Abstract
Objectives:
This paper systematically reviews all outcome studies of patients with mood disorders treated prior to the widespread use of antidepressants, mood stabilizers, and major tranquillizers. The aim is to estimate recovery and sustained recovery rates and to provide some evidence about the efficacy of modern drug treatments in changing the long-term outcome of mood disorders.
Methods:
MEDLINE and PSYCHINFO searches for studies on mood disorders published prior to 1970 were performed. Most studies were obtained by hand searching and extensive cross referencing. Information was independently extracted by the two authors.
Results:
A total of 29 relevant articles were obtained. The studies reviewed over 14,000 patients in total. Patients were mainly inpatients with a predominance of females. The majority of patients suffered from depression. The cohorts were followed up for 1–30 years. The median rate of recovery was 69% (range 17–91%). The time to recovery was generally several months. The median rate of recovering and remaining well was 51% (range 21–67%).
Conclusions:
The median rate of recovery is less than modern cohorts and the time to recovery longer. However, the rate of recovering and remaining well appears high compared to modern cohorts, although this result may reflect methodological issues. This review provides no support to the belief that pharmacological treatments have resulted in an improvement in the long-term outcome of patients with mood disorders.
Introduction
Studies on the outcome of patients with mood disorders prior to the introduction of psychopharmacology are of more than historical interest. They report data about the course of mood disorders in patients who were not given specific drug treatments such as antidepressants, mood stabilizers, or major tranquillizers. Such studies therefore provide indirect evidence about the efficacy of modern drug treatments in altering the course and outcome of mood disorders.
The modern era of drug treatment for mood disorders began with the demonstration of the value of imipramine in 1957 (Paykel, 1994). Any outcome studies reporting on patient cohorts with mood disorders who were followed prior to 1960 are unlikely to contain any individuals who received modern drug treatment. Fortunately, such studies are not only reasonably common but some are of high quality. There are a number of reasons for this.
First, most have long follow-up periods. Prior to 1960, clinicians appear to have had minimal concerns about the outcome of a single mood episode believing that its prognosis was favourable (Bond, 1921; Hohman, 1937). Their interest lay in whether the illness recurred. Kraepelin (1919), for example, considered that only long-term outcome was useful in evaluating accuracy of diagnosis and treatment response in patients with manic-depressive psychosis. Interestingly, there is now increasing acceptance by modern clinicians that most mood disorders are chronic and recurring and that the relevant measure of treatment success is long-term functioning rather than the outcome of a mood episode (Andrews, 2001; Judd, 1997). Successful treatment is when the patient recovers and remains well.
Second, there is some diagnostic uniformity. The diagnostic criteria for mood disorders in nearly all studies published prior to 1960 utilize Kraepelin’s definition of manic-depressive psychosis in the 6th edition of his textbook Lehrbuch der Psychiatrie in 1896 (Kraepelin and Diefendorf, 1912). Manic-depressive psychosis included periodic or circular insanity, simple mania, and melancholia. The description specifically excluded involutional melancholia (defined as pathological states of anxiety and depression in more advanced age) and reactive or neurotic depression (poorly defined but considered “environmental in origin and the psychic trauma is superficial in character”; Watts, 1956). In DSM-IV terms, manic-depressive psychosis would encompass bipolar I disorder, much of bipolar II disorder, major depression with melancholia and psychotic features, and severe major depression without these features. It should be noted that Kraepelin’s definition does not specify diagnostic criteria. The patients are therefore classified largely based on the subjective opinion of the treating psychiatrist.
Third, many of the cohorts are large and most retain a high proportion of subjects, possibly reflecting a less mobile and more complaint population. Fourth, the whole cohort is usually reviewed by one or two clinicians minimizing inter-rater reliability issues.
The aims of this paper are: (1) to extract from studies the rates of recovery and recurrence of patients with a diagnosis of manic-depressive psychosis treated prior to the use of drugs and published in English language journals; and (2) to obtain an estimate in each study of the proportion of patients who recovered and remained well over the follow-up period.
Methods
Search
We searched MEDLINE using the terms: manic-depressive psychos*, depressive disorder/or depressive disorder, major, melancholia, circular insanity, simple mania, depression and bipolar disorder and long-term outcome*, treatment outcome* and follow-up studies limited to English language and years “1902–1970”. A total of 63 studies were retrieved. The summaries of all these papers were studied, eight were read in full, and two were relevant. An identical search was conducted using PSYCHINFO. This yielded 22 studies whose summaries were reviewed, of which seven were fully reviewed and none were relevant. Most of the studies presented were obtained by hand searching reference lists of depression outcome studies and repeated extensive cross-referencing.
