Abstract
Objective:
The argument surrounding the safety and effectiveness of interventions for the population of individuals at a clinical high risk of developing psychosis has been ongoing for the past 30 years. However, few studies have assessed the needs of this special young population, who are struggling with the recent onset of psychotic symptoms.
Method:
The sample consisted of 171 family members of 108 clinical high-risk individuals included from the ShangHai at Risk for Psychosis research programme. A ‘WeChat’ group was established to provide mutual support. There were 22,007 valid messages sent within the group between 1 April 2015 and 27 June 2016. Chat records were subsequently analysed to determine the needs of families during intervention at the early stages of psychosis.
Results:
Families of clinical high-risk individuals were highly involved in the entire medical process, and the major concerns of the families of clinical high-risk individuals focused on both functional recovery and medication. The themes of ‘take medication’, ‘go to school’ and ‘study in school’ were often discussed within the group.
Conclusion:
A family-focused intervention targeting functional recovery and real-time professional explanations of medication would meet the major needs of families of Chinese clinical high-risk individuals.
Introduction
The clinical high risk (CHR) of psychosis is characterized by sub-threshold positive symptoms and functional decline, which often precede a phase of full psychosis (Duijff et al., 2012; Li et al., 2014; Zhang et al., 2016a). While recent studies assessing outcome in CHR individuals have revealed high remission rates (four times higher than the chance of conversion to psychosis) within 1 year (Cannon et al., 2016; Fusar-Poli et al., 2012; Simon et al., 2013), these people are obviously at higher risk than those who do not meet the criteria for CHR (Fusar-Poli et al., 2012; Ziermans et al., 2011). More importantly, our previous study showed that the frequency of CHR peaks in adolescence and early adulthood (16–21 years of age) (Zhang et al., 2014), which is a crucial age for development both personally and within the family in China. There has been a surge of interest in research into early interventions for this specific population (Sommer et al., 2016; Thompson et al., 2015); however, the major concerns of this population and the types of information and treatment they require remain largely unknown.
In a previous study, we found that, when seeking help from the mental health services, Chinese CHR individuals usually visit with family members (Zhang et al., 2015, 2016b). More than 95% of CHR individuals visit clinicians with at least one family member present. In some cases, the CHR youth is accompanied by more than five family members (parents, grandparents, etc.) during the visit to the doctor. Family members play a key role in decisions regarding treatment options for CHR individuals in China, not only in terms of the type of treatment but also in terms of clinicians providing the ‘right’ treatment plan. Since family members play such an important role (Kline et al., 2013), an attempt was made during the recruitment of CHR participants to additionally ask family members to fill in a questionnaire in order to assess their needs regarding early intervention and services. However, this is not ideal from a research perspective. This is because the participants may either underestimate or overestimate the severity of problems experienced by CHR individuals. For example, family members may attribute these youths’ problems to their excessive thinking. On the other hand, they may catastrophize and fear that their children exhibit symptoms consistent with schizophrenia.
Thus, a questionnaire-based cross-sectional study may not reflect the real needs of the families of CHR individuals, as those needs change through the course of treatment. At the initial stage of professional consultation, the main concern of the family is whether or not the CHR individual has a mental disorder. During the treatment phase, their concern is focused on whether the treatment will be effective in eliminating the psychotic symptoms. During the post-treatment period, functional recovery becomes the main cause for concern. Thus, both the methods used and the information gathered about the needs of individuals and families during early psychosis were limited and inaccurate.
People appear to prefer to discuss their needs regarding psychotic issues through social media, especially in China (Li et al., 2014). Stigma-related issues hinder psychotic patients in seeking professional help; however, no such stigma is associated with the use of social media. The ‘WeChat’ application (app) was first released in China in 2011 as a cross-platform (Android, iPhone, BlackBerry, Windows Phone and Symbian phones, Web-based OS X and Windows) instant messaging service. Official statistics show that the app had 500 million monthly active users by March 2015 and 700 million by March 2016, 90% of whom were Chinese. Users of this app can send instant messages, live pictures and videos in individual or group chats. Thus, this app has become an integral part of the daily lives of Chinese people due to the widespread use of smart phones (details can be found at https://en.wikipedia.org/wiki/WeChat). Given the high usage rates of WeChat, it is important to acquire a deeper understanding of the applications of social media in the mental health service. No doubt, the possibility of anonymous online communication may help overcome the stigma attached to psychiatry. Evidence from literature (Torous and Keshavan, 2016) suggests that patients with psychosis are highly engaged in the use of social media tools. In fact, younger persons and persons from lower socio-economic status are among the highest users of social media. Therefore, the use of social media in needs assessment is likely to benefit the CHR population.
