Abstract
Objective:
People with psychosocial disability are an important, although often neglected, subgroup of those living with severe and persistent mental illness. Rehabilitation, provided through clinical and non-government organisations in Australia, may contribute to their personal recovery goals. We hypothesised that people with psychoses with the greatest disability and complex needs would receive services from both sectors, reflecting treatment and rehabilitation needs.
Method:
Participants in the 2010 Australian national survey of psychosis (n = 1825) were interviewed to assess demographic, functional, mental and physical health characteristics and service use in the previous year. Two subgroups were created and compared: those using services from community mental health with, and without, non-governmental organisation involvement. Group membership was predicted by hierarchical logistic regression using variables selected on a priori grounds. Usefulness of the final model was examined by calculating improvement over the rate of accuracy achievable by chance alone.
Results:
The model was statistically significant but fell just short of useful (criterion 71.6%, model achieved 70.6%). Four independent variables contributed uniquely to predicting whether participants received both services (never married, childhood trauma, group accommodation, poor global functioning) consistent with the hypothesis. However, severe dysfunction in socialising was less likely to predict membership of the combined services group when compared with no dysfunction (p = 0.001, odds ratio = 0.384, confidence interval = [0.218, 0.677]), as was current smoking compared with none (p = 0.001, odds ratio = 0.606, confidence interval = [0.445, 0.824]).
Conclusion:
Findings suggest services provided by non-governmental organisations are targeted to those with the greatest disability although targeting could be improved. A subgroup of people with psychosis and severe disability in community mental health services do not access non-governmental services. Their unmet needs for rehabilitation and recovery have important implications for future development of community mental health, including the non-governmental sector.
Keywords
Introduction
People with psychosocial disability comprise an important, although often neglected, subgroup of those living with severe and persistent mental illness (SPMI) (Killaspy, 2014; National Mental Health Consumer and Carer Forum [NMHCCF], 2011). Psychosocial disability typically refers to the difficulties an individual with SPMI experiences in performing everyday tasks as a result of their impairments, which often excludes them from participation in the community through education, employment, recreation, relationships and having somewhere decent to live (Craig and Killaspy, 2015; Killackey et al., 2015). The term psychosocial disability emphasises the social consequences of disability, as distinct from psychiatric disability, which focusses on impairment (NMHCCF, 2011).
Disability is highest among people living with psychotic disorders, especially schizophrenia (Bottlender et al., 2010; Gureje et al., 2002; Siskind et al., 2012a). In all, 14% of people newly diagnosed with psychosis (Craig et al., 2004) and 44% of those with SPMI (Siskind et al., 2012b) live with the most severe disability and accompanying complex multi-agency support needs (Siskind et al., 2012a). The most potent individual risk factors for disability in people with psychosis are persisting symptoms, poor course of illness and poor premorbid adjustment (Gureje et al., 2002). Opportunities for participation in society may also be limited by stigma, discrimination and disadvantage and unfavourable social and political conditions (e.g. Killackey et al., 2015).
Persons living with severe psychosocial disability associated with their psychotic illness have a common set of difficulties which lead to complex needs. Typically, they have more severe illness characterised by frequent relapses and active and treatment-resistant symptoms, severe negative symptoms, cognitive impairments and co-morbid mental health problems, such as substance misuse. Consequently, they more often require supported accommodation. Most have physical health problems due to a combination of poor diet, inadequate exercise, smoking, unwanted effects of medication and economic disadvantage (Corrigan, 2003; Gureje et al., 2002; Holloway, 2005; Killaspy, 2014; Schöttle et al., 2013). There is also emerging evidence that childhood trauma and adversity complicate the course of illness and may lead to poorer functional outcomes (Shah et al., 2014). Compounding the difficulties of this subgroup, they tend to experience greater disadvantage on measures of income, employment and housing than those with physical or sensory disability (Beer and Faulkner, 2009; Kavanagh et al., 2015).
Psychosocial rehabilitation assists adults with psychosocial disabilities to progress in their recovery through strategies and programmes that support their goals in employment, housing and other aspects of community functioning (Corrigan, 2003; Corrigan et al., 2008; Killackey et al., 2015). There are important links between rehabilitation strategies and recovery-oriented policy and practice. However, rehabilitation is no longer emphasised in Australian mental health policy which instead features recovery, as well as social inclusion, as priorities (Department of Health (Australia), 2009; Gerrand et al., 2012). Even so, evidence-based rehabilitation practices can be used to promote recovery-oriented care by assisting individuals to manage, overcome or live with their mental illness and lead full lives in the community (Davidson et al., 2006; Killackey et al., 2015; Mueser, 2012). As articulated by Anthony (Anthony, 1993), ‘Recovery is what people with disability do. Treatment, case-management and rehabilitation are what helpers do to facilitate recovery’. Furthermore, separating rehabilitation from mental health treatment is counterproductive (Drake et al., 2003; Farkas and Anthony, 2010).
Within Australia, psychosocial rehabilitation is provided through clinical and independent sectors. Public community mental health (CMH) services in the clinical sector are increasingly recovery-focussed and offer inpatient or community-based rehabilitation to varying extents. However, the independent sector, mostly represented by non-governmental organisations (NGOs), is funded more explicitly to provide psychosocial rehabilitation and recovery support (Gerrand et al., 2012). In effect then, most rehabilitation and recovery services are separate from mental health treatment in Australia. This has resulted in unhelpful service fragmentation and gaps requiring increased care coordination, particularly for people with SPMI (Brophy et al., 2014; Whiteford et al., 2014).