Selection
Articles that were selected reported on the follow up on a cohort of patients diagnosed with manic-depressive psychosis, manic-depressive insanity, melancholic depression, or endogenous depression. Patient cohorts with involutional melancholia and neurotic or reactive depression were not included. Cohorts of non-specific patients were included if data on manic-depressive psychosis could be analysed separately. A total of 29 studies fulfilled these criteria.
Validity assessment
Each article was independently reviewed by a clinician (RM) and statistician (CF) who extracted the following data:
Subjects: number of patients, diagnostic category, and how sample was obtained
Follow-up length
Follow-up methods: whether readmission, interviewed, case notes, letter, questionnaire, or other methods
Treatment: if stated
Length of illness episode
Outcome: this is reported within a restricted range of terms. The term “recovery” is used in 17 of the 29 studies. Unfortunately, it is rarely defined using any form of operational criteria. The term implies a full resolution of symptoms over a specified period. The difficulty is in knowing the period the authors are discussing. On some occasions, recovery is consistent with the patient remaining well over the entire follow-up period; in others, it includes those who recover but then have a recurrence over the follow-up period.
Recurrence: We have attempted to distinguish recovery and recurrence independently in each study. Some studies noted the recurrence, or attack, or readmission rates in the results while others contained it in the discussion; with others we were unable to reach any estimate of recurrence and have left it not specified.
Recovery and remaining well over follow-up period: by combining recovery and recurrence, we independently estimated our prespecified outcome measure (recovered and remained well over the period of follow up).
We divided the samples into three groups. The first were patients reported to have recovered or become much improved. The second were those who were unimproved, unchanged, deteriorated, or committed suicide. The third were those who were lost to follow up or died outside the mental hospital. We excluded those in the third group since their outcome remains unknown. Those in the second group were all considered to have a poor outcome i.e., not recovered and remained well. Those in the first group were separated into: (i) those who remained well after their much improved or recovery status throughout the follow-up period; and (ii) those who relapsed or suffered a recurrence of their mood symptoms. We were unable to calculate these groups in six studies. Pierce (1910) did not report the length of follow up and reported on relapse in “inhibitory” depression only. The large study by Malzberg (1957) only covers patients functioning until they were discharged from hospital. The other four studies (Astrup et al., 1959; Hastings, 1958; Hohman, 1937; Landolt, 1957) did not provide sufficient results to calculate the numbers of patients who remained well. For the other studies, we have used criteria if specified and tried to operationalize our categories as accurately as possible.
Equivalent data was produced for 23 of the 29 studies using these criteria. In the remaining six studies, differences were related to misinterpretation or omission and a consensus reached.
Results
Subjects
Patients were inpatients in 25 of the 29 studies reviewed. One study (Shobe and Brion, 1971) was split between outpatients and inpatients. There was a female predominance in all studies which reported gender breakdown, with the exception of two: one of these was an outpatient study (Hohman, 1937); the other reported more males in part of their cohort (Huston and Locher, 1948). The samples were all adults ranging in age from 17 to 80 years; the mean age when stated was around 40 years. The exception was Landolt (1957) which studied youths aged 15–22 years.
All studies which separated out subgroups of manic-depressive psychosis into mania only, depression only, and mixed episodes reported that the majority of patients had depression only. The rates of depression within the samples ranged from 55% (Pollock, 1931), through 60% (Kraepelin, 1921), 68% (Lundquist, 1945), 75% (Stenstedt, 1952), 80% (Bratfos and Haug, 1968) to 86% (Shobe and Brion, 1971).
Length of follow up
Reported length of follow up varied from 1 to 30 years. In one study (Pierce, 1910), this was not stated, but in all others some estimate of length of follow up can be made. The most conservative estimate is reported in Table 1.
Long-term outcome of manic-depressive psychosis.
