Abstract
Objective:
Self-harm is closely associated with suicide in older adults and may provide opportunity to intervene to prevent suicide. This study aimed to systematically review recent evidence for three components of aftercare for older adults: (1) referral pathways, (2) assessment tools and safety planning approaches and (3) engagement and intervention strategies.
Methods:
Databases PubMed, Medline, PsychINFO, Embase and CINAHL were searched from January 2010 to 10 July 2021 by two reviewers. Empirical studies reporting aftercare interventions for older adults (aged 60+) following self-harm (including with suicidal intent) were included. Full text of articles with abstracts meeting inclusion criteria were obtained and independently reviewed by three authors to determine final studies for review. Two reviewers extracted data and assessed level of evidence (Oxford) and quality ratings (Alberta Heritage Foundation for Medical Research Standard Quality Assessment Criteria for quantitative and Attree and Milton checklist for qualitative studies), working independently.
Results:
Twenty studies were reviewed (15 quantitative; 5 qualitative). Levels of evidence were low (3, 4), and quality ratings of quantitative studies variable, although qualitative studies rated highly. Most studies of referral pathways were observational and demonstrated marked variation with no clear guidelines or imperatives for community psychiatric follow-up. Of four screening tools evaluated, three were suicide-specific and one screened for depression. An evidence-informed approach to safety planning was described using cases. Strategies for aftercare engagement and intervention included two multifaceted approaches, psychotherapy and qualitative insights from older people who self-harmed, carers and clinicians. The qualitative studies identified targets for improved aftercare engagement, focused on individual context, experiences and needs.
Conclusion:
Dedicated older-adult aftercare interventions with a multifaceted, assertive follow-up approach accompanied by systemic change show promise but require further evaluation. Research is needed to explore the utility of needs assessment compared to screening and evaluate efficacy of safety planning and psychotherapeutic approaches.
Introduction
Suicide prevention for older adults is a complex area which requires a dedicated older-adult focus to address the myriad contributing factors specific to this age group, including physical and mental health, cognitive and functional impairment, interpersonal and social factors (Conejero et al., 2018). There are few interventions to prevent suicide in older people specifically, even though the highest rates of suicide nationally and internationally have been identified among the very old (Australian Bureau of Statistics, 2020; Shah et al., 2016).
A spectrum of suicidal ideation and behaviours exist ranging from the wish to die, to suicidal thoughts and plans, self-harm (including with clear intent to die, i.e. suicide attempts) and suicide (Wand et al., 2018b). However, relationships between these are neither straightforward nor linear. External factors may determine whether self-harm results in death, not just the degree of intent to die (Barnow and Linden, 1997). Furthermore, although rates of completed suicide increase in late life, rates of suicidal ideation and attempts reduce with increasing age (Hawton and Harriss, 2008), and personality traits may differ between people who attempt suicide and those who die by suicide (Bonnewyn et al., 2009). Nonetheless, there is a close connection between self-harm and suicide in older people, with common risk factors for both (Sinyor et al., 2016), and the greater likelihood of death due to use of more lethal methods and greater intent to die compared with younger people (Finkelstein et al., 2015; Miret et al., 2010). Thus, older adults who have self-harmed must be a priority group for suicide prevention initiatives.
Aftercare following self-harm is a potential target area for the development of older-adult-specific suicide prevention initiatives, an important component of the Fifth National Mental Health and Suicide Prevention Plan 2017–2022 in Australia (Department of Health, 2017). Aftercare is defined as access to coordinated follow-up on treatment plans following a suicide attempt or crisis (Shand et al., 2018). Aftercare is explicitly included in suicide prevention programmes because of association of various aftercare components with reduced risk of further suicidal behaviours (Krysinska et al., 2016; Mann et al., 2005). Highlighted beneficial components of aftercare include timely planned follow-up, especially immediately after discharge from acute services to the community, and establishment of genuine engagement, compassion and connection with the suicidal person (Shand et al., 2019). Notably, the latter encouraging but mixed evidence base for aftercare (Shand et al., 2019) is based on broad age groups and the suitability for older persons is unknown. Indeed, the most recent Royal Australian and New Zealand College of Psychiatrists clinical guideline for the management of deliberate self-harm found no randomised controlled trial (RCT) evidence for any treatment to reduce the risk of repeat self-harm in older adults (Carter et al., 2016). Studies evaluating service organisation, outreach and primary care interventions and interventions targeting clinicians to reduce self-harm in older adults were included. It was concluded that a multicomponent, multilayered approach which includes the spectrum of suicidal behaviour and depression in older adults is needed to reduce self-harm (Carter et al., 2016). There is good evidence that the presentation, engagement and needs of older adults are different to younger adults, mandating adaptation of existing suicide prevention models based on evidence derived from older-adult populations. Such evidence (Wand et al., 2018a, 2018b, 2018c, 2019a, 2019b) has elucidated the specific importance of addressing ageism and treatment nihilism among health care professionals, and inclusion of primary care and transition services in the prevention of suicide in older adults (McKay et al., 2021; Wand et al., 2021a).
The aim of this study is to conduct a systematic review to provide an overview of the recent evidence for key components of aftercare of older adults following self-harm (including with suicidal intent), specifically evaluating (1) referral pathways for aftercare, (2) assessment tools and safety planning approaches and (3) engagement and intervention strategies.
Methods
The systematic review was conducted using PRISMA reporting guidelines (Moher et al., 2009). Electronic searches of databases including PubMed, Medline, PsychINFO, Embase and CINAHL were conducted using search terms designed to identify studies reporting self-harm (including with suicidal intent) aftercare in older people between 1 January 2010 and 10 July 2021. The following terms or combination of search terms were used:
‘older people’, or ‘older adults’, or ‘senior’, ‘senior citizen’, ‘elderly’, ‘aged’, ‘old*’, ‘geriatric*’, ‘elder’, ‘late life’, ‘aging’, AND
‘suicide’, or ‘self-harm*’, or ‘self-injur*’, ‘self-destructive behaviour’, ‘self-mutilation’, ‘self-inflicted’, ‘parasuicid*’, ‘overdos*’, ‘attempt* suicid*’ AND
‘aftercare’, or ‘prevention’, or ‘suicide treatment’, ‘engage*’, ‘intervention’, ‘referral’, ‘follow-up’, ‘community intervention’, ‘therapy’, ‘treatment’, ‘crisis intervention’, ‘management’, ‘safety planning’ ‘screening’ or ‘assessment tools’, or ‘checklist’. The search was limited to papers in English. The reference lists of included articles were screened to identify additional eligible studies. In addition to the database searches, reviewers identified other potentially relevant studies from the reference lists of systematic reviews on older persons’ aftercare.
Outcomes of interest
The evidence for each component of aftercare was examined according to the following primary or secondary outcomes:
Primary outcome: Completed suicide or repeat self-harm.
Secondary outcomes: A wide range of other outcomes were evaluated depending on the type of aftercare intervention, including,
● Suicidal ideation; ● Depressive symptoms; ● Rates of referral for follow-up; ● Patient satisfaction; ● Rates of screening for suicidal ideation/behaviours.
