Abstract

Dear Sir I have read with interest the article of N-F. Chi et al. on ‘Transtentorial herniation with cerebral infarction and duret haemorrhage in a patient with spontaneous intracranial hypotension’ (1).
We have observed 50 cases of patients with spontaneous intracranial hypotension (SIH), 22 of whom were treated with epidural blood patch (EBP) with recovery.
One patient was affected by SIH resulting in coma. Initially this patient developed acute, severe, diffuse, orthostatic headache with nausea and vomiting. After 15 days he became progressively obtunded. Brain computed tomography (CT) scan revealed mild bilateral chronic subdural haematomas (BCSE) without mass effect and increased attenuation in the sylvian fissures; cerebral angiography was normal. He was admitted to the Neurosurgery Department and underwent an evacuation of BCSE because these were considered the cause of obtunding. Two days later the patient progressively became comatose (GCS: 5 state), showed respiratory distress and was intubated for 10 h. He developed two similar episodes with intubation the 3 and 6 days after the operation.
Finally, 12 days after the operation, brain magnetic resonance imaging (MRI) with gadolinium was performed, which showed diffuse pachymeningeal enhancement, obliteration of the basilar cisterns and descent of midbrain structures (Fig. 1). These features were considered to be consistent with SIH and severe resultant diencephalic compression. Spinal and myelo-MRI failed to demonstrate a cerebrospinal fluid leak. He was placed in the Trendelenburg position (TP) at about 30° and awoke within 8 h. The next day (14 days after the operation) the patient underwent a lumbar autologous EBP with 35 cm3 of blood mixed with 1 ml of gadolinium, but spinal MRI post EBP showed that only a small quantity of blood went into the epidural space at the L5–S1 level, whereas considerable blood was localized into the paraspinal musculature (Fig. 2). The patient was kept in a 30° Trendelenburg position during the EBP and for the subsequent 24 h. Twenty-four hours after EBP, when he was sitting on the bed, he again became stuporous and inattentive. Another EBP was therefore given under fluoroscopy guidance with 30 cm3 of blood mixed with iodinated contrast medium. A multislice spiral spinal CT scan post EBP showed small quatities of air in the epidural space from L3 to D8 level and only a small quantity of blood mixed with iodinated contrast medium in the lumbar epidural space. He progressively improved over the next 15 days. He then became progressively stuporous again, aesthenic, and was affected by disphagia. Twenty-seven days after the second EBP, another EBP in TP was performed with 30 cm3 of blood mixed with iodinated contrast medium. A multislice spiral spinal CT scan post EBP showed blood mixed with iodinated contrast medium in the epidural space from L3 to C7–D1 level. After 24 h the headache disappeared and he progressively improved. BCSE were resolved completely after the first surgery. Brain MRI was normal after 4 months. After 6 months' follow-up the patient was in good health.

Sagittal T2-weighted brain magnetic resonance imaging shows obliteration of the basilar cisterns, enlargement of the pituitary gland, flattening of the pons and descent of brainstem and cerebellum.
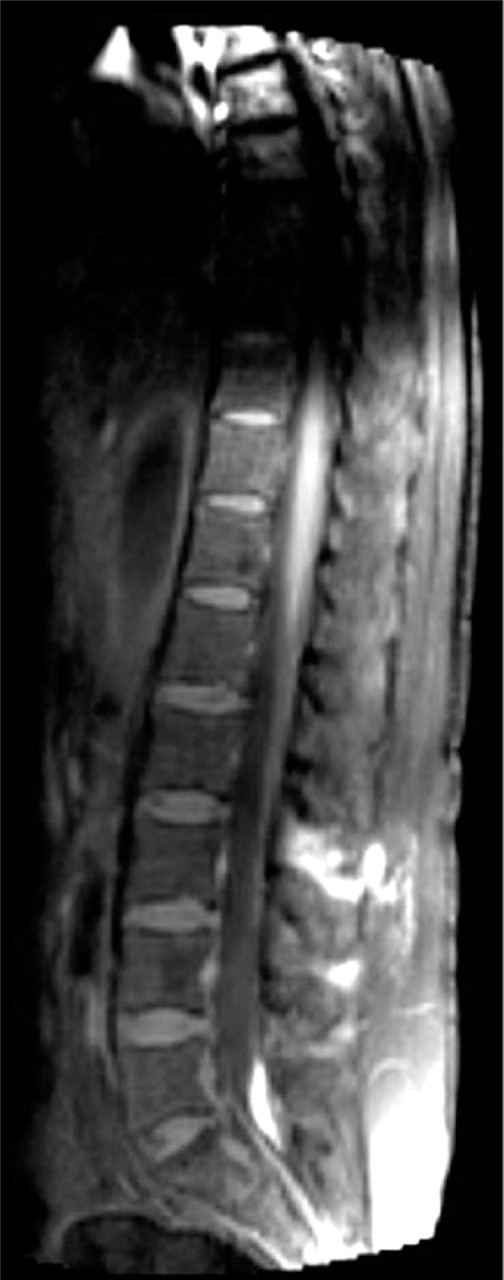
Sagittal T1-weighted postepidural blood patch spinal magnetic resonance imaging shows high signal with the gadolinium mixed with epidural blood patch in the paraspinal muscolature at the L2–S1 level and only a little quantity of blood in the epidural space at the L5–S1 level.
Our case suggests that placing a patient with rostrocaudal herniation by SIH in TP can be life saving and that the TP can favour the spread of blood into the epidural space from the lumbar to cervico-dorsal level (2). Furthermore, it shows that EBP is very effective in treating cases of SIH resulting in coma. It can sometimes appear ineffective because of the incorrect execution of this procedure, as shown in our case by neuroimmaging examinations after the first and second EBP. It is therefore necessary to perform a neuroimmaging examination post EBP to confirm the correct execution of EBP.
Our case suggests some questions for the authors: did they perform a neuroimaging examination post EBP to show the correct injection of blood in the epidural space? did they perform EBP under radiographic guidance?
I think that in N-F. Chi's case report the first EBP was probably ineffective because of incorrect injection of blood into the epidural space.
