included in the adjusted models were date of death, age at death, sex, Aboriginal and Torres Strait Islander status, remoteness area of residential address, developmental disorder, substance use disorder, personality disorder, anxiety disorder, childhood trauma, or sexual abuse. These confounders were selected as they did or could have occurred before being diagnosed with an SMI. Date of death was considered a confounding variable as it could be a proxy for suicide methods more commonly used around that period.
Data sources and methods of assessment
The QSR and iQSR collect demographic, socio-demographic, risk factor and event-related data. Most information comes from a police report of the death prepared for coroners by police officers attending the scene. This is then supplemented with toxicology reports and post-mortem autopsies prepared by forensic pathologists. Finally, coroners’ reports and sometimes inquests, interpret all this information together to determine a cause of death for the deceased and are used in the iQSR and QSR to substantiate information from the police report.
Regarding completeness, a comparison with total suicides from the Australian Bureau of Statistics’ Causes of Death releases from 2006 to 2020 found that the QSR and iQSR reported 224 more suicides (10,050 vs 9,826), a 2.2% difference (Leske et al., 2023). An individual-level concordance study of 9,520 deaths in the QSR from 2001 to 2015 found that the QSR reported 510 more suicides than the National Coronial Information System (NCIS) from 2001 to 2015 (Leske et al., 2024).
In terms of timeliness, although the lag between a death occurring and it being entered into the QSR or iQSR is not formally recorded in the database, recent NCIS operational statistics (NCIS, 2025) indicated that in Queensland, there was currently a lag of 2 years (2023 and 2024) until 80% of cases are closed, and a lag of 3 years (2022 to 2024) until 95% of cases are closed and thus available for entering into the QSR.
Aboriginal and Torres Strait Islander status was sourced from police reports (1993 onwards), the NCIS (2001 onwards) and the Queensland Registry of Births, Deaths and Marriages (reliable from 1996 onwards). All other variables were sourced from post-mortem autopsies (1990 onwards), police reports of deaths to a coroner (1993 onwards) and coronial reports, or in rare instances, coronial inquests, with this documentation coming from the NCIS from 2001 onwards.
Bias
We controlled for confounding through regression. The proximity of the residential address to the suicide site was uncontrolled due to a lack of data. Recall bias was limited by relying on police reports populated soon after officers attended the scenes of suicides. There was no attrition bias as no cohort was enumerated. Selection bias was minimised by using a register capturing all suspected suicides in the jurisdiction. Information biases, such as detection and interviewer bias, were avoided by using secondary data collected for other purposes.
Study size
The study size was the number of individuals dying by suicide in Queensland from 1989 to 2021. While these people were mostly Queensland residents, some were interstate or homeless.
Quantitative variables
Rarely used suicide methods were collapsed into similar categories, and non-specific ICD-10 suicide codes like ‘unspecified means’ and ‘late effects of self-inflicted injury’ were excluded from analysis due to insufficient detail.
Statistical methods
At a bivariate level, we reported risk ratios (RR) and their 95% confidence intervals (CI) with two-sided Fisher’s Exact P values. At a multivariable level, we controlled for confounding through including variables in a multinomial logistic regression model, estimating adjusted odds ratios and converting them to adjusted RR after estimation for presentation. We modelled the functional form of the continuous variables age at death and date of death using multivariable fractional polynomials (FPs), which were the best-fitting FP from 44 models tested for each variable. RR decimal places were reported per the rule of four (Cole, 2015a), and all other statistics were reported per recommendations (Cole, 2015b). Loss to follow-up was not applicable. We did not examine any interactions or conduct any sensitivity analyses.
We cleaned and analysed data in Stata version 13.1 (StataCorp, 2013), using several user-written commands: MDESC (Medeiros and Blanchette, 2011) for tabulating the prevalence of missing data, collin (Ender, 2010) for assessing multicollinearity, bacon (Weber, 2010) for detecting multivariate outliers using the blocked adaptive computationally efficient outlier nominators (BACON) algorithm (Billor et al., 2000) and ASDOC (Shah, 2021) for creating tables in Microsoft Word.
Data access and cleaning methods
SL and KK had full access to the database. Both investigators were on the primary ethical clearance for the project, approved by the State of Victoria’s Department of ’s Justice Human Research Ethics Committee (NCIS M0112 and JHREC CF/18/12771) and the secondary ethical clearance (prior review) from Griffith University’s HREC (GU Ref No: 2010/537).
SL cleaned data by reviewing individual police reports to ascertain age and remoteness for 11 people with missing data and using other sources to code Aboriginal and Torres Strait Islander status for the same 11 people. One person’s sex was corrected by checking the master dataset.
Results
Participants
Supplementary Figure 1 illustrates the selection of study participants for the analysis. The source dataset included 18,110 people. Exclusion of suicide methods due to sparse data included X83 Intentional self-harm by other specified means (n = 113, 0.6%). Suicide methods with insufficient detail excluded 85 people (0.45%). This left 17,912 individuals for analysis, of which a further 330 were excluded due to missing data on various confounding variables included in the models (see Supplementary Figure 1 and Supplementary Table 4).
For assumption testing, the BACON algorithm was applied using a threshold of the 15th percentile of the chi-square distribution to distinguish outliers from nonoutliers but otherwise retaining the package’s default settings to each model. This found no multivariate outliers. There was no multicollinearity, assessed by variance inflation factors of 10 or more. The FP models chose two variables for date of death to the power of −2 and −2 and two terms for age at death to the power of −0.5 and 0.
Table 1 presents descriptive data for each subgroup of interest and comparators without each individual SMI in the three multinomial logistic regressions, and the no SMI group. The average age of people in the study was 43, and 23% were female. Most people resided in Major Cities of Australia (57%), with proportions decreasing as remoteness increased.
Descriptive statistics on confounders for each severe mental illness group compared.
