Abstract
Objective:
While psychosis is considered a risk factor for offending, little is reported about mental health service utilisation in offenders with psychosis and its relationship with reoffending. We examined the association between contact with mental health services and reoffending in those diagnosed with psychosis.
Methods:
We linked health and offending records in New South Wales (Australia) and identified all individuals with a diagnosis of psychosis and a subsequent offence resulting in a non-custodial sentence between 2001 and 2012. We examined the incidence and risk factors for reoffending, and time to reoffending between 2001 and 2015 using Cox regression and Kaplan–Meier survival methods. We specifically examined the association between clinical contact with community mental health services following the index offence and reoffending.
Results:
Of the 7393 offenders with psychosis, 70% had clinical contact and 49% reoffended. There was a linear relationship between an increased number of clinical contacts and reduced risk of reoffending: those with no clinical contact had more than a fivefold risk of reoffending compared to those with the highest number of contacts (adjusted hazard ratio = 5.78, 95% confidence interval = [5.04, 6.62]). Offenders with substance-related psychosis and those convicted of non-violent offences had fewer clinical contacts and higher rates of reoffending when compared with controls (adjusted hazard ratio = 1.29, 95% confidence interval = [1.13, 1.47] and adjusted hazard ratio = 1.26, 95% confidence interval = [1.18, 1.35], respectively).
Conclusion:
This study supports an association between more frequent mental health service use and reduced risk of reoffending. Efforts to enhance mental health service utilisation in those with psychosis who are at a higher risk of reoffending should be promoted.
Keywords
Introduction
Reducing recidivism among prisoner populations is a challenge for the criminal justice system and has been recognised as a priority in the state of New South Wales (NSW), Australia (NSW Government, 2021). Over the past two decades, increasing attention has been given to the development of evidence-based programmes to reduce reoffending (Payne, 2007), but the overall recidivism rate has remained stubbornly high. In 2019–2020, nearly 55% of those released from Australian prisons in the past 2 years returned to corrective settings (Australian Government Productivity Commission, 2021). People with mental illness, including those diagnosed with psychosis, are at high risk of offending and return to the criminal justice system (Butler et al., 2006; Chowdhury et al., 2020; Douglas et al., 2009; Fazel and Grann, 2006; Fazel and Yu, 2011; Nielssen et al., 2019; Steadman et al., 2009). A meta-analysis of 204 studies found that psychosis was associated with a 49% to 68% increase in the odds of violence (Douglas et al., 2009). Pooled data from four studies comparing reoffending in 1121 individuals with psychosis and 71,552 individuals without mental disorders showed that the rate of reoffending was significantly higher in those with psychosis than the comparison group. However, when compared to those with other mental health disorders, a meta-analysis of 23 studies showed no significant difference between the reoffending rate in 2390 individuals with psychosis and 5446 individuals with other mental health disorders (Fazel and Yu, 2011).
Specific programmes exist which are designed to reduce recidivism in people with mental illness (Hayes et al., 2014; Martin, 2017; Morrissey et al., 2016; Stewart et al., 2017). A study in NSW found a lower risk of recidivism in forensic patients who were found not guilty for reason of mental illness and received supervision and treatment (Hayes et al., 2014). Using a whole of population data-linkage study in NSW, we recently showed that the risk of offending was five times greater in the cohort of all individuals diagnosed with psychosis between 2001 and 2012 than a matched comparison group with no such diagnosis (Chowdhury et al., 2020). We examined the effectiveness of the NSW court diversion scheme and found that those with psychosis who received a court order for mental health treatment had a 12% reduction in the risk of reoffending than those who received a punitive sanction (Albalawi et al., 2019). We also showed that contact with mental health services within 30 days following an offence was associated with 17% reduction in the risk of reoffending in the 2-year follow-up period. The risk of reoffending reduced by 30% in men with five or more clinical contacts within 30 days from their offence compared with men with no clinical contact. Only 37% of offenders with a psychosis had an early contact with a mental health service following an offence (Adily et al., 2020).
Several studies have shown a relationship between antipsychotic medication use and reduced rates of reoffending (Baruch et al., 2014; Fazel et al., 2014; Kasinathan et al., 2016; Mohr et al., 2017; Mortlock et al., 2017; Rezansoff et al., 2017). However, antipsychotic medication is only one dimension of effective care for people with psychosis, and these studies have not examined broader health service contacts. Therefore, this study provides the first investigation of the characteristics of a large population of offenders with psychosis who did not receive a custodial sentence (and thus at risk of reoffending in the community) during a 14-year study period. The findings from this follow-up study can inform models of care to reduce reoffending in those with psychosis.
Methods
We used data from a population-based data-linkage study, which examined the relationship between psychosis and offending behaviour using health and justice administrative data collections in NSW. For the purpose of this paper, offending is defined as a criminal charge that is proven in court (NSW Bureau of Crime Statistics, 2019).
Study population
Our study included all individuals in NSW who were diagnosed with psychosis on admission to a hospital or presentation to an emergency department before their index offence between 1 July 2001 and 31 December 2012, and who received a non-custodial sentence (i.e. not involving incarceration in either an adult prison or a juvenile detention centre) or a court outcome with no penalty.
