Abstract
Objective:
The aim of this study was to systematically review the evidence-base for the effectiveness of culturally unadapted, culturally adapted and culture-based interventions for Indigenous adults with mental or substance use disorders.
Methods:
We conducted a systematic search of scientific databases, government websites and web-based Indigenous research repositories. We sought studies using designs comparing an intervention group to a control/comparator group or pre- and post-test designs, published between 2000 and 2015 examining interventions to improve individual-level outcomes (e.g. remission, symptoms, quality of life, functioning) or service-level outcomes (e.g. number of interventions delivered) for Indigenous adults with mental or substance use disorders in Australia, Canada, New Zealand or the United States.
Results:
A total of 16 studies met inclusion criteria. Virtually all North American studies (6 US and 1 Canadian) evaluated culturally unadapted interventions, all of which were interventions for substance use. Two-thirds of Australian and New Zealand studies evaluated culturally adapted interventions and included samples with mental disorders. Of eight culturally unadapted psychological/psychosocial, pharmacological and educational intervention studies, seven reported significant improvements on at least one measure of psychological well-being, mental health problem severity, or significantly reduced alcohol or illicit drug use. Of seven culturally adapted psychological/psychosocial intervention studies, all reported significant improvement on at least one measure of symptoms of mental illness, functioning, and alcohol use. One culture-based psychological/psychosocial intervention study significantly reduced problem severity in medical and psychiatric domains.
Conclusion:
There remains inconclusive evidence regarding interventions due to a small and methodologically weak evidence-base. The literature would be enhanced by intervention replication and outcome standardisation, validating the outcome instruments used in Indigenous populations, including sample size calculations and using stronger research designs (e.g. interrupted time-series designs). Robust implementation and outcomes research is needed to further progress evidence-based practice in Indigenous mental health.
Keywords
Introduction
Indigenous people of Australia, Canada, New Zealand (NZ) and the United States experience significantly poorer health relative to their non-Indigenous counterparts, despite these countries ranking near the top of the United Nations Development Programme’s Human Development Index (King et al., 2009). Mental and substance use disorders make a major contribution to these health disparities (Michaud et al., 2006; Ministry of Health, 2013; Vos et al., 2009). Addressing the burden of mental and substance use disorders involves the delivery of evidence-based treatments (Miller et al., 2007); however, there is debate surrounding the extent to which interventions for Indigenous populations should incorporate a cultural focus (Benish et al., 2011; Dudgeon and Kelly, 2014; Kirmayer, 2012). A synthesis of the evidence-base, taking account of the extent to which interventions are culturally focused, is needed to guide the development of health services to close the mental health gap between Indigenous and non-Indigenous populations.
Mental health disparities between Indigenous and non-Indigenous populations have been quantified using disability-adjusted life years (DALYs). The DALY is a composite measure of non-fatal health loss, or years lived with disability (YLDs), and fatal health loss, or years of life lost (YLLs). One DALY is equivalent to one healthy year of life lost to a disease or injury (Murray et al., 2012). In Australia, mental and substance use disorders were the third leading contributor to disparities in total DALYs between Indigenous and non-Indigenous people in 2003, accounting for 10% of the total health gap (Vos et al., 2009). In NZ, total DALYs were almost 1.8 times higher among Māori than non-Māori in 2006, with 12% of this excess burden attributed to mental and substance use disorders (Ministry of Health, 2013). Alcohol use disorders accounted for a higher percentage of DALYs among Māori than non-Māori, compared to the total population (3.8% vs. 2.1%) and were ranked the 6th leading cause of DALYs among Māori compared to 11th in the general population (Ministry of Health, 2013). In the United States, alcohol use disorders were ranked as the leading cause of disease burden among Native Americans in 1996, accounting for 15.8% of total DALYs (Michaud et al., 2006). Unipolar depression was ranked fourth, accounting for 4% of total DALYs. Notably, substance abuse accounted for half of total YLDs in Native Americans, compared to about one-third in other race groups (Michaud et al., 2006).
Effective intervention strategies aimed at reducing this burden have yet to be fully identified and implemented. In the context of different cultural groups, such as Indigenous populations, there is debate regarding the role of culture in the delivery of health interventions (Benish et al., 2011; Dudgeon and Kelly, 2014; Kirmayer, 2012). Broadly, interventions can be organised into three groups: culturally unadapted, culturally adapted and culture-based. Culturally unadapted interventions are those that have not been systematically modified in a way that is consistent with clients’ values, contexts and worldviews (Bernal et al., 2009). A recent meta-analysis (Ünlü Ince et al., 2014) of 56 randomised controlled trials (RCTs) in ethnic minority groups found that culturally unadapted psychological interventions were superior to control conditions (care as-usual, waiting-list, placebo, or another control group) in reducing symptoms of depression. No significant moderating effects of race or ethnicity were observed. A subgroup analysis in Native Americans showed a moderately strong effect in favour of psychotherapy; however, no other Indigenous subgroup analyses were conducted (four studies of Indigenous Australians were subsumed under an ‘other’ racial-ethnic minority category).
