Abstract
Objective:
To (1) estimate the lifetime and 12-month prevalence of suicidal behaviours in Australian young people aged 12–17 years, (2) describe their co-morbidity with mental illness and (3) describe the co-variation of these estimates with social and demographic variables.
Method:
A national random sample of children aged 4–17 years was recruited in 2013–2014. The response rate to the survey was 55% with 6310 parents and carers of eligible households participating. In addition, of the 2967 young people aged 11–17 years in these households, 89% (2653) of the 12- to 17-year-olds completed a self-report questionnaire that included questions about suicidal behaviour.
Results:
In any 12-month period, about 2.4% or 41,400 young people would have made a suicide attempt. About 7.5% of 12- to 17-year-olds report having suicidal ideation, 5.2% making a plan and less than 1% (0.6%) receiving medical treatment for an attempt. The presence of a mental disorder shows the largest significant association with lifetime and 12-month suicidal behaviour, along with age, gender, sole parent family status and poor family functioning. Of young people with a major depressive disorder, 19.7% reported making a suicide attempt within the previous 12 months. There are also significant elevations in the proportions of young people reporting suicidal behaviour who have anxiety and conduct disorders.
Conclusion:
Mental disorders should be a leading intervention point for suicide prevention both in the primary health sector and in the mental health sector specifically. The associations examined here also suggest that efforts to assist sole parent and/or dysfunctional families would be worthy areas in which to target these efforts.
Introduction
Suicidal behaviours are taken sine qua non as indicators of psychological distress by lay and professional people alike (Zubrick and Kovess-Masfety, 2005). The relationship between suicide and psychiatric disorder has been demonstrated time and again, and suicide rates are commonly used or recommended as an indicator of cause-specific mortality and morbidity linked to psychological state and psychiatric illness (De Leo et al., 2010). Globally, in the past two decades, the suicide rate per 100,000 in boys aged 10–14 years in 81 countries has shown a minor decline (from 1.61 to 1.52), whereas in girls it has shown a slight increase (from 0.85 to 0.94). Although the average rate has not changed significantly, rates have decreased in Europe and increased in South America (Kõlves and De Leo, 2014).
Cross-national comparison of the prevalence of suicidal behaviours among populations of young people is difficult owing to variations in age aggregations, definitions and measures of these behaviours. A mix of lifetime and 12-month prevalence is reported, further complicating ease of comparison. Broadly though, US epidemiological findings for 14- to 18-year-old school age young people indicate a 12-month prevalence of 17.0% for suicidal ideation, 13.6% for suicidal plans, 8% for attempting suicide and with 2.7% reporting a need for treatment following the attempt (Centers for Disease Control and Prevention, 2014). In New Zealand, among 13- to 17-year-olds, the 12-month prevalence of suicidal ideation ranged from 13.0% to 17.9%, suicidal plans from 6.0% to 11.6% and attempts from 3.8% to 5.7% (reported mean 4.5%), with a prevalence range of 0.7–1.4% for those attempts which resulted in the need for treatment (Clark et al., 2013). In Great Britain, among those young people aged 16–24 years, the 12-month prevalence was 6.7% for suicidal ideation and 1.1% for suicidal attempts (Meltzer et al., 2002).
Australian national estimates of suicidal behaviour are available for populations of adults and young people. For young people aged 13–17 years, available national estimates of the 12-month prevalence of suicidal behaviour were last gathered in 1998 and reported in 2000. They showed that 12.0% of this age group had suicidal ideation, 8.9% had made a plan, 4.2% had made an attempt and 0.9% had made an attempt receiving treatment (Sawyer et al., 2000). Results for older Australians gathered in 2007 found a 12-month prevalence of suicidal ideation for adults aged 16–85 years of 2.3%, 0.6% for making a suicide plan and 0.4% for making an attempt (Johnston et al., 2009). This report also stratified the 12-month prevalence rates for young people aged 16–24 years, reporting rates of 3.4%, 1.0% and 1.1% for ideation, planning and attempting, respectively, in the previous 12 months in this younger age group. It is within this broad epidemiological context that we report recent national estimates of lifetime and 12-month suicidal behaviour collected on Australian young people aged 12–17 years in the 2013–2014 second Australian Child and Adolescent Survey of Mental Health and Wellbeing (i.e. Young Minds Matter – YMM). Our aims are to (1) estimate the lifetime and 12-month prevalence of suicidal behaviours in Australian young people aged 12–17 years, (2) describe their co-morbidity with mental illness and (3) describe the co-variation of these estimates with key social and demographic variables. These descriptions add to the extant literature by providing contemporary, community-based Australian population estimates of lifetime and 12-month prevalence of suicidal behaviours for young people.
Methods
The design, sampling and survey interview methods are described extensively elsewhere (Hafekost et al., submitted; Lawrence et al., 2015). Briefly, the survey employed area-based random sampling with voluntary recruitment and consent of households in scope where there was at least one child aged 4–17 years. Where there was more than one eligible child in the household, one was randomly selected for inclusion. The overall response rate to the survey was 55% with 6310 parents and carers of eligible households participating in the survey. In addition, 2655 (89.2%) of a possible 2976, 12- to 17-year-olds completed the youth questionnaire which contained questions about suicidal behaviour.
We examined the sample for its representativeness. Comparison with 2011 Census data showed that the YMM sample was broadly representative of the Australian population in terms of major demographic characteristics (Hafekost et al., submitted). The sample was found to include a higher proportion of children aged 4–7 years than would be expected based on random sampling with 34.2% of the main sample aged 4–7 years, compared to 29.4% in the 2011 Census. There was also a lower proportion of families with only one eligible child, with 37.9% of all participating families having one child compared with 45.8% of those in the 2011 Census. However, in all other regards, no differences were noted with respect to area-level socio-economic indicators (i.e. Socio-Economic Indexes for Areas [SEIFA]), population distribution, age, sex and country of birth of the total population of 4- to 17-year-olds in Australia and demographic characteristics including household income, family type, household tenure, parent/carer education and labour force status of families with children aged 4–17 years. We concluded that the achieved sample was broadly representative of the Australian population.