To date, there are no data on the needs of the CHR population in China. Understanding the expectations of patients and families of the CHR population is likely to help clinicians and social researchers develop targeted and effective services, strategies and policies (Thompson et al., 2015). To address this point, this study assessed the needs of the families of CHR individuals using a ‘WeChat’ group. The data from the chat records were collected for 1 year following the baseline assessment in a bid to identify the real needs of patients and their families in natural way during the early course of psychosis.
Methods
This study was performed over a period of 14 months from 1 April 2015 to 27 June 2016. This study was approved by the Research Ethics Committee of the Shanghai Mental Health Centre (SMHC) in 2015. A total of 121 CHR individuals were recruited over this period for a series of research projects (the ShangHai at Risk for Psychosis [SHARP] programme), and all family members accompanying CHR participants were informed that there was a ‘WeChat’ chat group available through which they could provide mutual support to each other (see example in Figure 1). The group allowed them to share messages, pictures and videos with other family members with similar needs to their own. There was no limit set on the number of messages shared, and they could raise any topic as they wished. The only limitation set was that they were not allowed to reveal their personal identity or contact information, or that of the CHR individual, to others. Three research staff and four psychiatrists were included in the ‘WeChat’ group in order to maintain the system and respond to any misleading information. Psychiatrists were trained to provide responses in a structured and standardized format. Responses are only given when questions are directed to them. If there is confusion in the chat, the psychiatrists were able to clarify on the WeChat. In case of an emergency, the psychiatrists were instructed to immediately contact the family member over the telephone.
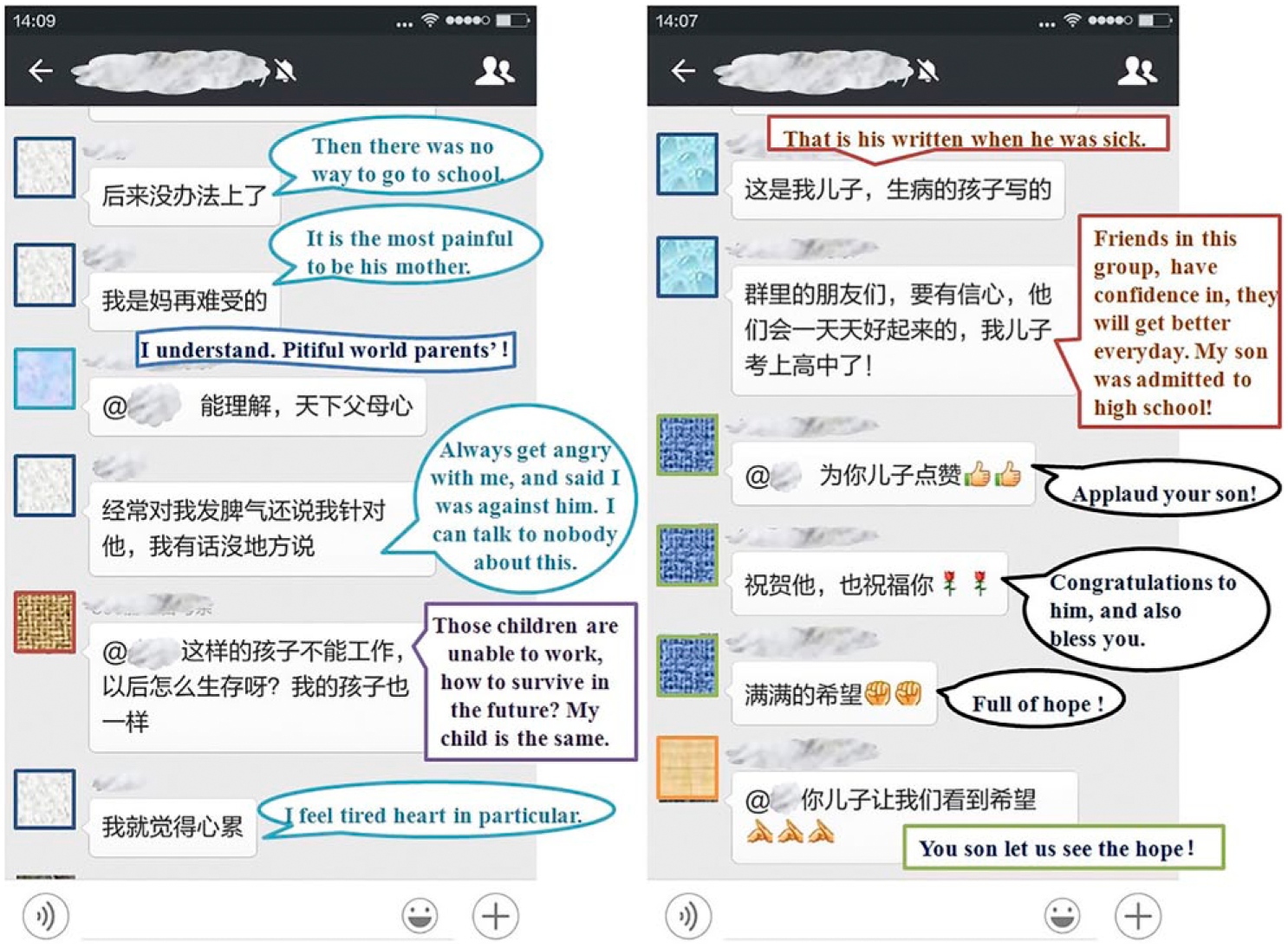
Sample chat window in ‘WeChat’.