Only data relevant to aftercare are reported even when the study measured other aspects.
Inclusion and exclusion criteria
The published peer-reviewed literature was reviewed to identify empirical (original) studies of any design (qualitative or quantitative), which included (1) participants aged 60 years and over (or articles describing a broader-aged cohort but which contained sub-group data on people aged ⩾60), and (2) evaluation of any of the three components of aftercare following self-harm (i.e. referral pathways for aftercare, assessment tools and safety planning approaches, engagement and intervention strategies).
Articles were excluded if they were reviews or meta-analyses, commentaries, editorials or letters or from the grey literature. Studies which described aftercare for people aged <60 years or included older adults within a broader-aged cohort but without separate analysis of data for people ⩾60 were excluded.
Assessment of quality
Two authors (R.B., A.P.F.W.) scored all included papers for quality, working independently. Differences in scoring were discussed until consensus was reached and a final rating was determined. Quantitative studies were appraised for quality using the Alberta Heritage Foundation for Medical Research Standard Quality Assessment Criteria (Kmet et al., 2004). The scoring system provides a framework for assessing the quality of studies of various methodologies. The checklist includes items such as study design and appropriateness, method of subject selection, random allocation and blinding, outcome measures, statistical methods (including confounding and estimates of variance) and reporting of results and conclusions. A formula is used to derive a final rating score, which is expressed as a percentage. Although there is no accepted cut-off for quality rating scores, other systematic reviews have defined >80% as high quality (Lee et al., 2008, 2020).
Qualitative studies were rated using the checklist developed by Attree and Milton (2006). The checklist was designed for qualitative systematic reviews. It evaluates aspects of methodological quality such as research aims and objectives, appropriateness of study design, sampling methods, data collection, analysis and results, reflexivity, value and usefulness of the study and ethical considerations. Each of the checklist items is rated from A (no or few flaws) to D (significant flaws threatening the validity of the entire study), with the final quality score (A–D) determined by the grade of the majority of items.
Assessment of level of evidence
The level of evidence of the quantitative studies was determined according to the criteria of the Oxford Centre for Evidence-Based Medicine (OCEBM, 2009). According to these criteria, level 1 includes systematic reviews of RCTs and individual RCTs; level 2 includes low-quality RCTs and ecological studies; level 3 includes cohort and case–control studies; level 4 includes case series, case report and poor-quality cohort and case–control studies; and level 5 is expert opinion. Qualitative studies are not included in the Oxford criteria (OCEBM, 2009).
Data extraction and synthesis
Database searches were performed by two reviewers (R.B., A.P.F.W.) working independently and the short-listed abstracts screened for eligibility against the inclusion criteria. Results were compared and a third assessor (C.P.) adjudicated when there were disagreements. Full-text articles were obtained for abstracts meeting inclusion criteria. These papers were screened by three authors (R.B., A.P.F.W., C.P.) working independently to determine the final list of included studies, with any discrepancies resolved by discussion until consensus was reached. A systematic review of included studies was undertaken by two authors (R.B., A.P.F.W.) working independently, using a standardised data extraction form consisting of general study information (author, location), study design and setting, participants (sample size, age, sex), description of the component of aftercare, results, level of evidence and aspects of methodological quality and score. The participants, interventions, comparisons, outcomes and study design (PICOS) are summarised in Tables 1–3. All authors reviewed the data synthesis.
Referral pathways.
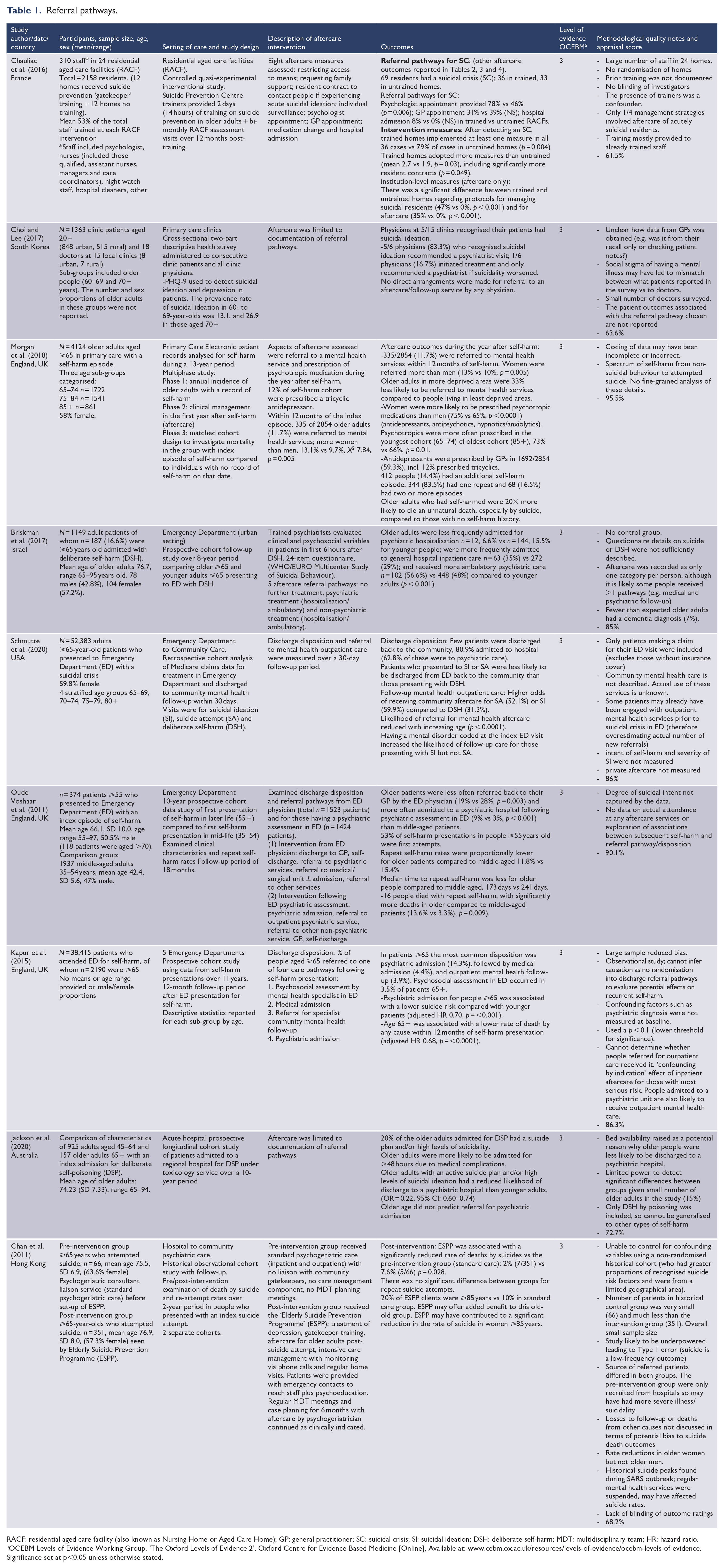
RACF: residential aged care facility (also known as Nursing Home or Aged Care Home); GP: general practitioner; SC: suicidal crisis; SI: suicidal ideation; DSH: deliberate self-harm; MDT: multidisciplinary team; HR: hazard ratio.
