Abstract
Endocannabinoids are involved in the modulation of pain and hyperalgesia. In this study we investigated the role of the endocannabinoid system in the migraine model based on nitroglycerin-induced hyperalgesia in the rat. Male rats were injected with nitroglycerin (10 mg/kg, i.p.) or vehicle and sacrificed 4 h later. The medulla, the mesencephalon and the hypothalamus were dissected out and utilized for the evaluation of activity of fatty acid amide hydrolase (that degrades the endocannabinoid anandamide), monoacylglycerol lipase (that degrades the endocannabinoid 2-arachidonoylglycerol), and binding sites specific for cannabinoid (CB) receptors. The findings obtained show that nitroglycerin-induced hyperalgesia is associated with increased activity of both hydrolases and increased density of CB binding sites in the mesencephalon. In the hypothalamus we observed an increase in the activity of fatty acid amide hydrolase associated with an increase in density of CB binding sites, while in the medulla only the activity of fatty acid amide hydrolase was increased. Anandamide also proved effective in preventing nitroglycerin-induced activation (c-Fos) of neurons in the nucleus trigeminalis caudalis. These data strongly support the involvement of the endocannabinoid system in the modulation of nitroglycerin-induced hyperalgesia, and, possibly, in the pathophysiological mechanisms of migraine.
Introduction
The endocannabinoid system has been demonstrated to be tonically active in several pathological conditions. Alterations of endocannabinoid levels have been found in animal models of pain, neurological diseases and inflammatory conditions (1,2). Endocannabinoids can induce antinociceptive effects in models of acute or chronic pain through type-1 cannabinoid (CB1) receptors located on neurons, both within and outside the brain and spinal cord (3). In a recent study, it was reported that anandamide [N-arachidonoylethanolamine (AEA)], an endogenous ligand of CB receptors, is capable of inhibiting neurogenic dural vasodilation induced by calcitonin gene-related peptide (CGRP) or nitric oxide (NO) in an animal model of migraine (4). Conversely, an increase of AEA degradation was seen in platelets of migrainous women, therefore providing an additional biochemical explanation for a higher prevalence of migraine in women than in men (5). Systemic administration of the NO donor nitroglycerin (NTG) has been used extensively as an animal model of migraine pain because NTG provokes spontaneous-like migraine attacks in migraine sufferers, and induces a condition of hyperalgesia in the rat through the activation of spinal and brain structures involved in nociception (6,7). In the brain, endocannabinoids may function as retrograde messengers to modulate neuronal physiology of presynaptic CB1 receptors (8,9). AEA is mainly metabolized by fatty acid amide hydrolase (FAAH) (10), whereas 2-arachidonoylglycerol (2-AG), another endogenous agonist of CB receptors, is mainly metabolized by monoacylglycerol lipase (MAGL) (11). Additionally, both endocannabinoids may be metabolized by type-2 cyclooxygenase (12). Endocannabinoids distribution does not seem to match exactly that of CB binding sites (13), therefore suggesting either that these compounds are not essentially produced near their molecular targets, or that they may play functional roles in addition to the activation of CB receptors.
In order to elucidate further the role of endocannabinoids in migraine, we investigated the changes in the biochemical mediators degrading endogenous cannabinoids, as well as the density of sites that bind endocannabinoids in specific areas of the rat brain in the migraine model based on NTG-induced hyperalgesia in the rat. In addition, in order to better contextualize these data within the pathophysiological mechanisms underlying cephalic pain, we also evaluated the effect of AEA on NTG-induced expression of c-Fos protein in the nucleus trigeminal caudalis (NTC), a pivotal area for the modulation of nociceptive processing in the cranial region.
Materials and methods
Experimental groups
Adult male Sprague-Dawley rats weighing 180–220 g were used in the present investigation. The Helsinki declaration and the International Association for the Study of Pain's guidelines for pain research in animals (1983) were followed. Rats were housed in plastic boxes in groups of three with water and food available ad libitum and were kept on a 12 : 12 h light–dark cycle. All animals were acclimatized for 2 h before treatment. Rats were subdivided into two groups formed by four to six animals each and were treated with 10 mg/kg of NTG (NTG group) or vehicle (Control group), and were sacrificed 4 h later by decapitation. Medulla, mesencephalon and hypothalamus were dissected out and utilized for biochemical analyses (14,15). Two additional groups of animals were treated with NTG or vehicle and utilized for immunohistochemical staining of c-Fos protein in the medulla (see below). Finally, two groups of animals were treated with NTG or vehicle and injected with 1% formalin (100 µl, intraplantar) 4 h later, to confirm the longlasting hyperalgesic state induced by NTG in rats. Total number of flinches/shakes were counted for 1-min periods from 1 to 5 min (Phase I) and, subsequently, for 1-min periods at 5-min intervals during the following 10–60 min (Phase II) after formalin injection (16).
