Abstract
Objective:
Most studies that examine psychiatric illness in people who offend have focused on incarcerated samples, with little known about the larger population of individuals with criminal justice system contact. We examine the overlap between proven offences and psychiatric diagnoses with an emphasis on experiences for Indigenous Australians.
Methods:
In a population-based birth cohort of 45,141 individuals born in Queensland, Australia, in 1990 (6.3% Indigenous), psychiatric diagnoses were identified from hospital admissions between ages 4/5 and 23/24 years and proven offences were identified from court records (spanning ages 10–24 years). Prevalence rates for offending, psychiatric diagnoses and their overlap were examined for Indigenous and non-Indigenous individuals. Associations between specific psychiatric diagnoses and types of offending were examined using logistic regressions.
Results:
There were 11,134 (24.7%) individuals with a finalised court appearance, 2937 (6.5%) with a diagnosed psychiatric disorder and 1556 (3.4%) with a proven offence and diagnosed psychiatric disorder, with Indigenous Australians significantly overrepresented across all outcomes. Compared with non-Indigenous Australians, Indigenous Australians were younger at their first court finalisation (Cohen’s d = −0.62, 95% confidence interval = [−0.67, −0.57]), experienced a higher number of finalisations (d = 0.94, 95% confidence interval = [0.89, 1.00]) and offences (d = 0.64, 95% confidence interval = [0.59, 0.69]) and were more likely to receive custodial (d = 0.41, 95% confidence interval = [0.36, 0.46]) or supervised (d = 0.55, 95% confidence interval = [0.50, 0.60]) sentences. The overlap between offending and psychiatric illness was more pronounced for Indigenous Australians compared with non-Indigenous Australians (14.8% vs 2.7%). Substance use disorders were the most prevalent psychiatric diagnosis among individuals with a court finalisation (9.2%).
Conclusions:
Indigenous Australians were significantly overrepresented in court finalisations and psychiatric diagnoses. Indigenous Australians with a psychiatric diagnosis were at highest risk of experiencing a court appearance, emphasising the importance of culturally appropriate mental health responses being embedded into the criminal justice system.
Research examining the association between psychiatric illness and criminal justice system (CJS) involvement has primarily utilised incarcerated samples and focused on violent offending and specific diagnostic categories. This research consistently highlights that serious psychiatric disorders are particularly prevalent among prisoners compared with the general community (Fazel and Danesh, 2002; Kessler et al., 2009). Comparatively less is known about the extent and nature of psychiatric illnesses experienced among the wider population of individuals who have contact with the CJS but are not necessarily incarcerated. In addition, large-scale studies examining mental health problems experienced by Aboriginal and Torres Strait Islander Peoples 1 involved in the CJS are rare. The aim of this study was to examine the overlap between diagnosed psychiatric disorders and contact with the CJS for Indigenous and non-Indigenous Australians using a population-based birth cohort of individuals born in the state of Queensland in 1990.
Prevalence of psychiatric illness in the CJS
Between 10% and 40% of prisoners have a history of a diagnosed psychiatric disorder, increasing to between 80% and 90% of prisoners when substance use disorders (SUDs) are considered (Kingston et al., 2016; Sirdifield et al., 2009). Less research has examined the prevalence of psychiatric illness among offenders in community as opposed to correctional settings. Both Brooker et al. (2012) and Lurigio et al. (2003) sought to estimate the prevalence of psychiatric illness in the broader population of individuals who come into contact with the CJS by examining offenders on probation. Brooker et al. (2012) estimated that 39% of their sample would meet criteria for at least one psychiatric illness, with anxiety disorders the most prevalent. Moreover, 47% of their sample would meet criteria for at least one personality disorder, which typically co-occurred with substance abuse. Similarly, Lurigio et al. (2003) found that 42.5% of probationers met criteria for substance dependence/abuse in the previous year, with those with a psychiatric disorder more likely to be dependent on one or more substances compared with those without a psychiatric disorder (55% vs 37%, respectively).
There remain several gaps in knowledge regarding the association between psychiatric illness and involvement in the CJS, including whether different psychiatric diagnoses have stronger links to offending behaviour. Efforts to examine specificity in the links between psychiatric illness and offending have been hindered by small sample sizes, where large-scale population-based studies may be better able to explore these links. Available evidence suggests that most psychiatric illnesses are associated with an increased risk of violent offending specifically (Arseneault et al., 2000; Brennan et al., 2000), possibly because all psychiatric illnesses share core psychopathological features (e.g. emotional dysregulation) that increase the risk of violence (Chang et al., 2015).
Australian research on the links between psychiatric illness and offending
Butler et al. (2006, 2007; Butler and Allnutt, 2003) conducted some of the first detailed examinations of the extent of psychiatric illness among incarcerated men and women in Australia. Given the well-documented overrepresentation of Indigenous Australians in the CJS, differences between Indigenous and non-Indigenous people were a key focus. Butler et al. (2007) found Indigenous women were more likely than non-Indigenous women to be diagnosed with psychosis, depression and obsessive-compulsive disorder. Furthermore, Indigenous women were more likely to be classified as experiencing high or very high psychological distress. These differences were not evident between Indigenous and non-Indigenous males, which suggests that Indigenous women who experience incarceration may be an especially vulnerable group in the Australian context (Heffernan et al., 2012).
Longitudinal population-based studies are a vital source of information about the broader overlap between psychiatric illness and offending. Stewart et al. (2020) examined sex and Indigenous status differences in the overlap between imprisonment and diagnosed psychiatric illness in a population-based cohort of individuals born in Queensland in 1990 followed up to age 23/24 years. One-third of prisoners had been diagnosed with a psychiatric illness. Indigenous Australians were significantly overrepresented in prevalence rates for both imprisonment and psychiatric illness diagnoses compared with non-Indigenous Australians. For example, 18.5% of Indigenous males had been sentenced to prison compared with only 1.5% of non-Indigenous males. In addition, 16.9% of Indigenous Australians had been diagnosed with a psychiatric illness compared with only 5.3% of non-Indigenous Australians.
Australian research is consistent with international findings that psychiatric illness is highly prevalent among prisoners. However, research directly comparing Indigenous and non-Indigenous rates of psychiatric illness among CJS-involved individuals who are not imprisoned is limited, which restricts efforts to accurately estimate differences in prevalence rates to inform practice and policy development.
Current study
This study extends previous work on psychiatric illness and incarceration (Stewart et al., 2020) to include all individuals with a proven offence from a finalised court appearance. Our emphasis is on examining psychiatric diagnoses and recorded offending among Indigenous Australians. We hypothesised that (1) Indigenous Australians will have a higher prevalence of proven offences from court appearances compared with non-Indigenous Australians; (2) psychiatric disorders will be more prevalent among individuals with a proven offence, and correspondingly that proven offences will be more prevalent among individuals with a psychiatric disorder and (3) a higher proportion of Indigenous Australians with a psychiatric disorder will have a proven offence compared with non-Indigenous Australians with psychiatric disorders.
Methods
Design and data sources
A longitudinal birth cohort design was used, based on data derived from the Queensland Cross-sector Research Collaboration (QCRC) repository (Stewart et al., 2015). The QCRC repository contains linked administrative records from multiple government agencies/systems, including Queensland Registry of Births, Deaths and Marriages (QLD RBDM); child protection; 2 youth justice (child courts); 3 Queensland Department of Justice and Attorney-General (adult courts) and Queensland Health.
The 1990 cohort used for the current study consists of 45,223 individuals (48.5% female) born in Queensland in 1990, including 2852 Indigenous individuals representing 6.3% of the cohort. Indigenous status was assigned if an individual had ever identified as Indigenous (Aboriginal and/or Torres Strait Islander) in any of the QCRC databases, which was consistent with best practice guidelines for linked data (Australian Institute of Health and Welfare, 2012). There were 266 deaths recorded for the cohort (representing 0.6%), with deaths occurring before 8 years old (n = 80; age of first psychiatric diagnosis) excluded. A further two cases were excluded due to missing estimated age at death, resulting in a final cohort of 45,141 individuals for analysis.