Survey data have been weighted to represent the full Australian population of 4- to 17-year-olds and to adjust for patterns in non-response as described above. Additionally 16- to 17-year-olds were specifically oversampled. The weighting accounts for these factors. Survey estimates and associated confidence intervals (CIs) have been calculated using the method of Taylor Series Linearisation (Wolter, 2007). The association between self-harm and mental disorders was examined using logistic regression, using the SAS SURVEYLOGISTIC procedure to account for the clustered nature of the sample design and the use of survey weights. All analyses were conducted using SAS software (SAS Institute Inc., 2014).
Ethics approval
The survey obtained the approval of the Australian Government Department of Health Human Research Ethics Committee and the University of Western Australia Human Research Ethics Committee for the conduct of the survey.
Measures
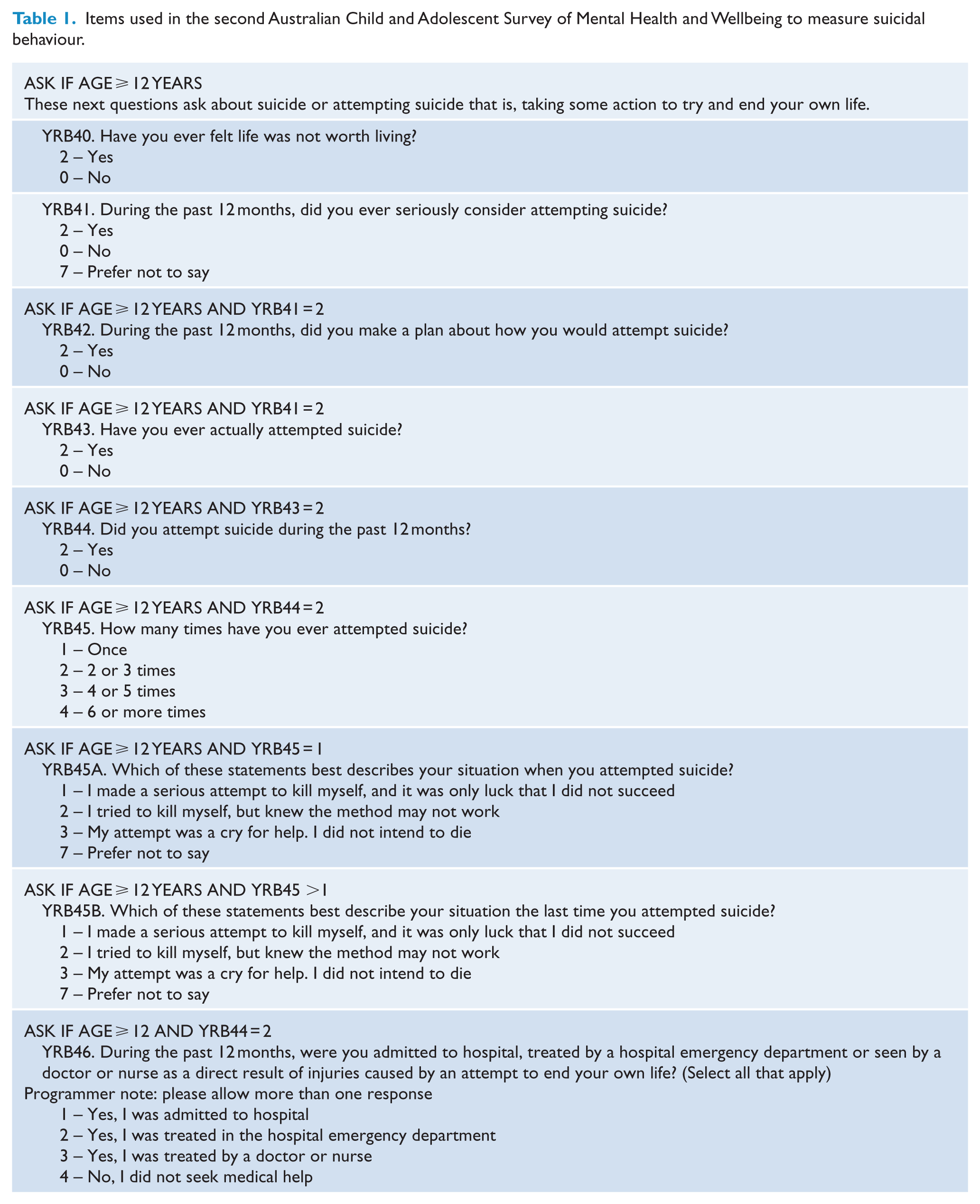
Young people aged 12–17 years completed a self-report questionnaire on a tablet computer in their home. All responses were confidential and not shared with the consenting parent. This included items from the Centers for Disease Control and Prevention (2014) Youth Risk Behavior Surveillance System (YRBSS), which ask respondents whether they have feelings that life was not worth living, the lifetime occurrence of a suicide attempt and the number of lifetime attempts. Additional items then probe the previous 12-month prevalence of suicidal ideation, making a plan for attempting suicide, making an actual attempt and whether an admission or access to emergency or other medical treatment occurred in the previous 12 months as a result of suicide attempt. The full text of the questions appears in Table 1. Participants were given the option in the initial screening question to answer ‘prefer not to say’ in addition to the ‘no’ and ‘yes’ response categories, an option not included in the 1998 First National Survey of Child and Adolescent Mental Health and Wellbeing. Young people who selected this option were sequenced out of the item set. This results in estimates that are not comparable to the 1998 survey (Sawyer et al., 2000).