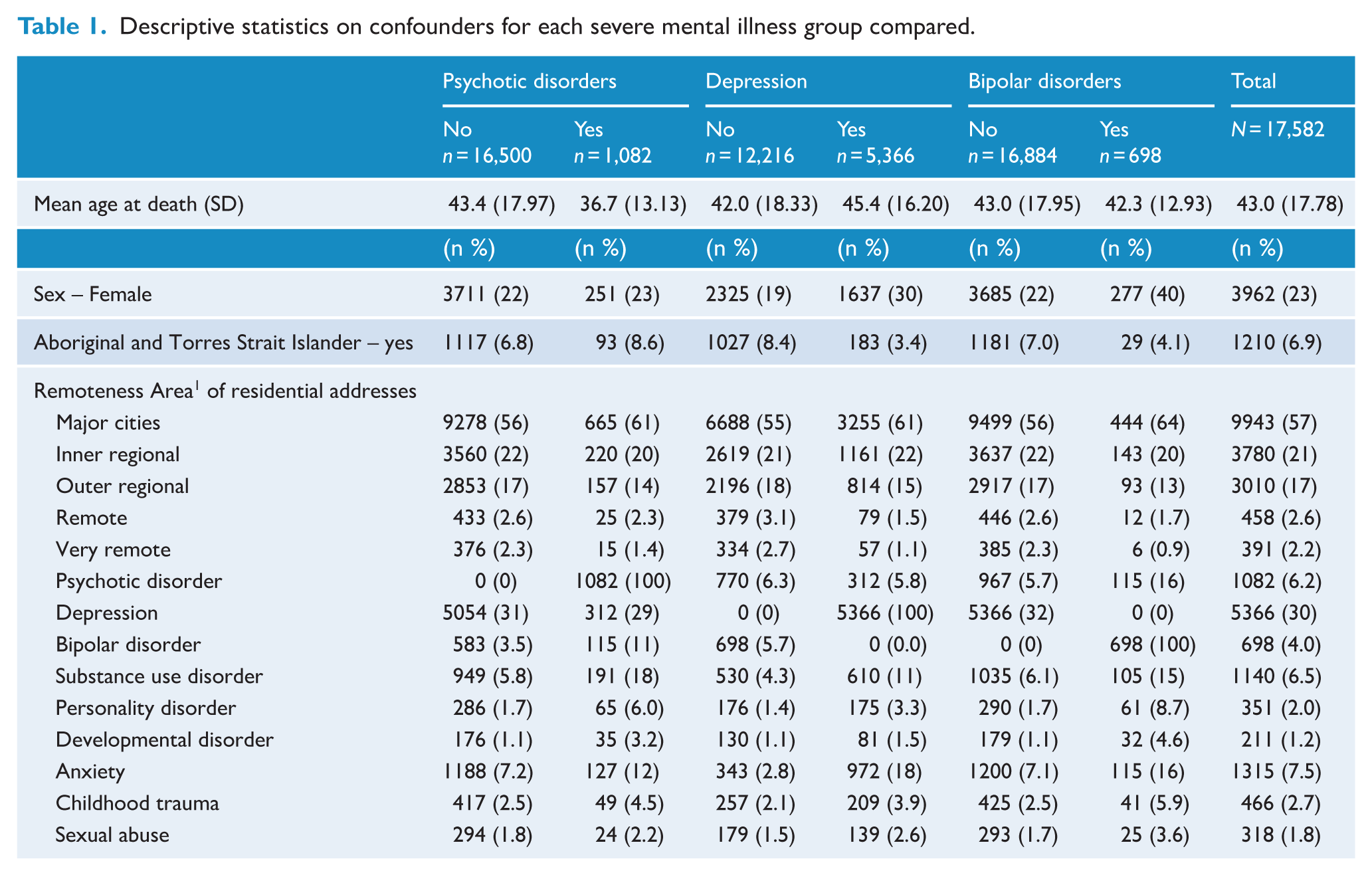
People with psychotic disorders were noticeably younger than those without psychotic disorders (M = 36.7 vs 43.4). Higher proportions of females were observed in the group with psychotic disorders (23% vs 22%), depressive disorders (30% vs 19%) and bipolar disorders (40% vs 22%) compared with the respective comparison groups without these disorders.
Supplementary Table 3 reports the number and proportion of people with each SMI using different suicide methods. Among individuals with and without each SMI, hanging was the most common method used, being slightly more frequent in those with depression as opposed to those with psychotic or bipolar disorders. The use of drugs was the second most frequent suicide method for people with all three SMIs. The third most common suicide method differed by SMI, being jumping from a high place for people with psychotic disorders, and non-drug poisoning (X67 to X69) for people with depression or bipolar.
Tables 2–4 provide unadjusted estimates of associations between psychiatric diagnoses and suicide methods. The most elevated unadjusted RRs for people with psychotic disorders compared to HSS, were for jumping or lying before moving object, jumping from a high place, using a sharp object and crashing of motor vehicle. For people with depression, suicide methods elevated compared to HSS included the use of drugs and drowning and submersion. For people with bipolar, compared to HSS, elevated suicide methods included the use of drugs and jumping from a high place. RR magnitudes were noticeably higher for people with psychotic disorders compared to people with depression or bipolar.
Unadjusted and adjusted multinomial logistic regression, showing the proportion using each suicide method vs hanging, strangulation and suffocation, people with vs without psychotic disorders (N = 17,582).