Reagents
The synthetic cannabinoid 5-(1,10-dimethyheptyl)-2-[1R,5R-hydroxy-2R-(3-hydroxypropyl)-cyclohexyl]phenol (CP55.940) was purchased from Sigma Chemical Co. (St Louis, MO, USA). [3H]2-Oleoylglycerol ([3H]2-OG, 20 Ci/mmol) was from ARC (St Louis, MO, USA). [3H]AEA (205 Ci/mmol) and 3H-CP55.940 (126 Ci/mmol) were purchased from Perkin Elmer Life Sciences (Boston, MA, USA).
Enzyme assays
The hydrolysis of AEA by FAAH in tissue homogenates was assessed by measuring the release of 3H-arachidonic acid from 10 µM 3H-AEA, through reverse-phase high-performance liquid chromatography, as reported (14,15). MAGL activity was assayed in supernatants from tissue homogenates, obtained at 39 000 g and incubated with 10 µM 3H-2-OG at 37°C for 30 min (11). The reaction was stopped with a mixture of chloroform/methanol (2 : 1, v/v), and the release of 3H-glycerol in the aqueous phase was measured in a β-counter (Perkin Elmer Life Sciences). Both FAAH and MAGL activities were expressed as pmol product per min per mg protein.
Binding to cannabinoid receptors
For CB binding studies, membrane fractions were prepared from cerebral area extracts as reported (14,15), quickly frozen in liquid nitrogen and stored at −80°C for no longer than 1 week. These membrane fractions were used in rapid filtration assays with the synthetic cannabinoid 3H-CP55.940 (400 pM), as described previously (14,15). Unspecific binding to CB receptors was assessed in the presence of 1 µM ‘cold’ agonist (14,15). Receptor binding was expressed as fmol 3H-agonist bound per mg protein.
Immunohistochemistry
Anandamide (Sigma), suspended in 4% Tween 80, was injected intraperitoneally at a dose of 20 mg/kg. Male Sprague-Dawley rats were injected with systemic AEA 30 min before NTG administration or vehicle and sacrificed 4 h later. Animals were anaesthetized and perfused transcardially with saline and 270 ml of ice-cold 4% paraformaldehyde 4 h after NTG/saline administration. Brainstems were removed, post-fixed for 12 h in the same fixative and subsequently transferred in solutions of sucrose at increasing concentrations (up to 30%) during the following 72 h. Brains were cut at 50 µm on a freezing sliding microtome. c-Fos expression in the rat brain was detected by means of the immunohistochemical technique with a rabbit polyclonal antiserum directed against c-Fos protein (residues 4–17 of human c-Fos). Tissue sections were incubated for 48 h at 4°C with the c-Fos antibody (Oncogene, Cambridge, MA, USA). After thorough rinsing in buffer, sections were processed with the avidin–biotin technique, using a commercial kit. Cells positively stained for c-Fos were visualized with nickel-intensified 3′,3′-diaminobenzidine tetrahydrochloride. After staining, sections were rinsed in buffer, mounted onto glass slides, air-dried and coverslipped.
Statistical evaluation
Comparisons between groups were carried out using Student's t-test for independent samples and the minimum level of statistical significance was set at P < 0.05. For c-Fos expression, cell counts in the NTC were made from every sixth section throughout the rostrocaudal extent of the nucleus for each rat and its control. In order to avoid differences related to the asymmetrical sectioning of the brain, c-Fos+ cells were counted bilaterally (three sections for each nucleus) (Scion Image Analysis) and the mean value obtained from the two sides was used for the statistical analysis. Student's t-test for unpaired data was used to compare differences in the mean number of c-Fos-immunoreactive nuclei per cell group between controls and treatment groups. A probability level < 5% was regarded as significant.
