Abstract
The present study was undertaken to elucidate the role of circulating neutrophils if any in oxidative stress in migraine by evaluating free radical generation and activities of enzymatic antioxidants in the blood in 55 patients with migraine and 60 healthy controls. Free radical generation was assessed by flow cytometry, while activity of catalase, superoxide dismutase (SOD) and glutathione peroxidase (GPx) was estimated in blood polymorphonuclear neutrophils (PMNs) by standard procedures. Platelet SOD was also measured. No significant change was found in free radical generation and in the activity of catalase, SOD and GPx in migraine patients. Univariate analysis of PMN catalase level revealed that migraineurs with a positive family history had significantly lower catalase activity compared with those with a negative family history. No correlation was found in the activity of antioxidant enzymes with age, duration of disease, time since last attack and headache index. The platelet SOD also did not show any significant change in patients of migraine without aura. Platelet aggregation in the presence or absence of PMNs was also not altered significantly. Thus the findings of the present study suggest that neutrophils are not the cause of oxidative stress observed in migraine patients.
Introduction
During the past several years, there has been a growing interest in the medical implications of free radicals. In certain situations excess production of free radicals can be neutralized by the defence mechanism of the body. This defence mechanism is dependent upon naturally occurring enzymes such as superoxide dismutase (SOD), glutathione peroxidase (GPx) and catalase (1). Although there are a number of intracellular sources of free radicals, the mitochondria are thought to be most important (2).
Clues from magnetic resonance studies (3) and DNA analysis (4) suggest that migraine, at least in a subset of individuals, may be the result of mitochondrial impairment. Episodic migraine-like headaches may occur in patients with MELAS (mitochondrial encephalopathy, lactic acidosis and stroke like episodes) syndrome which is caused by an A→G point mutation in the mitochondrial gene encoding for tRNA[Leu (UUR)] at nucleotide position 3243 (5). Some patients from Japan displayed an A→G point mutation in the coding region for the ND4 subunit of the respiratory complex I, another mitochondrial mutation potentially related to migraine (6). Migraine may thus be associated with a generalized disorder of mitochondrial oxidative phosphorylation and this may constitute a threshold for the triggering of migraine attacks (7).
The hypothesis of oxidative stress in migraine is supported by the findings of various studies (8–10). Direct evidence for the involvement of free radicals is difficult to obtain because of their intrinsic extreme reactivity, but can be done with electron spin paramagnetic resonance and flow cytometry using fluorescent dyes (11, 12). Hence the available evidence is largely of a derivative nature, consisting of elevated indices of lipid peroxidation markers, altered tissue antioxidant levels, and inhibition of adverse effects by free radical scavengers and redox-transition-metal chelators (1). A significant increase in the plasma levels of thiobarbituric acid reacting substances has been reported in migraine, suggesting that the ‘in vitro’ anomalous platelet behaviour seen in migraine may probably be related to an increased vulnerability to oxidative stress (8). Changes in platelet SOD have been reported in patients having migraine with aura (9). A recent study has reported a significant increase in urinary nitric oxide metabolites and lipid peroxidation by-products in migraine (10). Neutrophils are an important source of free radicals in the blood due to their capacity to generate free radicals following activation (13, 14). Oxidative metabolic burst of neutrophils can be assessed by cytochrome c reduction or by using fluorescent dyes (12, 15, 16). Among them flow cytometry is considered more specific as it measures only cell-specific fluorescence (12). The present study was therefore undertaken to measure the activity of antioxidant enzymes such as catalase, SOD and GPx in the blood polymorphonuclear neutrophils (PMNs) in migraine. In addition, to assess further the role of neutrophils in exerting the oxidative stress as reported in migraine patients, arachidonic acid-induced free radical generation as well as the effect of resting neutrophils on platelet activation was evaluated.