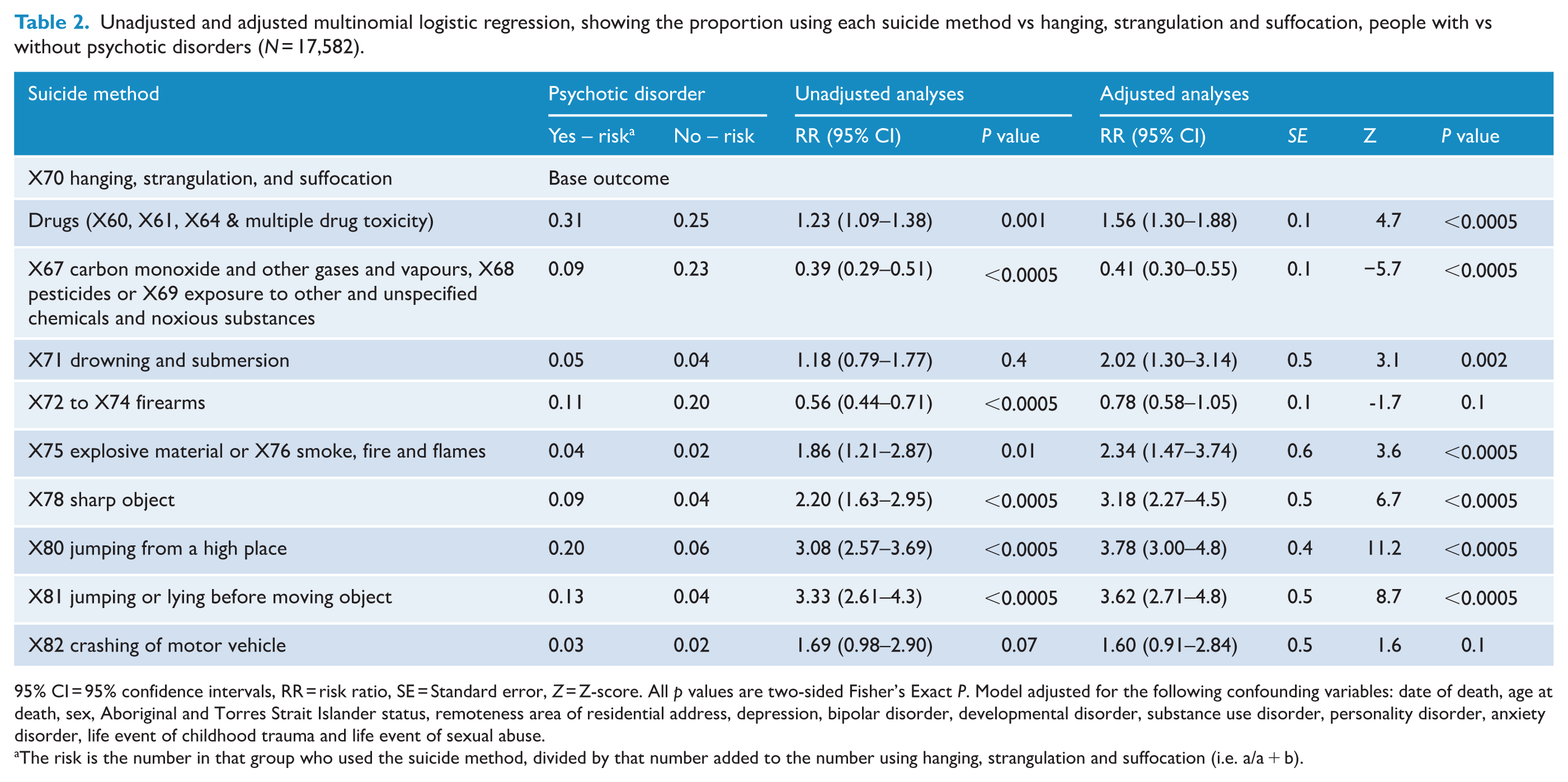
95% CI = 95% confidence intervals, RR = risk ratio, SE = Standard error, Z = Z-score. All p values are two-sided Fisher’s Exact P. Model adjusted for the following confounding variables: date of death, age at death, sex, Aboriginal and Torres Strait Islander status, remoteness area of residential address, depression, bipolar disorder, developmental disorder, substance use disorder, personality disorder, anxiety disorder, life event of childhood trauma and life event of sexual abuse.
The risk is the number in that group who used the suicide method, divided by that number added to the number using hanging, strangulation and suffocation (i.e. a/a + b).
Unadjusted and adjusted multinomial logistic regression, showing the proportion using each suicide method versus hanging, strangulation and suffocation, people with versus without depression (N = 17,582).