Items used in the second Australian Child and Adolescent Survey of Mental Health and Wellbeing to measure suicidal behaviour.
Mental disorders were measured using the Diagnostic Interview Schedule for Children Version IV (DISC-IV) (Fisher et al., 1993). The DISC-IV implements the criteria for mental disorders set out in the Diagnostic and Statistical Manual of Mental Disorders, 4th Edition (DSM-IV) (American Psychiatric Association [APA], 2013). These criteria are based on clinically significant sets of symptoms that are associated with impaired functioning by young people with the disorders. The DISC-IV contains several modules, not all of which were used in the YMM. Seven modules were used in the survey – social phobia, separation anxiety disorder, generalised anxiety disorder, obsessive–compulsive disorder, major depressive disorder (MDD), attention-deficit/hyperactivity disorder (ADHD) and conduct disorder. Parents were administered all of these modules in order to ascertain the parent reported prevalence for each of these disorders. Young people were administered the MDD module owing to the likelihood that parents might not know whether their child was suffering from depression.
Results
All questions about suicidal behaviour were gathered directly from young people aged 12 years and over via a computer-assisted self-report (see Table 1).
Prevalence of mental disorders
The prevalence of DISC-IV MDD for 12- to 17-year-old survey participants based on their own self-reports was 8.6% (95% CI = [7.6%, 9.7%], n = 265). The prevalence of DISC-IV MDD for 12- to 17-year-old survey participants based on their parent or carer report was 5.0% (95% CI = [4.2%, 5.9%], n = 168), for ADHD it was 6.3% (95% CI = [5.3%, 7.4%], n = 163), for conduct disorder it was 2.1% (95% CI = [1.5%, 2.8%], n = 55) and for any parent- or carer-reported anxiety disorder it was 7.0% (95% CI = [5.9%, 8.1%], n = 212).
There was a low level of agreement about depressive symptoms between adolescents and their parents and carers. Only 2.2% (95% CI = [1.6%, 2.8%], n = 66) of 12- to 17-year-olds would have been identified as having MDD if it was based on both their own report and parent/carer reports.
Suicidal behaviour, age and sex
The lifetime prevalence of suicide attempts among 12- to 17-year-olds was 3.2% (95% CI = [2.5%, 3.8%]) with 1.3% (95% CI = [0.9%, 1.7%]) having made two or more attempts within their lifetime (Table 2). Significantly higher proportions of 16- to 17-year-olds than 12- to 15-year-olds reported having ever attempted suicide (5.3%; 95% CI = [4.1%, 6.6%] vs 2.0%; 95% CI = [1.3%, 2.8%]; p < 0.001) and having ever done so more than once (2.5%; 95% CI = [1.7%, 3.3%] vs 0.6%; 95% CI = [0.2%, 1.0%]; p < 0.001).
Prevalence of suicidal ideation, suicide plans and suicide attempts among 12- to 17-year-olds by sex and age group.
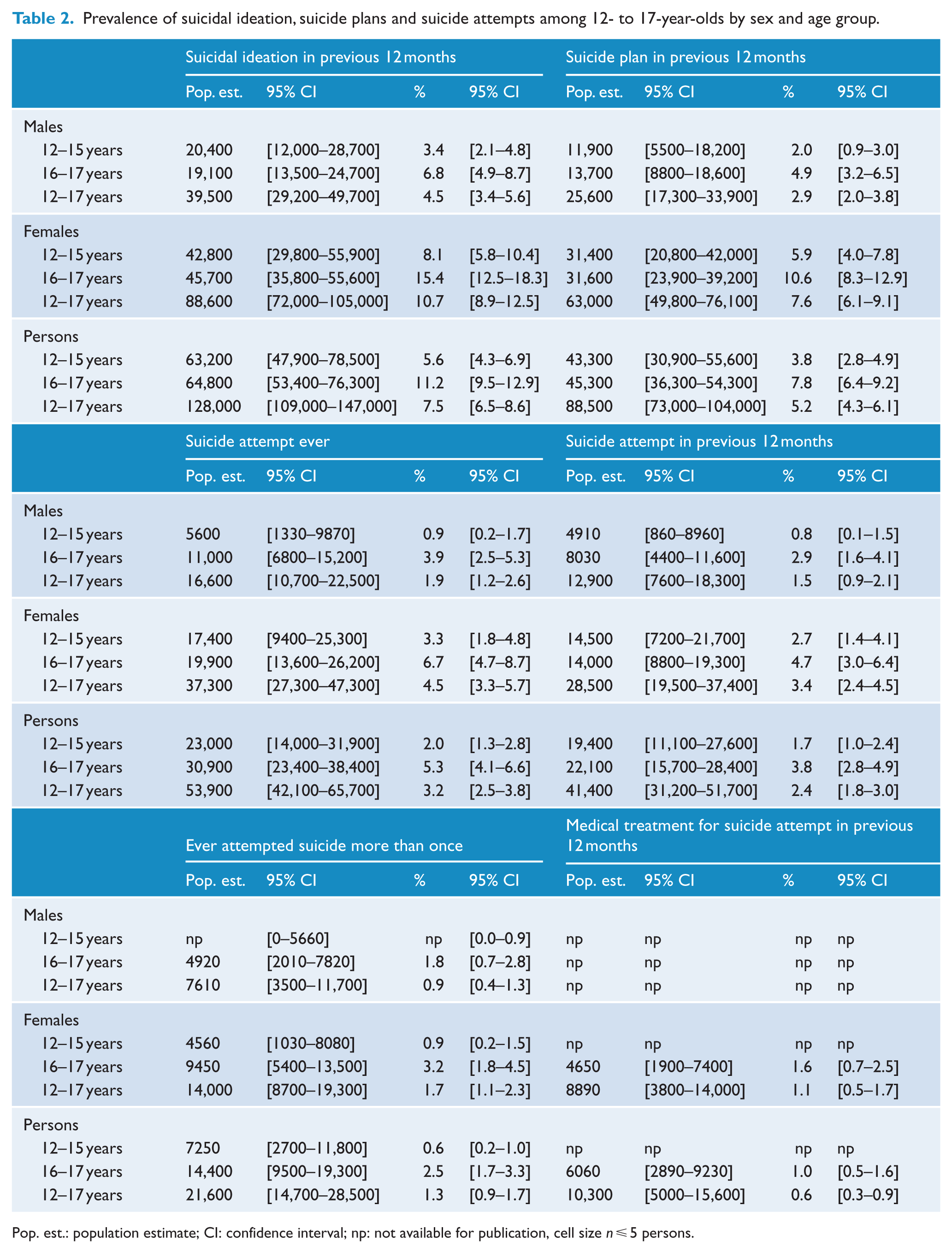
Pop. est.: population estimate; CI: confidence interval; np: not available for publication, cell size n ⩽ 5 persons.
