Abstract
Objective:
To assess the impact, in the Australian setting, of the COVID-19 lockdown on antipsychotic supplies for patients with schizophrenia following a prescription from a new medical consultation when compared to the same periods in the previous 4 years. A secondary objective was to assess the volume of all antipsychotic supplies, from new and repeat prescriptions, over these same periods.
Methods:
A retrospective pharmaceutical claims database study was undertaken, using the Department of Human Services Pharmaceutical Benefits Scheme 10% sample. The study population included all adult patients with three or more supplies of oral or long-acting injectable antipsychotics for the treatment of schizophrenia at any time between 1 June 2015 and 31 May 2020. The primary outcome compared volumes of dispensed antipsychotics from new prescriptions (which require a medical consultation) between 1 April and 31 May each year from 2016 to 2020. This was to analyse the period during which the Australian Government imposed a lockdown due to COVID-19 (April to May 2020) when compared the same periods in previous years.
Results:
There was a small (5.7%) reduction in the number of antipsychotics dispensed from new prescriptions requiring a consultation, from 15,244 to 14,372, between April and May 2019 and the same period in 2020, respectively. However, this reduction was not statistically significant (p = 0.75) after adjusting for treatment class, age, gender, location and provider type.
Conclusion:
The COVID-19 restrictions during April and May 2020 had no significant impact on the volume of antipsychotics dispensed from new prescriptions for patients with schizophrenia when compared to the volume of antipsychotics dispensed from new prescriptions during the same period in previous years.
Introduction
COVID-19 was first confirmed in Australia in late January 2020 (Department of Health, 2020a). Cases rose rapidly so a nationwide lockdown was implemented from 23 March 2020, including the closure of non-essential services and travel restrictions. Public health orders were put in place on 29 March 2020, requiring people to leave their homes only for work, study, grocery shopping, exercise and medical care (e.g. pharmacies, general practitioners, psychiatrists) (Moynihan et al., 2020).
Australia has had fewer cases of COVID-19 cases compared to many countries (Dong et al., 2020), with just under 30,000 confirmed cases and approximately 900 deaths by the end of 2020 (Department of Health, 2020a). From 13 March 2020, Medicare Benefits Scheme (MBS) telehealth items were introduced to protect patients and healthcare providers and ensure essential services were maintained during the lockdown (Department of Health, 2020b).
Data on the mental health effects of COVID-19 have been mixed and show variation by reporting method. In general, self-reported symptoms including those collected with the Patient Health Questionnaire (PHQ-9) depression rating or the 12-item General Health Questionnaire (GHQ-12) show increases in comparison with population norms or pre-pandemic assessments (Czeisler et al., 2020; Jia et al., 2020; Pierce et al., 2020). However, a subsequent systematic review found no evidence of an increase in symptoms during COVID-19 lockdowns (Richter et al., 2020). Similarly, there has been no rise in suicide rates in Massachusetts (USA), Victoria (Australia) and England in the early months of the pandemic (John et al., 2020), and in Japan and Norway, suicide rates fell (John et al., 2020) although there was evidence of a subsequent rise in Japan during the second wave (July to September 2020) (Sakamoto, 2021; Tanaka and Okamoto, 2020). While there are numerous studies of the effect of COVID-19 and lockdown restrictions on mental health in general, there are no known studies of its effect on the management of schizophrenia. This subject is particularly important due to the difficulty individuals with schizophrenia have self-advocating and engaging with mental health services.
In terms of health service contacts, there have been mixed findings. For instance, emergency department visits for mental health problems increased during the initial Australian lockdown period (Kam et al., 2020). By contrast, those related to other health issues fell (Kam et al., 2020). Data on billings for psychiatrist visits in Australia showed an increase during the lockdown but this masked a reduction in face-to-face consultations, which were only 64% of those in the equivalent quarter of 2019. The increase was therefore associated with the introduction of the MBS telehealth items noted above (Looi et al., 2020). The number of face-to-face contacts increased later that year although the demand for telehealth consultations remained steady (Looi et al., 2021). The need for a shift in focus from consultations in person to those through telehealth was underlined by the Italian experience during the initial wave of the epidemic in early 2020 where both residential and outpatient facilities experienced severe operational difficulties (De Girolamo, 2020).