OCEBM Levels of Evidence Working Group. ‘The Oxford Levels of Evidence 2’. Oxford Centre for Evidence-Based Medicine [Online], Available at: www.cebm.ox.ac.uk/resources/levels-of-evidence/ocebm-levels-of-evidence.
Significance set at p<0.05 unless otherwise stated.
Assessment tools and approaches to safety planning.
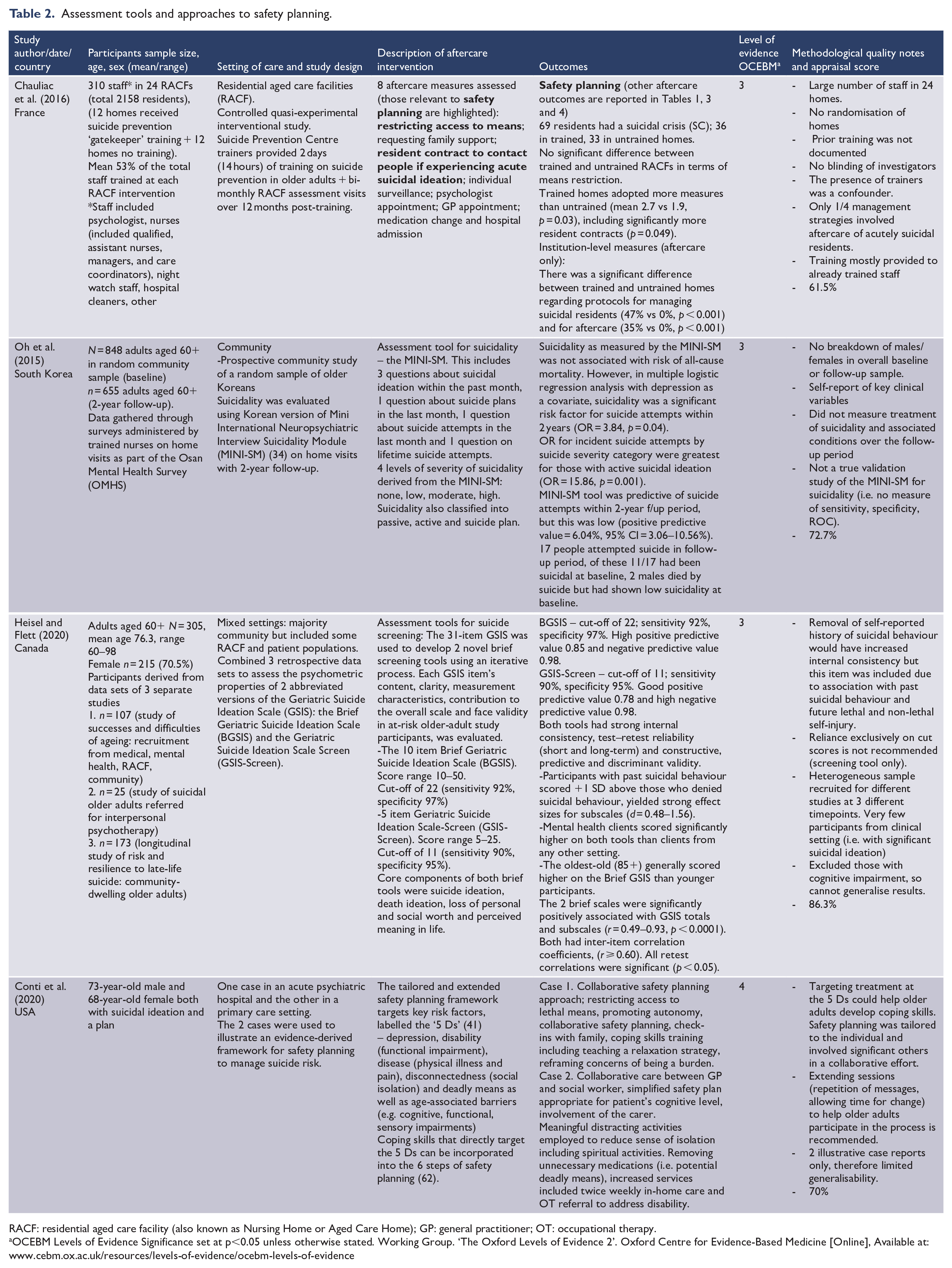
RACF: residential aged care facility (also known as Nursing Home or Aged Care Home); GP: general practitioner; OT: occupational therapy.
OCEBM Levels of Evidence Significance set at p<0.05 unless otherwise stated. Working Group. ‘The Oxford Levels of Evidence 2’. Oxford Centre for Evidence-Based Medicine [Online], Available at: www.cebm.ox.ac.uk/resources/levels-of-evidence/ocebm-levels-of-evidence
Engagement and intervention strategies.
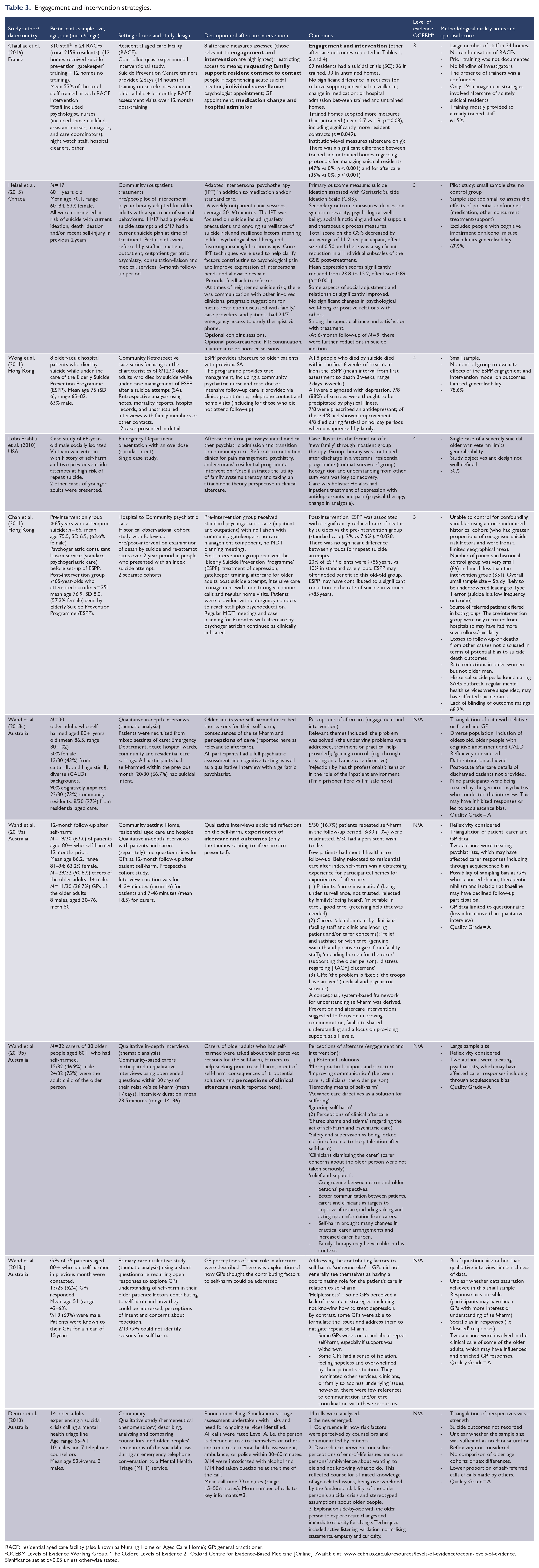
RACF: residential aged care facility (also known as Nursing Home or Aged Care Home); GP: general practitioner.