Culturally adapted interventions are those that have been systematically modified to take into account culture and context arising from specific clients’ values, contexts and worldviews (Bernal et al., 2009). Modifications may include delivery of the intervention by Indigenous staff, use of Indigenous language, and involving the family in treatment according to cultural protocols. A 2006 meta-analysis (Griner and Smith, 2006) of 76 studies in ethnic minority groups found a moderately strong benefit for culturally adapted mental health interventions compared to alternative mental health interventions (mostly culturally unadapted emotional support groups) or no intervention. The review also found a fourfold greater effect for interventions targeted to a single cultural group, rather than to multiple cultural groups, and a twofold greater effect for interventions administered in the recipient’s native language. The review included 7 studies of Native Americans, all of which demonstrated a moderately strong effect size in favour of culturally adapted psychotherapies. More recent reviews have also offered support for culturally adapted interventions (Benish et al., 2011; Chowdhary et al., 2014; Rojas-García et al., 2015; Van Loon et al., 2013), but these did not include any additional studies in Indigenous samples.
Culture-based interventions are those focusing on cultural knowledge, that is, Indigenous ways of knowing and practices (e.g. traditional healing, ceremonies and storytelling) (Bigelow and Walker, 2011). They originate from within specific cultures and are accepted as effective by the Indigenous group because of the long history of therapeutic refinement that predates contact with non-Indigenous populations (Gone, 2013). One example is the sweat lodge ceremony, a traditional Native American treatment involving sweat therapy, songs, prayers and sometimes communication (Schiff and Pelech, 2007). The sweat lodge ceremony is increasingly being used in mental health and substance abuse treatment centres in the United States (Garrett et al., 2011). In a 2014 review (Rowan et al., 2014), 14 of 19 studies of Indigenous culture-based substance use interventions demonstrated significant increases in abstinence or reductions in drinks/drugs consumed per occasion. Samples were exclusively Native American or Indigenous Canadian; no Australian or NZ studies were located.
Gathering evidence on the effectiveness of interventions is one component of an evidence-based approach to formulating and implementing policies, plans and programmes (World Health Organization, 2004). To our knowledge, no systematic review has specifically examined the effectiveness of interventions designed to improve mental health and substance use outcomes among Indigenous people, organised according to extent of cultural focus. Moreover, previous reviews have not usually focused on individuals who meet diagnostic criteria for a mental or substance use disorder, although this group is a high priority for treatment within the context of scarce health resources. We sought to systematically review the evidence for interventions targeting Indigenous adults with mental or substance use disorders in Australia, Canada, NZ and the United States. We examine the extent and scope of studies evaluating culturally unadapted, culturally adapted and culture-based mental health and substance use interventions and summarise the evidence regarding their effectiveness.
Methods
Search strategy
The search strategy adhered to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines (Moher et al., 2009). Searches were conducted in February 2015. Articles published in scientific journals were identified by searching the bibliographic databases CINAHL, EMBASE, PsycINFO and PubMed. The main search concepts were the population of interest (e.g. Indigenous or Aboriginal peoples), diagnostic categories (e.g. mental and substance use disorders) and treatments or service evaluations (e.g. therapy, treatment or intervention) (see Appendix Part A for detailed search strategies). Retrieval was limited to articles concerning human subjects aged 18 years and over, published in English and published since 2000 (because changes in available therapies and service systems may limit the generalisability of earlier studies to the present context).
In addition, we sought relevant systematic reviews from the Campbell Database of Systematic Reviews, the Database of Promoting Health Effectiveness Reviews, the Database of Abstracts of Reviews of Effects and The Cochrane Library (see Appendix Part B). We searched Indigenous-specific online repositories, federal government websites, and selected state and province government websites to locate grey literature (see Appendix Part C). Finally, we sought additional materials by contacting experts in the field, reviewing reference lists of key articles/reports, and citation searches.
Eligibility criteria
We included designs enabling within- or between-group comparison of outcome following the delivery of the intervention – RCTs, non-RCTs, matched comparison group designs or pre–post test studies. Valid comparator/control groups included no-intervention or treatment-as-usual group, alternative interventions, matched samples receiving the same intervention, and historical control groups.
We included studies with samples comprising a majority (⩾50%) Indigenous to Australia, Canada, NZ or the United States, or in which Indigenous subgroup analyses were conducted; ⩾50% aged 18 years and over, and ⩾50% with a mental or substance use disorder. These disorders could be determined by a structured clinical interview mapping to the Diagnostic and Statistical Manual for Mental Disorders (DSM) or the International Classification of Diseases (ICD) diagnostic criteria, a qualified health professional/clinician, or scores exceeding established thresholds on validated clinician or self-report symptom severity scales, consistent with DSM or ICD diagnoses.
We included studies that quantified any of the following outcomes: remission, i.e. no longer meeting diagnostic thresholds; change in symptoms, quality of life or functional outcomes related to mental or substance use disorders; change in health-care costs or service activity (e.g. bed days, admissions, outpatient contacts, counts of interventions provided); or cost-effectiveness ratios.
In the event that multiple studies reported the same data, the more comprehensive study was included.
