Abstract
Objective:
There is a lack of a systematic, coordinated approach to reducing the occurrence and impact of adverse childhood experiences. Hence, identifying feasible intervention priorities in this field will help inform policy and reformation of ongoing service delivery. The objective of this study was to identify expert consensus-driven priority interventions for reducing the occurrence and impact of adverse childhood experiences in children under 8 years of age in the Australian context.
Methods:
A three-round online Delphi survey was conducted to establish consensus on 34 interventions for adverse childhood experiences identified through a literature search. Six were general categories of interventions, 6 were broad intervention programmes and 22 were specific interventions. Participants were 17 health practitioners, 15 researchers, 9 policy experts, 7 educators and 3 consumer advocates with expertise in adverse childhood experiences or child mental health. Consensus was defined as an intervention being rated as ‘very high priority’ or ‘high priority’ according to its importance and feasibility by ⩾75% of all experts.
Results:
Seven of the 34 interventions were endorsed as priority interventions for adverse childhood experiences. These included four general categories of intervention: community-wide interventions, parenting programmes, home-visiting programmes and psychological interventions. Two broad intervention programmes were also endorsed: school-based anti-bullying interventions and psychological therapies for children exposed to trauma. Positive Parenting Program was the only specific intervention that achieved consensus.
Conclusion:
This is the first study to identify stakeholder perspectives on intervention priorities to prevent the occurrence and impact of adverse childhood experiences. Prioritisation of effective, feasible and implementable intervention programmes is an important step towards better integration and coordination of ongoing service delivery to effectively prevent and respond to adverse childhood experiences.
Introduction
Adverse childhood experiences (ACEs) are stressful and potentially traumatic events during childhood that can have lasting negative effects on physical and mental health. Although there is currently no standardised definition of ACEs, the common forms of ACEs include exposure to childhood maltreatment, maladaptive parenting practices (such as harsh discipline, aversiveness, over-involvement or parent–child conflict), household dysfunction (substance or alcohol misuse, family violence and parental separation/divorce), violence and socio-economic disadvantage (Fassel et al., 2019; Karatekin and Hill, 2019). ACEs are prevalent in high-income (HICs), middle-income (MICs) and low-income (LICs) countries, with up to 40–60% of adults having had at least one ACE and a quarter of adults having had at least three such experiences (Cuijpers et al., 2015; Kidman et al., 2020; Merrick et al., 2018)
There is substantial evidence demonstrating that ACEs are robustly associated with poor physical and mental health across the life course (Hughes et al., 2017; Kessler et al., 2010). The World Mental Health Survey, conducted in 21 countries worldwide, found that ACEs were associated with a twofold increased risk of first onset of common mental disorders (odds ratios of 1.6–2.0) across LICs, MICs and HICs (Kessler et al., 2010). These negative impacts were also demonstrated in meta-analyses that found a significant relationship between exposure to ACEs and subsequent onset of common mental disorders and suicidality (Bellis et al., 2019; Hughes et al., 2017). Previous studies have shown that approximately 30% of all mental disorders are attributable to ACEs (Kessler et al., 2010), including 30% of cases of anxiety disorders, 40% of cases of depression (Bellis et al., 2019) and 67% of lifetime suicide attempts (Dube et al., 2001). Given that ACEs are a major contributor to poor physical and mental health across the life course, interventions targeting the reduction in ACEs during childhood could contribute substantially to a reduction in the burden of mental disorders and other chronic diseases in the population (Hughes et al., 2017; Jorm and Mulder, 2018).
Although there is an abundance of interventions for ACEs documented in the literature, currently there exists no systematic and coordinated approach to prevent or respond to ACEs in community and clinical settings (Ellis and Dietz, 2017; Jones et al., 2020). The impact of ACEs on health and well-being is driven by a complex interplay between personal, social and environmental factors, often leading to intergenerational transmission of ACEs (Kinner and Borschmann, 2017; McEwen and McEwen, 2017). As such, interventions for ACEs vary significantly, in terms of their content, effectiveness and the type of ACEs and populations they target. Notwithstanding the range of ACE-related interventions, there is a lack of consensus from experts and stakeholders on which interventions for ACEs have the largest benefits and which are best suited for specific population groups and contexts (Ellis and Dietz, 2017; Jones et al., 2020). Similarly, decisions about which interventions to deliver need to consider several feasibility and implementation factors, including the availability of an appropriate workforce, acceptability of the intervention to stakeholders, how much the intervention costs to deliver, the ease of delivering the intervention and intervention intensity. To inform ongoing service delivery, efforts need to prioritise existing interventions that have an evidence base and are appropriate to the Australian context.