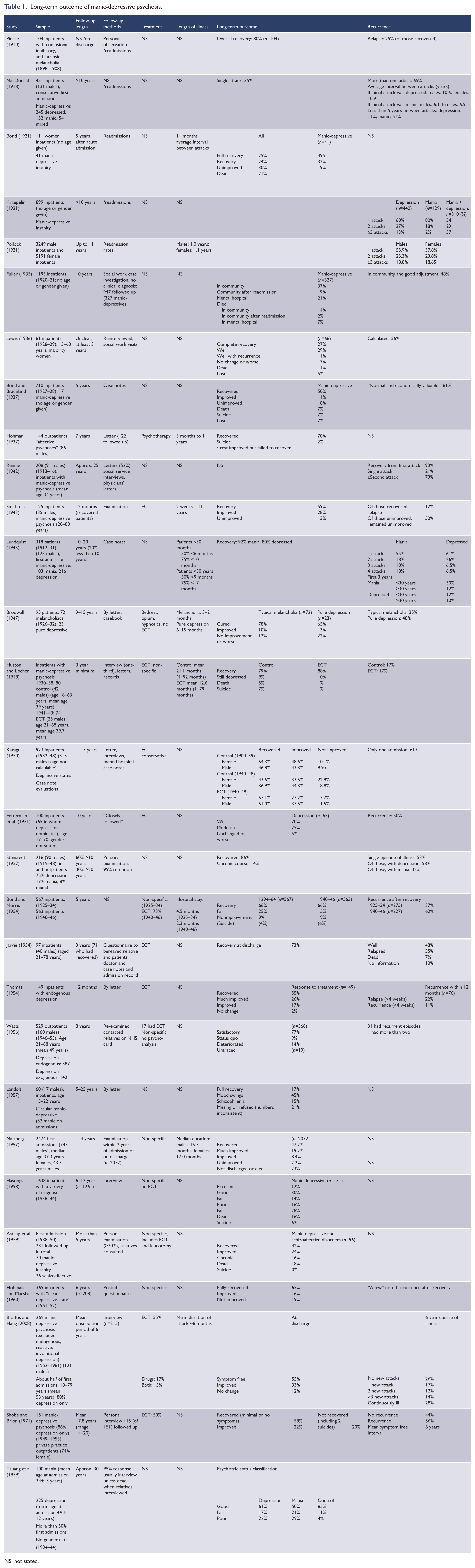
NS, not stated.
Follow-up methods
The follow-up methods are reported with increasing precision over time. The first five studies in Table 1 (Pollock, 1931; Pierce, 1910; MacDonald, 1918; Bond, 1921; Kraepelin, 1921) seem to have used readmission rates to judge outcome and relapse rates appear to have been based on this.
By the 1920s, follow-up methods grew in sophistication. Fuller (and colleagues; 1935) personally contacted a cohort of 947 (out of 1193) patients (including 327 with manic-depressive psychosis) 10 years after admission to a psychiatric hospital. The report on the patients functioning used “social case-work investigation” which consisted of detailed data relating to the patients physical, health history, employment, criminality, and their “degree of success in adjusting to the conditions of family and community life”. Other researchers used case notes (Bond and Braceland, 1937), letters (Hohman, 1937; Rennie, 1942), or interviews (Lewis, 1936; Rennie, 1942; Smith et al., 1943).
Similar follow-up methods continued in the 1930s and 1940s split between case notes and letters (Brodwall, 1947) a mixture of case notes and interviews (Huston and Locher, 1948; Karagulla, 1950), and personal examination (Stenstedt, 1952). In some later studies, vagueness about follow-up methods returns. Fetterman et al. (1951) reports only that his patients were “closely followed” for 10 years. Bond and Morris (1954) note difficulties in following up cases (the war, families moving) but do not state how they performed their follow up. By the 1940s and 1950s, studies largely used interviews often including interviewing relatives. Hohman and Marshall (1960) used a posted questionnaire.
Length of illness episode
While we felt the length of illness episode was important to record – it is one of the illness variables that appears to have changed most since the advent of drug treatment – but it was, perhaps due to low importance attached to it by earlier clinicians, generally not well assessed. Most early studies make no specific attempt to assess it, while in the latter studies it is generally vaguely stated: e.g. 2 weeks to 11 years (Smith et al., 1943) or 3 months to 11 years (Hohman, 1937). One estimate was based on the length of hospital stay in the large sample of Pollock (1931), who reported an average length of stay of 1.0 year for males and 1.1 year for females. The main studies which accurately assess the length of illness episode are those comparing cohorts receiving ECT with those who did not. Overall, length of illness is generally measured in months. Lundquist (1945) notes 50% of patients over 30 were ill more than 9 months, Huston and Locher (1948) report a range of 4 to 92 months with a mean of 21.1 months. The large first admission study by Malzberg (1957) reports median duration of illness of 15.7 months in males and 12.0 months in females.