Otherwise, no specific questions or introductions were set for the chat group. Users were encouraged to use the ‘WeChat’ group in their smart phone in the same way as any other chat group, rather than as participant in a study. Only the family members who had access to the ‘WeChat’ app on their smart phones were included in the group. Participation in this study was voluntary. In all, 33 family members were unable to join the chat group due to the lack of a smart phone or the absence of the app on their phones, and six quit the group for unknown reasons.
All CHR participants met the Criteria of Prodromal Syndromes (COPS) for the attenuated positive symptom syndrome (APSS), Brief Intermittent Psychotic Syndrome (BIPS), or Genetic Risk and Deterioration Syndrome (GRDS) according to the Structured Interview for Prodromal Syndromes (SIPS) (Miller et al., 2003). All participants were recruited during their first visit to a mental health service and were naïve to antipsychotics at baseline. Participants with a history of substance abuse, severe somatic disease, dementia or other psychoses with unrelated cognitive deficits were excluded. In the SHARP programme, CHR participants were followed up for outcomes every year for 5 years following the baseline assessment.
All messages were tabulated in a spreadsheet program (Excel 2007; Microsoft, USA) in order to graphically display the message distributions (usage) over weeks (see Figure 1). Trend lines were plotted using Excel. The messages were classified according to seven categories as follows: (1) functional recovery (school, job, etc.), (2) information from doctors and services, (3) psychotherapy, (4) medication, (5) non-psychotic symptoms (insomnia, anxiety, etc.), (6) psychotic symptoms and diagnosis (suspiciousness, etc.) and (7) complaints from family members. A pie chart is used to display the distribution of messages across these themes in Figure 4. Two experienced psychiatrists were employed to independently categorize the messages into themes. Finally, in order to explore the variety of topics in the chat group, we used ROST CM software to analyse 22,007 valid messages. Invalid words were removed, and the word frequency was calculated and is presented in Figure 4. All messages were imported into ROST CM 6 (ROST Content Mining System 6.0), which was developed by Shen et al. from Wuhan University (Shen, 2008). It is freely available for use in qualitative research and is especially useful for analysing the content of chats or microblogs. This software was used to analyse the sentences of the messages and divide them into several words automatically. Based on the results of the identified words, the frequency of words was automatically calculated and those words that appeared more than 100 times were listed in the form of a word frequency table.
Results
Demographic and clinical characteristics and familial relationships
The sample consisted of 171 family members of 108 CHR individuals. The demographics of the 108 CHR individuals were as follows: the mean age was 18.6 years (standard deviation [SD] = 5.6; range: 14–37), there were 51 males (47.2%) and 57 females (52.8%), the majority of individuals were single (4 married; 3.7%), the mean of number of years in education was 10.3 (SD = 2.7; range: 6–19), 19 individuals were born in Shanghai (17.6%), 36 were now living in Shanghai (33.3%), 79 individuals were living with their parents (73.1%) and 88 of the individuals were students (81.5%). The relationships between the CHR individuals and the family members involved in the ‘WeChat’ group are listed in Figure 2. The demographics of the 171 family members were as follows: the mean age was 40.4 years (SD = 4.9 years; range: 24–54 years), there were 68 males (39.8%) and 103 females (60.2%), and the majority of family members were parents (88.3%). All 108 CHR participants enrolled in the study were presenting to the mental health service for the first time and were antipsychotic naïve. Of these, 78 were prescribed medication by their clinician on the day of the baseline assessment (72.2%): 47 with antipsychotics, 17 with antidepressants and 14 with a combination of both types of medication.