For 12- to 17-year-olds, the 12-month prevalence of suicide attempts was 2.4% (95% CI = [1.8%, 3.0%]) with 7.5% (95% CI = [6.5%, 8.6%]) reporting suicidal ideation within the previous 12 months, 5.2% (95% CI = [4.3%, 6.1%]) having made a plan and 0.6% (95% CI = [0.3%, 0.9%]) receiving medical treatment within the previous 12 months for a suicide attempt.
All suicidal behaviours in the previous 12 months were significantly higher for 16- to 17-year-olds compared to 12- to 15-year-olds with 11.2% (95% CI = [9.5%, 12.9%]) having suicidal ideation (vs 5.6%; 95% CI = [4.3%, 6.9%]; p < 0.001), 7.8% (95% CI = [6.4%, 9.2%]) having made a plan (vs 3.8%; 95% CI = [2.8%, 4.9%]; p < 0.001) and 3.8% (95% CI = [2.8%, 4.9%]) having made a suicide attempt (vs 1.7%; 95% CI = [1.0%, 2.4%]; p < 0.01). About 1.0% (95% CI = [0.5%, 1.6%]) of 16- to 17-year-olds reported having medical treatment for a suicide attempt in the previous 12 months, but the numbers for 12- to 15-year-olds were too low for reporting.
Significantly more females than males reported having ever made a suicide attempt (4.5%; 95% CI = [3.3%, 5.7%] vs 1.9%; 95% CI = [1.2%, 2.6%]; p < 0.001) and having done so more than once (1.7%; 95% CI = [1.1%, 2.3%] vs 0.9%; 95% CI = [0.4%, 1.3%]; p < 0.05). Sex differences were also significant between both age groups, with consistently higher proportions of females than males having suicidal ideation, made a plan and attempted suicide within the previous 12 months.
Suicidal behaviour and mental disorder
Suicidal behaviour was more prevalent among young people meeting DSM-IV criteria for diagnosis (Table 3) and for females particularly. Compared with the lifetime prevalence of suicide attempt among 12- to 17-year-old females who had no mental disorder based upon their parent/carer reports (2.6%; 95% CI = [1.7%, 3.5%]), the prevalence of lifetime suicide attempt was significantly higher for those who met DSM-IV criteria for MDD (24.5%; 95% CI = [14.5%, 34.4%]; p < 0.001), conduct disorder (29.7%; 95% CI = [4.2%, 55.1%]; p < 0.05) and any anxiety disorder (15.6%; 95% CI = [8.4%, 22.8%]; p < 0.001). The prevalence of lifetime suicide attempts for those females with a DSM-IV diagnosis of MDD based on information they provided (28.4%; 95% CI = [21.2%, 35.5%]) was not different from the proportion of those with MDD reported by their parent or carer (24.5%; 95% CI = [14.5%, 34.4%]; p > 0.05).
Young people 12–17 years: suicidal ideation, suicide plans and suicide attempts, by mental health status and sex.
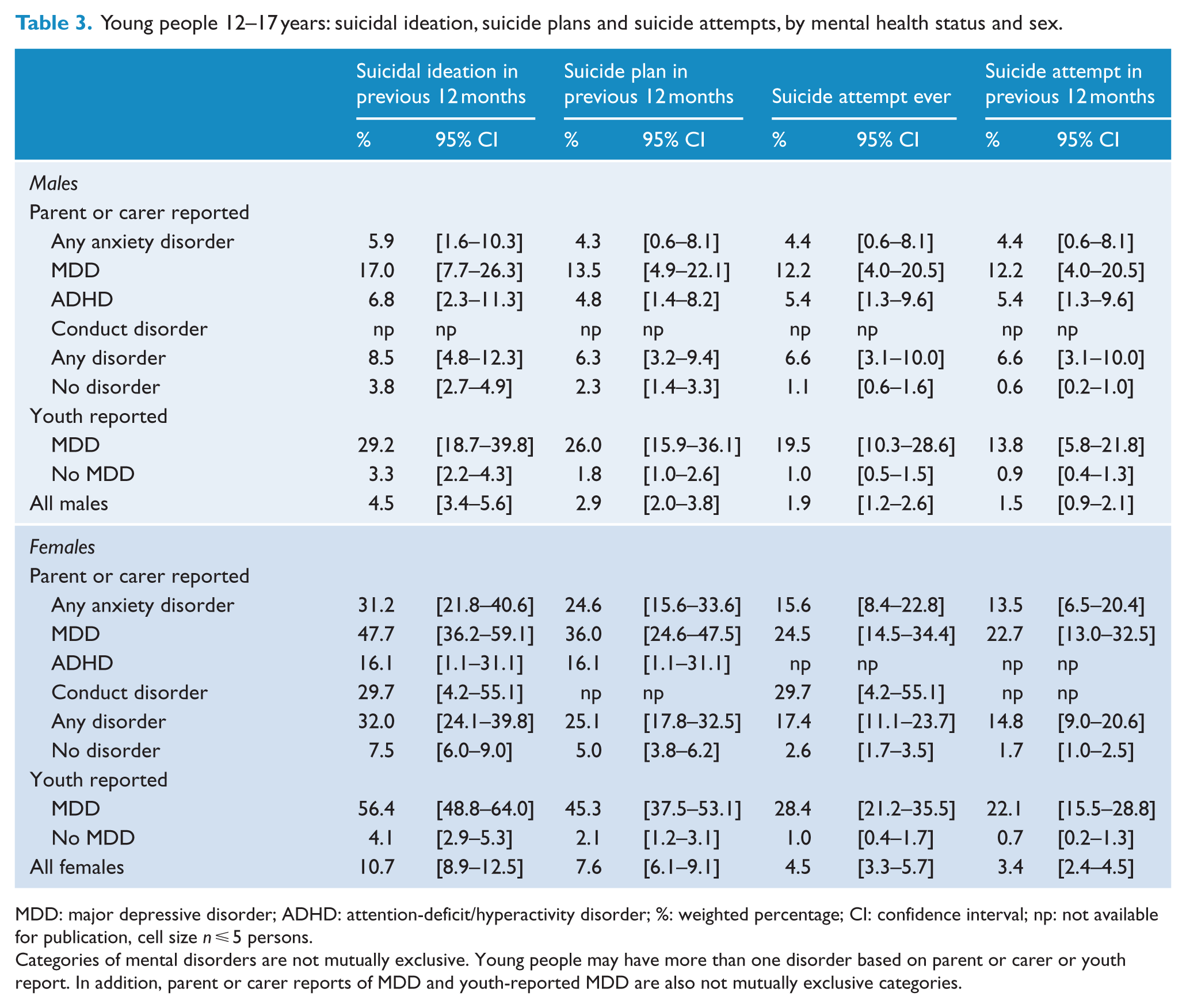
MDD: major depressive disorder; ADHD: attention-deficit/hyperactivity disorder; %: weighted percentage; CI: confidence interval; np: not available for publication, cell size n ⩽ 5 persons.
Categories of mental disorders are not mutually exclusive. Young people may have more than one disorder based on parent or carer or youth report. In addition, parent or carer reports of MDD and youth-reported MDD are also not mutually exclusive categories.