The study was approved by the Griffith University Human Research Ethics Committee (HREC 2010/479). Individual consent was not required given the use of anonymised administrative data. The STrengthening the Reporting of OBservational studies in Epidemiology (STROBE) guidelines were adopted for the current study (von Elm et al., 2008).
Offending
Offending information was obtained from finalised court outcomes collected by Youth Justice and the Queensland Department of Justice and Attorney-General that were available from the age of criminal responsibility (10 years) until December 2014. Proven offences from finalised court outcomes 4 include appearances where an individual is found guilty or pleads guilty to an offence(s). Multiple offences and offences occurring on separate dates can be finalised on a single date. All offences were coded according to the Australian and New Zealand Standard Offence Classification (ANZSOC; Australian Bureau of Statistics, 2011) and classified into six categories:
Offences against the person that were predominately violent offences. ANZSOC divisions 1 through 6.
Property offences. ANZSOC divisions 7 through 9.
Public order offences. ANZSOC division 13.
Drug offences. ANZSOC division 10.
Traffic offences. ANZSOC division 14.
‘Other’ offences. ANZSOC divisions 11, 12, 15 and 16.
Individuals could have multiple offences within and across categories. The offence category variables were coded both as binary indicators (present/not present for prevalence analyses) and frequency counts (for multivariate analyses) for each individual over the time span. In addition to offence categories, further details relating to offending were examined, including age at first finalised court appearance, number of finalised court appearances, total number of proven offences across finalised appearances, number of serious violent offences (i.e. offence against the person), number of custodial sentences, and number of probation orders.
Psychiatric disorders
The Queensland Hospital Admitted Patient Data Collection (QHAPDC) data set, which covers admissions to public and private hospitals in Queensland, was used to extract diagnosed psychiatric disorders for the cohort. Diagnoses were made by medical practitioners during the course of a patient admission and were subsequently coded according to the International Statistical Classification of Diseases and Related Health Problems, Tenth Edition, Australian Modification (ICD-10AM; World Health Organization, 2004). The current QHAPDC commenced 1 July 1995; hence, hospital admissions data were left-censored until age 4/5 years for the 1990 cohort. The hospital admission data were extracted on 30 June 2014 and were therefore available from age 4/5 to 23/24 years. An individual was classified as having a psychiatric illness if they had ever experienced a hospital admission and received a psychiatric diagnosis (ICD-10 Mental and behavioural disorders [codes F00–F99], as well as suicidal ideation [code R45.8] and self-harm [codes X60–X84]) as either a primary or additional diagnosis. All primary and secondary diagnoses across all admissions were considered up to the date of data extraction, therefore representing the lifetime prevalence of diagnosed psychiatric illness from hospital admissions up till age 23/24 years. Consistent with recent Australian cohort-based studies (Dean et al., 2018), psychiatric diagnoses were classified into six broad categories, with each broad category subdivided into more detailed subcategories (see Supplementary Table S1 for classification details):
Severe psychiatric disorders,
Common psychiatric disorders,
Personality disorders,
SUDs (excludes substance-induced psychoses, which are included under severe psychiatric disorders),
Adolescent- and adult-onset disorders,
Childhood onset disorders.
Diagnostic categories and subdivisions contained mutually exclusive sets of ICD-10 codes, and were coded as binary indicators (i.e. present/not present) for each individual in the cohort. Individuals could appear in more than one diagnostic category if they were diagnosed with more than one psychiatric diagnosis across different categories.
Analytical approach
Analyses were conducted using R version 3.6 (R Core Team, 2019). First, the prevalence of proven offences and details of offending were examined, separated by Indigenous status and sex. Second, the prevalence of diagnosed psychiatric disorders for individuals with a proven offence were explored, separated by Indigenous status and sex. Third, the overlap between offending and psychiatric disorders was explored descriptively (i.e. offence types and frequencies) and by the cumulative prevalence of offending. Cumulative prevalence was measured as the proportion of individuals experiencing their first proven offence by offence type up to age 24 years and was modelled using the survival package for R (Therneau, 2015). For deceased cases, age at death was taken as the point of censoring for the cumulative prevalence analysis. Differences in cumulative prevalence rates among groups were examined using Gray’s (1988) test. For overlap analyses, the cohort was stratified by psychiatric disorder diagnosis (present/not present) and Indigenous status (Indigenous/non-Indigenous), creating four possible groups for comparison: (1) Indigenous individuals with a disorder, (2) Indigenous individuals without a disorder, (3) non-Indigenous individuals with a disorder and (4) non-Indigenous individuals without a disorder. Finally, logistic regression models were used to examine the association between specific psychiatric diagnosis categories and the frequency of different types of offending with the full cohort, providing odds ratios (ORs) and their associated 95% confidence intervals (CIs). A multivariate model was estimated for each psychiatric diagnosis category as a dependent variable, with the frequency of each offence type included as covariates. A binary indicator of any offence (yes/no) was included as a covariate in each model, to control for the zero-inflated distributions of each offence type frequency. These analyses were conducted separately for Indigenous and non-Indigenous individuals to explore differences between these groups.
Results
Displayed in Table 1 are the prevalence rates for proven offences (up to age 24 years), diagnosed psychiatric illness (up to ages 23/24 years) and their overlap for the cohort.
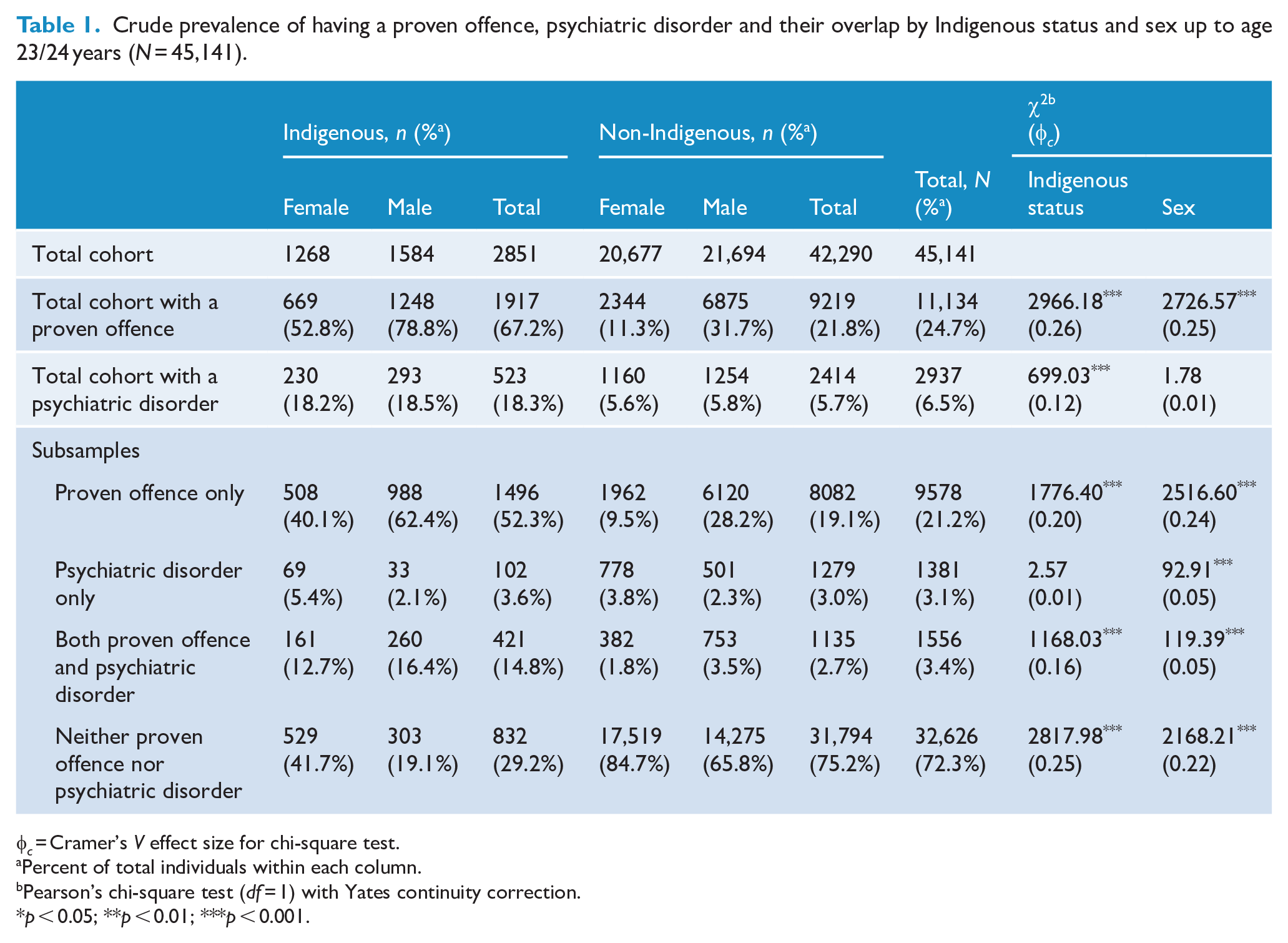
Crude prevalence of having a proven offence, psychiatric disorder and their overlap by Indigenous status and sex up to age 23/24 years (N = 45,141).