Data extraction
All citations identified in the systematic search were downloaded into an Endnote database. The first author (S.L.) screened titles and abstracts. Full-text records were retrieved for studies that appeared to meet the inclusion criteria or could not be excluded based on title and abstract alone. Other authors (A.B., A.F., F.C.) cross-checked 10% of all full-text articles retrieved, and there was 100% agreement with the main screening author.
The following data were extracted for each eligible study: publication information (authors, year of publication, country, service setting, funding sources, conflicts of interest); participant characteristics (Indigenous group and percentage of sample, eligibility criteria, participant diagnoses, age and gender); study characteristics (recruitment methods; study design; sample size; intervention description, control/comparison group and loss-to-follow-up) and outcomes (the effect of treatment/intervention). Two authors (S.L. and J.L.) independently extracted data and resolved discrepancies via consensus or with recourse to a third author (M.H.) as required.
Study quality assessment
Study quality was assessed using (1) the Quality Assessment of Controlled Intervention Studies tool and (2) the Quality Assessment Tool for Before–After (Pre–Post) Studies With No Control Group, both developed by the National Heart, Lung, and Blood Institute (NHLBI, 2014). The tools consist of 14 (controlled tool) or 12 (pre–post tool) items, each rated as yes, no or other (cannot determine, not reported or not applicable). A final quality rating (good, fair or poor) was assigned for each study and reasons for a rating of poor were noted. Two raters (S.L. and J.L.) independently applied the tool before coming to a consensus.
Data synthesis and analysis
The diversity of outcomes reported precluded the pooling of study findings for meta-analysis. Consequently, a narrative synthesis was undertaken.
Results
A total of 16 studies (14 articles in peer-reviewed journals and 2 doctoral theses) met inclusion criteria (see Figure 1). Four were conducted in Australia, 1 in Canada, 4 in NZ and 7 in the United States. Study designs were either pre–post (n = 10) or RCTs (n = 6). Intervention settings were diverse; most (n = 12) were conducted in formal and informal health settings (including outpatient clinical services, self-help groups, community pharmacies and residential treatment centres) or non-health settings (n = 3; universities and prisons); 1 study did not report the setting. All samples were non-probabilistic; 15 studies recruited convenience samples and 1 sampled purposively. Six studies had samples of fewer than 50 participants and 7 had more than 150 (the two largest being 1789 and 5168). Seven studies comprised exclusively Indigenous participants, 6 included a majority of Indigenous participants and 3 included a minority of Indigenous participants but conducted subgroup analyses.
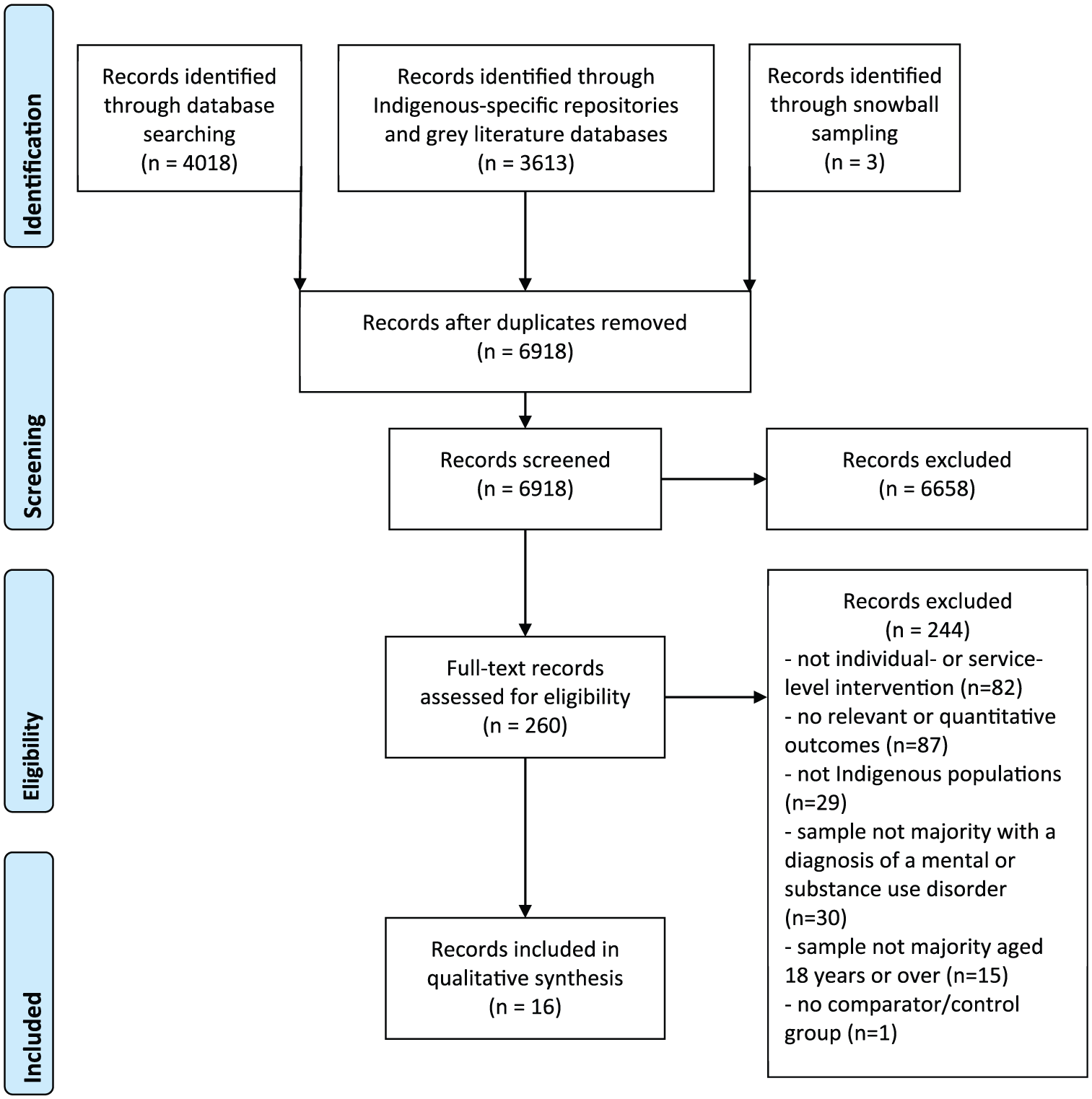
PRISMA flowchart indicating identification, screening, eligibility and inclusion of articles.