Psychosis was defined using the diagnostic codes from the International Classification of Diseases, Ninth and Tenth Revisions (ICD-9 and ICD-10) for schizophrenia and related psychoses (F20.1–F20.6, F20.8, F20.9, F22.0, F22.8, F22.9, F23.2, F23.3, F23.9, F25.0–F25.2, F25.9, F29 and 295), affective psychoses (F30.2, F31.2, F31.5, F32.3 F33.3, 296.8 and 296.9) and substance-related psychoses (F10.5, F13.5, F14.5, F15.5, F16.5, F19.5, 291 and 292) for admitted patients or the diagnostic codes from Systemized Nomenclature of Medicine – Clinical Terms (SNOMED-CT) that are mapped to ICD-9 and ICD-10 codes for the patients presented to the emergency departments. We aimed to maximise the reliability of the diagnosis by examining all diagnostic records between 1 July 2001 and 31 December 2012 for individuals and applying a hierarchical approach that has been validated by Sara et al. (2014). This involved classifying individuals into the following three categories based on the reported diagnoses: (1) any diagnosis of ‘schizophrenia and related psychoses’ regardless of other types of psychoses, (2) any diagnosis of ‘affective psychoses’ without a diagnosis of ‘schizophrenia and related psychoses’ (3) and any diagnosis of ‘substance-related psychoses’ in the absence of a diagnosis of other types of psychoses.
Data sources
We used three health administrative data collections to identify clinical contacts with mental health services: the NSW Admitted Patient Data Collection (APDC), the NSW Emergency Department Data Collection (EDDC) and the NSW Mental Health Ambulatory Data Collection (MH-AMB). The APDC and EDDC were used to identify the study population.
The APDC diagnostic data were available between 1 July 2001 and 31 December 2012, while EDDC data were available between 1 January 2005 and 31 December 2012. In the period studied, more than 95% of all NSW emergency department contacts were captured in the EDDC. Only very small rural emergency departments and polyclinics had not implemented electronic data systems that would have contributed to EDDC between 2005 and 2012 (NSW Health, 2020). Eighty-five percent of psychosis diagnoses were identified from the APDC. Any hospital admission time in APDC was removed from time-at-risk for the reoffending analysis. Mental health service contacts from the MH-AMB data collection were identified for the period between 1 July 2001 and 31 December 2014. We removed certain administrative codes such as those related to opening and closing requests, transport and accompanying clients, and recordings of missed appointments to ensure that only data for clinical contacts were included.
We used the NSW Bureau of Crime Statistics and Research’s Reoffending Database (ROD) to identify the presence and date of an index offence and any reoffence (excluding minor traffic offences) between 1 July 2001 and 30 June 2015. We used the NSW Registry of Births, Deaths and Marriages (RBDM) to identify and censor those who died during the study period between 1 July 2001 and 30 June 2015.
The linkage process
The linkage was performed by the NSW Centre for Health Record Linkage (CHeReL). Data custodians provided CheReL with demographic details for each record in their dataset such as name, address, a date associated with the address, sex and date of birth together with an encrypted source record number. CheReL used these personal identifiers and applied probabilistic matching techniques to identify records that are likely to belong to the same person. CheReL assigned a project-specific person number (PPN) to records that were found to belong to the same person. Data custodians received the PPNs and used them to extract the approved information for the researchers.
Statistical analysis
Characteristics of the study population at the time of index offence (baseline) and clinical contact with mental health services during the follow-up period were summarised using descriptive statistics (median, interquartile range [IQR] and proportions). Differences in proportions of categorical variables between men and women, and those with clinical contact and no clinical contact with mental health services during the follow-up period examined using Pearson’s chi-square tests. Predictors of reoffending during the follow-up period were identified for the cohort, and separately for men and women using Cox proportional hazard models. The proportional hazards assumption was examined and there was no evidence that this assumption was violated (p > 0.05).
Potential confounders in the Cox proportional regression models to adjusted hazard ratios (aHRs) included psychosis type, age group at the time of index offence, marital status, country of birth, Indigenous status and the Index of Relative Socioeconomic Disadvantage (IRSD) of the area of residence. IRSD is one of the four Socio-Economic Indexes for Areas (SEIFA) and ranks geographic areas in Australia according to relative socio-economic advantage and disadvantage using census data on income, education, employment, occupation and housing (Australian Bureau of Statistics, 2018). We used the IRSD ranks of the individuals’ geographic areas of residence at the time of the most recent diagnosis. Ten IRSD ranks of the individuals’ areas of residence were grouped into ‘disadvantage’ (IRSD scores = 1–5) and ‘advantage’ (IRSD scores = 6–10). Contact with mental health services was included in the regression models as the primary variable of interest and a fixed variable. For each individual in the cohort, the follow-up period was the time to a second offence or death following the court finalisation date for the index offence, whichever occurred first. For individuals who died during the study period without reoffending, the number of clinical contacts was counted from the time of the index offence to the time of death. For individuals who were alive with no second offence during the study period, the follow-up was the time between the finalisation court date for the index offence and end of the study period (30 June 2015).
Sensitivity analysis was conducted by removing individuals who had their court finalisations for index offence between 1 January 2012 and 31 December 2012 to maximise capturing follow-up contacts from APDC, EDDC and MH-AMB databases.