OCEBM Levels of Evidence Working Group. ‘The Oxford Levels of Evidence 2’. Oxford Centre for Evidence-Based Medicine [Online], Available at: www.cebm.ox.ac.uk/resources/levels-of-evidence/ocebm-levels-of-evidence. Significance set at p<0.05 unless otherwise stated.
A meta-analysis was considered but not possible given the heterogeneity of studies and limited data available.
Results
The PRISMA flowchart for study selection is shown in Figure 1. Electronic database searches identified a total of 2968 citations and an additional 36 records were identified through screening reference lists of systematic reviews about older persons’ aftercare. Finally, 20 publications met criteria for inclusion: 15 quantitative and 5 qualitative studies. Six studies were from Australia, five from North America, four from Europe, four from Asia and one from Israel. The 15 quantitative studies ranged in quality from 39.3% to 95.5% and levels of evidence were generally low (12 studies were rated level 3 and 3 studies were rated level 4). All five qualitative studies were rated ‘A’, the highest grade for methodological quality according to the Attree and Milton (2006) quality checklist.
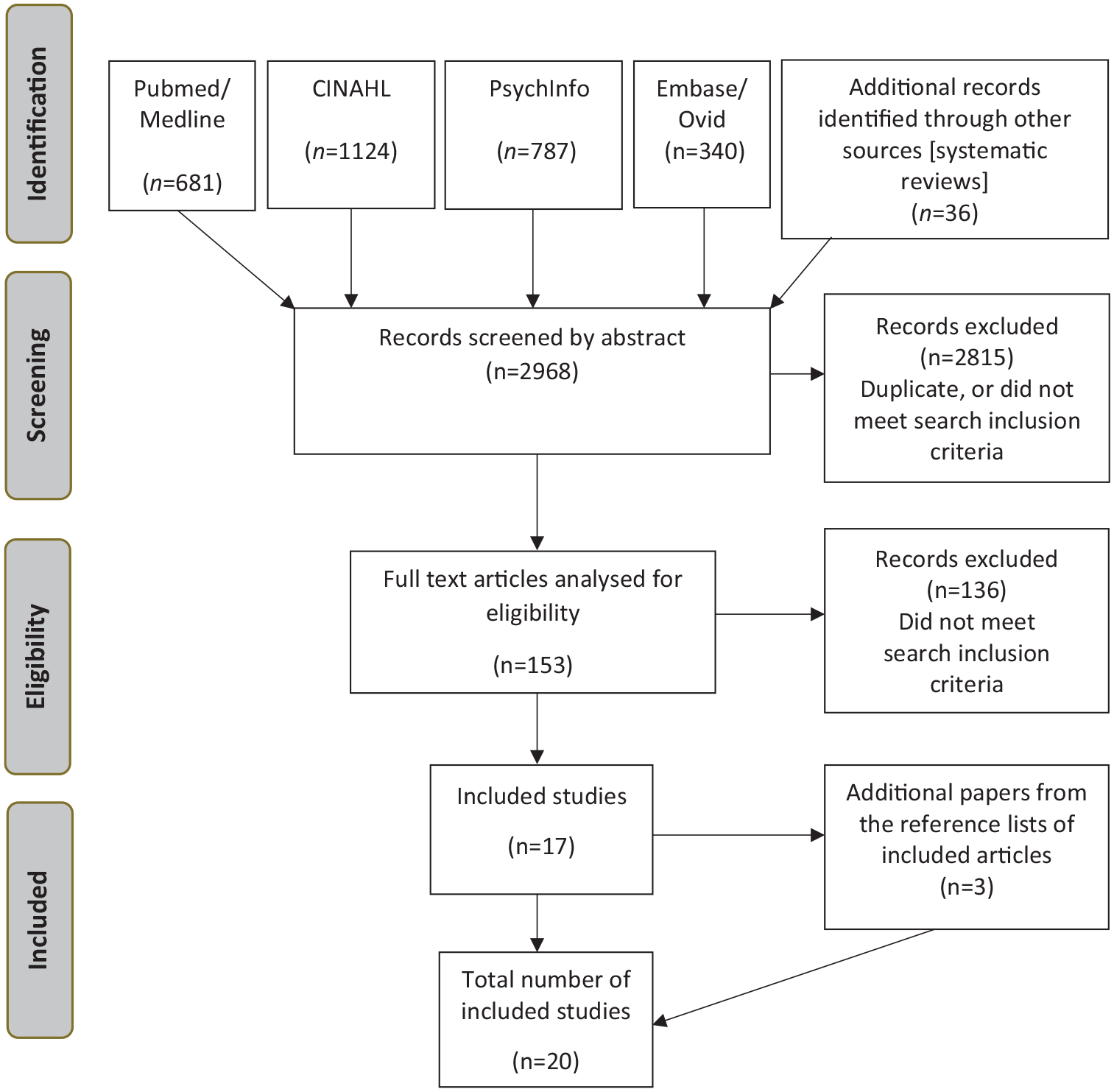
PRISMA flowchart of the results of the systematic review.
Of 15 quantitative studies, 3 were interventional studies, including 1 controlled quasi-experimental intervention (Chauliac et al., 2016), a pilot study using pre/post-intervention design (Heisel et al., 2015) and a historical control design (Chan et al., 2011). Eight cohort studies were included: five prospective (Briskman et al., 2017; Jackson et al., 2020; Kapur et al., 2015; Oh et al., 2015; Oude Voshaar et al., 2011) and three retrospective (Heisel and Flett, 2020; Morgan et al., 2018; Schmutte et al., 2020). An additional study was a cross-sectional health survey (Choi and Lee, 2017). Three studies included case reports/series (Conti et al., 2020; Lobo Prabhu et al., 2010; Wong et al., 2011) ranging from a single case to a series of eight decedent cases.
Study settings were broad and included Emergency Departments (EDs), inpatient hospital care (medical and/or psychiatric), community-based psychiatric care, residential aged care and primary care. Most studies were based in metropolitan/urban areas, and one had an urban/rural mix of patients (Choi and Lee, 2017). Study follow-up periods ranged from 30 days to 2 years. The youngest reported mean age in a patient group of interest was 66.1, age range 60–102. The detailed findings of the review, quality ratings and level of evidence for each study are summarised in Tables 1–3 according to the focus of aftercare or educational intervention.