The quality assessment (see Appendices F and G) indicated that studies did not typically include power calculations, blind outcome assessors, report on intervention fidelity or use interrupted time-series designs to establish underlying secular trends potentially influencing outcomes. Small sample sizes in some studies indicated that they might be underpowered and falsely accepting null hypotheses, notably though most studies observed significant findings. Non-blinded outcome assessors can bias outcomes towards favouring the intervention (Hróbjartsson et al., 2014), but many of these studies used patient-rated outcome measures thus minimising this bias.
Eight studies reported on culturally unadapted interventions, seven on culturally adapted interventions and one on a culture-based intervention. Interventions were mostly psychological or psychosocial (n = 11); fewer were pharmacological (n = 4) or educational (n = 1). All studies quantified patient-level health or functional outcomes; no studies provided cost-effectiveness or service-level outcomes.
Studies were grouped by level of adaptation (unadapted, adapted or culture-based). We further divided each category into interventions for either mental disorders or substance use disorders. Table 1 summarises each included study. More detail on publication information, general characteristics, interventions, comparison groups, findings and study quality ratings can be found in Appendices Part F and G.
Summary of studies meeting inclusion criteria.
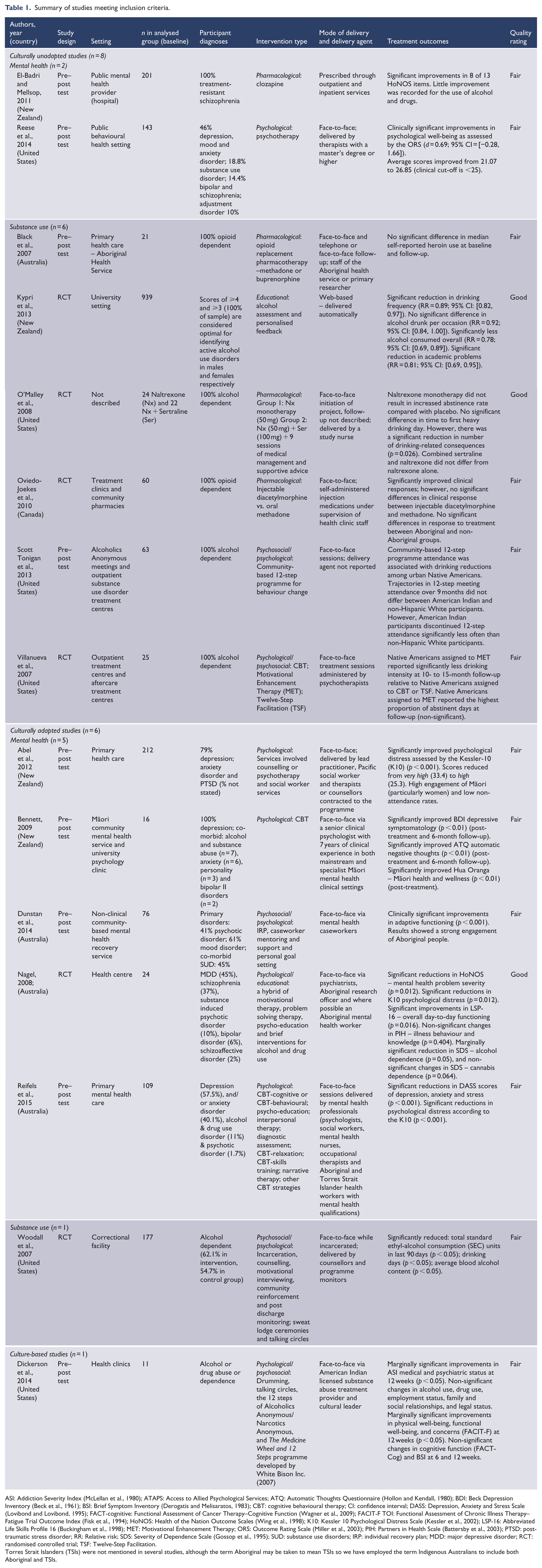
ASI: Addiction Severity Index (McLellan et al., 1980); ATAPS: Access to Allied Psychological Services; ATQ: Automatic Thoughts Questionnaire (Hollon and Kendall, 1980); BDI: Beck Depression Inventory (Beck et al., 1961); BSI: Brief Symptom Inventory (Derogatis and Melisaratos, 1983); CBT: cognitive behavioural therapy; CI: confidence interval; DASS: Depression, Anxiety and Stress Scale (Lovibond and Lovibond, 1995); FACT-cognitive: Functional Assessment of Cancer Therapy–Cognitive Function (Wagner et al., 2009); FACIT-F TOI: Functional Assessment of Chronic Illness Therapy–Fatigue Trial Outcome Index (Fisk et al., 1994); HoNOS: Health of the Nation Outcome Scales (Wing et al., 1998); K10: Kessler 10 Psychological Distress Scale (Kessler et al., 2002); LSP-16: Abbreviated Life Skills Profile 16 (Buckingham et al., 1998); MET: Motivational Enhancement Therapy; ORS: Outcome Rating Scale (Miller et al., 2003); PIH: Partners in Health Scale (Battersby et al., 2003); PTSD: post-traumatic stress disorder; RR: Relative risk; SDS: Severity of Dependence Scale (Gossop et al., 1995); SUD: substance use disorders; IRP: individual recovery plan; MDD: major depressive disorder; RCT: randomised controlled trial; TSF: Twelve-Step Facilitation.
Torres Strait Islanders (TSIs) were not mentioned in several studies, although the term Aboriginal may be taken to mean TSIs so we have employed the term Indigenous Australians to include both Aboriginal and TSIs.
Culturally unadapted interventions
Mental disorder interventions