Results
Confirmation of NTG-induced hyperalgesia
In the vehicle group, the injection of formalin resulted in a highly reliable, typical, biphasic pattern of flinches/shakes of the injected paw, being characterized by an initial acute phase of nociception within the first 5 min, followed by a prolonged tonic response from 15 to 60 min after formalin injection. In keeping with previous observations (17), NTG induced a significant hyperalgesic state that could be detected as an increase in the total number of flinches/shakes in Phase II of the formalin test (Figure 1), to suggest that NTG-induced hyperalgesia is mediated by central (spinal or supraspinal) neuromodulatory mechanisms, rather than by peripheral and purely chemical mechanism.
Hyperalgesic effect of nitroglycerin (NTG4h) at the formalin test. Histograms represent the total number of flinches and shakes in Phase I (a) and II (b) of formalin test and show that NTG induces hyperalgesia during Phase II of the test. Data are expressed as mean ± 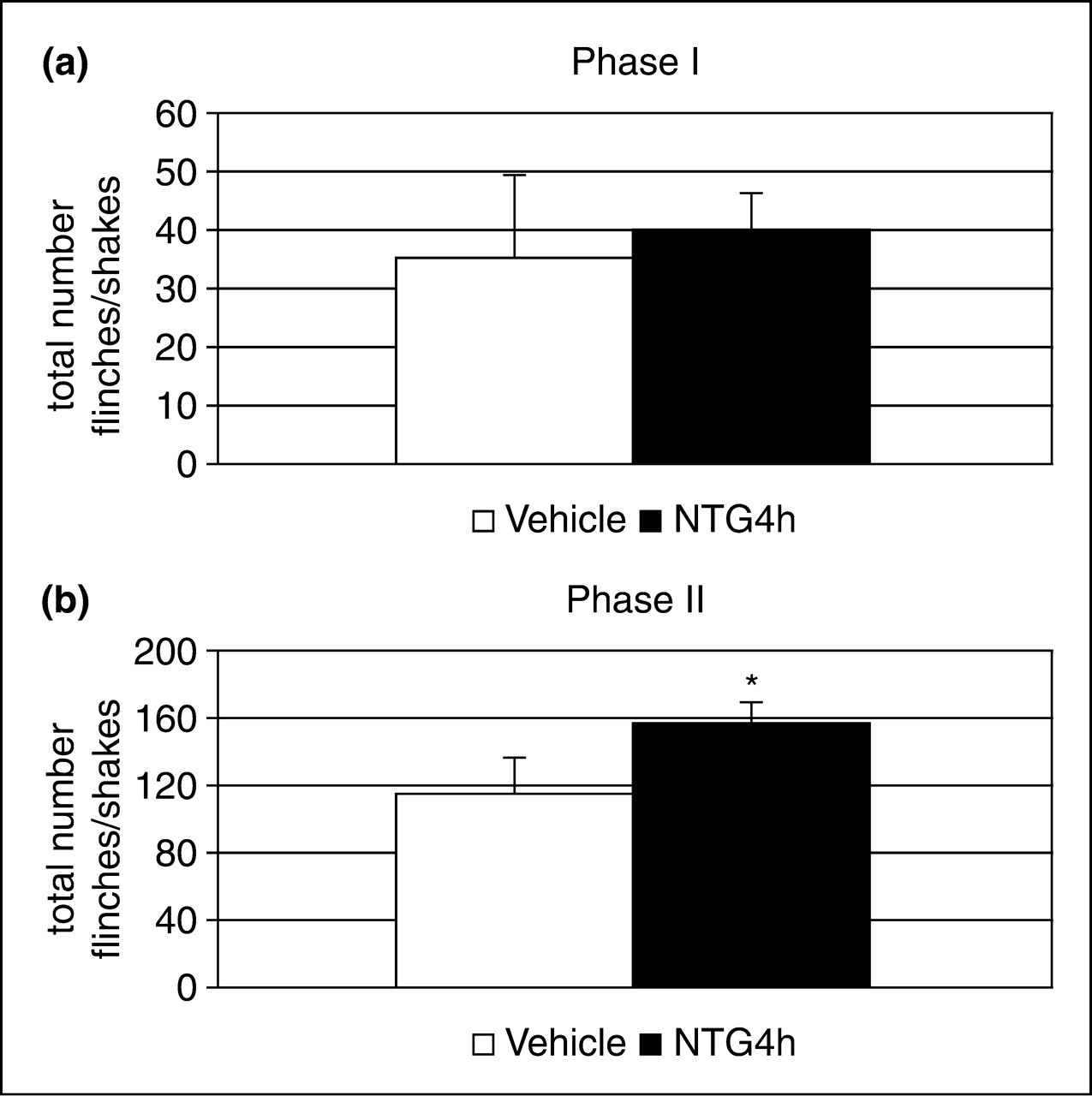
FAAH and MAGL activity
Activity of fatty acid amide hydrolase (FAAH), and of monoacylglycerol lipase (MAGL) in selected cerebral areas of rats

P < 0.05 vs. control group.