The Delphi method is a technique for systematically assembling expert opinion through a series of iterative surveys. It aims to arrive at an informed group consensus on a particular topic, (Flaherty et al., 2013) and is a preferred method to establish consensus among experts especially when evidence to support decision-making is lacking (Jorm, 2015; Thangaratinam and Redman, 2005). It has been widely used to identify intervention or policy priorities where the use of alternative methods is difficult or not feasible (Jorm, 2015). The Delphi method can also be conducted online, providing a feasible and efficient alternative to paper-based or face-to-face methods.
This study aimed to establish consensus on stakeholder priorities for effective interventions for reducing the occurrence of ACEs and their impact on mental health that are most feasible to implement in the Australian context. The findings from this study will be used to guide interventions planned by the Centre of Research Excellence in Childhood Adversity and Mental Health to co-design a sustainable service approach to prevent the significant child mental health morbidity.
Methods
The Delphi study focused on interventions targeting children under 8 years of age because the majority of ACEs in children are experienced in early childhood (Flaherty et al., 2013) and due to the substantial evidence demonstrating the benefit of interventions in the early years of life to prevent risk factors for adult mental and physical disorders (Forrest and Riley, 2004; Newton, 2015). This Delphi study was conducted in three phases: (1) literature search and identification of interventions for ACEs, (2) recruitment of expert panel members (participants) and (3) data collection and analysis. The study received ethical approval from the Melbourne School of Population and Global Health (MSPGH) Human Ethics Advisory Group (HEAG), The University of Melbourne (Ethics ID: 2056404.2)
Step 1: literature search and identification of ACE interventions
We conducted a literature search on PsycINFO (Ovid), PubMed, Embase, Cochrane Database of Systematic Reviews, Google Scholar and Cochrane Controlled Register of Trials (Central) in October 2019 to identify interventions that aim to prevent ACEs and/or ameliorate their impact. The search was performed using a combination of two search themes: (1) adverse childhood experiences, including specific ACEs (e.g. child maltreatment, household dysfunction), and (2) prevention, intervention, or reduction or mitigation. Each search theme included a comprehensive list of terms used to describe ACEs. A total of 24,099 publications were screened, and 2511 full-text publications were reviewed to identify interventions to be included in the survey. Search results were supplemented with additional searches of grey literature and reference lists of included studies. Broad and specific intervention programmes were chosen for the Delphi survey if they were (1) designed to prevent the occurrence of ACEs in children (0–8 years) or reduce their impact on mental health during or after childhood, and (2) evaluated for their effectiveness in Australia and other HICs.
A total of 32 interventions that have been evaluated for their effectiveness in preventing ACEs or reducing their negative impact on mental health in HICs were included in the Delphi. These include 6 general categories of interventions, 6 broad intervention programmes and 22 specific interventions. The list of interventions included in the Delphi is provided in Table 1.
