Abstract
The development of medical technologies is often assumed to improve medical treatment, but may also reproduce health inequalities if their benefits are unequally distributed. Sociological studies have shown that social and moral evaluations matter for medical decision making, and that inequalities in access and outcome exist even in universal health care systems. This article uses the distribution of medical technologies in the treatment of type 1 diabetes as a case for examining the social production of health care inequalities. Drawing on observational data and in-depth interviews with physicians and nurses working in a Norwegian hospital, I demonstrate that medical staff evaluate patients based on a combination of medical, social and moral criteria. The concept of selective empowering is then elaborated and refined as a term for the practice in which medical professionals steer resources towards patients based on evaluations of need, competence and compliance. While previous studies of inequalities in medical care have often focused on medical staff’s cognitive dispositions, I argue that selective empowering may be interpreted as a reflexive response to increasing health care costs and a structural dependency on expensive and commercially produced medical technologies.
Keywords
Introduction
The relationship between social inequality and health is a foundational theme of medical sociology, and has been the subject of empirical studies since the 19th century (Waitzkin, 2011). Socially determined inequalities in health have persisted despite medical advances and technological development, and are as prevalent in the Nordic welfare states as in countries with less extensive welfare arrangements. In Norway, social inequalities in mortality are currently larger than in countries such as England, Italy and Spain, and have increased throughout the post-war period (Therborn, 2013). Higher-educated patients have also been shown to receive more medical services than others, indicating that social status matters for treatment in the Norwegian health care system (Elstad, 2018; Finnvold, 2009). Referred to as the ‘Nordic health paradox’, the persistence of health and health care inequalities in the Nordic countries challenges widely held assumptions in health inequality research, and highlights the need for studies examining the social production of health inequalities within formally egalitarian welfare systems (Mackenbach, 2012; Therborn, 2013).
One way of approaching the Nordic health paradox is to consider the capacity of welfare institutions to not only reduce, but also create new social divisions and hierarchies (Lutfey and Freese, 2005). The present study tackles this issue by examining how social and normative evaluations impacted the distribution of medical technologies at a Norwegian hospital. As researchers have demonstrated, medical treatment is shaped by social and normative considerations that may privilege high-status patients over others (Lara-Millán, 2014; Lorber, 1975; Timmermans, 1999). Previous research has often focused on socio-interactional dynamics, normative discourses and the subjective orientations of medical practitioners (Shim, 2010; Sointu, 2017; Willen, 2012), leaving the structural context of medical decision making less examined (Spencer and Grace, 2016). By contrast, the present study foregrounds institutional agency, structural factors and economic constraints as key determinants of unequal treatment. Drawing on observational data and in-depth interviews with physicians and nurses, I show how medical practitioners worked to distribute scarce medical technologies in the treatment of type 1 diabetes. I then elaborate and refine the concept of selective empowering as a term for the practice in which medical workers selectively distribute resources according to medical, social and moral criteria. Rather than a case of medical workers judging patients according to a fixed set of internalized expectations, I argue that the distribution of medical resources is an uncertain and often conflicted social practice in which medical staff reflexively respond to systemic pressures emerging from budgetary restraints, rising patient demand and an increased dependency on commercially developed technologies. The article contributes to our understanding of health care inequalities by specifying three logics of unequal treatment, and by illuminating how the moral economy of the health care system is shaped and conditioned by structural factors operating beyond the control of medical professionals.
Health care inequalities, empowerment and technological innovation
In the Nordic health discourse, the development of new treatment technologies is often assumed to improve health outcomes and provide solutions for various organizational and economic problems (Thygesen, 2019). However, technological innovation may also create and reproduce social inequalities if its benefits are unequally distributed. Technological advances often outstrip the resources necessary for optimal use, increasing the decisional burden on medical practitioners who must decide whom is to benefit from new and expensive treatment options (Ihde, 1990: 178; Simmons and Simmons, 1971). Medical technologies may therefore appear as limited resources that patients have to individually compete over, creating a ‘Matthew effect’ in which medical resources flow towards motivated, communicative and successful patients (Link and Milcarek, 1980; Merton, 1968).