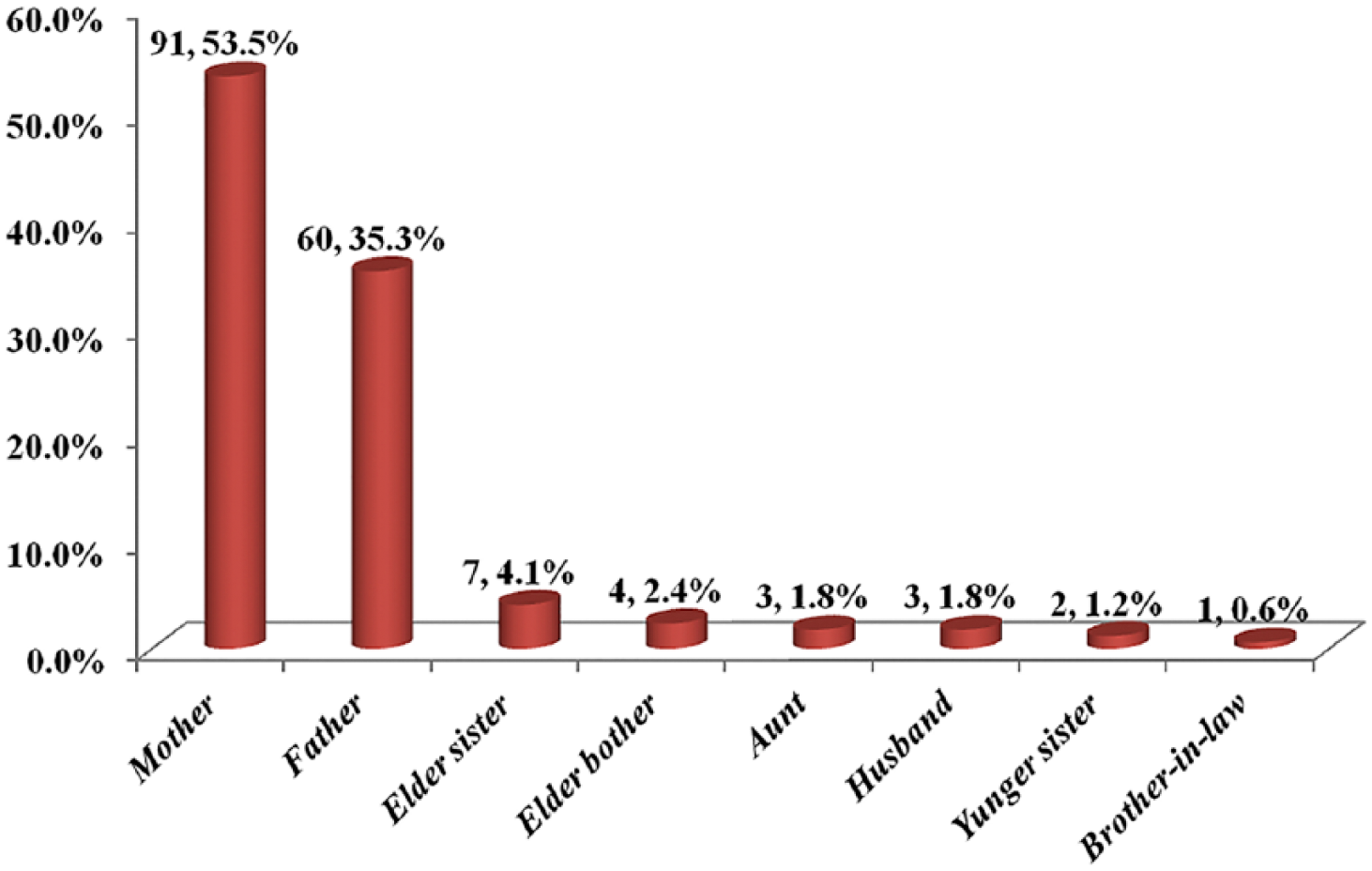
The relationship of the family members involved in the ‘WeChat’ group to the CHR participants.
Numbers of weekly active users and messages being sent
There were 22,007 messages sent in total by this group of family members during the study period. Figure 3 depicts the number of weekly active users and the number of messages that were sent in the ‘WeChat’ group from 1 April 2015 to 27 June 2016. In Figure 3(A), the Y-axis represents the number of messages and the X-axis represents the number of weeks over which the data were collected. Figure 3(B) depicts the number of active users per week, and the accumulation of users over the study period.