φ c = Cramer’s V effect size for chi-square test.
Percent of total individuals within each column.
Pearson’s chi-square test (df = 1) with Yates continuity correction.
p < 0.05; **p < 0.01; ***p < 0.001.
Prevalence and details of offending
By age 24 years, 24.7% (n = 11,134) of the cohort had a proven offence. Indigenous Australians were significantly overrepresented in having a proven offence compared with non-Indigenous Australians (67.2% vs 21.8%), with a moderate-to-large effect size. The highest prevalence rate was observed for Indigenous males, with 78.8% of this group having a proven offence by age 24 years. Men compared with women were more likely to have a proven offence (34.9% vs 13.7%), with a moderate-to-large effect size.
Figure 1 displays the proportion of individuals that had a proven offence at each age between 10 and 24 years stratified by Indigenous status and sex. The proportion of individuals experiencing a proven offence increased steadily from 10 years, peaked at age 18–19 years, and declined gradually from 20 years onwards. A greater proportion of Indigenous males and females experienced a proven offence at every age compared with non-Indigenous males and females and this was most pronounced for Indigenous males.
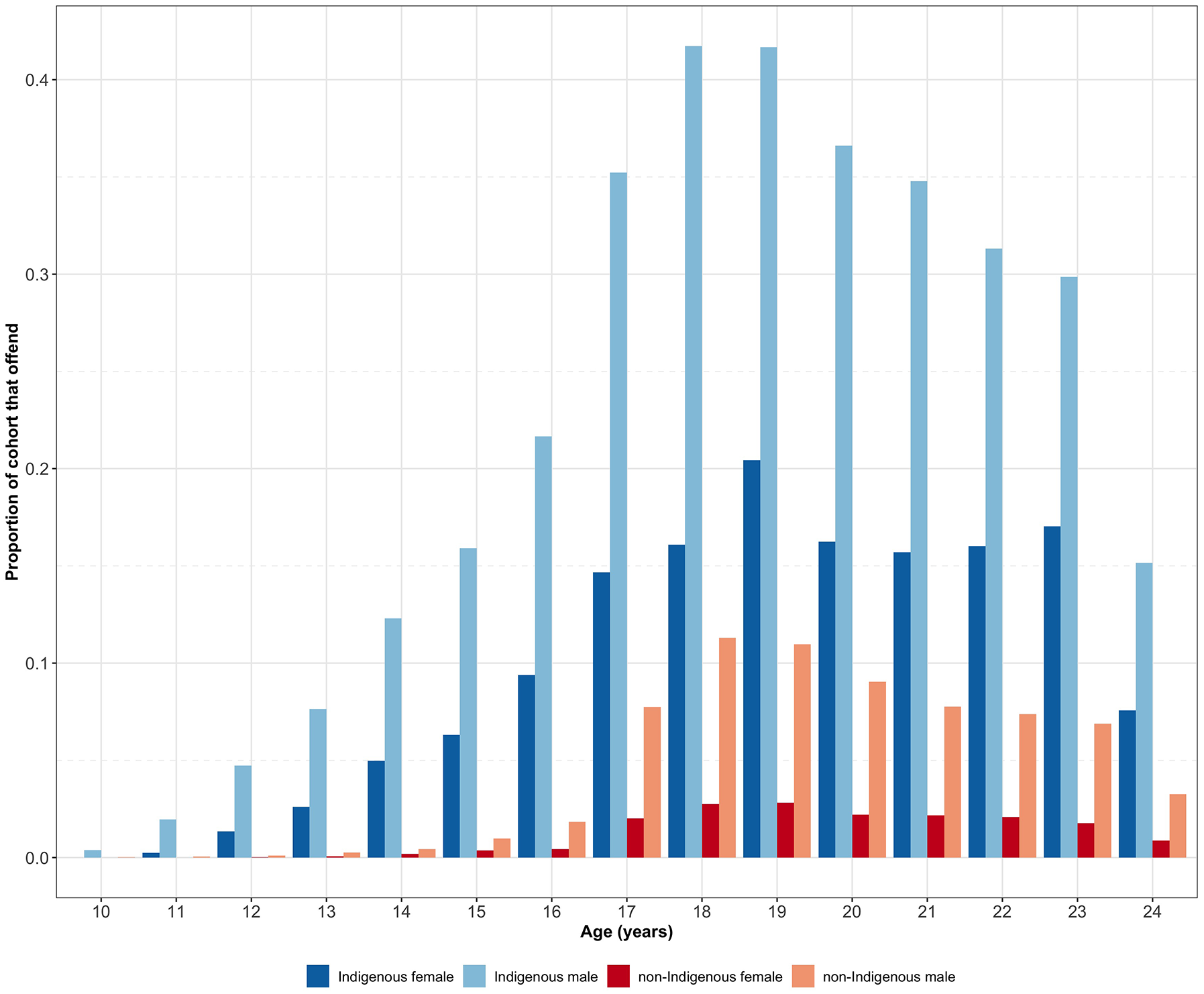
Proportion of individuals with a proven offence by age, separated by Indigenous status and sex (N = 45,141).
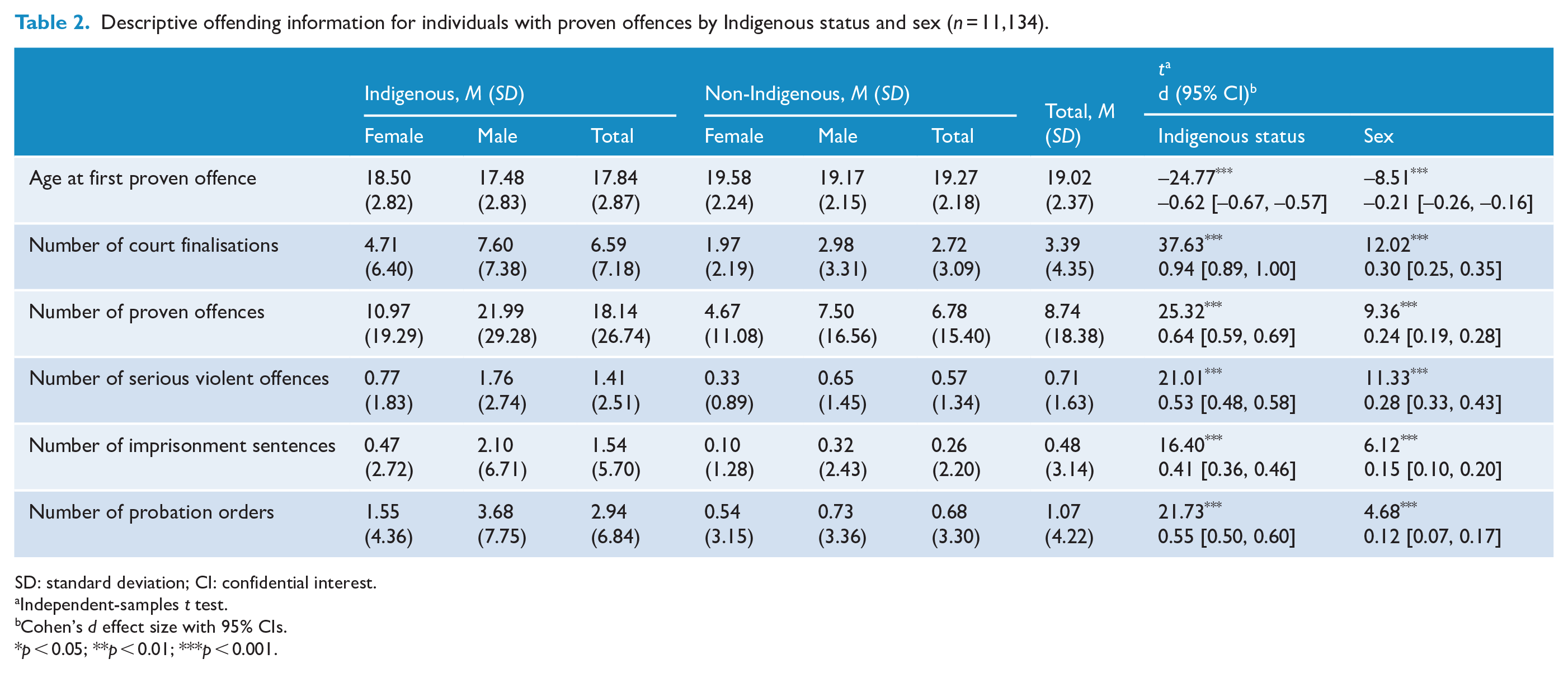
Table 2 displays descriptive information for offending characteristics by Indigenous status and sex. Compared with non-Indigenous Australians, Indigenous Australians on average were younger at their first proven offence and experienced a higher number of court finalisations, total offences, serious and violent offences, imprisonment sentences and probation orders. Males on average were younger at their first proven offence and experienced a higher number of court finalisations, total offences, serious and violent offences, imprisonment sentences and probation orders compared with females. Further details relating to offence prevalence and frequency are provided in Supplementary Table S2.