Time to reoffending was examined in those who had mental health service contact and those who did not by comparing the median survival time to second offence using Kaplan–Meier survival curves. Time to reoffending by type of offence (violent and non-violent: the Australian and New Zealand Standard Offence Classification [ANZSOC] defines violent offences a homicide and related offences; acts intended to cause injury; sexual assault and related offences; dangerous or negligent acts endangering persons; abduction, harassment and other offences against the person; and robbery, extortion and related offences, and non-violent offences are unlawful entry with intent/burglary; break and enter; theft and related offences; fraud, deception and related offences; Illicit drug offences; prohibited and regulated weapons and explosives offences; property damage and environmental pollution; public order offences; traffic and vehicle regulatory offences; offences against justice procedures; government security and government operations; and miscellaneous offences; Australian Bureau of Statistics, 2011) and type of psychosis were compared for those with and without clinical contact with mental health services during the follow-up.
The authors assert that all procedures contributing to this work comply with the ethical standards of the relevant national and institutional committees of human experimentation and with the Helsinki Declaration of 1975, as revised in 2008. All procedures involving human subjects/patients were approved by the NSW Population & Health Services Research Ethics Committee (HREC/15/CIPHS/17), NSW Aboriginal Health and Medical Research Council (1089/15), Justice Health and Forensic Mental Health Network (G324/14) and Corrective Services NSW (D15/138715). A waiver of consent for the linkage of study participants’ data was granted by the NSW Population & Health Services Research Ethics Committee.
Results
Characteristics of the study population
A total of 7393 offenders with psychosis were included in the analysis (70% men and 30% women; Table 1). Over two-thirds of the cohort (67%) had a diagnosis of schizophrenia and related psychoses, followed by substance-related psychoses (22%) and affective psychoses (11%). A higher proportion of men than women were diagnosed with schizophrenia and related psychoses (69% vs 62%). Conversely, women were slightly more likely than men to be diagnosed with substance-related psychoses (24% vs 22%) and affective psychoses (14% vs 9%) (Table 1).
Baseline characteristics of the study population and their contact with mental health services during the follow-up period, by sex.
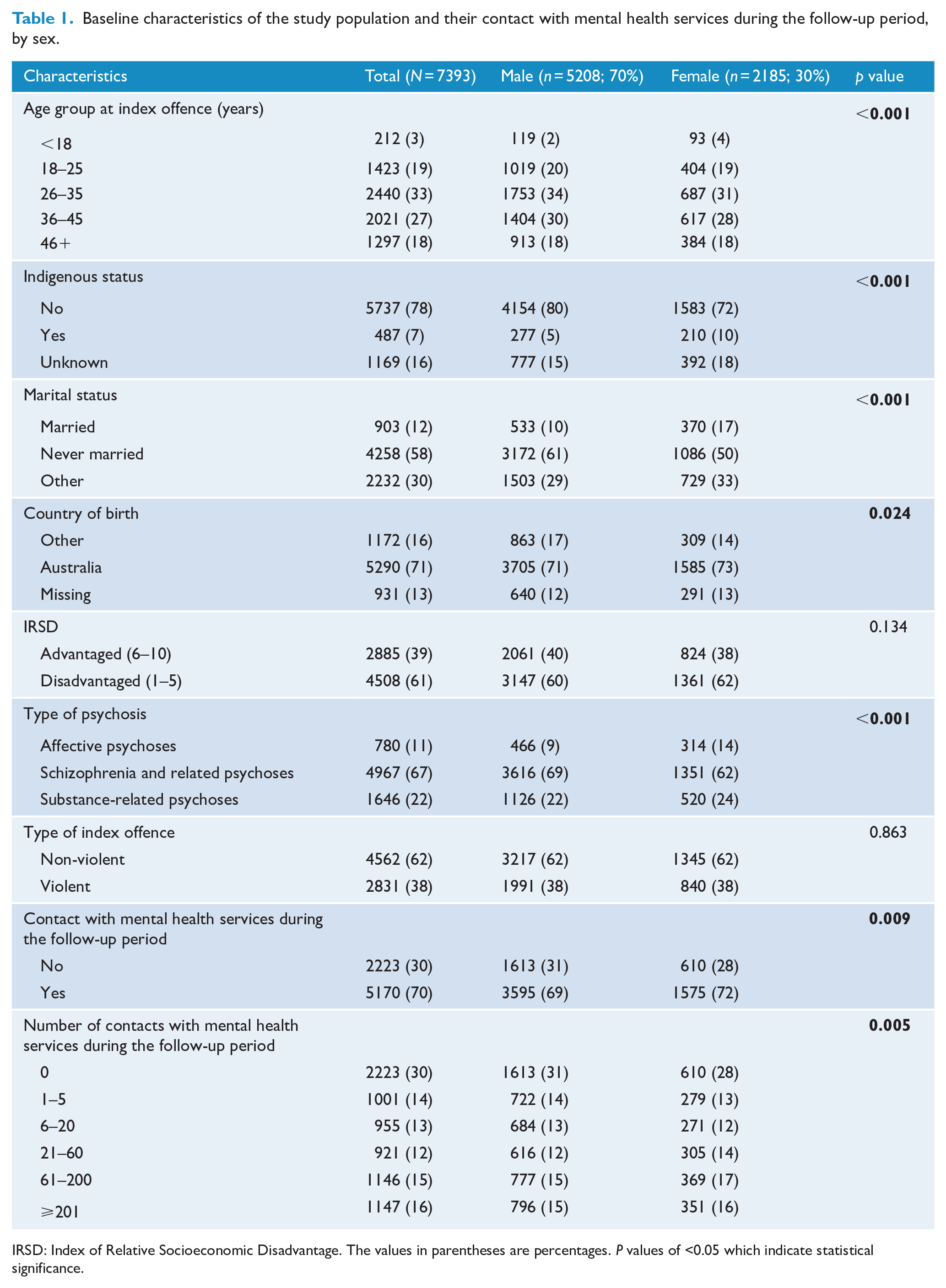
IRSD: Index of Relative Socioeconomic Disadvantage. The values in parentheses are percentages. P values of <0.05 which indicate statistical significance.