Substrate was 10 µ
Substrate was 10 µ
Data are expressed as mean ± standard deviation of four animals (pmol min−1 mg−1 protein).
CB receptor binding
The increase in enzymatic activity was associated with a significant increase of 3H-CB receptor binding (Figure 2) in the mesencephalon and in the hypothalamus, whereas no significant change was detected in the medulla.
Binding of 400 p
c-Fos expression in the nucleus trigeminal is caudalis
In agreement with our previous findings (18,19), NTG administration induced an increase in c-Fos expression in the NTC. Pretreatment with AEA significantly inhibited NTG-induced c-Fos expression in this area (Figure 3).
c-Fos expression in the nucleus trigeminalis caudalis and its modulation by anandamide treatment. (a) Number of Fos-positive neurons in the group of animals treated with nitroglycerin (NTG4h) or with vehicle (CT) or with anandamide 30 min before nitroglycerin (AEA+NTG). *P < 0.05 vs. NTG4h. (b) Micrographs of representative sections of the nucleus trigeminalis caudalis of rats treated with nitroglycerin (left) or pretreated with anandamide (right) before receiving nitroglycerin.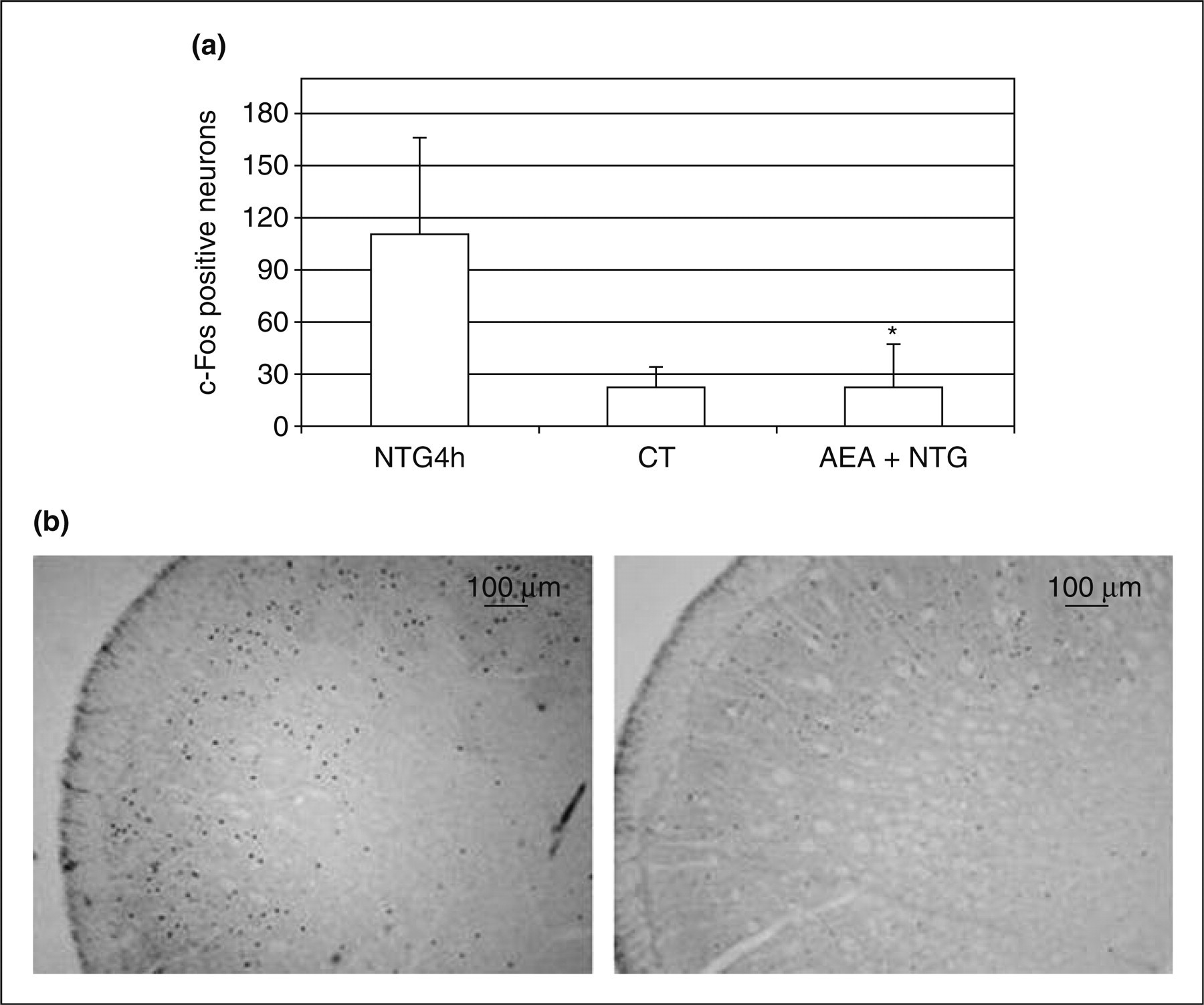
Discussion
Migraine is a disabling neurological disorder that involves the activation of the trigeminovascular system. NTG administration induces a spontaneous-like migraine attack, with a latency of several hours, and in rat it activates specific cerebral nuclei via the intervention of selected neurotransmitters and neuromediators (17–20). Experimental evidence has shown the antinociceptive action of endocannabinoids and their role in the modulation of trigeminovascular system activation (21). Recently, it was found that AEA and 2-AG levels in platelets are significantly lower in patients with chronic migraine compared with control subjects (22), therefore suggesting a dysfunction of the endocannabinoid system in this disorder.
Endocannabinoids, indeed, exert a critical control on cerebrovascular tone, by interacting with serotonergic transmission, NO production, and CGRP release (3). CB1 receptors seem to be involved in the NO/CGRP cross-talk, which causes headache and dural blood vessel dilation (4). Additionally, endocannabinoids may inhibit 5-HT2A serotonin receptors, which might make them suitable for the preventive treatment of migraine (23).
CB1 receptors are located in central and peripheral nerve terminals and may regulate the release of both excitatory and inhibitory neurotransmitters when activated (24). In the case of primary sensory neurons, CB1 receptor activation reduces the pathological pain sensation (25–27). In addition to the major role of brain CB1 receptors, there is recent evidence implicating also type-2 cannabinoid (CB2) receptors in the antihyperalgesic activity of cannabinoids in models of acute and chronic, neuropathic pain, especially of inflammatory origin (28).