Descriptive offending information for individuals with proven offences by Indigenous status and sex (n = 11,134).
SD: standard deviation; CI: confidential interest.
Independent-samples t test.
Cohen’s d effect size with 95% CIs.
p < 0.05; **p < 0.01; ***p < 0.001.
Overlap of psychiatric illness and offending
For the entire cohort, 3.4% (n = 1556) had experienced both a proven offence and received a psychiatric illness diagnosis from a hospital admission by age 23/24 years (for details of the prevalence of psychiatric illness diagnoses, see Ogilvie et al., 2021). Significantly higher rates of overlap were observed for Indigenous compared with non-Indigenous Australians (14.8% vs 2.7%) and for males compared with females (4.4% vs 2.5%).
Among individuals who received a psychiatric illness diagnosis, 53.0% also had a proven offence. This is about double the 24.7% baseline of individuals with a proven offence for the cohort. The overlap varied across Indigenous status, with 80.5% of Indigenous Australians compared with 47.0% of non-Indigenous Australians with a diagnosed psychiatric illness also having a proven offence.
From the perspective of individuals with a proven offence, 14.0% had also been diagnosed with a psychiatric illness compared with the baseline of 6.5% for the entire cohort. This highlights that, while the rate of diagnosed psychiatric illness among individuals with a proven offence was about double the rate compared with the entire cohort, most individuals who had a proven offence did not have a diagnosed psychiatric illness. There were significant variations across Indigenous status, with 22.0% of Indigenous Australians compared with 12.3% of non-Indigenous Australians with a proven offence also receiving a psychiatric disorder diagnosis.
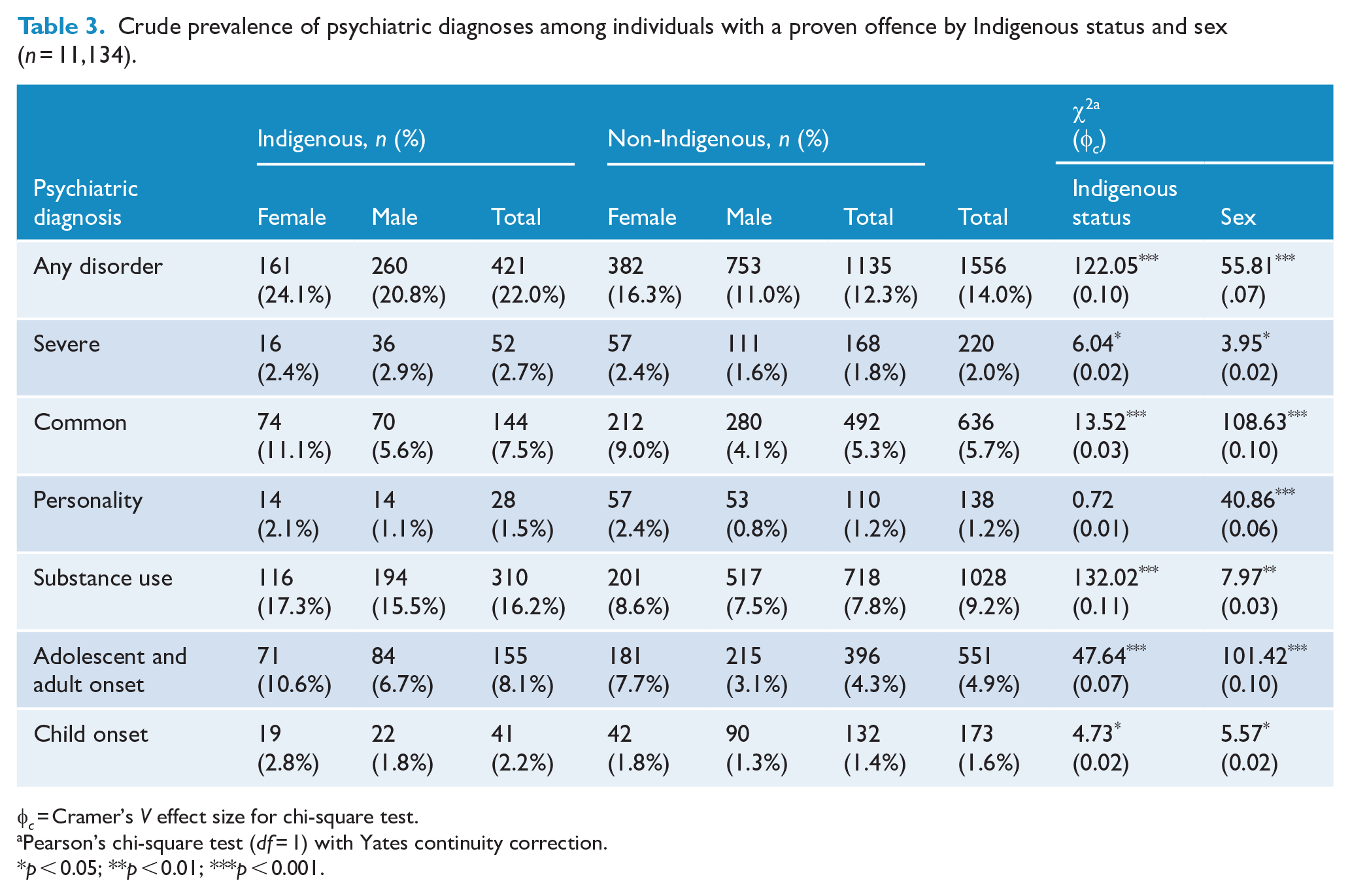
Crude prevalence rates of diagnosed psychiatric disorders for individuals with a proven offence were examined by broad categories of diagnosis and separated by Indigenous status and sex (see Table 3; prevalence rates by subdivisional categories of diagnosis are provided in Supplementary Table S3). At the broad classification level, Indigenous Australians were significantly overrepresented in all categories of psychiatric disorder except personality disorders. Indigenous overrepresentation was most pronounced for SUDs, where 16.2% of Indigenous Australians with a proven offence had received an SUD diagnosis by age 23/24 years, compared with 7.8% of non-Indigenous Australians with a proven offence.
Crude prevalence of psychiatric diagnoses among individuals with a proven offence by Indigenous status and sex (n = 11,134).
φ c = Cramer’s V effect size for chi-square test.
Pearson’s chi-square test (df = 1) with Yates continuity correction.
p < 0.05; **p < 0.01; ***p < 0.001.