A steady growth in the Australian mental health NGO sector has resulted in a workforce of comparable size to the clinical mental health workforce (Gerrand et al., 2012; National Health Workforce Planning and Research Collaboration, 2011). Recent developments have included better inter-sectoral care coordination through improved planning and collaboration (Department of Health and Human Services, 2012), a strong growth in partnership models between public mental health and NGOs and embedding the Commonwealth government funding of the Partners in Recovery in an effort to improve care coordination (Brophy et al., 2014). The National Disability Insurance Scheme (NDIS) has been extended to people with psychosocial disability, and this significant reform will enable increased emphasis on self-directed support and a wider range of options (Williams and Smith, 2014). However, there remains a lack of clarity regarding characteristics of individuals currently receiving services and what is provided (Siskind et al., 2012a) as well as about the respective contributions of NGO and public CMH services to recovery of individuals with psychosocial disability.
The 2010 Australian national survey of psychosis (Morgan et al., 2012) offered an opportunity to address this since, unlike the first national survey (Jablensky et al., 2000), it included NGOs funded to support people with mental illness. This study aimed to describe the demographic, social, functional, and mental and physical health profile of people with psychoses in receipt of public CMH services, with and without NGO services. We hypothesised as follows: people with psychoses with the greatest disability and complex needs would be in receipt of both NGO and public CMH services, and this latter subgroup would be more likely to receive rehabilitation and recovery-focussed interventions than those solely receiving public CMH services.
Methods
Survey and participants
All participants took part in the 2010 Australian national survey of psychosis (Survey of High Impact Psychosis). This covered seven catchment areas in five states, a total area of 62,000 km2 and population of 1.5 million people aged 18–64 years, approximately 10% of the Australian population in this age group. A two-phase design was used (Pickles et al., 1995). First, during March 2010, screening for psychosis occurred in public specialised mental health services (MHSs) and NGOs supporting people with a mental illness. Second, people who were screened as positive for psychosis in the census were randomly selected for interview, stratified by age group (18–34 years and 35–64 years). Of 7955 people who screened positive for psychosis and were eligible, 1825 were interviewed. In all, 44% of those approached for interview responded; comparison of screening data for interviewees and those not interviewed for any reason indicated no systematic selection biases. Full details of the survey methodology are given in Morgan et al. (2012). The study was approved by institutional human research ethics committees at each study site, and all participants provided written, informed consent.
Assessments
A 32-module interview schedule was used to collect data on education, employment, housing, relationships, functioning, symptomatology, substance use, mental and physical health, MHS utilisation, rehabilitation, medication and psychosocial treatments. A global assessment of ‘any distressing or traumatic event in childhood’ was derived from questions on childhood trauma. Housing was divided into the following categories: group (group accommodation with on-site support staff including hostels, group homes, NGO and clinical residential rehabilitation); owned (by self or family); rented (public or private); and homeless (primary, secondary or tertiary)/institutional (lodges, nursing homes, hospital)/other (e.g. prison). A number of externally developed and validated instruments were used in their entirety and contributed variables used in this study (Morgan et al., 2012). In particular, current cognitive ability was assessed with the Digit Symbol Coding Test (DSCT) from the Repeatable Battery for the Assessment of Neuropsychological Status (Randolph, 1998). Independent functioning relative to community norms was assessed by interviewers for the previous 4 weeks, using the Multidimensional Scale of Independent Functioning (MSIF) (Jaeger et al., 2003). The Personal and Social Performance Scale (PSP) (Morosini et al., 2000) assessed behavioural and social aspects of functioning and role performance over the course of a year. Harmonised criteria (Alberti et al., 2009) were used to determine the metabolic syndrome. Similar values within variables were grouped in order to reduce the number of response categories where required.
Diagnostic assessment was based on a semi-structured clinical research interview, the Diagnostic Interview for Psychosis–Diagnostic Module (DIP-DM) (Castle et al., 2006) which contains selected interview questions and probes from the World Health Organization (WHO) Schedules for Clinical Assessment in Neuropsychiatry (Wing et al., 1990) mapped on the OPCRIT (McGuffin et al., 1991). DIP scores are fed into the computerised OPCRIT algorithm which produces diagnoses according to different classification systems, in this case, the 10th edition of the International Classification of Disease (ICD-10) (WHO, 2015).
Interviewers were predominantly mental health professionals seconded from public MHSs. To reduce inter-site differences, interviewers received specialised training in administering and scoring the survey instrument. Inter-rater reliability among interviewers was good (averaged pairwise agreement of 0.94 for ICD-10 diagnoses).
MHS usage
Details of MHS usage over the previous 12 months were collected, including participants’ use of public CMH services and NGOs. In relation to NGOs, three catchment sites each contained more than 10 NGOs and two sites between 6 and 10 NGOs. NGOs varied in size and provided diverse services, including group-based day programmes, individual outreach services, employment services, family or youth-specific programmes, counselling, peer support and residential rehabilitation. The remaining two sites contained five or less NGOs.
There were two approaches to data collection concerning NGO service usage. First, all NGOs within the survey catchment sites were invited to participate in the census by conducting screening for psychosis for all people in contact with them in the census month. In all, 86% of individual centres that were part of these NGOs and located within the catchment areas participated. Non-participating centres were typically smaller centres within larger participating organisations, predominantly in rural areas. Thus, one or two eligible NGOs (or parts thereof) in six of the catchments did not participate, whereas almost half did not participate in the one regional and rural catchment. Clients in participating NGOs who were screened as positive for psychosis were added to the pool of people to be randomised and selected for interview: 205 were randomly selected and interviewed. Second, all 1825 survey participants were asked about their use of NGOs in the previous year.
Creation of subgroups based on service use
Three subgroups were created comprising participants in receipt of NGO services only (‘NGO only’), public CMH services only (‘public CMH only’) and both NGO and public CMH services (‘NGO and public CMH’).