Patients and methods
Fifty-five migraine patients attending the Headache Clinic in the Neurology Out-patient Department of the Chhatrapati Shahuji Maharaj Medical University were the subjects for the present study. A detailed history was taken and thorough physical examination was done using a predesigned structured proforma. The diagnosis of migraine was based on the criteria given by the International Headache Society (17). The severity of headache was obtained by calculating the Headache Index (a product of frequency of attacks per month × duration of pain in hours × severity of pain). Severity of pain was measured by a three-point scale: 1, mild headache, does not interfere with daily routine; 2, moderate headache, patient can carry on his daily routine activity in spite of pain; 3, severe headache, interferes with the daily routine and patient has to take bed rest. The control group consisted of 60 healthy subjects (including relatives of patients, most of them being spouses of patients and healthy volunteers from the laboratory). A thorough headache history was taken in all the control subjects and none of them was suffering from a headache disorder. There was no history of a mitochondrial cytopathy (history of short stature, exercise tolerance, diabetes, seizure disorder, cardiomyopathy, etc.) in the subjects included in the study, nor had they taken analgesics, psychotropics or antidepressant drugs, ergot alkaloid or sumatriptan for at least 7 days prior to inclusion in the study. The patient characteristics are given in Table 1.
Patient characteristics
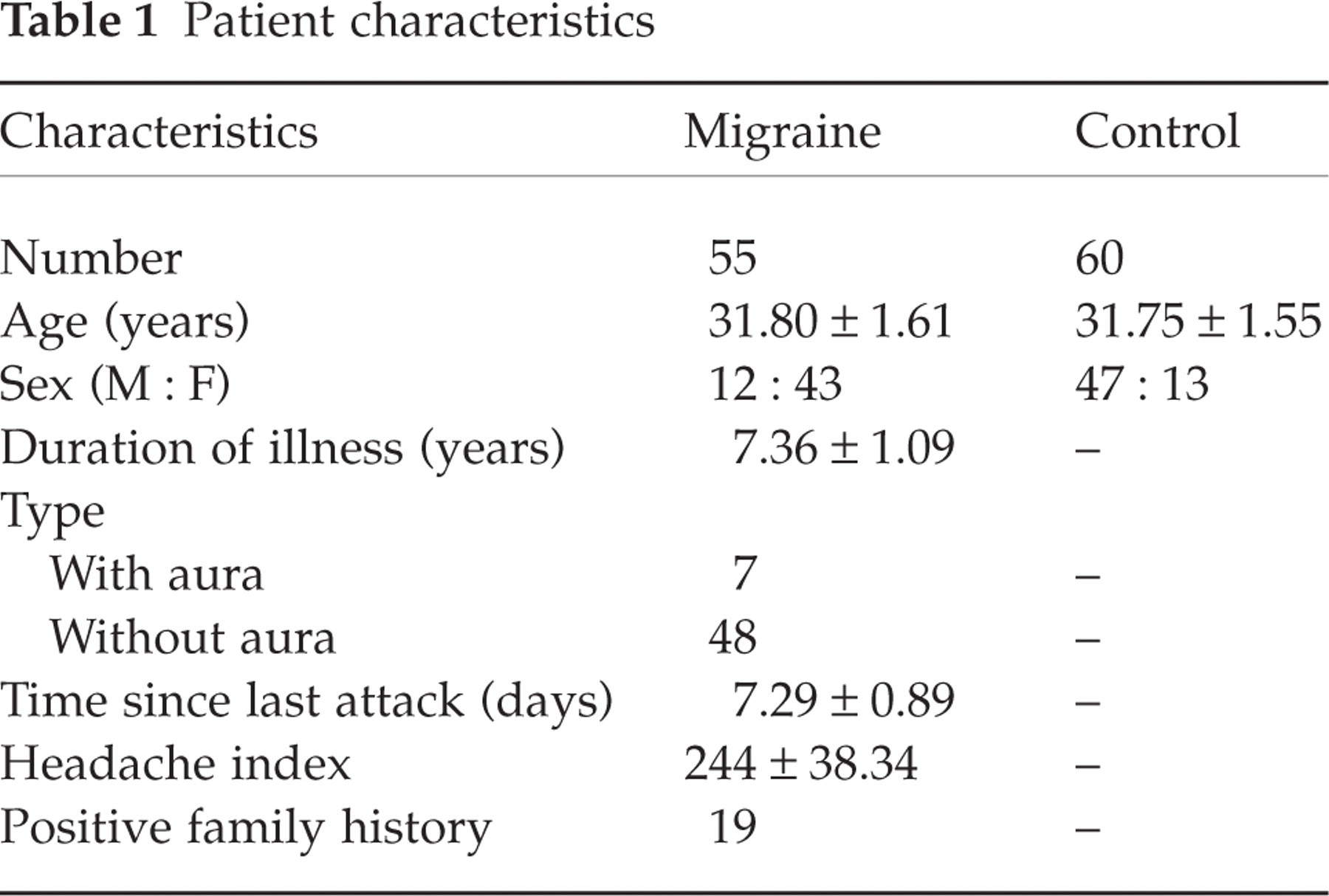
All subjects included in the study were normotensive with no evidence of anaemia, renal or hepatic dysfunction. Nutritional status of all the subjects included was normal (measured by skin fold thickness). None of the subjects had taken antioxidants, vitamins or nutritional supplements for at least 4 weeks prior to enrolment in the study.