Indigenous Australians with proven offences were not overrepresented in all subdivisions of diagnosis, but where significant differences between Indigenous and non-Indigenous Australians did exist, it was Indigenous Australians who had higher prevalence rates. For instance, Indigenous Australians had significantly higher prevalence rates of schizophrenia, schizoaffective and other psychotic disorders (1.9% vs 1.0%), psychotic disorders related to substance use (1.1% vs 0.7%), reaction to severe stress disorders (3.0% vs 1.5%), other anxiety disorders (2.3% vs 1.5%), alcohol use disorders (12.4% vs 5.7%), other substance disorders (7.5% vs 3.6%), self-harm (7.4% vs 3.9%) and intellectual impairment (0.7% vs 0.2%).
Cumulative prevalence rates by age of first proven offence by offence type were examined for the entire cohort stratified by psychiatric disorder diagnosis and Indigenous status (Figure 2). Significant differences in cumulative prevalence rates across the stratified groups were observed for each offence category: offences against the person, χ2(3,45,141) = 3122.77, p < 0.001; property offences, χ2(3,45,141) = 4077.27, p < 0.001; public order offences, χ2(3,45,141) = 4397.18, p < 0.001; drug offences, χ2(3,45,141) = 1993.45, p < 0.001; traffic offences, χ2(3,45,141) = 2350.65, p < 0.001 and other offences, χ2(3,45,141) = 5500.41, p < 0.001. Both Indigenous and non-Indigenous Australians who had received a diagnosis by age 23/24 years exhibited a higher cumulative prevalence of offending compared with their non-diagnosed counterparts. Indigenous Australians with a diagnosed disorder exhibited the highest cumulative prevalence rates across all offence types compared with all other groups. The disparity in cumulative prevalence rates of offending for Indigenous Australians with a diagnosed disorder history compared with all other groups amplified with age. Except for drug offences, Indigenous Australians without a diagnosed psychiatric disorder exhibited higher offending rates compared with non-Indigenous Australians both with and without a diagnosed psychiatric disorder.
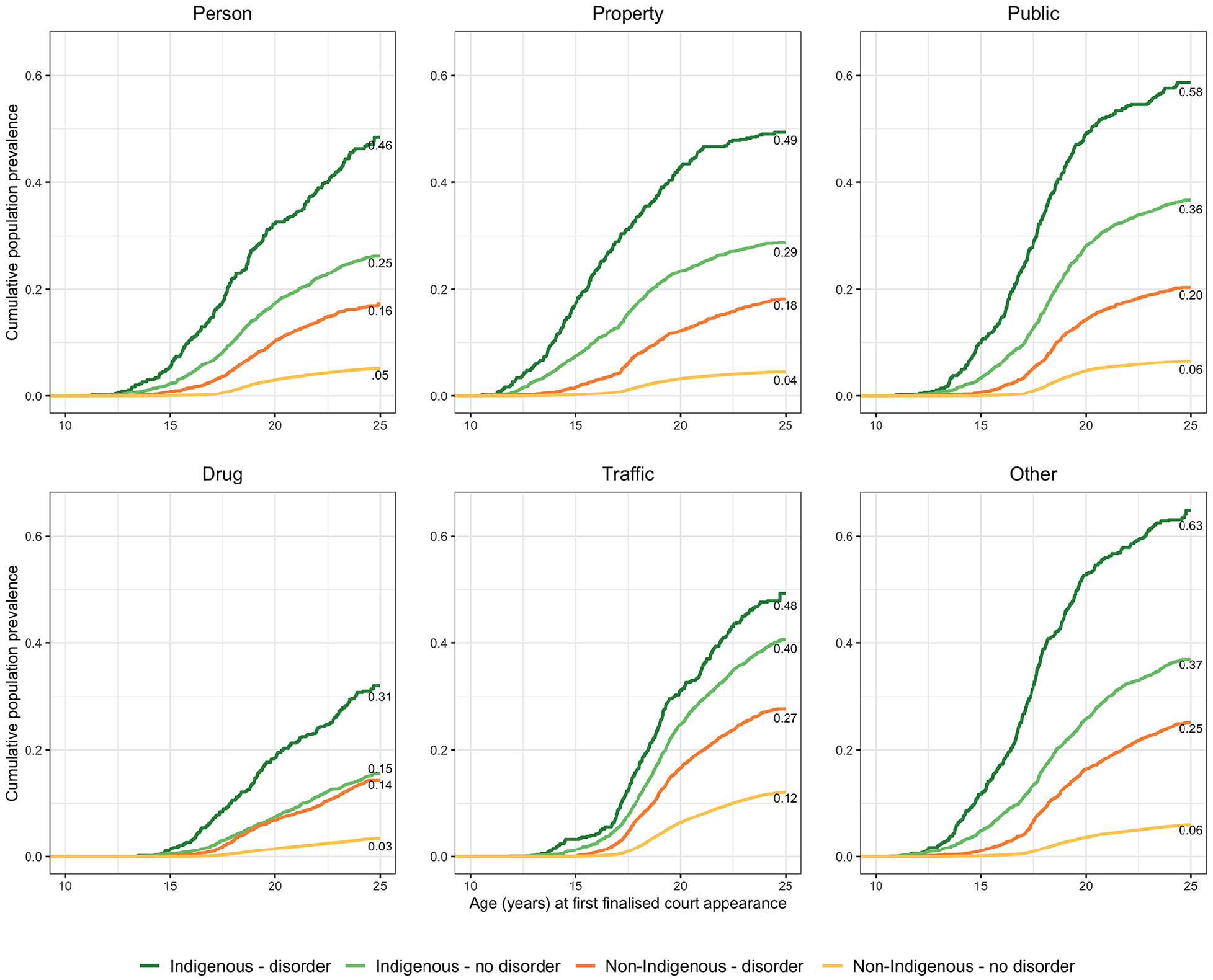
Cumulative prevalence rates of offending, with the cohort stratified by presence of a diagnosed psychiatric disorder and Indigenous status from ages 10 to 24 years (N = 45,141).
For offence frequency (Figure 3), Indigenous Australians with a diagnosed disorder were most likely to have more than five proven offences (39.2%). In contrast, only 3.3% of non-Indigenous Australians without a diagnosed disorder had more than five proven offences, with 77.7% of this group having one to two proven offences. Indigenous Australians both with and without a diagnosed disorder experienced a greater frequency of proven offences compared with non-Indigenous Australians (Kruskal–Wallis H = 892.86, p < 0.001). In addition, individuals with a diagnosed psychiatric disorder also experienced a greater frequency of proven offences compared with those without a diagnosed disorder (H = 463.00, p < 0.001).