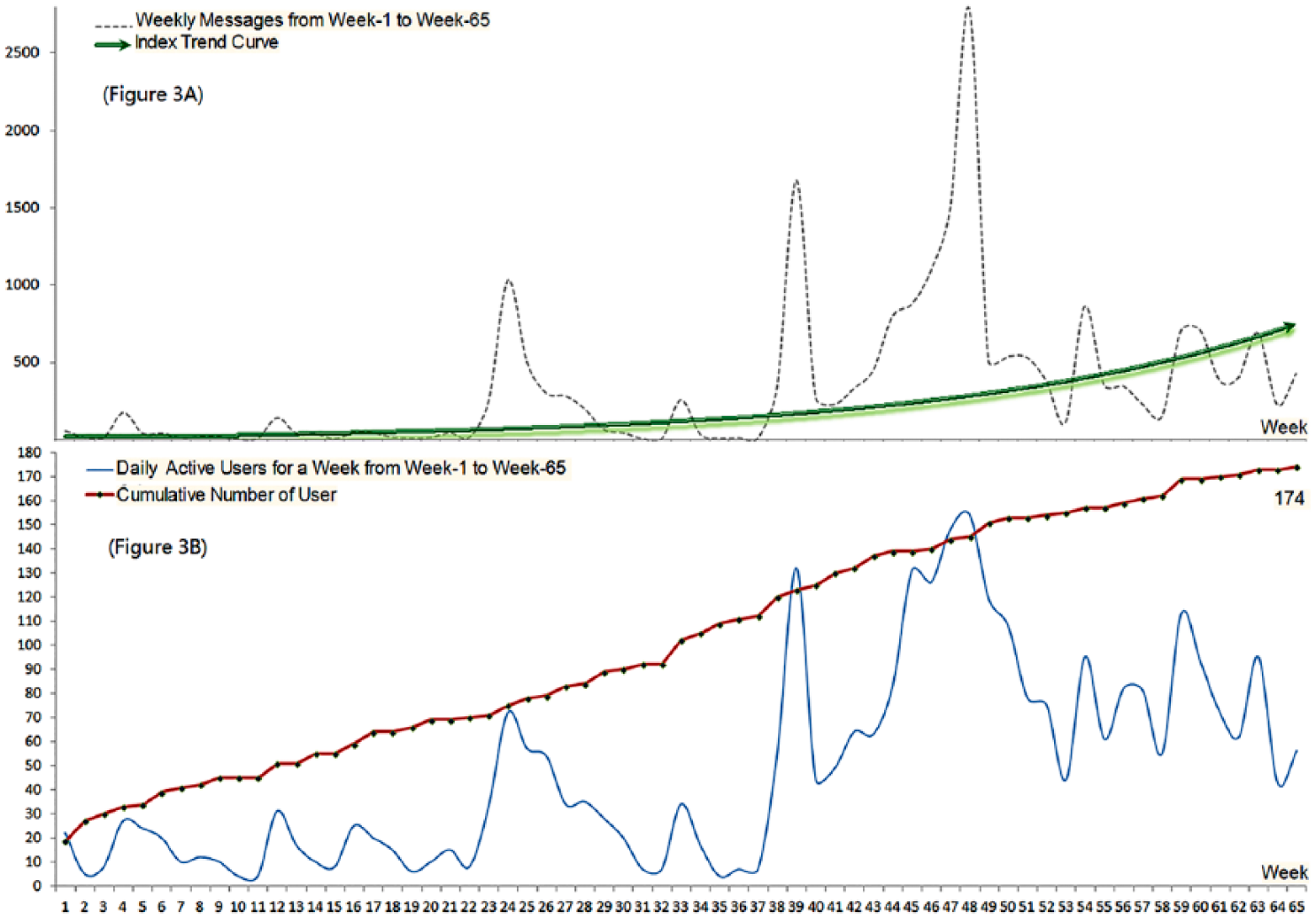
Weekly numbers of messages (A) and active users (B).
It is obvious that the ‘WeChat’ online mutual support group was used with increasing frequency over the study period, reflecting the popularity of this service. There were three peak periods in the 24th, 39th and 48th weeks, which correspond to 9–15 September 2015, 23–30 December 2016 and 24 February to 1 March 2016, respectively. Coincidentally, the 24th and 48th weeks are the first and second weeks after the new school term begins. The 39th week occurs at the end of the year, during which time many big festivals take place.
Themes that occurred in the ‘WeChat’ group
Messages were classified into seven categories, and the percentages of themes raised in the group are presented in Figure 4. The most frequent theme raised by family members was about medication, followed by the theme of functional recovery in school or work. Psychotic symptoms and information relating to doctors and treatment services were also commonly mentioned.