While most index offences were non-violent (62%; Table 1), nearly 30% involved violent acts intended to cause injury. Theft was the most frequent non-violent index offence (12.5%). The proportion of violent and non-violent index offences was similar among men and women.
Seventy percent of the study population had at least one mental health service contact during the study period, slightly higher in women (72%) than men (69%) (Table 1). The median number of mental health service contacts was 45 (IQR: 9–171). The median number of days from the court finalisation date (i.e. the date when the matter finishes in court) for the first offence to the first contact with mental health services during follow-up was 30 days (IQR: 4–173). Most (98%) clinical contacts during the follow-up occurred at community mental health services rather than involving admission to hospital (1.7%), or emergency rooms (0.3%). Our analysis showed that fewer individuals with substance-related psychoses (55%) had mental health service contacts than those with schizophrenia and related psychoses (75%) or affective psychoses (70%). Contact with mental health services was associated with the type of offence, with more violent offenders having contact than non-violent offenders (74% vs 67%; Table 2).
Baseline characteristics of the study population by contact with mental health services during the follow-up period.
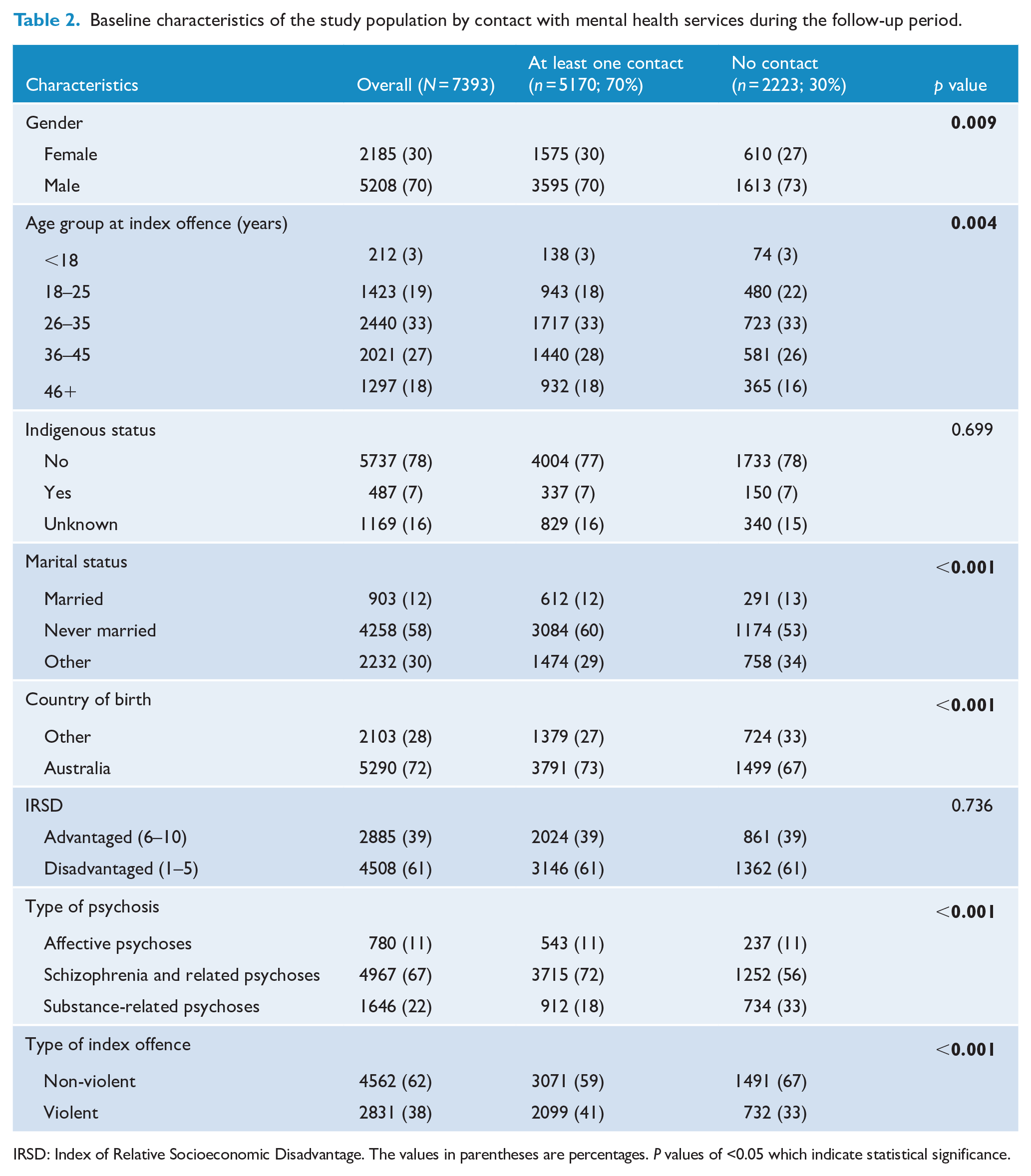
IRSD: Index of Relative Socioeconomic Disadvantage. The values in parentheses are percentages. P values of <0.05 which indicate statistical significance.