Intervention domains, interventions and the rating process.
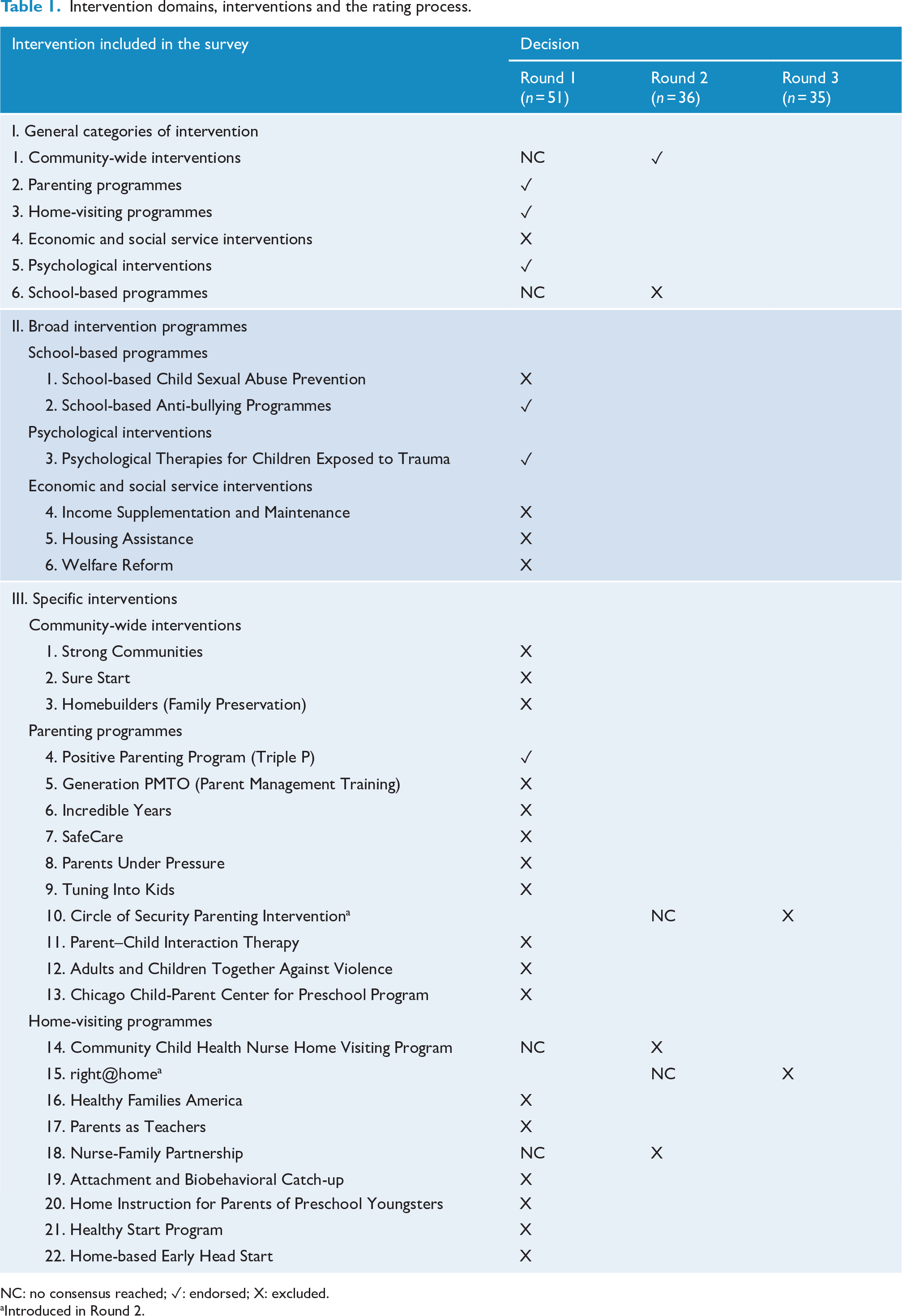
NC: no consensus reached; ✓: endorsed; X: excluded.
Introduced in Round 2.
The literature search was also used to prepare a short readable evidence summary of the interventions included in the Delphi, which panel members could use to inform their judgements. This evidence summary included a brief description of the intervention, target population, resources required for its implementation, intervention duration and intensity, levels of evidence and cost-effectiveness (Sahle et al., 2020).
Step 2: recruitment of expert panel members
As diversity of expertise among an expert panel improves quality of decision-making (Jorm, 2015), we sought to recruit participants with a variety of expertise relevant to ACEs. Researchers, health practitioners, educators, health and social policy experts, and mental health consumer advocates across Australia were invited to participate. The inclusion criteria for consumer advocates were adults (18 years or older) who have (1) experienced ACEs or been a carer to someone who has experienced ACEs, and (2) experience in a mental health advocacy role (e.g. membership of an advocacy organisation). Health practitioners, educators, and health or social services policy development experts were eligible if they had at least 5 years’ experience in the area of child mental health in Australia. Academic experts were individuals who have an established reputation in mental health and/or ACEs and have published articles relevant to ACEs and mental health. Participants were recruited via email or newsletters through consumer networks, professional organisations, examination of authorship of relevant literature on ACEs and child mental health, and snowball sampling (i.e. encouraging those who received the recruitment email to forward it on to other Australian experts who may have an interest in participating).
Step 3: data collection and analysis
A three-round online Delphi study was conducted between May and September 2020. All survey rounds were administered via Qualtrics Survey Software, and survey weblinks were distributed via email. Participants rated each intervention according to its importance and the feasibility of its implementation in the Australian context, as being of ‘very high priority’, ‘ high priority’, ‘medium priority’, ‘low priority’ or ‘very low priority’. In making their rating, in addition to their experience and knowledge about ACEs, experts were provided with an evidence summary (from Step 1 above) for each intervention to inform their judgement. The Round 1 survey included open-ended questions asking the participant to provide a rationale for each rating. The survey included a diverse range of interventions, and therefore, participants were given the option to skip a set of interventions if they believed it was out of the scope of their expertise. Participants could also suggest new interventions for ACEs in Round 1. Only participants who completed the Round 1 survey were invited to complete the Round 2 survey, and only those who participated in Round 2 were invited to complete the Round 3 survey. A sample size for Delphi studies of 15–60 panellists and assuming a drop-out rate across Delphi survey rounds of 20%, the remaining panel size of 23 has been shown to provide sufficient stability of responses in a bootstrap sampling study (Akins et al., 2005).
