Abstract
Objective:
Chronic diseases are a major challenge in Australia, contributing to disability, premature mortality, and a significant healthcare burden. This burden is intensified when depression, a common mental health issue, co-occurs with chronic diseases. This scoping review aimed to investigate the relationship between depression and comorbid chronic diseases, namely cardiovascular disease (CVD), diabetes, asthma, and chronic obstructive pulmonary disease (COPD) in the Australian population.
Methods:
Following Joanna Briggs Institute (JBI) methodology, this scoping review searched for English-language articles published between January 2013 and December 2023. The review targeted studies examining depression and selected comorbid chronic diseases within the Australian population. Two independent reviewers conducted data screening and extraction, with results synthesised into tables and summarised narratively.
Results:
The search yielded 31 quantitative studies, highlighting a high prevalence of depression co-occurring with chronic diseases. Key findings included the worsening of chronic disease severity by depression, compounded by gender and age disparities, and the impact of socioeconomic factors impairing the quality of life. The review also identified significant challenges in the provision of care, particularly in rural areas, emphasising the need for integrated care models, and enhanced healthcare training.
Conclusion:
This review revealed critical research gaps in understanding the relationship between depression and chronic diseases, particularly regarding underrepresented groups such as younger adults and rural populations. It highlights the need for improved diagnostic criteria, treatment approaches, and professional training, advocating for targeted research and policy interventions to improve outcomes and quality of life for individuals with depression and selected comorbid chronic diseases.
Introduction
Multi-morbidity is the presence of two or more disorders in an individual at a time, which can include both physical and mental health conditions. It presents numerous challenges such as increased disease burden, elevated management costs, and diminished quality of life (Harris et al., 2018; Valderas et al., 2009). The prevalence of multi-morbidity is escalating in the general Australian population, with higher rates observed among women, the elderly, and individuals from socioeconomically disadvantaged backgrounds (Australian Institute of Health and Welfare [AIHW], 2023b). According to the AIHW, 1 in 5 Australians had multi-morbid chronic conditions in 2017–2018 (AIHW, 2023b). A gender disparity was noticeable with females (22.8%) experiencing a higher prevalence than males (17.7%) (AIHW, 2023b). Multi-morbidity frequency also increases with age, rising to about 1 in 2 individuals aged 65 and above (AIHW, 2023b).
Chronic diseases, such as cardiovascular disease (CVD), chronic obstructive pulmonary disease (COPD), type 2 diabetes mellitus (T2DM), and asthma, have emerged as primary drivers of disability and premature mortality in Australia (Australian Health Ministers’ Advisory Council, 2017; World Health Organization, 2022). The conditions not only have high prevalence but also pose serious risks of premature death and hospitalisations, making them a priority for prevention and management in primary care settings (Australian Commission on Safety and Quality in Health Care, 2021; AIHW, 2023a). Together with mental and behavioural conditions, these chronic diseases accounted for 89% of deaths and contributed to 66% of the total disease burden in 2021 (Australian Bureau of Statistics, 2023; AIHW, 2023b). Chronic disease rates in Australia’s rural and remote areas compared to urban regions for CVD (6.6% vs 5.4%), diabetes (6.7% vs 5.8%), asthma (12.2% vs 11.2%), COPD (6.8% vs 3.9%), mental and behavioural conditions (32.6% vs 27.5%) are found to be disproportionately higher (AIHW, 2024).
Mental illnesses, particularly depressive disorders, often co-occur with chronic diseases. Depressive disorders, the sixth leading cause of disease burden in Australia in 2023, disproportionately affects females and individuals aged between 5 and 44 years (AIHW, 2023a). Approximately 2.4 million Australians live with both a mental health condition and a chronic disease, representing around 9.3% of the population (AIHW, 2023b; Harris et al., 2018). This comorbidity is common in individuals with multi-morbidity, further complicating disease management (Sharpe et al., 2017).
The interaction between depression and chronic diseases creates a vicious cycle, where each condition exacerbates the other, leading to worse health outcomes and greater strain on the healthcare system (Herrera et al., 2021). Primary healthcare providers, who are central to Australia’s healthcare system, are crucial in managing these comorbidities (AIHW, 2018). However, rural populations face significant barriers to accessing appropriate healthcare, such as workforce shortages, limited infrastructure, geographical distances, and stigma surrounding mental health (AIHW, 2023c; AIHW, 2024; Queensland Mental Health Commission, 2018).
Effective management of co-occurring depression and chronic diseases requires a better understanding of the relationship between these conditions in the general Australian population. This scoping review was conducted to answer the research question: ‘What does the current literature reveal about the relationship between depression and selected chronic physical health diseases in the general Australian population?’