Reoffending rate
Just less than half of the cohort (49%) reoffended during the study period with over half of second offences (66%) being non-violent. Similar to the index offence, the most common second offences were acts intended to cause injury (25%). The most frequent non-violent offences were those against justice procedures, government security and government operations (18%; e.g. breach of a community-based order). Reoffending was slightly higher among men than women during the follow-up period (aHR = 1.18, 95% CI = [1.09, 1.27]; Table 3).
The aHR a for reoffending of the study population during the follow-up period.
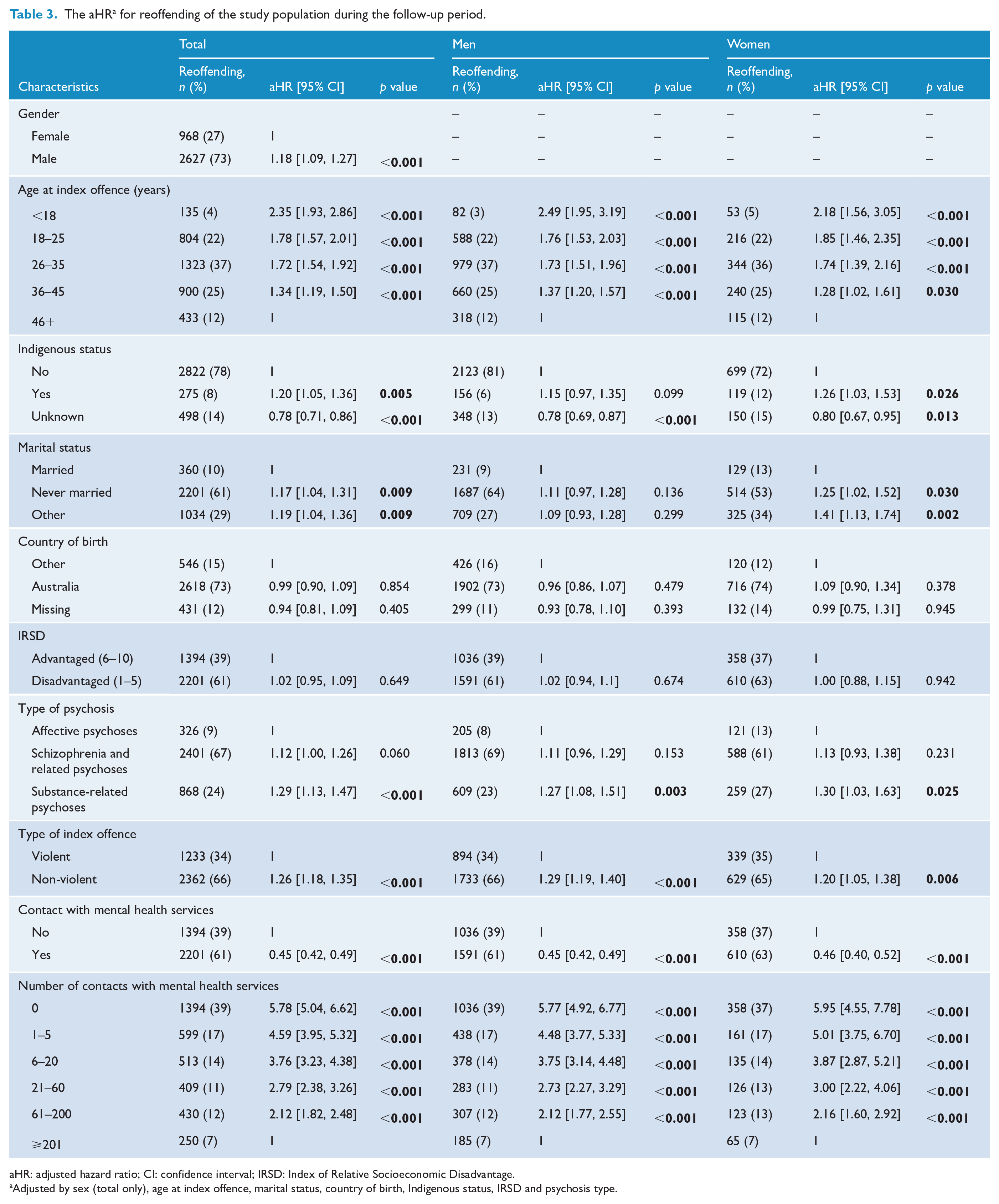
aHR: adjusted hazard ratio; CI: confidence interval; IRSD: Index of Relative Socioeconomic Disadvantage.
Adjusted by sex (total only), age at index offence, marital status, country of birth, Indigenous status, IRSD and psychosis type.
Reoffending among those who had contact with mental health services (clinical contact group) was significantly lower than those with no clinical contact during the follow-up period (aHR = 0.46, 95% CI = [0.43, 0.49]). Incidence of reoffending in the clinical contact group was 7.8 per 100 person–years (95% CI = [7.4, 8.1]), and for the group with no clinical contact, it was 19.1 per 100 person–years (95% CI = [18.1, 20.1]).