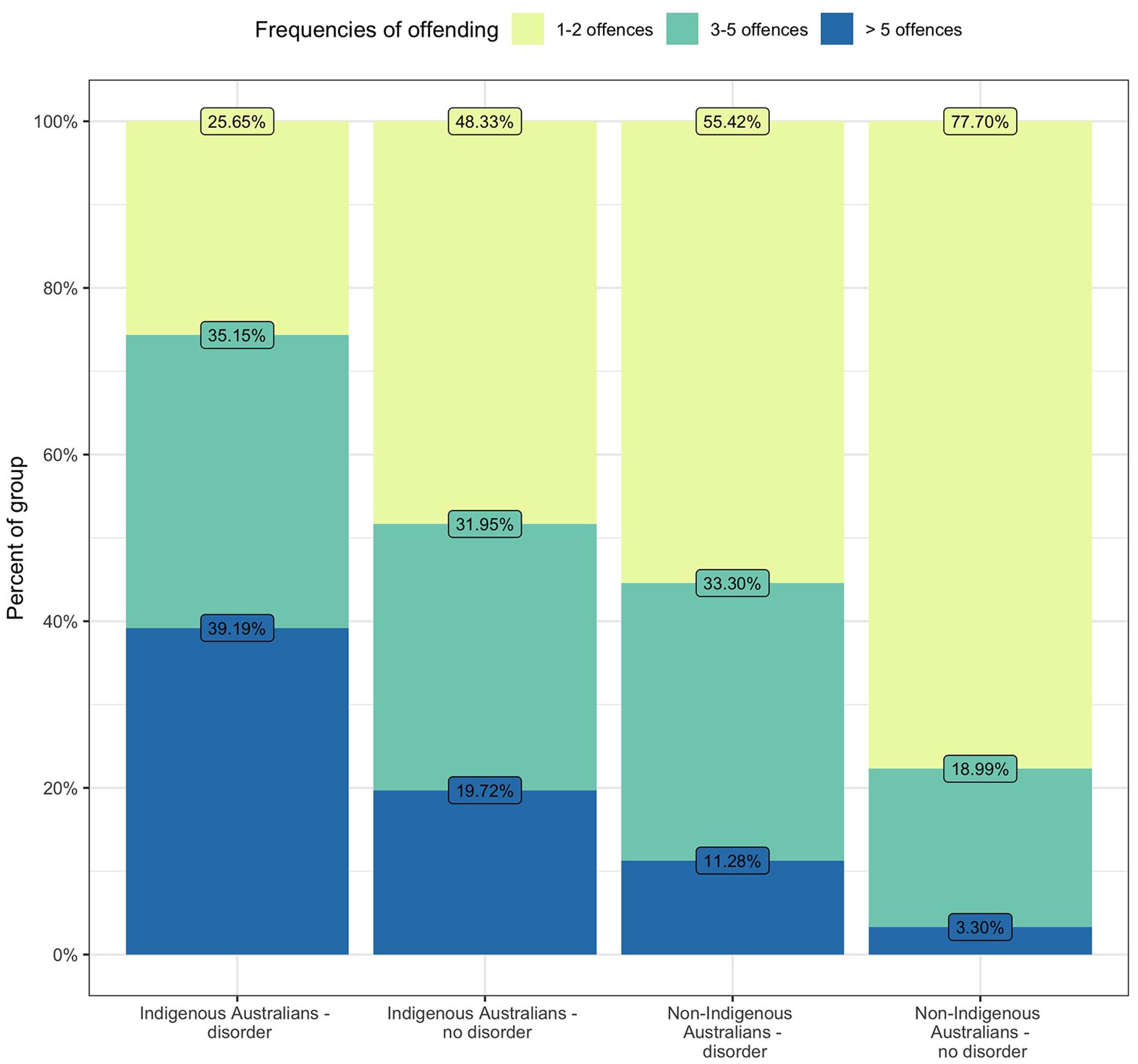
Frequency of proven offences for offenders in the cohort, stratified by Indigenous status and the presence of a diagnosed psychiatric disorder.
Associations between specific diagnoses and offences
The associations between specific psychiatric diagnoses and offence categories were examined separately for Indigenous (Table 4) and non-Indigenous (Table 5) individuals in the cohort. The pattern of significant associations between disorders and offences differed for Indigenous and non-Indigenous Australians. For non-Indigenous Australians, a consistent pattern of associations was evident, with every disorder category being associated with the presence of any offence and a higher frequency of offences against the person and drug offences. In addition, SUD and adult- and adolescent-onset disorders were also significantly associated with a higher frequency of public order offences. For Indigenous Australians, a less consistent pattern of associations was evident. First, severe disorders were not significantly associated with any offence category. Significant associations varied across the remaining disorder categories: common disorders were associated with a higher frequency of drug and other offences; personality disorders were associated with a higher frequency of offences against the person and drug offences; SUDs were associated with any offence and a higher frequency of public order and other offences and adolescent and adult-onset disorders were associated with any offence and a higher frequency of drug and other offences. Significantly lower frequencies of traffic offences were associated with adolescent and adult-onset and child-onset disorders for Indigenous Australians. Finally, for both Indigenous and non-Indigenous Australians, SUDs were most strongly associated with the presence of any offence.
Multivariate logistic regression models for associations between psychiatric disorders and categories of offending for all Indigenous individuals in the cohort (N = 2851).
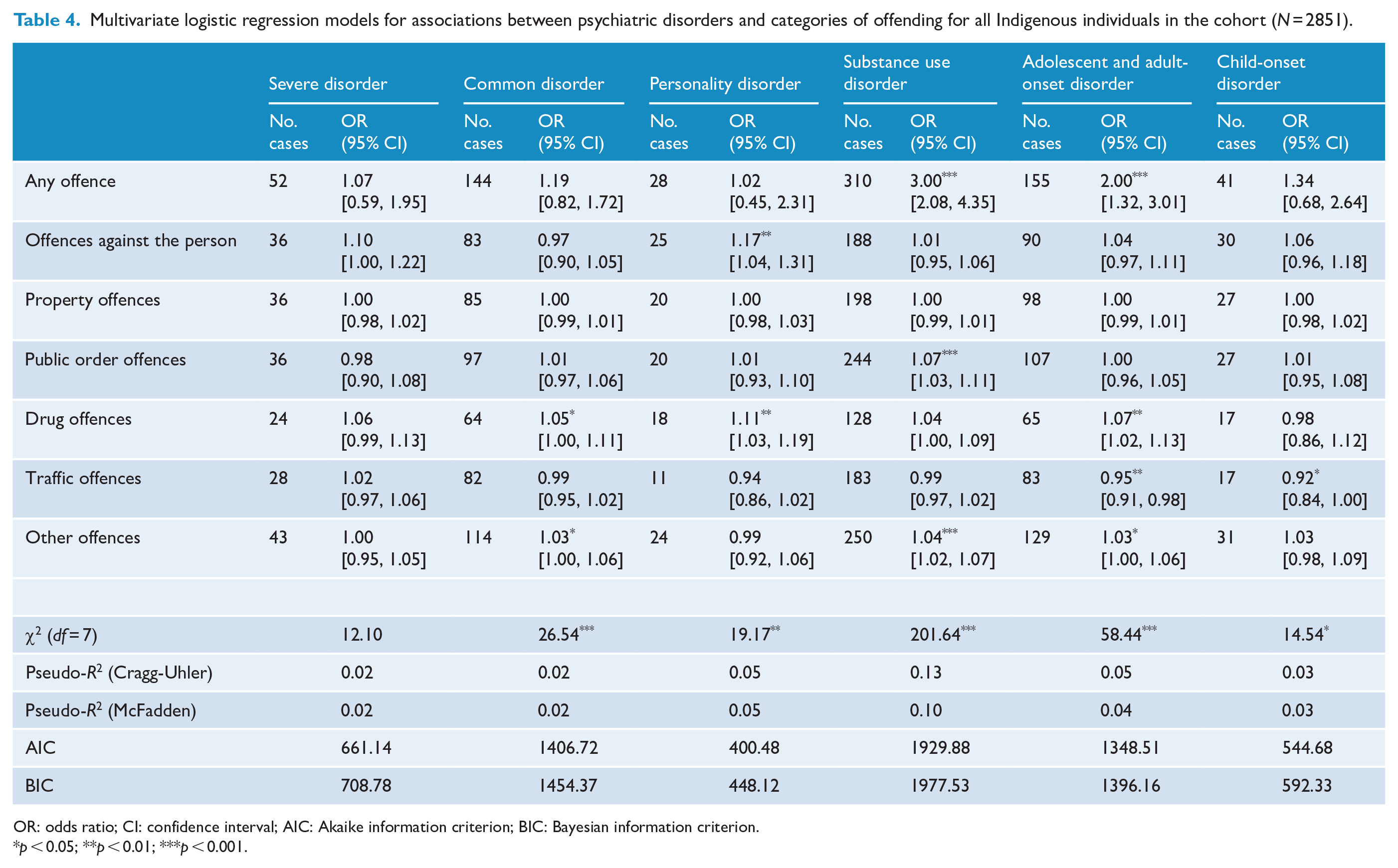
OR: odds ratio; CI: confidence interval; AIC: Akaike information criterion; BIC: Bayesian information criterion.
p < 0.05; **p < 0.01; ***p < 0.001.
Multivariate logistic regression models for associations between psychiatric disorders and categories of offending for all non-Indigenous individuals in the cohort (N = 42,290).