In this study, I use the rationing of diabetes technologies in a Norwegian hospital as a case for examining the unequal distribution of medical resources. My theoretical approach takes as its starting point the established sociological insight that patients are evaluated and treated according to a ‘moral economy’ patterned by various normative and cultural expectations (Lara-Millán, 2014; Sointu, 2017; Taylor-Gooby et al., 2019). To the extent that these moral economies are structured by general hierarchies of status and prestige, the distribution of medical resources may serve to produce, reinforce and justify health inequalities. By examining this issue, the study also addresses the larger field of health inequalities research. A popular framework within the field is the fundamental cause theory (FCT), which states that socioeconomic status acts as a ‘fundamental cause’ of disease by determining health through a variety of proximal mechanisms that generally serve to reproduce existing inequalities. As socially advantaged patients are in a better position to benefit from new treatment options than others, the theory proposes that technological innovation is likely to increase health inequalities (Link and Phelan, 1995; Phelan and Link, 2005).
Lutfey and Freese (2011, 2005) have expanded the FCT by suggesting the concept of compensatory inversion to refer to processes in which resources are disproportionately distributed to the patients who need them the least. Compensatory inversion may be produced through three meta-mechanisms: spillover benefits from the actions of others in social networks, inequalities in preferences and dispositions (habitus), and the agency of social institutions, the latter being of particular importance to the present study. While health inequality researchers have often viewed the medical system as an institution that simply reproduces or mitigates existing inequalities, Lutfey and Freese (2011) argue that welfare state institutions also have the dynamic capacity to produce social stratification. Examining the social production of health care inequalities in a Norwegian setting allows for understanding how this may occur even in formally egalitarian health care systems, in a way which also may help make sense of the persistence of health inequalities in Nordic welfare states more generally. The approach taken in this study therefore seeks to explicate the practices through which medical resources are distributed, how these practices are structured by institutional and economic constraints, and how they may create or reinforce unequal outcomes.
The present article also thematizes the recent turn towards patient empowerment in Nordic health care systems (Vallgårda, 2011). Characterized by an increased emphasis on patient autonomy and self-determination, patient empowerment is often framed as a way of achieving more egalitarian doctor–patient relationships. However, empowerment policies are also motivated by economic incentives to reduce expenditures by transferring responsibility onto the individual patient (Kendall and Rogers, 2007). As such, patient empowerment may be interpreted as part of a more general Nordic trend towards increased individual responsibility as a response to economic pressures (Mik-Meyer and Villadsen, 2013). By establishing institutional expectations not all patients are equally able to meet, empowerment discourses may serve to exacerbate and justify health inequalities (Hinder and Greenhalgh, 2012). Empirical studies have demonstrated that resource scarcity may be a barrier to implementing patient empowerment in practice, leading to a practice of ‘selective empowerment’ in which health care professionals steer resources towards patients they deem most likely to succeed (Scambler et al., 2012). In the discussion, I elaborate the concept of selective empowering by specifying three logics through which patients are assessed and categorized by medical staff, and by demonstrating how these three logics may produce social inequalities in medical care.
Methods and setting
Case description
Type 1 diabetes is a long-term condition where the outcome depends heavily on the patient’s ability to self-manage, and is a typical example of the chronic conditions increasingly prevalent in contemporary health care systems (Lutfey and Freese, 2005; Mol, 2008). During the last decades, diabetes treatment has been the subject of rapid technological development. While technologies such as insulin pumps and continuous glucose monitoring (CGM) systems make diabetes management safer and more convenient, they may also increase health inequalities if they are primarily provided to motivated and resourceful patients (Franklin, 2016). Previous studies of type 1 diabetes have identified significant social inequalities in outcome, treatment and access to technology (Lutfey and Freese, 2005; Naranjo et al., 2016; Sortso et al., 2018).