On completion of each round, the percentage of participants’ responses to the 5-point Likert-type scale (‘very high priority’ to ‘very low priority’) was calculated and categorised as follows:
Endorsed: An intervention was endorsed if it received ‘very high priority’ or ‘high priority’ ratings from at least 75% of the respondents, which is the most commonly used threshold to define consensus in Delphi studies (Diamond et al., 2014).
No-consensus: Interventions rated by 65–74% of the participants as ‘very high priority’ or ‘high priority’ were re-rated in one subsequent survey round.
Exclude: Interventions rated as ‘very high priority’ or ‘high priority’ by less than 65% of the panel members were excluded.
A summary report on Round 1 and 2 findings along with individualised feedback about how each expert’s responses compared to those from the rest of the group was provided to Round 2 and Round 3 participants, respectively. Participants could use these reports to modify their response in light of the overall endorsement by other Delphi panellists. The first author thoroughly read the responses to the open-ended questions about the rationale for each rating to identify the most common reasons why interventions were endorsed or excluded.
Results
Participants
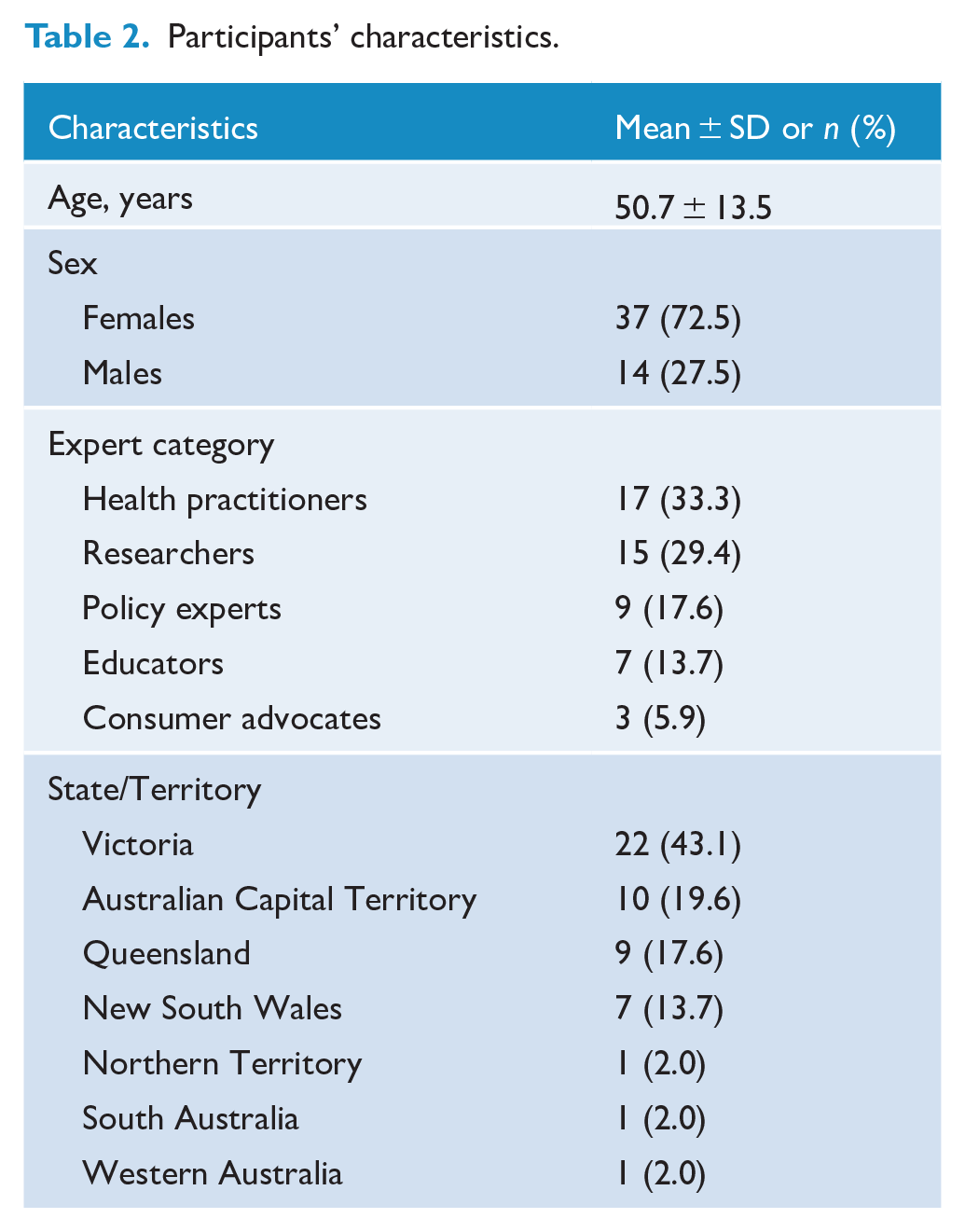
Fifty-one participants completed the first-round survey. Two-thirds of the participants were health practitioners (33%) or researchers (29%) and the remainder were policy experts (18%), educators (14%) or consumer advocates (6%). Of the 51 participants, 37 were females and 14 were males, and the average age was 50.7 years (standard deviation [SD]: 13.5 years; range: 19–82 years). Participants were recruited from seven Australian States and Territories, mostly from Victoria (43%) and New South Wales (20%). The participants’ characteristics are summarised in Table 2. Of the 51 experts in Round 1, 36 experts completed Round 2 and 35 experts completed Round 3.
Participants’ characteristics.