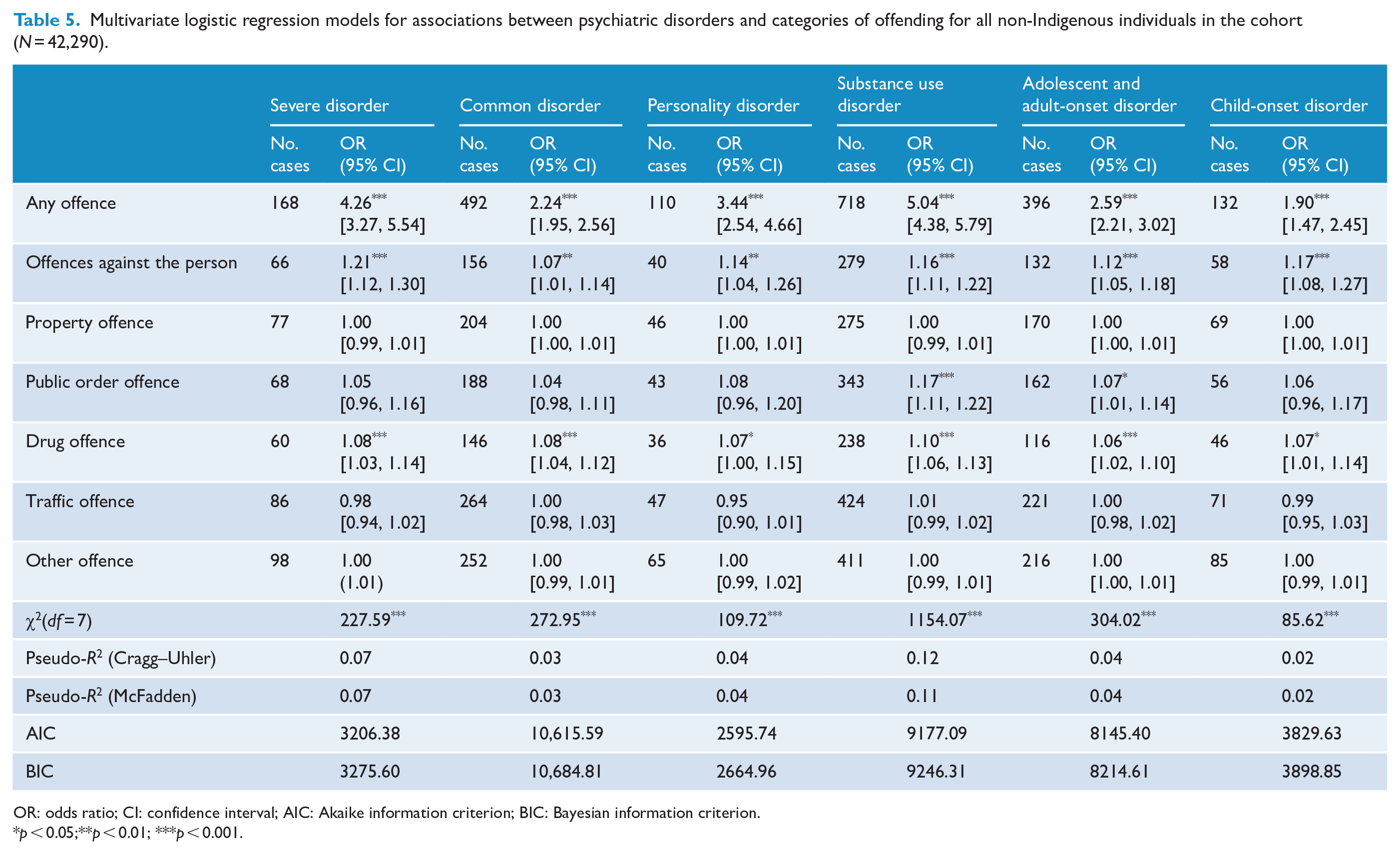
OR: odds ratio; CI: confidence interval; AIC: Akaike information criterion; BIC: Bayesian information criterion.
p < 0.05;**p < 0.01; ***p < 0.001.
Discussion
The current study extended the analysis reported by Stewart et al. (2020) to explore the overlap between diagnosed psychiatric disorders from hospital admissions and offending from proven offences for Indigenous and non-Indigenous Australians using a population-based cohort followed up to age 23/24 years. Four key findings were evident: (1) Indigenous Australians were overrepresented in proven offences; (2) the extent of the overlap between psychiatric disorders and proven offences depends on how the data were analysed; (3) the overlap between diagnosed psychiatric disorders and proven offences was most pronounced for Indigenous Australians and (4) there was some evidence of specialisation of crime type by psychiatric disorder.
Consistent with the first hypothesis, criminal justice overrepresentation was stark, with Indigenous Australians experiencing a proven offence at over 3 times the rate of non-Indigenous Australians (67.2% vs 21.8%). Indigenous individuals experienced earlier ages of onset, higher frequencies of court finalisations and proven offences, appearing for more serious offences (i.e. violent offences), and experiencing more intensive sentencing outcomes (i.e. incarceration). Indigenous males had the highest levels of overrepresentation relative to all other individuals (i.e. Indigenous females and non-Indigenous males and females), with nearly 80% experiencing at least one proven offence by age 24 years, compared with 31.7% of non-Indigenous males. With proven offences for individuals under 14 years occurring more frequently among Indigenous youth, raising the age of criminal responsibility to 14 years is a strategy to reduce overrepresentation, alongside early and targeted intervention programmes (e.g. diversion, programmes focused on serious and violent offending).
Stewart et al. (2020) found that the incarceration rate for Indigenous Australians was around 15 times greater compared with non-Indigenous Australians (12.1% vs 0.8%). The higher level of prison overrepresentation for Indigenous Australians compared with the rate of overall court finalisation overrepresentation reported for the current study indicates that overrepresentation becomes more pronounced with increasing intensity of CJS responses (i.e. custodial sentences). This is likely to reflect, in part, the seriousness and persistence of offending for Indigenous Australians (i.e. more violent offences and a higher number of overall offences over time), but ultimately it is more a reflection of the concentrated and systemic disadvantage experienced by Indigenous individuals that underlies their CJS contact (Behrendt et al., 2019). The most powerful correlates of CJS contact for Indigenous Australians include alcohol and illicit drug use among Indigenous males, as well as more concentrated economic and social disadvantage, as measured by unemployment, financial stress and low educational attainment (Weatherburn et al., 2008). These ultimately stem from the ongoing and intergenerational traumatisation and disadvantage Indigenous Australians experience from colonisation and the forced removal of children from families (Atkinson et al., 2014). Consistent with the recommendations of the Queensland Productivity Commission inquiry into imprisonment and recidivism (QPC, 2019), efforts to reduce CJS overrepresentation must be multifaceted, implemented at a community-wide level, embed Indigenous perspectives, be led by Indigenous Peoples, and be strengths-based to address the multiple determinants of increased CJS contact for Indigenous Australians. Addressing the underlying causes of overrepresentation arising from entrenched disadvantage will take time to have an effect. In the meantime, it will be important to adopt an approach that also addresses system-level drivers of overrepresentation, such as over-policing, lack of diversionary options, and inappropriate bail and remand policies that disproportionately impact vulnerable individuals (e.g. those without stable accommodation; Allard, 2010).
Consistent with the second hypothesis, psychiatric disorders were more prevalent among individuals with a proven offence, where 22.0% of Indigenous and 12.3% of non-Indigenous Australians with court contact received a psychiatric diagnosis. Among individuals with a proven offence, SUDs were the most prevalent diagnosis (9.2%), primarily driven by alcohol use disorders (6.9%). Indigenous Australians with a proven offence experienced about double the rate of SUDs compared with non-Indigenous Australians with a proven offence (16.2% vs 7.8%). The link between substance use and offending is well established and comorbidity with other mental disorders has been found to increase the risk of reoffending (Smith and Trimboli, 2010). High rates of SUD comorbidity with other disorders among Indigenous Australians have been linked to increased reoffending and incarceration (Australian Law Reform Commission, 2017). This emphasises the central role of integrated and culturally appropriate substance use and mental health interventions in addressing the needs of Indigenous Australians who have contact with the CJS to reduce overrepresentation.