Study design
The study began from the general research question of how medical staff work to distribute limited technological resources among patients, which was examined through a case study conducted at a clinic of endocrinology at a Norwegian hospital. In the Norwegian public health care system, medical technology is offered at little to no cost through a state-run prescription system. The hospital in which the case study was conducted was at the time of study one of the five largest hospitals in Norway, and served a population of several hundred thousand people largely representative of the general Norwegian population. Data were collected through observation of staff meetings where the clinic staff worked to distribute technology between patients, and in-depth interviews with staff members (n = 8). For background, I also interviewed patients with type 1 diabetes (n = 24). The period of observation began in November 2017 and ended in June 2018, during which I attended 20 meetings of approximately an hour each. During these meetings, a total of 94 patients were discussed. Meetings were typically attended by between five and 10 staff members, who collectively determined which patients to provide advanced diabetes technologies to on a case-by-case basis. Assessments would typically begin with a nurse giving a short presentation of the patient, and would end with the doctors either agreeing on an outcome or postponing the decision to a later date. While nurses would participate in the assessments, the formal authority to make the final decision lay with the doctors. Depending on the complexity of the case, a single discussion could last anywhere between two and 15 minutes. Two types of technological equipment were distributed: insulin pumps, which are semi-automated devices for delivering insulin; and continuous glucose monitoring systems (CGMs), which measure blood sugar levels at regular intervals and provide information in the form of detailed statistics and graphs. CGMs were the most expensive of the two, meaning that they were often also the subject of the most contested discussions. As CGM use has been associated with improved glycaemic control and quality of life (Rodbard, 2017), inequalities in the distribution of this technology may translate into unequal health outcomes. For this reason, the analysis will mostly focus on the distribution of CGMs.
During meetings, I initially took notes by hand and later switched to a portable computer when I felt that the staff had become more accustomed to my presence. More detailed field notes were written up immediately after the meetings ended. After the period of observation had ended, I conducted semi-structured interviews with three doctors, four nurses and one manager who were working or had previously worked at the clinic. Key themes included personal characteristics staff considered important for effectively managing type 1 diabetes, patient assessment and factors constraining their decision making. Each interview lasted between 35 and 70 minutes, and was transcribed verbatim and analysed concurrently with the observation data. Field notes and interview data were written in Norwegian, with relevant quotes translated into English by me with minor aesthetic and grammatical adjustments. The method of analysis was abductive, and was conducted with the aim of constructing theoretical insights rather than empirical generalization (Timmermans and Tavory, 2012). In cases where the staff’s accounts differed from each other and from my own impressions, I utilized a reflexive method of analysis in which I drew on previous theories and research in order to make sense of divergent meanings and interpretations (Alvesson, 2011). As the project concerns sensitive medical and personal data, I applied for and received clearance both from the Norwegian Centre for Research Data (NSD) and the Regional Committees for Medical and Health Research Ethics (REK) prior to data collection. I also refrained from transcribing names and other directly identifying details during observation.
The combination of observation and interview data provides a small but concentrated material for analysing how processes of resource distribution may contribute to the social production of health care inequalities. While several studies have examined physicians’ perceptions of patients through interview data and surveys (Higashi et al., 2013; Sointu, 2017), direct observation of medical decision-making processes allows for examining how these perceptions are produced and translated into medical practice. Furthermore, observational methods allow for examining the communicative practices medical practitioners use to reduce controversy and uncertainty in difficult situations. Observational studies of medical gatekeeping have traditionally focused on hospital emergency services, where staff usually interact with patients on a short-term basis based on a minimum amount of information (Johannessen, 2017; Lara-Millán, 2014; Roth, 1972). By contrast, the majority of the patients discussed during my observations had attended the clinic for years, which may have made the staff’s evaluations of them more nuanced than in situations with a high patient turnover. In keeping with the goal of theoretical generalization and development, quotes and examples have been selected in order to illustrate central and theoretically surprising themes in the data.
Analysis
Medical resource distribution as a contested process
At the time of observation, the staff at the diabetes clinic had no formal criteria for deciding which patients to offer CGMs and other technological equipment, which meant that every decision had to be reached through a process of deliberation. As an attempt to make technology distribution more consistent, the clinic had established weekly meetings with the purpose of reaching decisions collectively. The staff mainly assessed patients based on information from blood sugar measurements, medical journals and self-reported symptoms, as well as their impressions from direct interactions with the patient in question. While the staff aspired to treat patients as equally as possible, they often acknowledged that this was difficult to achieve in practice: Our main problem is that we don’t have formal criteria, which means that unequal treatment may happen, in large part involuntarily from our side. It may depend on our mood that day, who is present, the interaction in the group […] In clear-cut cases we’ll probably make the right decision, but sometimes we will listen more to an argument than we would at another meeting. (Physician, said during interview)
As the above exchange illustrates, the distribution of diabetes technologies was an uncertain and contested process which would occasionally trigger conflicts between staff members, particularly between doctors and nurses. During an interview, a nurse expressed that she felt that the doctors did not always treat patients fairly, and admitted that the nurses would sometimes use strategies to ensure that an application would have a higher chance of being approved (for example delaying a case until a particular doctor was absent). After a meeting, a physician took me aside and said that the nurses were more generous because they ‘didn’t always see the big picture’, and that the doctors needed to restrict expenditure by being discerning. These disagreements may stem from a division of labour in which the nurses interacted more closely with the patients than the physicians, while the latter nonetheless retained the formal power over treatment decisions. However, nurses and doctors both had to work together to make difficult decisions based on limited information, all the while being well aware of the risk that some patients would receive unfair treatment. The inherently contested and uncertain nature of their decision making should therefore be taken into account when reading the following analysis.