In this study, we have reported significant changes in the endocannabinoid system in the brainstem and hypothalamus of rat following NTG administration, which induces hyperalgesia and c-Fos expression in the NTC and which was adopted as an experimental model of migraine.
Medulla
In this region, NTG induced a significant increase of FAAH activity, which is indicative of a reduction of AEA levels in this area, associated with an increase in the density of CB binding sites.
It is known that NTG activates brainstem areas implicated in nociception and autonomic functions (17–19). The medulla is the area that contains NTC, one of the most important relay stations for pain transmission in the cephalic area: the observed changes in FAAH, compared with the stability of MAGL, seem to suggest that AEA, rather than 2-AG, is the endocannabinoid more likely to be implicated in the modulation of pain originating in the cephalic area. In agreement with this interpretation, AEA proved to act as an important negative modulator of pain transmission in the superficial layer of NTC, as shown by the reduction that AEA provoked in NTG-induced c-Fos expression in this area. AEA possesses vasodilator activity and it has been identified also in endothelial cells, confirming its potential role in the modulation of the vascular system (29,30). Furthermore, AEA reduces hyperalgesia and inflammation via inhibition of CGRP release in capsaicin-activated nerve terminals (25). Akerman et al. (4) have reported that AEA may act both presynaptically, to prevent CGRP release from trigeminal sensory fibres, and postsynaptically, to inhibit CGRP-induced NO release in the smooth muscle of dural arteries. We have shown that NTG administration induces a sustained (up to 4 h) decrease in CGRP immunoreactivity in NTC, thus suggesting a release of neuropeptide and an important role in the development of pain and hyperalgesia (31). CB1 receptors are localized on fibres in the spinal trigeminal tract and spinal NTC (32). The activation of CB1 receptors in trigeminal neurons after pretreatment with AEA (33) could be responsible for the inhibition of CGRP release from central terminals of primary afferent fibres, therefore reducing NTG-induced c-Fos expression. Against this background, we can hypothesize that the observed increase in FAAH levels in this area may be secondary to the release of AEA in response to NTG-induced CGRP release and hyperalgesia.