Methodology
A scoping review was conducted to explore the relationships between depression and chronic physical health diseases within the broader Australian population, particularly focusing on CVD, diabetes, and chronic respiratory diseases, such as asthma and COPD. Although common or pertinent, other chronic physical health diseases like cancer, chronic kidney disease (CKD), and musculoskeletal diseases were not the focus of this review. While CKD and cancer contribute significantly to the health burden, they often require more specialised care beyond the scope of primary care. Although cancer remains a leading cause of disease burden, its rank has decreased over the past two decades (2003–2023) (AIHW, 2023a), reflecting improvements in early detection and treatment. This contrasts with the relatively stable or increasing burden associated with heart diseases, respiratory diseases, and diabetes, which continue to rank within 1 to 12 and are among the top causes of fatal burden (AIHW, 2023a). Musculoskeletal diseases, while highly prevalent, largely contribute to non-fatal outcomes focused more on quality of life than on mortality (Australian Institute of Health and Welfare, 2023a).
The scoping review adhered to the Joanna Briggs Institute (JBI) methodology (Peters et al., 2020) specifically designed for conducting scoping reviews and aimed at revealing current knowledge gaps and proposing potential areas for future research. A protocol for conducting a scoping review was developed following the guidelines set by JBI Evidence Synthesis (Peters et al., 2020). The scoping review protocol is provided in Supplementary Appendix III.
Search strategy
An initial search of the Cochrane Database of Systematic Reviews and JBI Evidence Synthesis yielded no evidence of ongoing or completed systematic or scoping reviews on the topic that specifically included only an Australian population sample. A systematic search strategy was subsequently implemented using the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) for scoping review extension guidelines (PRISMA-ScR) (Page et al., 2021).