The contested distinction between ‘medical’ and ‘non-medical’ need
For the individual patient, the process of being considered for a CGM or an insulin pump could begin in one of two ways. The suggestion could come from a physician or a nurse, typically if the patient was pregnant or showed symptoms of complications, or the patient could request it herself. In cases where the patient herself had requested the technology, an important question for the clinic staff became whether the patient exhibited a ‘genuine’ need or not. This aligns with the common sociological argument that medical staff favour patients who make ‘legitimate’ demands over those who are perceived to seek help for trivial or non-medical problems (Roth, 1972). However, the question of what needs were ‘legitimate’ or not was often controversial. During interviews, patients generally described the CGM as an attractive treatment option, with most of them reporting that they had either applied for a CGM or were considering doing so. Some requested a CGM because they perceived the device as more convenient than other methods of blood sugar measurement (what may be described as practical need), while others thought a CGM would reduce fears and anxieties related to managing their diabetes (psychological need). Some also viewed owning a CGM as a symbolic asset distinguishing them from other patients by serving as a material representation of their ability to take control over their disease. Both practically and symbolically, therefore, patients often perceived CGMs as an empowering and limited technological resource, in some instances leading to a state of competition as they tried to ‘market’ themselves as needing and deserving candidates.
While clinic staff generally agreed that patients who wanted a CGM for practical reasons should be turned down, nurses were typically more sympathetic towards patients motivated by psychological reasons. As low blood sugar levels can lead to loss of consciousness and even death, many patients feared going into hypoglycaemia despite being ‘objectively’ at a low risk of doing so. Nurses and physicians often disagreed over whether or not such fears should be a sufficient reason for being granted a CGM, which could lead to heated discussions. This can be illustrated by a discussion regarding an elderly woman who had applied for a CGM because diabetes-related anxiety kept her from sleeping. The woman had previously worked in finance, and was described by the staff as a resourceful and slightly demanding patient. During her assessment, a physician commented that her situation sounded ‘more like a psychological issue than a medical issue. She wakes herself two or three times a night despite not having hypoglycaemia. To me it sounds like it is her personality that is the problem, and not the diabetes itself’. The patient’s nurse replied that he should try putting himself in the woman’s shoes, and that the lack of ‘objective’ risk didn’t make her fear less real. While this argument seemed to sway a second physician, the first quickly intervened: ‘In that case we would have to provide a CGM to everyone who expresses this type of fear’, noting that they had already turned down other patients who were in similar situations. Rounding off the discussion, a third physician somewhat provocatively suggested that they could all raise their hands to see who wanted to pay more taxes in order to finance more medical technology: ‘At the end of the day, that’s what it’s about. We simply don’t have the money to provide CGMs to everyone’.
Several interesting themes are present in this brief exchange. The first concerns how the first physician distinguishes between medical problems and problems arising from the patient’s ‘personality’, and the way in which the nurse troubles this distinction by noting that the fear is still ‘real’ despite having no clear medical basis. As with many other chronic conditions, type 1 diabetes profoundly shapes the daily lives of the people who have it, meaning that the distinction between the medical and the non-medical is difficult to uphold in practice. While the diabetes physicians in principle wanted to base their decisions on ‘objective’ medical indicators, they in practice often had to take the patient’s social situation and personal characteristics into account. The distinction between ‘legitimate’/medical and ‘non-legitimate’/non-medical need was therefore not fixed, but context-dependent and subject to dispute. This introduced a clear risk of unequal treatment into the decision-making process, a risk of which physicians were generally consciously aware and tried to avoid.