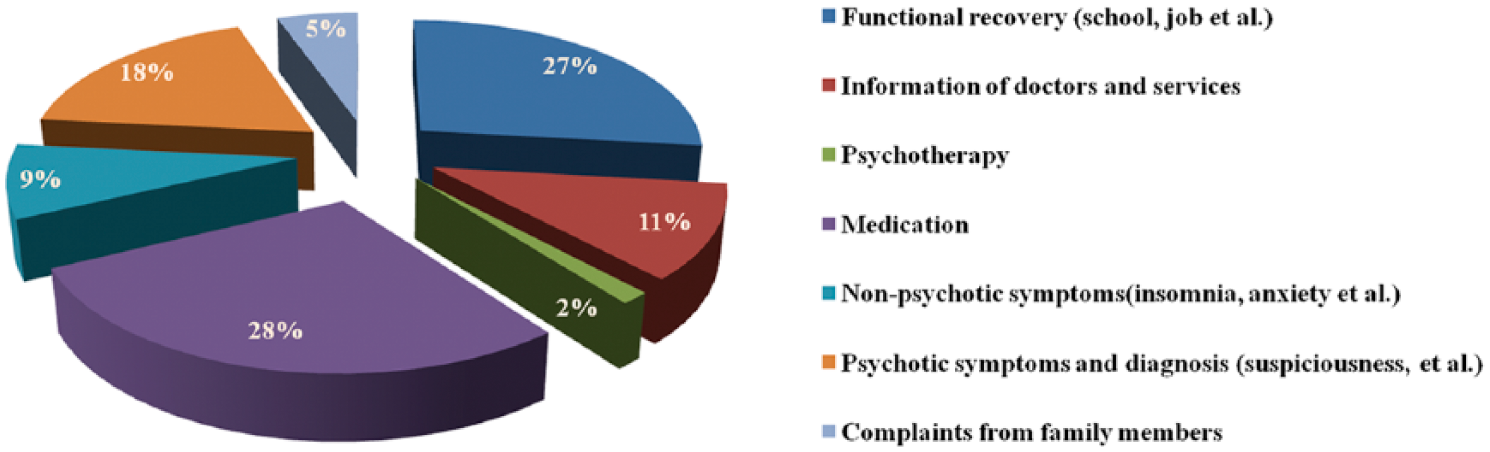
The percentages of themes raised in the ‘WeChat’ group.
Word and phrase frequency-of-use analysis
All of the messages were saved as one ‘.txt’ file and analysed using ROST CM version 6. Words and phrases that were repeated more than 100 times are listed in Figure 5. Figure 5 shows that the words ‘kid’, ‘doctor’ and ‘family’ occur most frequently. Other meaningful phrases such as ‘take medicine’, ‘go to school’ and ‘study in school’ were also frequently mentioned.
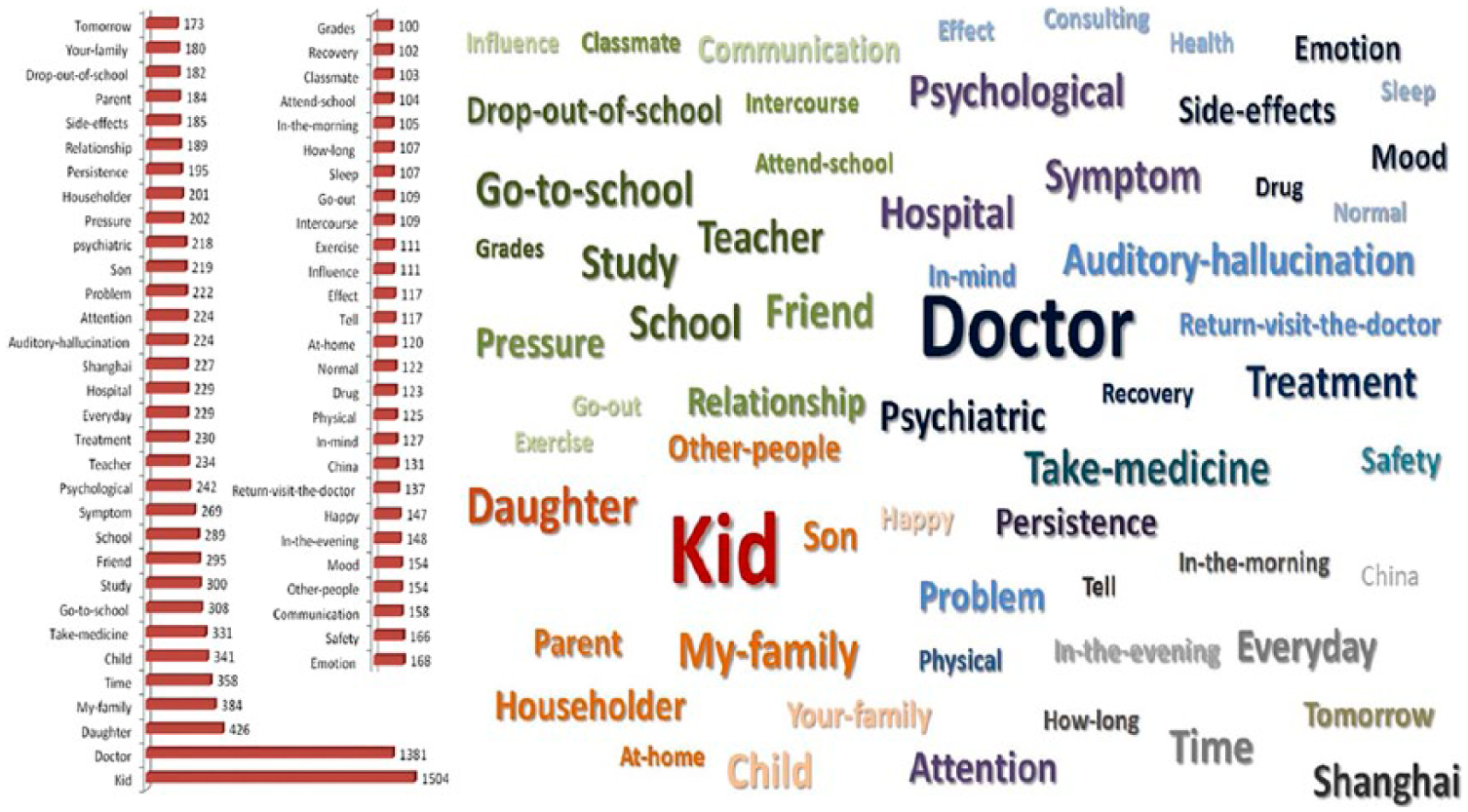
Words and phrases repeated more than 100 times in the ‘WeChat’ group.
Discussion
The results from this study suggest that concerns about family, school and medication were a centre of focus for the family members of CHR participants. To our knowledge, this is the first study to investigate the main concerns of the families of CHR patients, whose relatives were at risk of conversion to psychosis. The findings suggest that the introduction of family-based psychological interventions, school performance targeted training, medication- and symptom-related information, and counselling services might satisfy the needs of the families of CHR patients. The method applied for needs assessment in this study has obvious advantages in terms of real-world, long-term and natural expression of the concerns of these families. Knowing the needs of these families would help us to optimize and develop a better mix of strategies to meet their specific requirements. In addition, it would worth implementing an online mutual support chat group to allow the families of CHR patients to exchange useful information and to support and comfort each other. The introduction of a smart phone app has advantages as smart phones are in widespread use, therefore making such an intervention low cost and easily available.
It is not surprising that the family members are highly involved in the help-seeking behaviours of CHR youths. As the birth control policy was comprehensively carried out for more than 30 years in China, young people are often the only child in their family. The sample of 171 family members included from 108 CHR individuals has demonstrated the high involvement of Chinese families in the medical process. In a subsequent