Risk factors associated with reoffending in men and women
Younger age was associated with reoffending in both men and women (Table 3). The highest risk occurred in those less than 18 years of age. Compared to women who were married at the time of index offence, the risk of reoffending was higher for those women who were never married (aHR = 1.25, 95% CI = [1.02, 1.52]) and women who had other marital status (e.g. divorced, de facto relationship; aHR = 1.41, 95% CI = [1.13, 1.74]). Indigenous status was also a risk for reoffending among women compared to those of non-Indigenous heritage (aHR = 1.26, 95% CI = [1.03, 1.53]). Living in disadvantaged areas based on IRSD was not associated with reoffending in men or women (Table 3).
The reoffending risk for men and women with substance-related psychoses was higher compared to men (aHR = 1.27, 95% CI = [1.08, 1.51]) and women (aHR = 1.30, 95% CI = [1.03, 1.63]) with affective psychoses (Table 3). The risk of reoffending was higher for men (aHR = 1.29, 95% CI = [1.19, 1.40]) and women (aHR = 1.20, 95% CI = [1.05, 1.38]) with non-violent offences compared with the risk in men and women with violent offences (Table 3). A smaller proportion of those with non-violent offences had contact with mental health services than those with violent offences (33% vs 67%, p < 0.001; Table 2). For both men and women, reoffending was significantly lower for those who had mental health service contact than those who had no contact during the study period (aHR = 0.45, 95% CI = [0.42, 0.49] and aHR = 0.46, 95% CI = [0.40, 0.52], respectively). Furthermore, reoffending decreased with an increase in the number of mental health service contacts in both men and women (Table 3).
Time to reoffending
Time to reoffending following the index offence was examined in the clinical contact group and those with no contact using Kaplan–Meier survival analysis (Figure 1). A longer median survival time between the index and second offence was observed in the clinical contact group (13.56 years, 95% CI = [10.18, 14.03]) than those who had no mental health service contact during the follow-up period (1.69 years, 95% CI = [1.46, 1.98]).
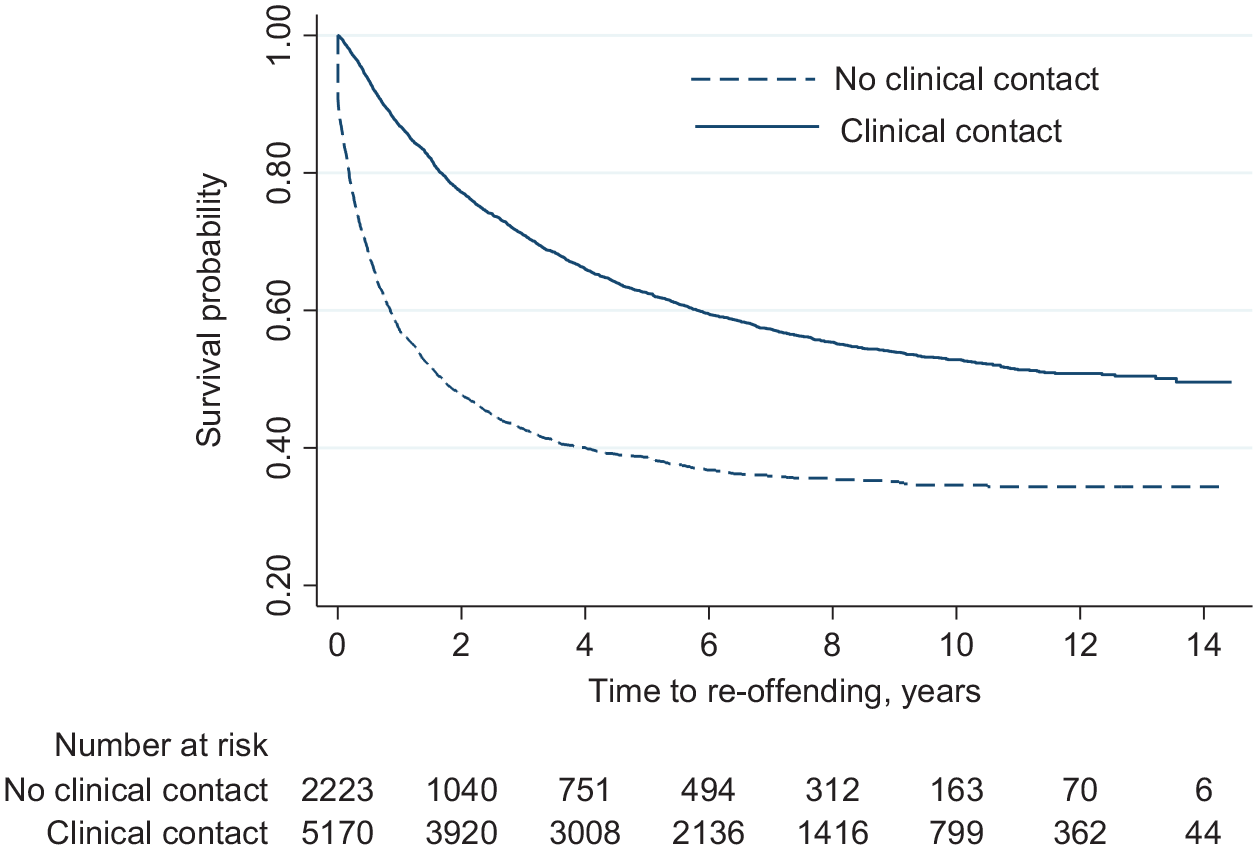
Kaplan–Meier plot of time to reoffending for those with and without clinical contact following their index offence.
The sensitivity analysis which was conducted by removing all 611 individuals who had court finalisation date for their index offence between 1 December 2012 and 31 December 2012 did not show any significant difference in results (Supplementary data).