Compared with the lifetime prevalence of suicide attempt among 12- to 17-year-old males who had no mental disorder based upon their parent/carer reports (1.1%; 95% CI = [0.6%, 1.6%]), the prevalence of lifetime suicide attempt was significantly higher for those who met DSM-IV criteria for MDD (12.2%; 95% CI = [4.0%, 20.5%]; p < 0.01) and ADHD (5.4%; 95% CI = [1.3%, 9.6%]; p < 0.05) but not for any anxiety disorder (4.4%; 95% CI = [0.6%, 8.1%]; p > 0.05). The prevalence of lifetime suicide attempts for those males with a DSM-IV diagnosis of MDD based on information they provided (19.5%; 95% CI = [10.3%, 28.6%]) was not different from the proportion of those with MDD reported by their parent or carer (12.2%; 95% CI = [4.0%, 20.5%]; p > 0.05).
Broadly stated then, slightly more than 1 in 10 (11.5%; 95% CI = [8.1%, 14.9%]) of all young people aged 12–17 years with any parent- or carer-reported anxiety disorder, MDD, ADHD or conduct disorder reported ever having attempted suicide (data not shown). This compared with 1.8% (95% CI = [1.3%, 2.3%]; p < 0.001) without any of these parent- or carer-reported diagnoses.
The higher lifetime prevalence of suicide attempt in those young people with a mental disorder versus no mental disorder as reported by their parent or carer was also mirrored in the 12-month prevalence of suicide ideation, plans and attempt.
Among the 12- to 17-year-old females with MDD based on their parent/carer reports, 47.7% (95% CI = [36.2%, 59.1%]) had suicide ideation, 36.0% (95% CI = [24.6%, 47.5%]) had made a suicide plan and 22.7% (95% CI = [13.0%, 32.5%]) had a suicide attempt within the previous 12 months. In contrast, for 12- to 17-year-old females with no mental disorder as reported by their parent or carer, 7.5% (95% CI = [6.0%, 9.0%]; p < 0.001) had suicidal ideation, 5.0% (95% CI = [3.8%, 6.2%]; p < 0.001) had made a suicide plan and 1.7% (95% CI = [1.0%, 2.5%]; p < 0.001) had made a suicide attempt in the previous 12 months.
Compared to those with 12- to 17-year-old females with a DSM-IV diagnosis of MDD as reported by their parent or carer, the prevalence of suicide behaviour was higher, although not significantly so, among those females with MDD based upon their own responses to the DISC-IV module: 56.4% (95% CI = [48.8%, 64.0%]; p > 0.05) of females reported having suicidal ideation and 45.3% (95% CI = [37.5%, 53.1%]; p > 0.05) had made a plan, while proportions of females who reported making at least one suicide attempt were similar to the proportion reported by their parent or carer (22.1%; 95% CI = [15.5%, 28.8%]; p > 0.05).
Among the 12- to 17-year-old males with MDD based on parent/carer reports, 17.0% (95% CI = [7.7%, 26.3%]) had suicide ideation, 13.5% (95% CI = [4.9%, 22.1%]) had made a suicide plan and 12.2% (95% CI = [4.0%, 20.5%]) had a suicide attempt within the previous 12 months. In contrast, for 12- to 17-year-old males with no mental disorder as reported by their parent or carer, 3.8% (95% CI = [2.7%, 4.9%]; p < 0.01) had suicidal ideation, 2.3% (95% CI = [1.4%, 3.3%]; p < 0.01) had made a suicide plan and 0.6% (95% CI = [0.2%, 1.0%]; p < 0.01) had made a suicide attempt in the previous 12 months.