The second theme concerns how economic constraints are invoked as a decisive argument for turning down the application. As previously noted, nurses would often take the patient’s side against the more cost-conscious physicians. In such cases, physicians would frequently maintain that they would ideally like to provide CGMs to everyone, but that budgetary restrictions necessitated a selective policy. Rhetorically, physicians would often invoke the hospital economy as an external constraint located outside their control, forcing them to make tough prioritizations.
The third theme I want to highlight is the physician’s appeal to equality of treatment as an argument for turning the application down. The physician often mentioned that the woman had previously worked in the financial sector, and was probably better at ‘marketing’ herself than other patients with similar needs. In this case the patient’s social status arguably worked against the patient, troubling the notion that medical staff produce health inequalities by directly valuing high-status patients over others. Rather, the effect of social status is mediated by other evaluative criteria, two of which I will outline below.
Competence: Technology as an ‘investment’
As is typical for chronic conditions, physicians exert little direct control over the treatment of type 1 diabetes, but must instead rely on patients to adhere to medical recommendations and advice (Lutfey et al., 2008). An important consideration for the staff during assessments was therefore the patient’s perceived ability to follow advice and use medical technology to their benefit: ‘[The patients] have to be able to use it in a reasonable way. It is no use giving it to someone without being sure that it will be used in such a way that the need is actually covered’ (physician, said during meeting).
This criterion was particularly salient when distributing the CGM. While a CGM produces detailed information about blood sugar levels, the device does not directly affect insulin dosage, which means that the success of treatment depends on the patient’s ability to understand and apply the information produced by the device. While the clinic did offer patient education specifically directed at technology usage, the staff frequently emphasized the importance of the patient’s own efforts: ‘It is one thing to wear it, but you also have to pay attention to what it shows you’ (physician, said during meeting).
Evaluations of competence were based on information from a variety of sources. In some cases, evaluations were based on informal judgements of the patient’s personal characteristics, while in other cases physicians would let the patient use a CGM for a limited period in order to ‘test’ their abilities over time. In cases such as these, physicians expected to see results in the form of more stable blood sugar levels or a reduced HbA1c, and would often express disappointment if patients failed to deliver: ‘[She] has not used the CGM to learn. She has just done as usual’ (physician, said during meeting). The monetary cost of the device was sometimes compared directly with the lack of results, with a physician in one case commenting that ‘we won’t pay this amount of money for nothing’. In conversations such as these, staff would often refer to diabetes technology as an ‘investment’, implying that it was the patient’s responsibility to ensure the investment ‘paid off’ in terms of medical results: If you don’t use it as it is meant to be used, if you don’t utilize the advantages that insulin pumps have over insulin pens, then in many cases it won’t be worth the investment in time and resources. It can depend on [the patient’s] motivation and ability. (Physician, said during interview)
In interviews, physicians and nurses would often describe the ideal patient as structured, self-disciplined and active. Occasionally, social characteristics would enter into these descriptions as well, as when this physician used a young and highly educated woman as an example of a model patient: You can take a patient that I saw today as an example. She’s teaching at an upper secondary school, highly educated, probably has seven years of higher education in total […] She has never had keto, never had so low blood sugar that she needed help, has an HbA1c around 5.9. She’s very well regulated. (Physician, said during interview)
Compliance: technology as a reward
Compliance may be defined as the patient’s perceived willingness to adhere to medical advice, and implies a moral judgement of the patient’s behaviour. Compliance is an established medical term, and would as such occasionally be referenced explicitly by staff. More often than not, however, the concept functioned as an implicit norm informing the staff’s decision making. There was a general agreement among staff that patients who had demonstrated their willingness to adhere to advice and prescriptions in the past were more ‘worthy’ of receiving CGM technology than those who had not. The clinic staff were generally hesitant to provide technologies to patients they perceived as unmotivated, careless or non-adherent: ‘The fact that they neglect the disease because they don’t care can’t be a sufficient reason to get a CGM. In that case, everyone would have to get one’ (physician, said during meeting). When assessing a patient who was ultimately refused a CGM, a physician commented that the patient ‘hadn’t made a serious attempt at measuring his blood sugar in the normal way’, implying that the device should be provided as a last resort for patients who had demonstrated their willingness to try other and more basic treatment options. In some cases, compliance seemed to be more important than competence when distinguishing ‘worthy’ from ‘unworthy’ patients. A woman who had applied for a CGM was introduced by a nurse as being ‘too well regulated’, and as under the impression that she expected to get a CGM because she was so competent at managing her disease. The physician replied that if the woman was really that competent, she ‘should have taken our advice’, suggesting that the patient had a record of non-compliance. In the end, a physician decided to offer the patient an insulin pump, but to withhold the more expensive CGM sensor: ‘She can get the pump, but if she wants a sensor, she has to listen to the advice we’re giving her’.