Arachidonic acid (AA)-induced free radical generation from the neutrophils was measured in 21 patients and in 19 controls. The PMN catalase, SOD and GPx enzyme activity were estimated in 21, 26 and 12 migraineurs, respectively, while in the control group antioxidant enzyme activity was measured in 44 (catalase), 26 (SOD) and 18 (GPx) subjects, respectively. Platelet SOD was measured in 12 migraine patients and 10 controls. The reason for the variability in the number of samples for various antioxidant enzyme activities in migraine and controls was that the present study was undertaken as part of a multicentre study evaluating peripheral markers in migraine and the PMNs and platelets were also used for the receptor binding studies. The laboratory personnel involved in biochemical studies were unaware of the patients’ identity and did not know whether the sample was from a migraine patient or from a control subject.
Collection of blood samples
Blood (9 ml) was collected by venepuncture from the antecubital vein using a disposable plastic syringe with a 20 G needle between 08.00 h and 09.00 h and immediately transferred to plastic tubes containing 1 ml of 3.8% sodium citrate. It was transported to the Central Drug Research Institute within an hour for biochemical analysis.
Platelets and PMN isolation
Platelets and PMNs from normal age-matched controls and patients were obtained from the venous blood collected in sodium citrate (0.129 M, pH 6.5, 9 : 1 v/v). Platelet-rich plasma (PRP) was removed by centrifugation at 250
Flow cytometric analysis of free radical generation
PMNs (1 × 105 cells) were equilibrated in 850 µl of HBSS with 50 µl DCFDA (2′ 7′dichloroflourescein diacetate, 10 µM) for 5 min at 37 °C. One group of PMNs was left unstimulated while the other group was stimulated with arachidonic acid (AA, 2 µM). Reactive oxygen species (ROS) generation was induced by AA (2 µM) and the cells were further incubated for 15 min at 37 °C. During flow cytometric analysis, individual granulocytes were discerned by the combination of low angle forward scattered and right angle scattered laser light; aggregating cells and other cell types and debris were excluded from the analysis. The fluorescence of 10 000 cells from both control cells and AA-stimulated cells was determined by a FACS Calibur (Becton Dickinson, San Jose, CA, USA) using the Cell Quest Software (Becton Dickinson). AA-induced free radical generation from PMNs has been represented as stimulation index (SI), which is the ratio of the mean fluorescence of the stimulated and unstimulated cells as described earlier (19, 20). Release of free radicals on stimulation of PMNs with AA led to increased mean fluorescence and SI in the control and migraine group.
Antioxidant enzyme activities
Catalase
A 10-µl PMN (1 × 107 cells/ml) supernatant was added to the buffered substrate (50 mM phosphate buffer pH 7.4, containing 10 mM H2O2) to make a total volume of 3 ml. Decrease in absorbance was monitored at 240 nm for 2.5 min at intervals of 15 s at 37 °C. The activity was calculated using H2O2 extinction coefficient 0.041/µmol per cm2 at 240 nm (21).
