Abstract
Introduction:
Single anastomosis duodenoileal bypass with sleeve gastrectomy (SADI-S), a modification of biliopancreatic diversion with duodenal switch, reduces the number of anastomoses and lengthens the common limb, mitigating short- and long-term complications related to other bilio-diverting procedures. 1 As recently reported, SADI-S achieves and maintains significant weight loss along with improvements in metabolic health. 2 However, it is a technically demanding procedure requiring extensive experience in bariatric and minimally invasive surgery. 3 This video reports a step-by-step SADI-S technique, performed on a 49-year-old male, with a body mass index (BMI) of 48 kg/m2 and multiple comorbidities including type 2 diabetes and hypertension.
Methods:
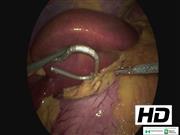
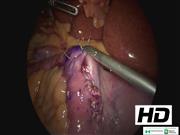
The patient is placed in a supine position, with legs apart, with the first surgeon positioned between the legs and one assistant on each side of the patient's abdomen. Six ports are placed as follows: a 12 mm trocar along the midline, 15 cm below the xiphoid process and 3 cm on the left side; 15 and 12 mm trocars at the same level on the right and left sides along the midclavicular lines; two 5 mm trocars along the anterior axillary lines along the costal margin bilaterally and symmetrically; and the last 5 mm trocar in the subxiphoid position. A sleeve gastrectomy is performed starting 6 cm from the pylorus and proceeding until the gastric fundus and the left diaphragmatic crus is divided (UltraCision, Ethicon Endosurgery, Cincinnati, OH). The gastric tube is fashioned on a calibrated probe of at least 45 Fr, using 60 mm staplers reinforced with polyglycolic acid. The pylorus and the first part of the duodenum are isolated, using the gastroduodenal artery as a landmark for dissection. The duodenum is transected 2–3 cm distal to pylorus. The first surgeon moves to the patient's left side. The small bowel is measured 250 cm from the ileocecal valve. A duodenoileal end-to-side hand-sewn anastomosis is fashioned with double-strand adsorbable running suture. An air-blue test is performed. Specimen extraction was done by minilaparotomy at the left 15 mm trocar.
Results:
Operative time was 190 minutes without intra-/postoperative complications. Clear liquids were given on postoperative day (POD) 1. Upper gastrointestinal series was obtained on POD 2, before starting a soft diet. Nutritional evaluation was provided before patient's discharge, which occurred on POD 5. Outpatient care included follow-up at 1, 3, 6, 9, and 12 months. After 12 months, the patient achieved a weight loss of 67 kg, with a final BMI of 20.7 kg/m2 and his medications for hypertension and diabetes were discontinued. He had no nutritional deficiencies.
Conclusion:
Owing to its technical features, we recommend bariatric surgeons and their multidisciplinary teams undertake extensive technical and medical training before embarking in SADI-S. A larger experience is needed to determine the role of this technique as a primary or conversion bariatric surgery.
Source of Work:
Video article of surgical practice.
Additional Declarations:
No previous presentations of this abstract occurred.
Acknowledgment:
The authors thank Letizia Maria Lasi for her valuable contribution to video editing.
No competing financial interests exist.
Runtime of video: 9 mins 20 secs

Keywords
Get full access to this article
View all access options for this article.