An initial search of Google Scholar and PubMed identified relevant articles to develop a comprehensive search strategy for multiple databases. The search included English-language studies published between January 2013 and December 2023. This time frame was opted as it reflects the most recent decade of research, ensuring that the review focuses on the latest developments in understanding the comorbidity of depression and chronic diseases.
The key databases searched were PubMed, EMBASE, PsycINFO (EBSCO), and SCOPUS. The search strategy included studies focused only on the Australian Population. A full search strategy is provided in Supplementary Appendix I.
After the searches, citations were imported into EndNote 20 (Clarivate Analytics, PA, USA) (The EndNote Team, 2013), then screened using Covidence (2023), a web-based tool designed to streamline the systematic review process, facilitating the importation, screening, and data extraction of studies. Two independent reviewers, GS and BN, screened titles and abstracts against the inclusion criteria. The full texts were assessed for citations that met these criteria. Discrepancies were documented and resolved through discussion.
Eligibility criteria
The eligibility criteria for the review are outlined in Table 1.
Eligibility criteria.
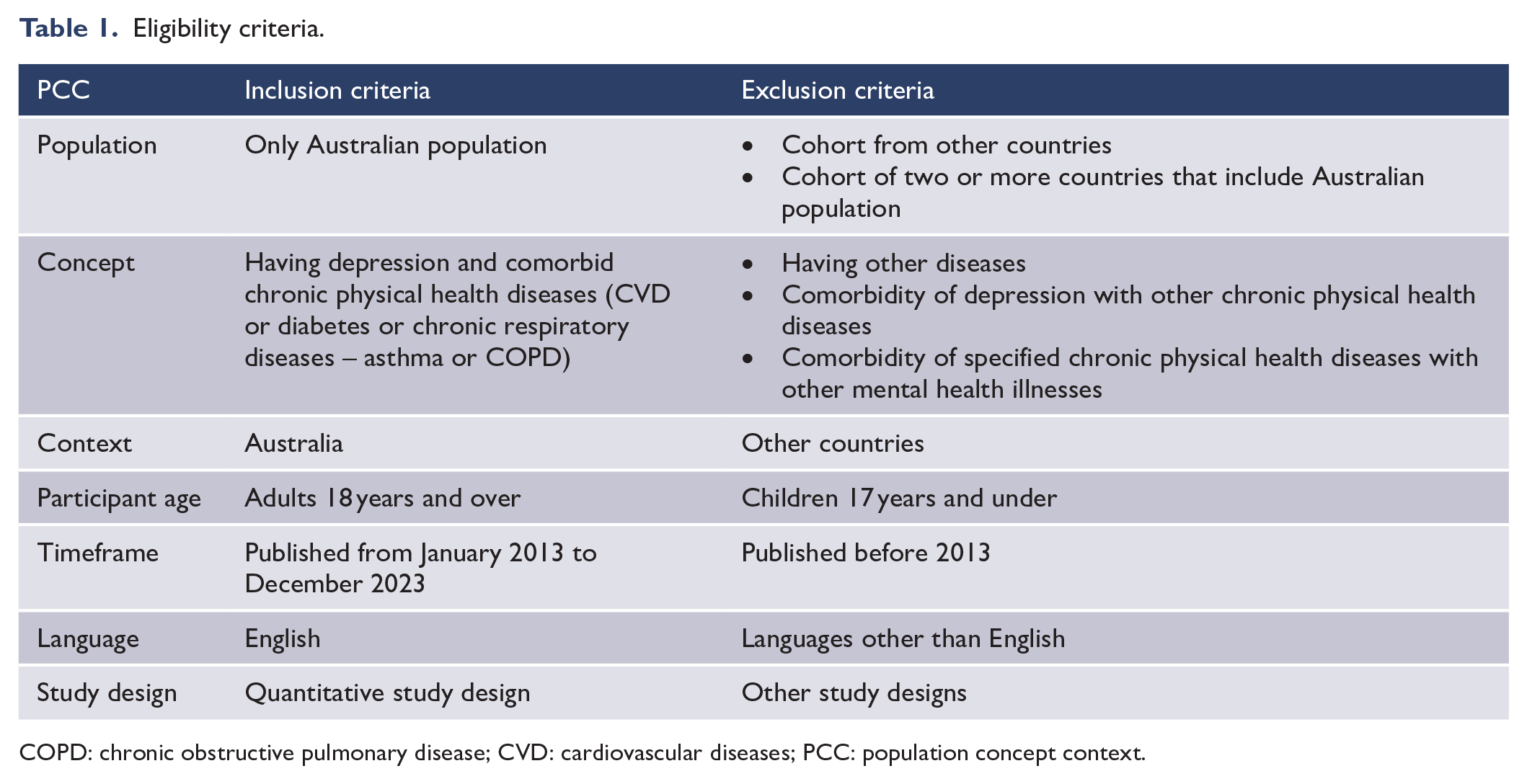
COPD: chronic obstructive pulmonary disease; CVD: cardiovascular diseases; PCC: population concept context.
Data extraction
A standardised data extraction template in Covidence (2023) was adapted to extract the relevant information from the selected studies. The extracted results are presented in tables and supplemented by a narrative summary organised according to the research question. This narrative elucidates the connections between the results and the review’s objective, discussing implications for practice and policy, limitations, and future research directions, with a specific focus on rural populations in Australia.
Results