Intervention priorities
Across the three survey rounds, four general categories of interventions, two broad intervention programmes and one specific intervention reached a consensus as priority interventions for ACEs. In Round 1, three general categories of interventions (parenting programmes, home-visiting programmes and psychological interventions), two broad intervention programmes (school-based anti-bullying programmes and psychological therapies for children exposed to trauma) and one specific intervention (Positive Parenting Program [Triple P]) achieved a consensus. At the same time, 22 interventions were excluded because they did not receive sufficient priority. Four interventions did not achieve consensus but satisfied criteria for re-rating in Round 2. In this round, two additional specific interventions (Circle of Security and right@home) were suggested by the experts to be included in the survey. Figure 1 outlines the number of interventions for ACEs that achieved consensus.
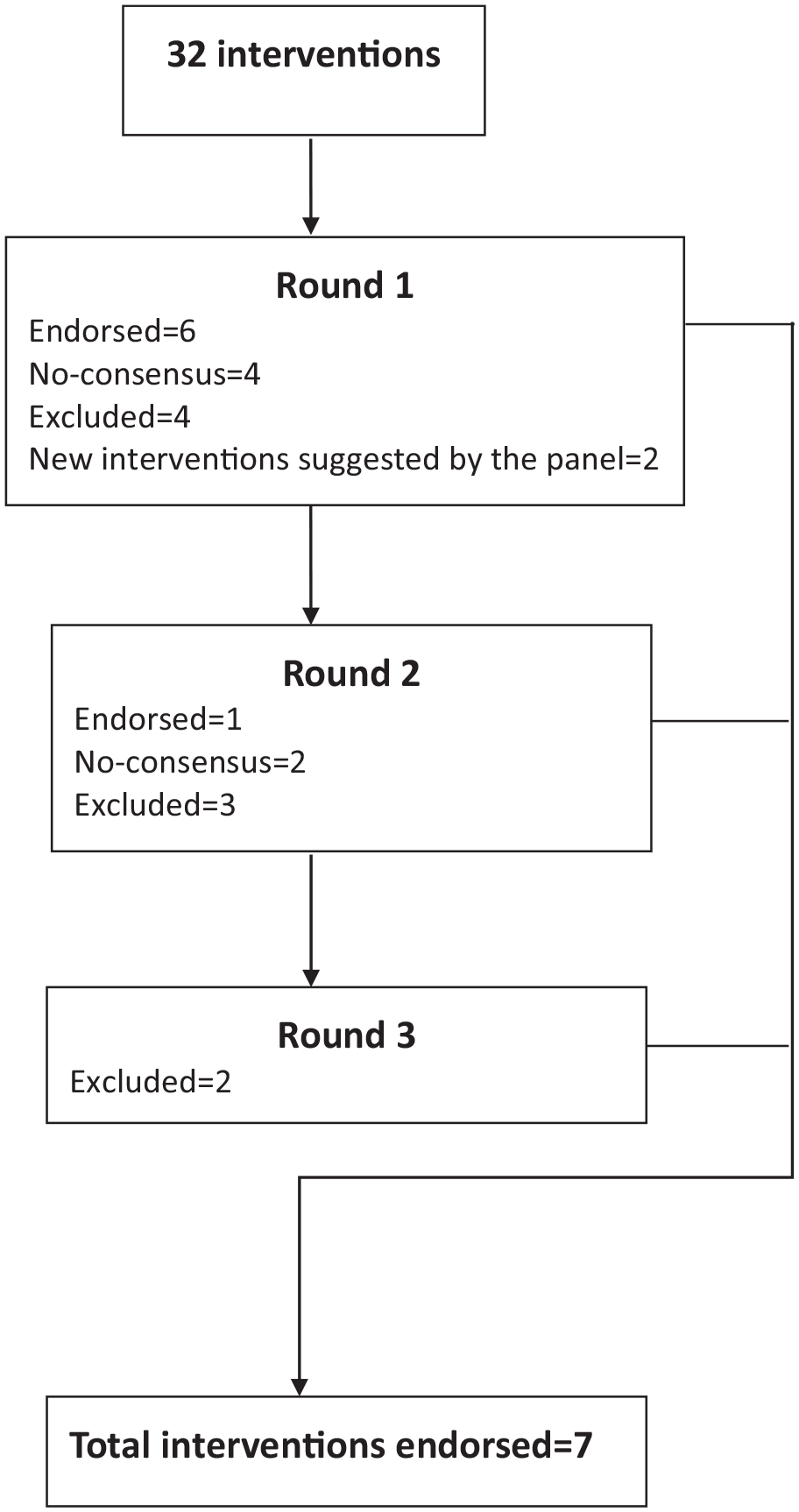
Number of interventions for ACEs that achieved consensus.
Of the six interventions included in the second round, only community-wide interventions reached consensus, while Circle of Security and right@home did not reach consensus but reached criteria for re-rating and were included in Round 3. The third round of the Delphi survey included two specific interventions, Circle of Security and right@home, and both interventions did not achieve a consensus. The summary item ratings across the three rounds are provided in Table 1, and the full list is summarised in Supplementary File 1.
The top five reasons why interventions were endorsed as a priority were also identified (Table 3). Among the commonest reasons for endorsing an intervention was the presence of evidence of effectiveness and/or cost-effectiveness to reduce ACEs or their impact on mental health. Other common reasons were that the intervention has been tried and tested in an Australian context; targets a broad range of ACEs