We aimed to create relatively homogeneous subgroups of participants likely to have been in receipt of their respective services for most of the previous 12 months, in order that any subgroup comparisons would reflect real differences. Therefore, only participants identified as having used services during the census month were included, since participants identified as using public specialised MHSs in the 11 months prior to the census included people who were not in receipt of such services for the full year, due to discharge or drop out from, or recent entry to, these services (Morgan et al., 2012).
Variables which concerned receipt of services over the past year were used to create these subgroups, as follows. The ‘public CMH only’ group consisted of participants who were in contact with public specialised MHS in the census month and NOT accessing an NGO in the previous year. To allocate participants correctly to the ‘NGO and public CMH’ group, those receiving only NGO services had to be correctly assigned to the ‘NGO only’ group, as follows: participants identified only by an NGO during the census month and without an identified case manager (n = 153), excluding those receiving community rehabilitation in a public hospital (n = 2) or government-funded community-based centre (n = 6), or attending a public CMH clinic (n = 24) or receiving public CMH care through home-based outreach (n = 2). Participants were retained in the ‘NGO only’ group if they attended public or private outpatients and/or received crisis home visits (final n = 119). All other participants were in the ‘NGO and public CMH’ group (Figure 1).
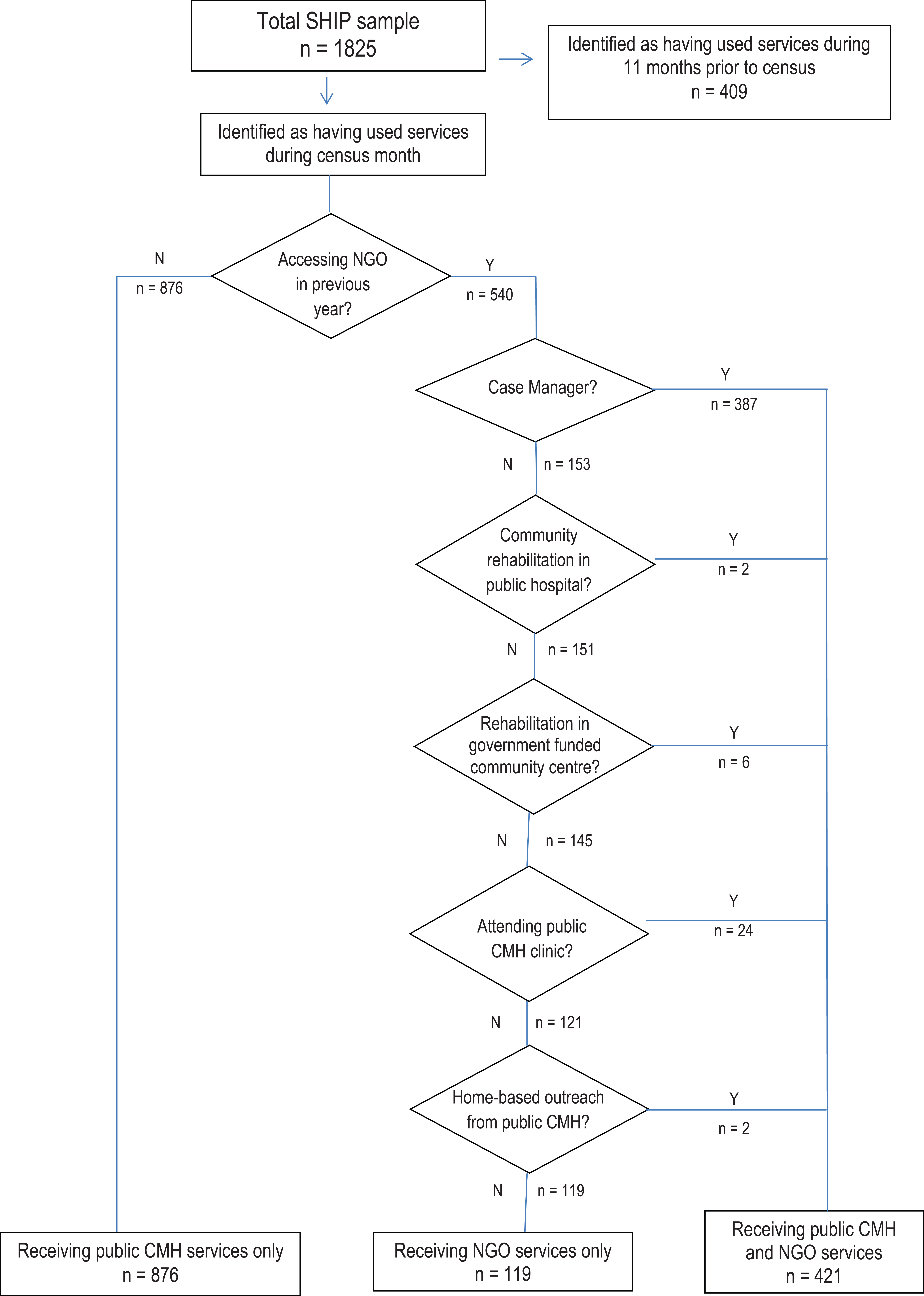
Flow chart for subgroup creation.
This article reports on those in receipt of public CMH services, with or without NGO services (n = 421 and n = 876, respectively).
Analysis
Data analysis was conducted using IBM SPSS for Windows Version 21 (SPSS, 2009). Univariate analyses to compare the two subgroups used the Chi-square test for independence for categorical variables. All variables had a minimum expected cell count of 5 or more and met assumptions. Any 2 × 2 tables utilised Yates’ Correction for Continuity. Standardised residuals (SRs) were used to examine the difference between expected and observed cases within values. Continuous variables describing receipt of services were extremely skewed and therefore reported as number (and proportion) of participants.