Superoxide dismutase
SOD activity was estimated following the procedure of Kakkar et al. (22). Assay mixture contained sodium pyrophosphate buffer (0.052 M, pH 8.3), phenazine methosulphate (PMS; 186 µM), nitroblue tetrazolium (NBT; 300 µM) and 100 µl of PMNs (1 × 107 cells/ml) supernatant. Samples were incubated for 5 min at 37 °C before the addition of reduced nicotinamide adenine dinucleotide (NADH; 780 µM). The mixture was further incubated for 120 s at 37 °C and 1.0 ml glacial acetic (17.4 M) was added to stop the reaction. The violet colour developed was extracted in 4.0 ml of n-butanol and absorbance of the butanol layer was measured at 560 nm against reagent blank. One unit of SOD was found to inhibit the chromogen generation by 50% in these assay conditions.
Glutathione peroxidase
Glutathione peroxidase was measured according to the spectrophotometric method (Lemaitre et al. (23)). The assay mixture consisted of 50 mM Tris–HCl, 0.1 mM EDTA pH 7.6, containing 2 mM glutathione (GSH), 0.14 mM nicotinamide adenine dinucleotide phosphate (NADPH) and 0.7 U/ml glutathione reductase. Fifty millilitres of PMN supernatant (1 × 107 cells/ml) were incubated at 37 °C along with assay mixture for 2 min. Reaction was initiated by addition of 0.2 mM tetra-butyl-hydroperoxide and absorbance was read at 340 mm for 2.5 min on a spectrophotometer. Activity was calculated using molar extinction coefficient for NADPH, 6.22/cm2 per µmole for NADPH.
Platelet aggregation
Blood was collected in sodium citrate (3.8% w/v; 9 : 1 v/v) and centrifuged at 200
Materials
ADP, AA, nicotinamide adenine dinucleotide phosphate-reduced form (NADPH), nicotinamide adenine dinucleotide reduced (NADH), N-(1-naphthyl) ethylene diamine, NBT, PMS, phosphoric acid, sodium pyruvate, sulfanilamide, and Histopaque (1077 and 1119) were purchased from Sigma Chemical Co. (St Louis, MO, USA). All other chemicals used in the study were of analytical grade (SRL, Bombay, India).
Statistical analysis
Antioxidant enzyme activity has been reported as mean ± SEM. The data for enzyme activities did not have normal distribution, so Mann–Whitney test was used to make comparisons between the control group and migraine patients. Platelet aggregation and free radical generation were analysed by Student's t-test. Univariate analysis of the clinical features of migraine and catalase activity was done. Correlation coefficient (r) was evaluated for correlation between the activity of catalase, SOD and GPx with age, duration of disease, time since last attack and severity of headache (determined by headache index). P-values < 0.05 were considered statistically significant.
Results
The subjects included in the control and study group were not age and sex matched, so the data for free radical generation and antioxidant enzyme activity in the controls were first analysed with respect to age and sex. Activity of SOD (M : F, 36.5 ± 10.7 U/108 cells and 66.4 ± 45.6 U/108 cells), catalase (M : F, 2.5 ± 0.4 mmol of H2O2 utilized/min per 108 cells and 1.4 ± 0.4 mmol of H2O2 utilized/min per 108 cells), GPx (M : F, 1.7 ± 0.3 nmol of NADPH utilized/min per 108 cells and 2.6 ± 1.1 nmol of NADPH utilized/min per 108 cells) and AA-induced free radical generation with respect to sex was also not significantly altered. There was also no correlation between the age of the subjects and levels of free radical generation, catalase (r = 0.23), SOD (r = 0.02) and GPx (r = 0.10).