Demand for virtual, online services in Australia has also reflected pandemic waves by time and place although increases in contacts and associated psychological morbidity have been short-lived as the number of COVID cases subsequently declined (Staples et al., 2020, 2021; Titov et al., 2020). It is also possible that immediate stimulus to the economy to protect incomes and preserve employment may have acted as a buffer and that the full consequences may only become apparent as these measures are rolled back.
Internationally, a recent systematic literature review of 81 studies across 20 countries found consistent evidence of major reductions in general healthcare use up to May 2020, compared to previous years (Moynihan et al., 2020). However, there was also a 30% increase in prescriptions from 28 studies (Moynihan et al., 2020). In general, there have been larger reductions in general health service in populations with milder or less severe general health problems (Kam et al., 2020), but it is uncertain whether these results apply to people with severe mental illness such as schizophrenia. The main objective of this study was to compare the volumes of new antipsychotic prescriptions dispensed in Australia during the nationwide lockdown in April and May 2020 due to COVID-19 to the same period in the previous 4 years.
Methods
Data source
This was a retrospective national pharmaceutical claims database study, using the national Pharmaceutical Benefits Scheme (PBS) ‘10% sample’ – a random sample, representative of the whole data. The ‘10% sample’ is the standard database administered by the Australian Government for analysis by third parties. Australia’s PBS subsidises prescriptions for all Australian citizens and permanent residents. The dataset contained all PBS supplies (new and repeat prescriptions) for individuals in the 10% random sample with a date of supply between 1 June 2015 and 31 May 2020. Approval to use the PBS 10% sample for this analysis was provided by the Government’s External Requests Evaluation Committee on 21 July 2020.
Study population
Second-generation antipsychotics are the most commonly prescribed medications for schizophrenia in Australia (Services Australia, 2020), and clinicians are required to provide an indication-specific authority code for this diagnosis so the patient can receive the PBS subsidy.
The general study population included all patients at least 18 years old with three or more supplies of antipsychotics for the treatment of schizophrenia at any time between 1 June 2015 and 31 May 2020. The population for the primary outcome included patients from the general study population who had a supply from a new prescription for an antipsychotic (requiring a medical consultation) during April or May in at least one of the five years from 2016 to 2020. The population for the secondary outcome included patients from the general study population who received at least one supply (new or repeat prescription) of an antipsychotic during the same time period. Repeat prescriptions allow a patient to obtain additional supplies of the same medication without a new medical consultation. An indication of schizophrenia was ascertained for each supply either from diagnosis-specific authority codes when required (i.e. second-generation antipsychotics) or by the dosage level for oral first-generation antipsychotics, as these do not require an authority code (e.g. chlorpromazine above 100 mg per day and haloperidol above 5 mg per day were considered to be doses associated with the schizophrenia diagnosis).
Low doses (<100 mg chlorpromazine equivalent) of some second-generation antipsychotics commonly used for other indications (olanzapine, quetiapine, risperidone) were not used to ascertain an indication of schizophrenia. All prescribed first-generation long-acting injectable (LAI) antipsychotics were assumed to be used for schizophrenia. The full list of included treatments with a designated indication for schizophrenia is listed by dose and PBS item number in Supplemental Table 1. No additional exclusion criteria were applied.
Patient demographics for patients supplied antipsychotics from new prescriptions, by year.