Compared to those with 12- to 17-year-old males with a DSM-IV diagnosis of MDD as reported by their parent or carer, the prevalence of suicide behaviour was higher, although not significantly so, among those males with MDD based upon their own responses to the DISC-IV module: 29.2% (95% CI = [18.7%, 39.8%]; p > 0.05) of males reported having suicidal ideation and 26.0% (95% CI = [15.9%, 36.1%]; p > 0.05) had made a plan, while proportions of males who reported making at least one suicide attempt within the previous 12 months were similar to the proportion reported by their parent (13.8%; 95% CI = [5.8%, 21.8%]; p > 0.05).
While suicidal behaviour is elevated particularly in the presence of MDD, with female proportions for these behaviours among this disorder elevated twofold to threefold higher than males, the presence of any mental disorder among females is associated with consistent elevations in the frequency of these suicidal behaviours (Table 3). For males, these associations are all substantially weaker and principally occur in the presence of MDD.
Co-variation with social and demographic variables
Suicidal behaviours were strongly associated with family composition, family income, parent and carer education and employment, family functioning and geographic location. Due to the inter-relationship between these factors, univariate and multivariate logistic regression was used to further examine these (Table 4). Because the quantitative information in these tables is voluminous, we confine our reporting here to the findings for suicidal ideation and 12-month suicide attempt only.
Suicidal behaviour in 12- to 17-year-olds by mental disorder and socio-demographic characteristics.
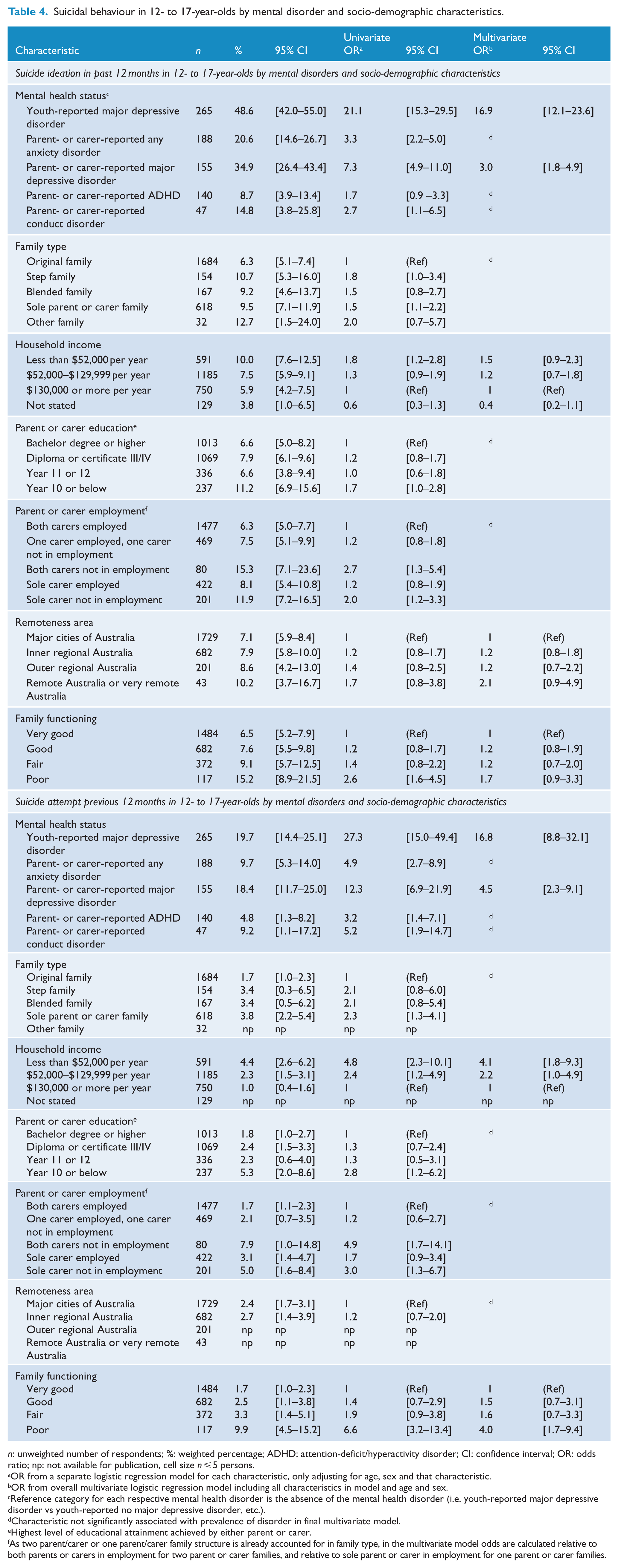
n: unweighted number of respondents; %: weighted percentage; ADHD: attention-deficit/hyperactivity disorder; CI: confidence interval; OR: odds ratio; np: not available for publication, cell size n ⩽ 5 persons.
OR from a separate logistic regression model for each characteristic, only adjusting for age, sex and that characteristic.
OR from overall multivariate logistic regression model including all characteristics in model and age and sex.
Reference category for each respective mental health disorder is the absence of the mental health disorder (i.e. youth-reported major depressive disorder vs youth-reported no major depressive disorder, etc.).
Characteristic not significantly associated with prevalence of disorder in final multivariate model.
Highest level of educational attainment achieved by either parent or carer.
As two parent/carer or one parent/carer family structure is already accounted for in family type, in the multivariate model odds are calculated relative to both parents or carers in employment for two parent or carer families, and relative to sole parent or carer in employment for one parent or carer families.