The screening process is detailed in the PRISMA flow diagram (Figure 1) (Page et al., 2021), and the PRISMA Extension for Scoping Reviews (PRISMA-ScR) Checklist (Tricco et al., 2018) is available in Supplementary Appendix II. Following the searches, 31 relevant articles were identified. These studies encompassed several chronic diseases, including CVD (n = 12), diabetes (n = 8), asthma and COPD (n = 5), and multi-morbidity (n = 6). An overview of the included studies, their characteristics, and main findings is presented in Table 2. A summarised description of study characteristics is provided in Table 3. While the majority of these studies focused on general Australian populations, six specifically examined the relationship between depression and selected chronic physical health diseases in rural settings (Srinivasan et al., 2024).
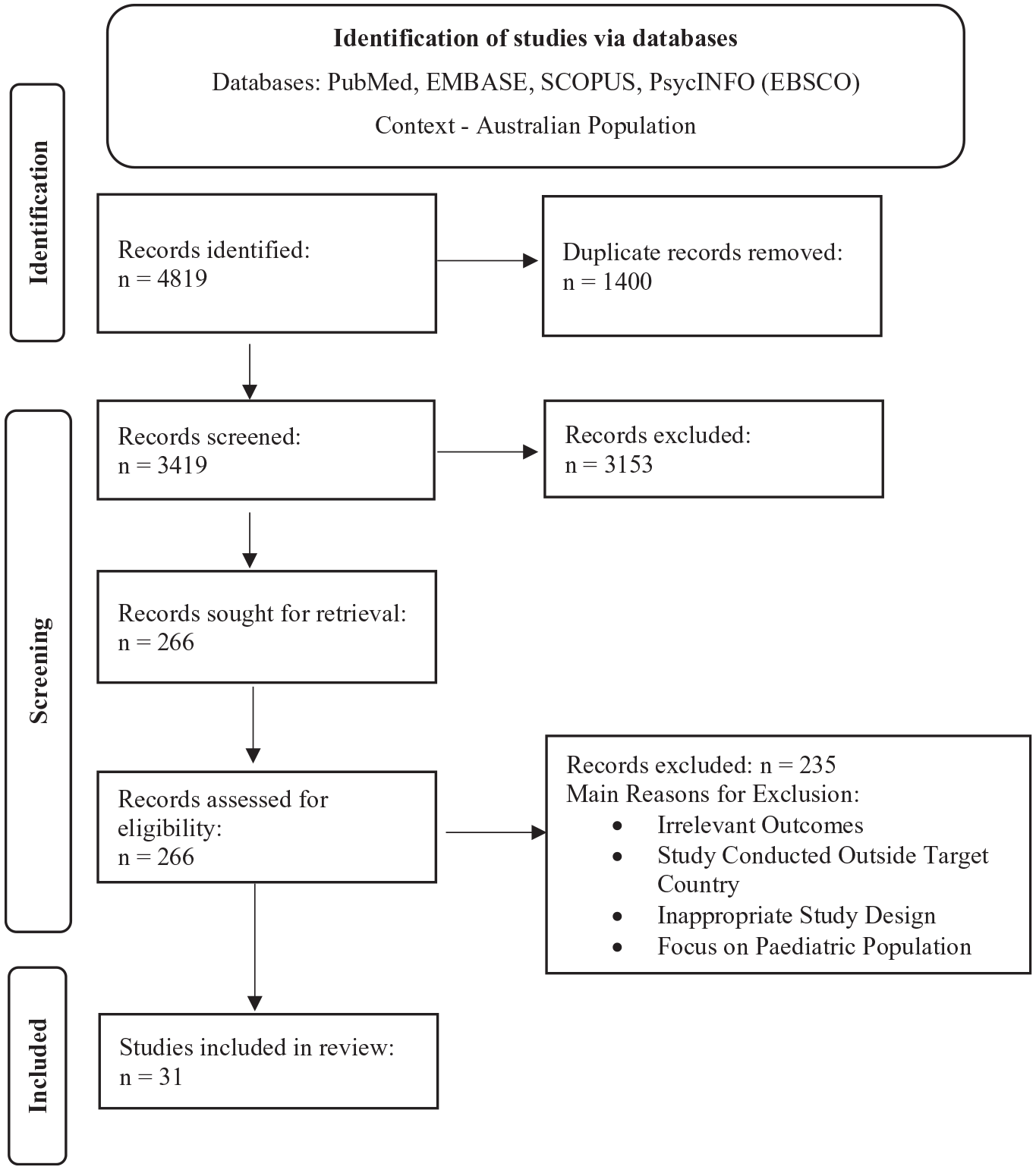
Preferred reporting items for systematic reviews and meta-analyses (PRISMA) flow chart.
Summary of studies.
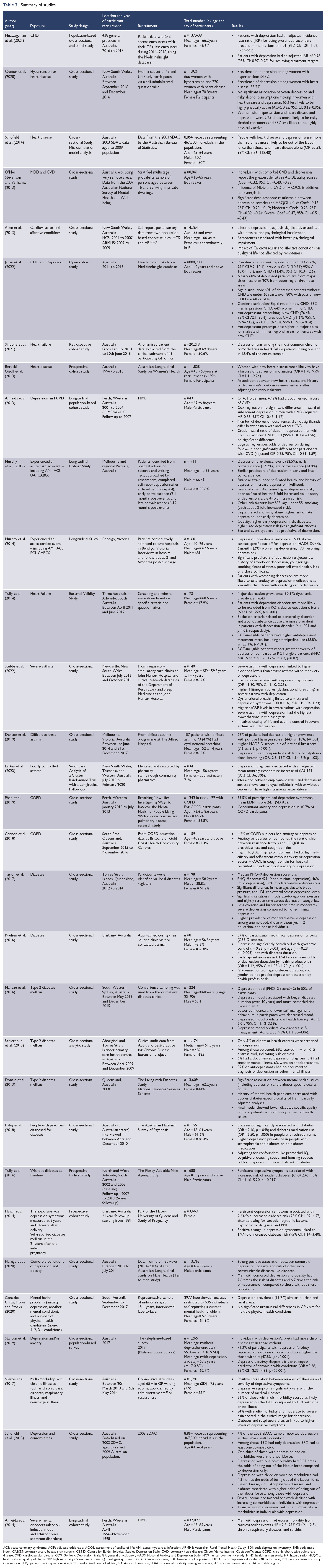
ACS: acute coronary syndrome; AOR: adjusted odds ratio; AQOL: assessment of quality of life; AMI: acute myocardial infarction; ARMHS: Australian Rural Mental Health Study; BDI: beck depression inventory; BMI: body mass index; CABGS: coronary artery bypass graft surgery; CES-D: Centre for Epidemiological Studies-Depression Scale; CHD: coronary heart disease; CI: confidence interval; Coef: coefficients; COPD: chronic obstructive pulmonary disease; CVD: cardiovascular disease; GDS: Geriatric Depression Scale; GP: general practitioner; HADS: Hospital Anxiety and Depression Scale; HCS: hunter community study; HIMS: health in men study; HR: hazard ratio; HRQOL: health-related quality of life; hsCRP: high sensitivity C-reactive protein; IQ: intelligent quotient; IRR: incidence rate ratio; LDL: low-density lipoproteins; MDD: major depressive disorder; OR: odds ratio; PCI: percutaneous coronary intervention; PHQ: patient health questionnaire; RCT: randomised controlled trial; SD: standard deviation; SDAC: survey of disability, ageing and carers; SES: socioeconomic status; UA: unstable angina.