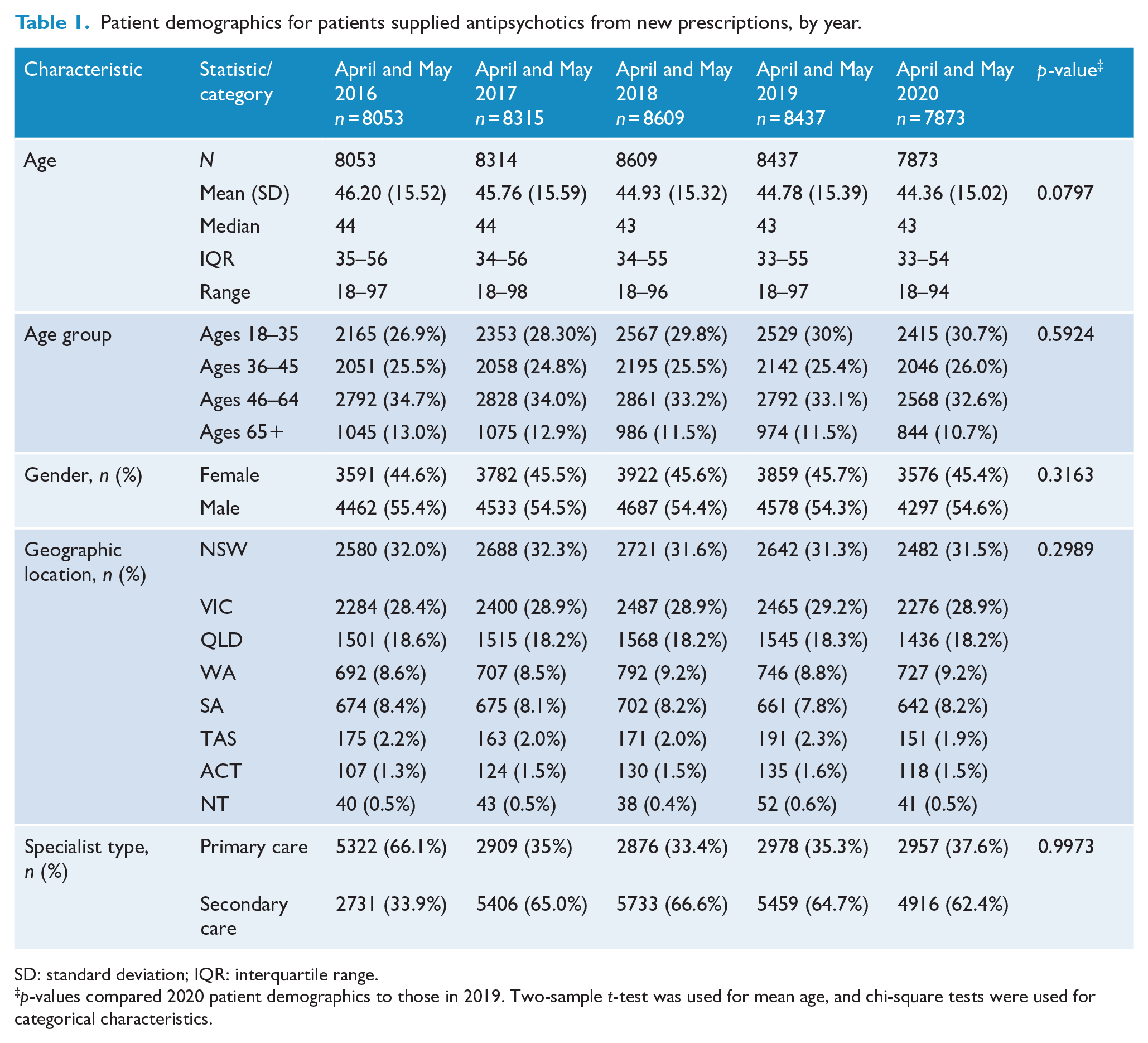
SD: standard deviation; IQR: interquartile range.
p-values compared 2020 patient demographics to those in 2019. Two-sample t-test was used for mean age, and chi-square tests were used for categorical characteristics.
Analyses
Descriptive statistics were used to present the patient characteristics and new antipsychotic prescriptions by period. Changes in patient characteristics between the periods pre and post COVID-19 lockdown (2019–2020) were evaluated using a Student’s t-test for continuous variables and a Pearson’s chi-square test for categorical variables.
The primary analysis examined the volumes of new antipsychotic prescriptions that required a medical consultation and were dispensed between 1 April and 31 May for each year from 2016 to 2020, based on the date of supply. A linear regression model which included covariates for year, treatment class, age, gender, state and provider type was used to assess the impact of year and date on prescription volumes while adjusting for secular trends.
A secondary analysis was conducted for all antipsychotic supplies (new and repeat prescriptions) using the same methods as for the primary analysis. All analyses were conducted in SAS v9.4.
Primary care provider settings consisted of general practice, emergency medicine and community healthcare. Other specialist types were classified as secondary care providers. Treatment class was based on formulation (oral or LAI) and type (first or second generation).
Results
In April and May 2020 a total of 40,582 antipsychotic treatments were dispensed to patients with schizophrenia in the PBS 10% sample, of which 14,373 (35%) were from new prescriptions. Similarly, in April and May during the preceding 4 years (2016–2019), 36% of the total antipsychotic supplies dispensed were from new prescriptions.