Referral pathways for aftercare
Nine studies investigated referral pathways for aftercare of older adults following a suicide attempt or crisis (Table 1). The majority of studies were observational, reporting percentages of older adults referred to services rather than evaluating the efficacy of such. One large residential aged care facility (RACF) study (Chauliac et al., 2016) investigated the implementation of eight aftercare measures in 12 RACFs following older-adult-specific ‘gatekeeper’ (staff) training. Two studies investigated primary care referral pathways to mental health services (Choi and Lee, 2017; Morgan et al., 2018), both of which reported low rates of aftercare referrals. In the South Korean primary care study, doctors made recommendations such as seeing a psychiatrist or treatment of depression but did not make a referral to specialist psychiatric services, despite the high prevalence of suicidal ideation and depression, especially in the 70+ age group (Choi and Lee, 2017). The UK primary care study reported that only 11.7% of older patients who deliberately self-harmed were referred to mental health services, 59.3% were prescribed an antidepressant (11.8% a tricyclic antidepressant) (Morgan et al., 2018). Notwithstanding this (and perhaps related to this, given the toxicity of tricyclic antidepressants), those who had self-harmed died from unnatural causes 20 times more frequently than the comparison cohort, particularly within 12 months. Notably, more women were referred to services than men and higher self-harm incident rates were observed in the oldest age patient groups (75–84, 85+), compared to a reference group of younger, older adults (65–74) (Morgan et al., 2018).
All four ED studies were cohort analyses with a range of rates of referral for psychiatric or medical admissions, with one study reporting more medical than psychiatric admissions compared to younger adults (Briskman et al., 2017), and other studies reporting high rates of psychiatric admissions (Kapur et al., 2015; Schmutte et al., 2020) (Table 1). Higher rates of medical complications and length of stay were noted for older compared to younger patients admitted for acute hospital care after deliberate self-poisoning (Jackson et al., 2020).
ED physicians were less likely to refer older people back to their GP than middle-aged patients (Oude Voshaar et al., 2011). Only one study investigated efficacy of a comprehensive assertive aftercare programme, inclusive of urgent referral with assignment of case manager and psychogeriatric appointment within a week with assessment and follow-up (Chan et al., 2011). The case manager provided their emergency contacts to the clients as well as frequent phone contacts, regular (biweekly or triweekly) and crisis-based home visits to monitor the client’s mental and social situations, promote compliance with treatment, provide psychoeducation and liaise with other caregivers (both professional and nonprofessional) for 6 months. A multidisciplinary team (comprising psychogeriatricians, care managers and medical social workers ± occupational therapists), at tertiary care level, held regular case conferences to review the care plan and clinical progress. This study reported significantly reduced deaths by suicide in the intervention group, compared to a comparatively small historical cohort receiving standard care (Chan et al., 2011).
Assessment tools and safety planning approaches
Four studies evaluated assessment tools and/or educational approaches to safety planning (Table 2). A multifaceted aftercare intervention compared RACFs who received training (including on risk assessment) in the management of suicidal crises with untrained RACFs (Chauliac et al., 2016). Use of rating scales, including the Geriatric Depression Scale (GDS) (Yesavage et al., 1982), and institution-level prevention protocols was significantly greater in trained RACFs (Chauliac et al., 2016). The study was limited by lack of randomisation to control or intervention group, uncontrolled confounding factors, missing data regarding prior training and lack of rater blinding (Chauliac et al., 2016). A community study used the three-question Mini International Neuropsychiatric Interview Suicidality Module (MINI-SM) (Sheehan et al., 1998) to predict suicide re-attempts in survivors, but positive predictive validity was low (Oh et al., 2015). A study examined the psychometric properties of two abbreviated versions of the Geriatric Suicide Ideation Scale (GSIS): the Brief Geriatric Suicide Ideation Scale (BGSIS) and the Geriatric Suicide Ideation Scale Screen (GSIS-Screen) in different cohorts from separate studies (Heisel et al., 2015). Both the BGSIS and GSIS-Screen yielded strong effect sizes (d = 0.48–1.56) (Heisel et al., 2015). Use of the brief 5-item GSIS-Screen in the oldest-old (85+) detected higher scores than in younger <85 participants. Finally, two cases were used to illustrate an approach to safety planning and enhanced coping skills based on the 5 ‘Ds’ (risk factors) of late-life suicide (Conwell et al., 2011) using personalised older-adult-specific adaptations (e.g. for cognitive or sensory impairment) (Conti et al., 2020).
Engagement and intervention strategies
Ten studies evaluated engagement and/or intervention strategies (Table 3). An educational intervention in RACFs which engaged at least 30% of staff in the trained RACFs was associated with the implementation of more measures to reduce suicides in residents compared to untrained RACFs (Chauliac et al., 2016). Two psychotherapy reports included an older-adult-adapted interpersonal psychotherapy delivered over 16 weeks to a small group of older people with suicidal thoughts/behaviours which demonstrated significant decrease in suicidal ideation (Heisel et al., 2015) and a case study of application of family systems therapy and continuous supportive care (Lobo Prabhu et al., 2010).
Only two studies evaluated mortality in a dedicated suicide prevention programme for older adults at high risk of suicide (by virtue of index presentation) (Chan et al., 2011; Wong et al., 2011). Both studies were evaluations of the Elderly Suicide Prevention Programme (ESPP) in Hong Kong. As this was arguably the only dedicated comprehensive older-adult aftercare service reviewed, the programme warrants some explanation. The ESPP is multifaceted and includes assertive specialist psychogeriatric aftercare for suicide attempters, care management, treatment of depression and gatekeeper training (primary care, frontline health workers, volunteers in older-adult services and non-psychiatric specialists in tertiary care) (Chan et al., 2011). A retrospective case series described the characteristics of the 8/1230 older adults who died by suicide while engaged in the ESPP, although no comparisons were made with survivors engaged in the programme (Wong et al., 2011). In the other study, the outcomes for the same ESPP were compared to a small historical cohort pre-commencement of the ESPP reporting a reduction in suicide rates with the intervention (Chan et al., 2011). However, the study was limited by important methodological flaws, such as small non-equivalent (for baseline characteristics) historical cohort, a likely underpowered sample, lack of rater blinding to suicide re-attempt and death outcomes, lack of randomisation to control or intervention group and other confounding factors (Chan et al., 2011).
Five qualitative studies explored aspects of engagement and intervention for older adults experiencing a suicidal crisis and/or self-harm. In-depth interviews (Wand et al., 2018c, 2019a, 2019b), GP questionnaires (Wand et al., 2018a) and qualitative analysis of crisis call interactions (Deuter et al., 2013) provided insights into strategies and preferences for engagement from the perspective of the older person themselves (Wand et al., 2018c, 2019a), their carer (Wand et al., 2019a, 2019b), their GP (Wand et al., 2018a, 2019a) at the time of the index self-harm and one year later and telephone counsellors responding to older person experiencing a suicidal crisis (Deuter et al., 2013). Emergent themes included GPs and phone counsellor education to enhance understanding of needs of older adults (including addressing ageism); enhanced communication between services, patients and carers; validation of older-adult experiences to avoid engendering feelings of rejection; practical support; means restriction; and raising awareness that interventions such as psychiatric admission or RACF placement may be perceived as controlling and/or invalidating.