While the clinic staff often spoke of technologies as investments when evaluating competence, they would often refer to the technology as a reward when assessing compliance. The CGM in particular was a coveted device among patients, something of which the clinic staff were well aware. During a discussion of a patient who had experienced a loss of consciousness after failing to measure his blood sugar levels, a physician questioned whether they should ‘reward him for not measuring’. In another instance, a physician commented that taking the CGM away when it was no longer necessary ‘felt like punishment’. In cases such as these, the control over technological resources functioned as a tool through which staff could enforce specific norms of patienthood by rewarding and punishing certain forms of behaviour, arguably entrenching and legitimating inequalities between patient groups.
Hospital budgets and the medical technology market as constraints on medical decision making
Economic considerations played an important role in patient assessment and technology distribution at the diabetes clinic. In interviews, clinic staff tended to downplay the role of budgetary constraints, often stating that there was no real limit as to how many CGMs they could provide. However, many expressed the sentiment that restricting health expenditures was an important value in itself: ‘We are encouraged to be frugal, and to use our money where it can do the most good’ (physician, said during interview). However, budgetary restrictions were a key concern during meetings. One meeting began with the head doctor informing the rest of the staff that the diabetes clinic had exceeded its budget two months in a row due to expenditures on CGMs and insulin pumps. On another occasion, the head doctor presented the newly negotiated prices for the varying technologies offered by the clinic, and encouraged the staff to keep the numbers in mind going forward.
During discussions staff would frequently weigh medical benefits against economic cost, suggesting that restricting expenditure was an important motivation. As previously noted, the patients interviewed for this study generally viewed insulin pumps and CGMs as attractive treatment options, and many would stay updated on technological development in diabetes care through social media, news coverage or member magazines distributed by the Norwegian Diabetes Association. A common perception among staff was that technological development made patients more demanding: ‘Sometimes I feel like the patients come here like they would come into a store. They just point at what they want. “Do you have any new equipment?”’ (nurse, said during meeting).
The staff also expressed worries regarding rising treatment costs, which they often attributed to their increasing dependency on medical technologies:
‘Let me put this into perspective for you. If we were to provide a CGM to all 27,000 people with type 1 diabetes in Norway, it would amount to 1.2 billion a year. That tells you something about the extreme expenses we’re looking at here’.
‘I think that we’re already up to half a billion a year. Prognoses show that it may double in the future’.
‘It is absolutely insane’.
As a result of increased patient demand and treatment costs, the clinic’s expenditure on technology routinely exceeded its annual budget. While most staff members expected that these expenditures would only increase in the future, they still wanted to retain control by distributing resources selectively and prudently. Interestingly, the main expense related to the CGM was not the actual hardware, but glucose sensors that needed to be replaced every one or two weeks in order to keep the device in operation. As these sensors were also provided by the Norwegian health service, providing a patient with a CGM on a permanent basis was not a one-time expenditure, but involved committing to an annual expense for an indefinite amount of time. For that reason, the staff generally preferred to provide the CGM for a limited time in order to see whether the investment would ‘pay off’ in terms of altered self-management and improved medical results.
Economic constraints arose not only from budgetary restraints within the Norwegian health care system, but also from developments in the global diabetes technology market. The staff frequently expressed scepticism towards the private corporations who produced the diabetes technologies, whom they perceived as primarily motivated by profit: ‘They are more interested in selling than in documenting results’ (physician, said during meeting). Staff members also argued that the prices of technological equipment were being artificially inflated by the companies selling them. After a particularly heated meeting, a physician took me aside and commented that ‘the technology companies act as if they’re concerned with the patients’ well-being, but all they really care about is the bottom line – do not have any illusions about this’. Occasionally, staff would express feelings of powerlessness: ‘We can say what we want, but the companies don’t care what we in Norway think. They care about the global market’ (nurse, said during meeting). In particular, the clinic staff were concerned about what they perceived as a development towards monopolization in the diabetes technology market, which resulted in higher prices and fewer treatment options. This exchange from a longer discussion during a meeting may serve as a general illustration of these concerns:
‘The equipment should be a lot cheaper. The companies are speculating in keeping prices high because they want to make money’.