Two of the eight culturally unadapted studies evaluated mental health interventions, both using pre–post test designs based on administrative mental health service data. A NZ study of patients with treatment-resistant schizophrenia (just over half were Māori) reported reductions on multiple dimensions of mental health problem severity at least 3 months after commencing clozapine, including overactive, aggressive, disruptive or agitated behaviour; non-accidental self-injury; cognitive problems; problems associated with hallucinations and delusions; depressed mood; problems with relationships; problems with living conditions and problems with occupation and activities (El-Badri and Mellsop, 2011). A study among Native Americans (Reese et al., 2014) reported a close-to-large positive effect (d = 0.69) for psychotherapy (therapeutic content not further described; involving a median of five sessions) on a composite measure of psychological well-being. Mean scores moved from the clinical to non-clinical range.
Substance use disorder interventions
Six studies evaluated culturally unadapted interventions designed to treat substance use disorders, of which four evaluated different treatments for alcohol use or dependence (Kypri et al., 2013; O’Malley et al., 2008; Tonigan et al., 2013; Villanueva et al., 2007). A single-session, web-based educational screening and brief intervention (SBI) (Kypri et al., 2013) was superior to screening alone in reducing drinking frequency and volume, heavy or binge drinking, and academic problems at 5-month follow-up among a community sample of Māori students. Naltrexone was found to be superior to placebo in reducing drinking consequences but not measures of drinking frequency or volume, alcohol urges, or depression at 16-week follow-up in Alaskan Natives (O’Malley et al., 2008). A slightly better response was observed in the full intention-to-treat analysis including Natives (n = 68) and non-Natives (n = 33), which also observed significant differences between the naltrexone and placebo groups in total abstinence and percentage of days abstinent. The differences were attributed to lower power in the Alaskan Native subgroup analysis and a better response to placebo among this subgroup. An evaluation of Alcoholics Anonymous (AA) (Tonigan et al., 2013) significantly reduced drinks per drinking day (DPDD) at 9-month follow-up. The change in percentage of days abstinent from alcohol was equivalent (both from 0% to 39%) between Native Americans and non-Hispanic Whites at 9-month follow-up. An evaluation of motivational enhancement therapy (MET) (Villanueva et al., 2007) showed reduced DPDD at 10- to 15-month follow-up (but not at 4- to 9-month follow-up). There were no significant reductions in the proportion of days abstinent at either follow-up.
Two studies addressed opioid dependence with pharmacological interventions. A pre–post test design evaluating methadone and buprenorphine (Black et al., 2007) found no significant reductions in self-reported heroin use. An RCT testing diacetylmorphine (Oviedo-Joekes et al., 2010) produced a reduction in illicit drug use in 68.8% of the sample, although this was not significantly different to the response to methadone maintenance therapy (53.4%). It was also not significantly different to the response of non-Aboriginal participants to injectable diacetylmorphine (66.7%) and methadone (43.9%) (Oviedo-Joekes et al., 2010). The different findings can plausibly be explained by selection bias; 86% of patients recruited to the methadone and buprenorphine study had been on opioid replacement pharmacotherapy for a mean duration of 1 year when initially interviewed, so baseline levels of opioid use were very low (zero median days per month).