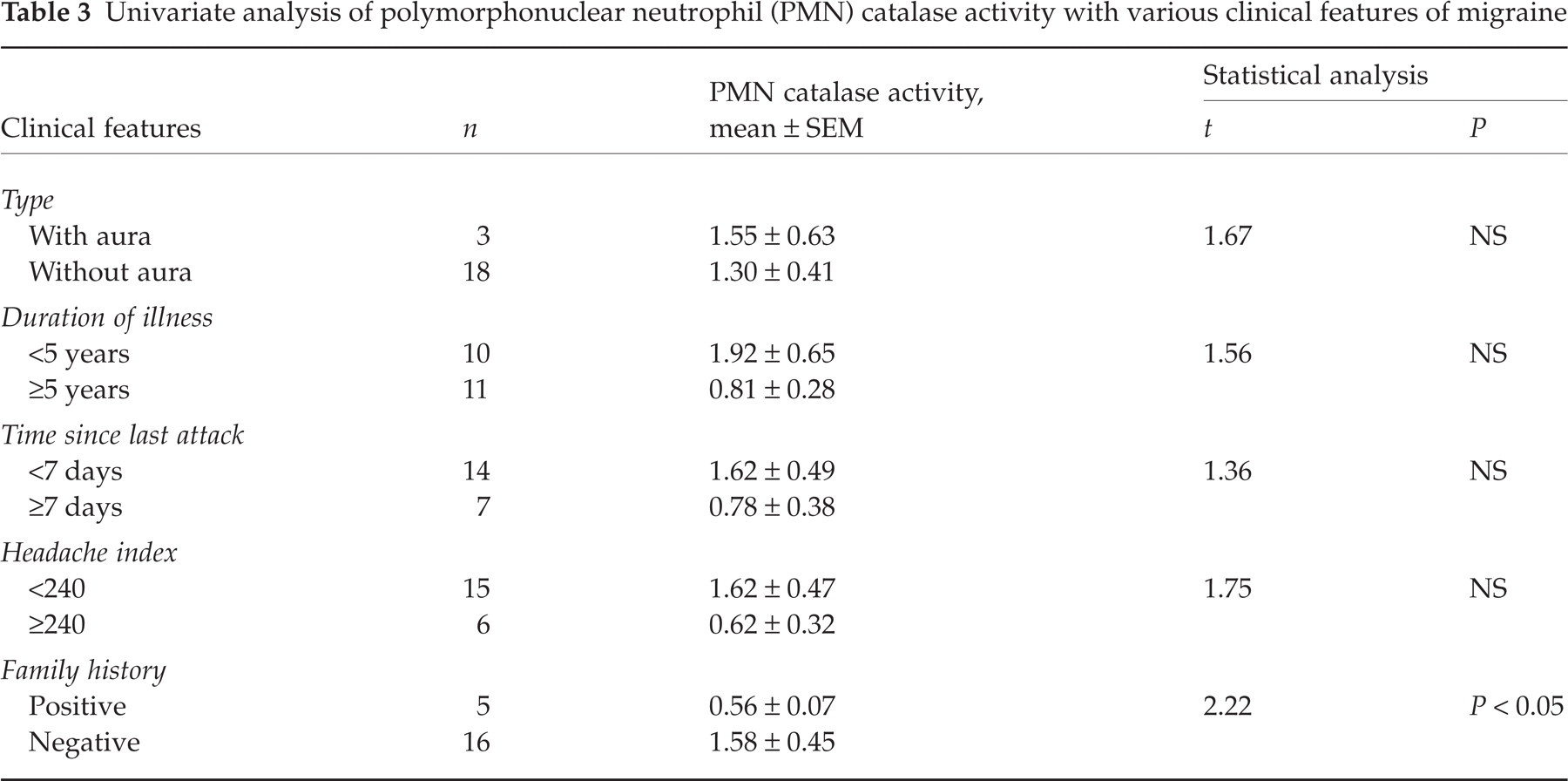
In migraine patients no significant decrease in the activity of catalase, SOD and GPx was found (Table 2). AA-induced stimulation represented as SI was also not altered significantly in the migraine patients (Fig. 1). There were four migraine with aura patients and 17 migraine without aura patients and the mean SI in both these groups was 1.35 ± 0.43 and 2.26 ± 0.28, respectively. There was no significant difference between these two groups. Univariate analysis of the various clinical features of migraine and PMN catalase activity revealed that migraineurs with a positive family history had significantly lower activity of catalase enzyme compared with those with a negative family history (Table 3). No correlation was observed between age, duration of disease, time since last attack, and headache index and antioxidant enzyme activity (Table 4). The platelet SOD was also measured in 12 migraine without aura patients and 10 controls. Migraineurs had decreased activity (1.70 ± 0.25 U/108 cells) compared with controls (2.62 ± 1.06 U/108 cells); however, the difference was not statistically significant. Platelet aggregation induced by ADP was not altered significantly in the presence or absence of PMNs (1 × 106 cells) (Fig. 2).