‘There’s not enough competition’.
‘They’re buying each other up. The small companies give up, and in the end two or three companies are controlling the entire market’.
When the Animas Corporation, a company specializing in making insulin pumps, exited the market in October 2017, this monopolization impacted the staff’s decision making directly. Discussing the news some weeks later, the staff found that they were faced with a dilemma: should they continue to offer the Animas pumps to patients, knowing that they would soon go obsolete, or should they cut their losses and store the remaining supply? While the staff did not arrive at a clear decision, this dilemma illustrates how the availability of medical resources is not only determined by budgetary restraints within the health care system, but also by the market conditions under which medical technologies and supplies are commercially produced.
The three logics of selective empowering
In this article, I have demonstrated how the distribution of medical technologies at a Norwegian hospital was shaped by an economy of eligibility that rewarded competent and compliant patients. The moral economy created as a result of these practices may be interpreted in light of the emergence of patient empowerment as a treatment ideology in Nordic health care systems. While patient empowerment is often framed as a challenge to medical paternalism, it also aims to reduce health care expenditures by pushing patients to take more responsibility for their own health and treatment (Kendall and Rogers, 2007). Genuine empowerment is dependent on access to resources, meaning that the power to empower individual patients will effectively lie with health care professionals and other actors that control medical technologies and other limited assets. In their study of patient empowerment in diabetes care, Scambler and colleagues (2012) proposed the term ‘selective empowerment’ for the practice in which medical professionals steer resources towards the patients they deem most likely to succeed. In the following, I will elaborate and refine this concept by proposing three logics of selective empowering: a logic where resources are employed as solutions for medical problems according to distinctions between legitimate and non-legitimate need; a logic of competence where medical staff invest resources in the patients who are most likely to succeed; and the logic of compliance, in which medical staff use resources in order to reward and punish certain forms of patient behaviour. These three logics are presented schematically in Table 1.
The three logics of selective empowering.
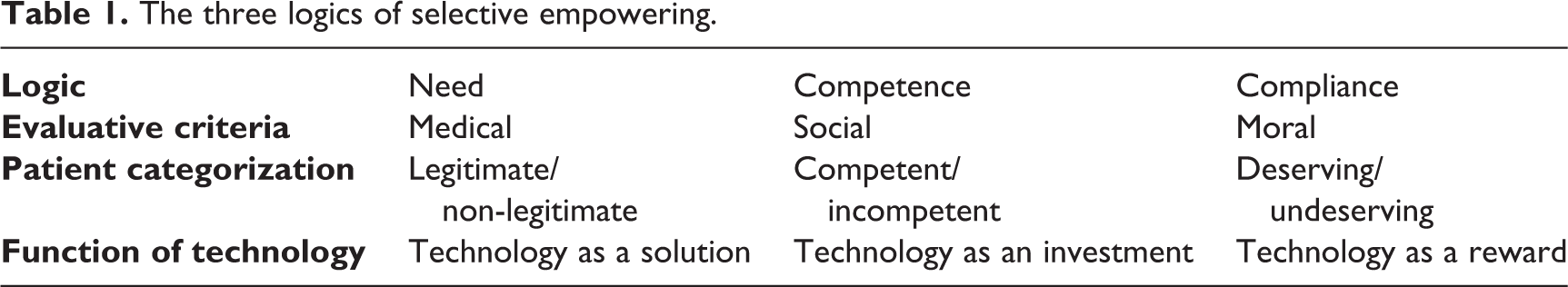
In my formulation of the concept, selective empowering may be defined as a communicative practice in which medical professionals simultaneously draw on, reproduce and transform a set of normative expectations in order to distribute limited resources of various kinds. As I have demonstrated, this practice is uncertain and often controversial, and is both enabled and constrained by structural factors operating outside the medical professionals’ control. It is therefore important to emphasize that the logics outlined above should not be interpreted as a static formula that medical professionals simply apply to individual patients, but as emerging from the practice of distributing medical technologies and other medical resources.