chat group, words related to the relationships within the family were frequently repeated. This suggests that the intervention strategy used for CHR youths might be more effective if the family were considered as an entity for the purposes of therapy. Conversely, a recent paper reported that the engagement of family members with the treatment of CHR youths was not favourable in a clinical research programme in the United States (O’Brien et al., 2007) since 13 out of 29 families (45%) declined participation or dropped out after one meeting, with almost half of this drop-out rate due to the caregivers being unavailable for participation. Given that the families of Chinese CHR patients are highly involved in the entire treatment process, including bringing the CHR youths to clinics, caring about their medical diagnosis and treatment and showing concern about the functional outcome of treatment, a family-based strategy for intervention is likely to be particularly welcome and acceptable in the Chinese CHR population (Wang et al., 2015).
In addition, this study found that family members often complain about their own distress and suffering due to the significant stresses imposed by the CHR youth in the ‘WeChat’ group (Li et al., 2014), at a much higher frequency than discussions about psychotherapy (Figure 4, 5% vs 2%). These negative emotions in parents themselves may also affect the treatment outcome of their children. In general, clinical staff do not typically deal with the stress experienced by family members (Kuipers, 2010). Chinese clinicians may fail to include family members in psychiatric assessment and treatment. However, many studies have shown that the ability of a caregiver to cope with psychosis can affect the recovery of the psychotic patient (Chien and Wong, 2007; Kuipers et al., 2010). More importantly, the literature suggests that a simple education and support programme may be of benefit to family members, as well as to psychotic patients (Chien and Norman, 2009; Lobban et al., 2013; Szmukler et al., 2003; Yesufu-Udechuku et al., 2015). Therefore, we believe that taking family members into account would be beneficial to treatment outcomes also (Galletly et al., 2016; Liu et al., 2015), especially for Chinese CHR patients.