Discussion
This systematic review is, to our knowledge, the first to focus exclusively on aftercare for older people following self-harm (including with suicidal intent). The aim was to examine the current empirical evidence for aftercare in older people. Despite yielding a large number of initial results (N = 2968), only 20 empirical studies met inclusion criteria for the systematic review; 15 were quantitative and 5 qualitative. The focus on three key components of aftercare demonstrated a range of approaches to aftercare across hospital and community settings and seven countries, notably among which Australia yielded the most studies. The quality of the quantitative studies varied widely; with only six studies rated as high-quality (score > 80%; Kmet et al., 2004). The variable quality of these, largely data-linked cohort studies and case studies, does raise the risk of bias (Viswanathan et al., 2018) and may limit the general applicability of the findings. The five qualitative studies, albeit most conducted by our research team conferring significant bias of a different sort, fared better in quality ratings (the highest level; Attree and Milton, 2006). Notwithstanding this, the qualitative research provided some insights into the key aspects of engagement and various aftercare components from the perspectives of older people, their carers, GPs and telephone crisis counsellors.
Three aspects of aftercare for older adults were evaluated (referral pathways for aftercare; assessment tools and safety planning approaches and engagement and intervention strategies). The review highlighted that the assessment and referral pathways of older adults after self-harm vary markedly across settings with neither clear guidelines nor imperatives for community psychiatric follow-up. This results in many older people not being referred to any form of community care. This is in direct opposition to NICE (National Institute for Health and Care Excellence) guidelines which recommend that all older adults (65+) be assessed by a specialist mental health service after self-harm, given the especially close association between self-harm and suicide in older adults and increased levels of suicidal intent (National Institute for Health and Care Excellence, 2004). The RANZCP guidelines identify that multifaceted care management is likely to be needed by older people seen by mental health services after self-harm to reduce risk of suicidal behaviour and repeat self-harm (Carter et al., 2016). Moreover, the one study which reported reduction in deaths by suicide among older people used a comprehensive and assertive aftercare model (ESPP), suggesting that ‘any community follow-up’ may not suffice. The ESPP in Hong Kong included urgent referral with assignment of and close ongoing contact with a case manager as well as psychogeriatric assessment and follow-up for 6 months (Chan et al., 2011), arguing against a tick-box approach to follow-up. While this intensive approach to specialist mental health aftercare makes intuitive sense, the strength of the evidence is poor; derived from a single study with significant methodological limitations including a very small absolute risk reduction for suicide outcomes which might be due to a Type 1 error (Chan et al., 2011). In addition, generalisability to the Australian and New Zealand context is unknown given Hong Kong’s different health system and unique cultural and geopolitical circumstances. Therefore, the results of the study, although promising, must be interpreted with caution.
The NICE guidelines also recommend consideration of referring older adults who have self-harmed for inpatient psychiatric care for ongoing monitoring of mental health risk and needs assessment (National Institute for Health and Care Excellence, 2004). Rates of referral for inpatient psychiatric care varied markedly in the studies reviewed ranging from 6.6% to 62.8% (Briskman et al., 2017; Kapur et al., 2015; Oude Voshaar et al., 2011; Schmutte et al., 2020). In two Australian cohorts of older people with deliberate self-poisoning, rates of older adults referred for psychiatric admission were comparable; 52/157 (33.1%) (Jackson et al., 2020) and 40/110 (36.4%) (Ticehurst et al., 2002). However, inpatient psychiatric care is neither necessarily warranted nor wanted after self-harm (Morrison et al., 1999), as reported by older people themselves who described complex responses to admission, including feeling imprisoned, under surveillance, invalidated or – in contrast – safe and relieved (Wand et al., 2018c, 2019a). The rates of referrals from primary care to community mental health aftercare were low, perhaps reflecting limited understanding of the high risk of suicide in this vulnerable population and even ageism in clinical decision-making and care provision (Wand et al., 2021b). These findings highlight the need to find a balance between combatting ageist therapeutic nihilism with assertive aftercare, while also respecting consumer empowerment and choice where possible.
There were few studies describing efficacy and therapeutic value of use of assessment or screening tools for detecting suicide risk in older adults following a suicidal crisis. Of the four tools evaluated in the review, three were suicide-specific (BGSIS, GSIS-Screen, MINI-SM), and one was a screening tool for depression (the GDS). The two screening tools derived from the GSIS (BGSIS, GSIS-Screen) performed well psychometrically but were tested indirectly by combining existing studies with divergent aims and including very few clinical participants (Heisel and Flett, 2020). The MINI-SM, although utilising three simple and pragmatic questions to evaluate suicidal ideation/behaviours, performed poorly in terms of predictive validity (Oh et al., 2015). The GDS appeared to be a useful tool when tested in RACF residents as part of a multimodal approach to aftercare which included institutional change, but it was not possible to determine which components conferred benefit (Chauliac et al., 2016). Validation studies are needed to establish sensitivity and specificity of these tools for detecting suicidal ideation/behaviours in older adults, and more importantly, whether they trigger action and intervention. A useful paradigm illustrating the lack of translational impact of screening tools is the failure to follow-up poor scores on mandated depression screening tools in residential care (Snowdon et al., 2011).
However, arguably a more pressing consideration is whether screening tools or risk assessment have any place in determining aftercare given minimal evidence that any type of suicide risk categorisation reduces repeat self-harm or suicide (Carter et al., 2016; Wand, 2012). Suicide screening tools have low sensitivity resulting in missed cases, and low-positive predictive values (suicide is a low-frequency outcome) leading to high false-positive rates (Carter and Spittal, 2018; Large et al., 2017). The results of these respective problems are that some ‘low-risk’ patients may miss out on interventions and most people who receive intervention due to ‘high-risk’ status will never die by suicide (Large et al., 2017). In addition, there are resource, ethical and legal implications of a risk assessment approach including inequitable resource allocation, potential denial of enhanced treatment to people who may benefit, harm in terms of patient perceptions of invalidation and rejection and legal claims in the case of denial of treatment or suicide where risk status was misclassified (Berman and Carter, 2020). An alternative approach which is consistent with current guidelines (Carter et al., 2016; National Institute for Health and Care Excellence, 2004) is to conduct an empathic person-centred clinical assessment of needs (Carter and Spittal, 2018; Large et al., 2017). Such an approach may lead to better addressing the myriad potentially modifiable individual reasons for self-harm in an older person (Wand et al., 2019a) while taking into account strengths, coping strategies and psychosocial circumstances (Carter and Spittal, 2018).
The only study focusing exclusively on safety planning utilised two cases to illustrate potential benefits of a systematic approach to this aspect of aftercare (Conti et al., 2020). Although the intervention was founded upon a solid evidence base regarding risk factors for suicide in older adults (Conwell et al., 2011) and coping skills for safety planning (Stanley et al., 2018), case reports are among the lowest evidence base with which to inform implementation.