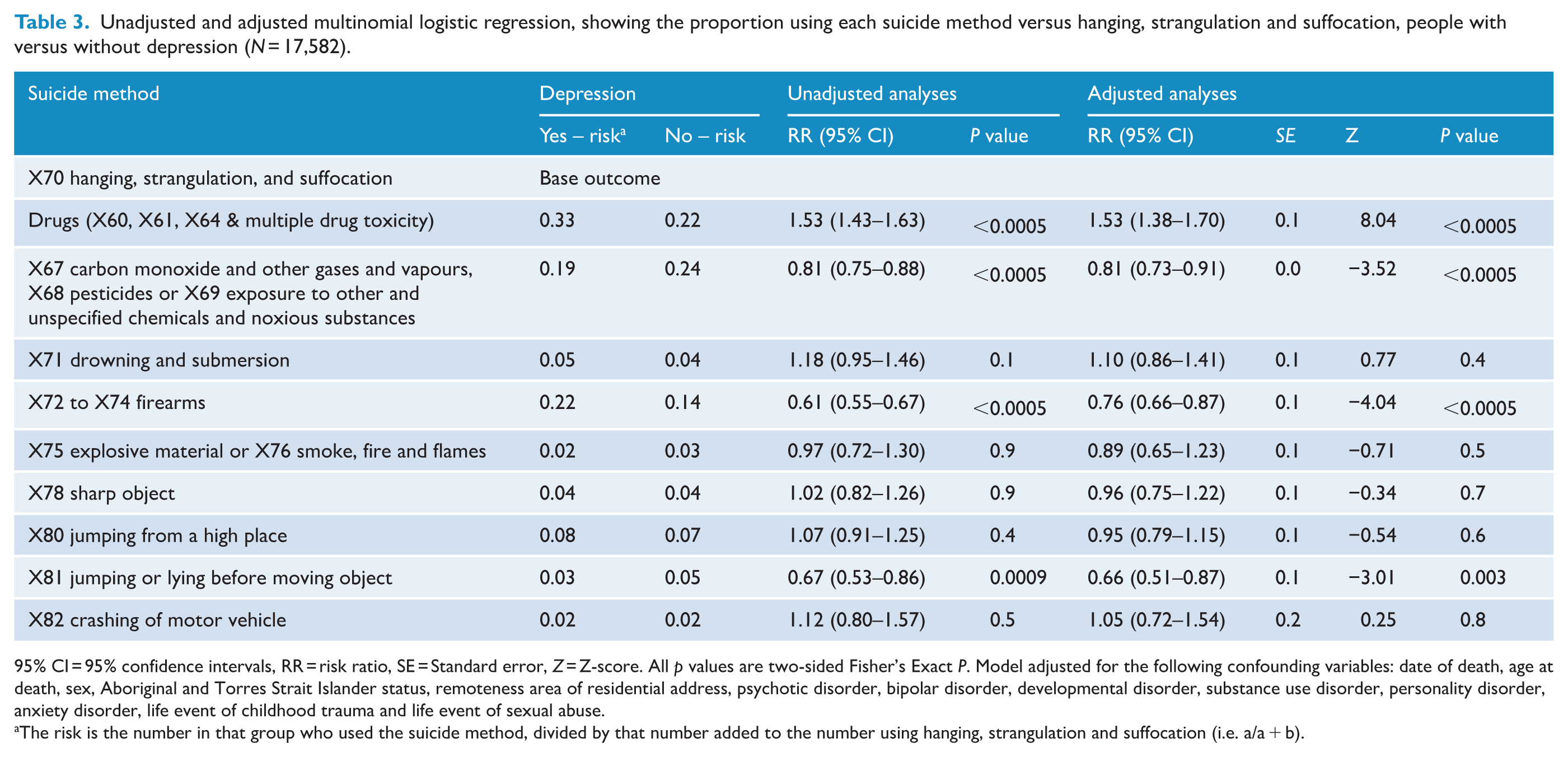
95% CI = 95% confidence intervals, RR = risk ratio, SE = Standard error, Z = Z-score. All p values are two-sided Fisher’s Exact P. Model adjusted for the following confounding variables: date of death, age at death, sex, Aboriginal and Torres Strait Islander status, remoteness area of residential address, psychotic disorder, bipolar disorder, developmental disorder, substance use disorder, personality disorder, anxiety disorder, life event of childhood trauma and life event of sexual abuse.
The risk is the number in that group who used the suicide method, divided by that number added to the number using hanging, strangulation and suffocation (i.e. a/a + b).
Unadjusted and adjusted multinomial logistic regression, showing the proportion using each suicide method versus hanging, strangulation and suffocation, people with versus without bipolar disorder (N = 17,582).
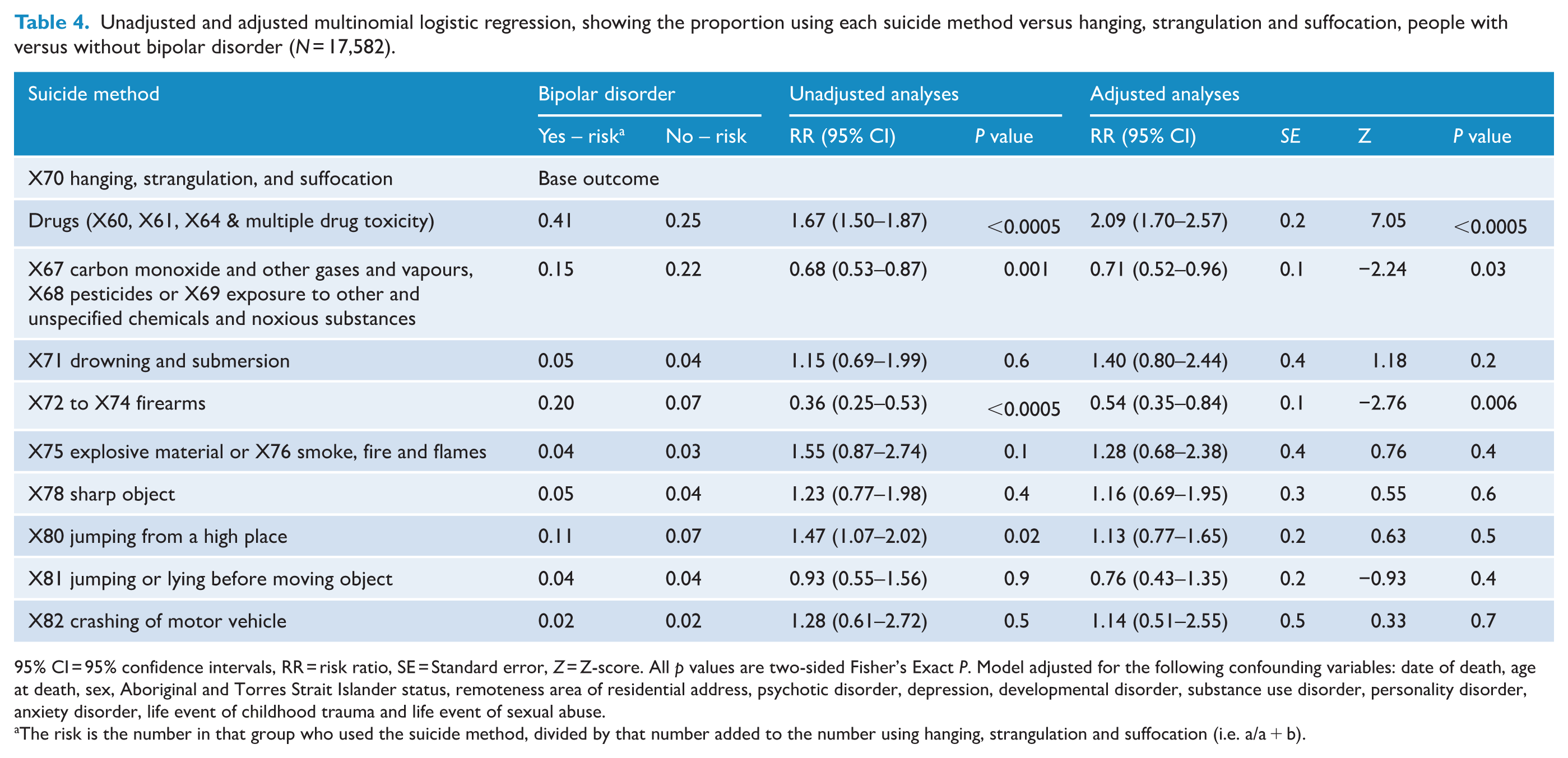
95% CI = 95% confidence intervals, RR = risk ratio, SE = Standard error, Z = Z-score. All p values are two-sided Fisher’s Exact P. Model adjusted for the following confounding variables: date of death, age at death, sex, Aboriginal and Torres Strait Islander status, remoteness area of residential address, psychotic disorder, depression, developmental disorder, substance use disorder, personality disorder, anxiety disorder, life event of childhood trauma and life event of sexual abuse.