Arachidonic acid-induced free radical generation represented by stimulation index in patients with migraine and controls.
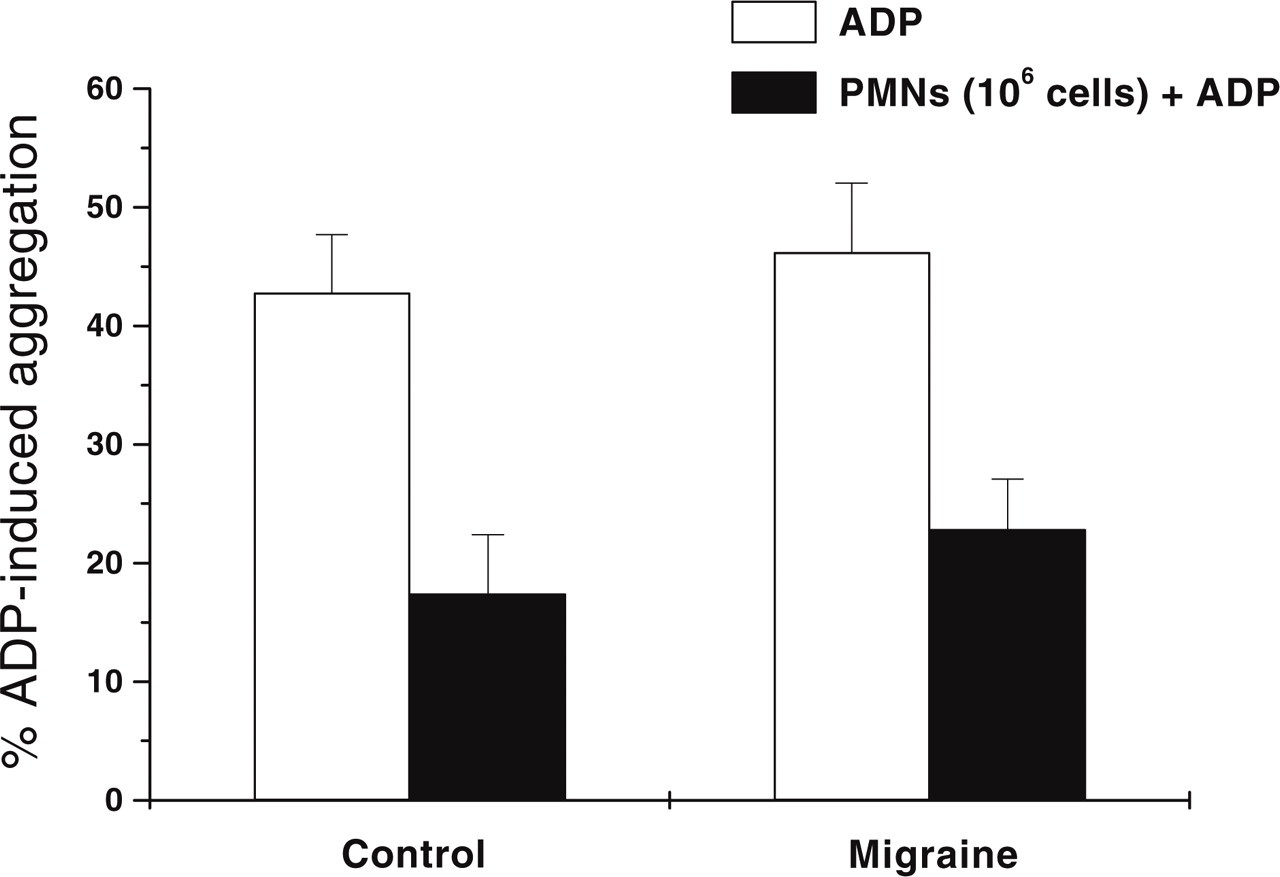
Histogram representing adenosine-5′-diphosphate (ADP)-induced platelet aggregation in patients with migraine and controls.