Summarised study characteristics.
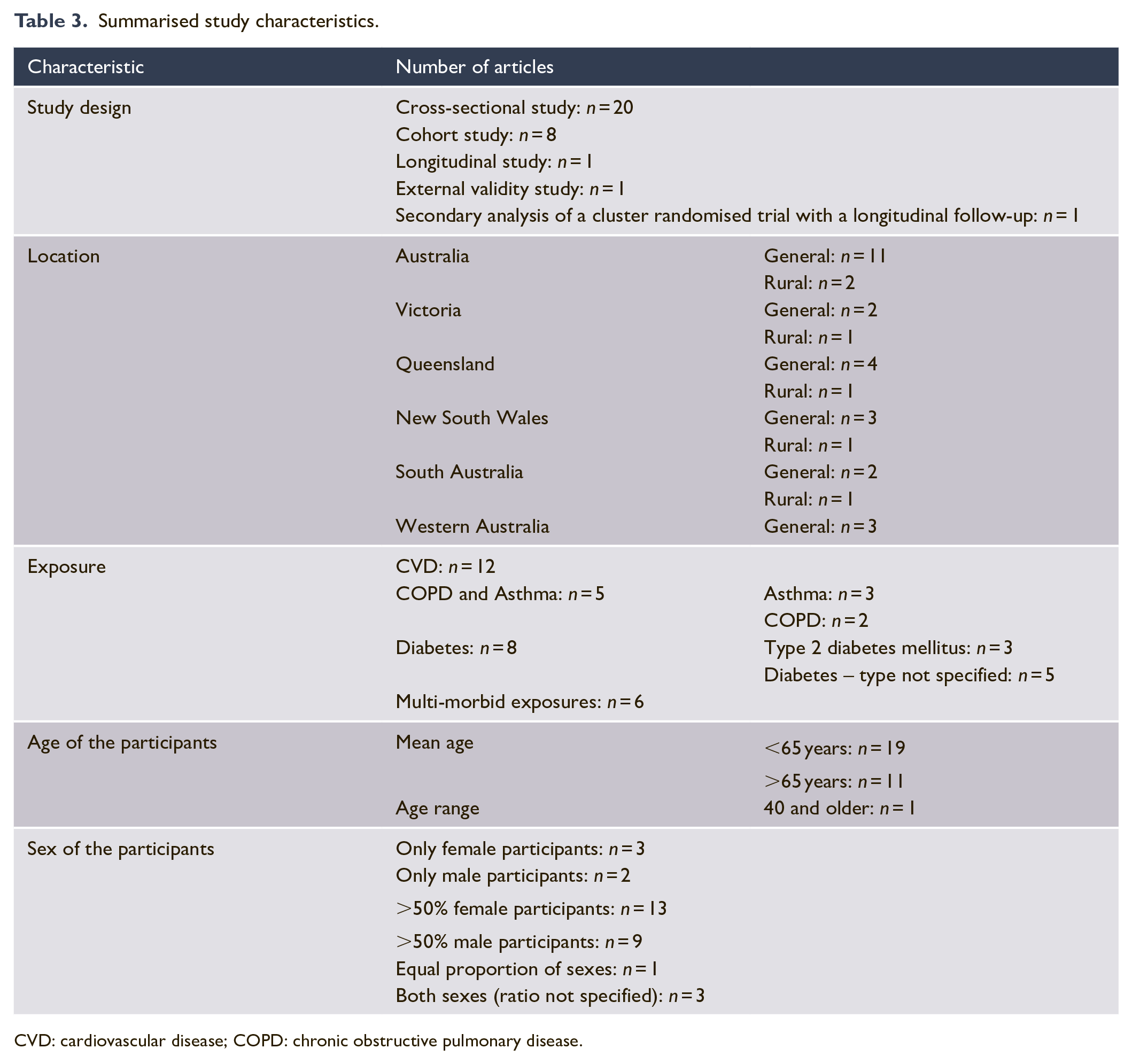
CVD: cardiovascular disease; COPD: chronic obstructive pulmonary disease.