The risk is the number in that group who used the suicide method, divided by that number added to the number using hanging, strangulation and suffocation (i.e. a/a + b).
Main results
Table 2 and Figure 1 show the findings of the multinomial logistic regression examining the relationship between psychotic disorders and suicide methods. In order of magnitude, people with psychotic disorders had an RR of jumping from a high place 3.78 times higher than those without psychotic disorders, followed by jumping or lying before moving object being 3.62 times higher, sharp object being 3.18 times higher. Another two methods had RR two or more times higher: explosive material or smoke, fire and flames and drowning and submersion. Finally, the use of drugs was elevated, being 56% higher in the group with psychotic disorders. The RR for crashing of motor vehicle was higher than this (1.60), and most of the confidence interval was above 1.00, yet this estimate had much wider CIs due to this method being rarer. In contrast, people with psychotic disorders were 59% less likely to use other non-drug poisoning, consisting of ICD-10 codes X67 to X69 (See Table 3). They were also 22% less likely to use firearms.
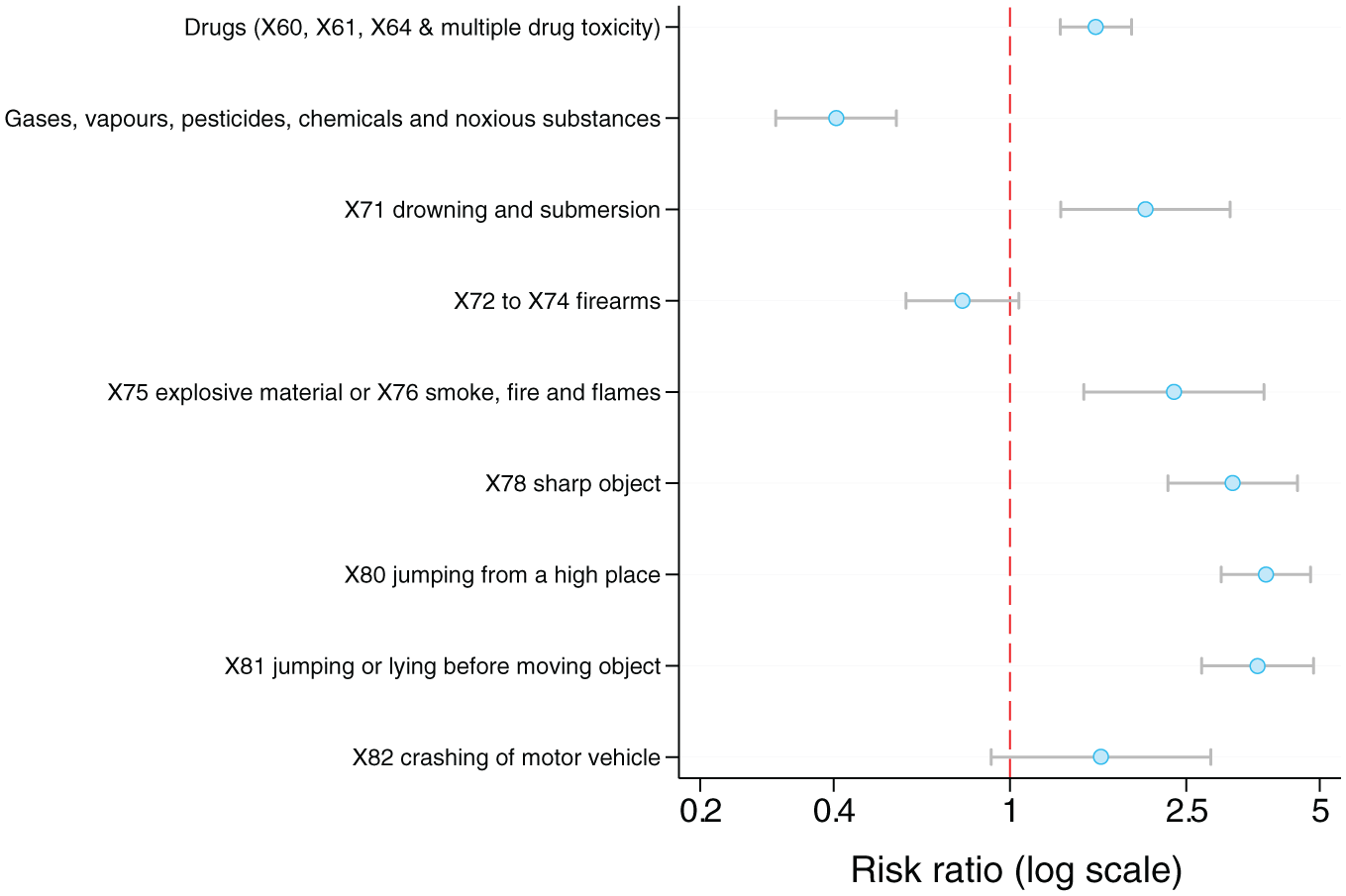
Forest plot showing adjusted risk ratios of suicide methods for people with psychotic disorders versus those without psychotic disorders.