Day-to-day functioning should be considered as a major target of early intervention in prodromal psychosis (Meyer et al., 2014; Schlosser et al., 2015), instead of focusing only on symptoms. Concerns about school performance and functional recovery in CHR youths are frequently raised by their family members. Our results demonstrate that the families of CHR patients care about the recovery of day-to-day functioning of CHR individuals. This concern is usually of the same or greater magnitude as concerns about symptomatic recovery. Interestingly, the distribution of messages (Figure 1) shows that there is a time-dependent effect on concerns about a CHR individual’s social and functional capacity, i.e., these concerns are increased during the early stages of a new school semester and around major holidays. This demonstrates, for example, that support targeting school performance in CHR youths should be carried out during a particular time period in order to enhance the effectiveness of the intervention. As such, a group psychotherapy session or cognitive training should be carried out prior to the start of a new semester, or a family-based intervention should be carried out during major holidays.
As this is the first time that the families of CHR patients have been exposed to antipsychotic medication, they had many misgivings and worries about it. First, in almost every case, the families asked about the side effects of the medication. For instance, the initial question was generally ‘would they become a fool after taking this medication’. Second, they were concerned about whether the patients would be taking this form of medication for their entire lives. Third, they were frightened by the drug inserts, which list schizophrenia as an indication. Moreover, the families of CHR individuals found the current medical treatment process confusing, especially in terms of the diagnosis and medication. Furthermore, they found that the diagnosis and treatment were contradictory as there are no useful clinical guidelines available for the CHR population. Our results show that there is a need for the provision of more information regarding psychiatric medication to families of CHR patients. While people can easily get important information through an Internet search, discussion with a professional about the implications of the medication being prescribed is very much needed. This might also lead to an improvement in therapeutic compliance in the Chinese CHR population.
One of the limitations of this study is that only family members, not the CHR individuals themselves, were invited to take part in the study. Also, there is a possibility that sensitive issues, that are likely to result in being stigmatized, are not discussed in this group setting. In addition, all of the participants were recruited from a single hospital, meaning that the sample might not be wholly representative. Moreover, in contrast to a questionnaire-based needs assessment, this is an open-ended and somewhat qualitative study that lacks randomization. A multi-centre study including urban and rural areas would aid in generalizing our findings. It would also be worth examining the support provided by the ‘WeChat’ group to the family members of CHR individuals through the use of structured questionnaires or interviews. Some of the strengths of this study include the fact that the needs of individuals were assessed in a natural and longitudinal manner, and the data are unique as they were collected from a real-world environment.
Our results suggest that the families of CHR individuals are highly involved in the whole medical process, and the major concerns of families were focused on both functional recovery and medication. The introduction of an app that provides mutual support is easily available, affordable and accessible may be both useful and practical for the families of CHR individuals. The widespread introduction of such an app would allow clinicians to work more effectively, and improve the communication of and awareness about the needs of CHR youths and their families. In summary, a family-focused intervention, targeting functional recovery and providing real-time professional explanations about medications, would meet some of the major needs of the families of Chinese CHR individuals. Future work should focus on the further development of this chat group application by concentrating on making the application more interactive, and improving the security features. Numerous online social networking sites have already been developed to improve mental health outcomes. This includes support groups for patients with depression (Griffiths et al., 2009; Rice et al., 2014) and suicide prevention (Robinson et al., 2015). Thus, in future, it is important to begin exploring effective, novel interventions through social media for the CHR individuals and their families.
Footnotes
Author contributions
TH.Z. conceptualized the study, wrote the first draft of manuscript and conducted the statistical analyses. LH.X., HR.C., HJ.L., LJ.J. YK.Z. and YY.W. interviewed participants and collected and organized the primary data. YY.T. and YY.X. managed the literature searches, statistical analyses and edited the manuscript. CB.L., KD.J. ZP.X. and JJ.W. designed the study and provided supervision in the implementation of the study. All authors have approved the final manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
This study was supported by National Natural Science Foundation of China (81671329, 81671332, 81361120403), Ministry of Science and Technology of China (2016YFC1306803), Shanghai Science and Technology Committee (15411967200, 14411961400), National Key Clinical Disciplines at Shanghai Mental Health Center (OMA-MH, 2011-873), Shanghai Key Laboratory of Psychotic Disorders (13dz2260500), Division of early psychosis (2013-YJTSZK-05), Shanghai Jiao Tong University Foundation (14JCRY04, YG2014MS40) and Shanghai Mental Health Center Foundation (2016-FX-01). It was also supported by SHSMU-ION Research Center for Brain Disorders (2015NKX001) and Program of Shanghai Academic Research Leader (16XD1402400).