Study design, location, and population demographics
A significant portion of the studies utilised cross-sectional designs (n = 20), with cohort studies accounting for eight articles. Studies were geographically diverse, with the majority conducted in general Australian settings. Only six studies focused explicitly on rural populations. Among the 31 studies reviewed, only two studies explicitly addressed Aboriginal and Torres Strait Islander populations, pointing to a significant underrepresentation of Indigenous groups in the literature (Schierhout et al., 2013; Taylor et al., 2017).
The majority of the studies included older adults, with 19 studies involving populations with a mean age of less than 65 years and 11 studies with a mean age of greater than 65 years (Table 3). In terms of specific diseases, the studies having participants over the mean age of 65 were found more only in CVD and COPD.
The gender distribution across the studies showed a higher representation of female participants in the majority of studies, with 16 studies including more females and 11 studies including more males (Table 3). CVD and T2DM had a higher number of studies with more male participants, while other diseases had more studies with a greater proportion of female participants.
Depression and selected chronic physical health disease comorbidity
Depression is a highly prevalent condition among patients with CVD, diabetes, COPD and severe asthma (Cannon et al., 2018; Cramer et al., 2020; Denton et al., 2019; Foley et al., 2018; Haregu et al., 2020; Hasan et al., 2014; Jahan et al., 2022; Maneze et al., 2016; Murphy et al., 2019; Murphy et al., 2014; Phan et al., 2019; Schierhout et al., 2013; Schofield et al., 2013; Sharpe et al., 2017; Sindone et al., 2021; Stanton et al., 2019; Tully et al., 2016; Tully et al., 2014). It is one of the most common comorbidities in people with more than one disease (multi-morbidity) (Sharpe et al., 2017). This indicates that depression should be considered as an integral part of managing chronic disease treatment. Clinicians should diagnose depression and consider its impact on the treatment of these diseases.
Research also indicates that a diagnosis of depression is a major predictor of chronic diseases, particularly diabetes, CVD, and dysfunctional breathing in severe asthma (Denton et al., 2019; Hasan et al., 2014; Stanton et al., 2019; Tully et al., 2016). Therefore, it is essential for GPs and mental health professionals who treat patients with depression to regularly monitor them for the development of chronic physical health diseases.
Impact on health outcomes
Depression has a substantial impact on the health outcomes of individuals with chronic physical health diseases. Depression significantly affects health outcomes by exacerbating the severity of chronic physical health disease. Depression impairs health-related quality of life (HRQOL) among individuals with comorbid conditions such as CVD and severe asthma (Cannon et al., 2018; Maneze et al., 2016; O’Neil et al., 2013; Stubbs et al., 2022). Individuals with comorbid depression and heart diseases were more likely to be out of the labour force (Schofield et al., 2014). Depression not only worsens disease symptoms but also diminishes self-management capabilities and overall quality of life. These findings suggest that interventions targeting depression and chronic physical health diseases should be considered to improve overall health outcomes.
Socioeconomic and demographic factors
The evaluation of socioeconomic and demographic factors has revealed that financial strain, poor self-rated health, and social isolation markedly increase the risk of depression (Murphy et al., 2019). The prevalence and impact of depression is significantly influenced by factors such as age, sex, lifestyle, and socioeconomic status among individuals with chronic physical health diseases such as CVD, specifically coronary heart disease (CHD) and diabetes (Almeida et al., 2013; Berecki-Gisolf et al., 2013; Cramer et al., 2020; Jahan et al., 2022; Lartey et al., 2023; Murphy et al., 2019; Poulsen et al., 2016; Schofield et al., 2013). Older adults and women, particularly those recently diagnosed with CHD, have a higher prevalence of depression, which is exacerbated by lifestyle factors such as reduced physical activity and alcohol consumption behaviours (Almeida et al., 2013; Berecki-Gisolf et al., 2013; Cramer et al., 2020; Jahan et al., 2022). Moreover, depression has a significant impact on socioeconomic outcomes, leading to increased healthcare expenditures and reduced workforce participation (Lartey et al., 2023; Schofield et al., 2013). This highlights the necessity for not only the clinical aspects of managing depression alongside chronic physical conditions, but also the socioeconomic dimensions to support improved health outcomes and quality of life.