For people with depression (Table 3 and Figure 2), associations were lower in magnitude but generally more precise, with the highest being drugs at 53% higher. Drowning and submersion was 10% higher, but more imprecise. Compared to hanging, strangulation and suffocation, there was a lower RR for several methods. In order of magnitude, these were jumping or lying before moving object, at 34% lower, firearms, at 24% lower, and non-drug poisoning, at 19% lower. The proportions of people using three methods were all quite similar for people with depression: explosive materials or smoke, fire and flames; the use of a sharp object, jumping from a high place and crashing of motor vehicle.
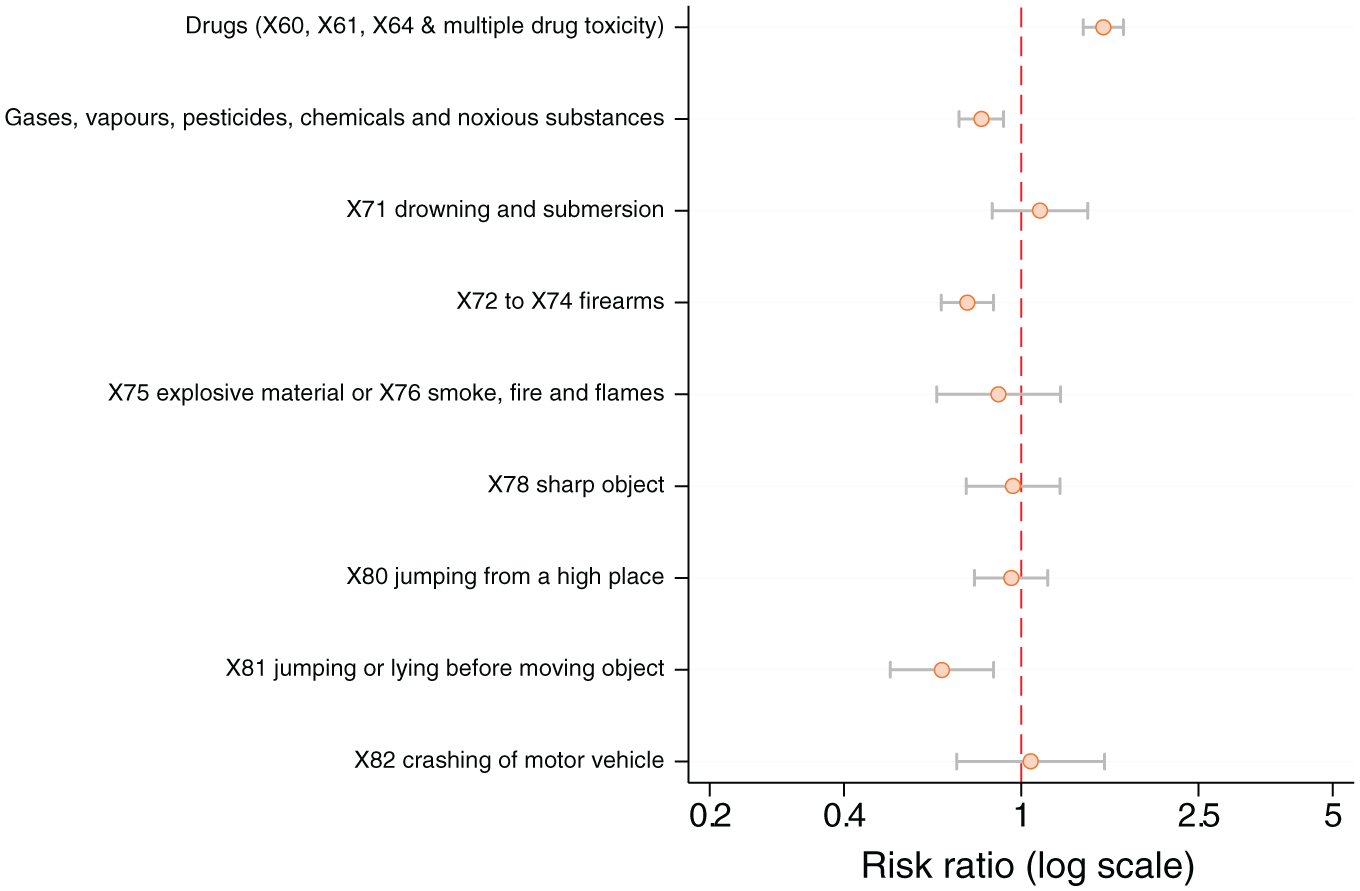
Forest plot showing adjusted risk ratios of suicide methods for people with depression, vs those without depression.
For people with bipolar disorder (Table 4 and Figure 3), the most elevated RR was for using drugs, which was 109% higher. Drowning and submersion was 40% higher in people with bipolar. Slightly lower than that RR was explosive material or smoke, fire or flames, at 28% higher. People with bipolar disorder used several methods proportionally less often. These included firearms, at 46% lower, non-drug poisoning, at 29% lower, and jumping or lying before a moving object, at 24% lower, although the CI was wider here due to sparse data.