Time to reoffending was longer for violent offenders who had clinical contact during the follow-up (median survival time = 12.07 years, 95% CI = [11.43, 13.92]) compared to that for violent offenders with no clinical contact (median survival time = 2.59 years, 95% CI = [2.05, 3.53]). Similarly, time to reoffending was longer for non-violent offenders who had clinical contact for mental health treatment (median survival time = 10.94 years, 95% CI = [8.74, 11.50]) than non-violent offenders with no clinical contact with health services (median survival time = 1.41 years, 95% CI = [1.24, 1.68]) (Figure 2).
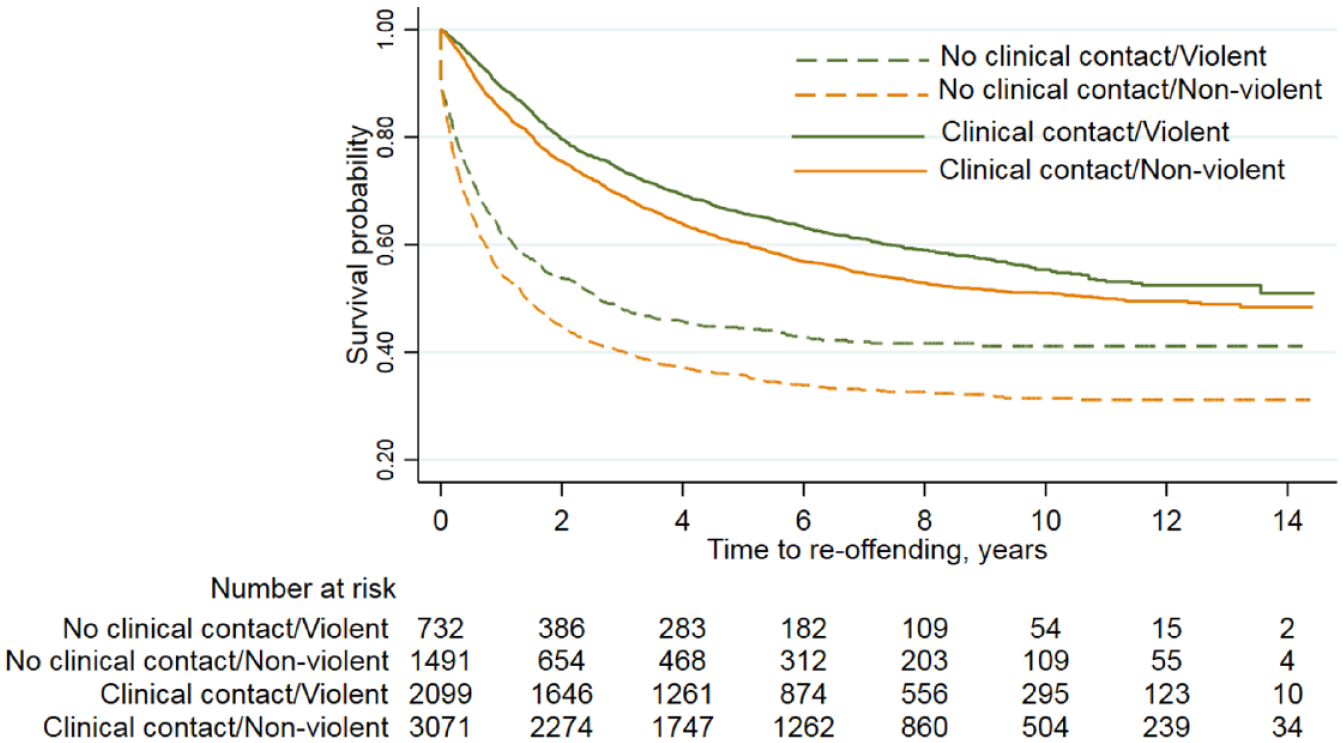
Kaplan–Meier plot of time to reoffending in those with and without contact with mental health services following their index offence by type of index offence.
Discussion
Main findings
This population-based study found an association between increased mental health service contacts and reduced reoffending in those diagnosed with psychosis in NSW. The risk of reoffending was over five times greater in those with no clinical contact with mental health services compared with those with the highest number of contacts (i.e. over 200 contacts) in both the overall and sex stratified analyses.
Our study is unique in following a large population of offenders with psychosis who did not receive a custodial sentence (N = 7393) (and thus at risk of reoffending) during a follow-up period of between 2.5 and 14 years to examine the relationship between their frequency of contact with health services and reoffending. Most of the cohort (70%) had clinical contact with mental health services following their index offence. Overall, most (98%) mental health service contacts occurred at community mental health services rather than emergency rooms or hospital admissions. Half of the index contacts with mental health services occurred within 30 days and 75% occurred within 6 months following the court finalisation date for the index offence.
Just less than half of the study population reoffended during the study period. Of those who reoffended, the median time to reoffending was over 12 times longer for those who had mental health service contact than those with no contact, regardless of the type of psychosis or offence.
Younger age, substance-related psychoses and non-violent offending were identified as risk factors for reoffending in both men and women. We found that fewer individuals with substance-related psychoses (55%) than those with schizophrenia and related psychoses (75%) and affective psychoses (70%) had clinical contact with community mental health services during the follow-up period. These results reflect differences in service models and eligibility criteria. People with substance-related psychosis are more likely to receive treatment by general practitioners or private mental health sector rather than a public hospital or community mental health service.