Group membership was predicted using hierarchical logistic regression. Three blocks were used: Block 1 included demographic and early life experience variables, Block 2 included clinical and substance use variables and Block 3 included functioning and disability. Putative predictor variables were selected on a priori grounds, with their distribution across groups assessed with univariate analyses. Two categories of duration of illness were created using a median split. The metabolic syndrome measure had missing data in a significant number of cases which limited the total sample size of the model. It was therefore excluded from the final analyses. All hierarchical logistic regression assumptions were met. Specifically, based on approximately 40 cases for every stepwise variable, a final 25 variables (see Table 1 for details) were entered in the regression which therefore required 1000 participants. Forward stepwise entry was used to refine the predictor variables. Multi-collinearity was assessed by inspecting correlations between the putative predictor variables and the respective tolerance scores. The highest correlation (0.609) was between number of negative symptoms and overall socialising, which was below the 0.9 cut-off for exclusion. The full model was also run, excluding each of these variables in turn, without altering the final model. There were no variables identified with a tolerance score below 0.1, indicating that none of the entered variables shared a high correlation with any other variable. Each variable was inspected individually for outliers; as there were no differences at the 5% trimmed mean level beyond 0.2, this indicated there were no outliers. In the final model, predictors were identified using a value of p < 0.05 as a cut-off, with odds ratios (ORs) and confidence intervals (CIs) also examined.
Demographic, clinical and functional profile of participants in receipt of public community mental health (CMH) services only and those receiving NGO and public CMH services.
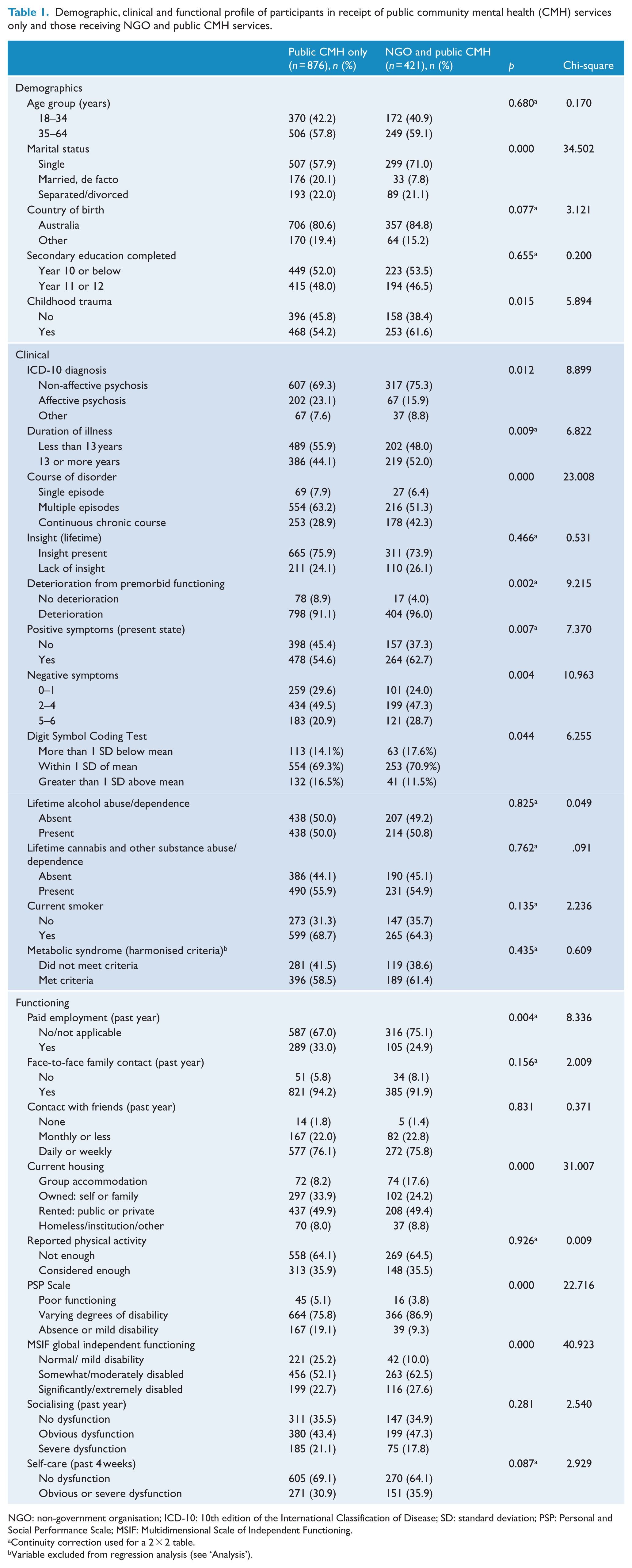
NGO: non-government organisation; ICD-10: 10th edition of the International Classification of Disease; SD: standard deviation; PSP: Personal and Social Performance Scale; MSIF: Multidimensional Scale of Independent Functioning.
Continuity correction used for a 2 × 2 table.
Variable excluded from regression analysis (see ‘Analysis’).
In order to evaluate the usefulness of the regression model, we assessed improvement over the rate of accuracy achievable by chance alone. The proportional by chance accuracy rate was calculated with the requirement that the model accuracy was 25% better than the chance criterion.
Results
Profile of people with psychosis receiving public CMH services with and without NGO services
Table 1 profiles participants in the two subgroups with respect to demography, functioning and disability, and clinical status. They were predominantly single, unemployed and in regular contact with family and friends despite experiencing at least moderate disability and obvious or severe dysfunction in socialising. Most were diagnosed with non-affective psychosis and had experienced multiple episodes of disorder.