Suicidal ideation, mental disorders and socio-demographic variables
The univariate associations for 12-month suicidal ideation are presented in Table 4. The odds of a young person reporting suicidal ideation in the previous 12 months were significantly higher when the young person had a mental disorder compared to those with no disorder. The odds of 12-month suicidal ideation was particularly high for young people with MDD based on their own reports (odds ratio [OR] = 21.1; 95% CI = [15.3, 29.5]), and less so, but still significant, for those young persons with MDD based on parent and carer reports (OR = 7.3; 95% CI = [4.9, 11.0]). In univariate analyses, there were significant associations with sole parent status (OR = 1.5; 95% CI = [1.1, 2.2]), low family income (OR = 1.8; 95% CI = [1.2, 2.8]), parent/carer unemployment (OR = 2.7; 95% CI = [1.3, 5.4]) and poor family functioning (OR = 2.6; 95% CI = [1.6, 4.5]).
In multivariate analyses, the only predictors of 12-month suicidal ideation that remained significant after adjusting for the socio-demographic variables were youth-reported MDD (OR = 16.9; 95% CI = [12.1, 23.6]) and parent- or carer-reported MDD (OR = 3.0; 95% CI = [1.8, 4.9]).
12-month suicide attempt, mental disorders and socio-demographic variables
The univariate associations for 12-month suicide attempt are presented in Table 4. The odds of a young person making a suicide attempt in the previous 12 months was significantly higher when the young person had a mental disorder compared to those with no disorder – these ORs ranged from 3.2 to 27.3. The odds of a 12-month suicide attempt was particularly high for young people with MDD based on their own reports (OR = 27.3; 95% CI = [15.0, 49.4]) and less so for those young persons with MDD based on parent and carer reports (OR = 12.3; 95% CI = [6.9, 21.9]). There were significant associations with sole parent status (OR = 2.3; 95% CI = [1.3, 4.1]), low family income (OR = 4.8; 95% CI = [2.3, 10.1]), low parent/carer educational status (OR = 2.8; 95% CI = [1.2, 6.2]), parent/carer unemployment (OR = 4.9; 95% CI = [1.7, 14.1]) and poor family functioning (OR = 6.6; 95% CI = [3.2, 13.4]).
Multivariate analyses of 12-month suicide attempt again produced ORs of a similar magnitude and pattern to those seen for 12-month suicidal ideation with 12-month suicide attempt more strongly associated with MDD when this was based on youth reports rather than parent and carer reports (OR = 16.8; 95% CI = [8.8, 32.1] vs OR = 4.5; 95% CI = [2.3, 9.1]; p < 0.05). It should be noted that the relatively low prevalence of 12-month suicide attempt prohibited reporting many effect estimations. Only low family income (OR = 4.1; 95% CI = [1.8, 9.3]) and poor family functioning (OR = 4.0; 95% CI = [1.7, 9.4]) remained significant in the adjusted model, with all other social and demographic variables being non-significant or not available for publication due to small cell sizes.
Discussion
The injury and/or loss of life caused by suicidal behaviour with its accompanying anguish and grief makes it a confronting circumstance for families, communities and governments. Our findings are positioned in an Australian context where there has been an extended national effort, since the early 1990s, to address mental health broadly and suicide specifically.
In 1993, the Commonwealth and State and Territory Governments established the First National Mental Health Plan with a focus on 12 priority areas across a range of activities which included consumers, the general health sector, service mix, promotion and prevention, workforce and standards (Whiteford and Buckingham, 2005). Prevention of suicide was not a specific focus of the original National Mental Health Plan but was incorporated progressively in three renewed national plans released over the next 15 years (Australian Health Ministers, 1998, 2003; Commonwealth of Australia, 2009).
Specific national activity on suicide prevention has been progressed through a separate process, running in parallel to the National Mental Health Plans. Beginning initially with the release in 1997 of the National Youth Suicide Prevention Strategy (Commonwealth Department of Health and Family Services, 1997) that was fuelled by a rapid rise of suicide in young Australian males over the preceding years, this subsequently evolved into a broader national suicide prevention framework covering the whole population (Commonwealth of Australia, 2000, 2008), complemented by state-level plans in all Australian states and territories and a separate national plan to reduce suicide and deliberate self-harm in mental health services and related service settings (National Mental Health Working Group, 2005). Implementation was accompanied by ongoing and substantial investments by the Commonwealth, State and Territory Governments to develop broad-based community and population prevention approaches (Commonwealth of Australia, 2009; National Mental Health Commission [NMHC], 2012).
Evidence of the effectiveness of these approaches in reducing suicide rates has been mixed (Chamberlain et al., 2012; Goldney, 2006; Page et al., 2011). There also remains an ongoing call for improvements in standardising the collection of data about the epidemiology of suicidal behaviour and the regular and timely monitoring of it (De Leo et al., 2010). Partly in response to these concerns, the Commonwealth Government established the NMHC in 2012 to promote best practice and measure performance of the mental health system including through an annual national report card on Mental Health and Suicide Prevention (NMHC, 2012, 2013).
Our results provide a current, high-level description of the Australian epidemiology of suicidal behaviours in young people aged 12–17 years. We present new estimates of suicidal behaviour relative to the 1998 child and adolescent survey. Our aims were to estimate the prevalence of suicidal behaviours, describe their co-morbidity with mental disorders and describe their co-variation with key social and demographic variables. There are several features of the findings that merit comment.
With regard to prevalence, the estimates for suicidal behaviour in 12- to 17-year-olds showed that in the previous 12-month period, about 2.4%, or 41,400 young people, would have made a suicide attempt. About 7.5% of 12- to 17-year-olds report having suicidal ideation, 5.2% making a plan and 0.6% receiving medical treatment for an attempt.