In April and May 2020, these 14,373 new prescriptions were dispensed to 7873 patients. Men made up 55% of patients dispensed antipsychotic treatments from new prescriptions for schizophrenia in all years. Distribution across Australian states was roughly proportional to the state populations with approximately 80% of all patients in the sample residing in New South Wales, Victoria and Queensland. Approximately two thirds of patients received prescriptions from secondary care providers between 2017 and 2020, although in 2016 the proportions were reversed.
Patient characteristics were consistent over the 5 years other than the percentage of antipsychotic prescriptions initiated in primary care versus secondary care in the 2016 period. There were no statistically significant differences in the characteristics of patients in 2020 compared to the years prior to COVID-19 (Table 1).
Primary outcome
In terms of the primary outcome, there was a small (5.7%) reduction in the number of new antipsychotic supplies from new prescriptions (from 15,244 to 14,372) between April and May 2019 and the same period in 2020. Second-generation oral antipsychotics were the most commonly dispensed group of antipsychotics from new prescriptions with 12,898 individual prescriptions during April and May 2020, being a reduction of 6.4% (from 13,775) during the same period in 2019. Second-generation LAI antipsychotic supplies from new prescriptions increased by 0.6% between April and May 2020 and the same period in 2019, continuing the positive trend from the previous years. The supply levels from new prescriptions of first-generation oral and LAI antipsychotics were comparatively low in April and May for all years assessed (Figure 1).
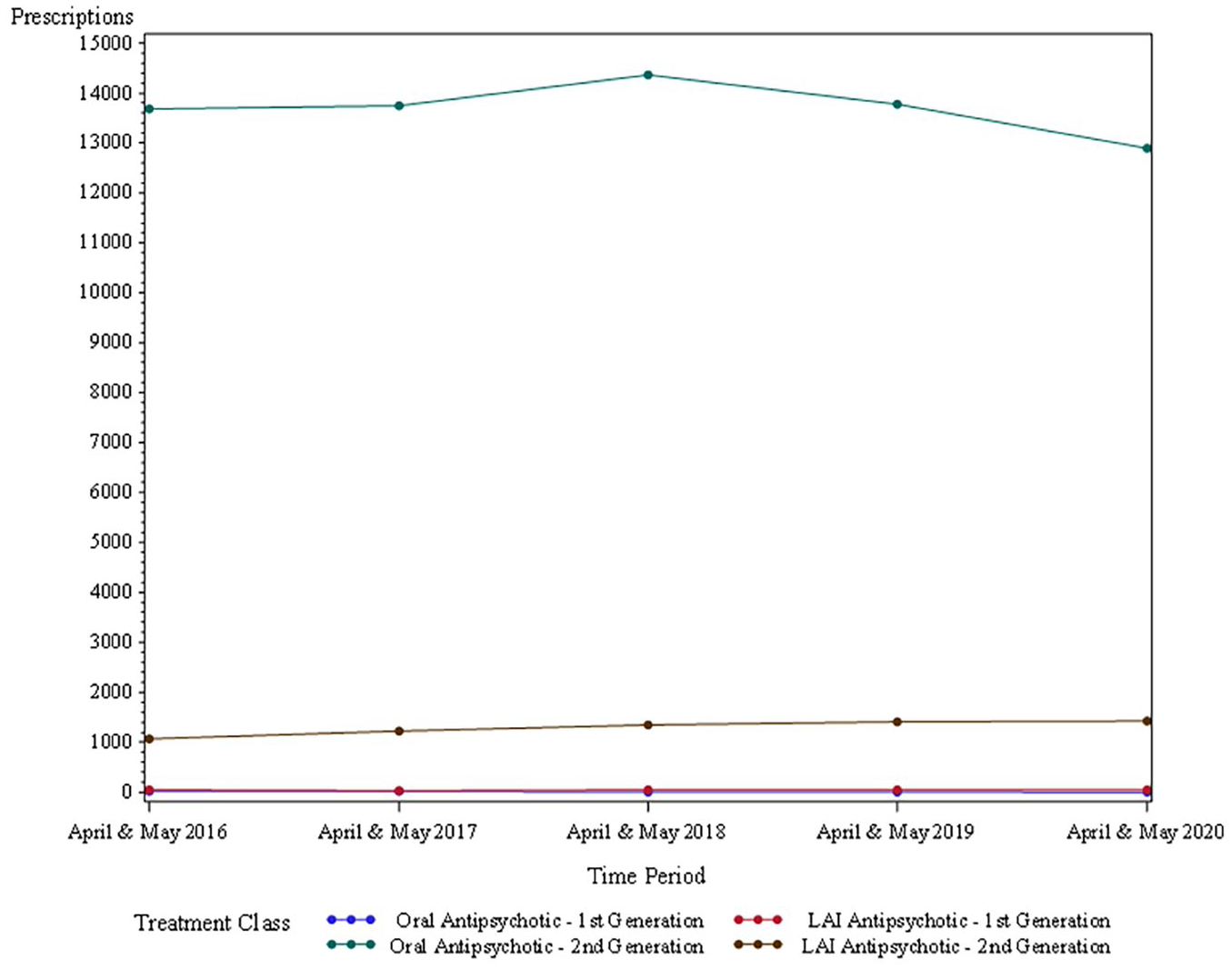
Number of antipsychotic supplies from new prescriptions by type and year.