Barriers to care and treatment gaps
The assessment of obstacles to care and treatment disparities discloses crucial shortcomings in managing depression, highlighting a limited patient comprehension of treatment adherence, substantial exclusion of individuals with depression from clinical trials, and low depression screening rates in healthcare settings (Poulsen et al., 2016; Schierhout et al., 2013; Tully et al., 2014). Tully and colleagues revealed that nearly half of patients with depression are excluded from research studies, often due to additional mental health issues or substance abuse, which skews research outcomes and potentially denies those most in need of new treatments (Tully et al., 2014). Furthermore, only a small proportion of patients are screened for depression in health centres, indicating a deficit in routine mental health assessments (Schierhout et al., 2013). This situation emphasises the need for patient education on comprehensive treatment strategies and greater inclusivity in clinical research to ensure findings are representative and applicable.
Rural and remote contexts
The findings related to urban–rural disparities in depression and selected comorbid chronic diseases reveal less about differences in prevalence and more about the quality of life and healthcare access challenges (Allen et al., 2013; Gonzalez-Chica et al., 2020; Jahan et al., 2022; Mnatzaganian et al., 2021; Murphy et al., 2014; Taylor et al., 2017).
Gonzalez-Chica et al. (2020) and Jahan et al. (2022) revealed that the prevalence of depression is surprisingly similar in urban and rural populations. This suggests that factors beyond mere access to healthcare and social services, such as urban living conditions, social isolation, and environmental stressors, may similarly influence the occurrence of depression in both urban and rural settings. However, these findings may not be generalizable at the population level.
Rural residents seem to experience lower levels of psychological impairment than their urban counterparts, which could suggest that individuals in rural areas possess a form of resilience or benefit from lifestyle factors unique to their environment, which might buffer against psychological distress (Allen et al., 2013). Individuals with depression and co-existing heart disease or diabetes in rural areas had a higher likelihood of being prescribed secondary prevention medications (Mnatzaganian et al., 2021). Moreover, lifestyle factors such as physical activity and screen time vary significantly with depression severity, indicating that the effects of depression extend into daily behaviours that can further influence physical health outcomes (Taylor et al., 2017). This aspect is particularly important in the context of chronic diseases, where self-management behaviours are crucial for disease control and quality of life.
Discussion
This scoping review was conducted to explore the relationship between depression and selected chronic physical health diseases in the Australian population. The review reveals that depression exacerbates the burden of chronic diseases such as CVD, diabetes, COPD, and asthma, impairing self-management and treatment outcomes. Depression complicates disease management, resulting in poorer health outcomes. Furthermore, this review highlights gaps in the literature that warrant further investigation.
A demographic trend identified in the literature is the higher number of female participants, particularly in studies focused on CVD, asthma, and diabetes. This is noteworthy as women are more likely to experience depression, especially in the context of chronic disease. However, the lower number of male participants highlights a significant gap in understanding of how depression affects men with chronic diseases. Future research should address this gender imbalance to provide more insights into sex-specific trends in depression and chronic disease management.
Age distribution is another important factor in the literature, with many studies focusing on older adults, particularly in CVD studies. However, there is a clear underrepresentation of younger adults (under 50). Only two studies (Schierhout et al., 2013; Taylor et al., 2017) specifically addressed the Aboriginal and Torres Strait Islander populations, despite well-documented health disparities. This underrepresentation of younger adults (aged under 50) and Indigenous Australians is a significant gap that future research must address to better understand the unique challenges faced by them in managing both depression and selected chronic diseases and to ensure that health interventions are inclusive and culturally appropriate.
Depression’s negative impact on disease management is well-established in the literature, with studies demonstrating how it impairs self-management of chronic diseases and diminishes the effectiveness of treatment strategies. However, current diagnostic tools for depression, particularly in chronic disease contexts, are insufficient (Coorey et al., 2023; Di Benedetto et al., 2014). Screening tools such as the PHQ-9 (Kroenke et al., 2001) could be integrated into chronic disease care settings to improve early detection of depression. Enhanced training for GPs and mental health professionals in recognising and treating this comorbidity is essential for providing timely, holistic care.
Considering the detrimental effect of depression on the management and outcomes of chronic diseases, integrated, and synergistic treatment approaches, such as holistic care models that address both mental and physical health, are essential for improving patient outcomes (Harrison et al., 2016). However, evidence from other countries shows that the success of these models depends on ensuring effective implementation (Baxter et al., 2018; Czypionka et al., 2020; Kumar and Cheng, 2023). The establishment of interdisciplinary teams and improved communication between healthcare providers are crucial for delivering holistic, patient-centred care that meets the complex needs of individuals with comorbidities.
By focusing on publications from 2013 onwards, this review ensures that only studies incorporating contemporary scientific analysis and methods are included. While restricting the search to the last decade may introduce some publication bias by excluding older studies, the inclusion of studies reporting on pre-2013 data mitigates this limitation to an extent. This focus on more recent publications also highlights current research trends, gaps, and emerging insights into the relationship between depression and selected chronic diseases in Australia.