There were few aftercare studies evaluating the efficacy of different approaches to engagement and intervention. The two most comprehensive approaches to aftercare involving RACFs (Chauliac et al., 2016) and hospital settings (Chan et al., 2011) reported better primary outcomes compared to comparison cohorts, but were limited by important methodological flaws. Thus, there may be small but potentially meaningful clinical benefits from these more comprehensive approaches to aftercare, but well-designed trials are needed to clearly evaluate outcomes. The multifaceted approaches to engagement and intervention including gatekeeper training, monitoring and close follow-up, means restriction, referrals to specialist clinicians and treatment components described in these studies are likely to be essential elements of aftercare, also highlighted in other reviews of suicide prevention initiatives (Lapierre et al., 2011; Motohashi et al., 2004). This has recently been supported by a meta-analysis, albeit not specific to older adults, finding that multilevel interventions are more effective than single-level interventions (Hofstra et al., 2020).
The single pilot study investigating a dedicated treatment approach of an adaptation of interpersonal therapy (IPT), using a pre/post-study design without a comparison group, demonstrated reduction in suicidal ideation (Heisel et al., 2015). Other studies were limited by virtue of case report methodology, e.g., regarding utility of family systems therapy (Lobo Prabhu et al., 2010). Qualitative studies described engagement and intervention from the perspective of the older person, their carer or clinician (Deuter et al., 2013; Wand et al., 2018a, 2018c, 2019a, 2019b). This work has informed key aspects of communication between the older person and the aftercare provider, based on an understanding of the context, experiences, and needs of the older person both before and after the suicide attempt, and their responses to aftercare which can be perceived as disempowering as they are ‘protective’ (Wand et al., 2019a; Wand et al., 2018c; Wand et al., 2019b).
Implications for practice, policy and future research
Collaboration with older people with lived experience and their families
Perspectives of both older adults who have had suicidal behaviours and their carers are essential to collaboratively guide planning of real-world, acceptable and effective aftercare services. The lived experiences of older people who have survived a suicide attempt or crisis have only recently been studied using rigorous qualitative methodology (e.g. Bonnewyn et al., 2014; Van Orden et al., 2015; Wand et al., 2018c, 2019a). Although psychological autopsy studies have examined the perceptions of healthcare and warning signs given to relatives before an older-adult suicide (Draper et al., 2018; Peters et al., 2013), there are scant qualitative studies of families/carers of older adults who have survived a suicide attempt or crisis (Wand et al., 2019b). Although there may be important distinctions between people who die by suicide and those who attempt suicide and survive (DeJong et al., 2010), insights from those who have self-harmed may inform what is helpful in terms of aftercare. The value of patient involvement has been demonstrated by two younger-adult studies, which found it can be a core component in the development and delivery of suicide prevention services (Ghio et al., 2011; Jones et al., 2018). This gap needs to be addressed in older-adult services, including through focus groups with older patients and their families.
Adapted psychotherapy for older people and their families
Given the highly individualised reasons for self-harm in older people, including loss of purpose and connectedness and the importance of perceptions of relationships (Wand et al., 2018c, 2019a, 2019b), intuitively aftercare might usefully include psychotherapeutic approaches. However, the lack of evidence-based psychotherapeutic interventions available to older people for aftercare remains another opportunity for development. We are not aware of any systematic reviews of psychotherapy for older adults who have self-harmed, although a recent Cochrane review of adults of all ages who self-harm found most evidence for cognitive behavioural therapy (CBT), mentalisation-based therapy and emotion-regulation psychotherapy (Witt et al., 2021). The relevance of these findings to older adults is unclear, given entirely different age-specific individual and systemic psychosocial contexts as well as cognitive comorbidities. However, CBT has been adapted for depression and suicide prevention in older adults (Bhar and Brown, 2012) and a systematic review of individual and group-based CBT to treat depression and anxiety in RACF residents showed some evidence of efficacy and good acceptability to residents and RACF staff (Chan et al., 2021).
Of direct significance to the present systematic review is a recent mini-review of psychosocial interventions to prevent suicide in older people (Zeppegno et al., 2019). This review identified only seven studies, but good evidence for the PROSPECT intervention (Prevention of Suicide in Primary Care Elderly which included IPT; Bruce and Pearson, 1999; Bruce et al., 2004), a geriatric outreach programme for older people at risk of suicide and 24-hour hotline (using well-being checks, emotional support, weekly home-visit counselling; Fiske and Arbore, 2001), a very small trial of Problem Adaptation Therapy (PATH) compared to Supportive Therapy for Cognitively Impaired Older Adults (ST-CI) (Kiosses et al., 2015) and outpatient interpersonal psychotherapy (Heisel et al., 2009, 2015). Key components of these psychosocial interventions included educating primary care clinicians, improving recognition and treatment of depression, home-based delivery of therapy, involvement of family members, follow-up and crisis support (Zeppegno et al., 2019). Notably, these studies had a focus on suicide prevention broadly, not as part of aftercare, and thus interventions described did not meet inclusion in the present review. The exception was the older-adult adaptation of IPT, which was identified in the present review as also having evidence of benefit in aftercare (Heisel et al., 2015). The single case of family therapy, while not providing any evidentiary support, is also illustrative of the potential role of family, systems and group therapy. More importantly, it builds on qualitative (Wand et al., 2018c, 2019a, 2019b) and other work (Hinrichsen and Hernandez, 1993; Lapierre et al., 2011; Peisah, 2006; Zweig and Hinrichsen, 1993) relating to the role of the family in late-life suicide which might be harnessed in aftercare strategies. Particular targets for family therapy may include addressing perceived burdensomeness (Van Orden et al., 2010; Wand et al., 2018c) or carers’ emotional responses to self-harm (Talseth et al., 2001; Wand et al., 2019b), and insight-orientated narrative approaches which facilitate shared understanding and problem-solving (Benbow and Sharman, 2014). It can be fruitful to help families recognise that their understandably anxious and angry responses to the older person’s self-harm may fuel the older person’s sense of helplessness, worthlessness and the sense that the family would be better off without them (Peisah, 2006). Such insights may shed light on reactions of older persons to well-meaning, but knee-jerk and risk-focused interventions following self-harm, including residential care placement.
There is significant overlap between the components of these psychosocial suicide prevention interventions and promising approaches to aftercare, which warrant further study. Approaches to individual and family therapy could be manualised and their clinical utility and cost-effectiveness tested in different settings. There is also a need for psychotherapeutic interventions which can be easily accessed by older adults, including those who may have limited transport, mobility and other health and functional impairments. The Improving Access to Psychological Therapies programme, developed in the United Kingdom (The National Collaborating Centre for Mental Health, 2021), has recently been employed for use with people presenting with suicidal risk in Australian ED settings (Bidargaddi et al., 2015). This model uses a telephone-based low-intensity approach, with reported clinical benefit, although included limited numbers of older adults.
Age and gender-specific adaptations
The demographics of suicide in late-life and also the efficacy of aftercare interventions demonstrate that older people who self-harm or attempt suicide are not a homogeneous group (Koo et al., 2017). Real differences exist between the needs of ‘young-old’, ‘middle-old’ and ‘old-old’ people (Koo et al., 2017). The latter group has greater risk of physically frailty, medial comorbidity and cognitive impairment. Age-specific services should target intervention tailored to the needs of the older person and clarify what can be effectively implemented at different points of care and in different settings (Wand et al., 2019a).