Antioxidant enzyme activity in polymorphonuclear neutrophils in migraine

Univariate analysis of polymorphonuclear neutrophil (PMN) catalase activity with various clinical features of migraine
Correlation of antioxidant enzyme activity in polymorphonuclear neutrophils with clinical features in migraine

Discussion
In the present study no significant change was observed in AA-induced free radical generation from circulating PMNs or in the activity of antioxidant enzymes such as catalase, SOD and GPx in PMNs of migraine patients compared with controls.
Shimomura et al. (9) have reported a significant reduction in platelet SOD concentrations in migraine with aura and migraine without aura, while platelet SOD activity was reduced only in migraine with aura patients. Platelet SOD activity in the present study was measured by the same method as that of Shimomura et al. (9) and the values observed in controls as well as in migraine without aura patients were similar to those reported here. However, we did not measure the protein level of SOD, and migraine with aura patients could also not be evaluated for SOD activity due to sample constraint, and will be investigated in future studies. Thus our studies are in agreement with the Shimomura study (9), that SOD activity in the platelets was not altered in migraine without aura patients.
A significant increase in the plasma levels of thiobarbituric acid-reactive substances was found by Tozzi-Ciancarelli (8). It was possibly responsible for increased rigidity, reduced cytosolic calcium in the resting and thrombin-stimulated cells and decreased aggregating response of platelets to ADP and collagen (8). Reactive oxygen and nitrogen species released from the neutrophils could be an important source and cause of oxidative stress in the blood. The present study investigated the possibility that PMNs might be involved in the oxidative stress in migraine patients due to their capacity to generate large concentrations of free radicals (3). Free radicals are known to affect the reactivity of platelets. Platelet activation was therefore monitored in the present study in the presence and absence of PMNs and was not altered significantly, suggesting that alterations in platelet activation as reported in the migraine patients was not due to PMNs. However, in the present study activation of platelets also did not exhibit any significant difference in the control and migraine patients. Our study comprised only four patients with aura, and more migraine with aura patients should be investigated for alterations of platelet activation.
It is also well documented that nitric oxide (NO) produced by neutrophils exerts an anti-aggregatory effect on platelets. One can postulate that if less NO is produced by neutrophils, it might increase the movement of these cells towards the site of inflammation, as NO donors inhibit neutrophil mobility and chemotaxis (25) and thus increase the probability of involvement of these cells, if any, in migraine. Second, the less NO might be responsible for the hyperactivation of platelets, as observed by many workers during migraine (26). We did not observe these changes in the status of NO and platelet activation in migraineurs during the headache-free period (27).
PMNs following activation generate both oxygen and nitrogen-derived radicals, which might lead to oxidative stress. We therefore measured release of free radicals from the activated PMNs, which was not altered significantly. In the present study we used AA, which is a direct activator of NADPH oxidase activity (28). There was no significant change in the AA-induced free radical generation in migraine patients compared with controls. Antioxidant enzyme activity in the PMNs was also not changed in the migraine patients. Subgroup analysis, however, revealed that migraineurs with a positive family history of migraine had a significantly lower activity of catalase in the PMNs compared with those with a negative family history. On the basis of the results obtained in the present study it is difficult to explain the decrease in catalase activity. Further studies are required to explore the transcriptional or post-translational modifications of catalase activity in migraineurs with a positive family history.
The results obtained from the present study suggest that the increased oxidative stress reported by various workers in migraine patients may possibly not be due to the circulating neutrophils. However, more work is needed in the Indian population to either support or refute the hypothesis of oxidative stress in migraineurs.
Footnotes
Acknowledgements
A financial grant from Department of Biotechnology, New Delhi, India to support this multicentre study is gratefully acknowledged.