Outcome: recovery
Table 2 shows the rates of recovery or much improved. The median rate of recovery was 69%, with a range of 17–91%. There is more consistency than this range suggests. The lowest recovery rate was in an atypical sample of young people (aged 15–22) with circular manic-depressive illness (Landolt, 1957). If this is excluded, the recovery or much improved rates varies from 46 to 91%, with most being in the 60–70% range (Table 2).
Summary table of overall outcome and proportion who recovered and remained well.
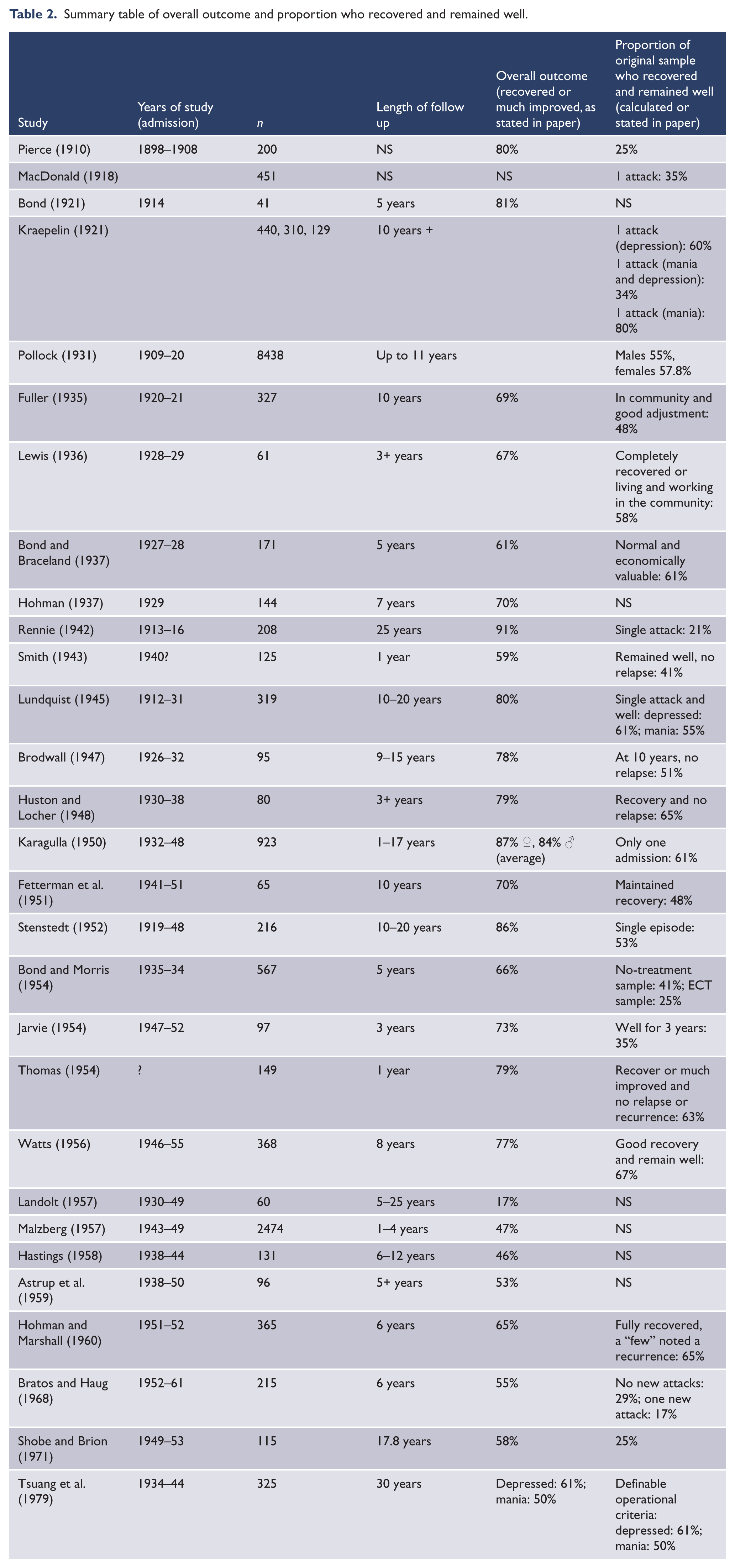
The recovered and remained well column involves more uncertainty. In some studies, the patients were reviewed once after a number of years; ranging from 1 to 7. In some cases, the absence of relapse was clearly stated: e.g. remained well – no relapse (Smith et al., 1943), single attack and well (Lundquist, 1945); in others, the recovery and remaining well rate was calculated using relapse and recurrence rates. The derived figure was conservative and, in some cases, may underestimate the proportion that recovered and remained well.