As we noted in the ‘Introduction’ section, comparability with cross-national estimates of suicidal behaviours in young people is methodologically challenging owing to differences in measures as well as age aggregations. Broadly though, in comparison with the results reported here, US estimates of these suicidal behaviours in young people are higher by a magnitude of 2–3 (Centers for Disease Control and Prevention, 2014), while our estimate of 12-month suicide attempt (i.e. 2.4%) falls midway between that of New Zealand (4.5%) (Clark et al., 2013) and Great Britain (1.1%) (Meltzer et al., 2002).
Our reported estimates are not directly comparable to the 1998 national child and adolescent survey. Young people participating in the current survey were given the option of not answering the suicide questions. About 5.6% of 12- to 17-year-olds chose ‘prefer not to say’ to the first question in the sequence: ‘During the past 12 months, did you ever seriously consider attempting suicide?’ Those responding by selecting ‘prefer not to say’ were sequenced out of the remaining questions. It is not possible to estimate the proportion of these young people who might actually have considered attempting suicide. If it were assumed that all of these represented legitimate ‘yes’ responses, then the current estimate of 7.5% of young people who seriously considered attempting suicide in the previous 12 months would be adjusted upwards to a maximum of 13.7% – a figure more comparable with the 12.0% found in 1998. Notwithstanding this, there is insufficient evidence to suggest that suicidal behaviours have increased significantly in young people in the last 15 years. This is consistent with findings of no reported changes between 2007 and 2012 in suicidal ideation and suicide attempts among New Zealand secondary students (Fleming et al., 2014).
Second, the estimates of the proportions of young people with suicidal behaviour increase with age, with 3.8%, 11.2%, 7.8% and 1.0% of 16- to 17-year-olds reporting in the previous 12-month period a suicide attempt, suicide ideation, making a plan or receiving medical attention for an attempt, respectively. These estimates are all higher than those reported for those aged 16–24 years suggesting that they peak in the younger (i.e. <20 years) epoch (Johnston et al., 2009). Our observation of consistently higher proportions of females than males reporting suicidal ideation, making a plan and attempting suicide within the previous 12 months is well established in the global literature (Centers for Disease Control and Prevention, 2014; Clark et al., 2013; Nock et al., 2008).
Third, in the presence of any mental disorder, the proportion of 12- to 17-year-olds reporting suicidal behaviour significantly increases. This is particularly true when young people were found to have an MDD based on youth self-report – about one in five (19.7%) reported making a suicide attempt within the previous 12 months. However, as the findings reveal, there are significantly higher proportions of young people with a range of other mental disorders reporting suicidal behaviour when compared to those with no disorder. MDD certainly carries the largest associated risk, but higher proportions are notable in young people with any anxiety disorder and with conduct disorders.
Fourth, suicidal behaviours show very systematic and similar covariance with social and demographic circumstances. Gender and age are principal factors with all suicidal behaviours showing significant increases for both older age and female gender. The highest proportions of these behaviours occur among 16- to 17-year-old females relative to 12- to 15-year-old males. This is a commonly reported and enduring association.
Fifth, more broadly though, social and demographic correlates of suicidal behaviour show commonalities in both magnitude and pattern. Social disadvantage remains a major correlate of suicidal behaviour. In unadjusted models, significantly higher proportions of suicidal behaviours are observed in families with low income, low parent/carer education, unemployed families and sole parent families. The extent to which these findings suggest that the same socio-economic determinants that predict adult suicide rates are also those that are associated with self-harm and suicidal behaviour in young people (Milner et al., 2012) is subject to further analysis of the YMM self-harm data (Zubrick et al., 2015). Certainly, efforts at addressing social disadvantage and/or at reducing barriers to provision and access to mental health care for this segment of the Australian population might produce onward reductions in prevalence and burden associated with suicidal behaviour.
Sixth, most, but not all, of these socio-economic determinants become non-significant once the young person’s mental health status is included. Typically, across all suicidal behaviours, the presence of a mental health disorder shows the single and largest association with lifetime and 12-month suicidal behaviour, with only sole parent family status and poor family functioning remaining significant. For young people, the context of the family and the interpersonal relationships that it entails are likely to be important contributors to elevating the risks of suicidal behaviour. These results show that social disadvantage has some pathways contributing to mental disorder (see Milner et al., 2012), but that once a mental disorder is present, only poor family function and sole parent status remain significantly associated with suicidal behaviours.
Finally, there are some results that are not significant that should be noted. The survey was a national survey and not designed to produce individual state or territory estimates. It was, however, possible to produce estimates distinguishing major cities from inner and outer regional areas and remote and very remote areas. None of these distinctions produced statistically significant differences in the proportions of young people engaging in suicidal behaviours.
There are important limitations to this report. Even with a large national sample, because the prevalence of some suicidal behaviour is low, some estimates of interest are not possible to produce owing to insufficient sample sizes. Second, these results rely entirely on self-reported data with all the caveats that apply to uncertain reliability, social desirability and incomplete information.
A considerable effort is expended across Australia in programmes aimed at suicide prevention. In population terms, mental disorders and their prevention, identification and treatment should be a leading intervention point for such programmes both in the primary health sector and in the mental health sector specifically. The associations examined here also suggest that efforts to assist sole parent and/or dysfunctional families would be worthy areas in which to target these efforts. The data here demonstrate that 41,000 Australian, 12- to 17-year-olds report attempting suicide in any 12-month period with over 10,000 having required medical attention for an attempt in this same period. This is not inconsequential in terms of the burden that this imposes on the health and mental health system or in terms of the likely suffering and misery of the young person themselves.
Footnotes
Acknowledgements
The authors wish to express their gratitude to the 6310 families who participated in the survey.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The second Australian Child and Adolescent Survey of Mental Health and Wellbeing was funded by the Australian Government Department of Health. Professor Zubrick is supported by a Centre of Excellence grant from the Australian Research Council (CE140100027).