The ‘NGO and public CMH’ group had significantly fewer than expected participants in married or de facto relationships (7.8% vs 20.1%, p = 0.000) and among those who did not report childhood trauma (38.4% vs 45.8%, p = 0.015) compared with the ‘public CMH only’ group. There were no differences in proportions of males within subgroups, with 60.1% of the combined NGO and public CMH group and 60.3% of the public CMH only group identified as male (SR = 0.0, χ2(1, n = 1297) = 0.000, p = 0.999, phi = 0.002). A number of statistically significant clinical differences emerged. A higher than expected proportion of those in the ‘NGO and public CMH’ group had a duration of illness of at least 13 years (52.0% vs 44.1%, p = 0.009), a continuous chronic course of disorder (42.3% vs 28.9%, p = 0.000) and were experiencing at least five negative symptoms of psychosis (28.7% vs 20.9%, p = 0.004), whereas the ‘NGO and public CMH’ group had fewer than expected participants with ICD-10 affective disorders (15.9% vs 23.1%, p = 0.012), no deterioration from premorbid functioning (4.0% vs 8.9%, p = 0.002), no current positive psychotic symptoms (37.3% vs 45.4%, p = 0.007) and performing greater than 1 standard deviation above the mean score on the DSCT (11.5% vs 16.5%, p = 0.044). With regard to social and functioning variables, significantly fewer than expected within the ‘NGO and public CMH’ group had absent or mild disability according to the PSP (9.3% vs 19.1%, p = 0.000), were rated as experiencing mild or absent disability on the MSIF Overall Global Independent Functioning scale (10.0% vs 25.2%, p = 0.000) or were in paid employment in the previous year (24.9% vs 33.0%, p = 0.004). Participants in the ‘NGO and public CMH’ group were also significantly more likely to be living in group accommodation (17.6% vs 8.2%, p = 0.000).
Prediction of subgroup membership: public CMH services with and without NGO services
Hierarchical logistic regression was performed to assess the impact of a number of factors on the likelihood that participants would belong to either the ‘public CMH only’ group or the ‘NGO and public CMH’ group. The full model containing all predictors was statistically significant (χ2(14, n = 966) = 109.102, p = 0.000), indicating it could distinguish between respondents using public CMH services, or these and NGO services. The model as a whole explained between 10.7% (Cox and Snell R square) and 15.0% (Nagelkerke R square) of the variance in group status, correctly classifying 70.6% of cases. Entry of functioning and disability variables in Block 3 improved the model fit (Block 1: 3.5% [Cox and Snell R2] and 4.9% [Nagelkerke R2] of variance explained, 69.0% correct classification; Block 2: 6.3%, 8.9% and 69.0%, respectively). The proportional by chance accuracy rate was calculated as 57.3%. The criterion for model usefulness was 25% higher than this rate (i.e. 1.25 × 57.3 = 71.6%). As the overall percentage at the final step was 70.6%, the model fell marginally short of useful.
As shown in Table 2, there were six independent variables that made a unique contribution to the model (marital status, childhood trauma, current smoking, current housing, MSIF global functioning and socialising in the past year), with three of these having more than two categories. The strongest predictor of group membership was current housing with all groups less likely to be in the NGO and public CMH group compared with those living in group accommodation. This was especially so for those who were homeless or living in institutionalised or marginalised accommodation (OR = 0.286, between 3 and 4 times less likely to be receiving both services). Marital status (OR = 0.333) was also a moderately strong predictor: those in de facto or married relationships were three times less likely than those who were never married to be in the NGO and public CMH group. Global functioning (as measured by MSIF) was a slightly less powerful predictor, with those who were significantly or extremely disabled (p = 0.001, OR = 2.356, CI = [1.399, 3.969]) and those who were moderately or somewhat disabled (p = 0.000, OR = 2.203, CI = [1.442, 3.364]) a little more than twice as likely to be in the NGO and public CMH group, compared with those with absent or very mild disability. Conversely, dysfunction in overall socialising was less likely to predict membership of the combined services group, by a factor approaching 3 for those assessed as having severe dysfunction in comparison with participants with no such dysfunction (p = 0.001, OR = 0.384, CI = [0.218, 0.677]). Finally, those in the NGO and public CMH group had a greater probability of childhood trauma but were significantly less likely to smoke cigarettes.
Hierarchical logistic regression: membership of subgroup according to mental health service provision (public community mental health [CMH] only vs NGO and public CMH combined; n = 966).