Table 2 shows a wide range of calculated values of individuals who recovered and remained well after their contact with mental health services. The median rate is 51% with a range is from 21 to 67%. To give a further crude idea of the distribution, we calculated the following: of the 23 studies in which we could reasonably estimate rates of recovery and remaining well, five had rates between 20–35%, four had rates of 35–50%, and 13 had rates above 50%. Using the numbers of patients, we calculated a total of 14,759 in the 23 studies: of these, 1615 were in studies where recovery and remaining well was 20–35%, 738 were in studies where the rates were 35–50%, and 12,406 were in studies where the rate was over 50%.
Treatment
The only specific treatment examined in these studies was ECT. Seven studies (Bond and Morris, 1954; Fetterman et al., 1951; Huston and Locher, 1948; Jarvie, 1954; Karagulla, 1950; Smith et al., 1943; Thomas, 1954) reported that ECT was used. Overall, the median rates of recovery and rates of recovering and remaining in these seven studies were 76 and 48%, respectively. Two studies (Huston and Locher, 1948; Karagulla, 1950) attempted an evaluation of the effect of ECT. Both contrasted a cohort of patients in an era before the use of ECT with one where ECT was used. Both reported no difference in rates of recovery or suicide. Huston and Locher (1948) reported a reduction in mean length of illness but Karagulla (1950) did not. Karagulla (1950) reported a higher incidence of relapse was associated with ECT but Huston and Locher (1948) did not.
Discussion
This paper systematically reviews all English language studies on the outcome of over 14,000 patients diagnosed with manic-depressive psychosis prior to the use of psychotropic drugs. The majority of these patients would now be considered to be suffering from major depression with a significant minority having bipolar disorder. Most studies reported on inpatient samples.
A majority of patients recover from their mood disorder. We estimate that a median of 69% of patients recover or are much improved over the follow-up period. However the time to recovery is highly variable and difficult to estimate in most studies. It is reasonable to state that the time to recovery is usually several months. Huston and Locher (1948) reported a mean of 21.1 months; Malzberg (1957) reported 15.7 months in males and 12 months in females. Brodwall (1947) noted that episodes of melancholia lasted 3–21 months while pure depression lasted 6–15 months. These estimates are consistent with other historical studies of inpatient length of stay. Evenson et al. (1994) reported a mean length of stay for major affective illness of around 16 months in the late 19th century. Healy et al. (2001) reported median lengths of stay of 9 months and 7 months for manic-depression and depression, respectively, in 1896. Both studies noted the contrast between lengths of stay a century later. Evenson et al. (1994) reported a mean length of stay of 48 days in the 1970s, while Healy et al. (2001) reported stays of 6.5 days for manic-depression and 3.5 days for depression in 1996.
The study by Ravn (1966) on endogenous depression reports that the mean length of hospital stay prior to 1937 was 313.4 days compared with around 70 days after the introduction of ECT and medications. Similarly Lenzi et al. (2008) reported that in the no-treatment era (prior to ECT), the mean length of single episode ranged between 7 and 14 months (although this was based on only three studies: Kraepelin (1921); Pollock (1931); Rennie (1942). They concluded that the length of episode had decreased from 1 year to 1 month.
No study specifies treatment prior to the study by Smith et al. (1943), which included patients who received ECT. The seven studies where ECT was used reported a median recovery rate of 76%, which is slightly higher than the overall recovery rate. The median rate of recovering and remaining well was 48% compared with 51% overall. The two studies which contrasted cohorts receiving ECT with earlier cohorts who had no access to ECT reported no differences in recovery rates or suicide rates (Huston and Locher, 1948; Karagulla, 1950). One reported a reduction in the length of admission for those receiving ECT (Huston and Locher, 1948), while the other reported a higher rate of relapse for this group (Karagulla, 1950). The mean differences in outcome are surprising given the general acceptance of the efficacy of ECT. It is little wonder that Karagulla concluded that although the “statistical evidence in this survey does not provide that ECT increases recovery rate, decreases duration, and prevents recurrence in depressive states, clinical observations testifying to its value cannot be disregarded” (p. 1091).