Mesencephalon
In the mesencephalon, NTG increased FAAH and MAGL activities, suggesting a reduction in the endogenous levels of both AEA and 2-AG. In fact, an inverse relationship between FAAH activity and AEA levels has been demonstrated in various cells and tissues (34). In line with this, several studies have confirmed the importance of a physiological role for 2-AG and AEA in suppressing pain, suggesting that FAAH and MAGL inhibitors may represent novel therapeutic tools for the treatment of diverse pain disorders by increasing the bioavailability of endogenous cannabinoids (35–37). Previous studies have shown that in the periaqueductal grey, a mesencephalic nucleus important for nociception and a putative migraine generator, endocannabinoid concentrations increase in response to peripheral inflammation (38,39). In the present study, we have reported that the increase of FAAH and MAGL in the mesencephalic area is accompanied by an increase in the density of CB binding sites. Petrosino et al. (40) have previously shown that AEA and 2-AG, operating at both spinal and supraspinal levels, are up-regulated during chronic constriction injury of the sciatic nerve, probably to inhibit pain. In a recent study, it was shown that CB1 receptors are up-regulated in dorsal root ganglion after the development of neuropathic pain (41), and that sciatic nerve injury induces CB1 up-regulation in the spinal cord partly mediated through tyrosine kinase receptors and the mitogen-activated protein kinase (42). Similarly, we can hypothesize that the observed up-regulation of CB binding sites during NTG-induced hyperalgesia is a compensatory mechanism to counteract the reduction of endocannabinoid levels that are released in response to the NTG-induced alteration of the nociceptive system.
Hypothalamus
The hypothalamus is known to modulate different functions and is probably involved in the pathophysiology of a variety of primary headaches, including cluster headache and chronic migraine (43). Recently, it was reported that during the headaches there is significant neuronal activation in the midbrain and pons, but also in the hypothalamus (44).
In the present study, up-regulation of CB binding sites and a significant increase of FAAH activity were found in the hypothalamus following NTG administration, whereas no change in the activity of MAGL was observed. In analogy with the findings obtained in the medulla, AEA emerged as the endocannabinoid involved in NTG-mediated changes, whereas 2-AG did not seem to play any significant role. Anatomical evidence supports the existence of synergistic interactions between the endocannabinoid system and NO in this area. Indeed, experimental evidence suggests a complex functional relationship between NO and hypothalamic–pituitary–adrenal (HPA) axis (45,46). Stress and headache are closely related through multiple ways (47). Nitric oxide synthase-positive neurons in the hypothalamic nucleus express CB1 receptor, confirming that NO and the endocannabinoid system are functionally linked (48). NO formation increases in the hypothalamus following systemically administered NTG, thus facilitating central sympathetic functions (49). NO released/produced by NTG could induce HPA axis activation causing indirectly CB1 up-regulation, as an endogenous defence mechanism of modulation (50).
In conclusion, the findings of this study univocally support a role for AEA and, to a lesser extent, for 2-AG in the modulation of NTG-induced hyperalgesia. Studies are presently underway for evaluating the antinociceptive/antihyperalgesic activity of FAAH and MAGL inhibitors, which may hopefully contribute to identify novel therapeutic targets and tools for the treatment of migraine. The inconsistent pattern observed as regards CB binding densities may depend on differences in terms of affinity in the medulla. Further studies are needed with full characterization of the receptor binding properties with increasing concentrations of ligand.
Footnotes
Acknowledgements
This investigation was supported by a grant of the Italian Ministry of Health (RC 06-07) to R.G., G.S., G.N. and C.T., by the Italian Ministry of University and Research (FIRB 2006), and by Fondazione TERCAS (Research Programs 2004 and 2005) to M.M.