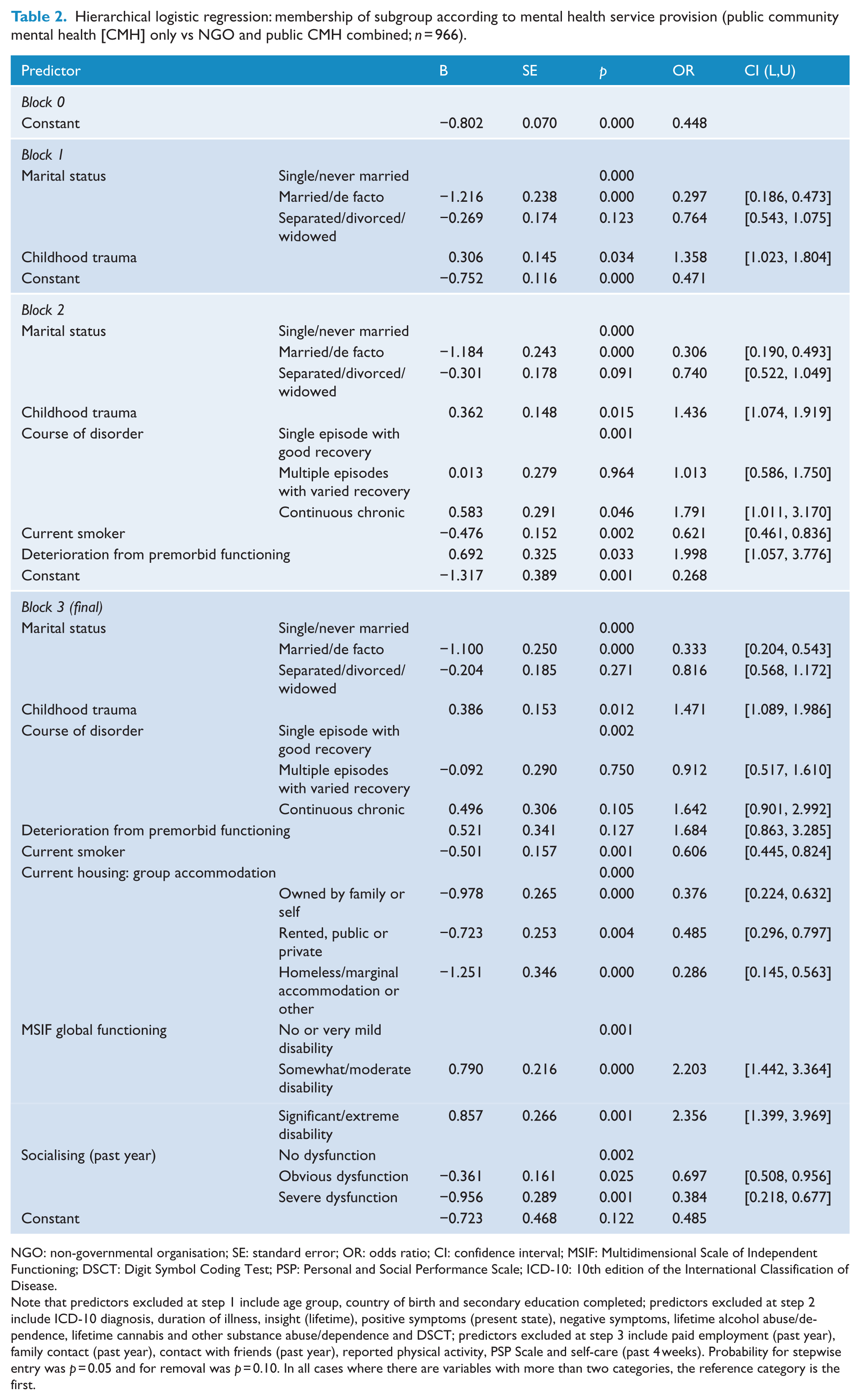
NGO: non-governmental organisation; SE: standard error; OR: odds ratio; CI: confidence interval; MSIF: Multidimensional Scale of Independent Functioning; DSCT: Digit Symbol Coding Test; PSP: Personal and Social Performance Scale; ICD-10: 10th edition of the International Classification of Disease.
Note that predictors excluded at step 1 include age group, country of birth and secondary education completed; predictors excluded at step 2 include ICD-10 diagnosis, duration of illness, insight (lifetime), positive symptoms (present state), negative symptoms, lifetime alcohol abuse/dependence, lifetime cannabis and other substance abuse/dependence and DSCT; predictors excluded at step 3 include paid employment (past year), family contact (past year), contact with friends (past year), reported physical activity, PSP Scale and self-care (past 4 weeks). Probability for stepwise entry was p = 0.05 and for removal was p = 0.10.
In all cases where there are variables with more than two categories, the reference category is the first.
Receipt of selected rehabilitation and recovery-focussed interventions
Subgroups were compared according to their receipt of services and interventions relevant to rehabilitation or recovery outcomes (see Table 3). People with psychosis receiving both NGO and public CMH services were significantly more likely to report receipt of a number of recovery-focussed services, compared with those receiving public CMH services alone. These included social skills training (29.0% vs 11.7%, p = 0.000), supported employment (30.3% vs 9.1%, p = 0.000), help to look after self or home (37.5% vs 21.1%, p = 0.000), financial (38.2% vs 32.1%, p = 0.034) and housing (51.2% vs 26.4%, p = 0.000) assistance. In addition, this group was significantly more likely to have participated in a community rehabilitation or day therapy programme in the past year (87.8% vs 17.5%, p = 0.000) and to report they had an individual recovery plan (43.5% vs 29.9%, p = 0.000) and less likely to endorse lack of any review of this plan in the previous year (15.5% vs 28.4%, p = 0.013). Approximately one-quarter in each group had been treated under a community treatment order at some time in the previous year. About one in five in both subgroups received Assertive Community Treatment (ACT) and more than half (216, 55.8%) of the combined group also received NGO outreach support. Peer-led support groups were used to a minor extent in both the public CMH (2.5%) and combined services group (4.7%). Home visits for crisis care were reported by just under one-third, regardless of subgroup (public CMH, 32.6%; NGO and public CMH, 29.0%). Approximately three-quarters in each group had a case manager from public MHSs (public CMH, 72.9%; NGO and public CMH, 76.7%).
Rehabilitation and recovery-focussed interventions received by participants in public community mental health (CMH) services only and those receiving NGO and public CMH services during previous year.