Supply volumes from new prescriptions in April and May 2020 were not significantly different to the supplies from new prescription volumes in the same period in 2019 (p = 0.75) after adjusting for treatment class, age, gender, location and provider type (Table 2). There were similar non-significant findings for previous years (Table 2).
Adjusted comparison of antipsychotic supplies from new prescriptions by year.
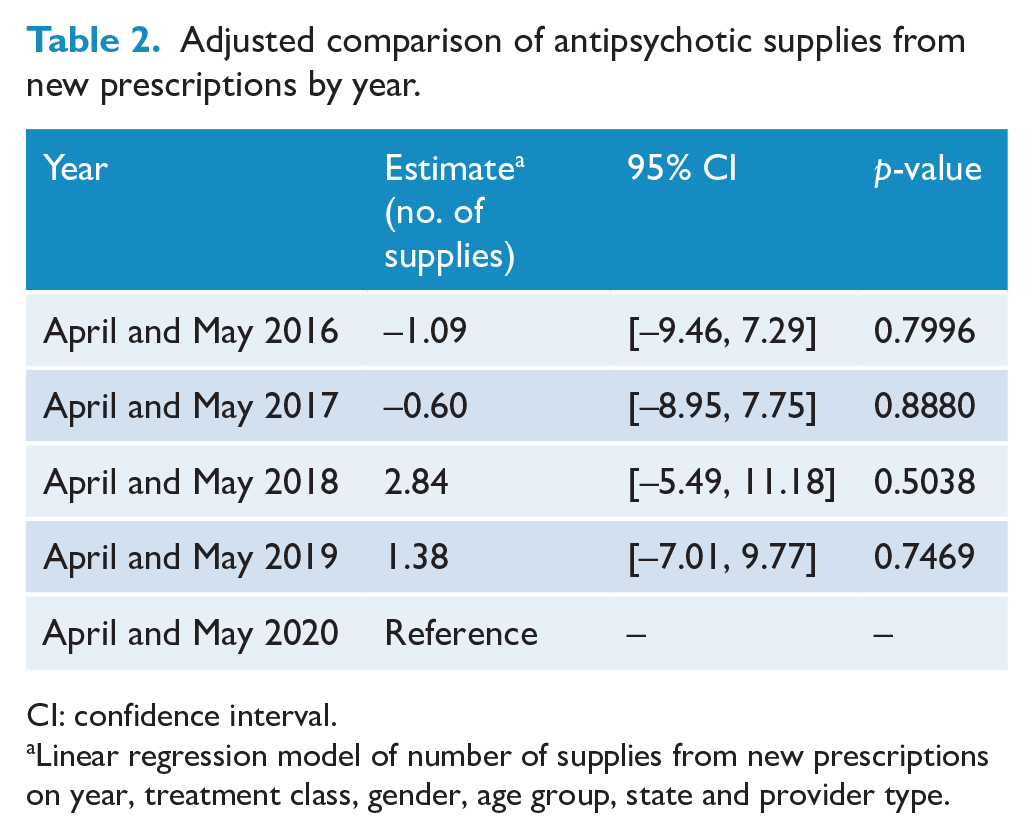
CI: confidence interval.