Culturally adapted treatments
Mental disorder interventions
Five of seven culturally adapted treatments evaluated psychological or psychosocial interventions designed to treat mental disorders. The nature of psychological intervention varied, and included cognitive behavioural therapy (CBT) (Bennett, 2009), a range of intervention options, primarily CBT (Reifels et al., 2015), psychotherapy not further defined (Abel et al., 2012), and multiple component interventions (Dunstan et al., 2014; Nagel, 2008). Adaptations to these interventions included employing Indigenous staff and including culturally specific elements in the recovery plan (Dunstan et al., 2014), ensuring practitioners received cultural competency training (Reifels et al., 2015), incorporating Māori worldviews (Abel et al., 2012) and interpersonal customs (Bennett, 2009) into the treatment process and incorporating Indigenous perspectives of mental illness into treatment (Nagel, 2008).
Studies evaluating CBT or psychotherapy (Abel et al., 2012; Bennett, 2009; Reifels et al., 2015) variedly showed significant pre–post improvements in symptoms of depression, anxiety and stress, and psychological distress. One study observed larger symptom reductions in non-Indigenous service users than Indigenous service users (Reifels et al., 2015). A study involving a multi-component psychosocial intervention (individual recovery plan, goal setting and caseworker mentoring and support) (Dunstan et al., 2014) found significant pre–post improvements in functioning in the domains of work, independent living, immediate and extended social networks. An RCT of motivational care planning (a hybrid of motivational therapy, problem solving therapy, psycho-education and brief interventions for alcohol and drug use) (Nagel, 2008) showed improvements in the severity of mental health problems, psychological distress and daily functioning (withdrawal, antisocial behaviour, self-care and compliance with medication and health professionals), compared to treatment as usual in a mental health centre. Large effect sizes were reported in some studies with significant results (Bennett, 2009; Nagel, 2008) and changes in scores on most inventories were also clinically meaningful. Despite this, some scores on symptom inventories still remained high or moderate at the conclusion of treatment (Abel et al., 2012; Reifels et al., 2015).
Substance use disorder interventions
One culturally adapted RCT (Woodall et al., 2007) compared 28 days of incarceration plus a multi-component psychological/psychosocial intervention to incarceration only among a predominantly Native American sample. The psychological intervention included individual counselling, motivational interviewing and post-discharge monitoring for 3–12 months (combined with the traditional Native American treatments of sweat lodge ceremonies and talking circles), and produced significantly greater reductions in 90-day alcohol consumption, drinking days and average blood alcohol content in the intervention group relative to the control group. A pre–post test of an intervention combining motivational interviewing and community reinforcement (Venner et al., 2016) observed significant reductions in percentage of days abstinent from alcohol, problem severity in the legal domain of the Addiction Severity Index, scores on the Brief Symptom Inventory and hopelessness. A significant increase in alcohol and drug use self-efficacy was also observed.
Culture-based interventions
One study tested a culture-based intervention for Native Americans with alcohol or drug dependence or abuse. Dickerson et al. (2014) assessed a 12-week, multi-component intervention including drumming, talking circles, the 12 steps of AA/Narcotics Anonymous, and The Medicine Wheel and 12 Steps (a culturally appropriate 12-step recovery programme) (White Bison Inc., 2007) using a pre–post test design. We classified this study as a culture-based treatment because drumming (a traditional practice among Native Americans) was the primary component of treatment. There were significant reductions in psychiatric severity, medical problem severity and measures of physical and functional well-being at the conclusion of treatment. Physical well-being, functional well-being and additional concerns improved significantly at 12 weeks. However, the study sample was very small (n = 10 at baseline), with 50% lost to follow-up at post-treatment assessment. Reasons for loss to follow-up were not reported.
Discussion
The aim of this study was to assess the evidence-base for interventions for mental and substance use disorders among Indigenous adults, according to extent of cultural focus. We identified only 16 studies meeting our criteria. There were regional variations in the focus of interventions being studied. Virtually all North American studies (6 Canadian and 1 from United States) evaluated culturally unadapted interventions, all of which were interventions for substance use. Two-thirds of Australian and NZ studies evaluated culturally adapted interventions and included samples with mental disorders.
Of eight culturally unadapted psychological/psychosocial, pharmacological and educational intervention studies, seven reported significant improvements on at least one measure of psychological well-being or mental health problem severity, or alcohol or illicit drug use. Of six culturally adapted psychological/psychosocial intervention studies, all reported significant improvement on at least one measure assessing symptoms of mental illness, functioning, or alcohol use. One culture-based psychological/psychosocial intervention study showed significantly reduced problem severity in medical and psychiatric domains.
Limitations
Our search strategy was extensive and included multiple publication types (academic or grey literature) obtained from a broad range of sources. We further strengthened the review by rating study quality using published tools. However, there were some limitations.
Articles published in French (Canada) or Indigenous languages (in all countries) may have been omitted – although this is unlikely because English is the dominant language spoken in nearly all jurisdictions in the four countries containing significant numbers of Indigenous people. Our review focused on adults only so we cannot comment on interventions in childhood or adolescence.