The limitations of current research methodologies, including the reliance on cross-sectional study designs and self-reported questionnaires, are significant barriers to a deeper understanding of depression-chronic disease comorbidity. In the studies reviewed, 20 were cross-sectional in design, limiting their ability to establish causal relationships and temporal dynamics between depression and selected chronic diseases. In addition, many studies used self-reported measures of depression, which can introduce bias and reduce the accuracy of the findings. There are also concerns about the use of datasets collected for purposes other than depression-chronic disease research. This aligns with previous research that has identified similar limitations, including the overuse of cross-sectional designs, reliance on self-reported data, and underrepresentation of key demographic groups (Aw et al., 2020; Bagai et al., 2022; Coorey et al., 2023; Cordova-Rivera et al., 2019; Di Benedetto et al., 2014; Gavino et al., 2018; Handley et al., 2019; Leach et al., 2021).
A notable gap in the literature is the lack of research on the relationship between depression and selected chronic diseases in rural Australian settings. Geographic isolation, limited access to specialised care, and the unique challenges faced by rural healthcare providers may significantly influence disease management and outcomes in these populations. A few studies have reported that lifestyle, socioeconomic status, and rural healthcare delivery models have an effect on depression and selected chronic disease comorbidities. Previous studies have pointed to the lack of representation and tailored approaches for rural areas, which presents a significant gap in understanding how to support these populations (Leach et al., 2021; Mnatzaganian et al., 2021).
Given the gaps identified, there is a pressing need for research employing diverse methodologies, particularly in rural Australian contexts. Large-scale epidemiological comparisons of depression prevalence between urban and rural settings are lacking. Longitudinal and prospective study designs are essential to address gaps and to provide more evidence on the temporal progression of depression and chronic diseases.
Policies and interventions should be designed with a deeper understanding of disparities in healthcare access and socioeconomic status to ensure equitable health services across geographic locations, from rural to urban areas. Ensuring that future research and healthcare strategies are inclusive of underserved populations, including rural residents, Indigenous Australians, and younger adults, is essential for improving health outcomes and addressing the complex interplay between depression and selected chronic physical health diseases.
Conclusion
This scoping review highlights the complex relationship between depression and chronic physical health diseases, namely CVD, diabetes, asthma, and COPD, among the Australian population. Also, it identifies significant gaps in the current literature which include gender and age disparities in study populations, underrepresentation of younger adults and Indigenous Australians, and an overreliance on cross-sectional study designs. To bridge these gaps, there is a need for collaborative efforts to improve diagnostic criteria, treatment approaches, professional training, and interdisciplinary communication to achieve equitable physical and mental health outcomes. Furthermore, this review draws attention to the importance of targeted research and policy interventions that address the unique challenges faced by individuals with comorbidities, particularly in rural areas where access to healthcare is limited. Addressing these issues is essential for improving health outcomes and the quality of life of individuals across Australia, ensuring that future healthcare strategies are inclusive, culturally appropriate, easily adaptable, and responsive to the needs of all populations.
Supplemental Material
sj-docx-1-anp-10.1177_00048674251317336 – Supplemental material for Depression and comorbid chronic physical health diseases in the Australian population: A scoping review
Supplemental material, sj-docx-1-anp-10.1177_00048674251317336 for Depression and comorbid chronic physical health diseases in the Australian population: A scoping review by Gouri Srinivasan, Srinivas Kondalsamy-Chennakesavan, Matthew McGrail, Vikas Garg and Bushra Nasir in Australian & New Zealand Journal of Psychiatry
Supplemental Material
sj-docx-2-anp-10.1177_00048674251317336 – Supplemental material for Depression and comorbid chronic physical health diseases in the Australian population: A scoping review
Supplemental material, sj-docx-2-anp-10.1177_00048674251317336 for Depression and comorbid chronic physical health diseases in the Australian population: A scoping review by Gouri Srinivasan, Srinivas Kondalsamy-Chennakesavan, Matthew McGrail, Vikas Garg and Bushra Nasir in Australian & New Zealand Journal of Psychiatry
Supplemental Material
sj-pdf-3-anp-10.1177_00048674251317336 – Supplemental material for Depression and comorbid chronic physical health diseases in the Australian population: A scoping review
Supplemental material, sj-pdf-3-anp-10.1177_00048674251317336 for Depression and comorbid chronic physical health diseases in the Australian population: A scoping review by Gouri Srinivasan, Srinivas Kondalsamy-Chennakesavan, Matthew McGrail, Vikas Garg and Bushra Nasir in Australian & New Zealand Journal of Psychiatry
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical considerations
Not applicable
Consent to participate
Not applicable
Consent for publication
Not applicable
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