We estimate that the proportion of patients who recover and remain well ranges from 21 to 67% with a median of 51%. On the face of it, this figure appears optimistic. Recent estimates suggest that a lesser proportion of depressed patients recover and remain well. Brodaty et al. (2001) summarized modern era long-term studies and reported that major depression is now viewed as a chronic illness with repeat episodes of around 75%, readmission rates of 35–62%, and chronicity in 5–25%. Mulder (2004) reported that depending on the sample studied, 80–90% of patients recover, but 70–80% of these patients relapse and 10–20% do not recover at all. Overall, 20–25% of patients have a sustained recovery following an episode of major depression.
While surprising, our findings are consistent with the very few studies comparing the long-term outcome of mood disorders in the predrug and modern era. Ravn (1966) noted “strikingly few” readmissions among patients treated in a specific hospital prior to 1937 compared to those treated with ECT and drugs. Lenzi et al. (2008) using a small number of studies contrasted the “no-treatment era” with the “psychopharmacological era” and noted that the number of mood episodes has dramatically increased. Epidemiological studies have also reported that the use of drugs has not been associated with an improvement in the long-term outcome of mood disorders. Dickson and Kendell (1986) observed that between 1970 and 1981, when the use of lithium increased 10-fold, the rate of admissions for mania in Edinburgh trebled. Patten (2004) reported that increases in antidepressant use have been accompanied by an increased prevalence and duration of depressive episodes.
Limitations
These findings need to be seen in the context of significant methodological limitations. First, we confined ourselves to studies in English. Most Scandinavian studies were published in English and some German ones were translated into English. Our search strategy relied largely on extensive cross-referencing which did not uncover important non-English language studies. However, this might reflect these studies authors’ lack of knowledge of the non-English language literature.
Second, as we have noted, Kraepelin’s definition of manic-depressive psychosis did not provide specific diagnostic criteria. It is possible that some cohorts contain patients with other diagnoses. The study by Landolt (1957), for example, contained only young patients, with most suffering a probably rapid cycling bipolar disorder with a poor outcome. This cohort could possibly have been excluded from the review. We chose to make the review as systematic as possible and included all studies which fulfilled our criteria. We can be confident that most subjects had a serious mood disorder, since 25 of the 29 cohorts were inpatients. In addition when contrasting them with modern depressed cohorts, they had higher rates of bipolar disorder and may have had more physical illness.
Third, follow-up methods have been noted where possible, but in some studies the methodology was not stated. This weakness is unavoidable. Of more concern is that the follow-up methods may lead to an artificially low rate of recontact with psychiatric services. The conditions prevalent in mental hospitals in the early part of the 20th century may have discouraged representing for treatment unless it was absolutely unavoidable thereby increasing apparent rates of sustained recovery and lowering relapse rates. Modern cohorts may have increased monitoring by mental health workers in community settings. Therefore, changes in mental state might lead to treatment in a way that would have been unlikely in the past. Comparative destigmatization might also contribute to lower thresholds for treatment and admission (Healy et al., 2001). It is also possible that recovered or much improved outcomes are judged differently now. We may be more demanding about the quality of what constitutes a clinical response so reducing the apparent rate of sustained recovery.
Fourth, judging our prespecified outcome measure of recovery and remaining well was limited by the fact that few studies were specifically designed to do this. However, independently rating each study by a clinician (RM) and statistician (CF) produced complete agreement that in six studies we were not able to calculate a recovery and remaining well rate, and agreement on 17 of the remaining 23 studies. A consensus was easily reached on the six remaining studies.
Fifth, we did not include patients who were lost to follow up or died from causes other than suicide. How this strategy may have biased our findings is difficult to know. Those who were lost to follow up were probably not readmitted so not including them may have led to lower rates of recovery and remaining well. Those who died may have had a more serious mood disorder so not including them might underestimate rates of poor outcome. Most studies were careful to separate out death from suicide versus other causes so we were able to count all suicides as a poor outcome.
Conclusion
This review shows that the long-term outcome for patients with mood disorders in the predrug era was reasonably positive. Most patients recovered and the majority seemed to remain well after their recovery. Comparisons with modern drug-treated cohorts are difficult due to methodological limitations. Nevertheless there are some consistent findings. The length of mood episode has decreased significantly from around 1 year to 1 month or less. Death rates, other than those due to suicide, have also reduced significantly. In contrast, the recurrence of mood episodes appears to have significantly increased. These data, to paraphrase Dickson and Kendell (1986), provide no comfort for those, including ourselves, who have believed that drugs provide an effective prophylactic treatment for at least a substantial minority of patients with affective disorders.
Footnotes
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Declaration of interest
The authors report no conflicts of interest. The authors alone are responsible for the content and writing of the paper.