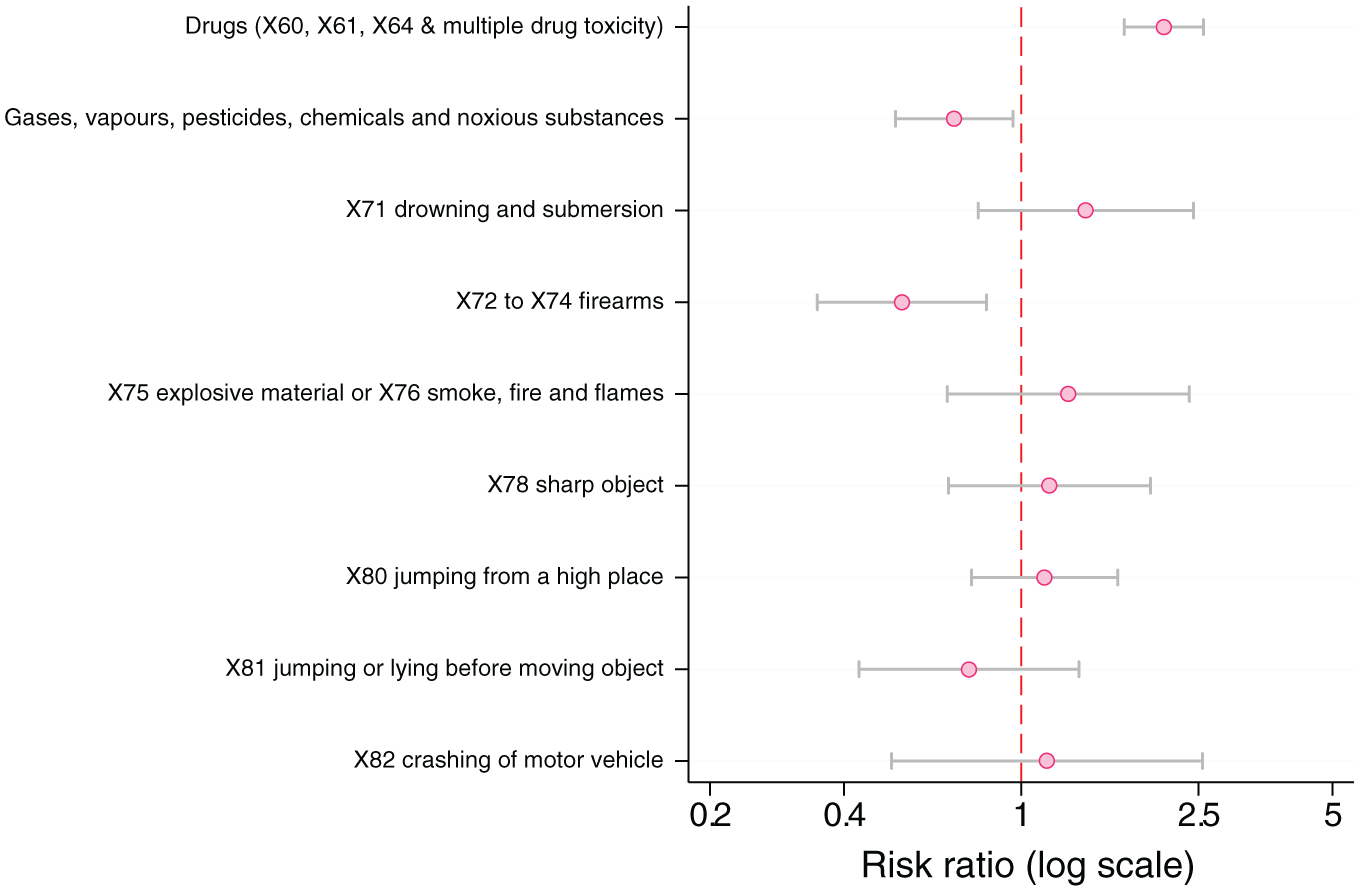
Forest plot showing adjusted risk ratios of suicide methods for people with bipolar disorder versus those without bipolar disorder.
Discussion
Key results
The aim of this study was to examine associations between three different psychiatric diagnoses and subsequent suicide methods. We found distinct associations with different suicide methods for each SMI, with the strongest associations observed between psychotic disorders and several violent suicide methods.
Limitations
Study limitations mainly pertain to the processes for establishing a death as a suicide and psychiatric diagnoses in coronial data, as well as the sparse numbers of people with less common diagnoses using rarer suicide methods, increasing imprecision. A comparison of 130 deaths by suicide between 2005 and 2007 in the QSR with interviews with the next-of-kin using a PA approach (De Leo and Sveticic, 2007) highlights the potential for misclassification in the QSR as discussed previously.
While it is unknown how the misclassification bias pertaining to the death being a suicide would influence the direction and magnitude of the associations, accounting for the misclassification bias concerning psychiatric diagnoses would reduce the magnitude of associations to a moderate extent, given the magnitude of misclassification observed against the PA method. Accounting for misclassification bias in both the intent of the deceased and psychiatric diagnoses would increase the precision of estimates, given that suicide methods are the same in the QSR and the PA approach (De Leo and Sveticic, 2007).
There are several implications of using data collected to inform the coroner. The misclassification bias for psychiatric diagnoses arises from this, as the information collected may not always include the medical records of the deceased. The information collected primarily comes from police reports, and so unmeasured confounding may exist if events are not recorded by police or asked for in the report they complete. Missing data are limited, given there is the opportunity for multiple parties (coroners, QSR staff) to obtain missing data during the investigation of the death. Knowledge of psychiatric conditions would have improved over time, meaning that associations might change in their magnitude over time.