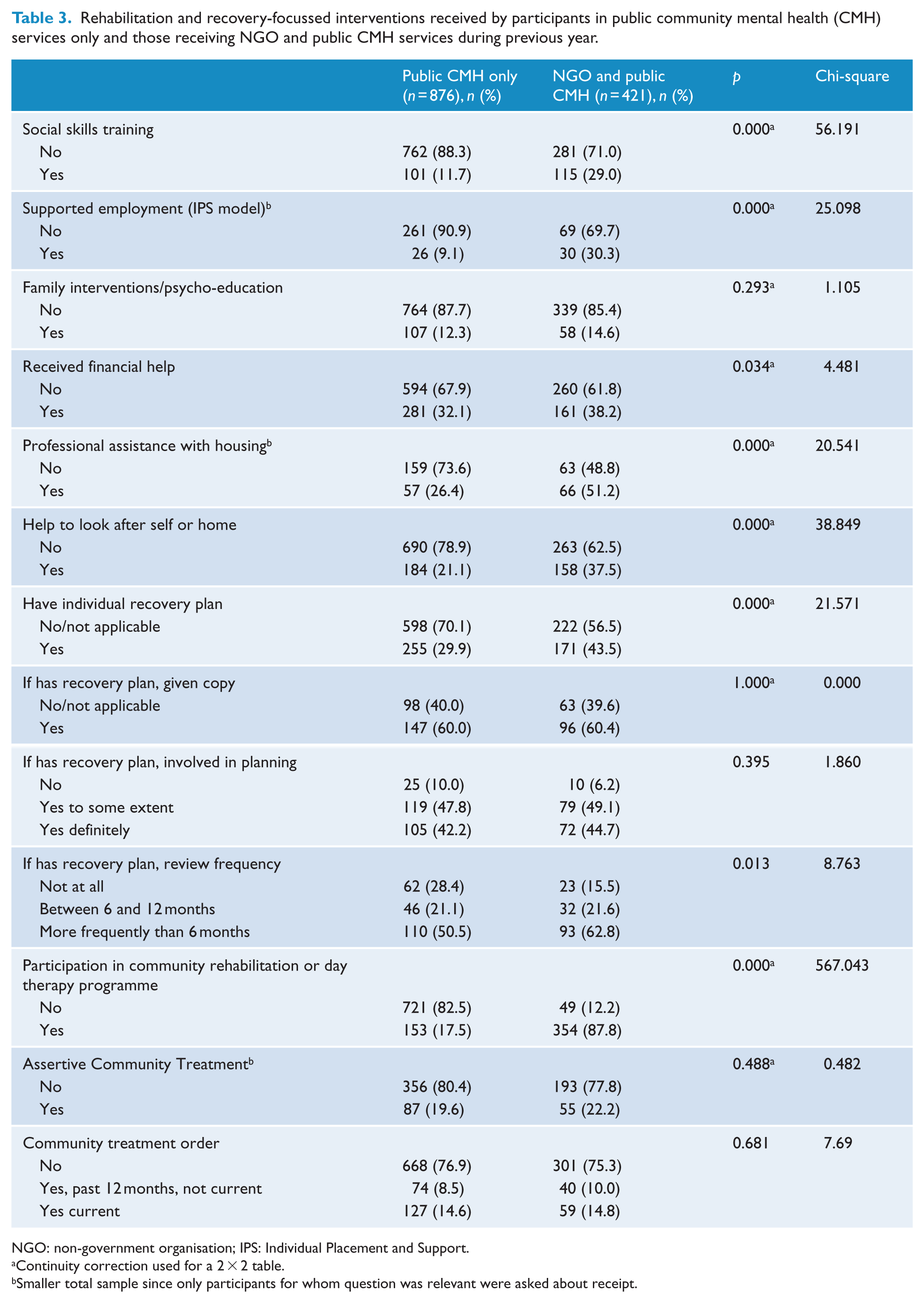
NGO: non-government organisation; IPS: Individual Placement and Support.
Continuity correction used for a 2 × 2 table.
Smaller total sample since only participants for whom question was relevant were asked about receipt.
Discussion
Our key finding is that people with greater disability and complex needs were receiving both public CMH and NGO services. Our model to predict CMH alone and CMH plus NGO subgroup membership was statistically significant, contributory variables possessed face validity and, for the most part, predictors were consistent with a picture of greater disability and complexity in the combined services group. However, an unexpected finding was that people living with psychoses with very restricted socialising were less likely to receive NGO services in addition to CMH services. Together with the regression model falling just short of useful in predicting group membership, this suggests the targeting of combined services to those with the greatest needs could be improved, especially for those with the most significant social disability.
To the best of our knowledge, this is the first study using epidemiological data to examine differences between people with psychosis with severe psychosocial disability and complex needs receiving clinical MHSs with or without NGO (or community-managed mental health) services in Australia. A strength of this study was the use of the large representative population-based sample ascertained from diverse catchment sites within the Australian national survey of psychosis. This provided an extensive suite of variables suitable for modelling purposes. The sampling methodology for the national survey specifically included NGO service users. Furthermore, NGO service use was ascertained through detailed interview enquiry using specially designed questions. Some predictors noted in the literature, for example, a measure reflecting the presence of treatment-resistant symptoms, were not available for these analyses which may have contributed to sub-optimal prediction of subgroup membership. Since people living with psychoses may transition between accessing and not accessing NGOs over time, this required a somewhat complicated process to create the subgroups. Hence, our findings may not reflect the full picture of service delivery in these sectors. Also, our data were reliant on participant self-report and may have been subject to recall bias.