and population groups; is preventive; and can be tailored to the needs of families. The most common reasons for interventions being excluded as less of a priority were also identified (Table 3). These included that the intervention is costly (resource intensive); there is limited supporting evidence base; has a narrow scope; is not readily transferrable to the Australian context; and existing programmes would offer the same services. The full list of most common rationales reported by the participants for rating each of the interventions is presented in Supplementary File 2.
Common reasons for rating interventions.
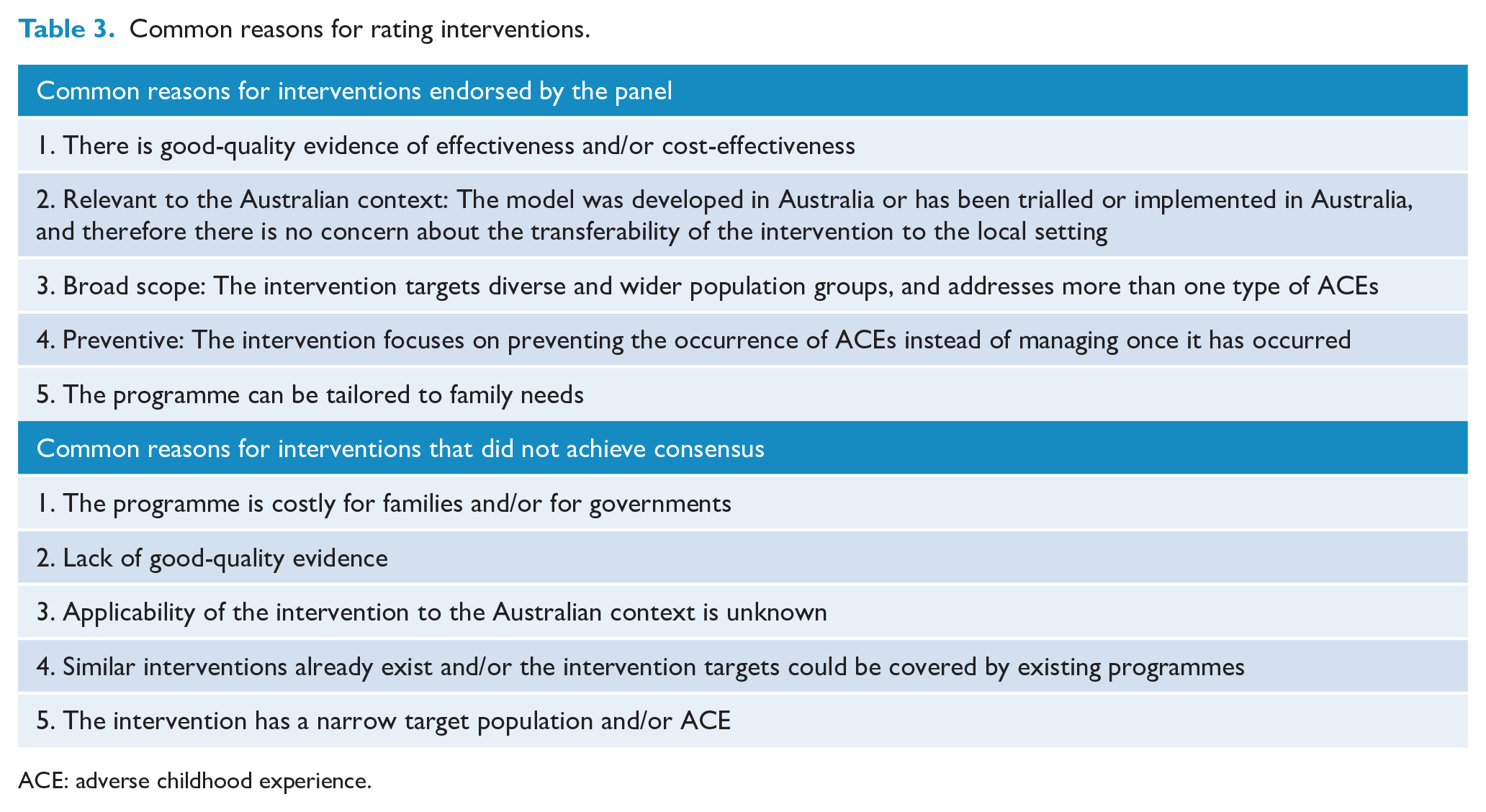

ACE: adverse childhood experience.
Discussion
This is the first study to identify intervention priorities for reducing ACEs and their impact, according to their feasibility for implementation in the Australian context. A consensus was reached on four general categories of interventions, two broad intervention programmes and one specific intervention. Experts with diverse expertise and background, including people with lived experience, were recruited into the Delphi, and thus multiple stakeholders have contributed to the identification of priority interventions reported in this study.
One of the main findings of our study is that 6 out of the 7 interventions that achieved consensus were general categories of interventions or broad intervention programmes compared to only 1 out of 26 specific interventions that reached consensus. This finding indicates that the experts agreed on broad areas where action is needed, but did not always think there were specific interventions that stood out from the others within these domains. The endorsement of the general or broader categories of interventions is also in line with the upstream approach to prevention that focuses on improving fundamental social and structural determinants of ACEs (Srivastav et al., 2019), which was also reflected in the participants’ responses to open-ended questions. For example, one policy and advocacy expert participant commented, ‘A single intervention may not be as successful as a more holistic approach for families with higher and more complex needs. They need to be combined with a range of other broadly targeted initiatives for more comprehensive effect’.
General categories of interventions
The consensus on parenting and home-visiting programmes is expected given that these programmes are the most common approaches for promoting child health and preventing common ACEs, such as maladaptive parenting and child maltreatment (Casillas et al., 2016; Holzer et al., 2006). Positive parenting practices and a safe and supportive home environment are essential for promoting and protecting health and development during childhood (Casillas et al., 2016; Kenneth et al., 2020). The experts also endorsed psychological interventions noting the significant effects of interventions that aim to enhance child social, emotional and behavioural competencies and resilience. The participants also endorsed community-wide interventions mentioning that community strength is an important social determinant of health and development. One participant said, ‘The most important factor countering mental disorders is enhanced social capital. Hence, community-wide programs have the greatest potential to influence the greatest number of people in need’. This aligns with the current evidence showing that empowering communities to promote normative changes in perceptions, beliefs and behaviour, and enhancing community connectedness and social capital are essential to create an inclusive child-friendly and family-supportive environment (Hall et al., 2012). From a policy perspective, endorsement of four out of the six general categories of interventions suggests that preventing and responding to ACEs require a system-wide approach that integrates and coordinates efforts across sectors, services and platforms such as antenatal care, maternal and child health services, and early childhood.