Study strengths include adjustment for confounding factors, disaggregation of previously combined suicide methods (e.g. jumping from heights and jumping or lying before a moving object), separate estimates for two affective disorders sometimes combined in previous analyses, and more precision in estimates than some smaller previous studies.
Interpretation
Our findings accord with previous studies that have used hanging as the reference group in analyses. Psychotic disorders were associated with using a train and jumping in the Netherlands in 505 deaths by suicide from 1996 to 2005 (Huisman et al., 2010). In contrast to their findings of bipolar patients having higher odds of using trains before hanging (Huisman et al., 2010), people with bipolar had lower odds of jumping or lying before a moving object over hanging in our study. Depression also was not associated with any specific suicide method (Huisman et al., 2010), although their sample size (505) was much smaller than ours, and some ORs were quite elevated (2.82 for train vs hanging). Agreeing with our findings, a 23-year study of 5288 suicide deaths in Toronto from 1998 to 2020 found that people with schizophrenia/schizoaffective/psychosis/delusional/psychotic symptoms had odds of jumping from height 3.02 times higher than hanging, 1.39 times higher odds of using poisoning rather than hanging and 1.47 times higher odds of poisoning rather than hanging (Men et al., 2024). People with bipolar disorder also had 1.49 times higher odds of using jumping from height than hanging (inconsistent with our findings) and 2.93 times higher odds of using poisoning rather than hanging (consistent with our findings). Finally, people with depression had odds of using jumping from height or poisoning 15% lower than hanging (both odds ratio [OR] = 0.85, inconsistent in direction for the poisoning finding) and odds of poisoning 1.43 times higher than hanging (consistent with our findings) (Men et al., 2024). Schizophrenia was also associated with jumping and drowning among 23,647 people in South Korea who died by suicide from 2013 to 2017 (Kim et al., 2021). People with psychotic disorders had 2.98 times higher odds of using jumping than hanging and 1.21 times higher odds of drowning than hanging in a smaller South Korean study of 467 individuals dying by suicide from January 1995 to December 2006 (Park et al., 2013). People with bipolar also had elevated odds of jumping (OR = 1.48) and drowning (OR = 1.42) relative to hanging.
Therefore, while the findings regarding psychotic disorders appear consistent with those internationally, the findings for people with depression or bipolar disorder appear more specific to Queensland. These findings suggest that, in Queensland specifically, interventions for people with psychotic disorders thought to be at risk for suicide should try to ensure they avoid, or are not alone, when in areas where they could jump from a high place or jump or lie before a moving object, which is typically a train or a car. The feasibility of means restriction interventions at train stations servicing major public and private hospitals with inpatient and outpatient psychiatric patients could be assessed if not already done. Such interventions include suicide pits, removal of grade crossings and platform screen doors (Barker et al., 2017; Belur et al., 2025). In addition, employing means restriction of sharp objects and potential ligatures in the home (given that HSS is still the most common method) would also likely be an important strategy. Other important strategies could include safety planning (Marshall et al., 2023; Nuij et al., 2021), or accompanying individuals with psychotic disorders in situations where they might have access to equipment and materials to generate smoke, fire and flames, or engage in drowning and submersion.
Generalisability
These findings do not necessarily generalise as the proportion of suicide methods varies worldwide due to the availability of different means for suicide (e.g. firearms and pesticides), the acceptability of different suicide methods, and the built infrastructure of different countries.
In conclusion, our consecutive case series study of suicides occurring between 1989 and 2015 found distinct associations with different suicide methods for each of the three SMI groups studied. The implications, in terms of means restriction and interpersonal interventions, are clearest for those with psychotic disorders who tended to use more violent methods. The findings for the group with psychotic disorders are mostly consistent with prior literature, while the findings for depression and bipolar are not. These findings provide new information in terms of the context of suicides in Queensland, Australia and disaggregated psychiatric diagnoses and suicide methods to the extent possible in routinely collected police and coronial data. These findings may generalise to other Australian jurisdictions, with future research necessary to confirm this.
Accessibility of protocol, raw data and programming code
There was no study protocol published for this paper. The title page contains information on requesting access to the raw data. The programming code used to analyse the data is available from the corresponding author upon reasonable request.
Supplemental Material
sj-docx-1-anp-10.1177_00048674251374848 – Supplemental material for A consecutive case series study of the association between psychiatric diagnoses and suicide methods using coronial data in Queensland, Australia, from 1989 to 2021
Supplemental material, sj-docx-1-anp-10.1177_00048674251374848 for A consecutive case series study of the association between psychiatric diagnoses and suicide methods using coronial data in Queensland, Australia, from 1989 to 2021 by Stuart Leske, Nicola Warren, Kairi Kõlves, Rebecca Soole, Dan Siskind and Steve Kisely in Australian & New Zealand Journal of Psychiatry
Footnotes
Acknowledgements
The authors acknowledge the funders of this research for their support of the larger QSR project, and this study specifically. The authors also acknowledge the National Coronial Information System (NCIS), as the database source for most of the data and the data custodian, and the Victorian Department of Justice and Community Safety as the source organisation of NCIS data. The authors also acknowledge the Coroners Court of Queensland as the data custodian of police reports and the Queensland Police Service for sending through reports of suspected suicides.
Author contributions
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The original study on which the present article was based was created through funding from the State of Queensland, managed by Queensland Health (1990 to June 2013) and the Queensland Mental Health Commission (July 2013 onwards). SL received seed funding through The University of Queensland Medical School to complete this study.
Ethical approval and informed consent statements
This research was conducted under ethical approval from the State of Victoria’s Department of ’s Justice Human Research Ethics Committee (NCIS M0112 and JHREC CF/18/12771) and the secondary ethical clearance (prior review) from Griffith University’s HREC (GU Ref No: 2010/537).
Data availability statement
Due to ethics restrictions, it is not possible to share the data.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