Further supporting hypothesis 2, the presence of a psychiatric diagnosis was associated with an increased prevalence of proven offences. Consistent with the third hypothesis, this effect was most pronounced for Indigenous Australians, with 80.5% of Indigenous compared with 47.0% of non-Indigenous Australians with a psychiatric diagnosis also having a proven offence. The cumulative prevalence of offending results illustrated that the vulnerability of a psychiatric illness amplified the risk of contact for every category of offending, particularly for Indigenous Australians. Current knowledge on the links between psychiatric illness and offending supports the hypothesis that the offending of mentally ill individuals is largely driven by the same criminological factors as offenders without mental illness, such as substance use, homelessness, neighbourhood disorder and violence, unemployment and victimisation (Dvoskin et al., 2020). It is possible that some individuals with a psychiatric illness experience a greater concentration of criminogenic risk factors (Carr et al., 2020) and that a lack of appropriate social support systems for these individuals directly contributes to increased CJS contact. Furthermore, it is possible that the emergence of offending and development of a psychiatric illness share common risk factors that are more prevalent among vulnerable groups. This may assist in explaining the increased prevalence of overlap for Indigenous Australians and the amplifying effect of psychiatric illness on their already elevated risk of CJS contact. This emphasises the importance of building culturally appropriate social support systems to address needs and reduce the risk of continued CJS contact.
CJS contact can act as a stressor that can contribute to deterioration in mental health, which in turn may increase the risk of engagement in further antisocial behaviour and/or contact with police (Sugie and Turney, 2017). This perspective may be reflected in the finding that offenders with a psychiatric illness included a higher proportion of individuals who had a greater frequency of offences (see Figure 3). CJS contact may be utilised to divert or refer individuals experiencing mental health difficulties to specialised interventions to manage illness symptomology and potentially reduce the risk of further contact with the CJS. Court diversion processes for individuals experiencing psychosis have been found to be effective in reducing reoffending and engagement with treatment services (Albalawi et al., 2019). This highlights the importance of policy to better manage individuals with mental health difficulties and improve their CJS outcomes, where the focus should be on increasing access to and engagement with appropriate mental health services and diversion options for Indigenous Australians (Charlson et al., 2021).
Patterns of association between specific disorder and offence groupings differed for Indigenous and non-Indigenous Australians, supporting the argument that approaches to the management of intersecting mental health and offending problems and should be culturally specific. For non-Indigenous Australians, the pattern of associations was relatively consistent, with all disorder categories being associated with any form of offending, as well as a greater frequency of person- and drug-related offences. This is consistent with available evidence that severe mental disorders (i.e. which our data arguably represented given it was drawn from hospital admission records) are associated with an increased risk of engagement in violent offences (Arseneault et al., 2000) and a higher prevalence of comorbid substance use difficulties (RachBeisel et al., 1999). In comparison, patterns of association between offence and disorder groupings were less consistent for Indigenous Australians. It is possible that the comparatively fewer significant associations between offence and disorder categories for Indigenous Australians reflect the heightened prevalence of both difficulties in the population. SUDs were most strongly associated with any offence for Indigenous Australians, suggesting that culturally appropriate and effective treatment of SUDs could be a promising approach to diverting and preventing contact with the CJS for some individuals.
The current findings should be interpreted in context of the limitations of this study. Hospital admission derived psychiatric diagnoses will not capture the full extent of psychiatric morbidity in the population, given not all psychiatric illnesses or difficulties will result in a hospital admission. Those that do will be biased towards more severe and/or acute psychiatric illnesses. Given this, the rates of psychiatric illness reported in the current study should be considered conservative. Like hospital admissions, proven offences from court appearances provide a conservative estimate of CJS contact, not capturing less serious forms of contact such as police cautions. We only included records from QLD, so individuals who received hospital admission diagnoses or had proven offences interstate or overseas have not been captured. Given the age of the data (i.e. extracted in 2014), an updated extraction would provide a longer follow-up period to examine links between offending and psychiatric illness. The links between specific psychiatric disorders and offences should be interpreted with caution due to the approach taken to grouping, which may have obscured more specific associations between offences and disorders (Vinkers et al., 2011). Furthermore, the current analyses did not examine the temporal ordering of onset for psychiatric illness and offending. Finally, the current study does not provide insight into the mechanisms linking psychiatric illness and offending behaviour.
There are systematic differences and biases in how Indigenous individuals with psychiatric illness come into contact with, interact and are treated within the health system, impacting rates of hospitalisation and diagnosis (Watego et al., 2021). Practitioners may lack the knowledge, skill and cultural sensitivity to accurately detect and identify psychiatric difficulties for Indigenous Australians. For example, rates of SUDs may be inaccurate due to the possibility that practitioners are more likely to ask about and record substance use as problematic for Indigenous compared with non-Indigenous individuals (O’Leary et al., 2013).
In conclusion, findings highlight the severe levels of overrepresentation Indigenous Australians experience in contact with the criminal justice and health systems. Indigenous Australians who experienced contact with the CJS also experienced higher rates of diagnosed psychiatric disorders from hospital admissions compared with non-Indigenous Australians. For Indigenous Australians, the presence of a psychiatric diagnosis could increase the risk of earlier and more frequent CJS contact, while more frequent CJS contact could exacerbate psychiatric illnesses, emphasising that Indigenous Australians with a psychiatric disorder are a highly vulnerable group that experience a pronounced risk of contact with the CJS. The prominence of SUDs among individuals with finalised court outcomes should demonstrate the importance of interventions to address these issues, particularly for Indigenous Australians, with culturally safe and preferably Indigenous-led responses. As is often highlighted by researchers, dual overrepresentation in criminal justice and health systems reflects the extreme and accumulated socio-economic disadvantage experienced by Indigenous Australians (Cunneen, 2006; Larson et al., 2007). Ultimately, this disadvantage arises from systemic racism embedded and reflected in the operation of these and wider colonial social systems (Watego et al., 2021). Initiatives to improve criminal justice and health services will have limited impact on overrepresentation and inequalities in outcomes without fundamental changes in how these systems interact with and ensnare Indigenous Australians.
Supplemental Material
sj-docx-1-anp-10.1177_00048674211063814 – Supplemental material for Psychiatric disorders and offending in an Australian birth cohort: Overrepresentation in the health and criminal justice systems for Indigenous Australians
Supplemental material, sj-docx-1-anp-10.1177_00048674211063814 for Psychiatric disorders and offending in an Australian birth cohort: Overrepresentation in the health and criminal justice systems for Indigenous Australians by James M Ogilvie, Troy Allard, Carleen Thompson, Susan Dennison, Simon B Little, Krystal Lockwood, Steve Kisely, Ellie Putland and Anna Stewart in Australian & New Zealand Journal of Psychiatry
Footnotes
Acknowledgements
The industry partners on the grant supporting this research were Queensland Health; Department of Premier and Cabinet, Office of Economic and Statistical Research (Queensland Treasury, now called the Queensland Government Statistician’s Office [QGSO]); Department of Children, Youth Justice and Multicultural Affairs; Queensland Police; Queensland Department of Justice and Attorney-General and Queensland Registry of Births, Deaths and Marriages. The authors thank the government partners for helpful comments on a previous version of this paper. The authors gratefully acknowledge the use of the services and facilities of the Griffith Criminology Institute’s Social Analytics Lab at Griffith University. The views expressed are not necessarily those of the departments or agencies, and any errors of omission or commission are the responsibility of the authors.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Ethical Standards
The authors assert that all procedures contributing to this work comply with the ethical standards of the relevant national and institutional committees on human experimentation, and with the Helsinki Declaration of 1975, as revised in 2008.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship and/or publication of this article: This research was funded by the Australian Research Council (Grant No. LP100200469). The funder had no role in study design, the collection, analysis and interpretation of data, the writing of the report or the decision to submit the article for publication. J.M.O. was supported by a Griffith University Postdoctoral Research Fellowship.
Data Availability Statement
The data for the study are held in Social Analytics Lab (SAL) at Griffith University. Due to privacy, ethical and legal considerations, the QCRC data cannot be shared without direct approval from relevant data custodians and QGSO. Any researcher interested in accessing the data can submit an application to the SAL management committee (
Supplemental Material
Supplemental material for this article is available online.
Notes
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