Although greater numbers of women than men were reported in most of the reviewed studies (Tables 1–3), there were no gender-specific approaches to aftercare described. The psychosocial contexts, needs and help-seeking styles of older men may differ from older women (King et al., 2020; Lapierre et al., 2011). There are gender-specific patterns of late-life suicide, with older men consistently having higher rates (Shah et al., 2016). Despite this fact, we found no studies specifically targeting the aftercare of older men. One study specifically observed higher referral rates for aftercare in women (Morgan et al., 2018). Other interventions with effects on suicide rates have similarly reported better uptake of psychosocial interventions with women compared to men (and reduced rates of suicide for women) (De Leo et al., 2002). The reasons for this gender discrepancy in referrals are unknown. In some cases, it may be that both men and women are referred, but that women are more likely to engage with mental health services and social resources than men (Drapeau et al., 2009). Older men may need more assertive and novel approaches to aftercare and follow-up. We echo calls for dedicated studies evaluating the differential impacts of suicide prevention initiatives by gender (Lapierre et al., 2011) and for studies specifically targeting the psychosocial context and needs of older men (King et al., 2020).
Guidelines
One of the manifestations of ageism in health care is inadequate representation of older people in clinical guidelines (Cox et al., 2011). The most recent RANZCP guidelines for managing self-harm stand out as an exception, with sections specific to older adults (Carter et al., 2016). Best practice guidelines should be developed for and specific to settings of older persons aftercare, including crisis supporters and telephone counsellors, community aged-care support staff, primary care, RACF, ED and inpatient wards (medical and psychiatric), as currently referral pathways appear to be generic or ad hoc, rather than based upon evidence and outcomes. Although more validation studies of screening tools for older adults in specific settings have been recommended (Heisel and Flett, 2020), the limits of risk assessment as a determinant of access to aftercare are considerable (Carter and Spittal, 2018; Large et al., 2017). Instead, studies evaluating approaches for assessment and management of individualised needs are warranted, rather than continued focus on risk assessment and screening (Large et al., 2017). This individualised approach aligns with other work highlighting that ageist assumptions about older people as a cohort may introduce or exacerbate risk factors for suicide (Wand et al., 2021b). This review signals that comprehensive interventions which target multiple aspects of aftercare provide assertive case management and specialist follow-up, and dedicated training may confer benefit (Chan et al., 2011; Chauliac et al., 2016) but require further evaluation in well-designed studies in a variety of countries. In addition, recent work has again emphasised that there may be important differences between people who attempt suicide and those who die by suicide, necessitating consideration of differential effects and outcomes of interventions across patient groups and settings (Hofstra et al., 2020). Thus, more studies are needed in these different groups, settings and outcomes to determine which interventions work for which populations and why, and guide recommendations (Hofstra et al., 2020).
Strengths and limitations
This systematic review was undertaken using PRISMA reporting guidelines, an established systematic process for identifying, reviewing and reporting data (Moher et al., 2009). Other key strengths were that multiple electronic databases were reviewed, and an inclusive approach was taken with respect to study design, optimising the chances of identifying relevant studies. The independent database searches, data extraction and quality ratings by two authors increased the validity of the results.
The systematic review was not pre-registered conferring a potential source of bias. The research question and search terms were deliberately broad to provide an overview of contemporary approaches to aftercare, contributing to heterogeneity of identified studies and outcomes. However, the temporal restriction of the search from the year 2010 may be considered a limitation as other potentially relevant approaches to aftercare may not have been included. The grey literature was excluded, as such studies have not been subject to peer review, independent scrutiny and validation crucial to quality assurance (Adams et al., 2017). Publication bias may have occurred in the systematic review by exclusion of the grey literature, as studies with negative or no results are less likely to be published (Paez, 2017).
It is notable that most studies identified for this review provided low-level evidence by virtue of their study design. The highest level of evidence was 3, with the majority of studies level 4 (OCEBM, 2009). This affects interpretation of the study findings and suggests the need for studies using more robust methodology. The overall quality ratings for included studies (range 39.3–95.5%) indicate significant methodological issues which raises the possibility of bias. There was no minimum quality rating set for inclusion of studies in order to maximise identification of all potentially relevant studies.
Finally, we acknowledge that four of the included publications were written by our group (Wand et al., 2018a, 2018c, 2019a, 2019b) and recognise the bias implicit in, and therefore limitations of, self-review. This limitation was partially mitigated by having another author (R.B.) (not involved in the aforementioned studies) independently appraise the quality of all studies, independent of the other raters.
Conclusion
With a specific focus on a previously neglected area of aftercare, this systematic review adds to the plethora of reviews examining late-life self-harm (Troya et al., 2019a; Wand et al., 2018b), suicide risk factors (Conejero et al., 2018) suicide risk identification and prevention in primary care (Raue et al., 2014; Troya et al., 2019b), general prevention (Conwell, 2014; de Mendonça Lima et al., 2021; Lapierre et al., 2011; Wallace et al., 2021), prevention in RACFs (Chauliac et al., 2020; Gleeson et al., 2019) and intervention (Okolie et al., 2017).
The review analysed the results, quality and level of evidence pertaining to three key components of aftercare for older adults following self-harm (including with suicidal intent). The 20 reviewed studies demonstrate a very limited evidence base for aftercare in older people, comprising generally low-level quantitative evidence (15 studies, level 3 or 4) and study designs with significant methodological limitations and variable quality, excluding the five qualitative analyses. Dedicated older-adult aftercare interventions with a multifaceted, assertive follow-up approach accompanied by systemic change appeared most promising in line with a recent review highlighting potential benefits from multilevel interventions for suicide prevention (Hofstra et al., 2020). However, more high-quality research is needed before definitive recommendations can be made. More work is needed to establish the efficacy and outcomes of various referral pathways following self-harm so that clinician responses are consistent and evidence based. Although assessment tools for suicidality in older adults have potential, formal validation is required and outcomes should be compared to needs assessment approaches. Assessing and managing individualised needs is arguably a better fit than screening tools (Carter and Spittal, 2018), especially given the qualitative evidence from older people who have self-harmed and their carers (Wand et al., 2018c, 2019a, 2019b). Safety planning for older adults includes means restriction, but broader collaborative approaches based upon known risk factors for late-life suicide and teaching-related coping skills (Conti et al., 2020) make intuitive sense and should be formally evaluated. Through qualitative studies, older adults and their carers highlight multiple targets for improved engagement with services, communication and provision of personalised aftercare responses including individual and family systems therapy. The review highlights multiple gaps in the contemporary aftercare literature and opportunities for further older-adult-specific research. Mixed methods approaches incorporating qualitative collaborative research with older adults, their carers and clinicians will help to understand why aftercare interventions work (or do not) for older adults (Wand and Reppermund, 2021).
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship and/or publication of this article: This work was supported by the Mental Health Branch of the New South Wales Ministry of Health. The funders had no role in undertaking or reporting the review findings.