Some interventions were described in limited detail. In some cases, this may have been due to the use of secondary data obtained from administrative datasets that were not established for the purpose of evaluating therapy-specific outcomes. For example, Reese et al. (2014) undertook secondary analyses of archival, routinely collected service data from a public behavioural health setting in the United States. In this study, the treatment delivered was described as ‘psychotherapy’, but no further specifications were provided. Abel et al. (2012) did not specify whether their intervention was delivered on an individual basis only or whether group programmes were also provided. Other interventions, although not clearly described in the journal articles, were based on well-documented treatment models (e.g. AA in Tonigan et al., 2013, MET in Villanueva et al., 2007); however, fidelity to the parent treatment model was not reported. Limited description of some interventions may have obscured cultural adaptations and thus may have resulted in misclassification of culturally adapted interventions into the culturally unadapted category. Because patient–provider alliances and communication positively affect medication-taking behaviour among psychiatric samples (Thompson and McCabe, 2012) and interpersonal factors are important for Indigenous people (Glover et al., 2015), we recommend that degree of cultural adaptation is still described in pharmacological interventions to ascertain whether it influences adherence and consequent outcomes. Deficits in the quality of reporting of psychological interventions are common and not unique to studies of interventions among indigenous populations. However, given the limited number of studies meeting inclusion in this review, it is important that studies among indigenous people are appropriately described. This situation could potentially be improved by the implementation of intervention reporting standards or guidelines (Grant et al., 2013; Mayo-Wilson et al., 2013).
A number of studies identified by the systematic search were ineligible for inclusion in the review solely because the diagnostic status of study participants was not reported. Our inclusion criteria required a majority of the sample to have a mental or substance use disorder diagnosis; therefore, we may have excluded some studies that would have met criteria if diagnostic information had been ascertained or reported. We did attempt to contact these authors for this information; where responses were received, the authors were not able to confirm the diagnostic status of participants. Information about diagnosis and symptom severity should be collected, via standardised measures used wherever possible, and reported in all studies.
Overall, intervention heterogeneity and use of co-interventions limit conclusions about the effectiveness of any one intervention. Outcome heterogeneity hinders comparisons between intervention findings. The literature would therefore benefit from replication of interventions and standardisation of outcome instruments. With regard to the use of co-interventions, ideally, studies with co-interventions would be restricted. However, this is often not feasible in health service settings because multiple practitioners may be involved in the delivery of care and multiple interventions may therefore be delivered. Thus, it is more appropriate in these circumstances that co-interventions are documented, included in datasets and subsequently tested as a predictor of treatment outcome. Of the six studies that used co-interventions (Abel et al., 2012; Black et al., 2007; Dunstan et al., 2014; Nagel, 2008; Reifels et al., 2015; Woodall et al., 2007), none tested the use of individual co-interventions as a predictor of treatment outcome.
The validity and reliability of measures in Indigenous populations was generally not discussed in the included studies, and no evidence of validity or reliability could be identified. In some studies (e.g. Nagel, 2008), tools adapted for use with Indigenous populations were utilised. Further research clarifying the psychometric properties of these scales in Indigenous populations is necessary to ensure they are sound measures to use. Our concerns about the validity of measures among Indigenous populations are shared by others (Black et al., 2015; Jorm et al., 2012; Reifels et al., 2015).
Sample size calculations were only provided in one-third of included studies. For some of the smaller samples (i.e. <30) with non-significant findings (Dickerson et al., 2014; Villanueva et al., 2007), this raises questions about whether they were large enough to detect important differences. Future studies would be strengthened by including a priori sample size calculations for the primary outcome measure.
Pre—post-test designs were used in nine studies, many of which made use of repeated follow-ups of participants. This study design could be strengthened by the use of an interrupted time-series design incorporating multiple baseline measurements to establish any underlying secular trends.
The overall study drop-out rate was very low in a number of RCTs; however, several used an intention-to-treat analysis to account for missing data. The Naltrexone RCT by O’Malley et al. (2008) assumed that individuals lost to follow-up had failed to be abstinent on the day following their last recorded data point, thus making the findings conservative. Only one study measured adherence to the intervention protocol, which was not classified as high, while others did not report adherence or adherence could not be determined from the available information. Blinding of outcome assessors and participants occurred infrequently. This may have resulted in bias favouring the treatment (see Hróbjartsson et al., 2013).
Directions for future research
To increase the evidence-base for interventions in Indigenous populations, a substantial increase in both quantity and quality of research is needed. Increased research providing empirical support for interventions would assist in securing funding for these interventions and advocating for them to be integrated into treatment programmes for Indigenous people (Bigelow and Walker, 2011). In Australia in particular, more evaluation of narrative therapy is necessary, given that it is funded for Indigenous clients only under Australia’s Access to Allied Psychological Services scheme. Process evaluation of aspects such as intervention feasibility, fidelity and acceptability would greatly enhance research findings beyond the basic treatment outcome measures that are typically reported in existing research.
Culturally unadapted interventions improved mental health and substance use outcomes; however, replications in different Indigenous populations and subgroup analyses are needed to confirm whether they can be effective interventions for Indigenous people. This is, for example, particularly important to know in the context of delivering psychotherapy to Native Americans, because there is evidence both opposing (Ünlü Ince et al., 2014) and supporting (Griner and Smith, 2006) the use of culturally adapted interventions.