As anticipated, our model, although falling just short of standard criteria for usefulness, was able to distinguish between people with psychosis using public CMH services or both public CMH and NGO services. According to two of the six variables making a unique contribution to the model (childhood trauma and poor global functioning as assessed by the MSIF) and in line with previous literature (Gureje et al., 2002; Holloway, 2005; Killaspy, 2014; Schöttle et al., 2013; Shah et al., 2014), those receiving both services were living with greater disability. This suggests there is reasonable targeting of NGO services to those in greatest need within public CMH services. However, these findings are qualified by our unexpected finding concerning social functioning, that is, those with greater social disability were less likely to access NGO services. We are unaware of similar findings. Consistent with their rehabilitation and recovery focus, NGO services emphasise their voluntary nature, promoting consumer empowerment, choice and self-determination (Commonwealth of Australia, 2013). This may mean that people with psychosis who have difficulties with social functioning are less likely to take up such services or services do not take into account difficulties in social functioning in design and delivery. An additional explanation for our findings is that NGO group-based programmes that may require participants to have better social functioning may also be less attractive to those with difficulties in social functioning. Alternatively, individualised approaches focussed on recovery and goal setting may inadvertently exclude people who struggle with not having the ‘right’ goals, as discussed by Rose (2014). Our findings also suggest a link between social difficulties, higher smoking rates and exclusion from NGO support. This is consistent with the literature suggesting people who are lonely or socially isolated are more likely to smoke and have other poor health behaviours (DeWall and Pond, 2011). Further research into social exclusion, smoking and targeted smoking interventions is needed.
Our data suggest Australians with psychosis who receive both public CMH and NGO services are much more likely to report participation in community rehabilitation or day therapy. Compared with those in the public CMH sector, participants receiving both CMH and NGO services reported greater receipt of interventions to assist with housing, employment and relationships. This is consistent with the type of support people are requesting and need and suggests there are limitations in accessing this type of support in the public CMH sector alone (Bird et al., 2014; Morgan et al., 2012). In the context of our findings concerning social disability, the relative lack of social skills training in public CMH settings is particularly concerning, considering its potential to improve social functioning (Killackey et al., 2015). Effective strategies to assist people to improve their social functioning should be developed and made more widely available in both the NGO and clinical sectors. Social skill deficits are likely to have pervasive detrimental effects on the ability to negotiate the business of everyday life, including participating in recovery and rehabilitation programmes.
Notwithstanding our finding that Australian MHSs are reasonably well targeted to people with psychosis and disability, it is evident there is a group of such individuals only receiving public CMH services. For example, in the public CMH group, 185 participants (21.1%) had severe dysfunction in socialising, 22.7% were significantly or extremely disabled (according to the MSIF), 30.9% had obvious or severe dysfunction in self-care and more than half reported childhood trauma (see Table 1). Our data suggest that their needs for rehabilitation and recovery-focussed services were only partially addressed (Table 3). Of note, a subgroup of people living with psychoses with very restricted socialising were less likely to receive NGO services in addition to CMH services. These people may be more accepting of individualised outreach services within the CMH sector providing rehabilitation in the form of ACT. This argues to retain such outreach models as others have concluded (Suggett et al., 2012) and in the face of changes to the contrary (Killackey et al., 2015; Rosen et al., 2013). Our data also strengthen the case for trauma-informed care to be provided by both CMH and NGO services (Shah et al., 2014).
Participants living in group accommodation were more likely to receive both CMH and NGO services. This is consistent with research reporting substantial disability and needs among this subgroup (e.g. Freeman et al., 2004; Hanson et al., 2007) and with the observation that group accommodation is commonly provided in the NGO sector, so this subgroup is more likely to access other NGO services. However, it is potentially concerning that those living in marginal or institutional settings are at a relative disadvantage here. Other studies, including the first national survey of psychosis, have suggested that those who are homeless and living in marginal accommodation experience the greatest disability which could be addressed by improved access to rehabilitation services or wider provision of ACT (Harvey et al., 2002; Herrman et al., 2004).
There are several implications for services and policy makers. Our findings suggest that targeting of, and access to, NGO services for those with the greatest disability could be further improved to better address their needs, especially those related to relationships. This may require additional strategies to improve service coordination and integration which should build on existing approaches (Brophy et al., 2014) as well as mechanisms identified in a recent systematic review (Whiteford et al., 2014). People living with psychosis and significant disabilities, especially social, who either cannot or will not attend group and clinic-based programmes require access to rehabilitation, including outreach, particularly within the public clinical mental health sector. Our study also suggests there is an important subgroup of people with psychosis and severe disability in public CMH services who do not access NGO services and accompanying opportunities for rehabilitation and recovery. Their unmet needs have important implications for those preparing the implementation of the NDIS as the scheme needs to consider how to engage those who are currently in need but marginalised from rehabilitation and recovery-focussed support services.
Unanswered questions and future research
Questions have been raised concerning how to best plan, develop and deliver services to ensure those with problems with social functioning have access to services that may assist them to improve their skills and social connection. The question of how rehabilitation needs can be adequately and comprehensively addressed within public clinical services and in the future NDIS environment also remains unanswered. Longitudinal studies would model access to rehabilitation and recovery-focussed MHSs and associated outcomes for people with psychosocial disability and complex needs.
Footnotes
Acknowledgements
This publication is based on data collected in the framework of the 2010 Australian National Survey of High Impact Psychosis. The members of the Survey of High Impact Psychosis Study Group are V. Morgan (National Project Director), A. Jablensky (Chief Scientific Advisor), A. Waterreus (National Project Coordinator), R. Bush, V. Carr, D. Castle, M. Cohen, C. Galletly, C. Harvey, B. Hocking, A. Mackinnon, P. McGorry, J. McGrath, A. Neil, S. Saw and H. Stain. Ethics approvals for the study were obtained from relevant institutional human research ethics committees. This report acknowledges, with thanks, the hundreds of mental health professionals who participated in the preparation and conduct of the survey and the many Australians with psychotic disorders who gave their time and whose responses form the basis of this publication.
Declaration of interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The study was funded by the Australian Government Department of Health and Ageing.