Linear regression model of number of supplies from new prescriptions on year, treatment class, gender, age group, state and provider type.
Secondary outcome
In terms of the secondary outcome, the volumes of all antipsychotic supplies (new and repeat prescriptions) declined by 3.5% from 42,044 in April and May 2019 to 40,582 in the same period in 2020, which was not significant (p = 0.69) after adjusting for treatment class, age, gender, location and provider type.
Discussion
There is evidence that treatment (and availability of treatment) for chronic health conditions declined during the COVID-19 pandemic, and thus we had concerns about similar reductions in care for people with severe mental illness (Richter et al., 2020; Williams et al., 2020). However, we found that after adjusting for secular trends, the COVID-19 lockdown did not lead significant reductions in antipsychotic prescriptions for patients with schizophrenia. This suggests that people with schizophrenia still had access to care providers during the COVID-19 lockdown in Australia. In April and May 2020, as with prior years, 35% of the total antipsychotic supplies dispensed were new prescriptions, indicating that many patients were able to rely on their prescription repeats to maintain continuity of their supply.
Schizophrenia is a severe condition with a profound impact on daily life, and the treatment of it was therefore likely viewed as essential by people with schizophrenia and their associated healthcare professionals in Australia.
Australia was fortunate that COVID-19 had a relatively limited impact on the supply of antipsychotics (Dong et al., 2020). The introduction of telehealth also provided an additional route to access health care, with recent studies providing evidence that telehealth improves the provision of medical services (Monaghesh and Hajizadeh, 2020), even though many patients with schizophrenia lack access to a mobile phone or the Internet (Wong et al., 2020). Taken together, telehealth services seem successful in providing care to those with access to digital communications, while reserving in-person visits for those without such access or those who prefer in-person care.
There are limitations to this study. Use of authority codes for second-generation antipsychotics or diagnostic coding by dosage level for first-generation oral antipsychotics does not eliminate the possibility that these agents were prescribed for conditions other than schizophrenia. In addition, we have no data on private non-PBS supplies, although we argue that this would be highly unlikely to occur in this population. Obtaining a supply of an oral antipsychotic does not guarantee that the medication was actually taken. Also, the data only cover the period of the initial lockdown and thus the long-term effects are unknown. In particular, we have no information on the effect of the second wave of COVID-19 infections in Victoria in mid-June 2020. The date of prescribing and thus the medical consultation may have occurred outside one of the five 2-month periods in the study. Finally, as noted above, Australia has one of the lowest levels of COVID-19 worldwide, and so our results may not be generalisable elsewhere. For instance, specialised mental health services in Italy faced severe challenges in looking after patients in both residential and outpatient facilities (De Girolamo et al., 2020).
This study has a number of strengths. To our knowledge, it is the first national large-scale retrospective cohort study examining the effect of COVID-19 on antipsychotic prescriptions covering both the public and private sector community populations. Our use of these national comprehensive longitudinal administrative health records reduces the possibility of selection bias. This is also a particularly large and representative community study of antipsychotic use in patients with schizophrenia (approximately 8000 patients per year).
Conclusion
The COVID-19 restrictions during April and May 2020 had no significant impact on the volume of antipsychotics dispensed from new prescriptions for patients with schizophrenia when compared to the volume of antipsychotics dispensed from new prescriptions during the same period in previous years.
Footnotes
Acknowledgements
The authors wish to acknowledge the following individual for their contributions to the development of this manuscript: Mona Taouk from Lundbeck Australia Pty Ltd.
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship and/or publication of this article: D.D.-K. and S.C. are employees of Covance, which received funding from Lundbeck/Otsuka to undertake the study. Lundbeck/Otsuka funded the study but had no control or study design or interpretation. S.G. and J.H. are employees of Lundbeck Australia Pty Ltd. D.L. has received hospitality and/or lecture fees and/or advisory board fees from Lundbeck, Janssen, Otsuka, Seqirus and Sevier in the last 3 years. M.T. has received hospitality and/or lecture fees from Lundbeck, Janssen and Otsuka in the last 3 years. S.K. has received a consultancy fee from Lundbeck/Otsuka.
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