Unadapted interventions, particularly those that are pharmacological or educational, may not need to be modified to produce beneficial outcomes, particularly if attitudes towards these interventions are favourable and result in good retention rates and treatment adherence. However, retention rates were mixed across studies and future research is needed to clarify why Indigenous people drop out of treatment and whether retention and adherence could be improved by cultural adaptations (e.g. use of Indigenous staff, incorporating Indigenous perspectives of health).
Among the interventions we categorised as culturally adapted, the role that adaptation plays in producing the observed outcomes was not studied. Thus, it is difficult to draw conclusions regarding whether and to what degree cultural adaptations improve outcomes. The two culturally adapted RCTs that compared interventions to treatment as usual (Nagel, 2008; Woodall et al., 2007) did not focus solely on the role of the adaptation in outcome. Instead, the intervention arms were complex and integrated several different forms of treatment, while the control arms were not the same treatment without the adaptation. Because previous reviews have found that culturally adapted interventions are more effective that unadapted interventions for racial-ethnic minority groups (Benish et al., 2011; Griner and Smith, 2006), there is a need for researchers to directly compare culturally unadapted and culturally adapted interventions using standardised outcomes measures.
Despite the high rates of co-morbid mental and substance use disorders among Indigenous populations (Vos et al., 2009), no interventions integrating treatment for participants with both mental and substance use disorders were found in our review. One study (Nagel, 2008) did have distinct strategies to reduce substance use and improve mental health among people with mental disorders. One study on opioid dependence (Black et al., 2007) was conducted in a health setting that also offered mental health services. To optimise interventions to achieve desired outcomes, theoretical models including mediators and moderators of treatment are needed to understand what works, for whom and why. Kypri et al. (2013) found, for instance, that the effects of their educational SBI did not vary by age, gender or drinking level. Dunstan et al. (2014) hypothesised that having Aboriginal staff increased service engagement and consequently improved health outcomes among Indigenous Australians. Another potential moderator of treatment effectiveness is session attendance; Reifels et al. noted a doubling in the rate of unattended sessions for Indigenous compared to non-Indigenous clients in the Access to Allied Psychological Services programme in Australia (Reifels et al., 2015). Tonigan et al. (2013) conjectured but did not test their hypothesis that acculturation among Native Americans would increase the effectiveness of AA because it would be seen as a more appropriate treatment. Villanueva et al. (2007) hypothesised a priori that MET would be more effective because it is consistent with American Indian interpersonal approaches to intervention, but surprisingly, while not testing specifically as moderators or mediators of treatment, they found that there were no between-treatment (MET vs. CBT vs. Twelve-Step Facilitation) differences in therapeutic alliance, therapy sessions attended or overall satisfaction with treatment. No assessment of between- or within-group diversity present in Indigenous people (e.g. specific tribal groups) means the interventions may be more or less effective for different Indigenous subgroups. Increased clarity about what works for whom would be gained by asking about the specific Indigenous subgroup/tribal group under study to allow this variable to be tested as a moderator of the impact of treatment.
Future collaborations between communities, clinicians and researchers could create a more robust evidence-base for interventions for mental and substance use disorders in Indigenous populations. Collecting and analysing service use data from routine practice would be simple and cost-effective method to achieve this objective. This would provide researchers with data that could establish or confirm the effectiveness of currently used treatments for mental and substance use disorders. The importance of collecting more consumer outcome data has also been raised by other authors in this area (Reifels et al., 2015). However, consumer data need to be supplemented with rigorous outcome and implementation research to further promote evidence-based practice in Indigenous mental health and make a discernible difference to Indigenous health outcomes and the well-being of Indigenous communities.
Conclusion
A small body of literature provides support for several different types of culturally unadapted and culturally adapted interventions in improving outcomes for Indigenous people with mental and substance use disorders. However, due to scarcity of studies and the heterogeneity of interventions evaluated, outcomes assessed and populations studied, it is difficult to draw conclusions regarding any one intervention. The findings from this study provide some directions for clinicians and service planners in determining what interventions may be effective for the populations with whom they work. However, robust implementation and outcomes research will be needed to further progress evidence-based practice in Indigenous mental health and improve the well-being of Indigenous people and their communities.
Footnotes
Acknowledgements
The authors wish to thank Grace Borchert for her assistance with conducting the grey literature review and Damian Santomauro for his assistance with screening titles and abstracts. We thank the following people for their assistance in locating relevant studies for inclusion in this review: Dr Jenny Chong (The University of Arizona), Dr Colleen Dell (University of Saskatchewan), Dr Daniel Dickerson (University of California, Los Angeles [UCLA]), Dr Elizabeth Evans (UCLA), Dr Melissa Haswell-Elkins (University of New South Wales), Dr Len Kelly (McMaster University), Dr Kypros Kypri (The University of Newcastle) and Dr Rick Rawson (UCLA). We would also like to thank Ernest Hunter for his comment and feedback. We also thank the two anonymous reviewers of this manuscript for their comments.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The authors wish to acknowledge Queensland Health for funding this study.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