Arguably, all three logics of selective empowerment may contribute to the social production of health care inequalities. While the logic of need appears as the least discriminatory of the three, evidence that patient–physician communication is influenced by social class shows that the ability to effectively communicate medical needs may vary between patient groups (Starfield et al., 2012; Verlinde et al., 2012). Furthermore, the analysis suggests that the distinction between legitimate and non-legitimate need is fleeting and shaped by economic concerns, and is difficult to uphold in practice. Secondly, the logic of competence privileges those who are already most adept at managing their disease, introducing a social component into medical decision making. Since the ability and motivation to adhere to medical recommendations may vary according to social position, even ‘neutral’ assessments of competence may serve to entrench and justify inequalities in access. As I have demonstrated, medical staff frequently operated under the assumption that higher-educated patients were generally better at self-managing, suggesting an at least tacit awareness of this dynamic. Finally, the logic of compliance highlights how the control over technological resources functions to maintain a moral economy that distinguishes between deserving and undeserving patients, a moral distinction which is often profoundly influenced by social hierarchies of status and power (Willen, 2012). Collectively, these logics may contribute to producing a situation in which technological resources flow towards already advantaged patients. While this is a topic for empirical examination, the concept of selective empowering may also be useful for studying social inequality and resource distribution in other welfare state institutions.
Previous studies of social categorization and resource distribution in medical care have often focused on the cognitive dispositions of medical actors rather than the structural context of medical decision making (Spencer and Grace, 2016). As important as the unconscious stereotypes and normative values of individual actors are, social evaluations are also profoundly shaped by the situations in which they occur. Contrary to theories that mainly see health care inequalities as the product of habitual and non-purposeful action (see for example Shim, 2010), I specifically highlight the importance of structural factors, primarily budgetary restraints, increased demand from patients, technological dependency and a tendency towards monopolization in the global diabetes technology market. While technological control has traditionally been conceived as a central component of medical professionalism (Freidson, 1988: 45), the analysis demonstrates that the relationship between medical technology and medical power is complex and often fraught. For the staff at the diabetes clinic, CGMs were simultaneously a solution to a medical problem, a means for rewarding and punishing certain forms of behaviour, and a limited resource where treatment results needed to be weighed against economic cost. Here it may be argued that the clinic staff confronted a basic tension between the use value of medical technologies as remedies and their status as commodities produced for profit by commercial manufacturers. The increasing importance of medical technology increased this tension, as the medical workers became more dependent on commercial firms operating outside the medical setting. Other contributory factors included increased patient demand for technologies and the tendency towards market concentration in the diabetes technology market, which increased costs while reducing the number of available treatment options. The staff’s expressions of powerlessness over this development illustrate how the technologization of treatment makes patients and medical professionals alike more dependent on commercial manufacturers and the market fluctuations of health-tech capitalism, including in formally de-commodified health care systems.
In their ethnographic study of diabetes treatment, Lutfey and Freese (2005) identified a dynamic of compensatory inversion in which resources were disproportionately given to patients who needed them the least. Similarly, Link and Milcarek (1980) warned against a Matthew effect in which medical resources were steered towards more motivated, communicative and competent patients rather than to the most needy. While these studies were conducted in the predominantly private-sector US health system, this article suggests that compensatory inversion may also occur in social-democratic health care systems in which patients formally have equal access to care. Specifically, unequal treatment is likely to occur if medical resources are distributed according to medical, social and moral criteria that reward competent, compliant and already successful patients. The concept of selective empowering contributes to our understanding of this process by specifying three logics of institutional stratification, and by emphasizing how the agency of social institutions is shaped and conditioned by external constraints. Going forward, more attention should be paid to how these constraints structure the social evaluation and categorization of patients, and how unequal treatment may arise from the complex interaction between technological development, resource inequalities and medical decision making.
Footnotes
Acknowledgements
The author wishes to thank Elias Nosrati, Terje A Eikemo, Aksel Tjora and Sigrid Strømmen for their valuable insights and comments on previous versions of the manuscript.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This publication is supported by a grant awarded by the Norwegian Research Council (Project No. 288638) to the Center for Global Health Inequalities Research (CHAIN) at the Norwegian University for Science and Technology (NTNU).