We previously showed that magistrates appeared less likely to issue treatment orders for those with substance-related psychoses compared to other types of psychosis (Albalawi et al., 2019). This could relate to limited confidence of magistrates about adherence to treatment offered in different service models. The magistrates may not be assured about the preparedness of general practitioners or private clinicians to report the court about the adherence or breaches of treatment plans (Albalawi et al., 2019). This suggests a need for a more assertive approach to follow-up by different service models including general practice, and private and public sectors for those with substance-related psychoses.
Somewhat reassuringly, having a violent offence was associated with increased levels of contact with mental health services. This might reflect the greater emphasis given to follow-up by mental health services in those at risk of harm to others. Not being married and having an Indigenous background were found to be specific risks of reoffending in women. These results suggest enhancing access to mental health services to include at-risk groups, and the need for culturally sensitive mental health services for Indigenous people, and supporting social and occupational management for this group (Mullen, 2006).
Previous studies have examined the impact on reoffending of specific forensic treatment services such as court diversion (Albalawi et al., 2019; Bradford and Smith, 2009; Davidson et al., 2016; McNiel and Binder, 2007; Newitt and Stojcevski, 2009; Skrzpiec et al., 2004; Steadman and Naples, 2005) or post-prison mental health transition programmes (Martin, 2017; Morrissey et al., 2016; Stewart et al., 2017). The current study looks at broader mental health care in the community, examining mainstream community mental health contact, and finds similar associations between receiving treatment and a reduced risk of reoffending. The findings from this study were used to inform a Delphi method designed to identify and describe the key attributes of an ‘optimal model of care’ for those with psychosis leaving prison in NSW by involving experts and consumers (Simpson et al., 2021). The outcomes of this process are currently being incorporated into a multidisciplinary transition care plan for those with psychosis exiting prisons in NSW by engaging multiple agencies including community treatment providers such as community mental health services, drug and alcohol services, and general practitioners, with the aim of preventing returns to custody and improving health, welfare and justice outcomes for this vulnerable and at-risk group (Justice Health and Forensic Mental Health Network, 2020).
Strengths and limitations
The results indicate that increased contact with mental health services has a positive association with reduced reoffending. This does not demonstrate a causal relationship. The association between lower service contact and higher reoffending risk is likely to be confounded by other risk factors, including individual’s personal and family supports, cognitive functioning, organisation, insight and substance use comorbidity. The findings are, however, consistent with previous studies which have shown a positive association between antipsychotic medications use and reduced reoffending (Baruch et al., 2014; Fazel et al., 2014; Kasinathan et al., 2016; Mohr et al., 2017; Mortlock et al., 2017; Rezansoff et al., 2017). Future work could examine the association between the nature of the treatment received, mental health service contact and reoffending.
In quantifying follow-up care, we have given hospital, community and emergency department mental health contacts equal weighting, because there is no consensus method for conversion or weighting of these service types. Exploration of different weightings could be explored in future work. However, impacts of this are likely to be marginal in this study because 98% of all contacts were with community mental health services.
Our cohort did not include individuals who were diagnosed and received treatment outside the public health system by general practitioners, and the private sector. Some diagnoses could be more likely to be managed by general practitioners or private-sector providers. For example, lower rates of follow-up for substance-related psychosis may reflect differences in service models and eligibility criteria, because people with substance-related psychoses do not receive assertive mental health care in all services.
We acknowledge the limitations of available data from administrative data collections. Specifically, the time periods for extraction of diagnostic data from APDC and EDDC were not the same. Offence history and previous diagnoses of psychosis prior to 2001 were not available. We also acknowledge that individuals who leave NSW at any point will have no data available for that period.
Conclusion
While our study cannot demonstrate a causal claim, the findings support the argument that increased care at community mental health services for offenders with psychosis may modify their risk of reoffending. Those with non-violent offences and substance-related psychosis appear to have reduced contact with community mental health services suggesting they ought to be a target of treatment efforts. Those of Indigenous heritage were at higher risk of reoffending suggesting a need for this group to have access to culturally appropriate mental health and other community support services. We recommend ensuring better access to ongoing treatment for these at-risk groups. Further work needs to compare the cost-effectiveness of treatment over punitive sanctions in reducing reoffending by those with psychosis and access to mental health treatments via different service models including community mental health services, private sector and general practice.
Supplemental Material
sj-docx-1-anp-10.1177_00048674221098942 – Supplemental material for Mental health service utilisation and reoffending in offenders with a diagnosis of psychosis receiving non-custodial sentences: A 14-year follow-up study
Supplemental material, sj-docx-1-anp-10.1177_00048674221098942 for Mental health service utilisation and reoffending in offenders with a diagnosis of psychosis receiving non-custodial sentences: A 14-year follow-up study by Armita Adily, Olayan Albalawi, Grant Sara, Azar Kariminia, Handan Wand, Stephen Allnutt, Peter Schofield, David Greenberg, Luke Grant and Tony Butler in Australian & New Zealand Journal of Psychiatry
Footnotes
Acknowledgements
The authors would like to thank the staff of the Centre for Health Record Linkage (CHeReL) who assisted with data linkage. Specifically, the authors would like to thank Ms Kate Irvin and Dr Elizabeth Moore for their technical advice during the linkage process.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship and/or publication of this article: This study was supported by the Mental Health Commission of New South Wales.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