Economic and school-based interventions were the two general categories of interventions that did not achieve consensus. In the open-ended responses, the participants noted that Australia has an already established social protection system to support low-income families, and that further change in economic policies would be neither a priority nor feasible. School-based system-level intervention was not rated as a priority intervention. The universal nature of schools provides opportunities to reach children. Nonetheless, participants indicated that numerous school-based intervention programmes are already available in Australia, making new interventions less appealing. For example, one researcher panel member said, ‘Many schools already have programs although they should be refreshed. There should be further attention to cultural appropriateness of the materials and further efforts to support teachers in religious private and independent schools’.
Broad intervention programmes
Experts endorsed anti-bullying interventions as school-based interventions that warrant implementation, suggesting that this intervention is feasible and important to the Australian context. These are an important group of interventions given that more than a quarter of all school children report bullying experiences,(Ford et al., 2017), and anti-bullying programmes reduce bullying victimisation and increase empathy and support for victims of bullying (Ttofi and Farrington, 2011). One participant said, ‘Any program that shows evidence of reducing rates of bullying perpetration and victimisation is likely to have population benefits’. Participants endorsed psychological therapies for children exposed to trauma, citing the evidence for the effectiveness in prevention of mental disorders and improving outcomes. This aligns with the current literature showing children exposed to ACEs have greater risk of adverse outcomes (such as depression, suicide attempt, conduct disorder, alcohol dependence, anxiety) (Merrick et al., 2018) and psychological therapies reduce the onset of mental disorders in children exposed to trauma (Gillies et al., 2016).
Specific interventions
Of the 22 specific interventions rated, only Triple P achieved consensus. The participants cited that Triple P is relatively costly and its suitability to low-income families is not well understood; however, it is an Australian programme, is adaptable to different environments (e.g. can be offered online) and has a robust evidence of its effectiveness. One participant said,
Triple P is an established program with strong evidence of positive outcomes. It will not be primarily targeted to some childhood adversities (e.g., parental separation), but is likely to build child/family resilience to dealing with the stress related with these adversities. It’s a tiered and targeted program.
Of the 21 specific interventions that did not achieve consensus, 18 were developed in the United States and their cost-effectiveness was not well established (Sahle et al., 2020).
Given the complexity of ACEs, no single intervention programme can be expected to effectively prevent the occurrence of ACEs and mitigate their impact on mental health. A multi-level holistic approach that takes into account the interplay between the individual, the family, the community and the larger socio-political structure is more likely to have the largest impact on the population burden of ACEs (Di Lemma et al., 2019; Oral et al., 2016). Consistent with this, the intervention priorities identified in this Delphi study reflect the need for a ‘whole of system’ approach involving multiple sectors and stakeholders to effectively and sustainably prevent ACEs and mitigate their impacts.
This study has a few limitations. The study focused on interventions that target children under 8 years of age, and those interventions that target children aged 0–8 years of age were not included in the Delphi. Another limitation of our study is that the effectiveness of interventions for ACEs has not been evaluated in children from indigenous or culturally and linguistically diverse populations. Further research is needed to better understand the needs, priorities or implementability of programmes for children from these families.
Conclusion
This Delphi study identified intervention priorities to reduce the occurrence of ACEs and their impact on mental health that are most feasible and implementable in the Australian context. The list of intervention priorities identified in the Delphi study reflect input from a diverse range of stakeholders and could inform the development of comprehensive and integrated approaches for preventing and responding to ACEs in Australia.
Supplemental Material
sj-xlsx-1-anp-10.1177_00048674211025717 – Supplemental material for A Delphi study to identify intervention priorities to prevent the occurrence and reduce the impact of adverse childhood experiences
Supplemental material, sj-xlsx-1-anp-10.1177_00048674211025717 for A Delphi study to identify intervention priorities to prevent the occurrence and reduce the impact of adverse childhood experiences by Berhe W Sahle, Nicola J Reavley, Amy J Morgan, Marie Bee Hui Yap, Andrea Reupert and Anthony F Jorm in Australian & New Zealand Journal of Psychiatry
Footnotes
Acknowledgements
We wish to acknowledge panellists who took part in the Delphi study and shared their expertise with us.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship and/or publication of this article: This study is funded by NHMRC and Beyond Blue co-funded Centre of Research Excellence in Childhood Adversity and Mental Health (#1153419). The funders had no role in study design or preparation of this report.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
